Mathematics for Computed Tomography Scanning Patient XRay beam

Mathematics for Computed Tomography
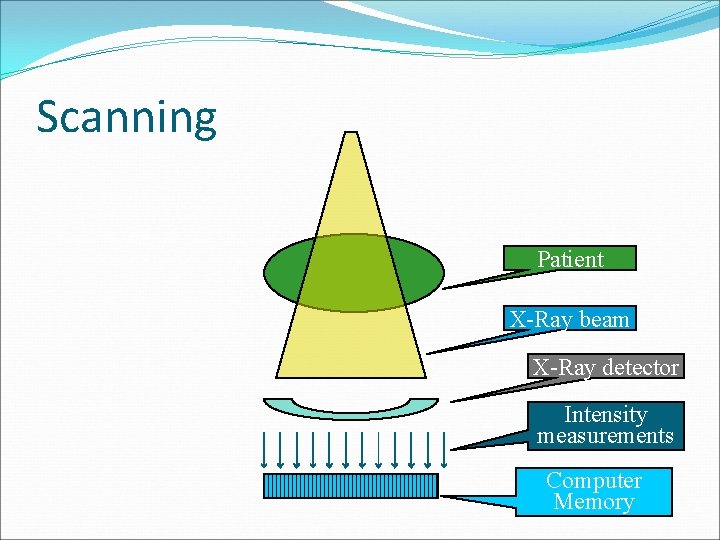
Scanning Patient X-Ray beam X-Ray detector Intensity measurements Computer Memory
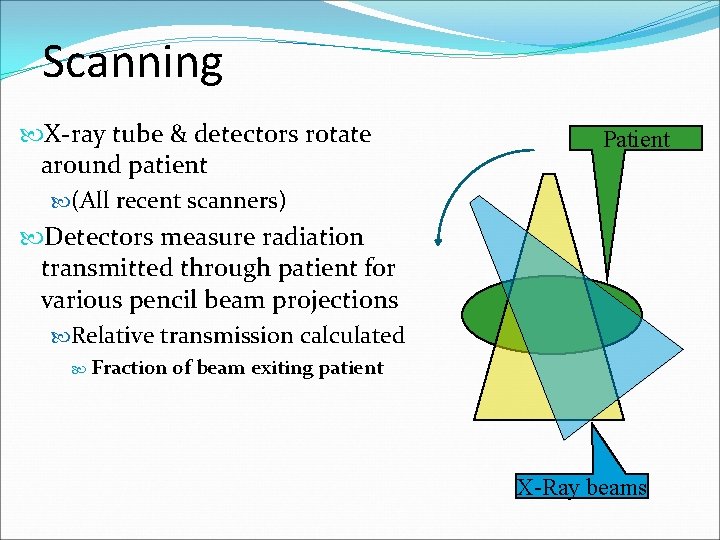
Scanning X-ray tube & detectors rotate around patient (All recent scanners) Detectors measure radiation transmitted through patient for various pencil beam projections Relative transmission calculated Fraction Patient of beam exiting patient X-Ray beams

CT Detectors electronic / quantitative extremely sensitive small radiation input differences measureable output digitized & sent to computer

Photon Phate What can happen to an x-ray photon passing through a material (tissue)? Incoming X-ray Photon Material ? ? ?

Photon Phate #1: Nothing �Photon exits unaffected � same energy � same direction �Good � These photons form the CT image Incoming X-ray Photon Material Outgoing X-ray Photon

Photon Phate #2: Absorption Photon disappears Its energy is absorbed by material Good Creates differential absorption which forms CT image Bad Source of patient dose Incoming X-ray Photon Material

Photon Phate #3: Scatter �Lower energy photon emerges �energy difference deposited in material �Photon usually emerges in different direction �Bad � Degrades image Incoming X-ray Photon Material Outgoing X-ray Photon

Photon Beam Attenuation Anything which removes original photon from beam absorption scatter Material Incoming X-ray Photon Material Outgoing X-ray Photon
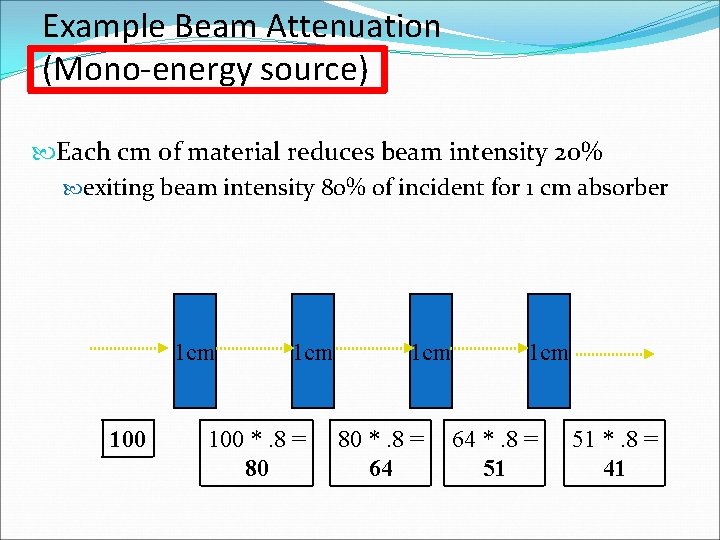
Example Beam Attenuation (Mono-energy source) Each cm of material reduces beam intensity 20% exiting beam intensity 80% of incident for 1 cm absorber 1 cm 100 *. 8 = 80 1 cm 80 *. 8 = 64 1 cm 64 *. 8 = 51 51 *. 8 = 41

Attenuation Equation for Mono-energetic Photon Beams I= -mx Ioe I = Exiting beam intensity Io = Incident beam intensity e = constant (2. 718…) m = linear attenuation coefficient • property of • absorber material • beam energy x = absorber thickness For photons which are neither absorbed nor scattered Io Material x I

More Realistic CT Example Beam Attenuation for non-uniform Material 4 different materials 4 different attenuation coefficients x Io #1 #2 #3 #4 ? ? I m 1 m 2 m 3 m 4 I= -(m +m +m +m )x 1 2 3 4 Ioe

Effect of Beam Energy on Monoenergetic Beam Attenuation Low energy photons more easily absorbed High energy photons more penetrating All materials attenuate a larger fraction of low than high energy photons 100 Material Higher-energy mono-energetic beam 80 100 Material Lower-energy mono-energetic beam <80
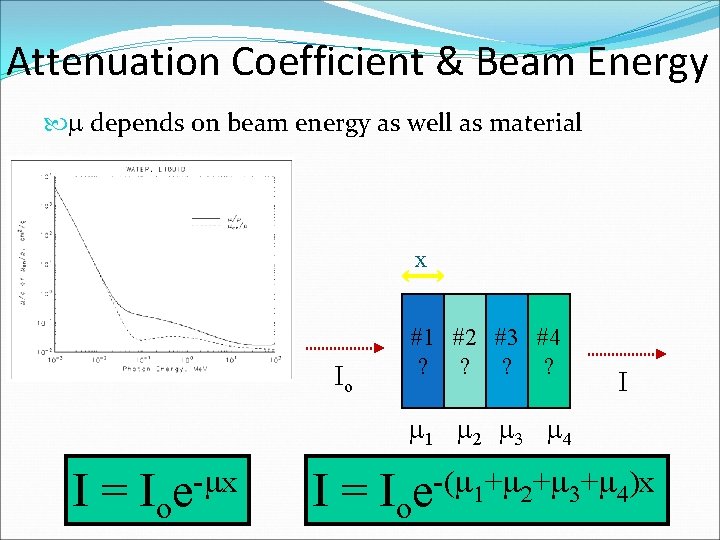
Attenuation Coefficient & Beam Energy m depends on beam energy as well as material x Io #1 #2 #3 #4 ? ? I m 1 m 2 m 3 m 4 I= -mx Ioe I= -(m +m +m +m )x 1 2 3 4 Ioe

Mono-energetic X-ray Beams Available from radionuclide sources Not used in CT Radionuclide intensity much lower than that of x-ray tube
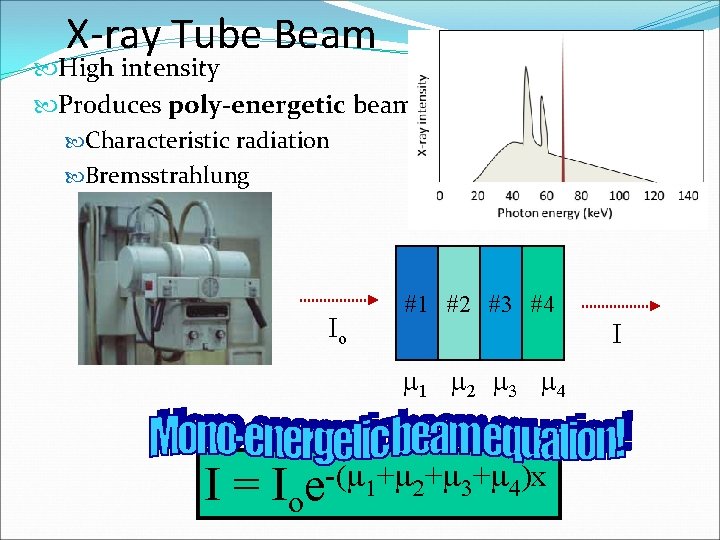
X-ray Tube Beam High intensity Produces poly-energetic beam Characteristic radiation Bremsstrahlung Io x #1 #2 #3 #4 I m 1 m 2 m 3 m 4 I = Ioe-(m 1+m 2+m 3+m 4)x
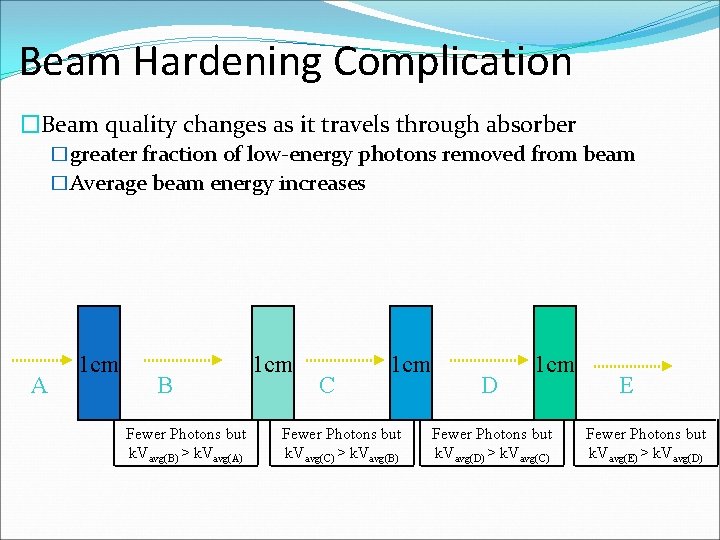
Beam Hardening Complication �Beam quality changes as it travels through absorber �greater fraction of low-energy photons removed from beam �Average beam energy increases A 1 cm B Fewer Photons but k. Vavg(B) > k. Vavg(A) 1 cm C 1 cm Fewer Photons but k. Vavg(C) > k. Vavg(B) D 1 cm Fewer Photons but k. Vavg(D) > k. Vavg(C) E Fewer Photons but k. Vavg(E) > k. Vavg(D)

Beam Hardening Complication Attenuation coefficients mn depend on beam energy!!! Beam spectrum incident on each block unknown Four m’s, each for a different & unknown energy 1 cm 1 cm m 1 m 2 m 3 m 4 I = Ioe-(m 1+m 2+m 3+m 4)x

Reconstruction Scanner measures “I” for thousands of pencil beam projections Computer calculates tens of thousands of attenuation coefficients one for each pixel Computer must correct for beam hardening effect of increase in average beam energy from one side of projection to other I = Ioe-(m 1+m 2+m 3+m 4 +. . . )x

Why is CT done with High k. V’s? Less dependence of attenuation coefficient on photon energy Attenuation coefficient changes less at higher k. V’s High k. V provides high radiation flux at detector
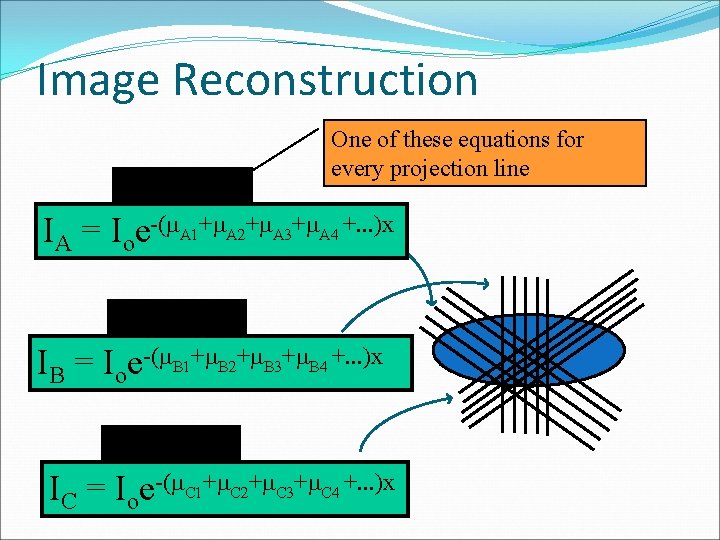
Image Reconstruction Projection #A One of these equations for every projection line IA = Ioe-(m. A 1+m. A 2+m. A 3+m. A 4 +. . . )x Projection #B IB = Ioe-(m. B 1+m. B 2+m. B 3+m. B 4 +. . . )x Projection #C IC = Ioe-(m. C 1+m. C 2+m. C 3+m. C 4 +. . . )x

* Image Reconstruction Projection #A What We Measure: IA, IB, IC, . . . IA = Ioe-(m. A 1+m. A 2+m. A 3+m. A 4 +. . . )x Projection #B IB = Ioe-(m. B 1+m. B 2+m. B 3+m. B 4 +. . . )x Projection #C IC = Ioe-(m. C 1+m. C 2+m. C 3+m. C 4 +. . . )x Reconstruction Calculates: m. A 1, m. A 2, m. A 3, . . . m. B 1, m. B 2, m. B 3, . . . m. C 1, m. C 2, m. C 3, . . . Etc.

CT (Hounsfield) Number Calculated from reconstructed pixel attenuation coefficient (mt - m. W) CT # = 1000 X ------m. W Where: ut = linear attenuation coefficient for tissue in pixel u. W = linear attenuation coefficient for water

CT Numbers for Special Stuff Bone: +1000 Water: 0 Air: -1000 (mt - m. W) CT # = 1000 X ------m. W
- Slides: 24