Mechanical Ventilation 101 An Introduction to Ventilatory Support













- Slides: 16

Mechanical Ventilation 101 An Introduction to Ventilatory Support

OBJECTIVES The student will be able to: u – – – – – State the two purposes of mechanical ventilation. List three indications for mechanical ventilation. State the primary reason for oxygenation failure. List three complications of mechanical ventilation. Differentiate between positive and negative pressure ventilation. Differentiate between invasive and non-invasive ventilation. Differentiate between pressure- and volume-based breaths. Describe how the mode of ventilation is related to patientventilation interaction. Differentiate between minute ventilation and alveolar ventilation. Describe the relationship between alveolar ventilation and Pa. CO 2.

OBJECTIVES u u u u u The student will be able to: State the two purposes of mechanical ventilation. List three indications for mechanical ventilation. State the primary reason for oxygenation failure. List three complications of mechanical ventilation. Differentiate between positive and negative pressure ventilation. Differentiate between invasive and non-invasive ventilation. Differentiate between pressure- and volume-based breaths. Describe how the mode of ventilation is related to patientventilation interaction. Differentiate between minute ventilation and alveolar ventilation.

OBJECTIVES u u u u u The student will be able to: Describe the relationship between alveolar ventilation and Pa. CO 2. State the two primary methods for controlling alveolar minute ventilation. State the normal range for spontaneous tidal volume. State the normal range for tidal volume during mechanical ventilation. List the four primary causes of hypoxemia. State two methods for improving Pa. O 2. Describe how Pa. CO 2 is managed in patients with chronic airflow obstruction. Describe how Pa. O 2 is managed in patients with chronic airflow obstruction.

Purposes of Mechanical Ventilators u TWO FUNCTIONS: – – u Remove Carbon Dioxide Deliver Oxygen Ventilate (Decrease Pa. CO 2) – WOB is excessive • • – – u Increased airway resistance Reduced lung compliance Defect with neuromuscular control Post-operative support Oxygenate (Increase Pa. O 2 [Sa. O 2]) – Shunt

Effects of Positive Pressure Ventilation u Increased – – – airway pressures Reduction in venous return/cardiac output. Reduced renal blood flow. Cerebral blood flow issues. u Airway related issues

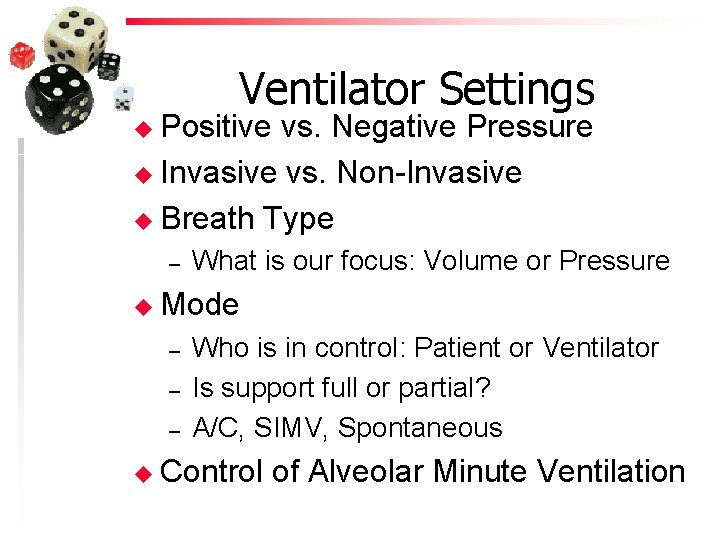
Ventilator Settings u Positive vs. Negative Pressure u Invasive vs. Non-Invasive u Breath Type – What is our focus: Volume or Pressure u Mode – – – Who is in control: Patient or Ventilator Is support full or partial? A/C, SIMV, Spontaneous u Control of Alveolar Minute Ventilation

Alveolar Minute Ventilation. u Pa. CO 2 levels are inversely related to VA – – u Minute Volume (VA) is (Tidal Volume minus Deadspace Volume) x respiratory rate. – – u Increase minute volume, decrease Pa. CO 2. Decrease minute. volume, increase Pa. CO 2. (Vt – Vd) x f Deadspace includes anatomic (doesn’t change), mechanical (stuff we add), and alveolar (�without �). We can control alveolar minute ventilation by: – – Changing Respiratory Rate (f) Changing Tidal Volume

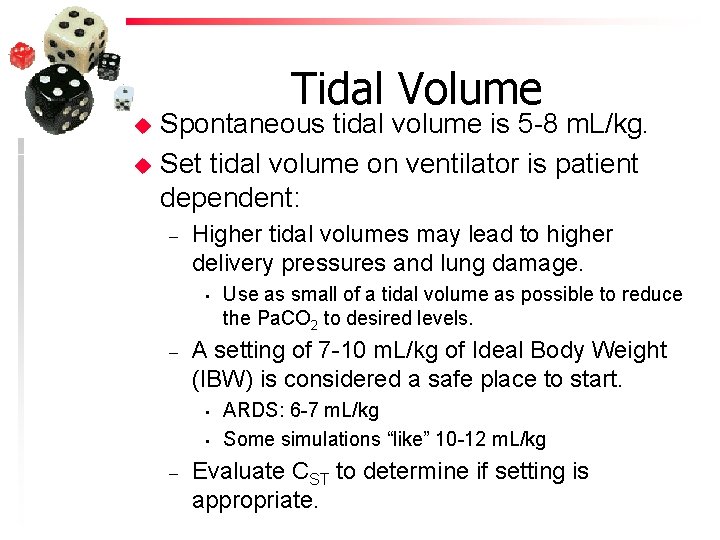
Tidal Volume u u Spontaneous tidal volume is 5 -8 m. L/kg. Set tidal volume on ventilator is patient dependent: – Higher tidal volumes may lead to higher delivery pressures and lung damage. • – A setting of 7 -10 m. L/kg of Ideal Body Weight (IBW) is considered a safe place to start. • • – Use as small of a tidal volume as possible to reduce the Pa. CO 2 to desired levels. ARDS: 6 -7 m. L/kg Some simulations “like” 10 -12 m. L/kg Evaluate CST to determine if setting is appropriate.

Oxygenation Issues u Causes – – – of Hypoxemia Reduced barometric pressure (move) Hypoventilation (ventilate). . V/Q imbalance (responds to increased Fi. O 2) Diffusion Defect (find cause and correct? ) Intrapulmonary Shunt • RECRUIT COLLAPSED ALVEOLI

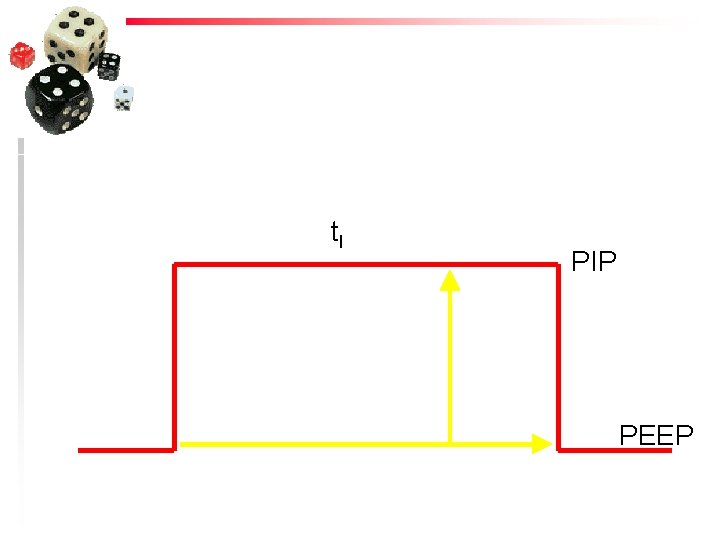
Steps in Correcting Pa. O 2 u Increase F i. O 2 u Increase Mean Airway Pressure – – “Space under the table” Increase starting pressure (PEEP) Increase delivery (ending) pressure (PIP) Lengthen inspiratory time (t. I)

t. I PIP PEEP

Mechanical Ventilation: COPD & Asthma u Treat increased Pa. CO 2 (and low p. H) – Use caution with increasing tidal volume. • • Increased RV leads to overdistension. Extend expiratory time. – Auto PEEP Shorten inspiratory time (increase inspiratory flow rate). – Use respiratory rate to control Pa. CO 2. • – – u Control patient (? ) pharmacologically. Permissive hypercapnia and acidosis. Treat reduced Pa. O 2 – – . . Usually a result of hypoventilation and V/Q imbalance. Responds well to increase in Fi. O 2.

u 5’ 10” male admitted to ICU. u Determine Ventilator settings – – – Mode Tidal Volume Respiratory Rate FIO 2 PEEP

u ABG – p. H: 7. 31, Pa. CO 2: 50, Pa. O 2: 60, HCO 3: 26

u ABG: – p. H: 7. 38, Pa. CO 2: 38, Pa. O 2: 62, HCO 3: 27