Management of pediatric pseudotumor cerebri in Germany A

Management of pediatric pseudotumor cerebri in Germany. A critical appraisal. Münster 2012 Daniel Tibussek, MD Leverkusen Children‘s Hospital University of Duesseldorf

Overview • Presentation of clinical/epidemiological data - ESPED-Survey 1 -12/2008 - Duesseldorf-Study 1997 -2007 - „Registry“ 2006 -today (own cases seen+ second opinion cases) >> www. pseudotumor. info << • Critical thoughts about diagnostic and therapeutic management

Definition

Pseudotumor cerebri/IIH • Klinische Zeichen/Symptome sind auf erhöhten intracerebralen Druck zurückzuführen • Liquoröffnungsdruck > 20 cm H 2 O unter standardisierten Bedingungen • Normale Liquor-Zusammensetzung (Zellzahl, Eiweiß, Zucker) • Unauffällige cerebrale Bildgebung (Ausnahme: empty sella): - Ausschluss cerebrale Raumforderung, strukturelle ZNSMalformation, Gefäßfehlbildung/Sinusvenenthrombose - Kein Hinweis auf druckbedingte Ventrikeldilatation Adapted from: Friedman DI, Jacobson DM. Diagnostic criteria for idiopathic intracranial hypertension. Neurology 2002; 59: 1492 -5.

Epidemiology in Germany

ESPED Study • • • Recruiting period Jan-Dec/2008 Alltogether 86 reports to ESPED office 3 erroneous reports withdrawn 5 reports withdrawn as clear secondary cases 1 case later withdrawn (identification as spinal tumor!) • 16 questionaires were not returned (? ) • 61 cases/questionaires could be analyzed

Incidence Germany • 2008: 61 pediatric cases per year • ≈ 0, 5/100. 000 children/year Previous data • General incidence: Ca. 1 per 100. 000 /y • Incidence ♀ 20 -44 yrs: 19 /100. 000 ♀ /y
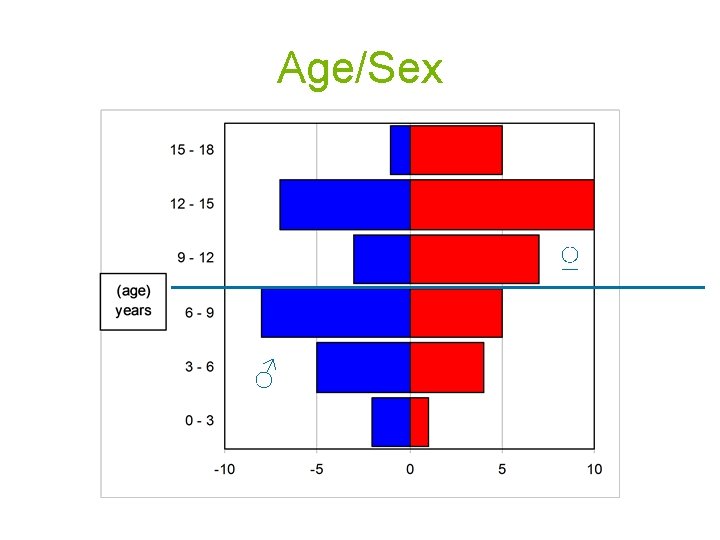
Age/Sex ♀ ♂
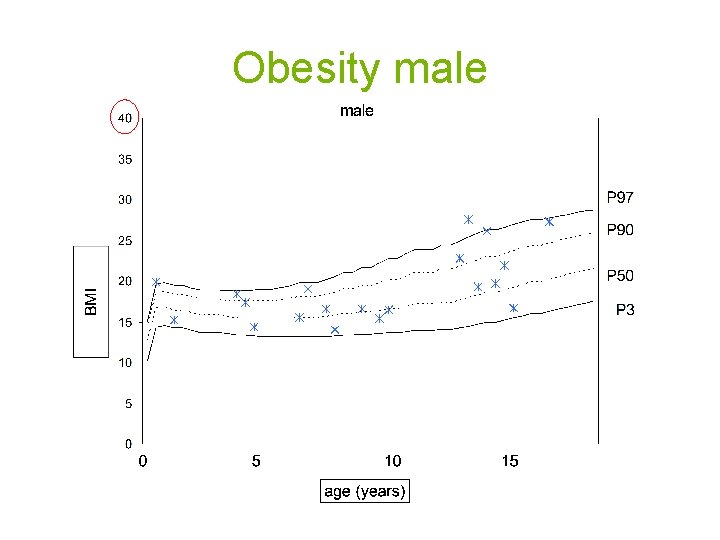
Obesity male
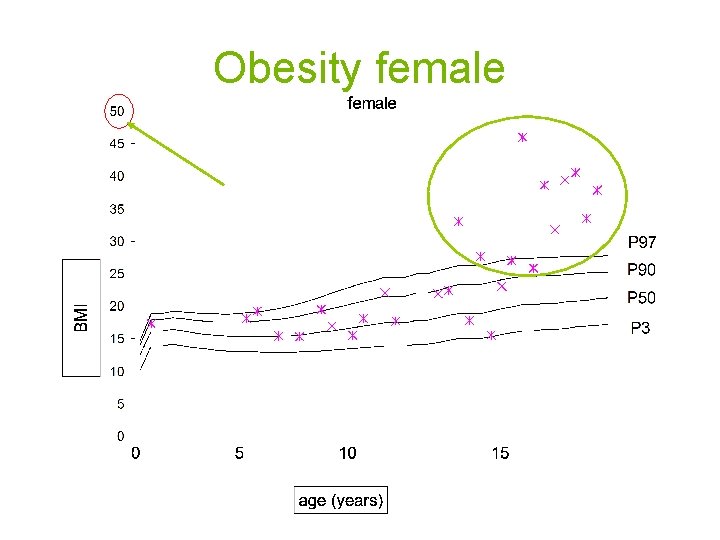
Obesity female

Clinical manifestation 1) IIH as accidental finding 2) Headache 3) Early eye symptoms

IIH as accidental finding • ESPED: • Düsseldorf: 5 von 61 Kinder 16 von 53 Kindern „An apparent lack of symptoms does not rule out chronic Literatur: increased intracranial pressure • Lim et al. 3 von 29 in young children. “ • Bassan et al. 14 von 45 Tibussek et al. Child Nerv Syst 2010; 26: 313 -21 Lim et al. Arch Dis Child 2005; 90: 206– 210 Bassan et al. Acta Neurol Scand. 2008 Oct; 118(4): 251 -5

Headache Should we measure CSF opening pressure Prebubertal: 53% d. F. in chronic headache? Pubertal: 79% d. F. MRV in chronic headache? Nature Reviews Neurology 2008; 4, 422– 423 Nature Clinical Practice Neurology 2007; 3, 254 -255
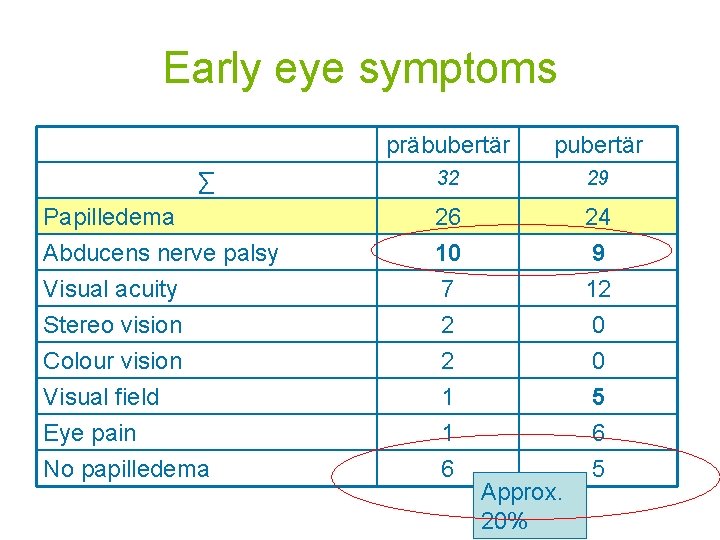
Early eye symptoms präbubertär pubertär 32 29 Papilledema Abducens nerve palsy 26 10 24 9 Visual acuity Stereo vision Colour vision Visual field Eye pain No papilledema 7 2 2 1 1 6 12 0 0 5 6 5 ∑ Approx. 20%
Does IIH without Papilledema exist? „idiopathic intracranial hypertension (IIH) without Papilloedema“ (IIHWOP)
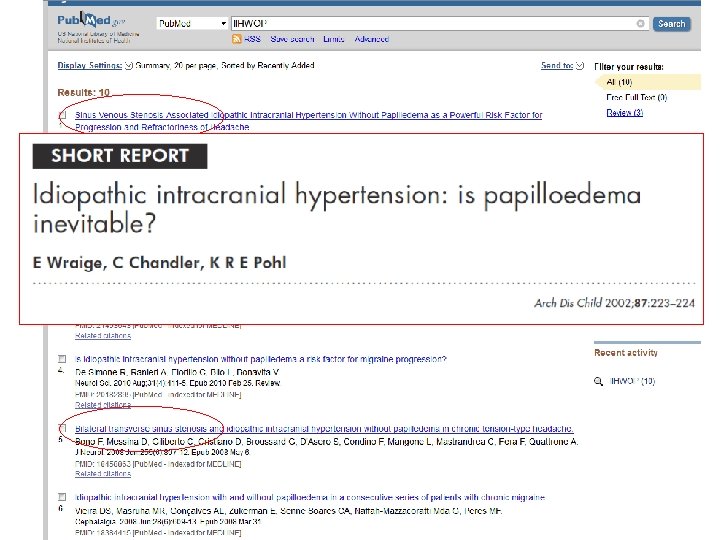
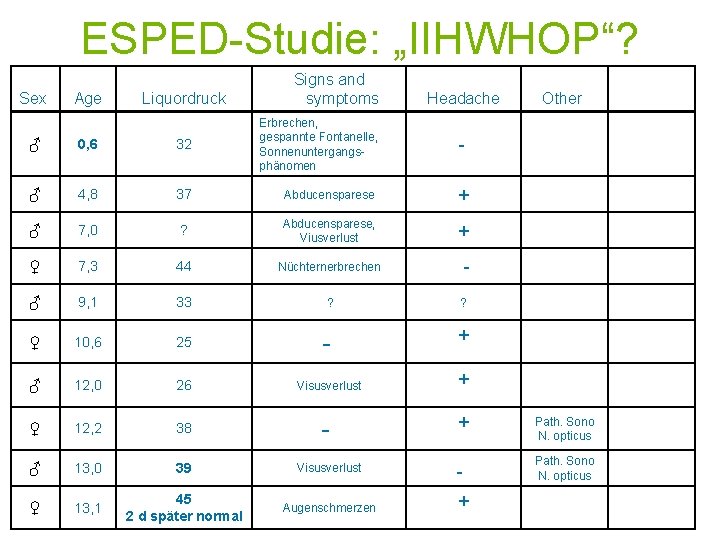
ESPED-Studie: „IIHWHOP“? Sex Age Liquordruck Signs and symptoms Erbrechen, gespannte Fontanelle, Sonnenuntergangsphänomen Headache Other - ♂ 0, 6 32 ♂ 4, 8 37 Abducensparese + ♂ 7, 0 ? Abducensparese, Viusverlust + ♀ 7, 3 44 Nüchternerbrechen - ♂ 9, 1 33 ? ? ♀ 10, 6 25 - + ♂ 12, 0 26 Visusverlust + ♀ 12, 2 38 - + ♂ 13, 0 39 Visusverlust - Path. Sono N. opticus ♀ 13, 1 45 2 d später normal Augenschmerzen + Path. Sono N. opticus
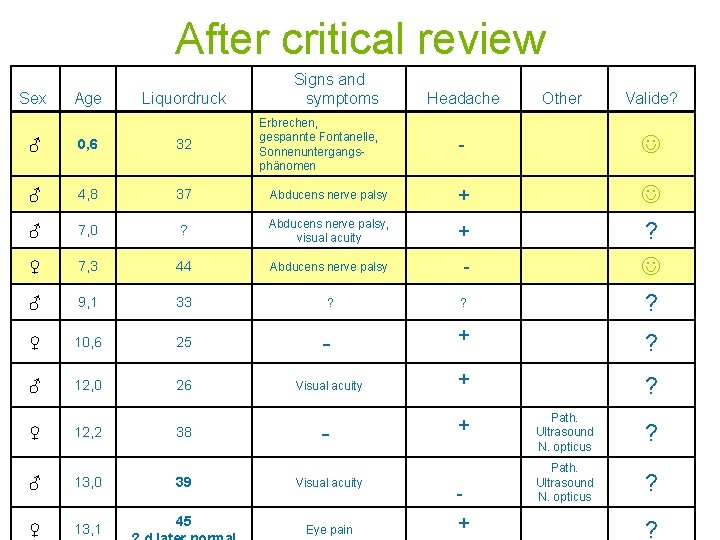
After critical review Sex Age Liquordruck Signs and symptoms Erbrechen, gespannte Fontanelle, Sonnenuntergangsphänomen Headache Other Valide? - ♂ 0, 6 32 ♂ 4, 8 37 Abducens nerve palsy + ♂ 7, 0 ? Abducens nerve palsy, visual acuity + ♀ 7, 3 44 Abducens nerve palsy - ♂ 9, 1 33 ? ? ? ♀ 10, 6 25 - + ? ♂ 12, 0 26 Visual acuity + ? Path. Ultrasound N. opticus ? - Path. Ultrasound N. opticus ? + ? ♀ 12, 2 38 - ♂ 13, 0 39 Visual acuity ♀ 13, 1 45 Eye pain + ?

IIH without papilledema does exist even after infancy! However, diagnosis should be questioned in these cases! Faz et al. J Child Neurol. 2010; 25: 1389– 1392
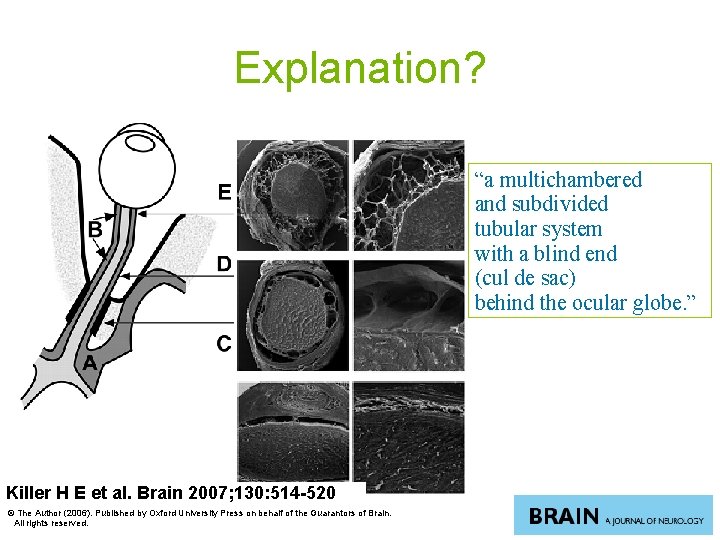
Explanation? “a multichambered and subdivided tubular system with a blind end (cul de sac) behind the ocular globe. ” Killer H E et al. Brain 2007; 130: 514 -520 © The Author (2006). Published by Oxford University Press on behalf of the Guarantors of Brain. All rights reserved.

But…

„False diagnosis of papilledema and IIH“ • 18 children referred with disc swelling and suspected IIH. • Following a tertiary ophthalmological review: papilloedema was excluded in 10. • In these 10 children, five had a mean opening pressure on lumbar puncture of 27. 2 cm H 2 O, range 19– 32 Mishra A et al. Eur J Paediatr Neurol 2007 ; 11 : 39 – 42

„Light at the end of the tunnel of the blind leading the blind? “ „Thus, for every child that truly has IIH, I typically see four or five other children without IIH but with CSF pressure measurement between 17 and 27 cm of CSF“ Colin Kennedy (Editorial) Dev Med Child Neur 2006; 48: 83 -83

LP pressure measurement and eye investigation frequently lead to false diagnosis of Pseudotumor cerebri

CSF Opening pressure measurement

„normal“ values ? Avery et al. N Engl J Med 2010; 363: 891 -893 Lee and Vedanarayanan. Pediatric Neurology 2011; 45: 238 -240

What is „controlled setting“? N Engl J Med 2006; 355: e 12.
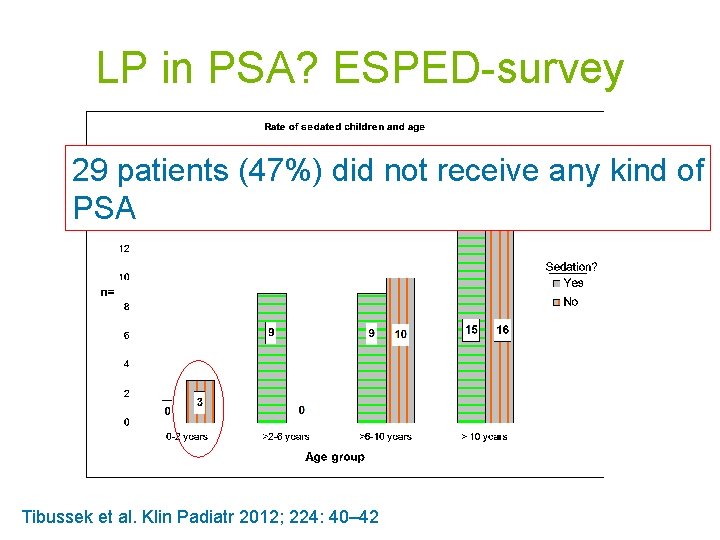
LP in PSA? ESPED-survey 29 patients (47%) did not receive any kind of PSA Tibussek et al. Klin Padiatr 2012; 224: 40– 42

Does it matter?

Advantages of LP in PSA • • No pain No trauma (repeated LP likely!) Higher success rate!! Comparability better if same PSA regime used

LP in PSA • …should be standardized >> guideline? To get routine LP pressure measurement should generally be done more often Siehe auch: Perry und Ebinger Monatsschrift Kinderheilkunde 2012; 3: 251 -259

But! How reliabel is a pressure of 112 cm H 2 O In a 7 year old boy Measured under Ketanest/Midazolam? Ben Yehuda and Watemberg J Child Neurol 2006; 21: 441 -3. Himmelseher and Durieux Anesth Analg 2005; 101: 524 -34. CAVE: Complex influences of different PSA regimes on ICP!
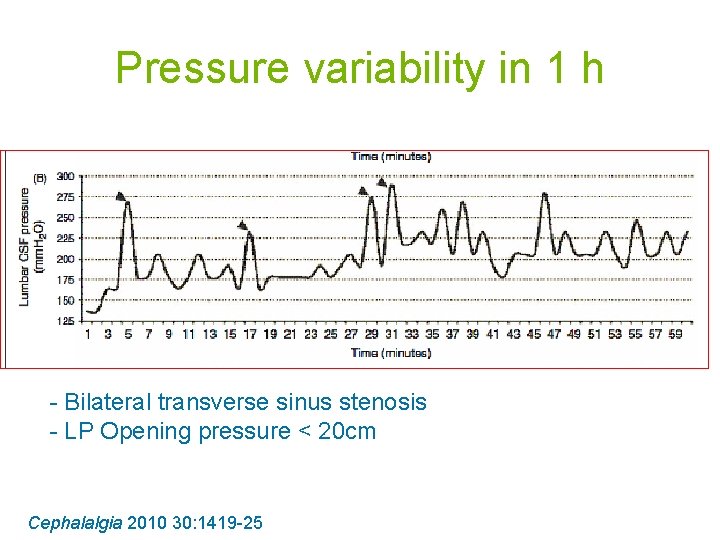
Pressure variability in 1 h - Bilateral transverse sinus stenosis - LP Opening pressure < 20 cm Cephalalgia 2010 30: 1419 -25

Remember! Deborah I Friedman: „A high opening pressure in and of itself is neither specific nor diagnostic and must be used in context with other data from the history, examination, neuroimaging and laboratory to arrive at the correct diagnosis“ Cephalgia 2010; 30: 1415 -16

The concept of „probable IIH“ 1) 2) 3) 4) 5) 6) 7) If symptoms present, they may only reflect those of generalized intracranial hypertension or papilledema. If signs present, they may only reflect those of generalized intracranial hypertension or papilledema CSF opening pressure may be < 20 cm H 2 O Normal CSF composition No evidence of hydrocephalus, mass, structural, or vascular lesion on MRI and/or MR venography Exclusion of other causes of intracranial hypertension Clear clinical response to initial pressure release Distelmaier F, Mayatepek E, Tibussek D (2008) Probable idiopathic intracranial hypertension in pre-pubertal children. Arch Dis Child 93: 356– 357

Therapy and therapy guidance Why do we decide how?

Therapy: ESPED-Data • Single LP: 14 Patienten • Serial LP: 1 Patient • Acetazolamid: 44 Patients (4 -46 mg/kg/d) • Early Escalation: 9 Patients - 5 x Steroid pulse - 2 x Furosemid - 2 x Topiramate • Stent 1 Patient (Stenosis Sinus transv. et sigmoid. ) • LP-Shunt 1 Patient (Sinus venous thrombosis)

Therapyresistence? • • • 7 yrs, boy, subjective visual disturbance since 6 wks Papilledema (Papille prominent, disc margin blurred, R>L) Normal visual acuity, visual fields OK OP 37 cm H 2 O 4 wks Acetazolamid 10 mg/kg, no adverse effects, BE – 8, 4 • No visual disturbances any more • after wks: 35 cm H 2 O, eyes did not chance • Plus Furosemid: side effects • E-mail to Dr Tibussek: „Doctors talk about VP-shunt“

Therapy: Controversies • Medication: (when, what, how long? ) • Monitoring: How? How long? • Re-LP to controll pressure? • What is therapy-resistence? • When and which invasive therapy? • Role of sinus venous stenosis? >> Stent in children?

Antworten? "If the evidence base for management of IIH were ice, I would not walk on it, even if I were a duck" Colin Kennedy, DMCN 2006 Guideline of the German Society of Neurology

What are our treatment goals? 1) Maintain/regain normal visual function With good interdisciplinary work and good drug adherence realistic goal in > 90% of pediatric patients. „Level of evidence 5 -6“ 2) Relief headaches 3) (prevent invasive therapies)

Step-wise approach Step 1: No visual loss: Step 0: pressure release! - Symptomatic headache (migraine) therapy - Weight reduction, correct other secondary causes - If necessary Acetazolamide Step 2: Mild visual loss: - Acetazolamide - Furosemide - (Topiramate) - Weight reduction, if necessary Step 3: Severe, or progression of visual loss: - Optic nerve sheath decompression (ONSD) - High-dose IV steroids and acetazolamide - Lumboperitoneal shunt for failed ONSD or intractable headache Liu et al. 2011 in: Neuro-Ophthalmology, Diagnosis and Management, Saunders, Elsevier

Pressure release as the only therapy ESPED-Studie • 14 Patients got LP pressure release as the only treatment. • In 1 case succesful as serial LP. „Interestingly, it is not uncommon to observe a lasting clinical remission after a single lumbar puncture in some IIH patients“ Bruce BB, Biousse V, Newman NJ. Update on Idiopathic Intracranial Hypertension. Am J Opthalmol 2011; 152: 163 -169
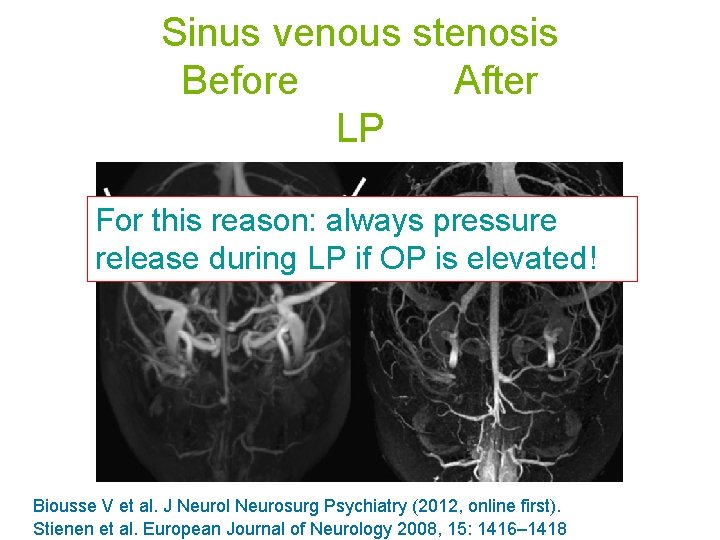
Sinus venous stenosis Before After LP For this reason: always pressure release during LP if OP is elevated! Biousse V et al. J Neurol Neurosurg Psychiatry (2012, online first). Stienen et al. European Journal of Neurology 2008, 15: 1416– 1418

Therapie-Escalation: When and Why? „Corbett and Thompson have emphasized that treatment decisions should not rest on … the severity of papilledema, or CSF opening or closing pressure. “ „Instead, the modern management of pseudotumor cerebri is based largely upon the level of visual loss. “ Aus: Liu et al. : Neuro-Ophthalmology. Diagnosis and Management. Second edition. 2010

The case… 8 months later: „The eye doctor now questions the diagnosis of PTC. Ultrasound suggest drusen. “ Fluorecence confirmed it This child did NOT have PTC! W. A. Lagrèze. Differenzialdiagnose der Papillenschwellung. Ophthalmologe. 2001· 98: 417– 433 Capo et al. Optic nerve abnormalities in children: A practical Approach. J AAPOS 2011; 15: 281 -290
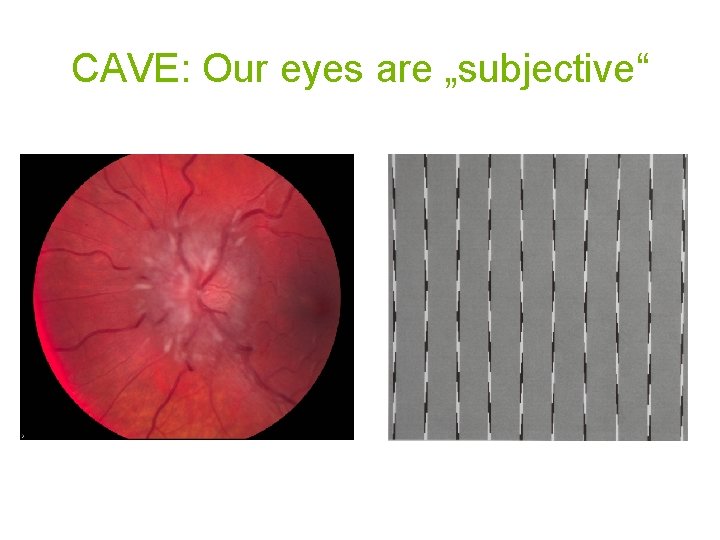
CAVE: Our eyes are „subjective“

Neuroophtalmological Follow-up When, what, how long? How do we objectify results of the ophthalmological investigation?

Neuroophthalmology • • Papilledema: Photodocumentation! Frisen classification? Visual field, how? Optical Coherence Tomography? Contrast sensitivity? VEP? Ultrasound? Fluorescein angiography?

The so called „Therapy resistence“ Without visual disturbances no • „still papilledema“ escalation! • „still blurred border of papilla“ • „still headache“ Exception: worsening papilledema • „still high OP on repeated LP“ LP control: not routinely! Often • … unreliable in childhood! Mathews et al. Curr Opin Ophthalmol 2003; 14: 364 -370

Headache as criteria for success? • A „classical“ patient shows rapid headache „Many IIH patients have persistent headaches, relief after LP even after normalization BUT of the intracranial pressure“ • Headache often confounds treatment decisions! „Patients with IIH frequently have headaches not necessarily related to increased intracranial pressure“ Bruce BB, Biousse V, Newman NJ. Am J Ophthalmol 2011; 152: 163 -169 Friedman DI, Rausch A. Neurology 2002; 58: 1551 -1553

CAVE: Compliance • Düsseldorf: 2 Patients with Non-Compliance 1 x optical atrophy (adolescent) 1 x VP-Shunt • Israel: „visual outcome was less favorable in pubertal patients“ due to adherence problems? Stiebel-Kalish et al. Puberty as a risk factor for less favorable visual outcome in idiopathic intracranial hypertension. Am J Ophthalmol 2006; 142: 279– 283.
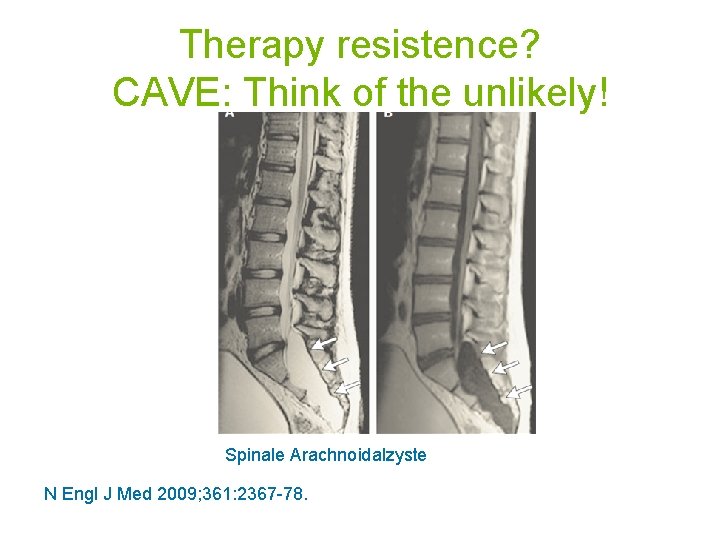
Therapy resistence? CAVE: Think of the unlikely! Spinale Arachnoidalzyste N Engl J Med 2009; 361: 2367 -78.
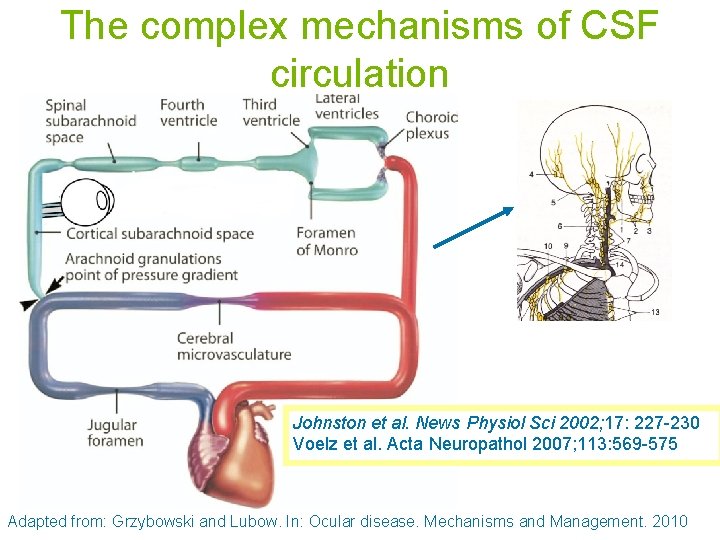
The complex mechanisms of CSF circulation Johnston et al. News Physiol Sci 2002; 17: 227 -230 Voelz et al. Acta Neuropathol 2007; 113: 569 -575 Adapted from: Grzybowski and Lubow. In: Ocular disease. Mechanisms and Management. 2010

C) Invasive Therapy • FIRST: DO NO HARM! • SECOND: WHAT IS YOUR TREATMENT GOAL?

Interdisziplinary decision! • Optimal management of IIH requires input from ophthalmology, neurology and neurosurgery and good communications between specialties are essential to protect the patient from unnecessary lumbar punctures and CSF diversion surgery on the one hand avoidable visual loss on the other. Standridge SM. Idiopathic intracranial hypertension in children: A review and algorithm. Pediatr Neurol 2010; 43: 377 -390.

Take Home Messages • The doubtless diagnosis of IIH is diffucult! • Therapy escalation follows visual function. • Critically question if invasive procedure are unpreventable. • Critically question diagnosis in atypical cases. • Interdisciplinary approach! • Many open questions!

Frühstückseminar zur Erarbeitung einer SOP zum Pseudotumor cerebri Morgen 07: 30 – 08: 30 Uhr, Weißer Saal

Vielen Dank für Ihre Aufmerksamkeit
- Slides: 59