Managing Slow Weight Gain in the Breastfed Infant

Managing Slow Weight Gain in the Breastfed Infant Assessment & Management Strategies Elaine Webber DNP, PPCNP-BC, IBCLC

Weight Gain Concerns Approached in orderly diagnostic process ◦ ◦ Complete history and PE Details of feeding Observation of feeding Appropriate labs Data organization Will help identify factors that appear under maternal and infant cases separately

Failure to Thrive (as defined by Ruth Lawrence) Weight loss after 10 days Birth weight not regained by three weeks Rate of weight gain below 10 th% beyond one month of age

Slow Weight Gain Weight gain slow but consistent Weight, length and HC proportional Developmental milestones normal

Differentiating Slow Weight Gain and Failure to thrive Infant who is slow to gain weight Alert Good muscle tone At least six wet diapers/day Pale, dilute urine Stools frequent, seedy (or if infrequent, large and soft) Eight or more nursings/day of active feeds Weight gain consistent by slow Infant with failure to thrive Apathetic or crying Poor tone Poor turgor Few wet diapers “Strong” urine odor Stools infrequent, scanty Fewer than eight feedings, often brief No evidence of milk-ejection reflex (no swallowing noted) Weight erratic, may be losing weight

Normal Growth Initial weight loss ◦ Normal 7 -10% of birth weight ◦ What might impact excessive weight loss? Expected weight gain ◦ “Normal” daily weight gain? ◦ Regain birth weight by 2 -3 weeks

Is there really a problem? Differences in growth charts ◦ Breastfed infants grow more rapidly first 2 months of life ◦ Less rapidly from 3 -12 months Weight gain only one parameter ◦ Length and HC also important Familial considerations
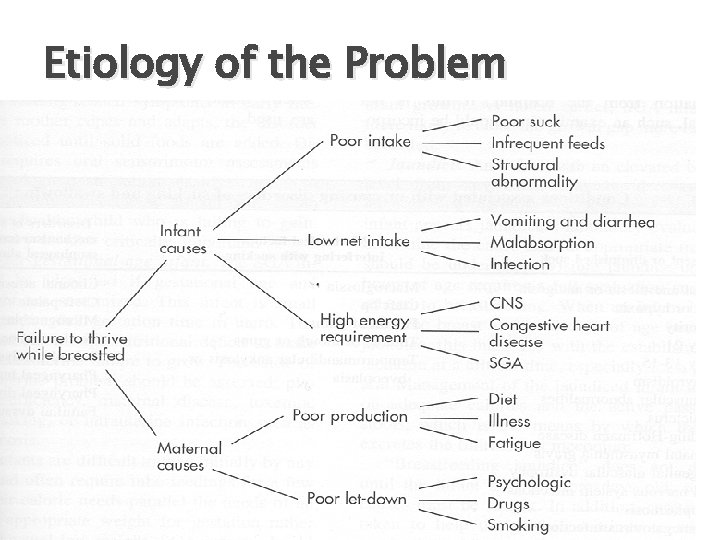
Etiology of the Problem

Evaluation of the Infant Underlying physical problems ◦ Metabolic conditions ◦ Congestive Heart Failure ◦ Cystic fibrosis Mechanical Abnormalities of the Mouth ◦ ◦ Ankyloglossia Short tongue Bubble palate Tight jaw

Evaluation of Infant (cont. ) Neurologic ◦ ability to root, suck and coordinate swallows Acute infections ◦ Septic, GI issues Chronic fetal infections ◦ CMV, HIV, Toxoplasmosis, etc. High energy requirements ◦ Some CNS disorders, fetal exposure to stimulants, stimulants transferred in breast milk,

Conditions associated with or causing disorders of sucking and swallowing Absent or diminished suck Maternal anesthesia or analgesia Anoxia or hypoxia High bilirubin Prematurity Trisomy 21 Hypothyroidism Neuromuscular abnormality ◦ ◦ Mechanical factors interfering with sucking Disorders of swallowing Macroglossia Choanal atresia Cleft lip Cleft palate Fusion of gums Micrognathia Tumors of mouth or gums Ankylossia (tongue or labial) Post-intubation dysphagia Pharyngeal tumors Familial dysautonomia Werdnig-Hoffmann Muscular dystrophy Central nervous system infections ◦ ◦ ◦ Toxoplamosis CMV Meningitis Adapted from Lawrence & Lawrence (2005)

Muscle Tone – a continuum When does it become “abnormal”? Hypotonia Normal Tone Slightly hypotonic infants may demonstrate: Weak Suck Poor lip closure Frequent slipping off the breast Hypertonia Slightly hypertonic infants may demonstrate: Extended posture Excessive irritability Strong bite reflex Note that some infants show “soft signs” or very mild indications of either hypo or hyper tone. These infants are often missed because they appear more “normal” than “abnormal”. Tone should always be assessed with any feeding difficulty.

Physiology of Milk Production

Prolactin Causes milk production Circadian rhythm Can be increased by emotional and physical stress Inhibited by dopamine, nicotine and alcohol Pharmacologic stimulation Prolactin levels

Oxytocin Released from the posterior pituitary Immediate reaction to nipple stimulation Causes contraction of smooth muscle epithelial cells surrounding the mammary alveoli Largely influenced by psychological factors Pharmacologic stimulation?

Lactogenic effects of Prolactin Modulated by the complex interplay of many hormones System which requires significant exploration when faced with a an unknown cause of poor milk production

Endocrine vs. Autocrine Control Initial milk production governed by prolactin production, activation of prolactin receptors and oxytocin release Eventually prolactin levels decline and milk production is governed by milk removal Early stimulation and milk removal are essential in the establishment and continuation of a robust milk supply
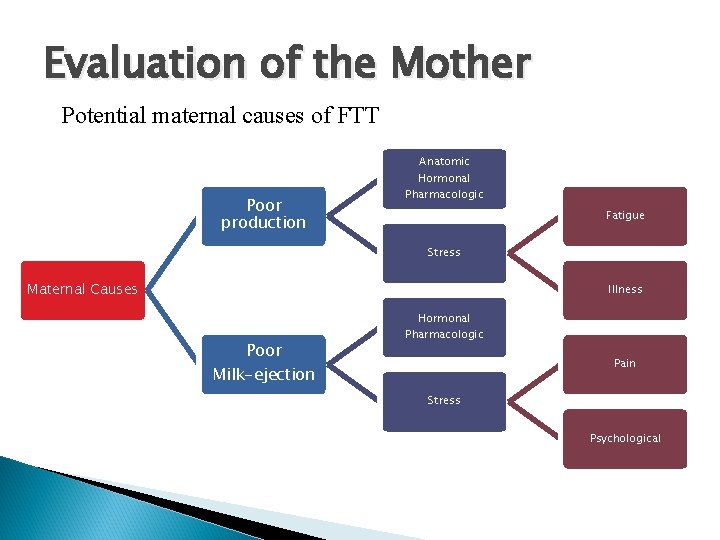
Evaluation of the Mother Potential maternal causes of FTT Poor production Anatomic Hormonal Pharmacologic Fatigue Stress Maternal Causes Illness Poor Hormonal Pharmacologic Pain Milk-ejection Stress Psychological

Maternal Health History Endocrine History ◦ Difficulty conceiving ◦ Thyroid problems ◦ Pituitary problems ◦ PCOS Previous Breast Surgery Prenatal History ◦ Breast changes during pregnancy ◦ Leaking colostrum

Maternal Health History (cont. ) Delivery ◦ Length of labor ◦ Drugs during labor ◦ Epidural ◦ Delivery of Placental fragments ◦ Excessive bleeding/hemorrhage Sheehan’s syndrome

Maternal Health History (cont. ) Postpartum ◦ Stress and exhaustion ◦ Maternal illness ◦ Maternal medications

Lesser known causes of Maternal Low Milk Supply (Pre)Diabetes Mammary Hypoplasia PCOS

Maternal Physical Exam Breast inspection Assessment of nipple and areola Scars

Nipple and Areola Firm, fibrous breast tissue ◦ nipple and areolar compressibility Nipple protractility ◦ Flat ◦ Dimpled ◦ Inverted
Breast and Nipple Anatomy Breast Turgor Large Nipples Flat/Fibrous Nipples Inverted/dimpled Nipples

Putting It All Together Management of FTT or slow Weight Gain ◦ Complex cause-and-effect relationship ◦ Direct attention to both mother and baby There is NO substitute for direct observation of the breastfeeding couplet

Maternal Factors Inadequate Milk Production ◦ Breastfeeding Mismanagement Positioning Frequency/duration of feeds Engorgement Use of nipple shields Complimentary/supplemental feeds

Identify and treat (if possible) hormonal causes Measuring Prolactin ◦ Varies based on stage of lactation ◦ Draw baseline (prior to a feed), then 45 minutes after nursing or pumping to measure the surge ◦ In early months; should at least double ◦ If cost an issue – baseline is more important Adapted from Lawrence & Lawrence 2005.

Identify and treat (if possible) hormonal causes PCOS ◦ ◦ Metformin – Informal feedback- variable impact on milk production Dosages vary (500 mg-2500 mg daily) Goat’s Rue Hypothyroid ◦ Be alert for “low normal” TSH and T 3 ◦ Has been correlated with low milk production ◦ Low thyroid during pregnancy should always be rechecked after delivery (2 weeks, 4 -5 weeks)

Inadequate Milk Production Secondary Factors (Physiologic/psycho-emotional) ◦ Maternal Illness/fatigue/diet ◦ Mental illness (PP depression) ◦ Emotional disturbances ◦ Impaired maternal-infant attachment

Maternal Factors Impaired Milk Ejection reflex ◦ Primary factors (pituitary disease, surgery) ◦ Secondary factors (pain, smoking, alcohol, meds) Milk Composition ◦ Vegan diet ◦ Extreme maternal malnourishment (can also lead to decreased milk production) ◦ Low fat content of milk

Infant Factors Inappropriate Suckling Response ◦ Identify problem Tongue tie ◦ Identify provider who will clip NP, ENT, Dentist, etc.

Identify milk transfer issues Uncoordinated suck swallow Active feeding

Basic Management Strategies Diagnose the problem (methodical) ◦ Remember interplay of various conditions ◦ Various problems can lead to same effect Don’t make assumptions Evaluate Mom and baby and OBSERVE THE FEEDING!

After determining possible causes: Support/improve mom’s milk supply Increase intake for the baby When to follow up? When to refer?

Important Tools Accurate Electronic Scale Supplemental Nursing System or other tube feeding devises Cup/syringe feeds Nipple Shields Piston Action Electric Breastpump

To improve milk production: Galactagogues: ◦ Metaclopromide ◦ Domperidone ◦ Goat’s rue ◦ Fenugreek ◦ Brewers Yeast ◦ Homeopathics

To improve milk production: Improve Milk Removal ◦ Correct latch ◦ Correct suck ◦ frequency and/or length of time nursing ◦ Discontinue pacifiers

Disorganized Suck Leads to milk removal, then supply Stategies ◦ Improve latch ◦ Finger feed (suck training) ◦ SNS ◦ Referrals

Finger Feed with Syringe

Poor Milk Supply Improve Milk Removal ◦ Correct suck ◦ length of time nursing ◦ Correct latch

Assessing Latch Deep latch Shallow latch

Poor Milk Supply Labs ◦ Thyroid ◦ Prolactin Term pregnancy 200 -500 ng/ml During lactation: 1 st 10 days up to 500 10 -90 days ranges from 60 -110

Galactagogues Metaclopromide (rx required) ◦ 10 mg TID 7 -10 days Fenugreek Brewers Yeast Homeopathics ◦ Lactuca Virosa ◦ Alfalfa Tablets

Important Tools - Review Accurate Electronic Scale Supplemental Nursing System Nipple Shields Piston Action Electric Breastpump

Babyweigh Scale

Nipple Shields/Breast Shells

Expressing Milk

Pumping Ask what kind of breastpump After every nursing session 8 -10 x daily if not nursing Night-time pumping very important


Impaired MER Psychological approach Artificial oxytocin

Increasing Overall Intake Get rid of the pacifier!!! Switch nursing ◦ Takes advantage of MER Bring baby into bed throughout the day

Increasing Caloric Intake at Breast Frequent feeds One sided feeds ◦ fat content of milk Lengthy active feeds Pump first to elicit MER Maternal diet

Monitoring Progress Scale rental for home use Expectation for weight gain Weight checks (don’t wait too long) ◦ daily, q other day, weekly Phone contact and encouragement

Good Office Resources Making More Milk : Diane West & Lisa Marasco Breastfeeding: A Guide for the Medical Profession : Ruth Lawrence Breastfeeding management for the Clinician: Marcia Walker Medications and Mother’s Milk : Thomas Hale
- Slides: 55