Management of Verbal Aggression In Health Care Settings

Management of Verbal Aggression In Health Care Settings Barbara Huggins, MN, RN, PMHCNS - BC “This workforce product was funded by a grant awarded by the U. S. Department of Labor’s Employment and Training Administration. The product was created by the grantee and does not necessarily reflect the official position of the U. S. Department of Labor. The U. S. Department of Labor makes no guarantees, warranties, or assurances of any kind, express or implied, with respect to such information, including any information on linked sites and including, but not limited to, accuracy of the information or its completeness, timeliness, usefulness, adequacy, continued availability, or ownership. ” Retrieved from: https: //www. doleta. gov/grants/pdf/SGA-DFA-PY-13 -10. pdf This work was developed by Saddleback College and is licensed under the Creative Commons Attribution 4. 0 International License. To view a copy of this license, visit http: //creativecommons. org/licenses/by/4. 0/.

Objectives Identify potential situations that may trigger verbal aggression in healthcare settings. Discuss concerns about violence and the threat of client aggression in healthcare settings. Practice verbal skills needed to manage verbal aggression in healthcare settings. Identify measures to maintain personal and environmental safety if signs of verbal aggression emerge.

Acknowledgements Background for this course obtained from: Crisis Prevention Institute http: //educate. crisisprevention. com/CPI. html? code=ITG 004 SCWE&src=Pay-Per. Click&gclid=CIHJ 4 f. CJq 8 MCFQisa. Qod 4 Z 0 A 1 A Management of Aggressive Behavior Training International, Inc. https: //www. moabtraining. com/main. php Centers for Disease Control http: //www. cdc. gov/niosh/topics/violence/training_nurses. html

Is Violence a Part of the Job? Violent and threatening behavior is not acceptable here. “SCHA 2015_015” by South Carolina Hospital Association is licensed under CC BY 2. 0

j 4 p 4 n Assault and Battery By j 4 p 4 n. https: //openclipart. org/detail/212897/men-in-suits-punch

• • • Clinical Situations that Can Increase Aggression Head/Brain Injuries Self. Actualization Psychiatric Illnesses Hypoxia Hypoglycemia Delirium Pain Confusion Dementia Substance Use – intoxication or withdrawal Esteem Needs Social Needs Safety Needs Physiological Needs

Environmental and Social Characteristics Long waits Short staffed Perceived negative attitude from staff History of previous violence Problems with authority Evidence of recent psychosocial stress

Nurses – Lit Review When encountering a person with mental illness medically hospitalized Difficult & Challenging Environment does not support the level of need Safety Concerns https: //openclipart. org/detail/172287/clinical-nurse Unpredictable Behaviors Takes more time (Buckley, 2010; Gertz et al. , 2012; Macneela et al. , 2012; Plant & White, 2013; Reed & Fitzgerald, 2005; Zolnierek, 2009)

BASICS ON VERBAL/NONVERBAL COMMUNICATION Verbal Intonation Pace Volume Congruency between verbal and nonverbal message Ability to demonstrate empathy

Verbal Signs of Increasing Anxiety Raising one’s voice Pressured questions Increasing demands Name calling Other derogatory words

Non-Verbal Cues Breathing Pattern Position of head Expression; Facial color Eyebrows Lips Body Language
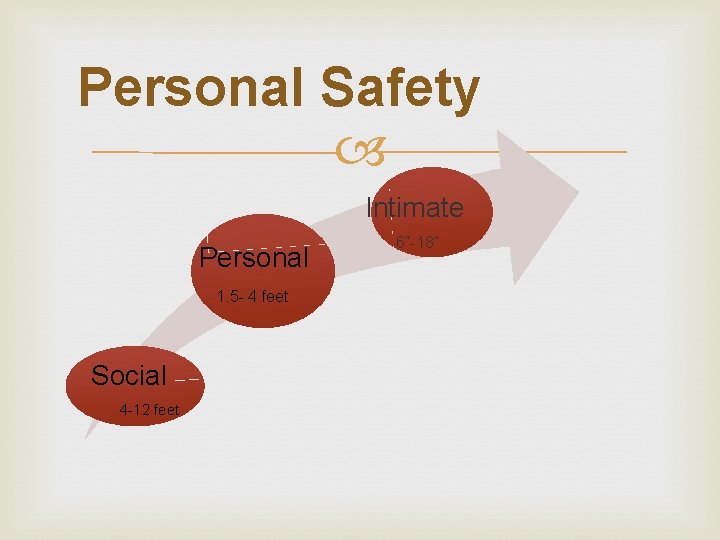
Personal Safety Intimate Personal 1. 5 - 4 feet Social 4 -12 feet 6”-18”

Body Position Body is bladed at 45 degrees Feet are shoulder width apart Equal weight on feet Knees slightly bent Slight forward lean of the body Hands at side – waist level Open hand / bladed hand (CPI, 2008)

Predictors of Violence: Risk Factors Brought in by Police – cuffed Recent conflict – bruises, contusions Involuntary admission Intoxication History of previous violence Cannot conform to what is expected

When Tempers Flare Times of high levels of interaction with patient Meal times Visitation Patient Transportation Service is denied Activity is denied or a limit is set When alcohol/drugs or medication is used

Crisis Acute Behavioral Emergency : Agitation: An acute behavioral emergency requiring immediate intervention because it quickly escalates from: anxiety -> intense anxiety ->aggression ->violence. .

Verbal De-Escalation Mitigates potential crises Manage and maintain safety in the environment Helps the person to regain self control Enhances the relationship through Negotiation Problem Solving Limit Setting Verbal Feedback
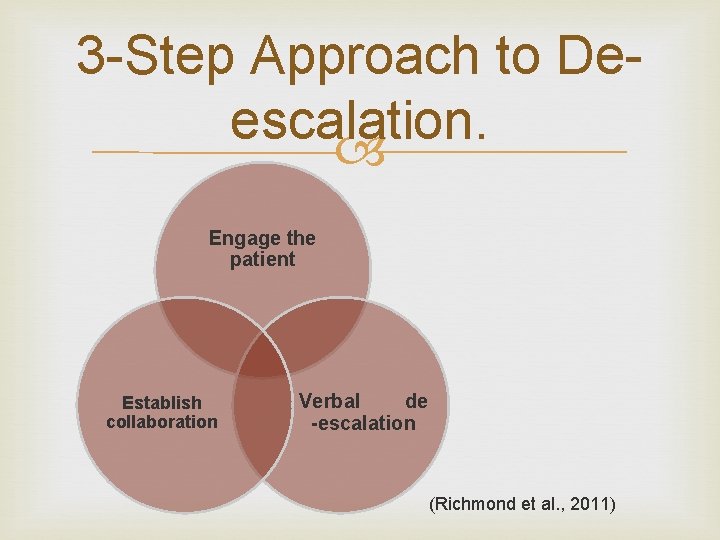
3 -Step Approach to Deescalation. Engage the patient Establish collaboration Verbal de -escalation (Richmond et al. , 2011)
Useful Phrases Focusing -------Tell me what is upsetting you Validate--------Having to wait is frustrating Take Action-----I’ll see what I can do… Proactive-------Maybe we can do something to keep this from happening again Make Observations-I sense that you are calmer after we talked Closure--------Is there anything else I can do…

Professionalism Neutral Appearance/facial expression Approach and Attitude Privacy/ Confidentiality Work Place Civility Top physician, nurse leaders carve out time for patient care. U. S. Army photo by Robert T. Shields is licensed under CC BY 2. 0, https: //creativecommons. org/licenses/by/2. 0/

Escalating Behavior What would you do? https: //www. youtube. com/watch? v=7 c. ZDf. Wc. Iitg � What should be the first step? � What aggression/violence predicting factors were present? � What, if anything, could have been done to de-escalate the situation earlier? � What resources are available to the staff?

Follow Up Considerations Is there a workplace violence prevention policy in your work setting? Self awareness of personal triggers and responses Think of things that can frustrate patient that we as health providers have control of Personal Safety Measures you can take Culture of Safety includes health care workers

REFERENCES Buckley, S. (2010). Caring for those with mental health conditions on a children's ward. British Journal of Nursing, 19(19), 1226 -1230. Centers for Disease Control and Prevention (2016). The National Institute for Occupational Safety and Health. Workplace Violence Prevention for Nurses. (CDC Course N. WB 1865. NIOSH Publication No. 2013 -155). Retrieved from https: //www. cdc. gov/niosh/topics/violence/ training_nurses. html Gerdtz, M. F. , Weiland, T. J. , Jelinek, G. A. , Mackinlay, C. , & Hill, N. (2012). Perspectives of emergency department staff on the triage of mental health-related presentations: Implications for education, policy and practice. Emergency Medicine Australasia, 24(5), 492 -500. doi: 10. 1111/j. 1742 -6723. 2012. 01592. Mac. Neela, P. , Scott, P. A. , Treacy, M. , Hyde, A. , & O'Mahony, R. (2012). A risk to himself: attitudes toward psychiatric patients and choice of psychosocial strategies among nurses In medical-surgical units. Research in Nursing and Health, 35(2), 200 -213. doi: 10. 1002/nur. 21466

Plant, L. , D. , & White, J. , H. (2013). Emergency room psychiatric services: A qualitative study of nurses' experience. Issues in Mental Health Nursing, 34, 240 -248. doi: 10. 3109/01612840. 2012. 718045 Reed, F. , & Fitzgerald, L. (2005). The mixed attitudes of nurses to caring for people with mental illness in a rural general hospital. International Journal of Mental Health Nursing, 14(4), 249 -257. doi: 10. 1111/j. 1440 -0979. 2005. 00389. x Richmond, J. , Berlin, J. , Fishkind, A. , Holloman, G, et al, Verbal de-escalation of the agitated patient: Consensus statement of the American Association for Emergency Psychiatry Project BETA De-escalation Workgroup. Western Journal Emergency Medicine, 13(1), 17 -25. Zolnierek, C. D. (2009). Non-psychiatric hospitalization of people with mental illness: systematic review. Journal of Advanced Nursing, 65(8), 1570 -1583. doi: 10. 1111/j. 1365 -2648. 2009. 05044. x
- Slides: 24