Management outcome of adhesive small bowel obstruction in
![Management outcome of adhesive small bowel obstruction in children [Role of conservative management] NABIL Management outcome of adhesive small bowel obstruction in children [Role of conservative management] NABIL](https://slidetodoc.com/presentation_image_h2/fd30358ab91ecd5bcd1a457c20d1ecbf/image-1.jpg)
Management outcome of adhesive small bowel obstruction in children [Role of conservative management] NABIL YOUSEF ABOU ELDAHAB SURGARY DEPARTMENT, SOHAG FACULTY MEDICINE, SOHAG UNIVERSITY

Introduction • Adhesions following abdominal and pelvic surgery is important in view of their morbidity and frequent hospital admission. • In children, acute adhesive intestinal obstruction is the most common reason for emergency admission re-admission.

Introduction • Adhesive small bowel obstruction after laparotomy is not uncommon. • In children, the adhesive obstruction usually occurred after major surgery e. g. [peritonitis, intestinal obstruction and obstructed hernia ]. But it may occur after minor surgery e. g. [appendicectomy and pyleromyotomy]. • Though the diagnosis can be made easily, the role of conservative management in children is controversial.

Aim of the work • Evaluation of different modalities of management including conservative, laparoscopy and open surgery. • We highlight some predictive factors of conservative management that affect the outcome in children with Adhesive small bowel obstruction.

Patients and methods: • Seventy child presented with adhesive small bowel obstruction were admitted to surgery and emergency department of Sohag faculty of medicine from March 1998 to March 2005. • The age ranged from one month to 12 years.

Patients and methods • Analysis of the patients was done as regard to the age at presentation, type of primary disease for which original laparotomy was done, time between primary surgery and time of presentation, frequency of attacks of bowel obstruction, frequency of previous laparotomy, clinical examination and radiological studies. .

Patients and methods • A comparative study was performed between outcome of different methods of management [conservative, laparoscopy and laparotomy]. • We highlight some predictive factors of success of conservative management.

Protocol of conservative management: • Duration: 2 - 7 days. • 1 - N. P. O. , intravenous fluids and prophylactic antibiotics. • 2 - Nasogastric tube for decompression and suction / 6 hours. • 3 - Rectal tube application if associated distended loop of colon filled with gases. • 4 - Record vital signs and nasogastric tube contents /6 hours. • 5 -X ray abdomen and pelvis erect, supine poster anterior view/6 hours. • 6 -Evaluation of the patients clinically and radiologically /12 hours

1. Cases are classified into 3 groups according to radiological and clinical data: 2. Group [1]. [Early small bowel obstruction]. 3. Group [2]: [Late small bowel obstruction]. 4. Group [3] [Early large and small bowel obstruction].

Results
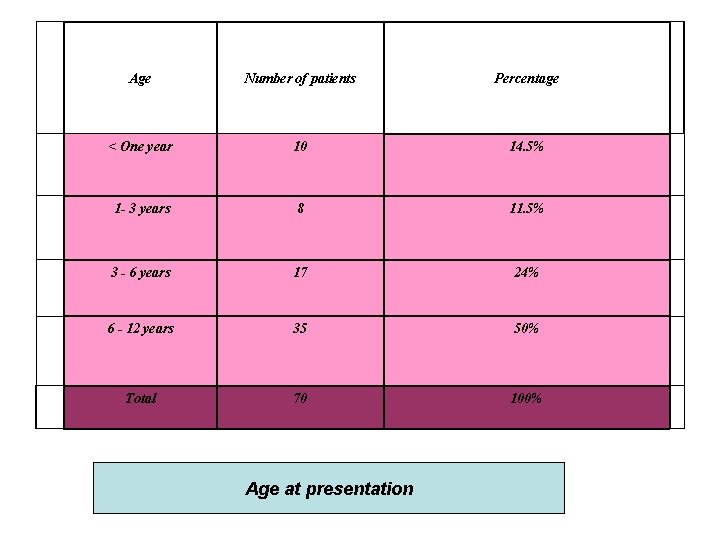
Age Number of patients Percentage < One year 10 14. 5% 1 - 3 years 8 11. 5% 3 - 6 years 17 24% 6 - 12 years 35 50% Total 70 100% Age at presentation
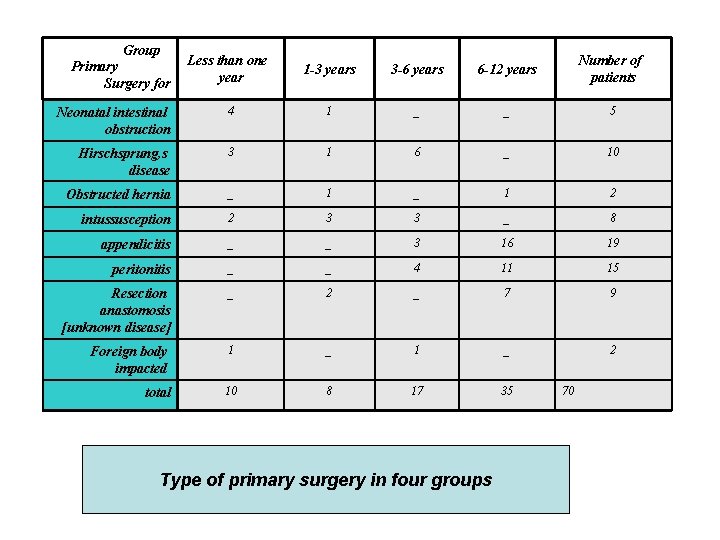
Group Less than one year 1 -3 years 3 -6 years 6 -12 years Number of patients Neonatal intestinal obstruction 4 1 _ _ 5 Hirschsprung, s disease 3 1 6 _ 10 Obstructed hernia _ 1 2 intussusception 2 3 3 _ 8 appendicitis _ _ 3 16 19 peritonitis _ _ 4 11 15 Resection anastomosis [unknown disease] _ 2 _ 7 9 Foreign body impacted 1 _ 2 total 10 8 17 35 Primary Surgery for Type of primary surgery in four groups 70
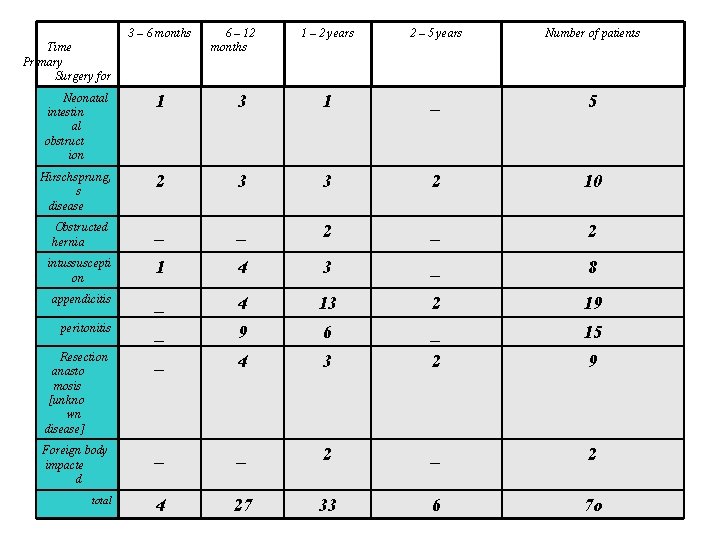
3 – 6 months Time Primary Surgery for 6 – 12 months 1 – 2 years 2 – 5 years Number of patients Neonatal intestin al obstruct ion 1 3 1 _ 5 Hirschsprung, s disease 2 3 3 2 10 Obstructed hernia _ _ 2 intussuscepti on 1 4 3 _ 8 appendicitis _ 4 13 2 19 peritonitis _ 9 6 _ 15 Resection anasto mosis [unkno wn disease] _ 4 3 2 9 Foreign body impacte d _ _ 2 total 4 27 33 6 7 o
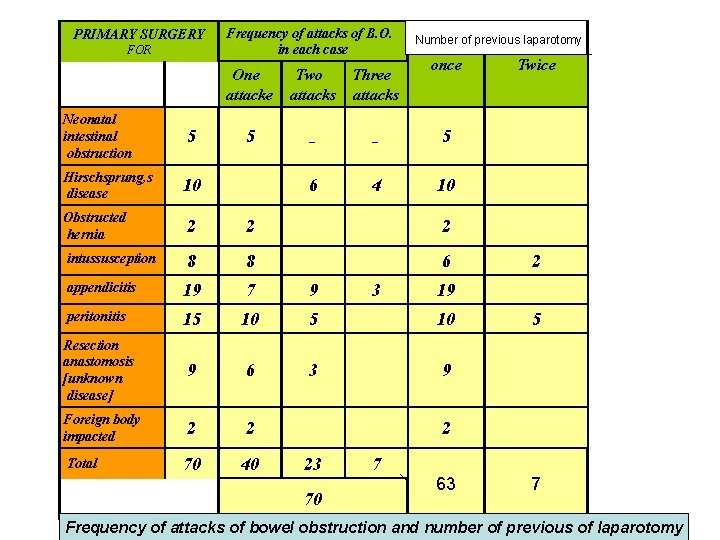
PRIMARY SURGERY FOR Neonatal intestinal obstruction Hirschsprung, s disease 5 Frequency of attacks of B. O. in each case Number of previous laparotomy once One attacke Two attacks Three attacks 5 _ _ 5 6 4 10 10 Obstructed hernia 2 2 2 intussusception 8 8 6 appendicitis 19 7 9 peritonitis 15 10 Resection anastomosis [unknown disease] 9 6 3 9 Foreign body impacted 2 2 70 40 Total 3 Twice 2 19 5 2 23 70 7 63 7 Frequency of attacks of bowel obstruction and number of previous of laparotomy
![management • Group (1) [Early small bowel obstruction]. (56 patients were subjected to conservative management • Group (1) [Early small bowel obstruction]. (56 patients were subjected to conservative](http://slidetodoc.com/presentation_image_h2/fd30358ab91ecd5bcd1a457c20d1ecbf/image-15.jpg)
management • Group (1) [Early small bowel obstruction]. (56 patients were subjected to conservative management: 30 cases were improved within 3 days. ) • Group (2) [Late small bowel obstruction]. 4 patients were exposed to open laparotomy at the time of presentation. • Group (3) [Early small and large bowel obstruction] 10 patients were subjected to conservative management. 9 of them responded, one patient was treated laparoscopy.
![management Group[1] Group[2] Group[3] Total Percentage Number conserv laparosc of ative opy patients Open management Group[1] Group[2] Group[3] Total Percentage Number conserv laparosc of ative opy patients Open](http://slidetodoc.com/presentation_image_h2/fd30358ab91ecd5bcd1a457c20d1ecbf/image-16.jpg)
management Group[1] Group[2] Group[3] Total Percentage Number conserv laparosc of ative opy patients Open surgery 56 4 30 10 16 4 10 70 9 39 1 11 _ 20 100% 55. 5% 15. 5% 29% Radiological data at x-ray abdomen [erect] in correlation with clinical data.
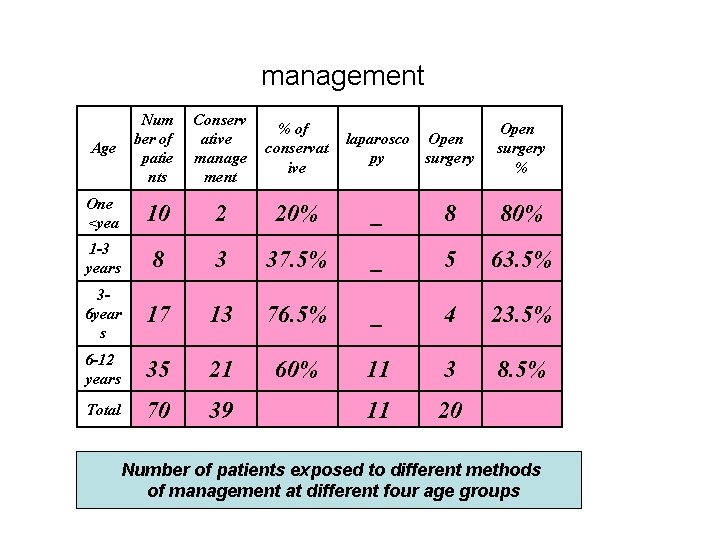
management Age Num ber of patie nts Conserv ative manage ment % of conservat ive One <yea 10 2 20% _ 8 80% 1 -3 years 8 3 37. 5% _ 5 63. 5% 36 year s 17 13 76. 5% _ 4 23. 5% 6 -12 years 35 21 60% 11 3 8. 5% Total 70 39 11 20 laparosco Open py surgery Open surgery % Number of patients exposed to different methods of management at different four age groups
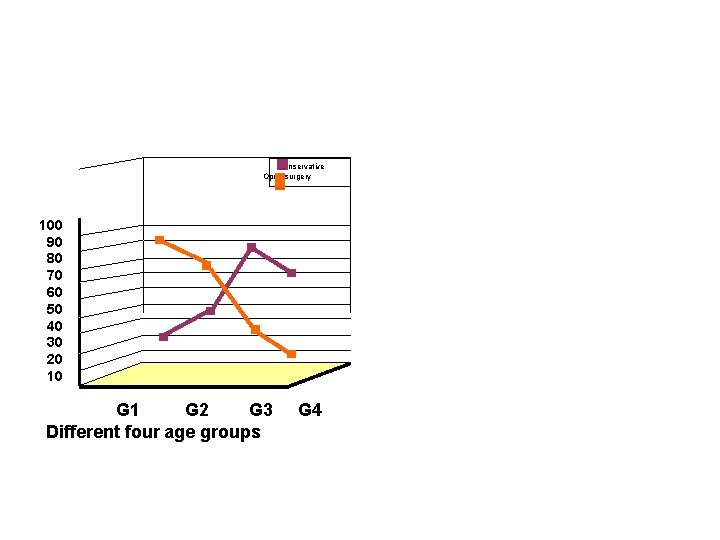
Conservative Open surgery 100 90 80 70 60 50 40 30 20 10 G 1 G 2 G 3 Different four age groups G 4

Results • 39 patients were managed conservatively(55. 5%) , 11 patients were managed by laparoscopy (15. 5%) and 20 patients were subjected to laparotomy. • Majority of children developed ASBO within from 6 months to 2 years after the primary laparotomy. 60 patients(85. 7%).

conclusion • Successful rate of conservative treatment was increased with increasing age, in patients who had more than one previous attack and at early stage of adhesive intestinal obstruction. • It decreased in patients who had primary surgery at neonatal age for intestinal obstruction.

Conclusion • Number of previous laparotomy and time between the primary surgery and time of presentation didn't affect the outcome of conservative management.

Conclusion • Laparoscopy is successful in release fine, flimsy adhesions that developed usually after minor surgery. • Laparotomy is indicated in suspected or impending ischemic bowel or failure of response to conservative management.

thank you
- Slides: 23