Mayo Clinic Discharge Planning for Improved Orthopedic Outcomes
















































- Slides: 69

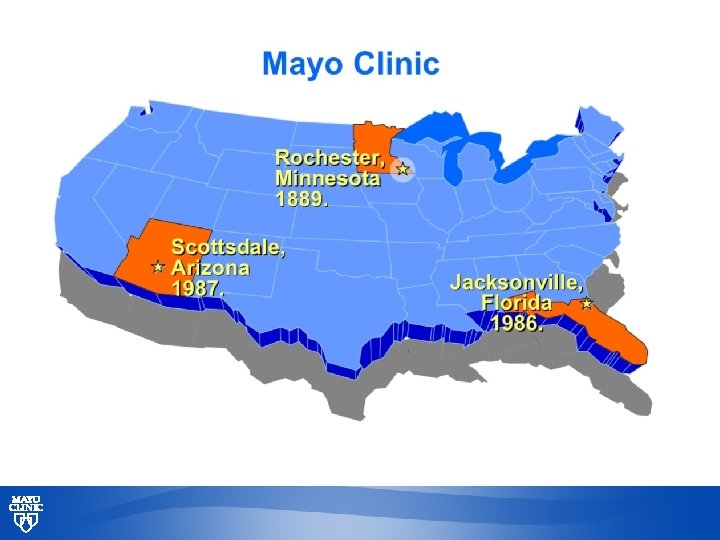
Mayo Clinic Discharge Planning for Improved Orthopedic Outcomes Lisa C. Carter M. A. , R. N. Nurse Administrator © 2014 © 2013 MFMER | 3335126 -1 | slide-1

Objectives • Describe how Mayo Clinic improves outcomes for orthopedic patients through coordination of care transitions • Identify how work culture impacts the success of care transitions for orthopedic patients • Explain the importance of including family caregivers in planning and executing successful care transitions © 2013 MFMER | slide-2

© 2013 MFMER | slide-3

© 2013 MFMER | slide-4

Number of Patients Seen • In 2017, Mayo Clinic provided direct care to • More than 1. 3 million people • From all 50 states • From 137 countries © 2013 MFMER | slide-5

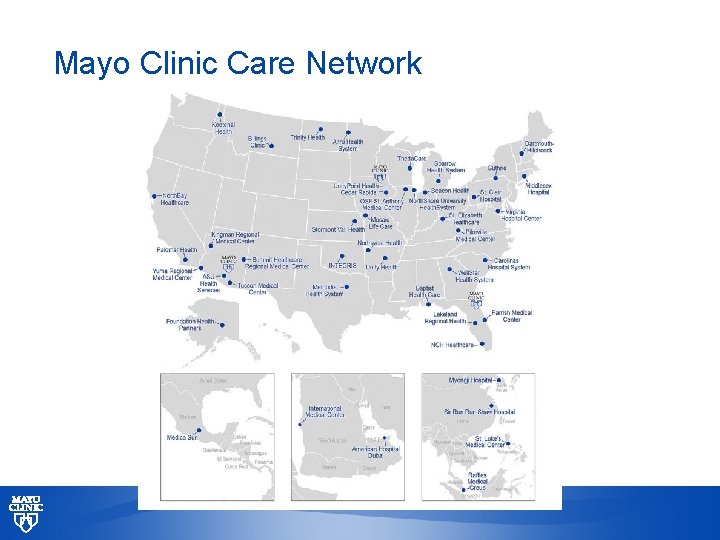
Mayo Clinic Care Network © 2013 MFMER | slide-6

Respect Integrity Compassion Healing The Needs of the Patient Come First Teamwork Innovation Excellence Stewardship © 2013 MFMER | slide-7 © 2015 MFMER | 3442127 -7

Mayo Clinic Primary Value, Mission, Vision • Primary Value • The needs of the patient come first. • Mission • To inspire hope and contribute to health and wellbeing by providing the best care to every patient through integrated clinical practice, education and research. • Vision • Mayo Clinic will provide an unparalleled experience as the most trusted partner for health care. © 2013 MFMER | slide-8

Three Shields of Mayo Clinic • Practice • Education • Research © 2013 MFMER | slide-9

Mayo Nursing Care Model Foundation • Theoretical Frameworks • Caring • Watson’s Model of Human Care • Relationship Based Care • Koloroutis • Evidence-Based Practice • Mayo Nursing Model of Evidence-Based Practice • Patient - Nurse Relationship Based Care is the center of model © 2013 MFMER | slide-10

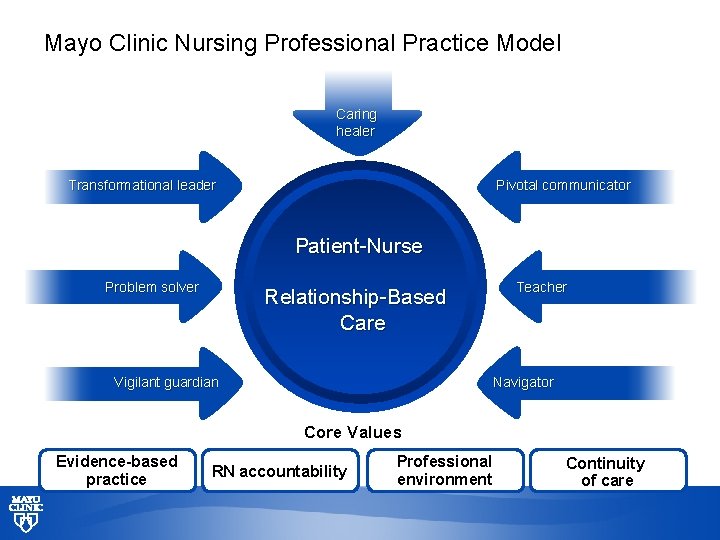
Mayo Clinic Nursing Professional Practice Model Caring healer Transformational leader Pivotal communicator Patient-Nurse Problem solver Relationship-Based Care Vigilant guardian Teacher Navigator Core Values Evidence-based practice RN accountability Professional environment Continuity of care © 2013 MFMER | slide-11

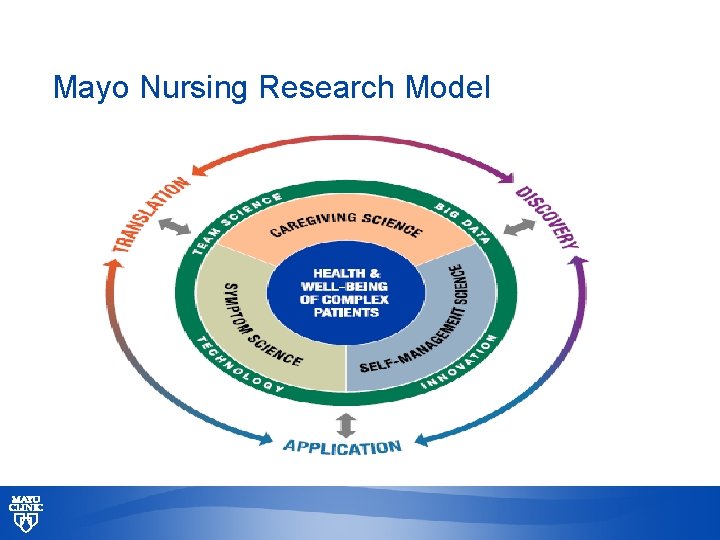
Mayo Nursing Research Model © 2013 MFMER | slide-12

Recognized for Excellence © 2013 MFMER | slide-13

A Destination of Hope and Healing © 2013 MFMER | slide-14

Healing • Inspire hope and nurture the well-being of the whole person, respecting physical, emotional and spiritual needs • WHO definition of health: Health is a state of complete physical, mental, and social well being, and not merely the absence of disease or injury © 2013 MFMER | slide-15

Care Transitions: Critical connections on the pathway to successful outcomes © 2013 MFMER | slide-16

Evidence-Based Discharge Planning Definition: Preparation for moving a patient from one level of care to another within or outside the current health care agency (Dochterman& Bulechek, 2004) © 2013 MFMER | slide-17

Effective Discharge Interventions – Level of Evidence I • Assist the patient/family/so in planning for the supportive environment necessary to provide the patient’s post hospital care • Arrange for caregiver support, as appropriate • Coordinate referrals relevant to linkages among health care providers • Communicate the patient’s discharge plans, as appropriate © 2013 MFMER | slide-18

© 2013 MFMER | slide-19

Strategies to enhance outcomes © 2013 MFMER | slide-20

Strategies – Orthopedics Enhanced Pre. Hospital Education Expected Date of Discharge on Patient’s Whiteboard Improved Outpatient Phone Triage Access/Process Pre-Operative Discharge Assessment Daily Multidisciplinary Discharge Rounds Patient Support Group Pharmacy – Medication Reconciliation Multidisciplinary Discharge Summary Follow-up Appointment within 7 days © 2013 MFMER | slide-21

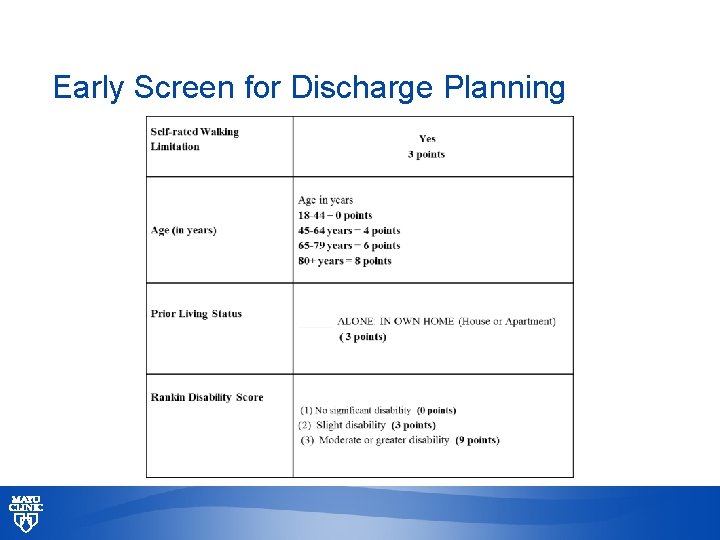
Coordination of Care Transitions for Elective Orthopedic Procedures • Begins when decision made for surgical intervention • Educate on requirements for successful experience/recovery • Pre-op classes scheduled early/include caregivers • Assess for needs related to transition from hospital (POE calls) • Caregiver availability • Transportation • Prescription drug insurance/pharmacy identification • Home compatibility (steps, bedroom/bath location, width of bed/bath doors, adaptive equipment) • Early Screen for Discharge Planning (ESDP) • Explain goals of care and consequences to discharge disposition if met/not met during hospital © 2013 MFMER | slide-22

During hospital stay • ESDP – early intervention • Standardized Discharge Planning Assessments • Care Coordination • Daily multidisciplinary discharge planning rounds (RN, Care Manager, Social Worker, mid-level provider, PT, pharmacist) • Identified Caregiver involved in therapy sessions • Standardized Multidisciplinary Discharge Summary • Delayed discharge reviews © 2013 MFMER | slide-23

Orthopedic Specific Discharge Summary • Admitting Diagnosis- Final Diagnosis • Admission and Discharge Date • Contact information (primary care provider, hospital providers) • Detailed patient history – medical, daily living, home environment • Course in hospital • Falls • Bone health • Consult services and recommendations • Summary of key results • Medications • Post discharge health management plan © 2013 MFMER | slide-24

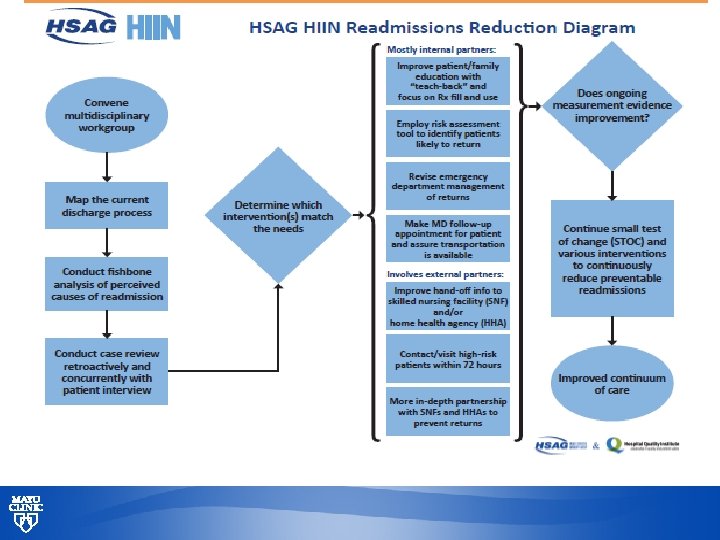
Inpatient Activities to target readmissions § ESDP and LACE Plus screen by Nursing – on admission creates a score to trigger a case management consult § Readmission screening questions – required field on all readmissions within 30 days to identify causes § Readmissions flag in the ED to notify them of a readmission § Geographical location of patients coupled with target multidisciplinary rounding § Partnership with community care provider care teams © 2013 MFMER | slide-25

Interventions to Reduce Readmissions • Systematic review of interventions to reduce 30 -day readmissions Hansen LO, Young RS, Hinami K, et al. 2011. Interventions to reduce 30 -day rehospitalization: a systematic review. Ann. Intern. Med. 155: 520– 28 © 2013 MFMER | slide-27

Care Transition Team § Begins on admission § Care Navigators § Multidisciplinary Process – CM, SW, CNS, MD, APP § Multimodal – F 2 F, Telephonic, Telehealth, Telemedicine, Adjunct service support § Consistent Communication § Ease of access to outpatient clinicians © 2013 MFMER | slide-28

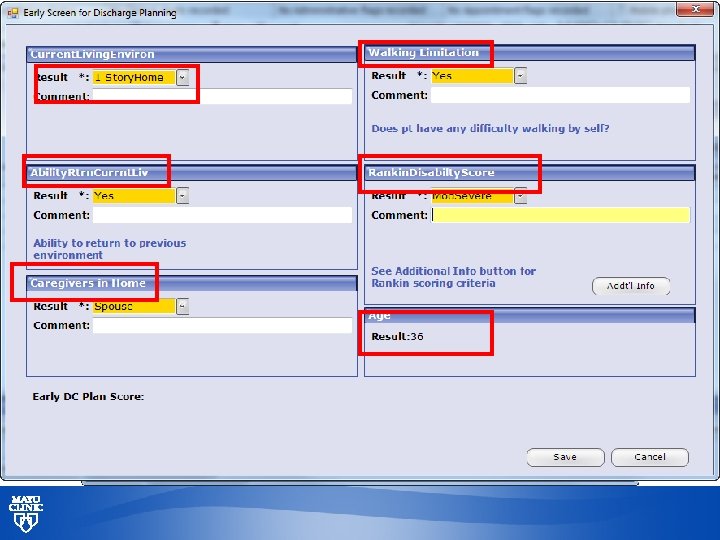
Early Screen for Discharge Planning © 2013 MFMER | slide-29

© 2013 MFMER | slide-30

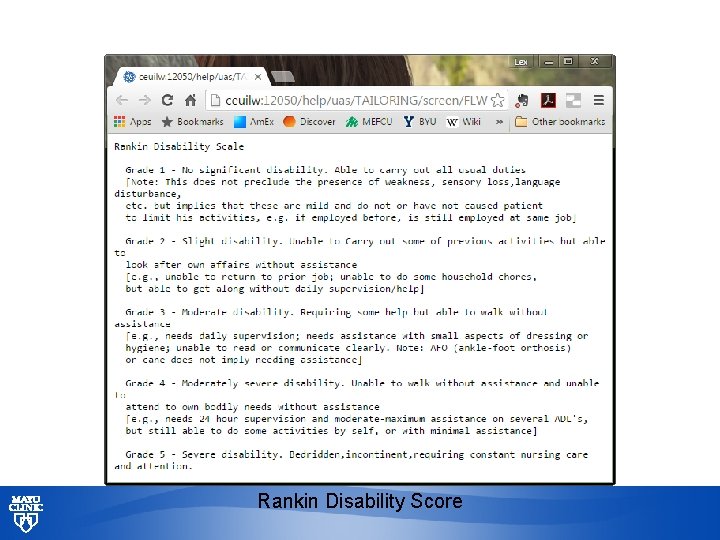
Rankin Disability Score © 2013 MFMER | slide-31

© 2013 MFMER | slide-32

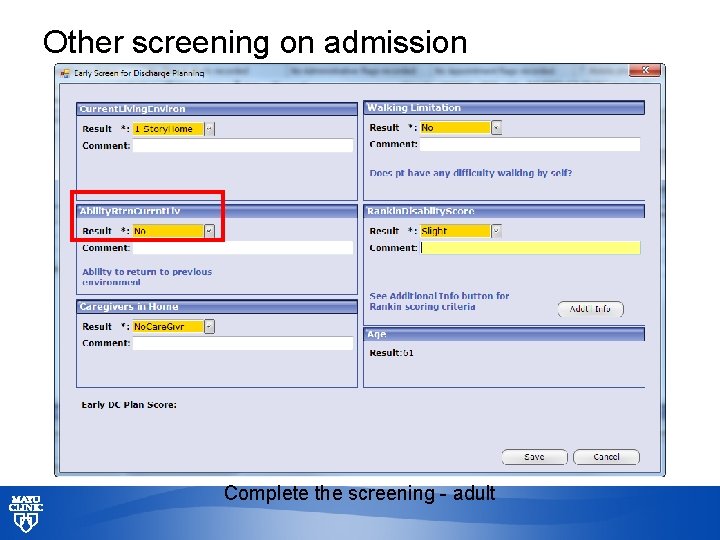
Other screening on admission Complete the screening - adult © 2013 MFMER | slide-33

Blaze pop up on ‘unable to return to current living environment’ screen © 2013 MFMER | slide-34

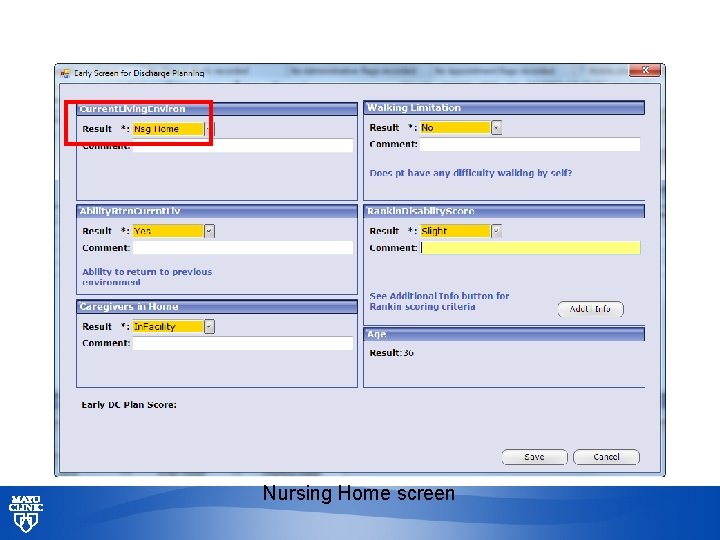
Nursing Home screen © 2013 MFMER | slide-35

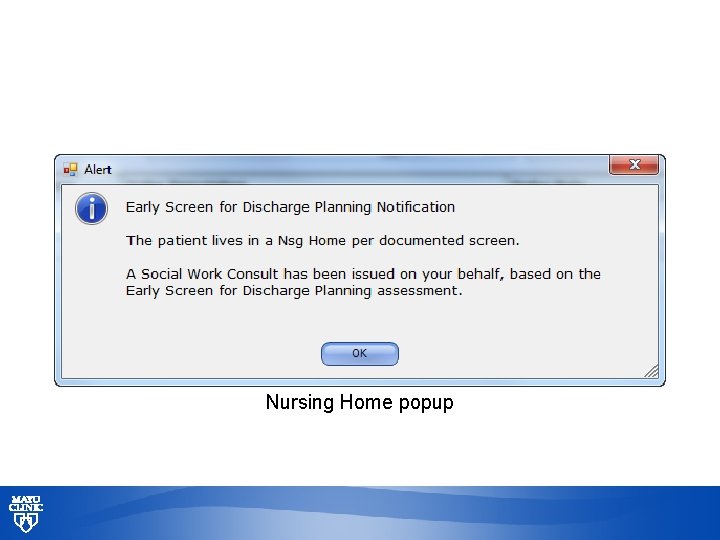
Nursing Home popup © 2013 MFMER | slide-36

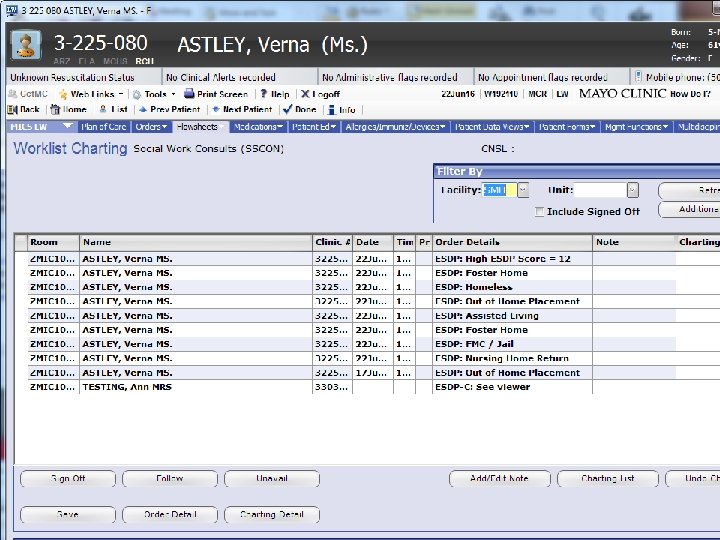
© 2013 MFMER | slide-37

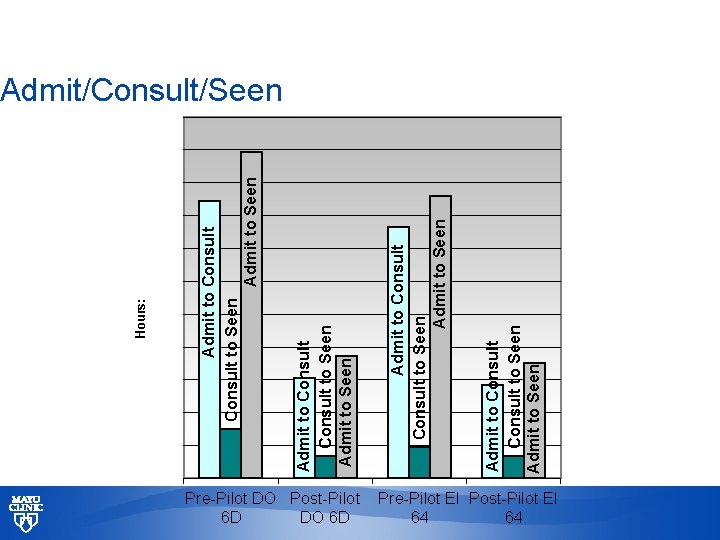
Pre-Pilot DO Post-Pilot 6 D DO 6 D Admit to Consult Consult to Seen Admit to Seen Hours: Admit/Consult/Seen Pre-Pilot EI Post-Pilot EI 64 64 © 2013 MFMER | slide-38

Staff RN Focus Groups 4 themes emerged from interviews 1. Moving from a reactive to a proactive approach 2. Anticipatory readiness 3. Heightened awareness of need to learn more about discharge planning 4. Deeper understanding of meaningfulness of their contribution to planning process © 2013 MFMER | slide-39

We’re in this together! § Building a partnership with Post Acute Care providers and the healthcare community is key! § Utilize system resources (MPAC) § Creating a narrowed network § Creating trust and accountability § Supporting the transition/education process § Transparent Open Communication § PAC collaboration i. e. Mayo Clinic Quarterly Meetings and Community © 2013 MFMER | slide-40

Improved Outcomes • Decreased LOS • Improved patient satisfaction • Improved teamwork/team satisfaction • Decrease Preventable Readmissions © 2013 MFMER | slide-41

Monitor for Failures! § Symptoms of system/process failures will manifest § Problem solving tools will help identify the steps necessary to correct the failure § Plan-Do-Check/Study-Act (PDSA/PDCA) § People are not the problem! § Learn from those that do the work § Listen to the voice of the patient 36 © 2013 MFMER | slide-42

Readmission is…often a Process Failure Inadequacies in discharge preparation are associated with ED visits and readmissions within 30 days of discharge. • Patients readmitted within 8 days of discharge – more likely to experience complications from the original condition treated during their hospital stay • Patients readmitted between 8 and up to 30 days of discharge – more likely to experience improper follow-up care or develop other illnesses or complications References listed at the end of the presentation. 37 © 2013 MFMER | slide-43

© 2013 MFMER | slide-44

Impact of Work Culture • Culture of Caring • The importance of self-care and care for colleagues to relationship-based care • Nurturing healthy, meaningful relationships with yourself and with those around you • Resiliency Training – Dr. Amit Sood • Empathic communication © 2013 MFMER | slide-45

Commitment to Safety • Every Mayo staff member is expected to embed the 5 safe behaviors into daily work • Pay Attention to Detail • Communicate Clearly • Have a Questioning and Receptive Attitude • Handoff Effectively • Support Each Other • Behavioral choices are managed with the principles of a fair and just culture © 2013 MFMER | slide-46

Value Collaboration: Foster Teamwork In a teamwork environment, people understand believe that thinking, planning, decisions and actions are better when done cooperatively. People recognize, and even assimilate, the belief that "none of us is as good as all of us. " © 2013 MFMER | slide-47

Team Building • Set clear goals and expectations • Work together instead of against • Have a attitude of cooperation rather than competition • Give recognition for a job well done • Show appreciation and make it personal • Value and respect each other’s opinions • Share ideas and thoughts • Positive attitude • Smile © 2013 MFMER | slide-48

Impact of Family Caregiving Why pay attention to them? • provide an estimated $470 billion in caregiving services annually • frequently requires a commitment equivalent to full-time employment • Costs from a societal perspective include time and money • Lost productivity at work • Lost opportunity for social activities © 2013 MFMER | slide-49

Additionally, Factor in • Assisting in transfers (chair to standing, bed to standing) • Driving • Shopping • Housework • Meal prep • Shlepping luggage, packages © 2013 MFMER | slide-50

Family Caregivers • Successful implementation of the patient’s postacute plans of care by assisting in symptom control • managing medications, • coordinating follow-up visits, and • anticipating and sequencing care • May have substantial personal health needs equal to or greater than the patients’ needs • Absence of transitional care models that address the needs of FCGs who transition care from the hospital to home © 2013 MFMER | slide-51

Caregiver Advise, Record, Enable (CARE) Act The CARE Act requires hospitals to: • Record the name of the family caregiver on the medical record of your loved one. • Inform the family caregivers when their loved one is to be discharged. • Provide the family caregiver with education and instruction of the medical tasks he or she will need to perform for the patient at home. © 2013 MFMER | slide-52

Caregiver Assessment • Health Literacy • Social Determinants of Health • Financial burden • Social isolation and supports • Housing (stable, safe) • Food insecurity • Caregiver load (other dependents, children) • Transportation © 2013 MFMER | slide-53

Follow-up • Talk about their priorities, goals, and strengths to clarify whethere are useful ways for your health system to provide support services. • “Are any of your needs urgent? ” • Referrals as appropriate © 2013 MFMER | slide-54

Use of Data to Monitor for Failures! § Symptoms of system/process failures will manifest § Problem solving tools will help identify the steps necessary to correct the failure § Plan-Do-Check/Study-Act (PDSA/PDCA) § People are not the problem! § Learn from those that do the work § Listen to the voice of the patient 36 © 2013 MFMER | slide-55

© 2013 MFMER | slide-57

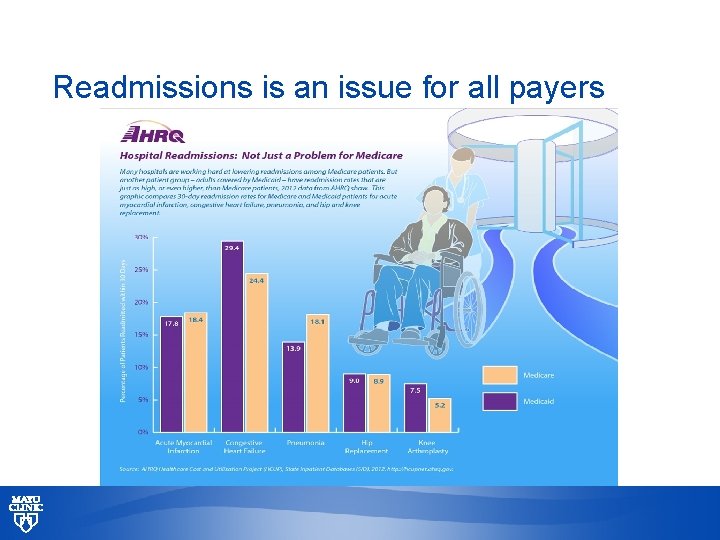
Readmissions is an issue for all payers © 2013 MFMER | slide-58

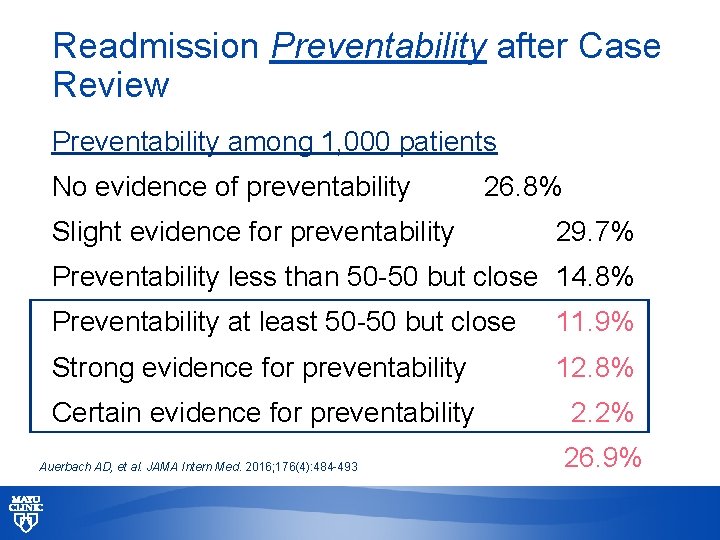
• 1000 readmissions • 12 sites • Classification of preventability • Patient and provider surveys • Deep dive into medical records JAMA Intern Med. 2016; 176(4): 484 -493 © 2013 MFMER | slide-59

Readmission Preventability after Case Review Preventability among 1, 000 patients No evidence of preventability 26. 8% Slight evidence for preventability 29. 7% Preventability less than 50 -50 but close 14. 8% Preventability at least 50 -50 but close 11. 9% Strong evidence for preventability 12. 8% Certain evidence for preventability 2. 2% Auerbach AD, et al. JAMA Intern Med. 2016; 176(4): 484 -493 26. 9% © 2013 MFMER | slide-60

New Metric – Excessive Days in Acute Care § 30 day post discharge access to acute care § Calculated in comparison to other facilities § ED visit – 0. 5 Days § Observation Stay – measured in hours, round to the next half day § Readmissions – Day for Day count © 2013 MFMER | slide-61

Are we really that different? § Hospital Compare demonstrates similar numbers across the board § Multiple strategies are executed simultaneously – difficult to monitor specific impact § We don’t have time to wait! Have to keep the elephant in the rear view mirror. © 2013 MFMER | slide-62

The Benefits of Collaboration § Palomar and Mayo Clinic relationship § Ask Mayo Expert (AME) § e. Consults § Co-Branded Patient Education Materials © 2013 MFMER | slide-63

Ask Mayo Expert © 2013 MFMER | slide-64

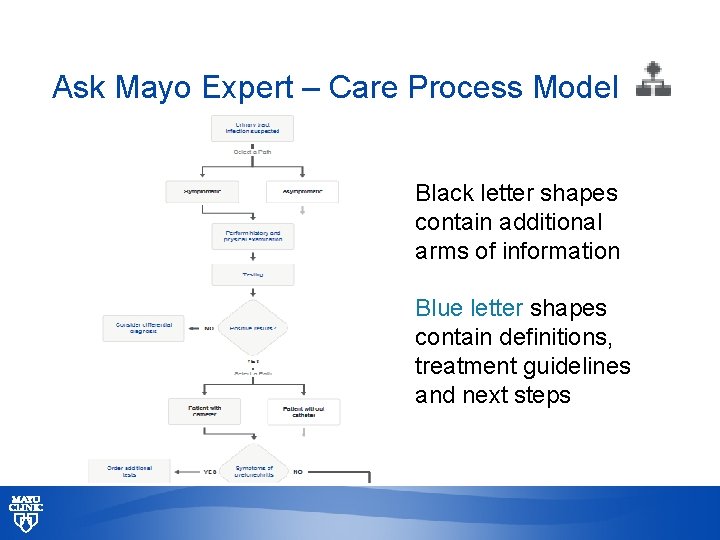
Ask Mayo Expert – Care Process Model Black letter shapes contain additional arms of information Blue letter shapes contain definitions, treatment guidelines and next steps © 2013 MFMER | slide-65

Co-Branded Patient Education Materials • Mayo Clinic Care Network members have access to approximately 2, 500 patient education documents and videos developed by Mayo Clinic multidisciplinary teams who are in daily practice of delivering patient care. © 2013 MFMER | slide-66

References – Impact of Family Caregiving Coleman EA, Roman SP. Family caregivers' experiences during transitions out of hospital. J Healthc Qual. Jan-Feb 2015; 37(1): 12 -21. Coleman EA, Roman SP, Hall KA, Min SJ. Enhancing the care transitions intervention protocol to better address the needs of family caregivers. J Healthc Qual. Jan-Feb 2015; 37(1): 2 -11. Coleman E, Min S, Chomiak A, Kramer A. Posthospital care transitions: patterns, complications, and risk identification. Health Services Research. Oct 2004; 39(5): 1449 -1465. Grady PA, Gullatte M. The 2014 National Nursing Research Roundtable: The science of caregiving. Nurs Outlook. Sep-Oct 2014; 62(5): 362 -365. Hudson P. Improving support for family carers: key implications for research, policy and practice. Palliat Med. Jul 2013; 27(7): 581 -582. Levine C, Halper D, Rutberg J, Gould DA. Engaging Family Caregivers as Partners in Transitions: TC-Qu. IC: A Quality Improvement Collaborative. 2013; http: //www. uhfnyc. org/publications/880905. Accessed September 11, 2015. 43 © 2013 MFMER | slide-67

References – Care Transitions Kansagara D, Chiovaro, J, Kagen, D, Jencks, S, Rhyne, K, O’Neil, M, Kondo, K, Relevo, R, Motu’apuaka, M, Freeman, M, Englander, H. So Many Options, Where Do We Start? An Overview of the Care Transitions Literature. Journal of Hospital Medicine. 2016. 11(3): 221 -230. Krumholz, H. Post-Hospital Syndrome — An Acquired, Transient Condition of Generalized Risk. NEJM. 2 b 013; 368(2): 100 -102. Naylor MD, Marcille J. Managing the transition from the hospital. Managed care (Langhorne, Pa. ). Jun 2014; 23(6): 27 -30. Naylor MD, Aiken LH, Kurtzman ET, Olds DM, Hirschman KB. The Importance Of Transitional Care In Achieving Health Reform. Health Affairs. 2012; 31(3): 746 -754. Naylor MD, Keating SA. Transitional care: Moving patients from one care setting to another. American Journal of Nursing. 2009; 108(9 S): 58 -63. Maloney LR, Weiss ME. Patients' perceptions of hospital discharge informational content. Clin Nurs Res. Aug 2008; 17(3): 200 -219. . © 2013 MFMER | slide-68

References - ESDP Holland DE, Harris MR, Leibson CL, Pankratz VS, Krichbaum KE. Development and validation of a screen for specialized discharge planning services. Nursing research. Jan-Feb 2006; 55(1): 62 -71. Rhudy L, Holland DE, Bowles KH. Illuminating Hospital Discharge Planning: Staff Nurse Decision Making. Applied Nursing Research 2010; 23(4): 198 -206. Holland DE, Hemann MA. Standardizing Discharge Planning at the Mayo Clinic. The Joint Commission Journal on Quality and Patient Safety. January 2011; 37(1): 29 -36. Holland DE, Knafl GJ, Bowles KH. Targeting hospitalised patients for early discharge planning intervention. Journal of Clinical Nursing. 2012, 22: 2696 -2703. doi: 10. 1111/j. 13652702. 2012. 04221. x. Bowles, KH, Hanlon, A, Holland, DE, Potashnik, SL & Topaz, M. Impact of discharge planning decision support on time to readmission among older adult medical patients. Prof Case Manag. 2014, 19(1): 29 -38. Salentiny-Wrobleski, DM, Joswiak ME, Dunn, DF, Maxson, PM Holland, DE. Discharge Planning Rounds to the Bedside: A Patient and Family Centered Approach. MEDSURG Nursing. 2014, 23(2): 111 -116. Holland DE, Brandt C, Targonski PV, Bowles KH. Validating Performance of a Hospital Discharge Planning Decision Tool in Community Hospitals. Prof Case Manag. 2017 Sep/Oct; 22 (5): 204 -213 PMID: 28777233 DOI: 10. 1097/NCM. 0000000233 © 2013 MFMER | slide-69

References – Culture of Caring & Resiliency Carter LC, Nelson JL, Sievers BA, Dukek S, Pipe TB, Holland DE. Exploring a culture of caring. Nursing Administration Quarterly 2008; 32 (1): 57 -63. Magtibay D, Chesak S, Coughlin K, Sood, A. Decreasing stress and burnout in nurses: Efficacy of blended learning program. The Journal of Nursing Administration 2017; 47: 391 -395. Sood A. The Mayo Clinic handbook for happiness: A four-step plan for resilient living; 2015; Da Capo Lifeling Books. © 2013 MFMER | slide-70

Thank You © 2013 MFMER | slide-71