Managing Gestational Diabetes Cynthia V Brown RN MN

Managing Gestational Diabetes Cynthia V. Brown, RN, MN, ANP, CDE Southeastern Endocrine & Diabetes

Managing Gestational Diabetes • The management of gestational diabetes is necessary for a healthy baby and mom. • Managing this disorder well is a….

Richard Shafer: …CHALLENGE!!!

Definitions Gestational Diabetes Pre-gestational Diabetes

Gestational diabetes. . . • May have its’ onset or be first recognized during pregnancy • Diabetes may have previously existed but not diagnosed

Pre-gestational diabetes. . . • May be present and undiagnosed • Evolving • Already present and under treatment

Why is this important? • Pre-existing diabetes at conception can lead to congenital anomalies • Gestational diabetes leads to macrosomia and premature delivery

Congenital Malformations • Cardiovascular: transposition, vsd, asd, hypoplastic left ventricle, anomalies of the aorta • CNS: anencephaly, encephalocele, meningomyelocele, microcephaly

Malformations. . . • Skeletal: caudal regression, spina bifida • GU: Potter syndrome, polycystic kidneys • GI: tracheoesophageal fistula, bowel atresia, imperforate anus
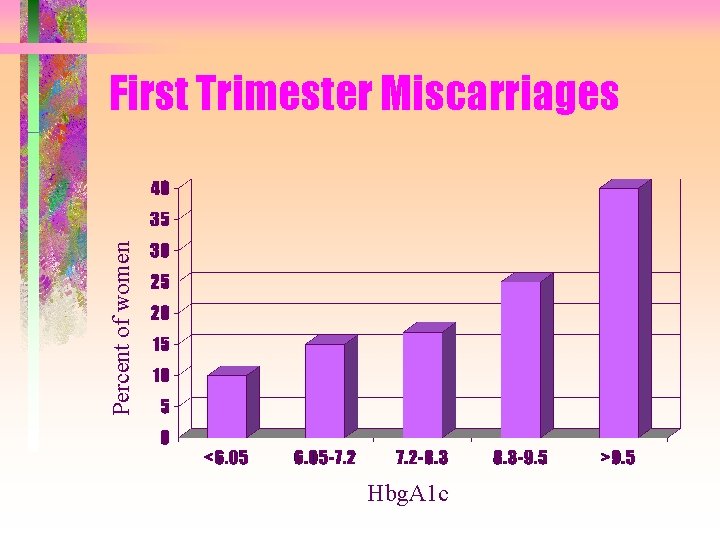
Percent of women First Trimester Miscarriages Hbg. A 1 c

Complications by Trimester • First – Still births – Miscarriages – Congenital defects • Second and Third – Hyperinsulinism – Macrosomia – Delayed lung development

Complications. . . • Delivery – Injuries – RD – Pregnancy loss – Neonatal hypoglycemia

Hormonal Influences

Decreased glucose levels • Due to passive diffusion to fetus • Causes hypoglycemia, even in non-diabetic patients • Greatly decreases insulin need in first trimester

Accelerated starvation. . . • Due to glucose diffusion • Leads to elevated ketone production • Unsure if this hurts baby or not • Use as guide for increased calories

Decreased maternal alanine • Gluconeogenic amino acid • Results in further lowering of FBS

Counterregulatory hormones • Suppressed responses to hypoglycemia • Study found BS as low as 44 did not elicit a response • Level at which glucose & GH released 5 -10 mg/dl lower in pregnant women with Type 1 DM • Hypoglycemia aggravated by lower intake due to AM sickness

Prolonged hyperglycemia • Enhances transplacental delivery of glucose to fetus • Resistance to insulin x 5 -6 hours PC • Resistance related to several anti-insulin hormones • Results in hyperglycemia

Hormones affecting blood sugar • • Insulin Glucagon Epinephrine Steroids Growth hormone Progesterone Human placental lactogen
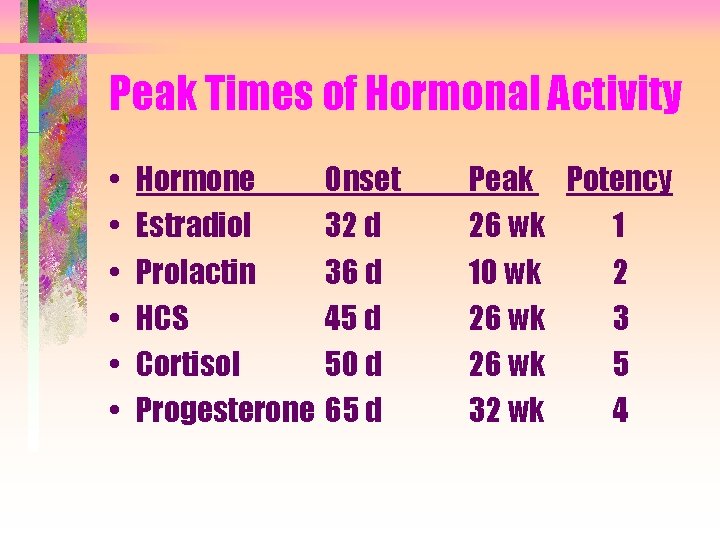
Peak Times of Hormonal Activity • • • Hormone Estradiol Prolactin HCS Cortisol Progesterone Onset 32 d 36 d 45 d 50 d 65 d Peak Potency 26 wk 1 10 wk 2 26 wk 3 26 wk 5 32 wk 4

Risk Factors • • Over 25 years of age Family history of Type 2 diabetes Obesity Prior unexplained miscarriages or stillbirths • History GDM or baby >10 pounds • PCOS

Dietary Modifications • • Decrease carbohydrate content Frequent small feedings Small breakfast meals Bedtime snacks No > 10 hours overnight fast NO JUICE Adequate calorie intake

Blood Sugar Goals • • • Fasting: Premeal: One-hour post-prandial: Two-hour post-prandial: 2 AM-6 AM: < 90 mg/dl 60 -90 mg/dl <120 mg/dl 60 -90 mg/dl

Estimated insulin needs • • • Prepregnancy Weeks 2 -16 Weeks 16 -26 Weeks 26 -36 Weeks 36 -40 Postpartum 0. 6 U/kg 0. 7 U/kg 0. 8 U/kg 0. 9 U/kg 1. 0 U/kg <0. 6 U/kg

When to Start Medications • Allow 1 week of dietary changes • Continue with diet if BS in target • First week with 2 elevated sugars, insulin starts • Frequent testing so as not to miss elevation • Anticipate need increasing • Do not be afraid!

Medications • Sulfonylureas: – Glyburide typically used – Anecdotal evidence – Not very effective – Unable to achieve higher insulin levels for meals – No long-term studies for safety

Medications • Insulin: – NPH: • • BID dosing Can start only at HS if FBS elevated Long history of safety Inconsistent absorption

Medications • Lantus: – 24 hour coverage – Sometimes hard to affect dawn rise without nocturnal low BS – Does not rise to meet meal-time rise of BS

Medications • Insulin analogs: – Humalog, Novolog, Apidra – Very rapid acting – Very effective pre- and post prandial – Less risk of hypoglycemia

Medications • Regular insulin: – Slower onset – Longer duration – May be necessary in those who do not want to take as many injections

Insulin Dosing During Labor • Need decreases dramatically • BS must be perfect in 72 hours prior to delivery • May not need insulin during labor • Type 1 needs only basal insulin with PRN supplementation

Postpartum • • Continue periodic testing Aim to lose weight Glucose challenge @ 6 wk check Breast-feeding lowers BS, leads to hypoglycemia

Managing Gestational Diabetes THANK YOU! Cynthia V. Brown, RN, MN, ANP, CDE Southeastern Endocrine & Diabetes
- Slides: 33