MECHANICAL VENTILATION INTUBATION n Endotracheal Intubation n n

MECHANICAL VENTILATION
INTUBATION n Endotracheal Intubation: n n Placement of tube into trachea through mouth or nose Indications: Upper airway obstruction n Facilitate secretion removal n For positive pressure ventilation n
Endotracheal Tube
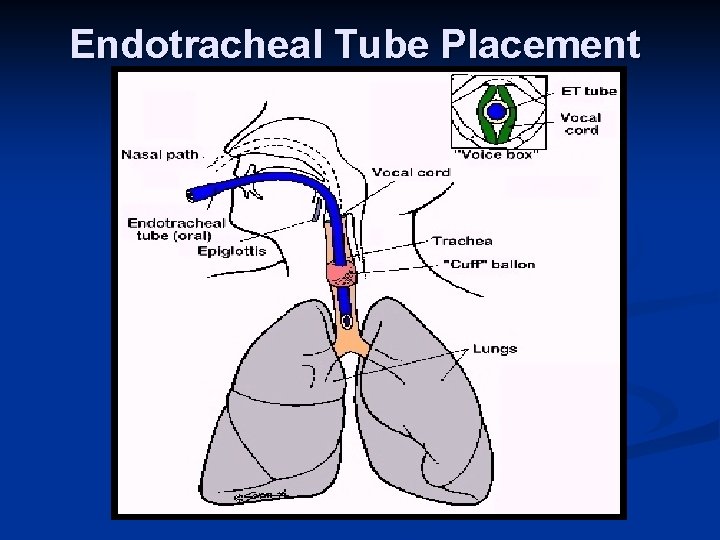
Endotracheal Tube Placement

Complications of Endotracheal Intubation n Improper placement n Esophageal intubation n Right mainstream intubation n Management: auscultate, CXR, bilateral respiration, mark point at lips/nose

Complications of Endotracheal Intubation n Cuff problems n Ineffective seal leads to aspiration n Too much pressure leads to tracheal necrosis n Use minimal occluding volume (keep pressure <20 mm Hg) n Suction throat before deflation

Nursing Role: Intubation Maintain correct placement n Maintain proper inflation n Maintain/monitor ventilation and oxygenation n Maintain tube patency n Mouth care; repositioning ET; promote communication n

Complications of Extubation n Laryngeal edema or spasm n Respiratory failure

Mechanical Ventilation n Air/O 2 moves in and out of lungs via machine n Types Ventilators n n n Negative Pressure Positive Pressure* Ventilator Settings n n n Rate Tidal volume FIO 2 Pressure limit PEEP Alarms etc

Mechanical Ventilation n Three types Positive Pressure Ventilators Volume-cycled: terminates breath when preset volume delivered n Time-cycled: terminates breath after preset time elapsed n Pressure-cycled: terminates when present airway pressure achieved n

Volume-Cycled Ventilators: Modes n Controlled mechanical ventilation n Preset volume n Preset rate n Unable to trigger (initiate a breath)

Volume-Cycled Ventilators: Modes n Assist-Control n Preset ventilation volume n Present rate n Can trigger and receive more than preset rate n Patient-triggered breaths are delivered at preset volume

Volume-Cycled Ventilators: Modes n Synchronized Intermittent Mandatory ventilation (SIMV) n Preset volume and rate n Spontaneous breathing n Spontaneous breaths not assisted (patient’s own volume) n Often used for weaning

n PEEP n n Other Ventilation Maneuvers Positive end-expiratory pressure Application positive pressure during ventilation n Increases distension of alveoli n Prevents alveolar collapse n “Recruits” previously collapsed alveoli

Other Ventilation Maneuvers n PEEP n n n Increases surface area available for gas exchange Allows delivery lower FIO 2: reducing risk O 2 toxicity Complications n n Reduced CO Barotrauma
Other Ventilation Maneuvers n CPAP n n n Continuous positive airway pressure Continuous (i. e. , inspiration and expiration) positive pressure applied to airway For spontaneously breathing patients

Other Ventilation Maneuvers n Pressure Support Ventilation (PSV) Positive pressure applied only on inspiration n Applied to spontaneous breaths only n Supports inspiratory effort n Patient determines inspiratory length and rate n Often used for weaning n

Mechanical Ventilation: Complications n CVS Increased intrathoracic pressure n Reduced CO n n Pulmonary n Barotrauma (trauma d/t pressure) n Pneumothorax n Pneumomediastinum n Subcutaneous emphysema

Mechanical Ventilation: Complications n Pulmonary n Alveolar hypoventilation n Cuff leak n Ventilator settings n Secretions n Atelectasis

Mechanical Ventilation: Complications n Pulmonary n Alveolar hyperventilation n Due to hypoxemia, fear, pain, anxiety → alkalosis n n Due to inappropriate ventilator settings n n n RX: sedate, analgesia, communication, correct hypoxemia high tidal volume High rate Pulmonary Infection n Upper airway defenses bypassed

Mechanical Ventilation: Complications n n Neurological complications n Positive pressure ventilation → increased intrathoracic pressure n interferes with venous drainage; increased ICP GI n Stess ulcers and GI bleeds; Rx with H 2 receptor blockers n MV → Gastric and bowel dilation

Mechanical Ventilation: Complications n Musculoskeltal n Muscle n n n atrophy d/t immobilization Mobilize ROM Psychologic n Stress n Communication very important n Sedate, explain, family visits, pain management n Facilitate expression of needs

Weaning n Criteria Effective cough n Adequate respiratory muscle strength n

Weaning n Approaches to weaning T-piece (spontaneous breathing for short periods of time) n SIMV, PSV n

Weaning n Monitor closely n resp rate n accessory muscle use n shallow respirations n paradoxical breathing n ABGs n n n rising PCO 2 → acidosis falling PO 2 BP (↓ or ↑) LOC (restless, tiring, somnolence, anxiety) Pulse oximeter
- Slides: 25