Maternal Health Interventions NRHMRCHII Maternal Health Division Ministry





















- Slides: 32

Maternal Health Interventions NRHM/RCH-II Maternal Health Division Ministry of Health & Family Welfare Government of India

GOALS OF NRHM Universal Health Care • access • affordability • equity • quality

Maternal Mortality. Magnitude of the Problem • About 30 million pregnancies occur every year in India. • 27 million deliveries • 15% of these are likely to develop complications. • Complications cannot be predicted. • 77, 000 avoidable maternal deaths per year

Maternal Mortality Ratio “ number of women who die in a year due to causes related to pregnancy and child birth for every 100, 000 live births ” Wide Variations: Ø Ø Ø India 301/100, 000 live births Tamil Nadu 134/100, 000 live births U. P. 517/100, 000 live births Sweden/USA 8 -12/100, 000 live births Sri Lanka 24/100, 000 live births Malaysia 20/100, 000 live births

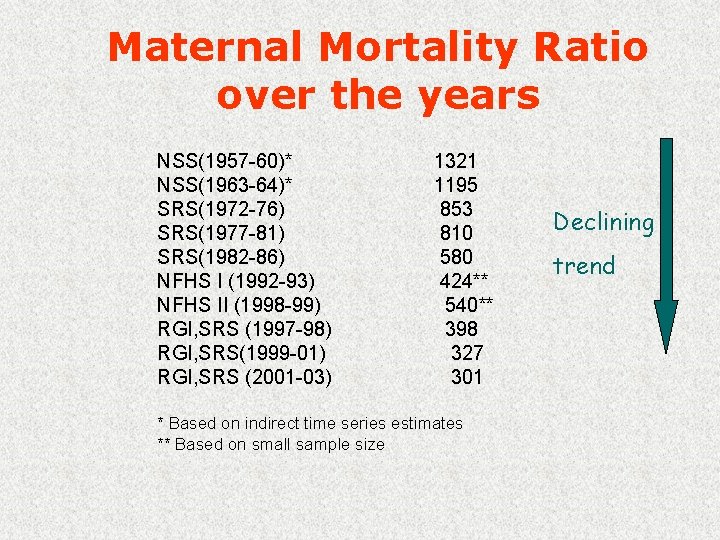
Maternal Mortality Ratio over the years NSS(1957 -60)* NSS(1963 -64)* SRS(1972 -76) SRS(1977 -81) SRS(1982 -86) NFHS I (1992 -93) NFHS II (1998 -99) RGI, SRS (1997 -98) RGI, SRS(1999 -01) RGI, SRS (2001 -03) 1321 1195 853 810 580 424** 540** 398 327 301 * Based on indirect time series estimates ** Based on small sample size Declining trend

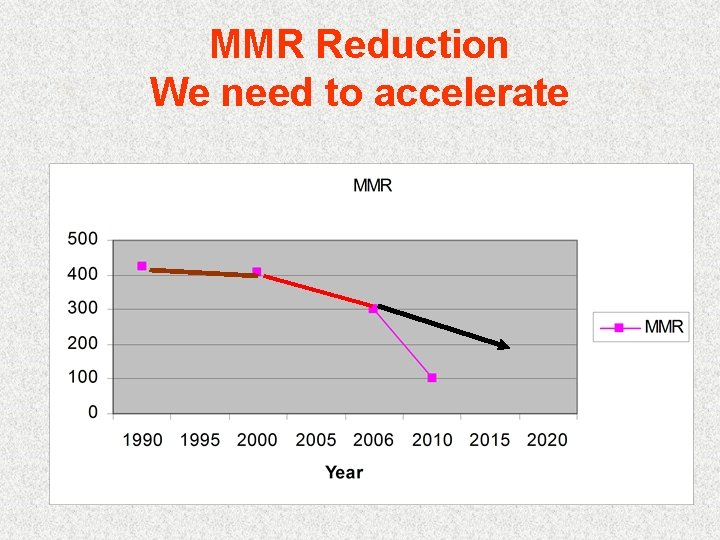
MMR Reduction We need to accelerate

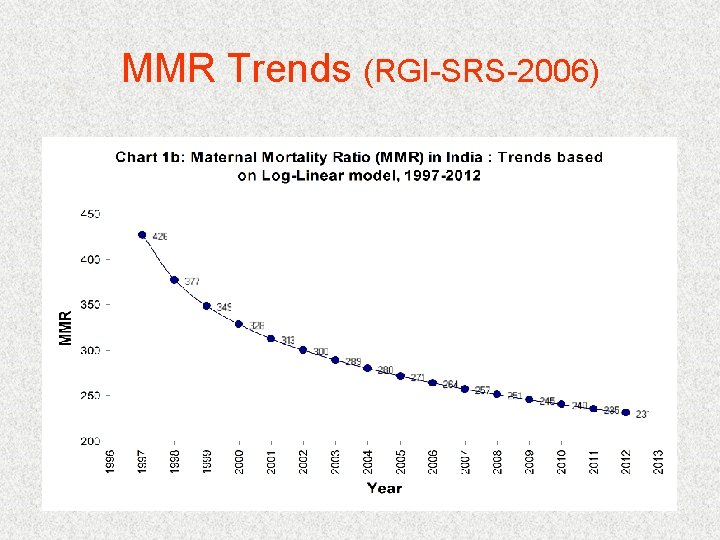
MMR Trends (RGI-SRS-2006)

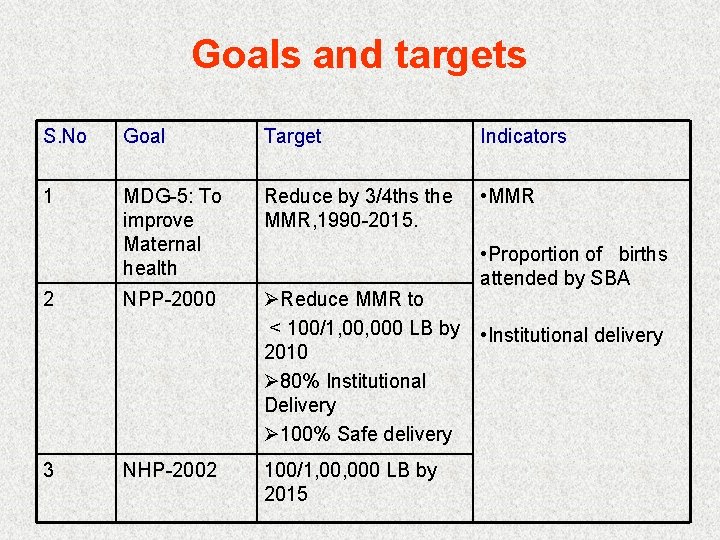
Goals and targets S. No Goal Target Indicators 1 MDG-5: To improve Maternal health Reduce by 3/4 ths the MMR, 1990 -2015. • MMR NPP-2000 ØReduce MMR to < 100/1, 000 LB by 2010 Ø 80% Institutional Delivery Ø 100% Safe delivery 2 3 NHP-2002 100/1, 000 LB by 2015 • Proportion of births attended by SBA • Institutional delivery

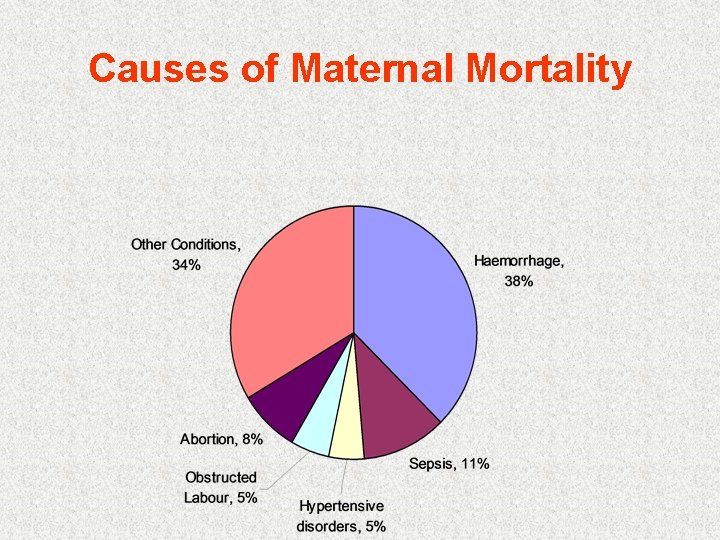
Causes of Maternal Mortality

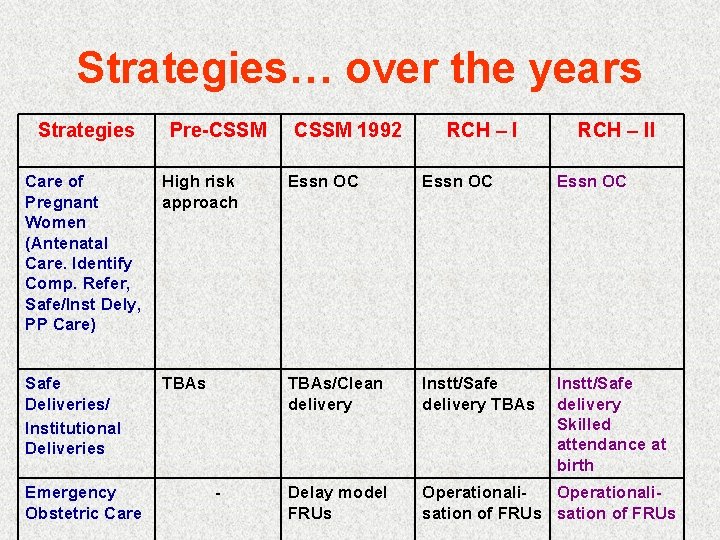
Strategies… over the years Strategies Pre-CSSM 1992 RCH – II Care of Pregnant Women (Antenatal Care. Identify Comp. Refer, Safe/Inst Dely, PP Care) High risk approach Essn OC Safe Deliveries/ Institutional Deliveries TBAs/Clean delivery Instt/Safe delivery TBAs Instt/Safe delivery Skilled attendance at birth Delay model FRUs Operationalisation of FRUs Emergency Obstetric Care -

ISSUES IN MATERNAL HEALTH • SOCIAL • Age at marriage • Maternal Care • Women’s status • PROGRAMMATIC • Antenatal care • Skilled attendance at birth • Emergency Obstetric care • Adopting a Lifecycle approach to Women’s health

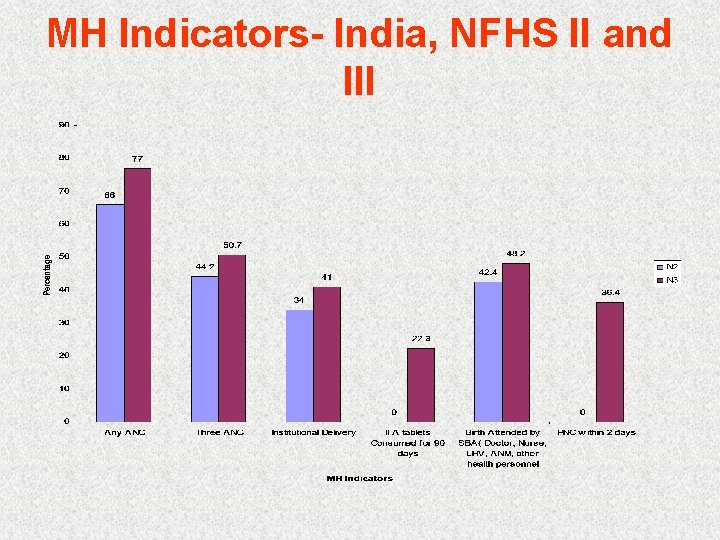
MH Indicators- India, NFHS II and III

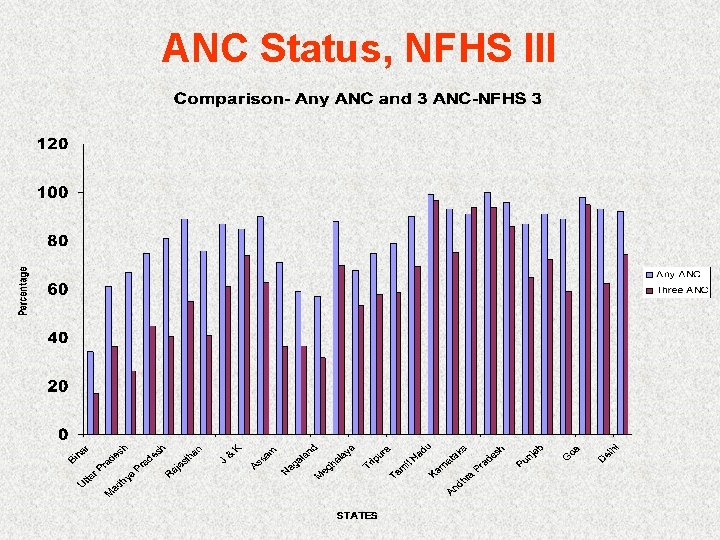
ANC Status, NFHS III

INSTITUTIONAL & SAFE DELIVERIES NFHS III

Key MH Strategies in RCH-II • Essential and Emergency Obstetric Care Ø Quality ANC, PNC, Institutional and Safe Delivery. Ø Skilled Attendance at birth (domiciliary & health facilities). Ø Operationalise FRUs, CHCs and 24 Hrs PHC. Ø Strengthen Referral Systems. • • • Management of RTIs & STIs at PHCs & CHCs/FRUs. Safe Abortion Services - MVA at PHC level. Infection Management and Environment Plan (IMEP).

NRHM • Accredited Social Health Activist (ASHA) – one per 1000 population • Janani Suraksha Yojana • Inter-sectoral Convergence. Facility Strengthening / Improving Access • • • Strengthening of Infrastructure- IPHS Improving availability of Human Resource Untied funds at sub centres Rogi Kalyan Samitis (Hosp. Mgmt. committees) Involvement of Professional associations and medical colleges • Public private partnership

Essential Obstetric Care • • • Early Registration (12 -16 wks) 3 Antenatal Check-ups Prevention & Treatment of anemia Institutional /Safe Delivery Postnatal Check-up

Basic. Em. OC • • Parenteral A/B Parent. Oxytocics Anticonvulsants Digital removal of POC • MRP • Assisted vaginal delivery Comp. Em. OC • • All functions of Basic. Em. OC + Cs sections Blood transfusion

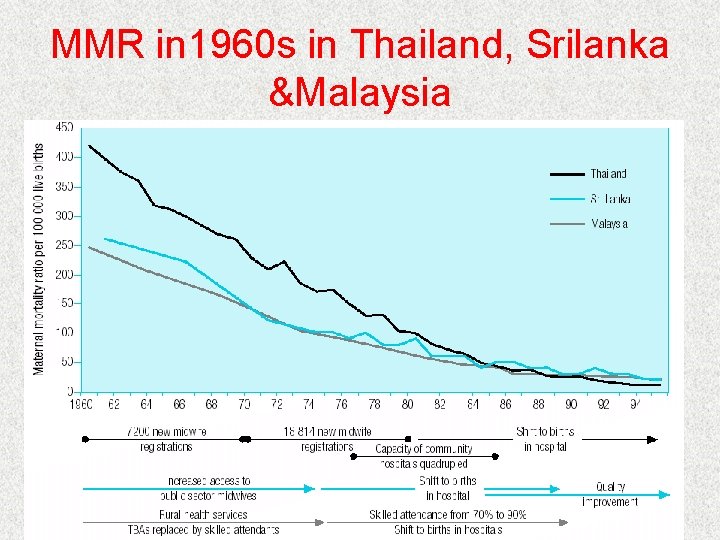
MMR in 1960 s in Thailand, Srilanka &Malaysia

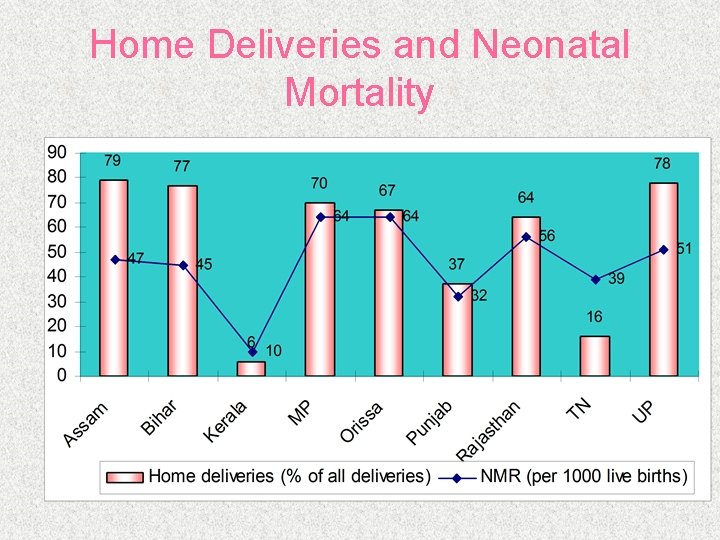
Home Deliveries and Neonatal Mortality

SKILLED BIRTH ATTENDANCE • Skilled Birth Attendant • Enabling Environment

Issues related to Skilled attendance at Birth • Reorienting Medical Officers • Preservice & inservice training for SNs/LHVs/ANMs • Operationalising SCs/ PHCs/CHCs/FRUs for skilled attendance at birth. (Enabling Environment)

Skilled Birth Attendance POLICY DECISIONS Empower Health Worker for some Basic Em. O. C. interventions • Permission to use drugs for prevention of PPH. • Permission to use drugs in emergency situations before referral • Permission to perform basic procedures at community level in emergency situations

Emergency Obstetric Care § Critical factor- TIME: 3 delay model. ü Decision to seek care ü Arrival at health facility ü Provision of adequate care at health facility § 24 X 7 PHCs First Referral Units (FRUs) at sub-district level.

Janani Suraksha Yojana • 100% centrally sponsored scheme • Promotes institutional delivery among poor pregnant women • Cash assistance to eligible women for delivery • Special dispensation for 10 states with low institutional delivery ( LPS) • ASHA- Link between beneficiary & govt. in LPS—other states are HPS

Policies and guidelines • Operationalising FRUs. • Setting up Blood Storage Units. • Operationalisation of 24 x 7 PHCs. • MTP up to 8 weeks pregnancy using MVA technique • Training of MBBS Doctors in Anesthesia skills. • Training of MBBS Doctors in Em. OC including CSection in partnership with FOGSI. • Pregnancy care and Management of Common Obstetric Complications by MOs. • AN Care and SBA for ANMs /LHV/Staff Nurses. • Guidelines for RTIs and STIs including HIV/AIDS

Thrust Areas of Maternal Health • Operationalising all FRUs for Em. OC • Establishing Blood storage Centers/ Banks • All CHCs and 24 Hrs PHCs for round the clock delivery, newborn services, MTP and RTI/STI services • Expediting the Implementation of • SBA training • Anesthesia training • Em. OC training • Regular Quality assurance, implementation review and monitoring

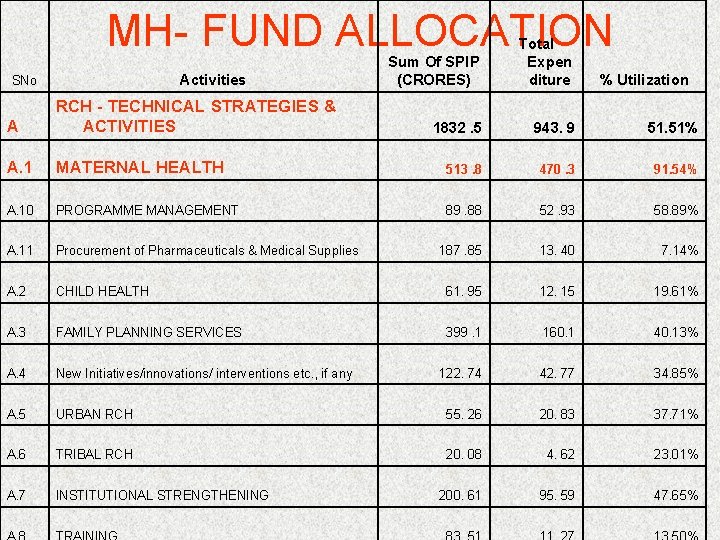
MH- FUND ALLOCATION Activities SNo Sum Of SPIP (CRORES) Total Expen diture 1832. 5 943. 9 51. 51% % Utilization A RCH - TECHNICAL STRATEGIES & ACTIVITIES A. 1 MATERNAL HEALTH 513. 8 470. 3 91. 54% A. 10 PROGRAMME MANAGEMENT 89. 88 52. 93 58. 89% A. 11 Procurement of Pharmaceuticals & Medical Supplies 187. 85 13. 40 7. 14% A. 2 CHILD HEALTH 61. 95 12. 15 19. 61% A. 3 FAMILY PLANNING SERVICES 399. 1 160. 1 40. 13% A. 4 New Initiatives/innovations/ interventions etc. , if any 122. 74 42. 77 34. 85% A. 5 URBAN RCH 55. 26 20. 83 37. 71% A. 6 TRIBAL RCH 20. 08 4. 62 23. 01% A. 7 INSTITUTIONAL STRENGTHENING 200. 61 95. 59 47. 65%

MIES –NRHM : MH Indicators ØAnnual Return-Part C: Annual. xls ØQuarterly Return : Part Q 3, Q 4, Q 7, Q 13, Q 14, Q 24 Quarterly. xls ØMonthly Return : Part A: M-100, 200, Part B : M 1, 2, 3, 5, 6, 7, 8, 9 Monthly. xls

Operating Manual- State PIPs-RCH-II Flexipool Ø Annexure 3 b : Indicative format for current status and targets. Annexure 3 b. doc Ø Annexure 3 d: Format for Annual Work Plan Annexure 3 d. xls Ø Annexure 3 e: Detailed Budget Format Anne 3 e. xls Ø Annexure 4 a : Format for Quarterly progress Report (QPR)-Physical and Financial Annex 4 a. xls

Maternal Health Division- Reporting formats Ø Maternal health activities : Monitoring Format for MH Activities. doc Ø Anesthesia Training: Reporting Format for States for Anesthesia. Trg. Final. doc Ø SBA Training : SBAplanmatrix( Final). doc Ø Em. OC Training : Reporting format for FOGSI Training. doc
