Management of patients with Unstable Angina Raffaele Bugiardini

Management of patients with Unstable Angina Raffaele Bugiardini

Key Assumptions • The euros available for health care limited • The medical profession must play a significant role in the critical evaluation of the use of diagnostic procedures and therapies
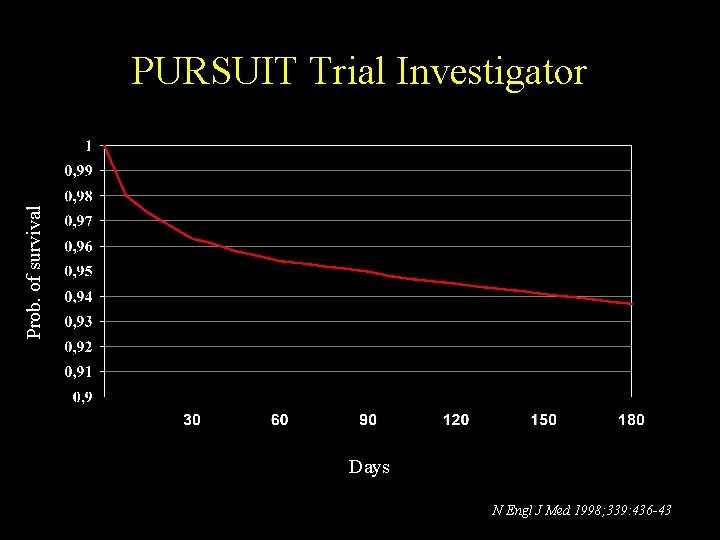
Prob. of survival PURSUIT Trial Investigator Days N Engl J Med 1998; 339: 436 -43

INITIAL EVALUATION AND MANAGEMENT Patients with suspected unstable angina must be evaluated rapidly The physician then must place the evaluation in the context of 2 critical questions: • Are the symptoms a manifestation of an unstable angina? • If so, what is the prognosis?

Are the symptoms a manifestation of ACS ? If so, what is the prognosis ?

“The presence or absence of the traditional risk factor ordinarily should not be used to determine whether an individual patient should be admitted or treated for ACS. However, the presence of these risk factors does apper to relate to poor outcomes in patients with established ACS. ” ACC/AHA Practice Guidelines 2002

Likelihood that Signs and Symptoms Represent an Unstable Angina History High Likelihood Intermediate Likelihood Low Likelihood Typical Angina CAD history Typical Angina, Age >70 yrs, Sex M, Probable ischemic symptoms Diabetes Mellitus Recent cocaine use Examination Transient MR Hypotension Diaphoresis, Pulmonary Edema Extracardiac vascular disease Chest disconfort by palpitation ECG New ST-segment deviation or T-wave inversion Fixed Q waves Abnormal ST or Twaves not documented to be new TTwaveflattering or inversion in laeds with dominant R Normal Cardiac Markers cardiac Tn. I, Tn. T or CK-MB Modified from Braunwald E et all 1994; AHCPR Pub. 94 -0602

Risk Stratification Non Invasive Stress Testing • LOW RISK PTS • INTERMEDIATE RISK PTS free of ischemia at rest and of CHF for a minimum 12 - 24 hours 2 - 3 days ACC/AHA Practice Guidelines 2002

Are the symptoms a manifestation of ACS ? If so, what is the prognosis ?
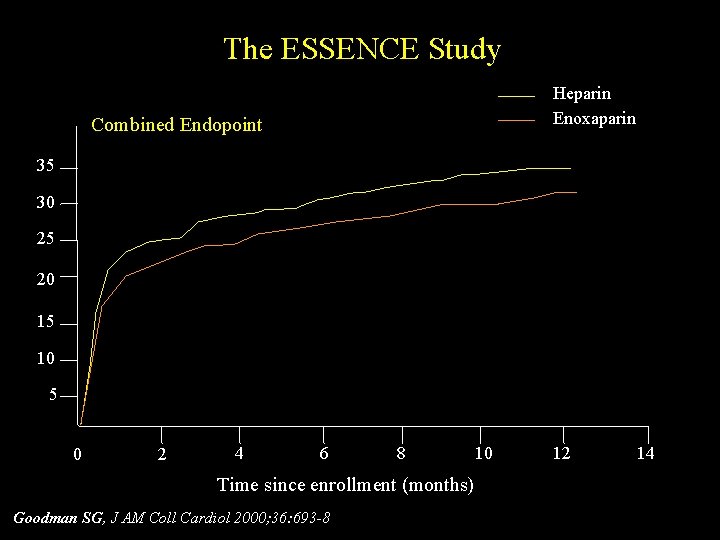
The ESSENCE Study 40 Heparin Enoxaparin Combined Endopoint 35 30 25 20 15 10 5 0 2 4 6 8 Time since enrollment (months) Goodman SG, J AM Coll Cardiol 2000; 36: 693 -8 10 12 14

TIMI risk score 1 - age > 65 yrs 2 - > 3 coronary risk factors 3 - more that 2 angina events within 24 hrs 4 - prior angiographic obstruction 5 - aspirin (in the 7 prior days) 6 - ST-segment deviation 7 - elevated cardiac markers Antman EM et al. JAMA 2000; 284: 835 -42
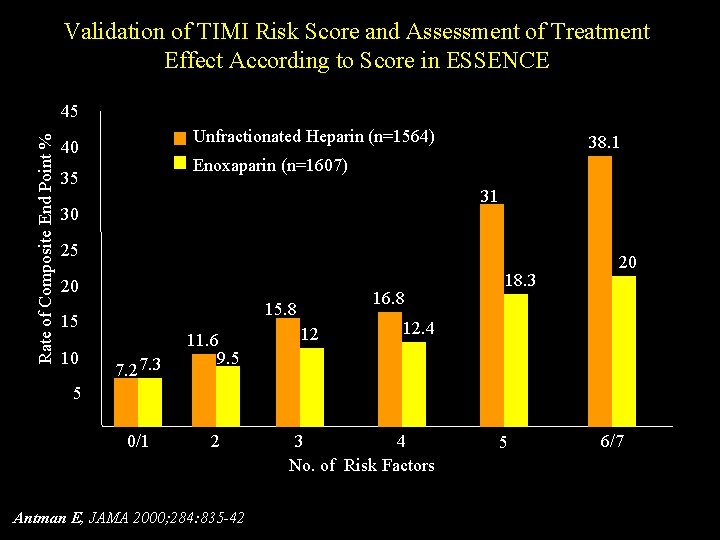
Validation of TIMI Risk Score and Assessment of Treatment Effect According to Score in ESSENCE Rate of Composite End Point % 45 Unfractionated Heparin (n=1564) 40 38. 1 Enoxaparin (n=1607) 35 31 30 25 20 15 10 16. 8 15. 8 7. 2 7. 3 11. 6 9. 5 12 18. 3 20 12. 4 5 0/1 2 Antman E, JAMA 2000; 284: 835 -42 3 4 No. of Risk Factors 5 6/7

Tools for risk stratification initial management • • • Age and History Symptoms Standard ECG Biochemical Markers Continous ECG
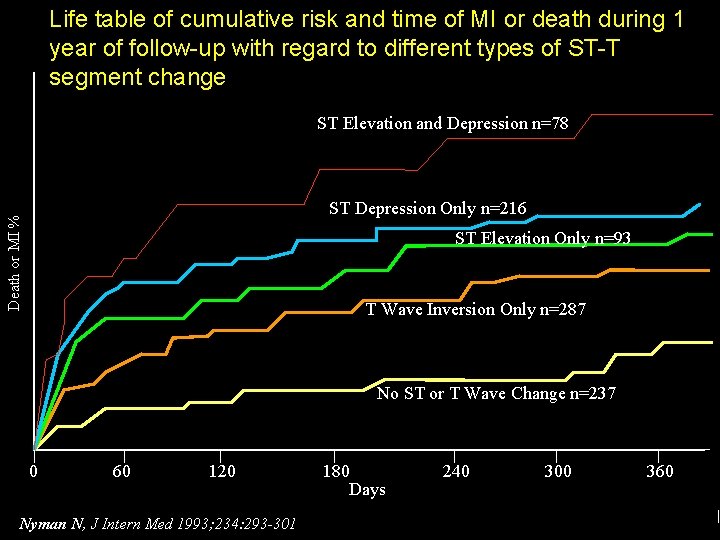
Life table of cumulative risk and time of MI or death during 1 year of follow-up with regard to different types of ST-T segment change ST Elevation and Depression n=78 Death or MI % ST Depression Only n=216 ST Elevation Only n=93 T Wave Inversion Only n=287 No ST or T Wave Change n=237 0 60 120 Nyman N, J Intern Med 1993; 234: 293 -301 180 Days 240 300 360
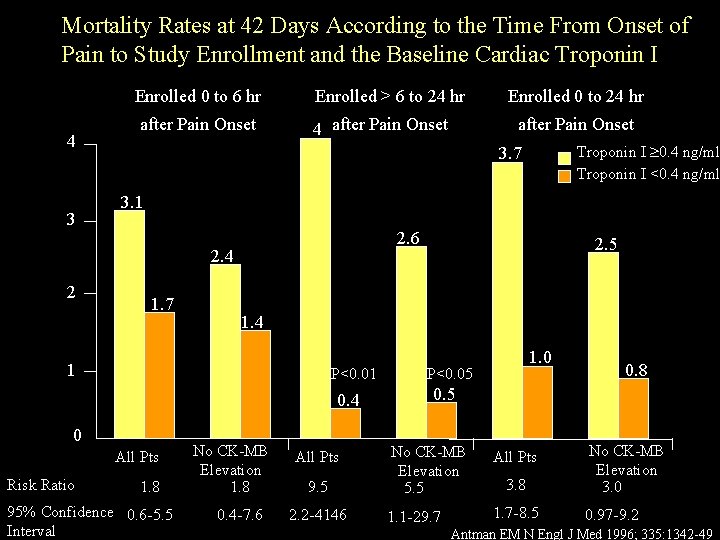
Mortality Rates at 42 Days According to the Time From Onset of Pain to Study Enrollment and the Baseline Cardiac Troponin I Enrolled 0 to 6 hr 4 3 after Pain Onset Enrolled > 6 to 24 hr 4 after Pain Onset Troponin I 0. 4 ng/ml Troponin I <0. 4 ng/ml 3. 1 2. 6 1. 7 P<0. 01 0. 4 0 All Pts 1. 8 95% Confidence 0. 6 -5. 5 Interval 2. 5 1. 4 1 Risk Ratio after Pain Onset 3. 7 2. 4 2 Enrolled 0 to 24 hr No CK-MB Elevation 1. 8 0. 4 -7. 6 All Pts 9. 5 2. 2 -4146 1. 0 P<0. 05 0. 8 0. 5 No CK-MB Elevation 5. 5 All Pts 1. 1 -29. 7 1. 7 -8. 5 3. 8 No CK-MB Elevation 3. 0 0. 97 -9. 2 Antman EM N Engl J Med 1996; 335: 1342 -49
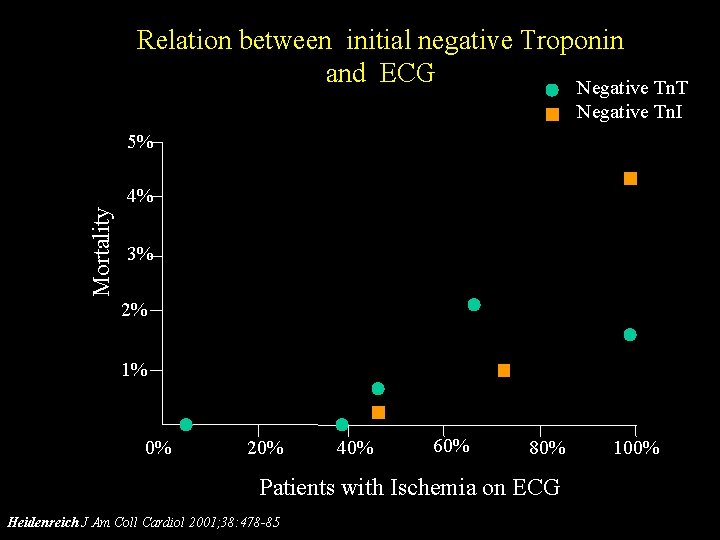
Relation between initial negative Troponin and ECG Negative Tn. T Negative Tn. I 5% Mortality 4% 3% 2% 1% 0% 20% 40% 60% 80% Patients with Ischemia on ECG Heidenreich J Am Coll Cardiol 2001; 38: 478 -85 100%
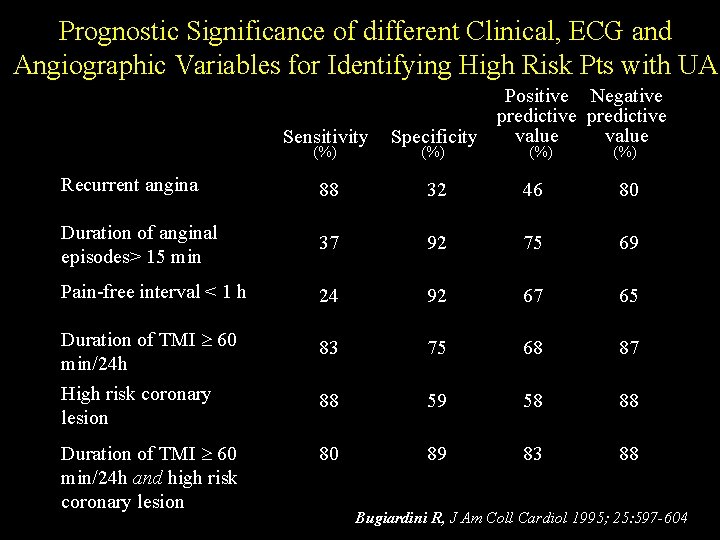
Prognostic Significance of different Clinical, ECG and Angiographic Variables for Identifying High Risk Pts with UA Sensitivity (%) Positive Negative predictive value Specificity (%) (%) Recurrent angina 88 32 46 80 Duration of anginal episodes> 15 min 37 92 75 69 Pain-free interval < 1 h 24 92 67 65 83 75 68 87 88 59 58 88 80 89 83 88 Duration of TMI 60 min/24 h High risk coronary lesion Duration of TMI 60 min/24 h and high risk coronary lesion Bugiardini R, J Am Coll Cardiol 1995; 25: 597 -604
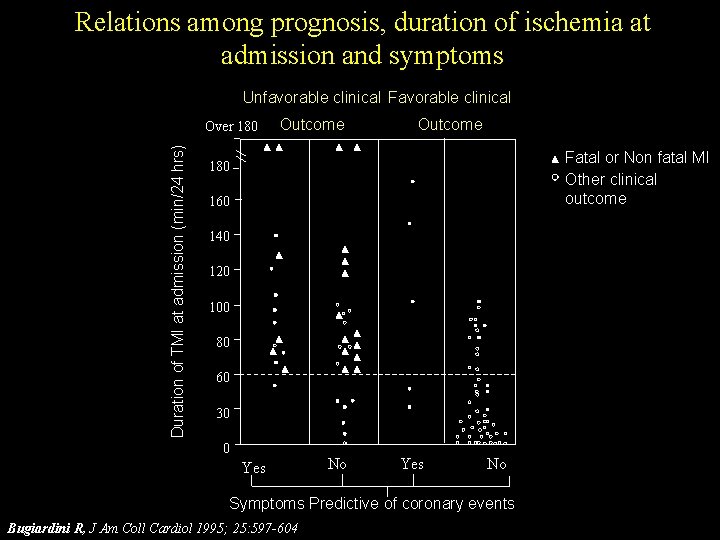
Relations among prognosis, duration of ischemia at admission and symptoms Unfavorable clinical Favorable clinical Duration of TMI at admission (min/24 hrs) Over 180 Outcome Fatal or Non fatal MI Other clinical outcome 180 160 140 120 100 80 60 30 0 Yes No Symptoms Predictive of coronary events Bugiardini R, J Am Coll Cardiol 1995; 25: 597 -604
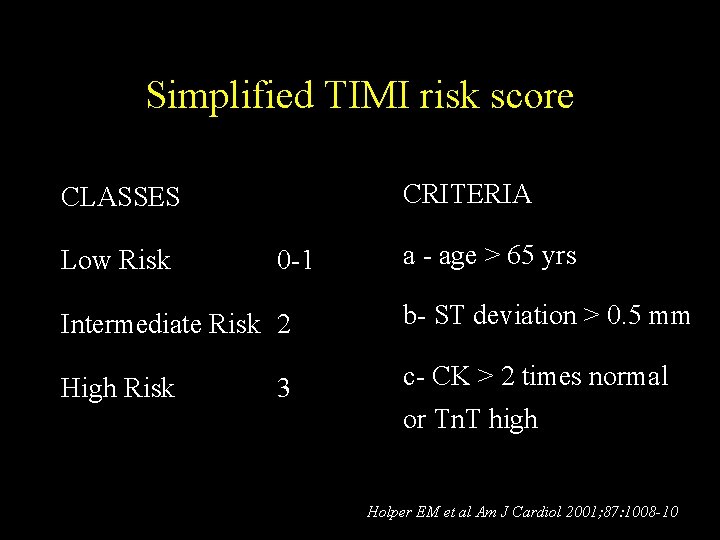

Simplified TIMI risk score CRITERIA CLASSES Low Risk 0 -1 a - age > 65 yrs Intermediate Risk 2 b- ST deviation > 0. 5 mm High Risk c- CK > 2 times normal 3 or Tn. T high Holper EM et al Am J Cardiol 2001; 87: 1008 -10
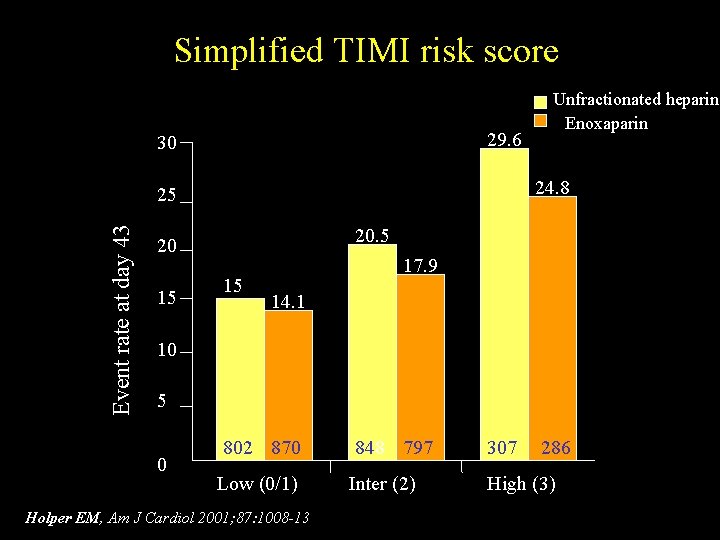
Simplified TIMI risk score 29. 6 30 24. 8 Event rate at day 43 25 20 15 Unfractionated heparin Enoxaparin 15 17. 9 14. 1 10 5 0 802 870 848 797 307 Low (0/1) Inter (2) High (3) Holper EM, Am J Cardiol 2001; 87: 1008 -13 286

NORMAL REST ECG Abnormal LVEF 2% Normal LVEF 98 % Am Heart J 2000: 139: 584
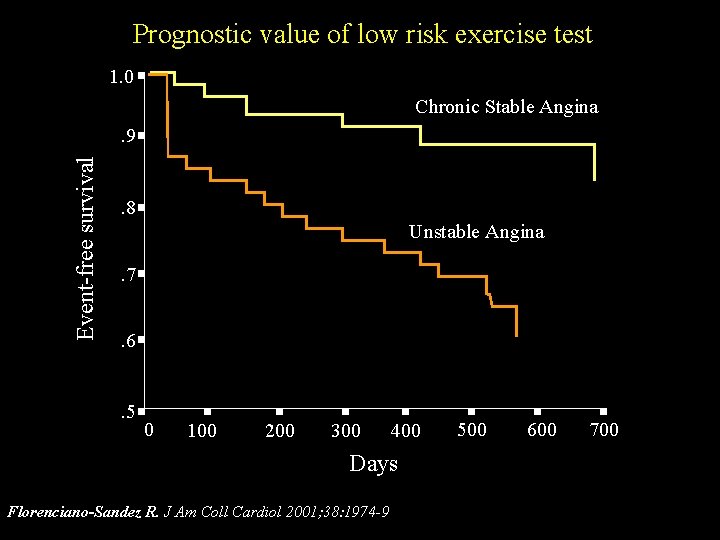
Prognostic value of low risk exercise test 1. 0 Chronic Stable Angina Event-free survival . 9. 8 Unstable Angina. 7. 6. 5 0 100 200 300 400 Days Florenciano-Sandez R. J Am Coll Cardiol 2001; 38: 1974 -9 500 600 700
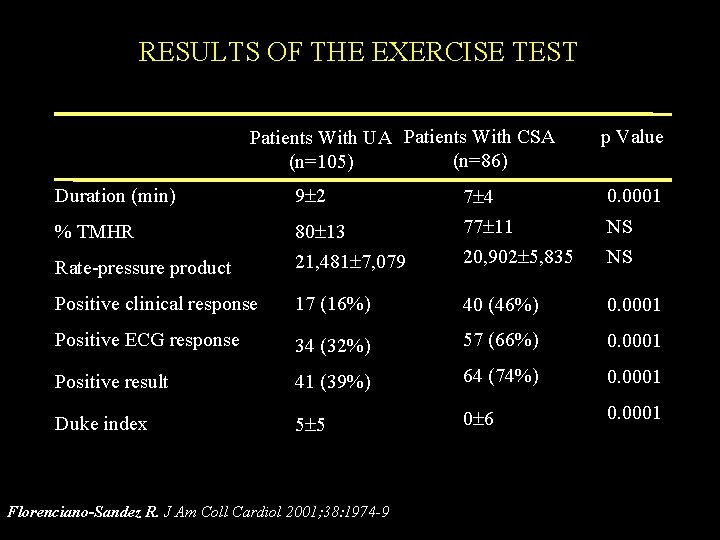
RESULTS OF THE EXERCISE TEST Patients With UA Patients With CSA (n=86) (n=105) Duration (min) 9 2 % TMHR 80 13 Rate-pressure product p Value 0. 0001 21, 481 7, 079 7 4 77 11 20, 902 5, 835 Positive clinical response 17 (16%) 40 (46%) 0. 0001 Positive ECG response 34 (32%) 57 (66%) 0. 0001 Positive result 41 (39%) 64 (74%) 0. 0001 Duke index 5 5 0 6 0. 0001 Florenciano-Sandez R. J Am Coll Cardiol 2001; 38: 1974 -9 NS NS

In patients with suspected ACS and negative ECG-Exercise Stress Test, physycians should proceede to pharmacological stress or cardiac scintigraphy.
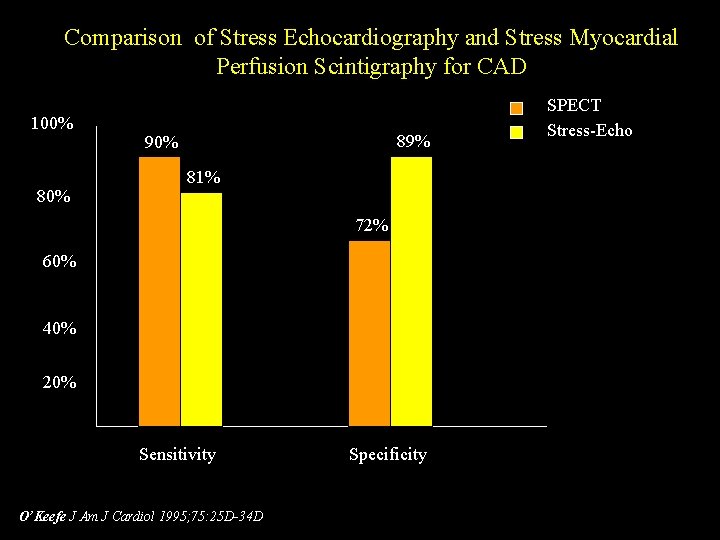
Comparison of Stress Echocardiography and Stress Myocardial Perfusion Scintigraphy for CAD 100% 89% 90% 81% 72% 60% 40% 20% Sensitivity O’Keefe J Am J Cardiol 1995; 75: 25 D-34 D Specificity SPECT Stress-Echo

Do not judge yourself harshly. Without mercy for ourselves we cannot love the world. The Buddha

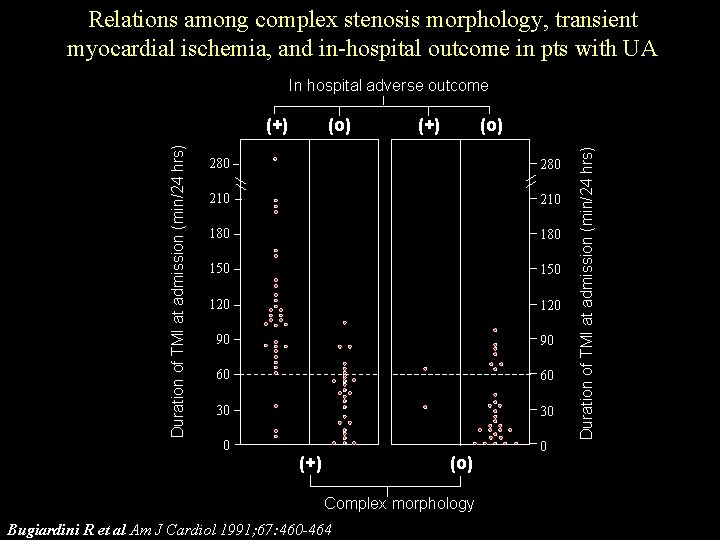
Relations among complex stenosis morphology, transient myocardial ischemia, and in-hospital outcome in pts with UA In hospital adverse outcome (o) (+) (o) 280 210 180 150 120 90 90 60 60 30 30 0 0 (+) (o) Complex morphology Bugiardini R et al Am J Cardiol 1991; 67: 460 -464 Duration of TMI at admission (min/24 hrs) (+)
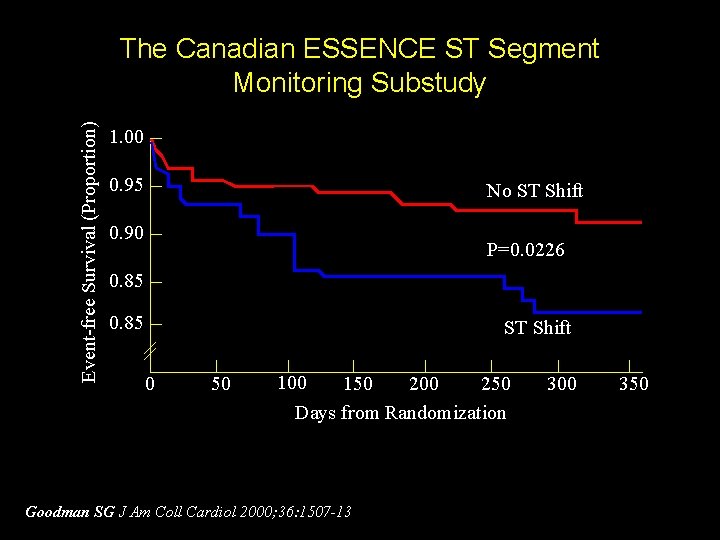
Event-free Survival (Proportion) The Canadian ESSENCE ST Segment Monitoring Substudy 1. 00 0. 95 No ST Shift 0. 90 P=0. 0226 0. 85 ST Shift 0 50 100 150 200 250 Days from Randomization Goodman SG J Am Coll Cardiol 2000; 36: 1507 -13 300 350
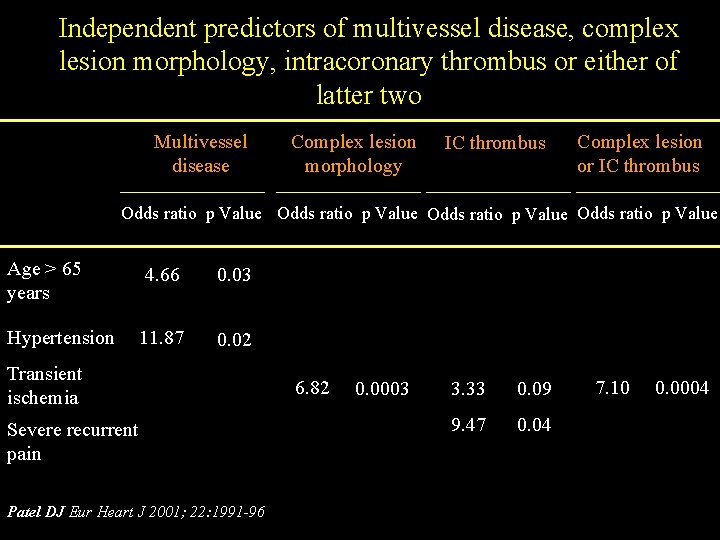

Independent predictors of multivessel disease, complex lesion morphology, intracoronary thrombus or either of latter two Multivessel disease Complex lesion morphology IC thrombus Complex lesion or IC thrombus Odds ratio p Value Age > 65 years 4. 66 0. 03 Hypertension 11. 87 0. 02 Transient ischemia Severe recurrent pain Patel DJ Eur Heart J 2001; 22: 1991 -96 6. 82 0. 0003 3. 33 0. 09 9. 47 0. 04 7. 10 0. 0004

If exercise ECG is so bloody good, why is it abnormal so infrequently during dobutamine echocardiography when ischemia (inducible wall motion abnormality) is present ?
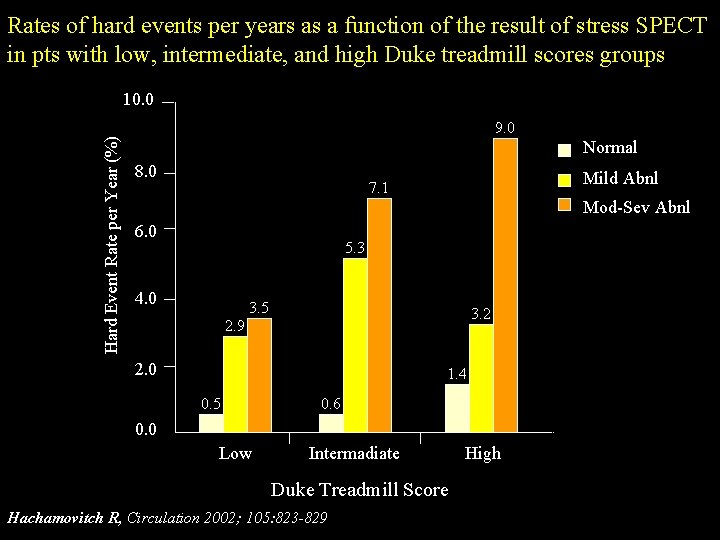
Rates of hard events per years as a function of the result of stress SPECT in pts with low, intermediate, and high Duke treadmill scores groups Hard Event Rate per Year (%) 10. 0 9. 0 Normal 8. 0 Mild Abnl 7. 1 Mod-Sev Abnl 6. 0 5. 3 4. 0 3. 5 3. 2 2. 9 2. 0 1. 4 0. 5 0. 6 0. 0 Low Intermadiate Duke Treadmill Score Hachamovitch R, Circulation 2002; 105: 823 -829 High
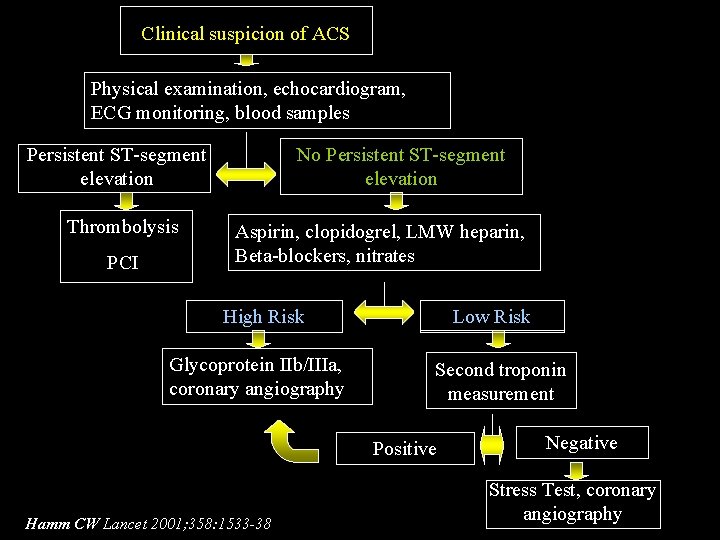
Clinical suspicion of ACS Physical examination, echocardiogram, ECG monitoring, blood samples Persistent ST-segment elevation Thrombolysis PCI No Persistent ST-segment elevation Aspirin, clopidogrel, LMW heparin, Beta-blockers, nitrates High Risk Glycoprotein IIb/IIIa, coronary angiography Low Risk Second troponin measurement Positive Hamm CW Lancet 2001; 358: 1533 -38 Negative Stress Test, coronary angiography

• Early Conservative Strategy? • Early Invasive Strategy?
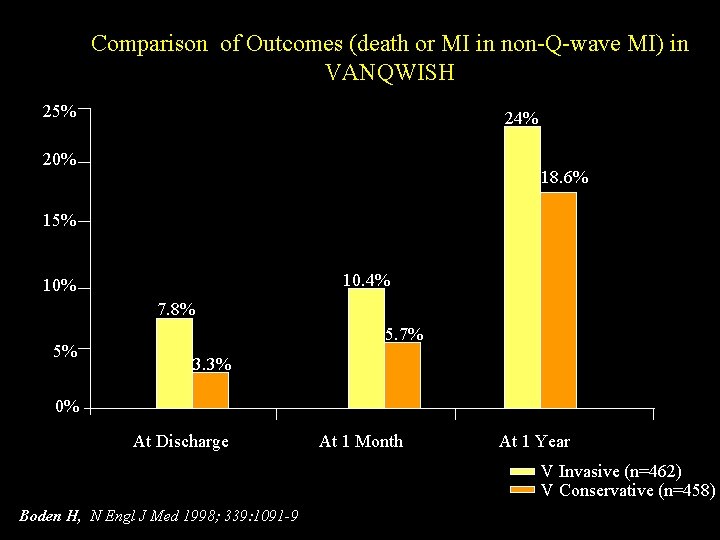
Comparison of Outcomes (death or MI in non-Q-wave MI) in VANQWISH 25% 24% 20% 18. 6% 15% 10. 4% 10% 7. 8% 5% 5. 7% 3. 3% 0% At Discharge At 1 Month At 1 Year V Invasive (n=462) V Conservative (n=458) Boden H, N Engl J Med 1998; 339: 1091 -9
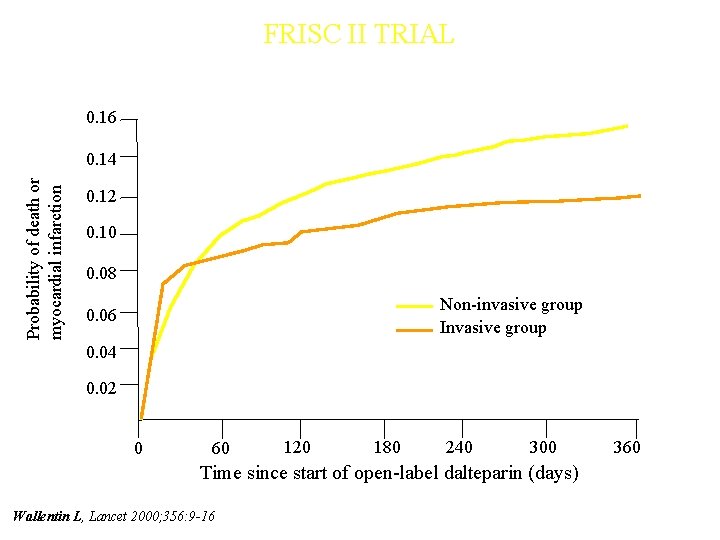
FRISC II TRIAL 0. 16 Probability of death or myocardial infarction 0. 14 0. 12 0. 10 0. 08 Non-invasive group Invasive group 0. 06 0. 04 0. 02 0 60 120 180 240 300 Time since start of open-label dalteparin (days) Wallentin L, Lancet 2000; 356: 9 -16 360

Early Invasive Strategy coronary angiography class I - Level Evidence A • Recurrent angina-ischemia at rest or with low level activities despite intensive anti-ischemic therapy • Elevated Tn. T or Tn. I • New or presumably new ST-segment depression • Recurrent angina/ischemia with CHF symptoms • High-risk findings on noninvasive stress testing • Depressed LV systolic function • Hemodynamic Instability • Sustained Ventricular Tachycardia • PCI within 6 months • Prior CABG ACC/AHA Practice Guidelines 2002

Early Conservative Strategy Coronary angiography is reserved for patients with: • Evidence of recurrent ischemia - angina at rest or with minimal activity - dynamic ST-segment changes • Strongly positive stress-test (despite vigorous medical therapy) ACC/AHA Practice Guidelines 2002

Early Invasive Strategy coronary angiography class I - Level Evidence A • Recurrent angina-ischemia at rest or with low level activities despite intensive anti-ischemic therapy • Elevated Tn. T or Tn. I • New or presumably new ST-segment depression • Recurrent angina/ischemia with CHF symptoms • High-risk findings on noninvasive stress testing • Depressed LV systolic function • Hemodynamic Instability • Sustained Ventricular Tachycardia • PCI within 6 months • Prior CABG ACC/AHA Practice Guidelines 2002
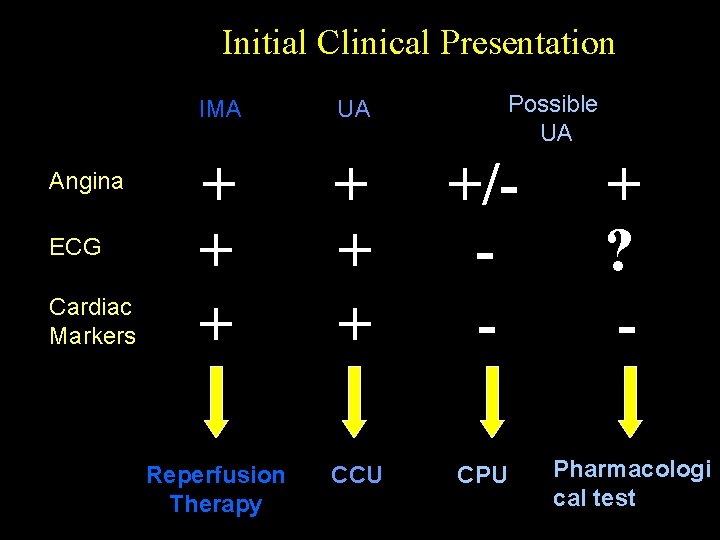
Initial Clinical Presentation Angina ECG Cardiac Markers Possible UA IMA UA + + + +/- Reperfusion Therapy CCU CPU + ? Pharmacologi cal test
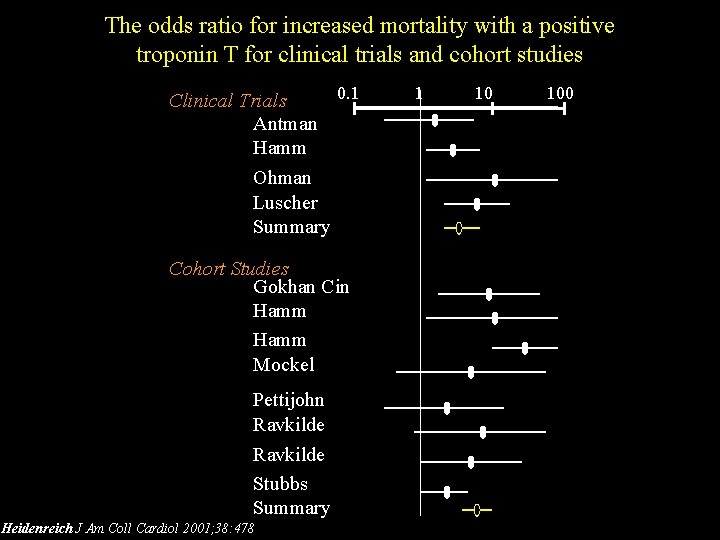
The odds ratio for increased mortality with a positive troponin T for clinical trials and cohort studies 0. 1 Clinical Trials Antman Hamm Ohman Luscher Summary Cohort Studies Gokhan Cin Hamm Mockel Pettijohn Ravkilde Stubbs Summary Heidenreich J Am Coll Cardiol 2001; 38: 478 -85 1 10 100
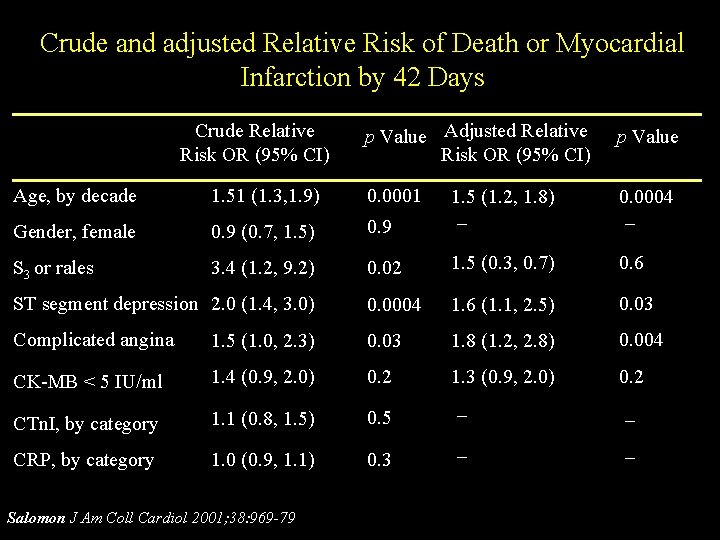
Crude and adjusted Relative Risk of Death or Myocardial Infarction by 42 Days Crude Relative Risk OR (95% CI) p Value Adjusted Relative Risk OR (95% CI) p Value 1. 5 (1. 2, 1. 8) _ 0. 0004 _ Age, by decade 1. 51 (1. 3, 1. 9) 0. 0001 Gender, female 0. 9 (0. 7, 1. 5) 0. 9 S 3 or rales 3. 4 (1. 2, 9. 2) 0. 02 1. 5 (0. 3, 0. 7) 0. 6 ST segment depression 2. 0 (1. 4, 3. 0) 0. 0004 1. 6 (1. 1, 2. 5) 0. 03 Complicated angina 1. 5 (1. 0, 2. 3) 0. 03 1. 8 (1. 2, 2. 8) 0. 004 CK-MB < 5 IU/ml 1. 4 (0. 9, 2. 0) 0. 2 CTn. I, by category 1. 1 (0. 8, 1. 5) 0. 5 1. 3 (0. 9, 2. 0) _ CRP, by category 1. 0 (0. 9, 1. 1) 0. 3 _ _ Salomon J Am Coll Cardiol 2001; 38: 969 -79 _

Why are the guidelines so misleading? • Composition of members • Selection bias • Peer pressure

The purpose of this study was to compare the effects of nitrates and calcium channel blockers on electrocardiografic (ECG) ischemia during exercise in a group of women admitted to our laboratories because of the occurrence of effort angina associated with ST depression. The results of this investigation demonstrate that simply acquired ECG variables during exercise stress testing on drugs contain diagnostic information, and may reflect the underlying pathogenetic substrate of angina.
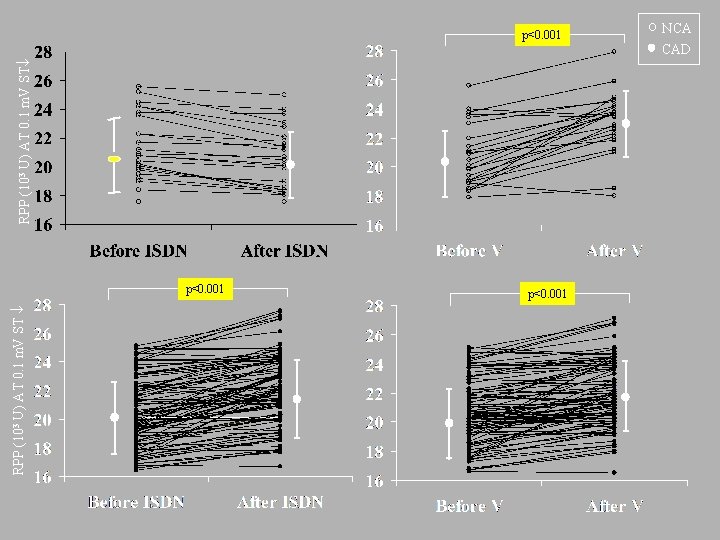
RPP (103 U) AT 0. 1 m. V ST p<0. 001 NCA CAD
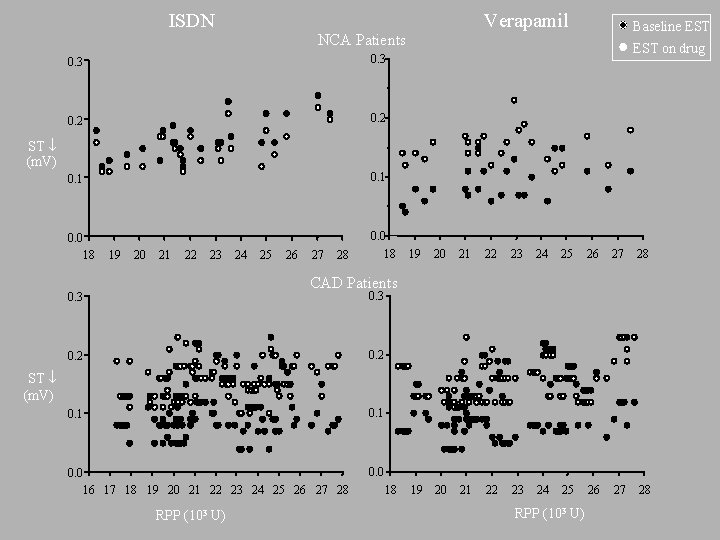
ISDN Verapamil NCA Patients 0. 3 0. 2 0. 1 0. 0 18 0. 0 Baseline EST on drug ST (m. V) 19 20 21 22 23 24 25 26 27 28 18 19 20 21 22 23 24 25 26 27 28 CAD Patients 0. 3 0. 2 0. 1 0. 0 16 17 18 19 20 21 22 23 24 25 26 27 28 0. 0 ST (m. V) RPP (103 U) 18 RPP (103 U)
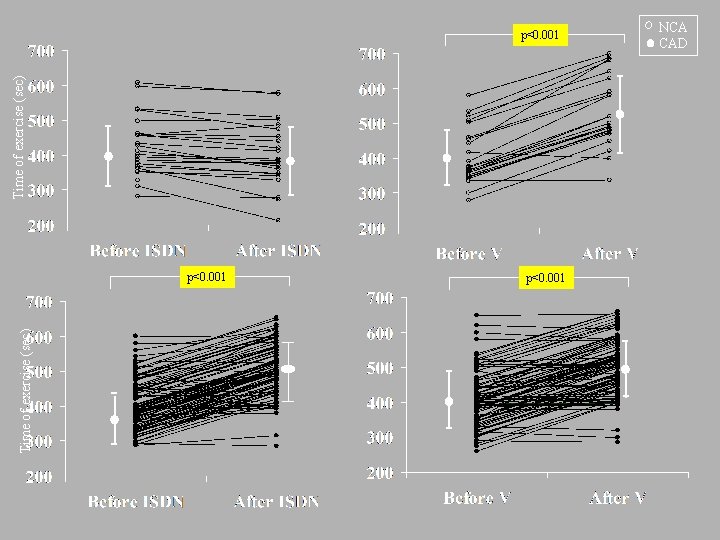
Time of exercise (sec) p<0. 001 NCA CAD
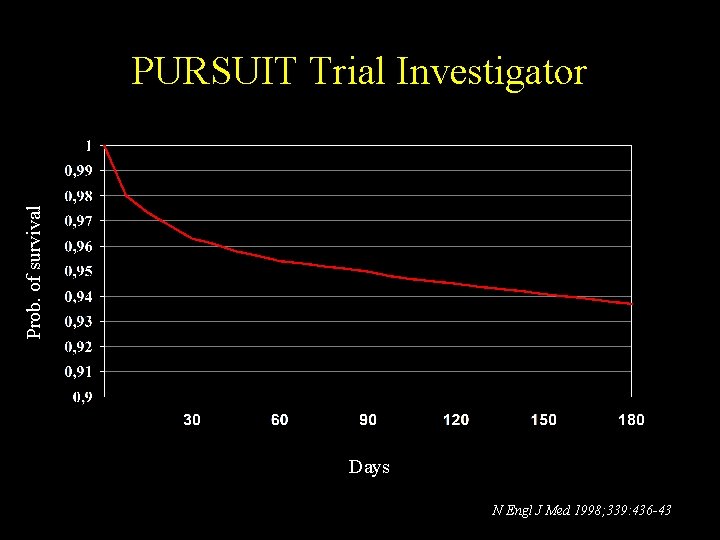
Prob. of survival PURSUIT Trial Investigator Days N Engl J Med 1998; 339: 436 -43
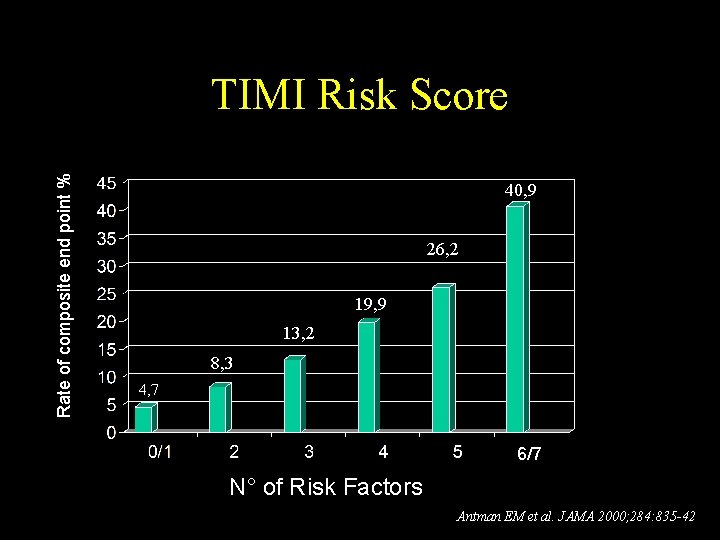
Rate of composite end point % TIMI Risk Score 40, 9 26, 2 19, 9 13, 2 8, 3 4, 7 6/7 N° of Risk Factors Antman EM et al. JAMA 2000; 284: 835 -42
- Slides: 49