Management of Stable Angina Unstable Angina PK 7

Management of Stable Angina & Unstable Angina PK 7조 강병진

Treatment of Stable Angina • Explanation and Reassurance • Identification and Treatment of Aggravating Condition • Adaptation of Activity • Treatment of Risk Factors • Drug Therapy • Coronary Revascularization

Medical Treatment • Anti-ischemic therapy – Nitrate – Beta-Adrenergic Blockade – Calcium Channel Blocker • Anti-thrombotic therapy – Oral Antiplatelet Therapy (Aspirin, Clopidogrel) – Statins • ACEi • Ranolazine • Nicorandil

Nitrates • 작용기전 – 심근의 산소 요구량 감소 : Systemic venodilation & EDV↓ – 심근의 Blood Flow 증가 : Coronary vasodilation • 효과 – Angina Sx의 감소 – Exercise tolerance의 증가 • 사용 – Chest pain 발생 or 유발 상황 5분 전 (5분 간격으로 3 rd dose까지) – Sublingual Tablet, Spray 등 – Long acting : Oral, IV, 연고, Patch • 부작용 – Headache, Facial flushing, Hypotension • 금기증 – Hypertrophic obstructive CMP, Sildenafil과 병용 • Nitrate tolerance

β-Adrenergic Blockers • 작용기전 – 심근 산소 요구량 감소 : HR, BP, Myocardial Contractility 증가 억제 • 효과 – – HR 증가 억제 (특히 운동시) 협심증 증상 감소 Antihypertensive effect MI 후 Mortality, Reinfarction 감소 (Ischemia의 호전) • 금기증 – Asthma, COPD, AV conduction disturbance, Severe bradycardia, Raynaud’s phenomenon, 부작용 발생시 • 부작용 – Fatigue, Reduced exercise tolerance, Nightmares, Cold extremities, Intermittent claudication, Bradycardia, Hypoglycemia의 악화 • β 1 -specific β-blocker (Metoprolol, Atenolol) – Pts. with mild bronchial obstruction and Insulin-requiring DM

Calcium Channel Blockers • 작용기전 – 심근 산소 요구량 감소 : BP, Myocardial Contractility 증가 억제 • Combine with β-blocker – Verapamil (X) – Diltiazem (O) : Normal Vent. Function & No conduction abnormality – Amlodipine & other 2 nd generation dihydropyridine calcium antagonists (O) : HTN과 angina가 동반될 시 유용 • 적응증 β-blocker와 Nitrate의 병용에 잘 반응하지 않을 때 β-blocker에 부작용이 있을 때 (우울증, 피로감, 성기능 장애) Asthma나 COPD등의 과거력 Sick-sinus syndrome이나 Significant AV conduction disturbance 있을 때, – Variant angina – Symptomatic peripheral arterial disease – – • 부작용 – Verapamil, Diltiazem : Conduction abnormality와 Bradyarrhythmia 유발 가능

Antiplatelet Agents • Atherosclerosis의 악화 방지 및 Acute MI의 발생 예방 • Aspirin – – Irriversible inhibitor of Platelet COX activity Platelet activation 방해 IHD가 있는 모든 환자에서 사용 부작용 : GI bleeding, Dyspepsia, Allergy • Clopidogrel – ADP receptor-mediated platelet aggregation 억제 – Aspirin에 side effect 있을 시에 대체 가능 – Aspirin과 병용 • • ACS 환자에서 Coronary ischemic event와 사망을 줄임 Stent 시술 시 thrombus formation risk를 줄임 ACS 환자에서 DES implantation 시에 적어도 1년간 투여 Chronic IHD에서는 병용의 효과가 증명되지 않음

Lipid lowering agents • Dyslipidemia의 치료 – Long term relief from angina – Reduced need for revascularization – Reduction in MI and death • HMG-Co. A reductase inhibitors (Statins) – LDL-Cholesterol, TG↓, HDL-Cholesterol↑ – 효과 • • 혈관 내피세포 기능 회복 Atherosclerosis의 thrombotic complication 감소 Smooth muscle cell의 증식 억제 항 염증 작용
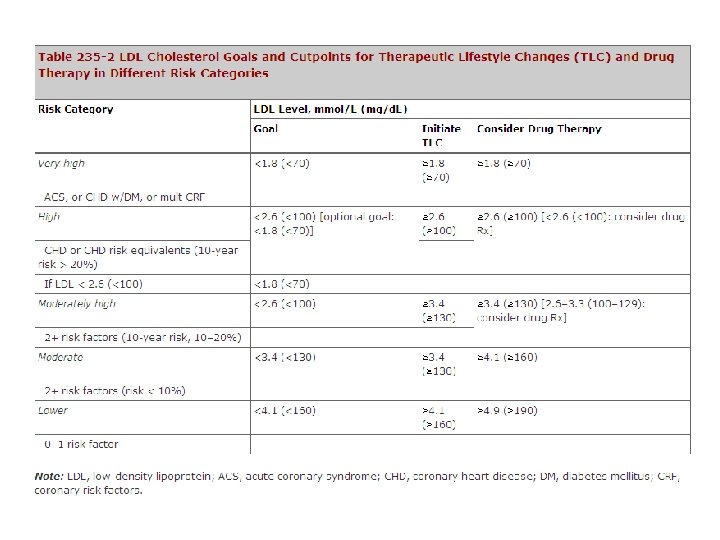

Other Therapies • Angiotensin Converting Enzyme Inhibitor (ACEi) – Vasculoprotective effect : 2차 예방적 목적 – Survivors of MI, Patient with HTN, chronic IHD – DM이나 LV dysfunction이 동반되고, β-blocker와 Statin으로 BP와 LDL-cholesterol이 잘 조절되지 않을 때 • Ranolazine • Nicorandil (K+ channel opener)
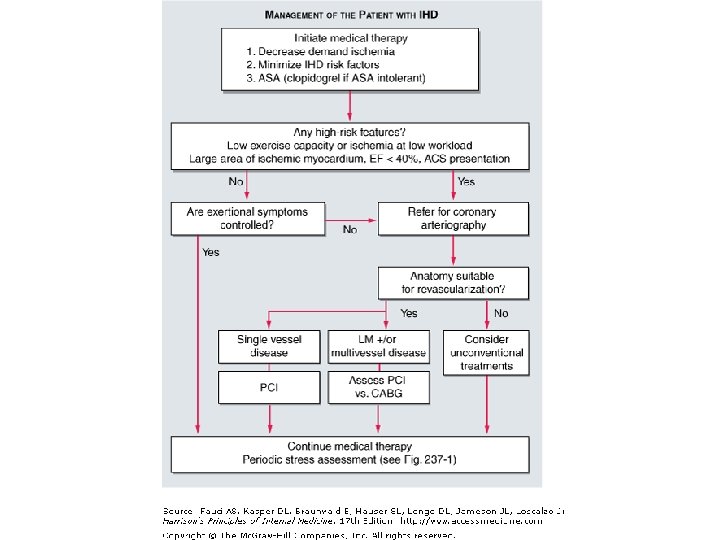

Surgical Treatment • Coronary Revascularization – Percutaneous Coronary Intervention (PCI) – Coronary Artery Bypass Grafting (CABG)

Percutaneous Coronary Intervention • Balloon dilatation + Coronary artery stenting • Indication – Stress test에서 양성소견이며, Medical therapy에도 불구하고 지속되는 Angina – CABG or PCI 후에 발생한 recurrent angina • Risk – Thrombosis with vessel occlusion, Uncontrolled ischemia, Ventricular failure ⇒ Aspirin, Clopidogrel, Antithrombin

Percutaneous Coronary Intervention • Efficacy – Primary success • Luminal diameter 증가 >20%, Residual obstruction <50%, Angina Sx. 호전 • > 95%에서 달성 – After Bare Metal Stent(BMS) Insertion • Restenosis : ~20% within 6 months • Recurrence of angina : ~10% within 6 months • 호발 상황 : DM, Incomplete dilation of the stenosis, Dilation of the LAD coronary artery, 작은 혈관, 폐쇄되었던 혈관, Vein graft의 폐쇄, stenoses containing thrombi – Drug Eluting Stent (DES) • Antiproliferative effect : Sirolimus(Cypher), Paclitaxel(Taxus) • 시술 후 Aspirin은 평생, Clopidogrel은 1년 이상 복용 권장
Coronary Artery Bypass Surgery • Graft : Int. mammary a. , Radial a. , Saphenous v. • 비교적 안전 – Mortality rate < 1% • 적응증 (CABG 권장) – Lt. main CAD – Proximal LAD의 significant occlusion 있는 2 - or 3 -vessel disease – LV dysfunction (LVEF < 50%) – DM patients • Perioperative mortality 증가 – – – CHF or LV dysfunction Age > 80 재수술 응급 수술 DM patients
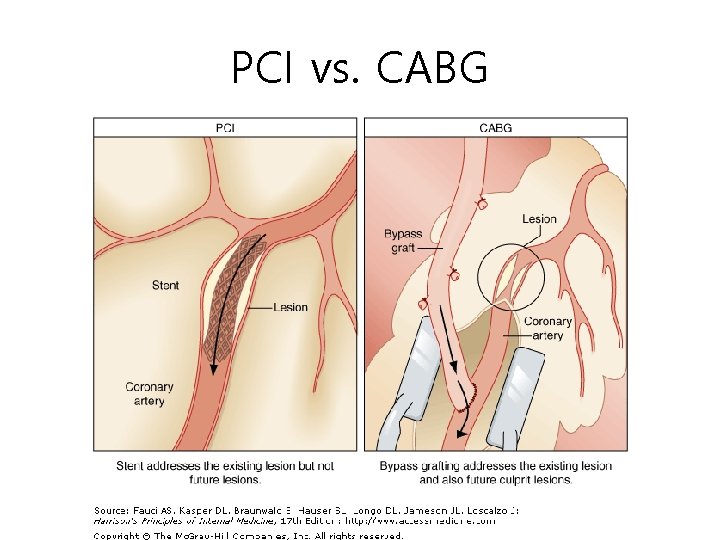
PCI vs. CABG
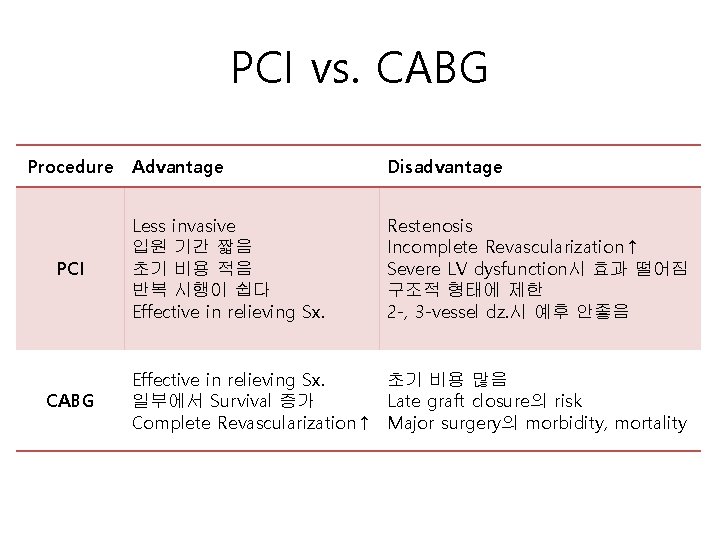
PCI vs. CABG Procedure PCI CABG Advantage Disadvantage Less invasive 입원 기간 짧음 초기 비용 적음 반복 시행이 쉽다 Effective in relieving Sx. Restenosis Incomplete Revascularization↑ Severe LV dysfunction시 효과 떨어짐 구조적 형태에 제한 2 -, 3 -vessel dz. 시 예후 안좋음 초기 비용 많음 Effective in relieving Sx. 일부에서 Survival 증가 Late graft closure의 risk Complete Revascularization↑ Major surgery의 morbidity, mortality

Treatment of Unstable Angina/NSTEMI • Medical therapy – Anti-ischemic therapy • Nitrate • Beta-Adrenergic Blockade • Calcium Channel Blocker – Anti-thrombotic therapy • Oral Antiplatelet Therapy (Aspirin, Clopidogrel) • IV Antiplatelet Therapy (GP IIb/IIIa inhibitors) – Eptifibatide, Tirofiban, Abciximab • Heparin (UFH, LMWH), Factor Xa inhibitor (Fondaparinux) • Statins – ACEi • Early invasive therapy – PCI, CABG

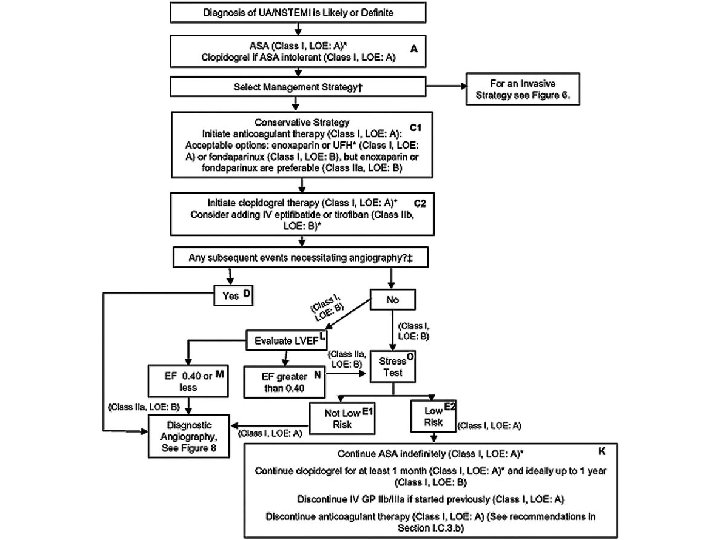
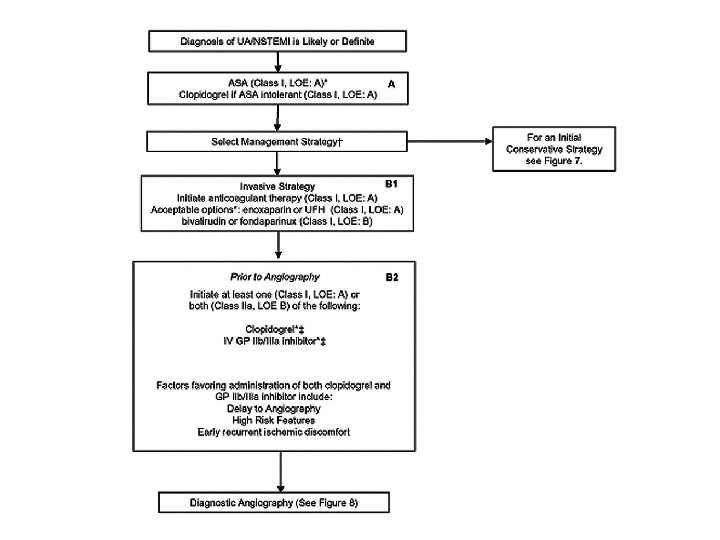
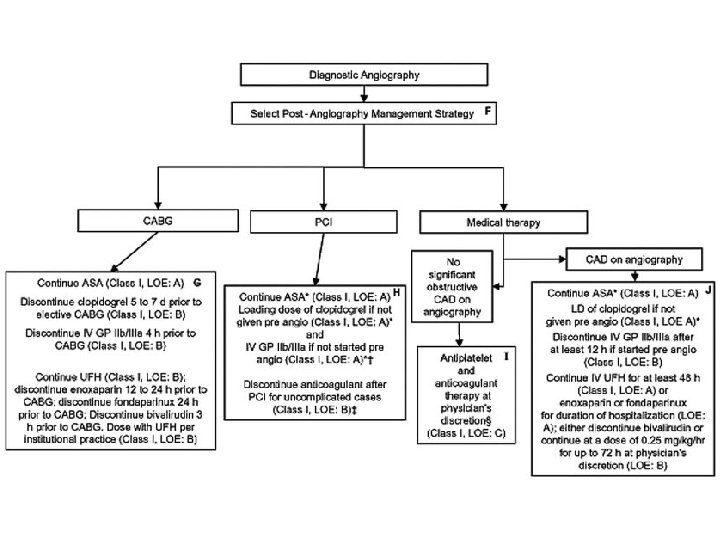

Reference • Harrison's Principles of Internal Medicine, 17 e • ACC/AHA 2007 Guidelines for the Management of Patients With Unstable Angina/Non–ST-Elevation Myocardial Infarction: Executive Summary
- Slides: 23