MCQ Which of the following anti TB drug

MCQ Which of the following anti TB drug may cause convulsions ? (a) Rifampicin (b) Pyrazinamide (c) Ethambutol (d) Isoniazid

MCQ Which of the following anti TB drugs may cause arthralgia (a) Pyrazinamide, Rifampicin, Streptomycin (b) Pyrazinamide, Ethambutol, Isoniazid (c) Pyrazinamide, Isoniazid, Streptomycin (d) Pyrazinamide, streptomycin, Ethambutol

Prevention and Management of adverse anti TB drug reactions Prof. Zuber Ahmad

Ø Most patients on 1 st line drugs complete their treatment without any significant adverse drug effects. Ø A few patients do experience adverse effects. Some of the drug induced side effects can be prevented Ø Many 2 nd line drugs are associated with more side effects Ø It is therefore important that patients be clinically monitored so that adverse effects can be detected promptly and managed properly
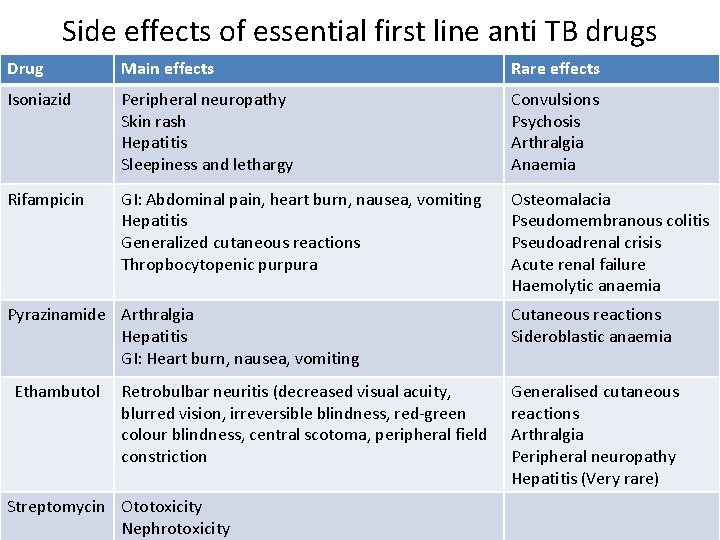
Side effects of essential first line anti TB drugs Drug Main effects Rare effects Isoniazid Peripheral neuropathy Skin rash Hepatitis Sleepiness and lethargy Convulsions Psychosis Arthralgia Anaemia Rifampicin GI: Abdominal pain, heart burn, nausea, vomiting Hepatitis Generalized cutaneous reactions Thropbocytopenic purpura Osteomalacia Pseudomembranous colitis Pseudoadrenal crisis Acute renal failure Haemolytic anaemia Pyrazinamide Arthralgia Hepatitis GI: Heart burn, nausea, vomiting Ethambutol Retrobulbar neuritis (decreased visual acuity, blurred vision, irreversible blindness, red-green colour blindness, central scotoma, peripheral field constriction Streptomycin Ototoxicity Nephrotoxicity Cutaneous reactions Sideroblastic anaemia Generalised cutaneous reactions Arthralgia Peripheral neuropathy Hepatitis (Very rare)

Symptom-Based Approach to manage side-effects of Anti-TB drugs
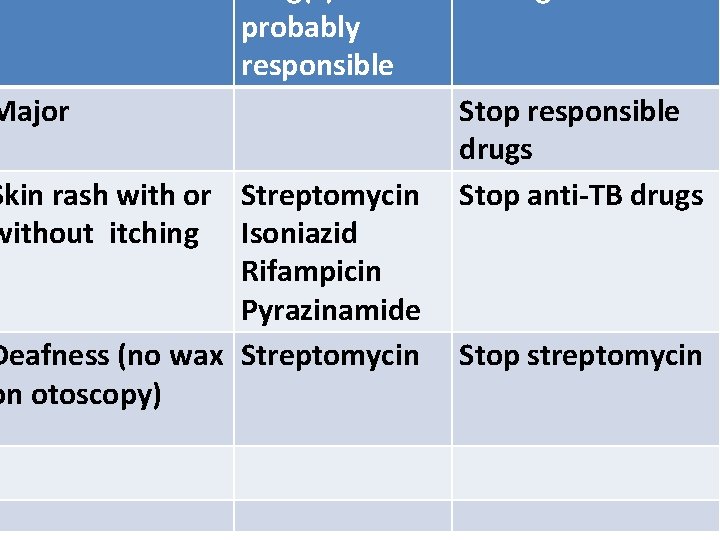
probably responsible Major Skin rash with or Streptomycin without itching Isoniazid Rifampicin Pyrazinamide Deafness (no wax Streptomycin on otoscopy) Stop responsible drugs Stop anti-TB drugs Stop streptomycin
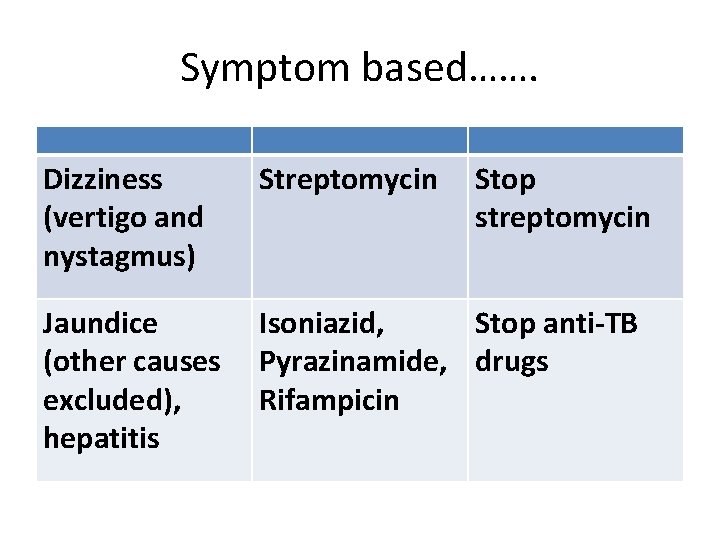
Symptom based……. Dizziness (vertigo and nystagmus) Streptomycin Stop streptomycin Jaundice (other causes excluded), hepatitis Isoniazid, Stop anti-TB Pyrazinamide, drugs Rifampicin
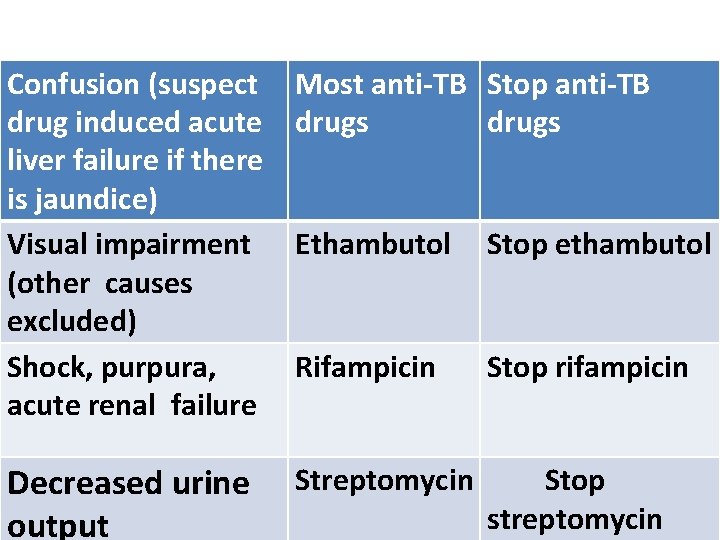
Confusion (suspect drug induced acute liver failure if there is jaundice) Visual impairment (other causes excluded) Shock, purpura, acute renal failure Most anti-TB Stop anti-TB drugs Decreased urine output Ethambutol Stop ethambutol Rifampicin Stop rifampicin Streptomycin Stop streptomycin
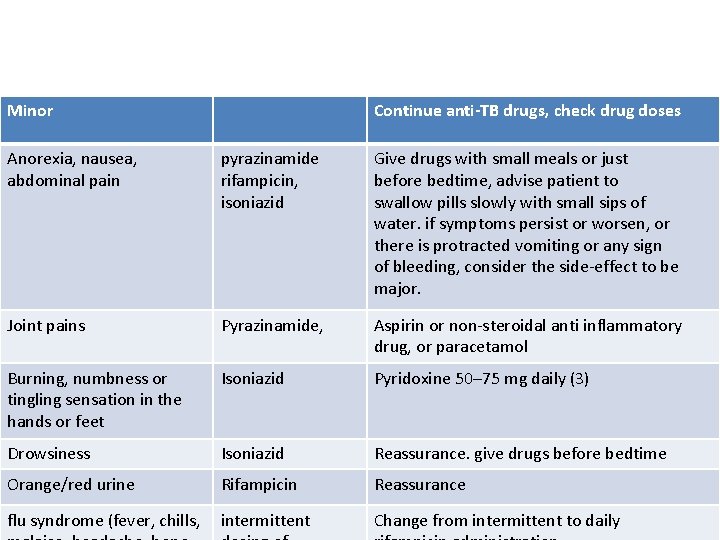
Minor Continue anti-TB drugs, check drug doses Anorexia, nausea, abdominal pain pyrazinamide rifampicin, isoniazid Give drugs with small meals or just before bedtime, advise patient to swallow pills slowly with small sips of water. if symptoms persist or worsen, or there is protracted vomiting or any sign of bleeding, consider the side-effect to be major. Joint pains Pyrazinamide, Aspirin or non-steroidal anti inflammatory drug, or paracetamol Burning, numbness or tingling sensation in the hands or feet Isoniazid Pyridoxine 50– 75 mg daily (3) Drowsiness Isoniazid Reassurance. give drugs before bedtime Orange/red urine Rifampicin Reassurance flu syndrome (fever, chills, intermittent Change from intermittent to daily

Management of cutaneous reactions • If a patient develops itching without a rash, the recommended approach is to try symptomatic treatment with antihistamines and skin moisturizing, and continue TB treatment while observing the patient closely. • If a skin rash develops, Stop all anti-TB drugs. • Once the reaction has resolved, anti-TB drugs are reintroduced one by one, starting with the drug least likely to be responsible for the reaction (rifampicin or isoniazid)

Cutaneous reaction……. . • Start with a small challenge dose, such as 50 mg isoniazid. The dose is gradually increased over 3 days. • This procedure is repeated, adding in one drug at a time. A reaction after adding in a particular drug identifies the offending drug. • Once drug is identified, do desensitization or use alternative regimens when a particular drug cannot be used.

Management of drug-induced hepatitis Isoniazid, pyrazinamide and rifampicin can all cause liver damage (drug-induced hepatitis). • Rifampicin cause asymptomatic jaundice without evidence of hepatitis. • It is important to try to rule out other possible causes before deciding that the hepatitis is induced by the TB regimen. • The management of hepatitis induced by TB treatment depends on: — whether the patient is in the intensive or continuation phase of TB treatment; — The severity of the liver disease; — The severity of the TB — The capacity of the health unit to manage the side-effects of TB treatment. •

Drug induced hepatitis…… • • • If it is thought that the liver disease is caused by the anti-TB drugs, Stop all drugs. If the patient is severely ill with TB and it is considered unsafe to stop TB treatment, a non-hepatotoxic regimen consisting of streptomycin, ethambutol and a fluoroquinolone should be started. If TB treatment has been stopped, it is necessary to wait for liver function tests to revert to normal and clinical symptoms (nausea, abdominal pain) to resolve before reintroducing the anti-TB drugs. If it is not possible to perform liver function tests, it is advisable to wait an extra 2 weeks after resolution of jaundice and upper abdominal tenderness before restarting TB treatment. If the signs and symptoms do not resolve and the liver disease is severe, the nonhepatotoxic regimen consisting of streptomycin, ethambutol and a fluoroquinolone should be started (or continued) for a total of 18– 24 months

• Once drug-induced hepatitis has resolved, the drugs are reintroduced one at a time. • If symptoms recur or liver function tests become abnormal as the drugs are reintroduced, the last drug added should be stopped. Some advise starting with rifampicin because it is less likely than isoniazid or pyrazinamide to cause hepatotoxicity and After 3– 7 days, isoniazid may be reintroduced. • In patients who have experienced jaundice but tolerate the reintroduction of rifampicin and isoniazid, it is advisable to avoid pyrazinamide.

Alternative regimens • Alternative regimens depend on which drug is implicated as the cause of the hepatitis. • If rifampicin is implicated, a suggested regimen is: 2 SHE+ 10 HE • If isoniazid cannot be used: 6– 9 RZE • If pyrazinamide is discontinued before the patient has completed the intensive phase, the total duration of isoniazid and rifampicin therapy may be extended to 9 months

• If neither isoniazid nor rifampicin can be used: 18 -24 SEQ • Reintroducing one drug at a time is the optimal approach, especially if the patient’s hepatitis is severe. Try following approach, which depends on whether the hepatitis with jaundice occurred during the intensive or the continuation phase.

• • When hepatitis with jaundice occurs during the intensive phase of TB treatment with isoniazid, rifampicin, pyrazinamide and ethambutol: once hepatitis has resolved, restart the same drugs EXCEPT replace pyrazinamide with streptomycin, 2 RHEZ (RHES) + 6 RH • • When hepatitis with jaundice occurs during the continuation phase: once hepatitis has resolved, restart isoniazid and rifampicin to complete the 4 -month continuation phase of therapy.

THANK YOU
- Slides: 19