Maternal Early Warning System MEWS Implementation Tips Electronic





















- Slides: 27

Maternal Early Warning System (MEWS): Implementation Tips: Electronic Health Record Integration and Data July 11, 2019 Texas Collaborative for Healthy Mothers and Babies Texas Perinatal Quality Collaborative

Presenters Catherine Eppes, MD, MPH Baylor College of Medicine TCHMB OB Subcommittee Co-Chair Christina Davidson, MD Baylor College of Medicine TCHMB OB Subcommittee Co-chair

Objectives • Review maternal early warning systems • Illustrate integration examples for the electronic health record • Discuss how data can assist with implementation • Q&A 3

Maternal Early Warning Systems • System of escalation based on maternal vital signs • Developed to facilitate timely recognition, diagnosis, and treatment for women developing critical illness 4

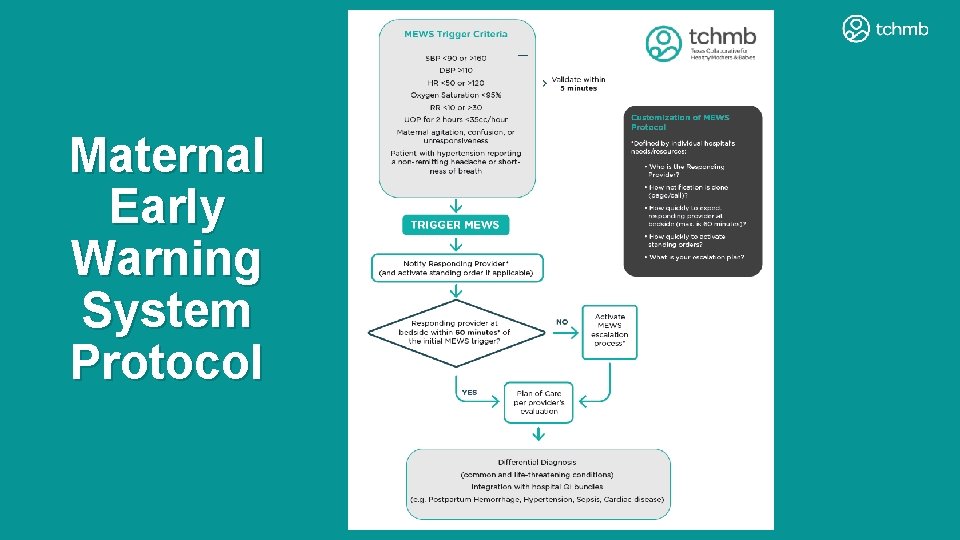
Maternal Early Warning System Protocol

Validate vital signs 5 minutes 6 6

Action Steps 1. Educate all health care personnel on the vital signs/scoring system to trigger the MEWS 2. Create a SPECIFIC response system in your hospital to MEWS 3. Create and educate on the ESCALATION system 4. Collect data to track your outcomes

Electronic Health Record Integration

Example 1: No integration • Care team is aware of vital signs that should activate MEWS • Nurse calls provider to notify him/her of MEWS • Provider comes to bedside immediately or activates order set and then comes to bedside • Nurse and provider document their intervention, diagnosis and plan in the chart • Data is tracked by audits and clinical collection

Example 1: No integration • ADVANTAGES • No delay in recognition and response: immediate recognition of MEWS triggers with immediate provider notification • DISADVANTAGES • Pregnant/post-partum women in nonobstetric units (e. g. emergency department, ICU) may have primary care team not as familiar with MEWS triggers • Reliance on individual knowledge of MEWS triggers in non-obstetric units may lead to delayed recognition and response that could be averted with alert from electronic health record (EHR)

Example 2: Utilize Best Practice Alerts to notify care team of vital signs Alert: MEWS Trigger Criteria: HR 124 Activate MEWS Alert: Score 3 = MEWS Trigger Criteria: HR 124, SBP 85 Activate MEWS

Example 2: Utilize Best Practice Alerts to notify care team of vital signs • ADVANTAGES • DISADVANTAGES • Eliminates exclusive reliance on an • Reliance on nurse/provider to enter a patient’s chart to be notified of the alert individual to activate MEWS rather than immediate notification after an abnormal vital sign is obtained • Provides an additional layer of recognition to ensure a trigger is • Inherent time delay between abnormal vital not missed sign and nurse/provider notification • Trains care team to wait for the EHR to • In more complex MEWS systems prompt them of worsening maternal that are based on scoring or more condition rather than recognizing the than 1 trigger, may help reduce abnormal VS on their own error in calculations/recognition

Example 3: Build order sets for MEWS (with or without BPA) q q q q Alert: MEWS Trigger Criteria: HR 124 Activate MEWS q q q q Order Set for MEWS with concern for PPH: Place peripheral IV Bolus 500 cc lactate ringers Methergine 0. 2 mg IM every 2 -4 hours up to 5 doses Hemabate 0. 25 mg IM every 15 minutes up to 8 doses Pitocin 30 units in 500 m. L infusion or 10 units IM Misoprostol (cytotec) 400 -1000 mcg rectal or 600 mcg buccal Tranexamic acid 1 g to be infused over 10 to 20 minutes (infusion >1 m. L/minute can cause hypotension). If bleeding persists after 30 minutes, a second one gram dose can be administered CBC INR, PTT Fibrinogen Thromboelastogram Crossmatch XX units Transfuse XX units of XX Vitals signs q 5 min for XX time

Example 3: Build order sets for MEWS • ADVANTAGES • DISADVANTAGES • Same as examples 1 and 2 • Built-in order sets for the more common diagnoses associated with MEWS triggers facilitates rapid diagnostic work-up even before provider is at bedside • High reliance on order sets without consideration of patient’s medical history may distract from less common but life-threatening diagnoses • Example: order set for fever and tachycardia may only focus on sepsis evaluation and omit important labs in a woman with poorly-controlled hyperthyroidism who may be in thyroid storm

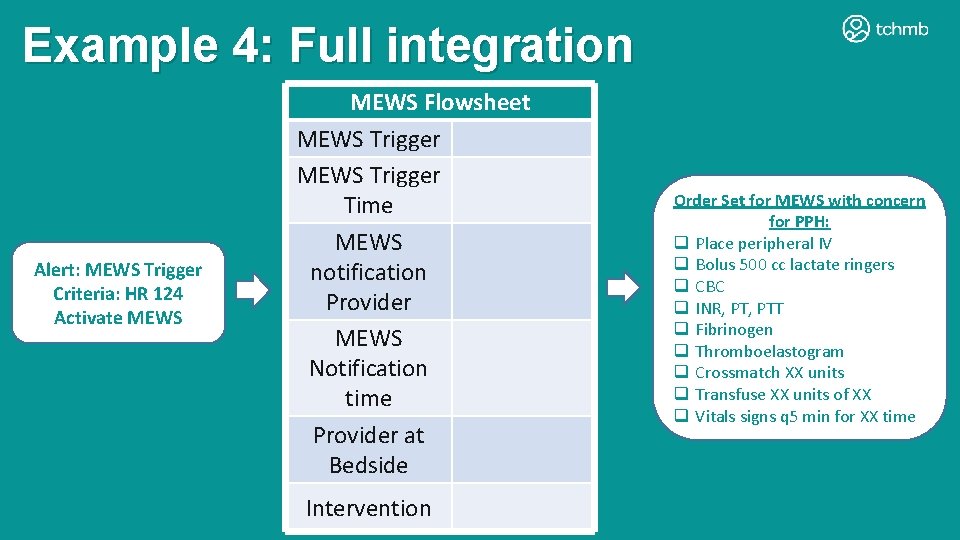
Example 4: Full integration Alert: MEWS Trigger Criteria: HR 124 Activate MEWS Flowsheet MEWS Trigger Time MEWS notification Provider MEWS Notification time Provider at Bedside Intervention Order Set for MEWS with concern for PPH: q Place peripheral IV q Bolus 500 cc lactate ringers q CBC q INR, PTT q Fibrinogen q Thromboelastogram q Crossmatch XX units q Transfuse XX units of XX q Vitals signs q 5 min for XX time

Example 4: Full Integration • ADVANTAGES • DISADVANTAGES • Same as examples 2 and 3 • MEWS documentation tool is prompted by EHR recognition of MEWS trigger; eliminates need to enter separate part of EHR for documentation and ensures documentation occurs (“hard stop” prior to diagnostic workup) • Activating an order set based on VS alone may lead to work-up of incorrect diagnosis due to overlap in VS abnormalities • Example: a woman with tachycardia and hypotension may have either hemorrhage or sepsis and diagnostic work up should incorporate clinical history and physical exam findings

MEWS Flowsheet Example: Flowsheet or Documentation Tool for MEWS Process in EHR MEWS Trigger SBP 80 MEWS Trigger Time 16: 15 MEWS notification Provider Dr Eppes MEWS Notification time 16: 20 Provider at Bedside 16: 26 Intervention 16: 45

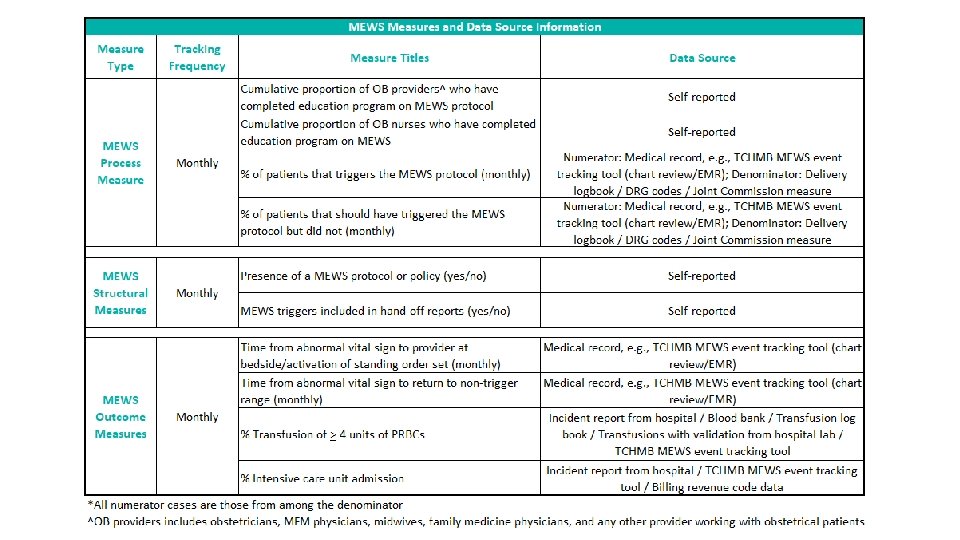
Example: Creating an audit from aspects of EHR for process/outcome measures

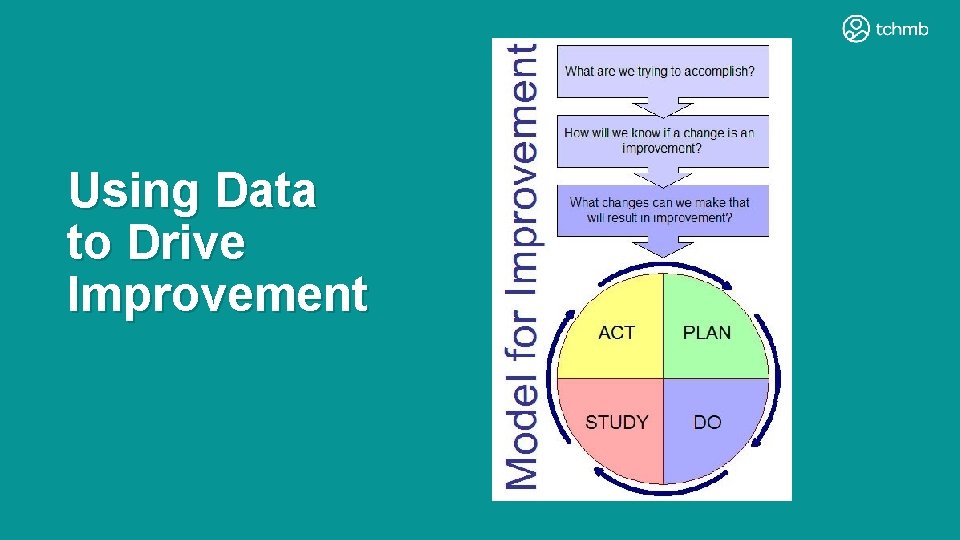
Using Data to Drive Improvement

20

MEWS Documentation

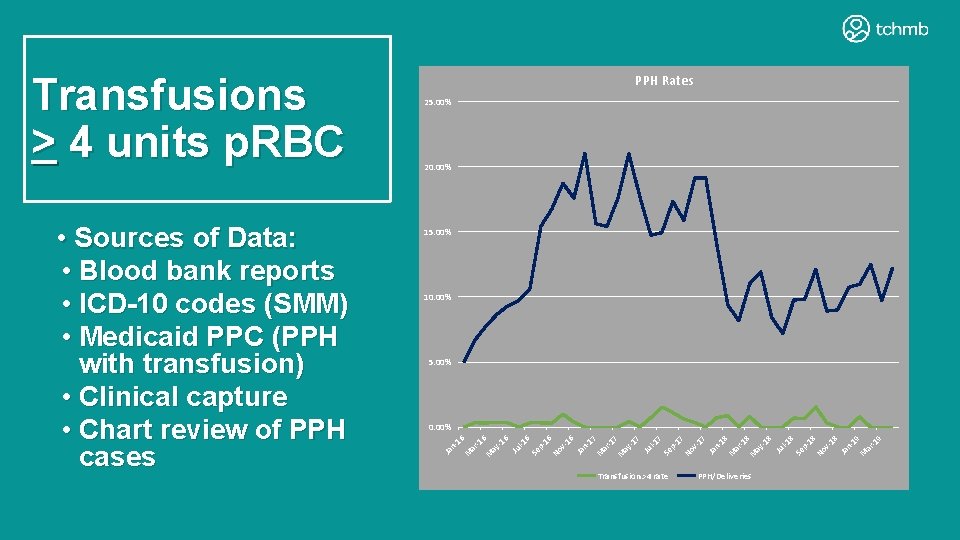
20. 00% 15. 00% 10. 00% 5. 00% 9 -1 ar n- 19 M 18 Ja v- 18 p- No 8 Se l-1 8 -1 ay PPH/Deliveries Ju 8 -1 M ar n- 18 M 17 Ja v- 17 p- Transfusion >4 rate No 7 Se l-1 7 -1 ay Ju 7 -1 M ar n- 17 M 16 Ja v- 16 No p- 6 Se l-1 6 -1 ay Ju 6 -1 M ar n- 16 0. 00% M • Sources of Data: • Blood bank reports • ICD-10 codes (SMM) • Medicaid PPC (PPH with transfusion) • Clinical capture • Chart review of PPH cases 25. 00% Ja Transfusions > 4 units p. RBC PPH Rates

MEWS Vital sign and time MEWS Triggers and Times Location of patient Time and person who is notified Time at Bedside Time vital sign is not in MEWS range

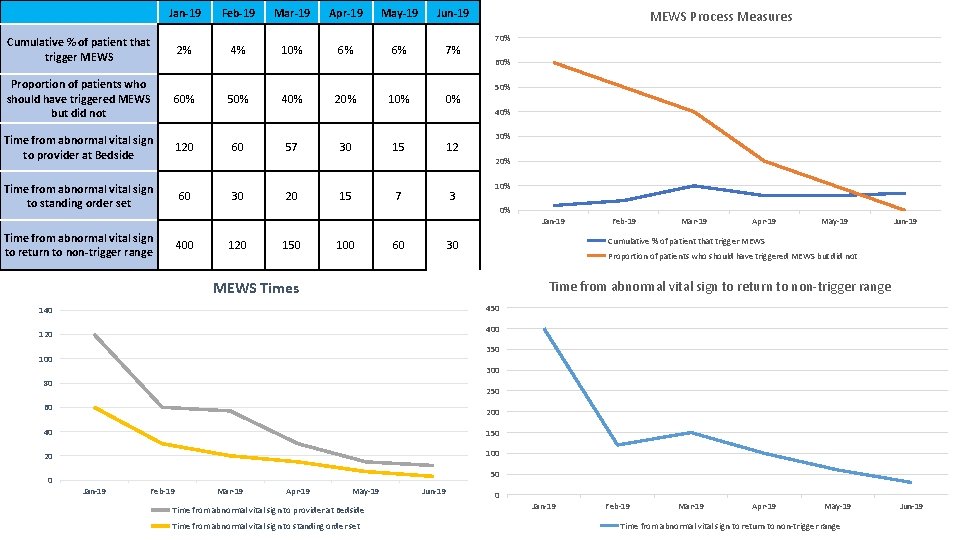
Jan-19 Feb-19 Mar-19 Apr-19 May-19 Jun-19 Cumulative % of patient that trigger MEWS 2% 4% 10% 6% 6% 7% Proportion of patients who should have triggered MEWS but did not 60% Time from abnormal vital sign to provider at Bedside 120 Time from abnormal vital sign to standing order set 60 MEWS Process Measures 70% 60% 50% 40% 20% 10% 0% 50% 40% 60 57 30 15 12 30% 20% 30 20 15 7 3 10% 0% Time from abnormal vital sign to return to non-trigger range 400 120 150 100 60 Jan-19 Feb-19 Mar-19 Apr-19 May-19 Jun-19 Cumulative % of patient that trigger MEWS 30 Proportion of patients who should have triggered MEWS but did not Time from abnormal vital sign to return to non-trigger range MEWS Times 450 140 400 120 350 100 300 80 250 60 200 40 150 20 100 0 50 Jan-19 Feb-19 Mar-19 Apr-19 May-19 Time from abnormal vital sign to provider at Bedside Time from abnormal vital sign to standing order set Jun-19 0 Jan-19 Feb-19 Mar-19 Apr-19 May-19 Time from abnormal vital sign to return to non-trigger range Jun-19

Texas Perinatal Quality Collaborative: TCHMB Questions?

Texas Perinatal Quality Collaborative: TCHMB Technical assistance from TCHMB QI nurse Amanda Wagner Contact information: Texas. AIM@dshs. texas. gov

Texas Perinatal Quality Collaborative: TCHMB Thank you!!