Maternal Sepsis Mark Ballard MD Obstetrics and Gynecology

Maternal Sepsis Mark Ballard, MD Obstetrics and Gynecology FACOG

Objectives �Recognize the patient with early sepsis �Acknowledging unique situations with the antepartum and peripartum patient �Improve the coordination of care for the maternal sepsis patient �Begin resuscitative efforts for the septic patient �Initiating empiric antibiotic therapy

Critical Illness During Pregnancy and the Peripartum �Less than 2% of women require admission to ICU during pregnancy or peripartum � 0. 7 to 13. 5 per 1000 deliveries �Most common reasons for ICU admission �Postpartum hemorrhage �Hypertensive disorders (severe preeclampsia, HELLP) �Anything is possible during pregnancy, including sepsis

Maternal and Fetal Mortality �Maternal and fetal mortality rates are high when ICU care is required �Fetal rates vary due to multiple factors � EGA at delivery, maternal illness, maternal blood loss, maternal shock, drug abuse, lack of prenatal care, etc. �Maternal 3. 4 to 14 percent � Leading cause cardiovascular disease and cardiomyopathy � Also VTE, hemorrhage, AFE, and infection � 18% of deaths considered preventable (Am J Obstet Gynecol. 2008; 199(1): 36. e 1)

Preventable Maternal Deaths �Postpartum hemorrhage �Preeclampsia �Medication errors �Many Infections �Early bacterial sepsis �Early viral pneumonia �Pyelonephritis

So what about Maternal Sepsis? �Severe Sepsis or Septic Shock is rare � 0. 002 to 0. 01 percent of all deliveries �Or better stated � 2 to 10 out of every 100, 000 deliveries � 2015 Birth statistics �United States 3, 977, 745 � 80 to 398 cases annually expected �South Dakota 12, 323 � 0 to 1 case annually
Like winning the Lottery? �Fox News September 30, 2012 �Michigan lottery winner found dead of apparent drug overdose

Maternal Mortality with Sepsis �Maternal mortality ranges from 20 -28 percent in patients with septic shock and multiple organ failure �Risks increase �African American �Native American �Smoking- Tobacco or Marijuana �Age > 35 �Illicit drug use �Poorly controlled diabetes

Antenatal Sepsis Causes �Septic abortion �Chorioamnionitis �Complicated pyelonephritis �Pneumonia �Streptococcus pneumoniae �Influenza

Postnatal Sepsis Causes �Endometritis- most common �Wound infections �Necrotizing fasciitis �Toxic Shock Syndrome (TSS) �Pelvic abscess �Gas gangrene of myometrium- usually clostridial species of GI and vagina �Septic pelvic thrombophlebitis �Pyogenic sacroiliitis �Clostridium difficile colitis

So what is Sepsis?

Sepsis �Clinical syndrome characterized by systemic inflammation due to infection �May lead to septic shock �Mortality estimates dependent on pre-infection health status �Greater that 10 to 40 percent when shock is present � Elishauser A. - Septicemia in US Hospitals, 2009.

Sepsis �Early sepsis — Infection and bacteremia may be early forms of infection that can progress to sepsis �Identification of early sepsis is key �Sequential (Sepsis-related) Organ Failure Assessment score (SOFA) �Society of Critical Care Medicine (SCCM) and the European Society of Intensive Care Medicine (ESICM) created in 2016 �Scoring system to assess risk of mortality from sepsis in patients outside the ICU setting

Sepsis �Modified SOFA score- quick SOFA (q. SOFA) �Easily calculated with only three components �Respiratory rate >22 breaths per minute �Altered mentation �Systolic blood pressure <100 mm Hg �Mortality from sepsis 24% when two or more components are present �Prompt transfer to ICU should follow �Full SOFA score calculators are available online

Where do I Start? �When all else fails, examine your patient

The ABCs �Intubation may be required �Dyspnea common with sepsis �Depressed level of consciousness �Oxygenation �Pulse oximetry �Increased demands with sepsis �Venous access �Initial peripheral but consider central access early

Initial Investigations �Initial brief history and physical �Patient, family, emergency medical personnel, medical records �Laboratory �Microbiology �Imaging �Consider early consultation and transfer to ICU

Sepsis Management Team �Pulmonology/ ICU team leader �Obstetrics �General surgery (wound related) �Infectious disease �Neonatology (if antepartum) �Any specialty may require consultation dependent upon area of suspicion

Sepsis Management Team �What are we basing our decisions on?

Laboratory � Complete blood count with differential � Chemistries � Liver function tests � Coagulation studies including D-dimer level � Serum lactate to assess severity � Arterial blood gas analysis � Peripheral blood cultures- aerobic and anaerobic � Urinalysis � Microbiologic cultures- sputum, urine, IV catheter, wound or surgical sites, body fluids, etc. � Targeted imaging at the suspected site of infection

CBC Changes in Normal Pregnancy Non-Gravid 1 st Trimester 2 nd Trimester 3 rd Trimester White blood cell count 3. 5 -9. 1 (x 103/mm 3) 5. 7 -13. 6 5. 6 -14. 8 5. 9 -16. 9 Hemoglobin¶ (g/d. L) 12 -15. 8Δ 11. 6 -13. 9 9. 7 -14. 8 9. 5 -15. 0 Platelet (x 109/L) 165 -415 174 -391 155 -409 146 -429
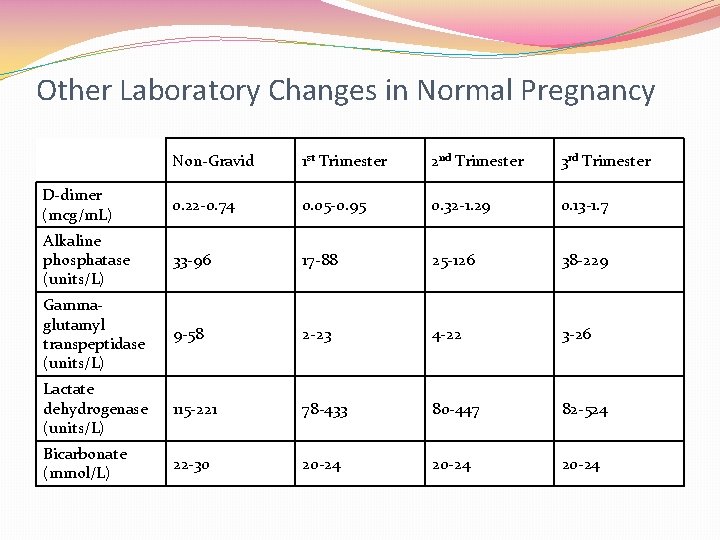
Other Laboratory Changes in Normal Pregnancy Non-Gravid 1 st Trimester 2 nd Trimester 3 rd Trimester D-dimer (mcg/m. L) 0. 22 -0. 74 0. 05 -0. 95 0. 32 -1. 29 0. 13 -1. 7 Alkaline phosphatase (units/L) 33 -96 17 -88 25 -126 38 -229 Gammaglutamyl transpeptidase (units/L) 9 -58 2 -23 4 -22 3 -26 Lactate dehydrogenase (units/L) 115 -221 78 -433 80 -447 82 -524 Bicarbonate (mmol/L) 22 -30 20 -24

Sepsis Management Team �The obstetrician is a vital member of the sepsis management team in the gravid patient to avoid delay in treatment, unnecessary attempts to correct normal pregnancy findings, and provide good outcomes for the fetus �Vital signs �Laboratory values �Imaging changes and limitations

Initial Resuscitative Therapy

Initial Resuscitative Therapy �Tissue perfusion with aggressive IV fluids � 30 ml/kg of actual body weight within the 1 st three hours �This will typically be 2 to 3 liters of IVFs �Ringer’s Lactate or Normal Saline �Caution of pulmonary edema risk in pregnancy, especially in the setting of pneumonia �Guidelines recommend against routine use of glucocorticoids but consider early use if antepartum

Initial Resuscitative Therapy �Start empiric antibiotic therapy within the first hour �Linear increase in risk of mortality for each hour of delay � Ferrer R. , Crit Care Med 2014; 42: 1749 �Obtain cultures prior to antibiotics �Do not delay antibiotics if unable to obtain cultures �Target suspected organisms and sites of infection �Fetal exposure risks to be considered prior to administration

Choosing an Antimicrobial

Choosing an Antimicrobial �Patient history- recent antibiotics, prior infections �Comorbidities- pregnancy, diabetes, organ failures �Immunologic status- HIV �Clinical setting- community vs hospital acquired �Suspected site of infection �Presence of invasive device or foreign body �Gram stain data �Local prevalence and resistance patterns

Choosing an Antimicrobial �Sepsis without shock �Broad spectrum therapy with coverage for grampositive and gram-negative therapy � May require more than one agent �Antifungal and antivirals as indicated �Sepsis with shock �Combination therapy with at least two antimicrobials from two different classes with the intent of covering a suspected pathogen with more than one agent

Choosing an Antimicrobial

Most Common Organisms in Sepsis �Escherichia coli �Staphylococcus aureus �Methicillin resistant S. aureus (MRSA) �Klebsiella pneumoniae �Streptococcus pneumoniae

Choosing an Antimicrobial �MRSA �Vancomycin �Pseudomonas �Combination of vancomycin and two of the following antipseudomonal agents � Cephalosporin, carbapenem, beta-lactam/beta-lactamase inhibitor, monobactam � Fluoroquinolones, aminoglycosides should be used cautiously with antepartum infections

Choosing an Antimicrobial �Non pseudomonal gram-negative organisms �E. coli, K. pneumoniae �Monotherapy with a third generation cephalosporin or carbapenem �Adding an aminoglycoside my increase risk for nephrotoxicity

Choosing an Antimicrobial �Empiric fungal and viral therapy is usually reserved for when the clinician has a high index of suspicion �Extended-spectrum beta-lactamases (ESBL) are enzymes that confer resistance to most beta-lactam antibiotics, including penicillins, cephalosporins, and the monobactam aztreonam �Infections with ESBL-producing organisms have been associated with poor outcomes

Choosing an Antimicrobial �Consult Infectious Disease �Consult Pharmacology �Talk to microbiology daily for results �Consider repeat cultures if not improving �Examine patient frequently if not in an ICU setting

Vasopressors �May be required with hypotension of shock �May cause vasoconstriction of uterine blood vessels �Decreased fetal blood flow, non-reassuring fetal assessment, fetal compromise, etc. �Norepinephrine- 1 st line agent in pregnancy when IV fluid resuscitation fails �Phenylephrine- 2 nd line agent, used safely to treat hypotension from spinal anesthesia �Ephedrine- 2 nd line agent, increased uterine blood flow in animal studies

Pneumonia in Pregnancy �Increased susceptibility to respiratory infection �Respiratory changes in pregnancy � 20% increase in oxygen consumption � Mild respiratory alkalosis with alveolar hyperventilation � Patient will develop hypoxia and acidosis very quickly �Increased risk aspiration pneumonia � Decrease lower esophageal sphincter tone, increase intraabdominal pressure �Increased risk acute pulmonary edema � Preeclampsia, cardiomyopathy, multiple gestation, pyelonephritis, IVF overload, tocolytic therapies, etc.

Pneumonia in Pregnancy �Incidence 0. 2 to 8. 5 per 1000 deliveries �Accounted for 30 percent of pregnancies with severe sepsis in United States �Risk factors include anemia, asthma, smoking, illicit drug use, immunocompromised �Increased risk of preterm labor and delivery, and pulmonary edema �Chest radiograph (PA and lateral) �Same indications as non-pregnant patient �Fetal radiation exposure < 0. 001 rad with abdominal shielding

Postpartum Endometritis �Infection of the decidua (endometritis), myometrium (endomyometritis), or parametrium (parametritis) �Temp >38. 0 C on any 2 of the first 10 days (excluding 1 st 24 hr postpartum) �Polymicrobial in over 70% of cases � 60% of patients had facultative gram positive and gram negative bacteria � 40% of patients had anaerobes � 30% of patients had mycoplasmas

Postpartum Endometritis �Risk factors include � Chorioamnionitis � Prolonged labor � Prolonged rupture of membranes � Multiple cervical examinations � Internal fetal or uterine monitoring � Meconium in liquor � Manual extraction placenta � Preterm birth � Operative vaginal delivery � Postterm pregnancy � Group B Streptococcus � HIV infection � Low socioeconomic status � Limited or lack of prenatal care

Postpartum Endometritis �Toxic Shock Syndrome (TSS)- early onset, high fever, hypotension and involvement of two additional organ systems (renal, liver, pulmonary, coagulopathy, tissue necrosis, skin rash with desquamation) �Group A streptococcus (GAS)- Streptococcus pyogenes �Staphylococcal TSS- often high Temp >38. 9 C � Consider MRSA �Clostridium sordellii and Clostridium perfringes � Sudden onset of clinical shock and highly lethal, absence of fever or rash

Wound Infections � 2015 Cesarean rate in United States is 32% � 1, 272, 503 cesarean births � 2015 Cesarean rate in South Dakota 25. 7% � 3167 cesarean births �Endometritis in cesareans � 6% without labor � SD~ 190 cases � 11% with labor � SD~ 348 cases �Early consideration for postoperative antibiotic coverage with cesarean delivery in the setting of endometritis

Wound Infections �Infection of the wound with cesarean 5% of patients �SD ~150 patients per year �Usually develops 4 -7 days postoperatively � 40% diagnosed after discharge �Staphylococcus epidermidis or aureus, Escherichia coli, Proteus mirabilis, or cervicovaginal flora �Early wound infections (first 48 hrs) �Group A or Group B beta-hemolytic Streptococcus �High fever, cellulitis

Maternal Sepsis �Assess your patient- exam, labs, radiology �ABCs �Drugs- initiate a broad spectrum antibiotic or combination therapy when appropriate �Consult early and often �Transfer to ICU setting �Assess your patient- exam, labs, radiology �ABCs �Etc. , etc.

Questions
- Slides: 45