Massive and Submassive PE Is intravenous therapy sufficient

Massive and Submassive PE Is intravenous therapy sufficient or is intervention indicated? Piotr Sobieszczyk M. D. Cardiovascular Division Vascular Medicine Section Cardiac Catheterization Laboratory

No Financial Disclosures

Pulmonary Embolism Wide spectrum of clinical manifestations and risk Choice of therapy depends on severity of PE, patient substrate and local expertise Low Clinical Risk Intermediate Clinical Risk Subsegmental, hemodynamically tolerated PE. Favorable prognosis with AC alone 30 -50% are sub-massive PE RV strain w/o hemodynamic compromise. Increased mortality, ? 10% progress to massive PE ? Long term functional status High Clinical Risk 4. 5% of PE are “massive”: RV failure hemodynamic instability SBP<90 mm. Hg, ↓ BP by 40 mm. Hg>15 min Syncope, cardiac arrest. 90 -day mortality of 50%%.

Massive and Submassive PE: Treatment Strategies § Basic therapies § Intravenous anticoagulation § Supportive care, supplemental oxygen § Advanced Therapies § Intravenous thrombolysis: t. PA, TNK § Invasive therapies § Surgical embolectomy § Catheter-based embolectomy and thrombolysis

Massive PE: Thrombolytic Therapy § Reversal of RV failure, restoration of hemodynamic stability and oxygenation § Despite paucity of data, systemic thrombolysis is the accepted standard of care § 50% of these patients have contraindication to thrombolysis § Hemorrhagic complications § Delayed onset of action, prolonged infusion

Intravenous Thrombolytic Delivery In vitro model of obstruction in the right main PA. High-speed photo of systemically injected glass beads demonstrates how a vortex forms proximal to the obstruction and alters systemic drug delivery away from target embolus. Schmitz-Rhode. Cardiovasc Intervent Radiol 1998; 21: 199 -204

Massive PE: Surgical Embolectomy § Surgical embolectomy proposed by Trandelenburg 1908 § First performed by Kirschner 1924 and soon abandoned § Revisited in 1960 s and associated with 30% mortality § Technical advances lead to renewed interest, systemic reviews over last 10 -20 years still describe 20% mortality § Limited to centers with expertise and ability to rapidly mobilize the resources § Complete or near complete thrombus removal and reduction in RV afterload

Endovascular Therapy § Less invasive, rapidly available § Lack of devices designed to deal with large volume of organized thrombus § Adaptation of techniques designed for acute thrombus in small vessels § Incomplete relief of obstruction – maybe enough to reverse RV failure in massive PE
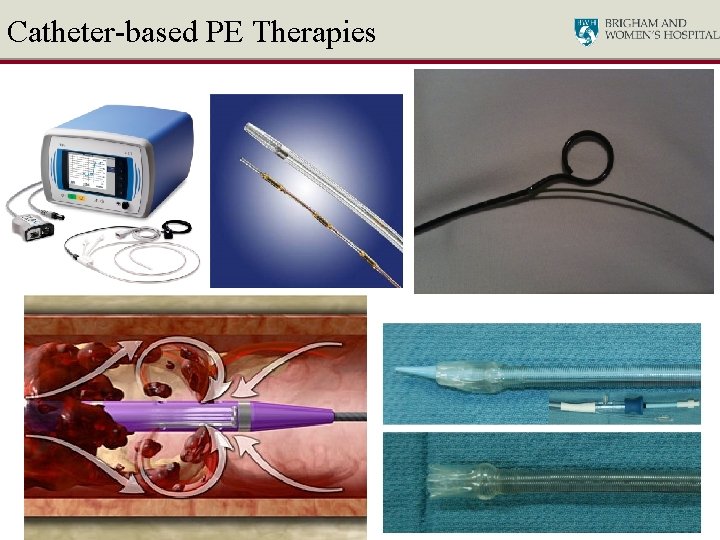
Catheter-based PE Therapies
Endovascular Therapy: § Pooled clinical success rate: 86. 5% (p=0. 004) § Clinical success much higher with local lytic delivery during procedure and higher still with extended delivery § Minor complication rate was 8% § Major complication rate was 2. 4% Kuo WT, JVIR 2009; 20: 1431

Submassive PE: More of a dilemma…. § Many of these patients do well with anticoagulation and supportive care § Some do not…. . § Chronic PHT rare, RV remodels…. . § Escalation of therapy may be harmful in many § Systemic thrombolysis not shown to be effective § But want is the long-term fate of the RV? ?
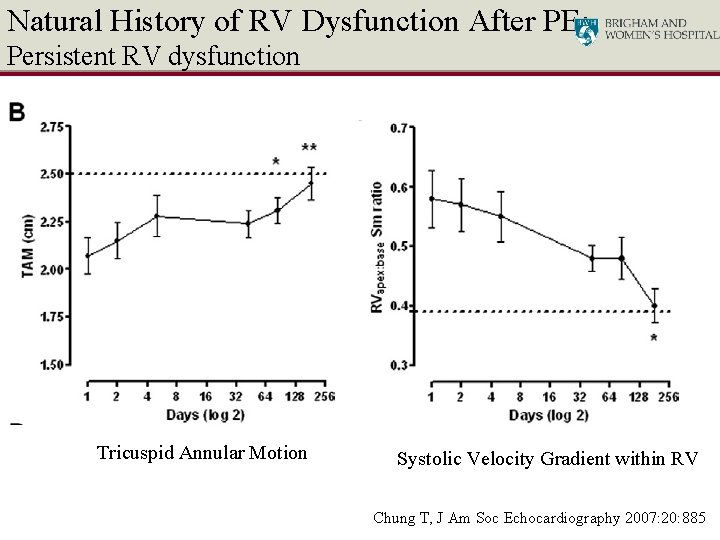
Natural History of RV Dysfunction After PE: Persistent RV dysfunction Tricuspid Annular Motion Systolic Velocity Gradient within RV Chung T, J Am Soc Echocardiography 2007: 20: 885
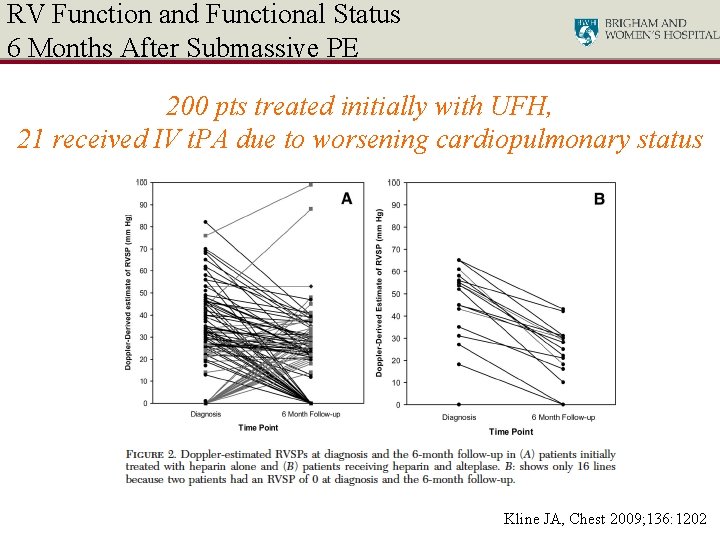
RV Function and Functional Status 6 Months After Submassive PE 200 pts treated initially with UFH, 21 received IV t. PA due to worsening cardiopulmonary status Kline JA, Chest 2009; 136: 1202
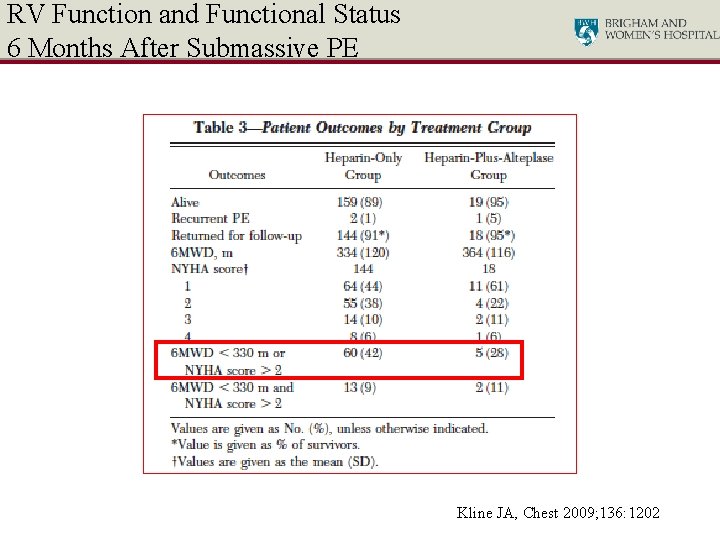
RV Function and Functional Status 6 Months After Submassive PE Kline JA, Chest 2009; 136: 1202
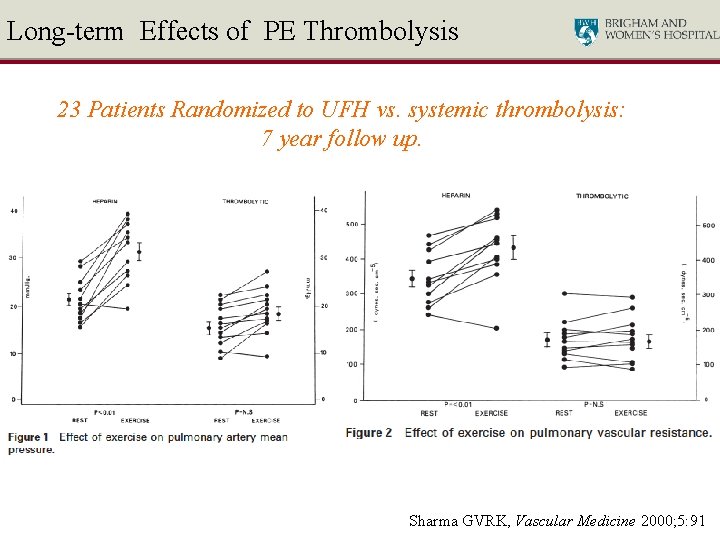
Long-term Effects of PE Thrombolysis 23 Patients Randomized to UFH vs. systemic thrombolysis: 7 year follow up. Sharma GVRK, Vascular Medicine 2000; 5: 91

Long-term Effects of PE Thrombolysis 23 patients randomized to UFH vs. systemic thrombolysis: 7 year follow up Sharma GVRK, Vascular Medicine 2000; 5: 91
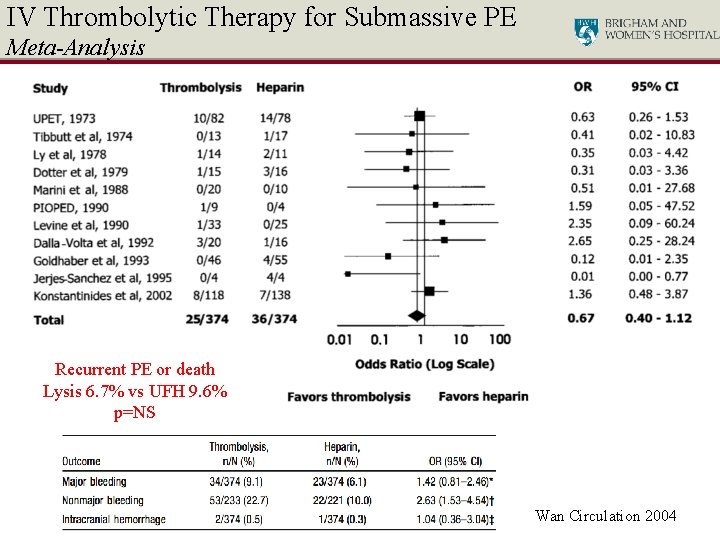
IV Thrombolytic Therapy for Submassive PE Meta-Analysis Recurrent PE or death Lysis 6. 7% vs UFH 9. 6% p=NS Wan Circulation 2004

Systemic thrombolysis in submassive PE: ongoing randomized trials § PEITHO: Pulmonary Embolism Thrombolysis Study (tenectaplase): § 1000 pts in Europe with RV dysfunction on echo and elevated troponin § Primary outcome: development of circulatory shock or respiratory failure § TOPCOAT: Tenectaplase or Placebo: Cardiopulmonary Outcomes at Three Months § 200 patients in US with RV HK on echo, elevated troponin, elevated BNP or RA sat<95% § Primary outcome: RV dysfunction and NYHA association worse than II and 6 minute walk <330 m 18
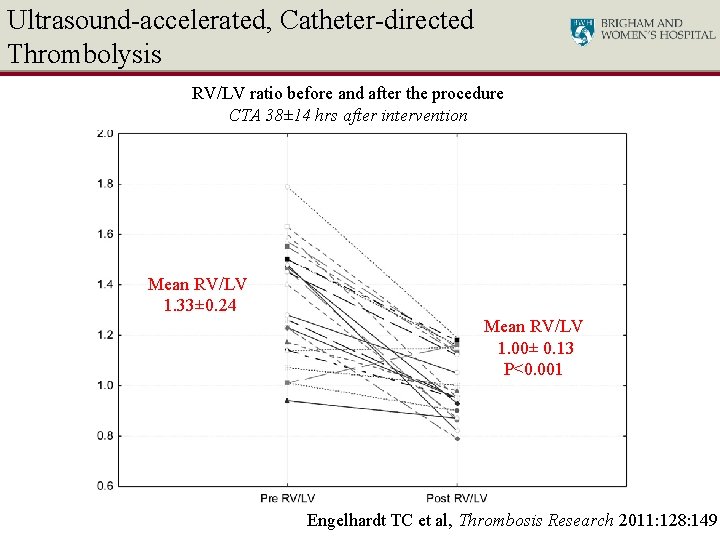
Ultrasound-accelerated, Catheter-directed Thrombolysis RV/LV ratio before and after the procedure CTA 38± 14 hrs after intervention Mean RV/LV 1. 33± 0. 24 Mean RV/LV 1. 00± 0. 13 P<0. 001 Engelhardt TC et al, Thrombosis Research 2011: 128: 149
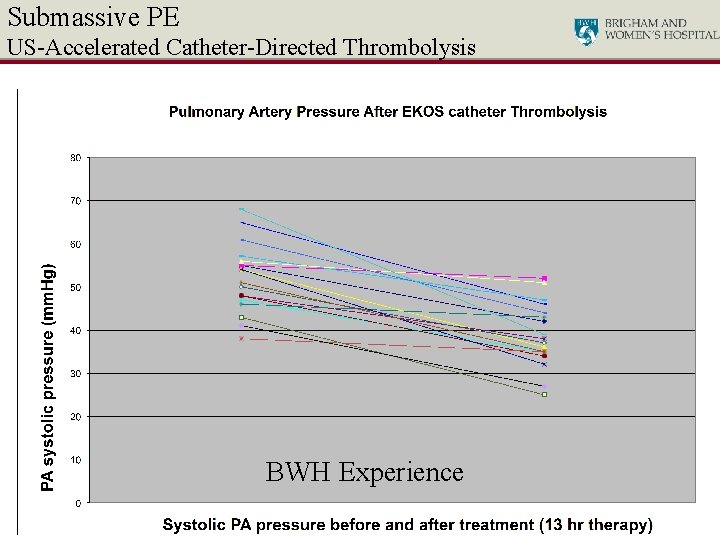
Submassive PE US-Accelerated Catheter-Directed Thrombolysis BWH Experience

SEATTLE Trial § Hypothesis: Treatment of selected pulmonary embolism (PE) patients with intra-clot delivery of ultrasound-accelerated, lowdose thrombolysis will significantly improve their right heart function at 48 hours compared to anticoagulant-treated historical controls § Safety objectives: Major bleeding within 72 hours, periprocedural complications, death and recurrent PE at 30 d § Study population: 100 pts with acute, symptomatic PE and RV/LV end-diastolic ratio >0. 9 on CT § Treatment: EKOS catheter delivered t. PA 1 mg/hr per lung for 12 hrs. if bilateral PE or 1 mg/hr for 24 hrs if unilateral PE § Primary Efficacy Outcome: Change in RV/LV ratio from baseline to 48 hrs. § Secondary Efficacy Outcome: Change in PA pressure from baseline to end of t. PA infusion. PA pressure on echo 48 hrs. after start of procedure. 21

Massive PE: choice of therapy § Rapid triage similar to acute coronary syndrome care § Hemodynamic support § Inotropes § Percutaneous RVAD § ECMO § Rapid reduction of thrombotic burden: strategy based on local expertise § IV thrombolysis – transfer to “PE center” § Catheter-based intervention § Surgical embolectomy

Submassive PE: choice of therapy § § Anticoagulation, supportive care Systemic thrombolysis not beneficial at present Surgical embolectomy: an “overkill” Catheter-based thrombolysis in “PE center” § More rapid clinical improvement § Potential for shorter hospitalization § Possible long term functional benefit in selected patients. § More data is desperately needed

24
- Slides: 24