Mark Bromley Emergency Medicine PGY3 BOWEL DISEASE LARGE

Mark Bromley Emergency Medicine PGY-3 BOWEL DISEASE LARGE AND SMALL

Overview Cases Approach – Work-up Appendicitis Dealing with surgeons Mesenteric Ischemia ABD films SBO 2

Case 21 ♂ with ABD pain onset ~ 24 h Pain Peri-umbilical Escalating to 8/10 Fevers/Chills Emesis x 3 this AM OE: 38. 1 o. C 16 85 122/81 ABD: Diffuse peri-umbilical No Rebound/Guard 3

Case PMHx: Well PSHx: None Meds: Nil Allergies: NKDA 4

Approach Anatomic Systems 5
Work-up Bloodwork Urine R&M CBC, lytes, Cr INR, PTT ALT, ALP, Bili, GGT Lipase Blood cultures ♀ BHCG Imaging Plain films - 3 views CT ABD/Pelvis US ESR/CRP 6
Case Order your work-up Morphine 2. 5 -5 mg IV for pain Return in 1 -2 h Comfortable Pain – now in RLQ Tender at Mc. Burneys 7

Appendicitis - Classic Pain Vague peri-umbilical pain that localizes to the RLQ (Mc. Burney’s) …↑ over 12 to 24 h period Pain lasting more than 36 h is rare – or perfed Febrile Anorexic Elevated WBC Rosvings, Psoas, Obturator 8

Signs Psoas sign With pt supine, flex hip against resistance by pushing down against knee -- pain = +ve Obturator sign Passively flex hip & knee and internally rotate leg at the hip -- pain = +ve Rosvings sign press down in LLQ then release suddenly - pain = + ve

Differentiate into 3 groups 1. High suspicion for appendicitis – need for immediate surgery i. e. classic presentation 2. Intermediate suspicion for appendicitis – no clear-cut need to go to OR yet 3. Atypical presentation Low suspicion for appendicitis

Appendicitis Expedient diagnosis Non-ruptured - - -Mortality 0. 6% Ruptured - - - - Mortality 5% …the blood was clotted …nurses are sure the lab dropped it Surgeon wants a WBC before seeing 11

Appendicitis – Role of WBC Methods: prospective consecutive case series All patients presenting to the ED in whom the diagnosis of appendicitis was the attending physician’s primary consideration Patient temperature as taken in the ED, initial total WBC count, and discharge diagnosis. Results: N=293 wbc > 10 (+LR) 1. 59 wbc > 12 (+LR) 2. 70 (-LR) 0. 46 Fever > 37. 2 o. C (+LR) 1. 30 (-LR) 0. 82 12

Liklihood Ratio likelihood ratio, is the ratio of the maximum probability of a result under two different hypotheses Probability of ↑WBC with Appy -------------------- = LR Probability of ↑WBC w/o Appy 13

Probability of ↑WBC with Appy __________ Probability of ↑WBC w/o Appy 14
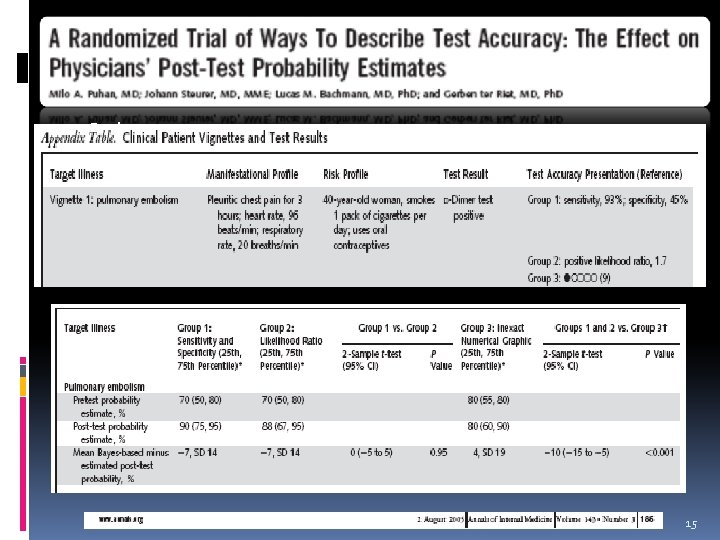
Design: Setting: Auditorium at a continuing medical education conference. Participants: 183 physicians. Intervention: Random assignment of vignettes with different presentation formats of diagnostic test accuracy. After estimating probabilities of 6 common illnesses described in patient vignettes, physicians Results: post-test probability estimates deviated to a small and similar extent from Bayes-based estimates in the groups informed by sensitivity and specificity or likelihood ratios. An inexact numerical graphic led physicians to come closer to Bayes-based estimates in the PE and chronic obstructive pulmonary COPD vignettes some physicians estimated lower illness probabilities after a positive test result if it was accompanied by a low test accuracy value. 15
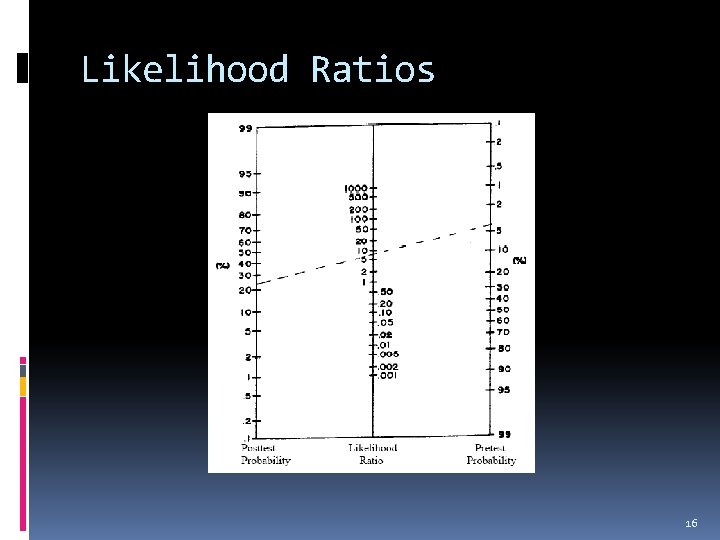
Likelihood Ratios 16

Odds and Probability …only works with odds I’ll give you twenty to one odds 20: 1 probability = 20/total (21) = 95% chance Forty to sixty odds = 40: 60 = 40/60 = 0. 66 probability = 40/total (100) = 40% chance 17

Likelihood Ratios 18

Likelihood Ratio % chance this guy has an appy = 0. 4 (40%) Convert that to odds (pretest) 0. 4/0. 6 = 4/6 = 2/3 (2/3) x 3 = 6/3 = 2 Convert back to probability (posttest) 2/3 = 0. 67 (67%) 19
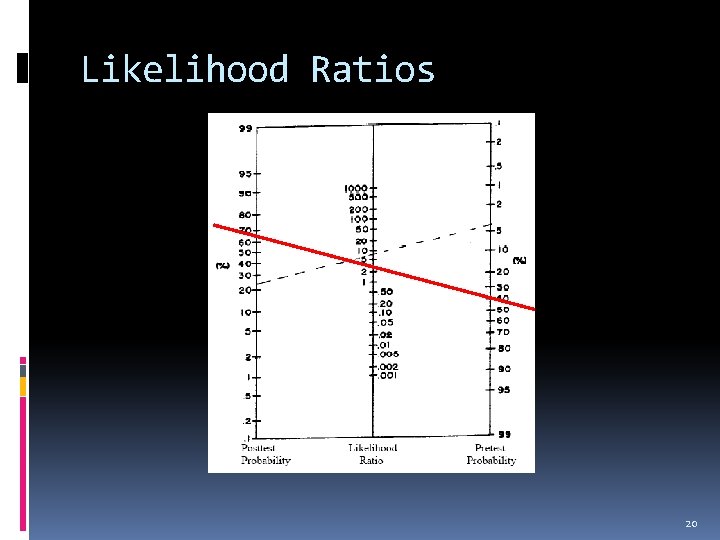
Likelihood Ratios 20

Likelihood Ratio As a rule (+) LR > 10 (-) LR <0. 1 …useful 21
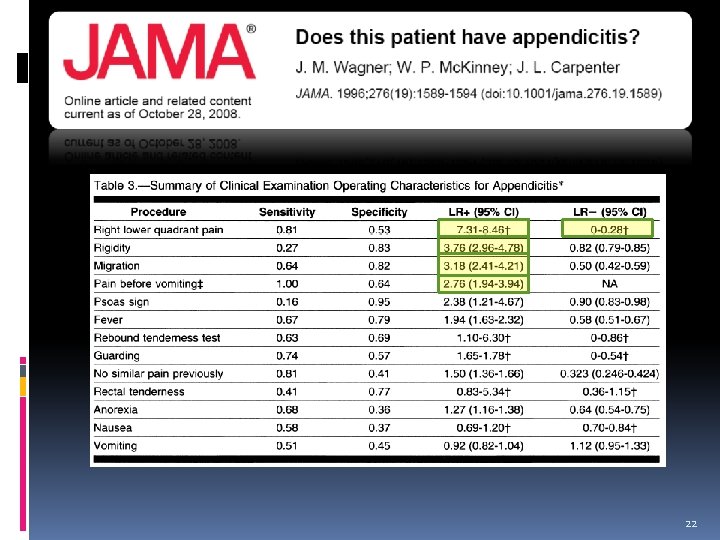
22

Case Resident comes down and sees the patient …hmm, didn’t do a rectal? Wow. hmmm…. 23

Appendicitis - Rectal Why do we do a rectal exam? Should we do a rectal exam? Looking for other diagnoses PR bleeding Peri-anal disease Mass in the vault Does everyone need a rectal? 24

Patients and Methods: 100 consecutive adults admitted to the emergency surgical unit with acute abdominal pain Following DRE, patients completed an anonymous questionnaire The house officer conducted the rectal examination at admission and also completed an evaluation sheet Results: A working diagnosis of acute appendicitis in 38 patients and gastroduodenal, pancreatobiliary pathology in 24 patients was made DRE did not alter clinical diagnosis or initial management in any patients Routine DRE did not detect any unrelated pathology 93 wanted to know why rectal examination was required 78 patients rated the DRE as uncomfortable 43 were willing for DRE as a routine 54 patients preferred to have the DRE at the time of other bowel tests rather than at emergency admission 25

Patients Results 1204 consecutive patients admitted to hospital with RLQ pain 1028 had a rectal examination on admission Main outcome measures - Odds ratio for each symptom and sign related to final diagnosis Results of multiple logistic regression analysis for acute appendicitis Right sided rectal tenderness (odds ratio 1. 34, p<005) RLQ tenderness (odds ratio 5. 09) Rebound tenderness (3. 34) Guarding (3. 07) Muscular rigidity in the abdomen (5. 03) In the logistic regression analysis of patients with acute appendicitis, when allowance was made for the presence or absence of rebound tenderness, rectal tenderness on the right lost its significance Six patients had masses palpable rectally, of which three were palpable on abdominal examination; the other three patients had acute appendicitis. No other unexpected diagnoses were established, and no useful additional Conclusion If patients presenting with pain in the RLQ of the abdomen are tested for rebound tenderness then rectal examination does not give any further diagnostic information 26

Case The resident agrees – this sure looks like appendicitis. But the boss would like some imaging. …thoughts? 27

Ultrasound (Graded Compression) Test Characteristics Sensitivity 75 -90%, Specificity 86 -100% Pros No radiation, safe in kids, pregnant pts Can identify alternate Dx esp. in female pts Cons Difficult for us to get Operator-dependant Limited in obese pts or with ↑ bowel gas Identifies alternate Dx less often than CT Painful

CT scan Test characteristics Sensitivity 90 -100%, specificity 91 -99% Pros Identifies alternate Dx more often than U/S Fast & accessible in our practice setting Cons Radiation dose (~100 CXR’s) Delay time to surgery Multiple techniques in literature: controversial as to which is best but all ~90 -100% sensitive Less accurate in pts w/ little intraabdominal fat

CT vs U/S 2 prospective RCT’s of U/S vs CT more sensitive & specific than U/S 94 -97% sensitive vs. 76 – 100% for U/S 100% specificity vs. 76 -90% for U/S More alternate Dx identified by CT Horton et al. Am J Surg 2000; 179: 379 -81 Walker et al. Am J Surg 2000; 180: 450 -55

CT vs U/S Methods: 120 consecutive pts 8 -81 yo w/ ? appy who were too well to go to OR but too ill to simply D/C Did focused CT w/ rectal contrast & U/S w/in 1 hr Gold standard - pathology or clinical f/u x 6 m Results: CT: 95% sensitive, 89% specific U/S: 87% sensitive, 74% specific CT identified 14 alternate Dx vs. 9 for U/S missed 2/3 of pts w/ perforation *Pickuth et al. Suspected acute appendicitis: Is ultrasonography or computed tomography the preferred imaging technique? Eur J Surg. 2000; 166: 315 -19

Does imaging change mgmt? 2 studies of CT in pts w/ ? appendicitis comparing Tx plan before & after access to results of scans Results: CT changed disposition in 27 – 59% of pts Prevented d/c of ~3% pts w/ appendicitis Prevented negative laparotomy in 3 -13% Alternate Dx in 11 -20% …yes Frank et al. Unenhanced helical CT scanning of the abdomen and pelvis changes disposition of patients presenting to the emergency department with possible acute appendicitis. J Emerg Med 2002; 23: 1 -7 Rao et al. Effect of computed tomography of the appendix on treatment of patients and use of hospital resources. N Eng J Med. 1998; 338: 141 -6

Bottom line Group 1 Appendectomy regardless of imaging result Group 2 Image Group 3 Clearly instructed when to return for re-evaluation 33

Appendicitis - Mgmt Hydration Antibiotics Ancef/Flagyl (surgical wound) Fluroquinalone/Flagyl (gram(-) rods / anaerobes) Surgery

Case 65 ♂ with ABD pain Diffuse ABD pain 8/10 Rapid onset Opiod resistant N/V/D Watery stools x 3 OE: 104 20 145/67 37. 2 ABD: Diffuse tenderness - no rebound/guard Rectal: Normal (-) FOB PMHx: HTN/DMII/smoke/AFIB/MI x 3 35
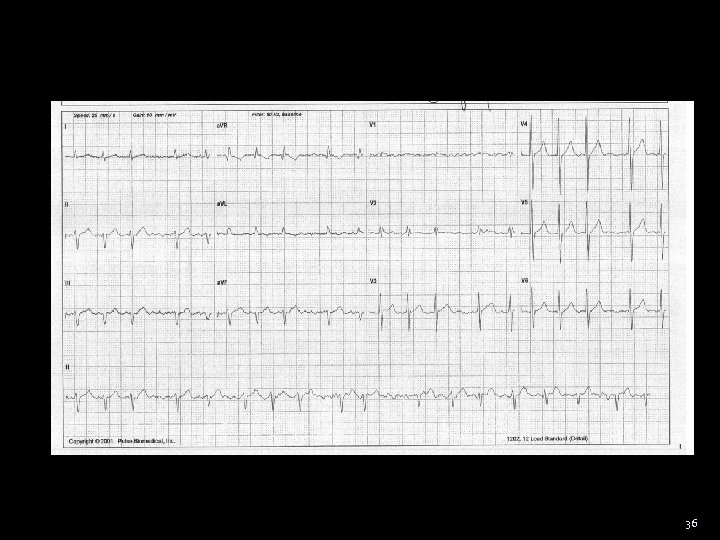
36

Approach Differential 37

Ischemic bowel - etiology Embolic LA LV Cardiac Valves SMA is most susceptible to embolism Multiple emboli Concomitant vasoconstriction occurs 38

Ischemic bowel - etiology Thrombotic Arterial Acute event Chronic intestinal ischemia from progressive atherosclerosis Involves multiple vessels Venous venous thrombosis →mesenteric venous flow → bowel wall edema, fluid efflux into lumen ↓BP ↑ blood viscosity Risk Factors Hypercoagulable states Portal hypertension Abdominal infections Blunt abdominal trauma Pancreatitis Splenectomy Malignancy in the portal region 39

Ischemic bowel - etiology Non-occlusive etiology systemic illness → systemic shock → ↓CO cocaine → vasospasm Venous thrombosis → ↓ venous return → interstitial swelling of bowel wall → ↓ arterial flow 40

Mesenteric Ischemia – clinical ABD pain rapid onset severe out of proportion to exam N/V/D forceful bowel evacuation Risk factors AFIB CHF peripheral vascular disease hypercoagulability 41

Ischemic bowel - diagnostics Labs (non-specific) Lactate WBC INR/PTT Imaging Plain films (nonspecific late findings – not useful) Thumbprinting Pneumatosis intestinalis Portal venous gas CT Angiography 42

CT scan sensitivity 64 -100% specificity 89 -94% Evidence of ischemia in bowel wall & mesentery Evidence of clot in SMA First investigation done routinely here If suspect mesenteric ischemia let radiology know Good but not good enough If CT is negative & high pre-test probability you need an angiogram

Ultrasound Doppler can determine major obstruction to flow in venous & arterial systems Dilated, tubular vessels with echogenic material (clot) Abnormal flow Limitations Studied primarily in venous thrombosis & chronic mesenteric ischemia Unsure how it performs for acute mesenteric ischemia Only good for more proximal blockages Has limitations inherent to all U/S exams

Angiography Gold standard (~90% sens) Diagnostic and therapeutic Infuse vasodilators into SMA (papaverine) Angioplasty Drawbacks Time-consuming Risks of contrast & invasive procedure Expensive

Angiography: Early vs Late Angiography → early in pts w/o peritonitis & ↑ suspicion Can buy time (papaverine) Can aid in surgical decision making Surgical: embolectomy, thrombectomy, endarterectomy, bypass graft Non-surgical: angioplasty Early (before peritonitis) angio & intervention ↓ mortality 70 -90% → 10% Down side: ↑ negative angios Associated risks & costs 46

Angiography: When to say no Contraindications: 1. Unstable hypotensive pts on vasopressors Difficult to differentiate b/w occlusive & nonocclusive etiologies Can’t infuse vasodilators 2. Pts w/ peritonitis Delays surgery

Case 32 ♀ with nausea and vomiting Abdominal pain periumbilical and crampy paroxysms of pain q 4 -5 min abdominal distension Vomiting q 30 min BM none x 48 h PMHx Crohns – dx in 1997 - resection 2002, 2007 48

Crohn’s Extra-intestinal manifestations Skin manifestations erythema nodosum, pyoderma gangrenosum Peripheral arthritis (asymmetric involvement of larger joints) Ankylosing spondylitis and sacroiliitis Aphthous ulcers Ocular manifestations (eg, episcleritis, recurrent iritis, uveitis) Amyloidosis and thromboembolic manifestations Liver elevation of enzyme levels Cholangitis Autoimmune chronic active hepatitis, and cirrhosis 49

Comparisons of Crohn's and UC Terminal ileum involved Colon involvement Rectum involvement Peri-anal disease Bile duct involvement Distribution of Disease Endoscopy Depth of inflammation Fistulae Stenosis Surgical cure Smoking Crohn's Ulcerative colitis Commonly sually Seldom Common No ↑ in PSC Patchy (Skip lesions) Deep geographic ulcers May be transmural Common Often risk for smokers Seldom Always Usually Seldom Higher rate Continuous ulcer Shallow, mucosal Seldom Cured by colectomy ↓risk for smokers 50

Complications of Crohn’s Perforation Fistula Adhesions - obstruction Deficiency / Malabsorption Protein Vitamins Abscess Megacolon Steroids 51

Abdominal Films What are they good for? Rule out Obstruction Perforation Foreign Body 52

Obstruction Small Bowel 1. Distended loops of bowel proximal to obstruction Intramural width > 3 cm 2. Multiple intra-luminal air fluid levels more distal obstruction → more gas-fluid levels 3. Discrepancy b/w bowel size proximal/distal to obstruction 4. Obstruction →→ Intramural gas 2 o to ischemia This is a late poor prognostic sign 53
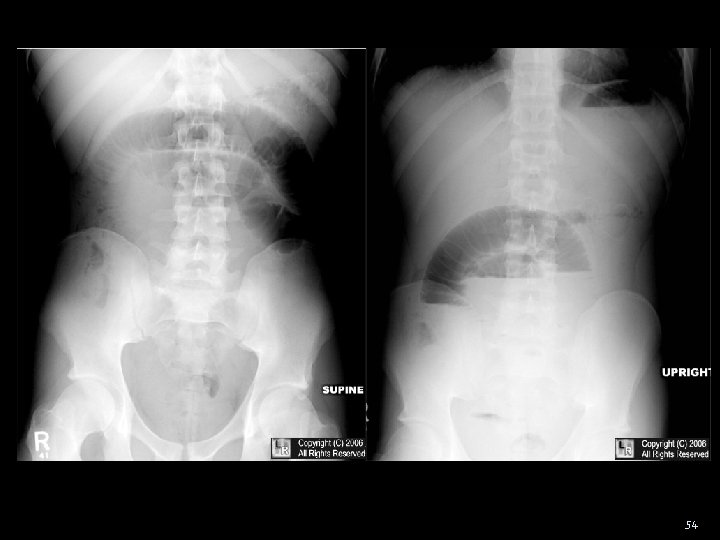
54
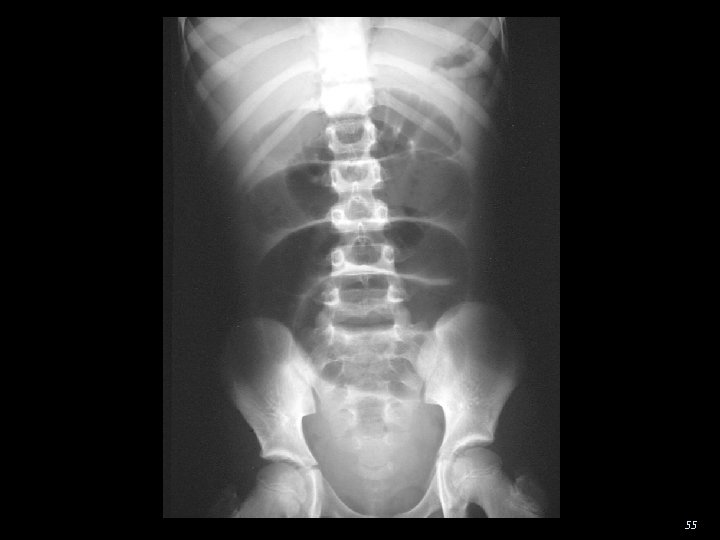
55
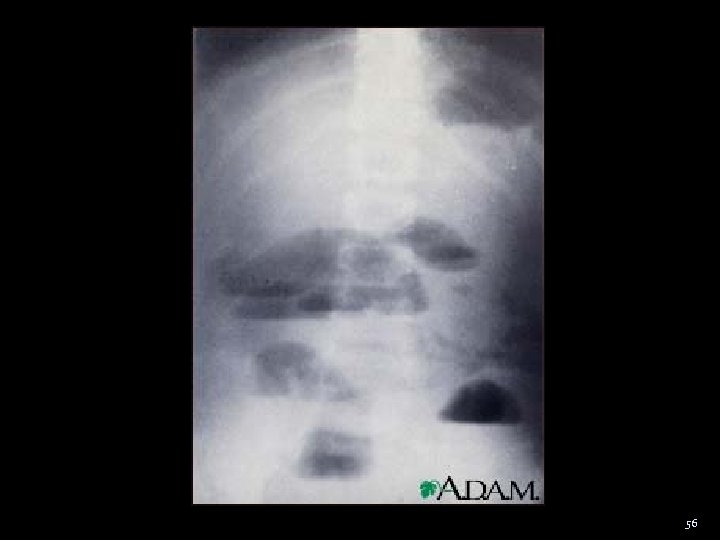
56
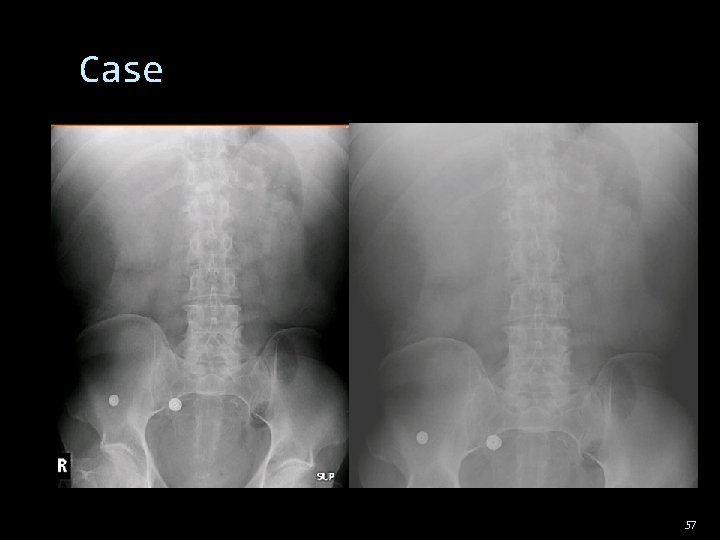
Case 57

MATERIALS AND METHODS. A blinded retrospective analysis was done on 78 pts who underwent plain abdominal radiography, CT, and enteroclysis to assess for suspected SBO. The findings at enteroclysis and the clinical outcomes were used as standards of reference. RESULTS Plain film radiography for SBO sens: 69% (44/64) specificity 57% (8/14). Overall accuracy of plain film radiography was 67% (52178). CT sensitivity 64% (41/64) and specificity 79% ( I 1/ 14) 58

Abdominal Films What are they good for? Rule out Obstruction Perforation Foreign Body Skip Films 59
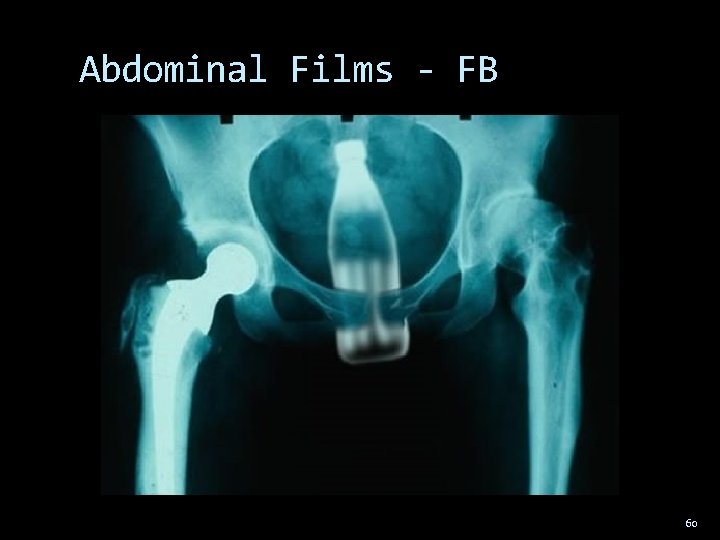
Abdominal Films - FB 60
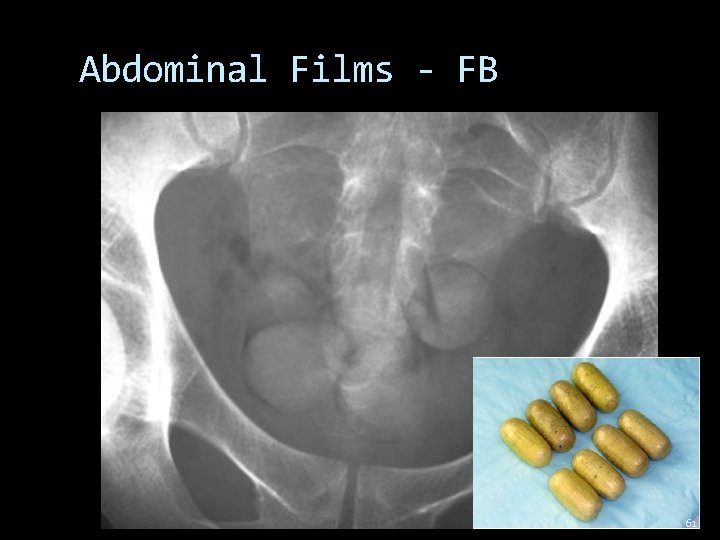
Abdominal Films - FB 61

Abdominal Films What are they good for? Rule out Obstruction Perforation Foreign Body Skip Films 62
63

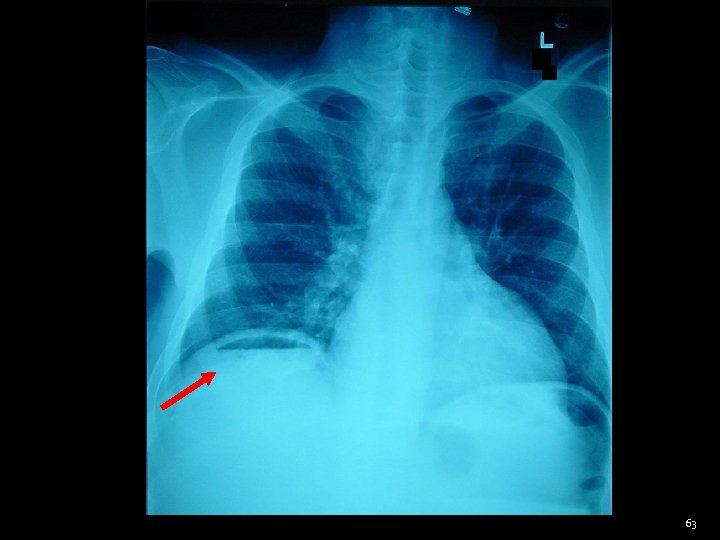
Crescent sign Air may be trapped anteriorly in the cupola of the diaphragm permitting visualisation of the undersurface of the central portion of the diaphragm 64
65

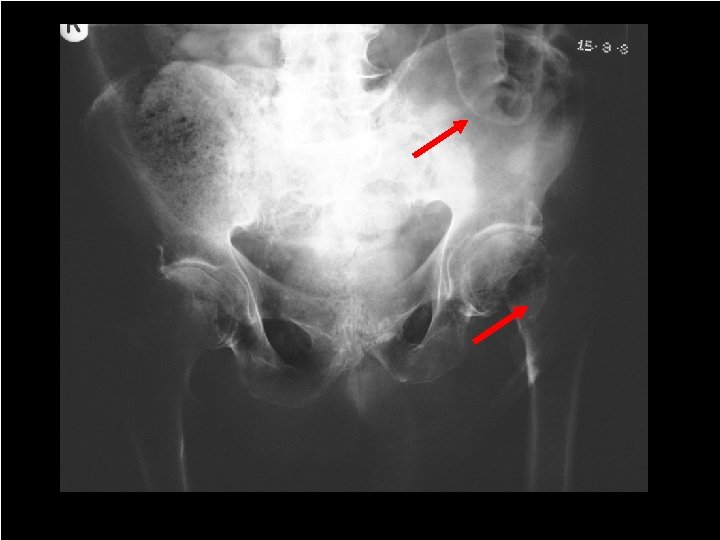
Rigler’s sign Double Wall sign Gas-relief sign Air is present on both sides of the intestine (usually requires > 1 L of free air) 66
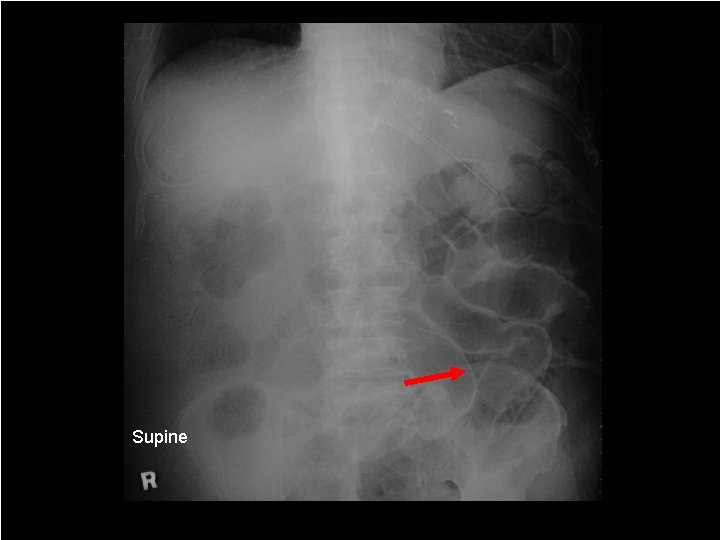
Supine 67
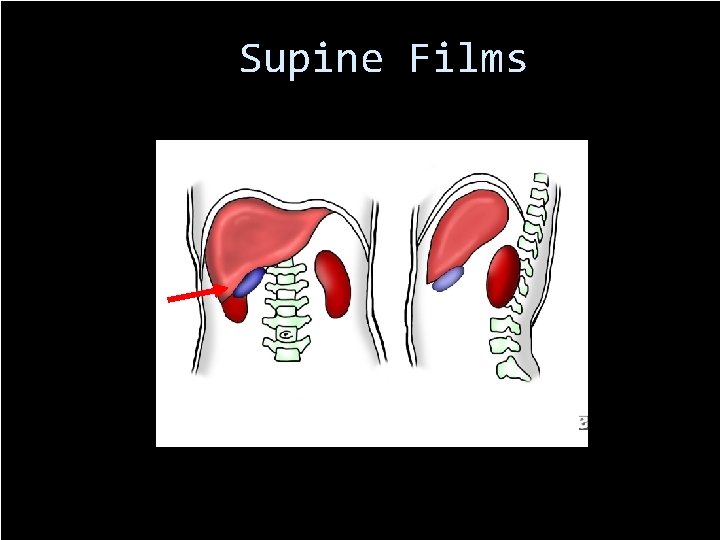
Supine Films 68
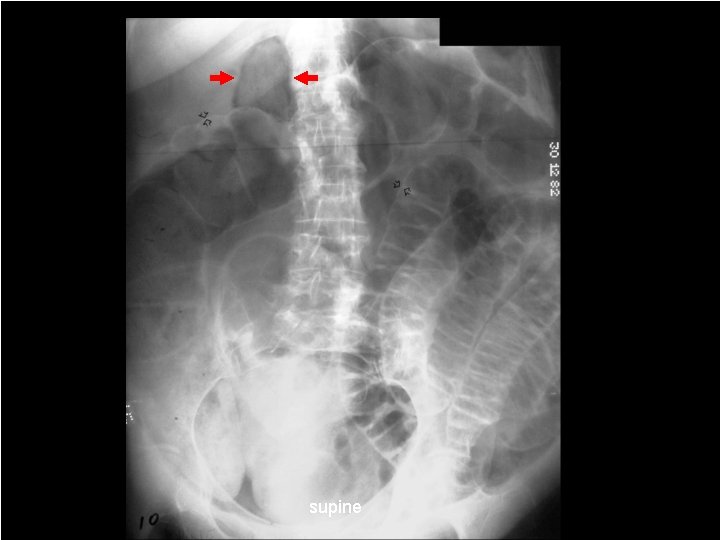
supine 69
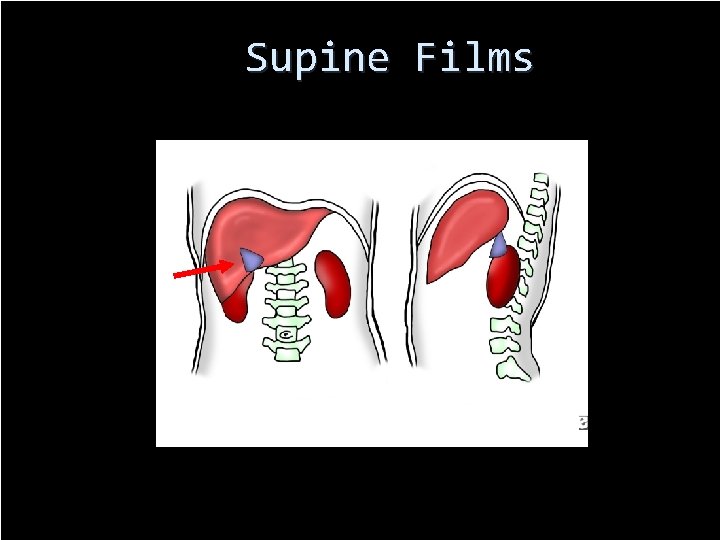
Supine Films 70
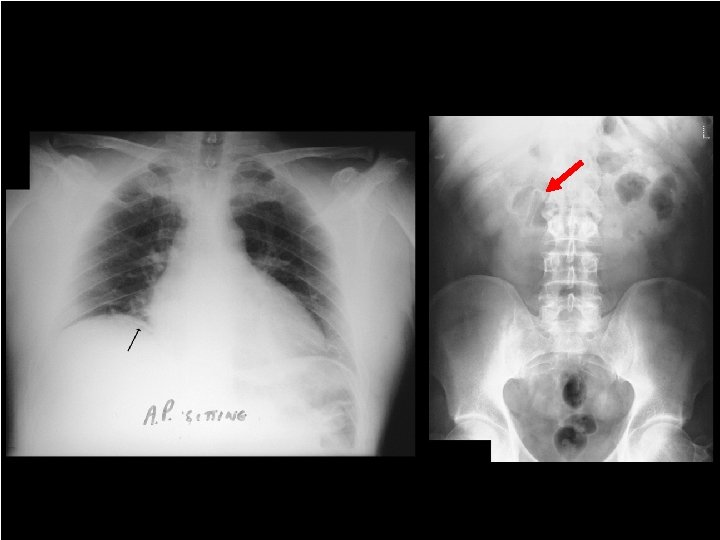
71

Supine Films Double Blind Retrospective Supine films from 44 cases of pneumoperitoneum were randomly interspersed among supine films from 87 control subjects without free air One or more of these signs were present (59%) Right-upper-quadrant gas sign (41%) Rigler's sign (32%) Falciform ligament and football signs (2%) 11 false-positive cases (13%)

SBO - case 32 ♀ with nausea and vomiting Abdominal pain periumbilical and crampy paroxysms of pain q 4 -5 min abdominal distension Vomiting q 30 min BM none x 48 h PMHx Crohns – dx in 1997 - resection 2002, 2007 73
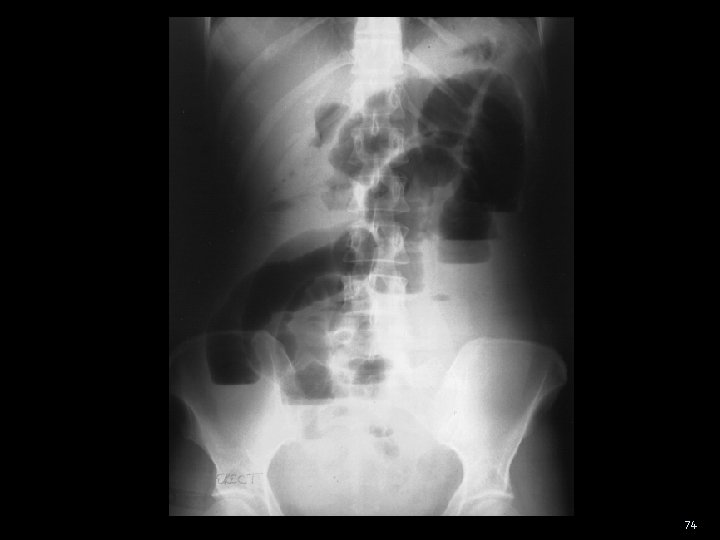
74

SBO - pathophysiology Swallowed air and gas from bacterial fermentation accumulates Bacterial overgrowth occurs in the proximal small bowel the contents of which are normally nearly sterile emesis can become feculent due to bacterial overgrowth The bowel wall becomes oedematous Normal absorptive function is lost Fluid is sequestered in the bowel lumen ↑ secretion of fluid into the lumen of the proximal bowel ↑ transudative loss of fluid into the peritoneal cavity Dehydration → tachycardia, oliguria, azotemia, and hypotension Emesis → loss of Na, K, H, and Cl 75

SBO - Treatment Degree of dehydration Need for surgery – timing of surgery Partial vs Complete “…never let the sun rise or set on a SBO!" IV access – fluid resuscitation Non-operative NG tube 76

Case 42 female presents with diarrhea PMHx Dental Surgery 2 weeks ago Recent travel to mountains ? questionable water Diarrhea Onset ~ 4 -5 days ago Large volume – watery Tried some immodium - ? helped a little No N/V ABD pain Diffuse generalized abdominal pain 77

Thoughts? Differential? Work-up? 78

C. difficile 1978 C. difficile identified as the causative pathogen Implicated Abx Clindamycin Penicillins Cephalosporins Any antibiotic can predispose to C. diff colonization Risk Factors Abx Broad spectrum Abx Multiple Abx Increased duration Advanced Age Gastric Acid Suppression Protective Factors Neonates 79

C. Difficile pathogenesis 80

C. Difficile - presentation Typical Watery diarrhea Onset durring Abx course or 10 -15 d post Abd cramping Fever (low grade) Leukocytosis OE: Abd tenderness Colonoscopy: patchy erythema → pseudomembranous colitis Atypical Protein losing enteropathy Involvement in IBD Extra colonic involvement

C. Difficile - treatment IV, O 2, Monitor Fluid resuscitation Discontinue antibiotics ∆ to less associated abx Infection control – contact precaution Avoid opiates / loperimide Metonidazole Vancomycin (PO) Probiotics Intermittent therapy 82
Case Pt is admitted under hospitalist (capped) You see the patient 3 handovers later Diarrhea has slowed Abd distension Altered sensorium OE: Vitals: 120 107/42 19 38. 1 Distended tender lower ABD No peritoneal signs
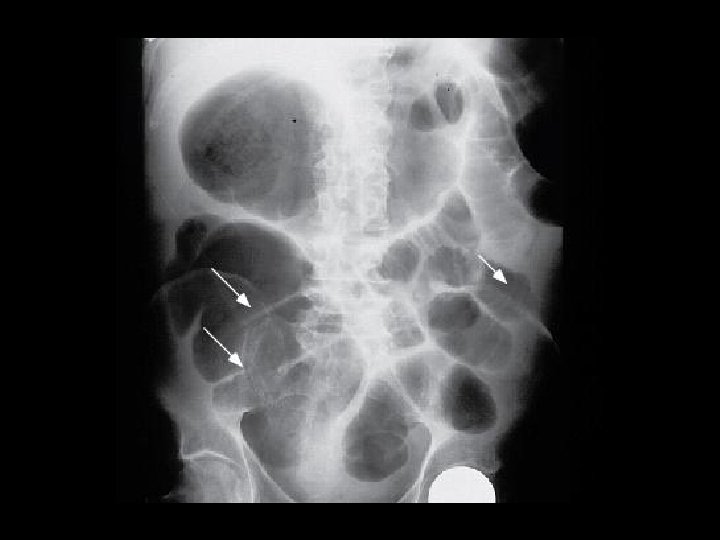

Toxic Megacolon - Diagnosis Radiographic dilation of colon (>6 cm) PLUS 3 of: Fever > 38 HR > 120 WBC > 10. 5 Anemia PLUS 1 of: Dehydration Altered Sensorium Hypotension Electrolyte disturbances

Toxic Megacolon – pathophysiology Nitric Oxide → generated by macrophages/inflamed smooth muscle → inhibitor of smooth muscle tone Inflammation Extension → paralyzes smooth muscle

Toxic Megacolon - Treatment Goals: Reduce colitis severity Restore colonic motility Decrease likelihood of perforation Medical Mgmt Bowel Rest / NG decompression D/C anti-motility agents Opiates, Anticholinergics Abx ? Steroids Surgical Mgmt Colectomy

Thank you! THE END

89

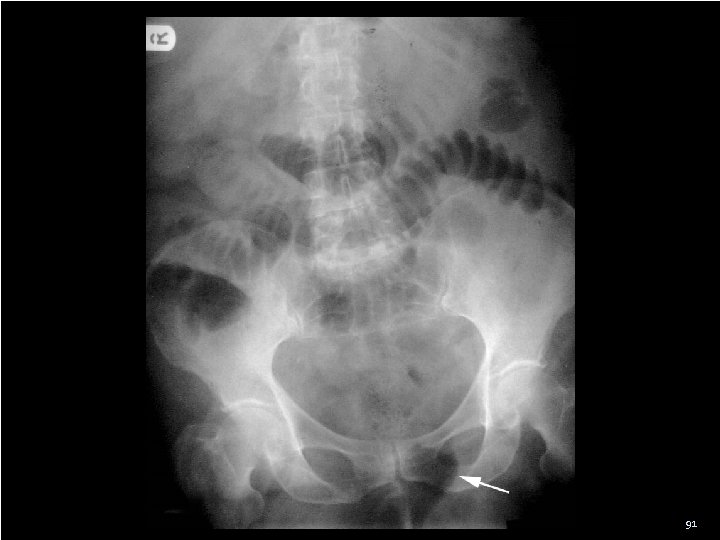
Incarcerated Hernia - Case 52 ♂ with pain, edema → scrotum nausea, vomiting, and low-grade fever …if you listen bowel sounds in the scrotal sac inguinal mass can be palpated separately from the testes 90
91

Incarcerated Hernia - Mgmt Trendelenburg posn with an ice to the groin Sedation Slow, gentle pressure to reduce the hernia If the hernia cannot be reduced or strangulation is suspected (fever, overlying cellulitis, peritonitis) fluid resuscitation broadspectrum Abx emergent surgical consultation 92

Hernia (non-incarcerated) Patients who have a hernia on routine exam or who have had the hernia reduced and are without symptoms of incarceration or strangulation Refer for out pt surgical repair 93

Hernia - Peds Fun Facts Inguinal hernias occur ~ 10 -20/1000 live births Prematurity and low birth weight ↑ risk ♂: ♀ 4: 1 → ↑ ♀ incarceration Most common indication for surgery < 2 yrs Presentation Abdominal or inguinal pain, an inguinal or scrotal mass, nausea, vomiting, and low grade fever Mgmt Attempt reduction if the child appears well Analgesia, sedation Trendelenburg position Slow gentle pressure 94

Diverticulitis - case 65 ♂ presents with bloating and LLQ pain Stool: ↓ freq no change in caliber/consistency OE: 37. 5 87 135/24 18 ABD: soft tender LLQ. No rebound/guard Rectal: FOB positive 95

Hb: 146 WBC: 10. 6 Urine: clean Bili/ALT/ALP/Lipase: N Imaging CT Barium Enema / Non-contrast Enema US Endoscopy Plain Films 96

CT scan: Evaluates the colon and surrounding structures Diagnose diverticulitis Evaluate the extent of the disease Peri-colonic fat Thickening of bowel wall > 4 mm Free air Abscess Guide perc drainage Our guy: Multiple diverticuli Local inflammation 97

Diverticulitis Colon is penetrated by vasa recta (vessels) Site of penetration is weak Diverticula form 2 o to ↑ itracolonic pressure Assymptomatic Obstructed → inflammation → microperf 98

Diverticulitis Uncomplicated Peri-colonic fat inflamation Complicated Fistula Abscess Adjacent obstruction → mass effect (abscess) → stricture 99

Diverticulitis – Mgmt uncomplicated Oral Abx x 7 -10 days* Septra DS BID and flagyl 500 mg q 6 h Cipro 500 mg BID and flagyl 500 mg q 6 h Amoxicillin/clavulanate 500/125 mg TID Diet Liquid High-fiber (↓ recurrence) Pain NSAIDs / opiods Admission Unable to tolerate PO Poor social support / compliance / Follow-up *Gilbert DN, Moellering RC Jr, Eliopoulos GM, Sande MA (eds): The Sanford Guide to Antimicrobial Therapy, 34 th ed. Hyde Park, Vt, Antimicrobial Therapy, Inc, 2004. 100

Diverticulitis – Mgmt Complicated IV Abx* Mild to Moderate Infection Ticarcillin/clavulanate 3. 1 gm IV q 6 h Ampicillin/sulbactam 3 g IV q 6 h Ciprofloxacin 400 mg IV q 6 h and flagyl 500 mg IV q 6 h Severe Infection Ampicillin, 2 g IV q 6 hr, and metronidazole, 500 mg IV q 6 hr, and gentamicin, 7 mg/kg q 24 hr, or ciprofloxacin, 400 mg IV q 12 hr Trovafloxacin, 300 mg IV once a day Imipenem, 500 mg IV q 6 hr NPO – bowel rest Surgical Mgmt Peritonitis Perforation Sepsis resistant to medical mgmt Fistula Strictures *Gilbert DN, Moellering RC Jr, Eliopoulos GM, Sande MA (eds): The Sanford Guide to Antimicrobial Therapy, 34 th ed. Hyde Park, Vt, Antimicrobial Therapy, Inc, 2004. 101

Pediatric Issues SMALL BOWELS

NEC - Case HPI: 10 day ♂ presents with feeding intolerance and bloody stools Mom also notes abdominal distension, lethargy the bedside nurse notes a decrease in the infant activity level and temperature instability PMHx: Ex-36 wk 3 days in SCN - uneventful Some ongoing difficulties with feeding / wt gain – formula fed OE: 160 60/42 50 35 o. C Decreased tone – slip through Mottled ABD: distended and tender 103
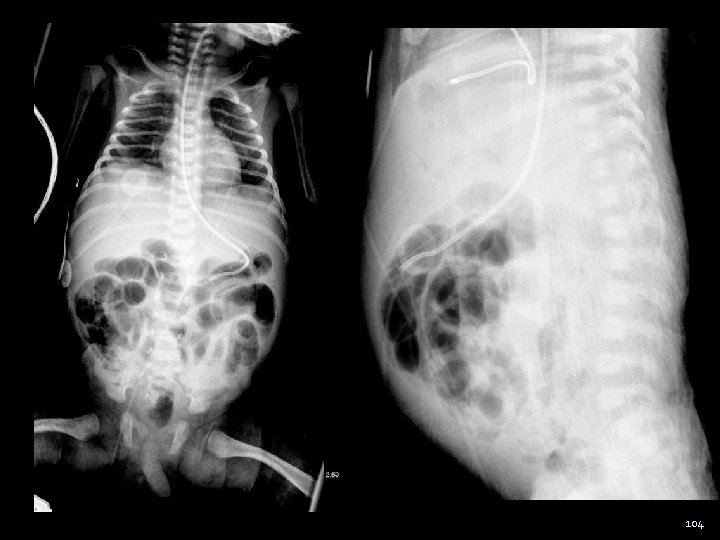
104
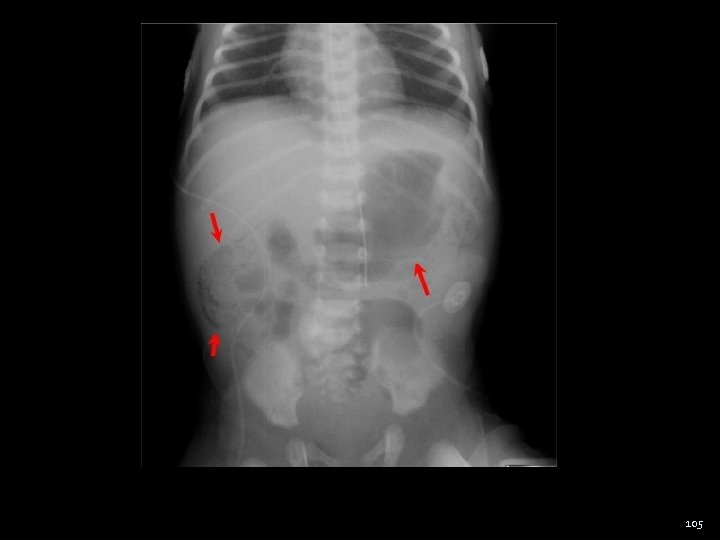
105

NEC Most common GI emergency in the neonates Acute fulminant dz associated with ulceration and necrosis of the distal small intestine and colon Pathophysiology – poorly understood Infectious – nursery epidemics Prematurity - ↓ after 36 wks Enteral alimentation- ↑ metabolic demand Inflamatory mediators - 106

NEC - Diagnosis Radiology Pneumatosis intestinalis Portal venous air Pneumoperitoneum Non-specific localized dilated loop of bowel thickened loops gasless abdomen Labs Thrombocytopenia Leukocytosis Electrolyte imbalance Metabolic acidosis Hypoxia or hypercapnia 107

NEC - Mgmt 1. Early bowel decompression by NG suction 2. Prompt IV Abx therapy Ampicillin Gentamycin Anaerobic bacterial coverage (clindamycin) Maintain volume/ mesenteric perfusion. 3. NEC is associated with third spacing of fluid into the mesentery Intra-vascular volume supplementation is required to maintain mesenteric perfusion Follow perfusion of the extremities and urine output (1 -2 ml/kg/hour) 4. Except in the milder cases, because of respiratory failure and worsening acidosis, intubation mechanical ventilation is often necessary 5. 6. 7. Pain control is essential → extremely painful disease Surgical consultation ICU consultation 108

Intussusception - case Hx: 13 month ♀ with profound lethargy A bit snot nosed last week but mom thought she was doing better Earlier today she was quite irritable and was noted to bring her legs up to her ABD PMHx - well OE: AVSS Afeb Child is lethargic ABD distended Diffuse poorly localized tenderness Not firm Rectal FOB (-) 109
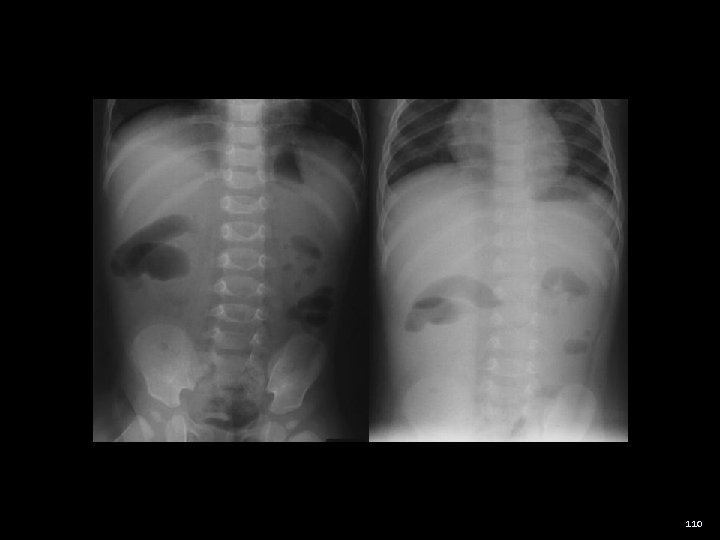
110
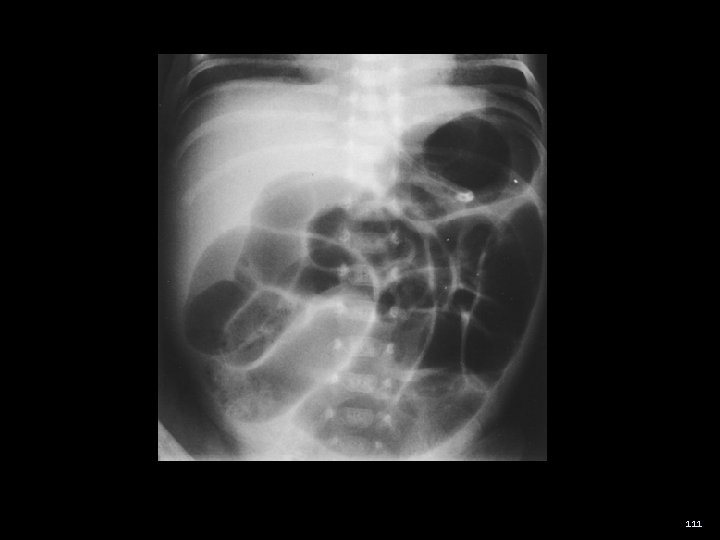
111
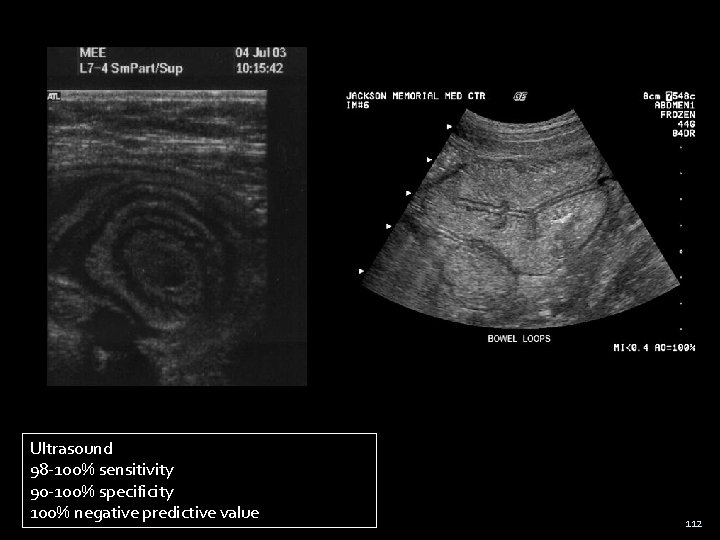
Ultrasound 98 -100% sensitivity 90 -100% specificity 100% negative predictive value 112

Intussusception lead point causes telescoping of one segment of intestine into another Edema develops and obstructs venous return Ischemia of the bowel wall peritoneal irritation → perforation 113

Intussusception - presentation Classic Triad (~30%) 1. Abdominal pain 2. Vomiting 3. Bloody stools Drawing the legs up to the abdomen Profound lethargy Dance’s Sign - a sausage-like mass in the RUQ and an empty space in the RLQ representing the displaced cecum 114

Intussusception - Mgmt IV fluids 20 m. L/kg NS bolus Repeat PRN NPO NG tube decompression Ill-appearing or febrile children → ABx 1. 2. 3. Ampicillin Gentamicin Clindamycin or metronidazole Air or hydrostatic barium enema Surgical intervention if… reduction is unsuccessful perforation occurs 115

WHAT CAN KILL THIS PATIENT?
60 ♂ with DM presenting with back pain 32 ♀ with RLQ pain 5 month ♀ with “colic” 117

118

Which pairing correctly matches the radiological finding with the cause of abdominal pain in infants? A. Volvulus: Double-bubble sign with associated dilatation and increased gas pattern distal to the volvulus B. NEC: Asymmetric pattern of gas with dilatation early in the course of illness and subsequent air in bowel wall (pneumatosis intestinalis) C. HPS: String and pearls sign is seen with a barium upper GI series D. Intussusception: Proximal colonic dilatation and distal narrowing in barium study 119

The most common GI emergency in the neonatal period is necrotizing enterocolitis. A. True B. False 120

Diffuse abdominal pain occurs in all of the following except: A. sickle cell crisis. B. inflammatory bowel disease. C. inguinal hernia. D. diabetic ketoacidosis. 121

Which of the following statements is true regarding intussusception? A. The condition is more common in females. B. It is the most common cause of intestinal obstruction in children younger than 2 years. C. Most commonly, the intussusception is ileoileal. D. Plain films are reliable in diagnosis. 122

Which of the following statements is true of hernias in children? A. Prematurity and low birth weight increase the risk. B. They are more common on the left side. C. They occur more in females. D. Males incarcerate more often. 123

Which of the following is/are non-abdominal cause(s) of abdominal pain? A. Lead poisoning B. Black widow spider bite C. Diabetic ketoacidosis D. Sickle cell pain crisis E. All of the above 124
- Slides: 124