Measuring blood lactate Lactate n Lactate production is
Measuring blood lactate

Lactate n Lactate production is a normal physiologic process and occurs in all animals n n its presence does not indicate disease A key indicator of hypoxia Correlates with mortality Lactate can also be used to characterize fitness levels
SUGAR OXYGEN CO 2 and WATER ENERGY
Anaerobic conditions: without oxygen SUGAR OXYGEN CO 2 and WATER ENERGY LACTATE

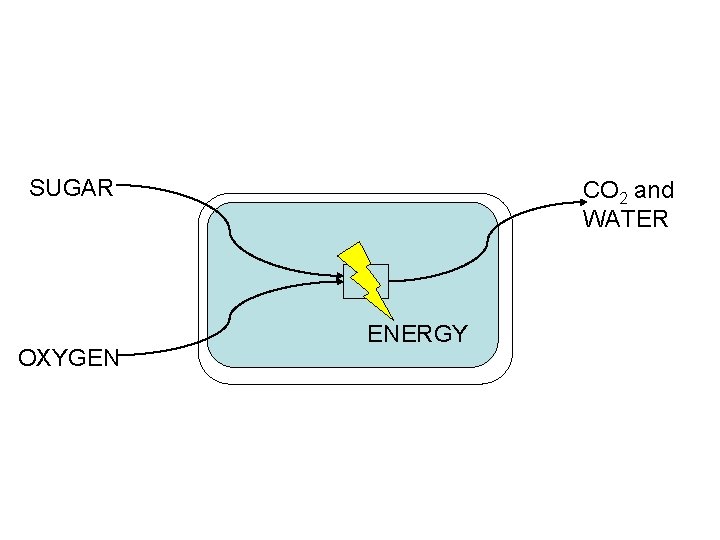
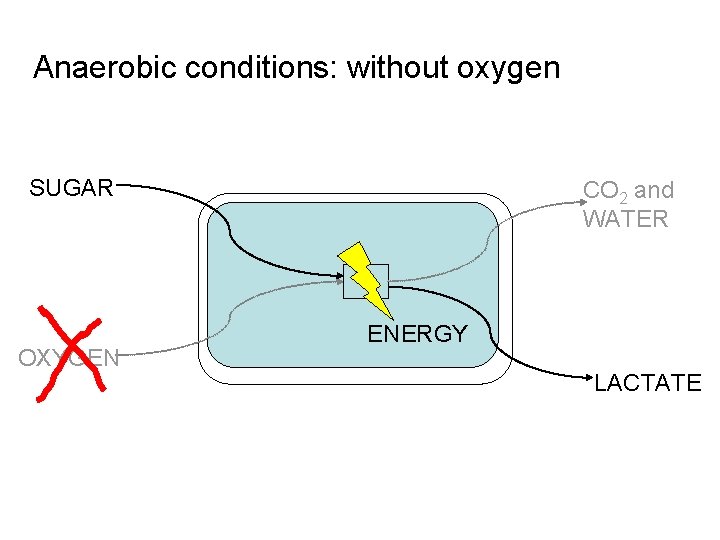
Why do cells make lactate? n n n Cells consume oxygen in a process that produces energy When the oxygen supply is insufficient (anaerobic conditions) cells produce energy by another pathway that results in the production of lactate Lactate accumulation is the price to be paid for maintaining energy production under anaerobic conditions

A clinical example Dog with gastric dilatationvolvulus (GDV) n A relatively common abdominal catastrophe requiring aggressive stabilisation and surgery n A vet’s nightmare n
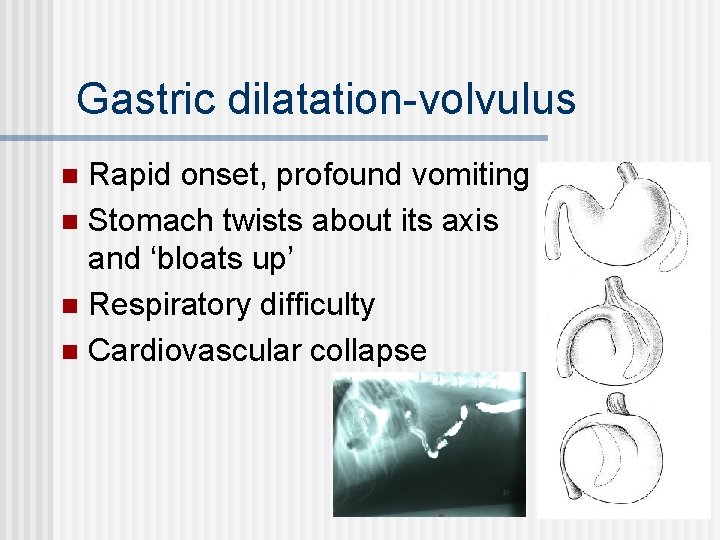
Gastric dilatation-volvulus Rapid onset, profound vomiting n Stomach twists about its axis and ‘bloats up’ n Respiratory difficulty n Cardiovascular collapse n

Gastric dilatation-volvulus n Lactic acidosis from hypoperfusion n Initial rise after restoring circulation n If it fails to fall rapidly, then you have not fully restored oxygen delivery n With GDVs, it is a strong indicator of likely outcome +1 hour +3 hours +2 hours +4 hours

Do not over interpret the result n n Vets (and owners) want tests that tell them the likely outcome Magnitude of elevation corresponds to the severity of the underlying problem Generally, severe disease is associated with poor prognosis (likely outcome) However, some severe diseases are easily treatable

Lactate trends n n High lactate levels: the patient’s condition warrants aggressive treatment Serial evaluation is a must A decreasing trend towards normal is a good sign A rising trend in the face of aggressive treatment is a very poor sign +1 hour +3 hours +2 hours +4 hours
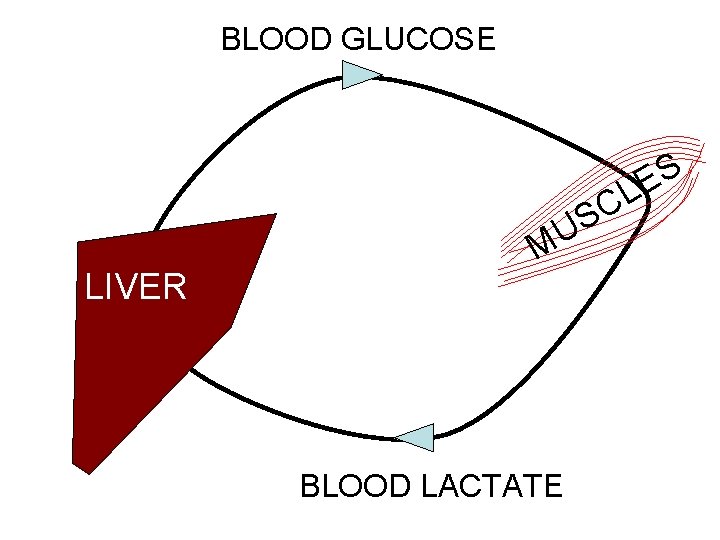
BLOOD GLUCOSE S E CL S U LIVER M BLOOD LACTATE
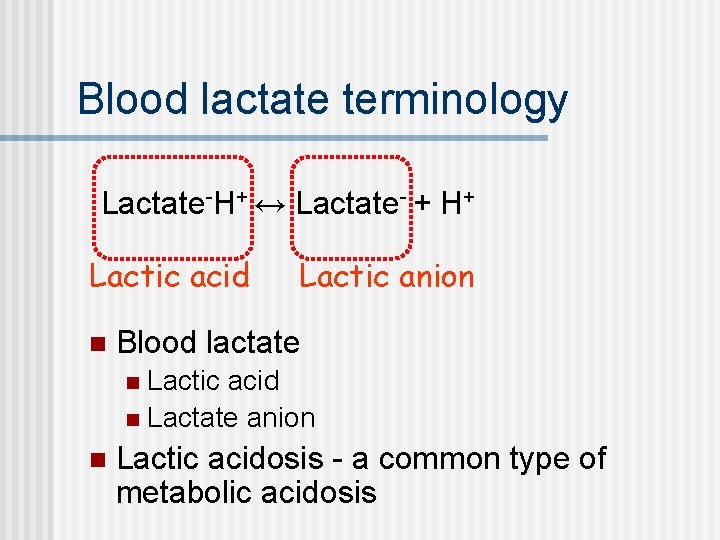
Blood lactate terminology Lactate-H+ ↔ Lactate- + H+ Lactic acid n Lactic anion Blood lactate Lactic acid n Lactate anion n n Lactic acidosis - a common type of metabolic acidosis
Blood sampling n n Arterial blood is best Venous blood drawn from a central venous catheter is essentially equivalent Restraint and prolonged venous occlusion cause mild increases Venous blood drawn from a peripheral site should be interpreted with caution
Handling blood samples Do NOT use serum n Separate plasma within 5 minutes n n n lactate values can increase if sample stay in contact with RBCs Only useful if fast turn around

Avoiding confused vets n Does not replace acid-base analysis there are other types of metabolic acidosis n does not look at respiratory component n poor correlation between blood lactate concentration and magnitude of metabolic acidosis n

Avoiding confused vets n Hartmann’s fluid a. k. a. Lactated Ringer’s Solution or Compound Sodium Lactate n a treatment for mild metabolic acidosis n lactate converted by the liver to bicarbonate n
Respiratory/blood gases cassette

Respiratory/blood gases cassette n Na+, K+, Cl-, HCO 3 -, anion gap, p. H, p. CO 2, TCO 2, p. O 2 n Use this cassette for patients with respiratory and cardiovascular disorders, advanced anesthetic cases and all patients on ventilators to improve their chances of success in critical situations. Assess respiratory and breathing abnormalities Monitor cardiovascular and respiratory functions Assess a critical patient’s need for supplemental oxygen immediately Monitor oxygen and respiratory function n n

Respiratory/blood gases cassette Na+, K+, Cl-, HCO 3 -, anion gap, p. H, p. CO 2, TCO 2, p. O 2 n Electrolytes and acid-base (like the fluid therapy/acid-base cassette) but also gives p. O 2 n Use this one whenever you are questioning the content of oxygen in the patient’s arterial blood n
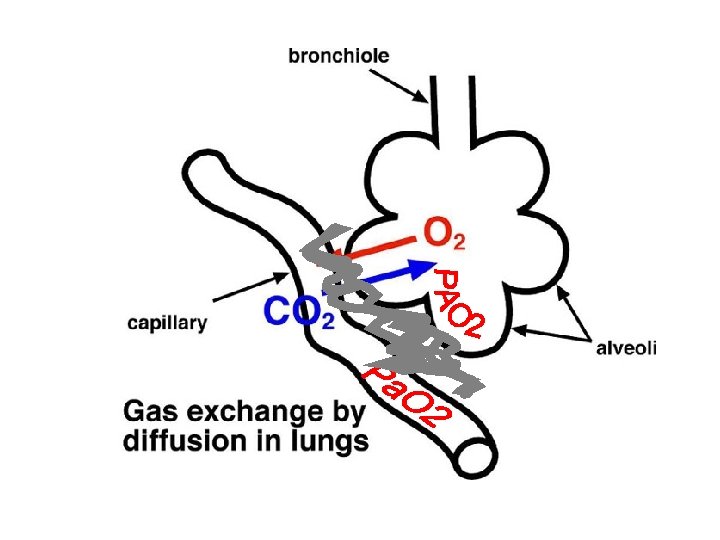
Why do we need to do blood gases? An arterial blood sample is useful for assessment of: 1. alveolar ventilation 2. oxygenation 3. acid-base balance

Our first example… Eight-year-old Labrador n Increased respiratory rate n Chest x-ray: no abnormality detected n Previously treated with oxygen n
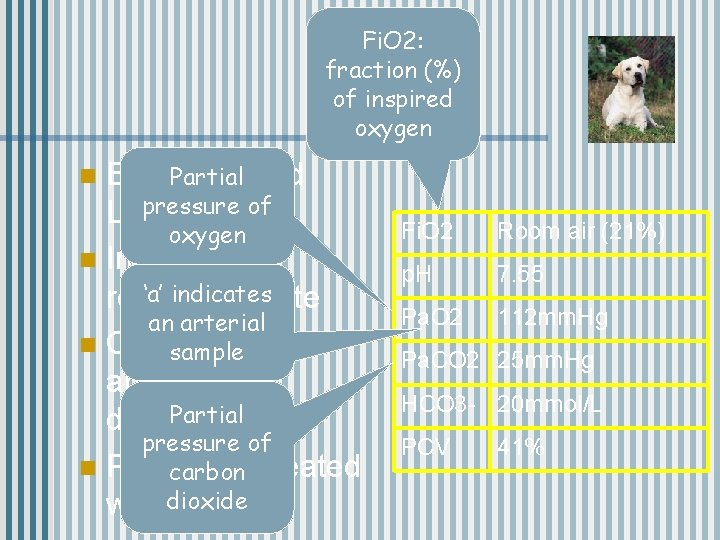
Fi. O 2: fraction (%) of inspired oxygen Eight-year-old Partial pressure of Labrador oxygen n Increased ‘a’ indicatesrate respiratory an arterial n Chest x-ray: no sample abnormality Partial detected pressure of n Previously carbon treated with dioxide oxygen n Fi. O 2 Room air (21%) p. H 7. 55 Pa. O 2 112 mm. Hg Pa. CO 2 25 mm. Hg HCO 3 - 20 mmol/L PCV 41%
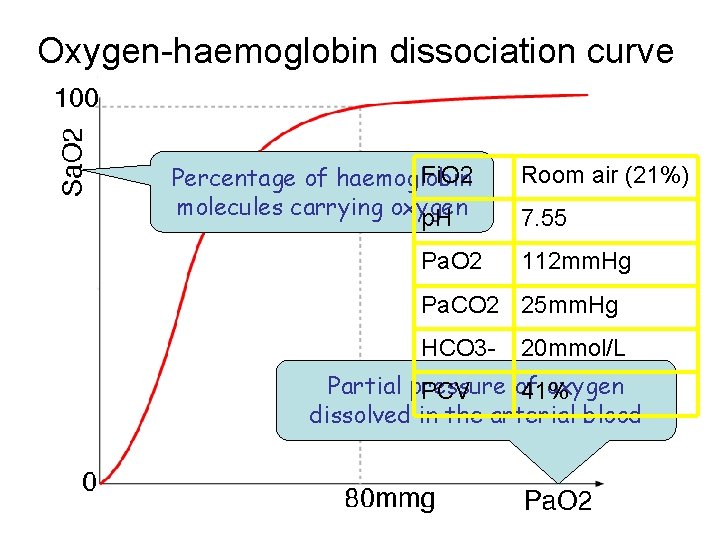
Oxygen-haemoglobin dissociation curve Fi. O 2 Percentage of haemoglobin molecules carrying oxygen p. H Pa. O 2 Room air (21%) 7. 55 112 mm. Hg Pa. CO 2 25 mm. Hg HCO 3 - 20 mmol/L Partial pressure of oxygen PCV 41% dissolved in the arterial blood

How did the blood gas help? n High p. H and low Pa. CO 2 are consistent with respiratory alkalosis n ? pain ? fear n Changed direction of the treatment
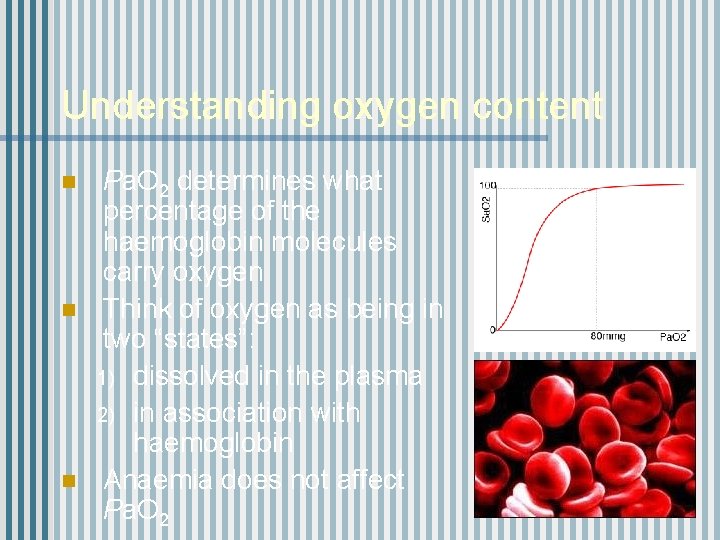
Understanding oxygen content n n n Pa. O 2 determines what percentage of the haemoglobin molecules carry oxygen Think of oxygen as being in two “states”: 1) dissolved in the plasma 2) in association with haemoglobin Anaemia does not affect Pa. O 2
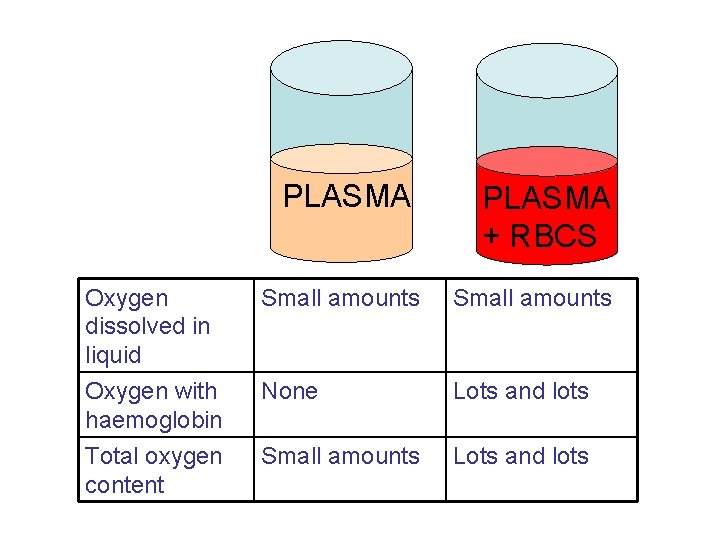
PLASMA + RBCS Oxygen dissolved in liquid Small amounts Oxygen with haemoglobin None Lots and lots Total oxygen content Small amounts Lots and lots
![How much oxygen is in the blood? Pa. O 2 mm. Hg [Hb] g/DL How much oxygen is in the blood? Pa. O 2 mm. Hg [Hb] g/DL](http://slidetodoc.com/presentation_image_h2/8de895f7aeeabcceeb2eba251f678d73/image-27.jpg)
How much oxygen is in the blood? Pa. O 2 mm. Hg [Hb] g/DL O 2 content ml/DL Patient A Patient B 50 100
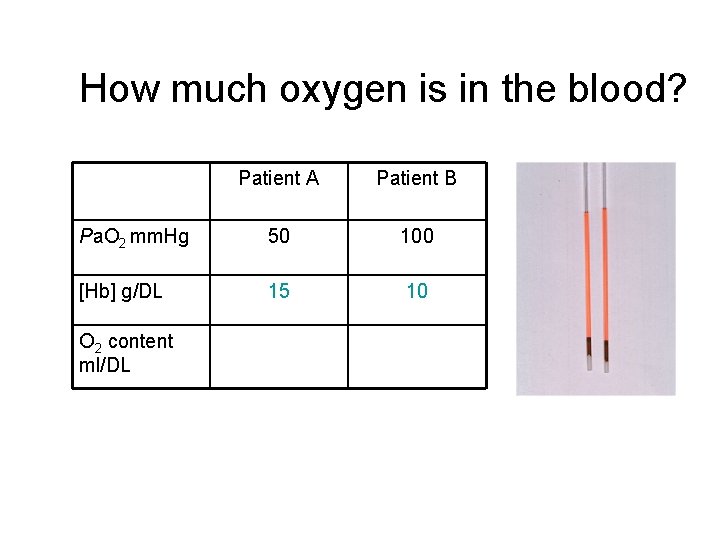
How much oxygen is in the blood? Patient A Patient B Pa. O 2 mm. Hg 50 100 [Hb] g/DL 15 10 O 2 content ml/DL
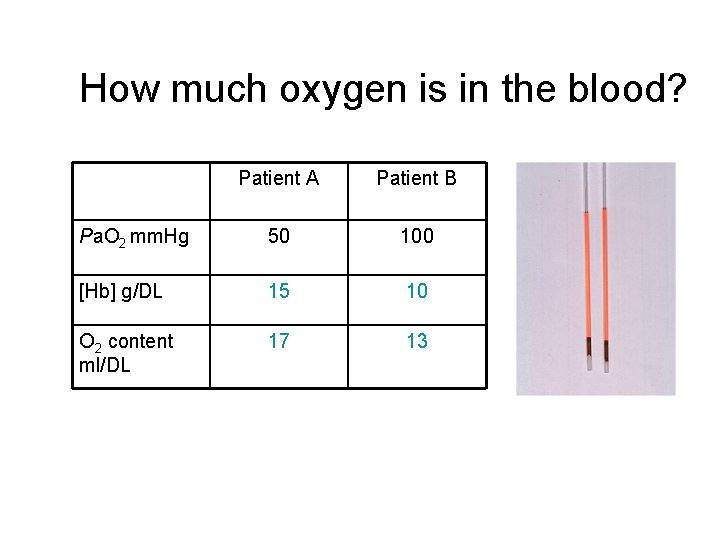
How much oxygen is in the blood? Patient A Patient B Pa. O 2 mm. Hg 50 100 [Hb] g/DL 15 10 O 2 content ml/DL 17 13

Adequate oxygenation If the Pa. O 2 is less than 70 mm. Hg (further) oxygen therapy is required n Alternative methods of assessment are of limited use n

Pulse oximetry Non-invasive, easy to attach n Movement artifacts n Few vets attempt to use this on conscious patients n

Mucous membranes n Pink is desirable! n A pale colour could be due to: n n drug induced vasoconstriction n poor peripheral perfusion Cyanosis: takes 5 g/d. L of unoxygenated haemoglobin to generate the blue colour

Our second example n One-year-old Newfie n Very flat one day following surgery for a fractured femur
Using a pulse oximeter to estimate the % of haemoglobin molecules in association with oxygen Fi. O 2 21% (room air) Sp. O 2 Failed p. H 7. 43 Pa. O 2 92 mm. Hg Pa. CO 2 22 mm. Hg PCV 21% n One-year-old Newfie n Very flat one day following surgery for a fractured femur

Fi. O 2 21% (room air) Sp. O 2 Did not attempt p. H 7. 43 Pa. O 2 92 mm. Hg n PAO 2 calculated by Vet. STAT as 124 mm. HG n PAO 2 - Pa. O 2 = 32 mm. Hg n 10 to 20 mm. Hg considered normal Pa. CO 2 22 mm. Hg PCV 21%

Assessing alveolar ventilation n High Pa. CO 2 = hypoventilation Low Pa. CO 2 = hyperventilation Capnography can provide a non-invasive estimate of Pa. CO 2 n only intubated patients

Our third example n Two-year-old spaniel n Rescued from the river yesterday n Near-drowning episode n Give oxygen via a face-mask
Acidaemia if blood p. H <7. 3 n Fi. O 2 Face-mask (40%) p. H 7. 22 Pa. O 2 92 mm. Hg a rule-of-thumb, n As Rescued from thethe Pa. O 2 should be 4 to 5 river timesyesterday the percentage inspired oxygen n Near-drowning Pa. CO 2 38 mm. Hg HCO 3 - 15 mmol/L Metabolic acidosis Two-year-old spaniel episode n Give oxygen via a face-mask
- Slides: 39