Management of ovarian cysts Dr Matt Hewitt Benign

Management of ovarian cysts Dr Matt Hewitt

Benign Ovarian cysts • e. g functional cysts, serous cystademonas, dermoid (teratoma) Malignant • • Epithelial tumours 90% - e. g serous cystadenoacrcinomas Sex cord tumours Germ cell tumours Metastatic Non ovarian • e. g Hydrosalpinx, tubovarian abcess
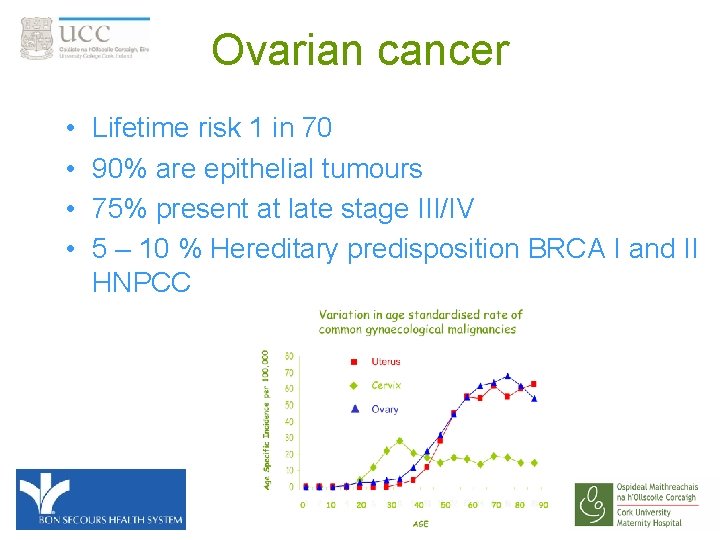
Ovarian cancer • • Lifetime risk 1 in 70 90% are epithelial tumours 75% present at late stage III/IV 5 – 10 % Hereditary predisposition BRCA I and II HNPCC
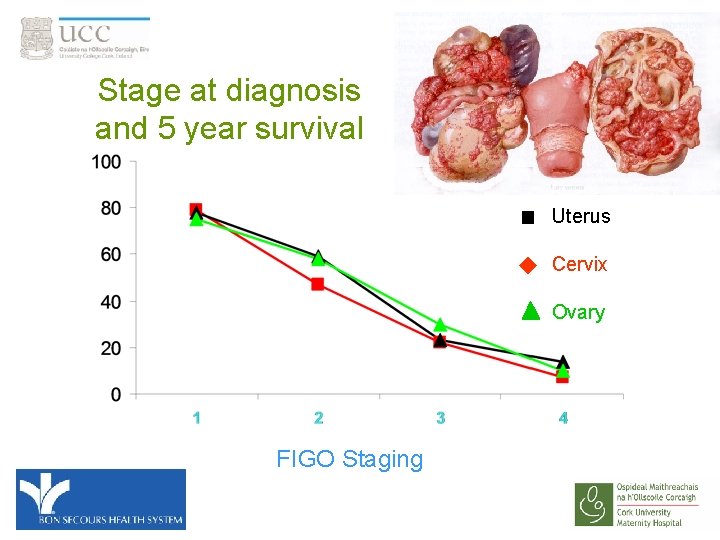
Stage at diagnosis and 5 year survival Uterus Cervix Ovary FIGO Staging

Pre menopausal ovarian cysts • 10% of women will undergo ovarian surgery at some point • Symptomatic cysts 1 to 3 1000 population • Simple cysts < 5 cm usually resolve, do not require follow up • PCO on scan do not require follow up scan

Post menopausal cysts • Increasing detection of ovarian cysts • 21% have abnormal ovarian pathology • Simple Cysts <5 cm – low risk of malignancy

Clinical examination • • • If its palpable it needs surgery Ascites Tenderness Fixed Differentiating between uterus and ovarian mass

Imaging Ultrasound – good assessment of the ovary and presence of ascites MRI – good but expensive assessment of ovary – Rarely gives additional information on nature of cyst – Is good in CT scan – not good at evaluating cyst - good in presence of ascites
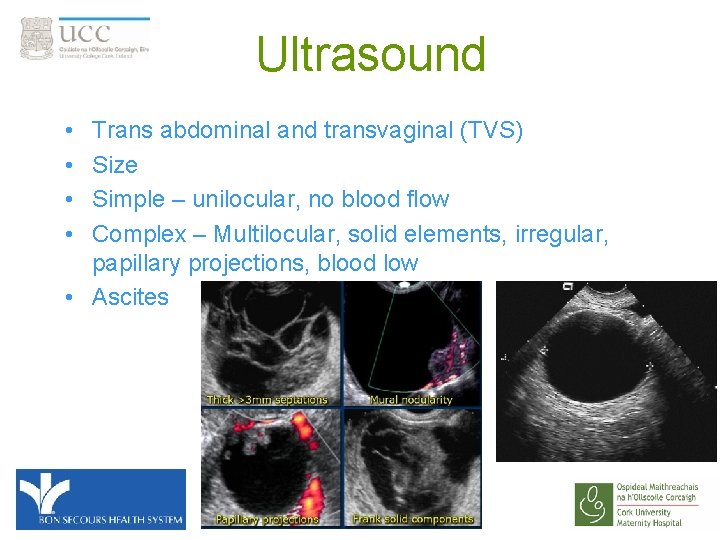
Ultrasound • • Trans abdominal and transvaginal (TVS) Size Simple – unilocular, no blood flow Complex – Multilocular, solid elements, irregular, papillary projections, blood low • Ascites

Tumour markers • Ca 125 – not sensitive and not specific – Should not be used in assessment of abdominal pain • h. CG, α-FP, LDH – Should not routinely be used – Secondary care assessment germ cell tumours
Surgical management • • • Laparoscopy – up to 12 cm Laparotomy Cystectomy – if confident not malignant Unilateral oophorectomy Bilateral oophorectomy

WHO Principles of Screening Diagnostic test • • sensitive and specific simple and cheap safe and acceptable reliable Disease • • serious high prevalence of preclinical stage natural history understood lead time bias, length bias Diagnosis & Treatment • facilities are adequate • effective, acceptable, safe treatment available
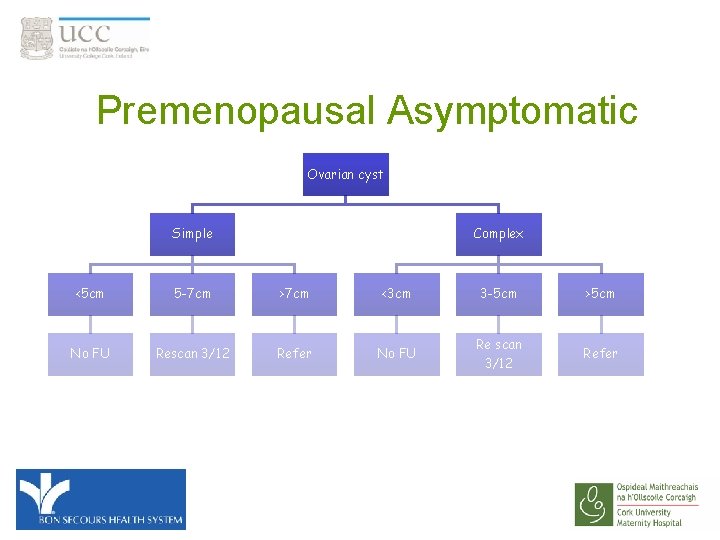
Premenopausal Asymptomatic Ovarian cyst Simple Complex <5 cm 5 -7 cm >7 cm <3 cm 3 -5 cm >5 cm No FU Rescan 3/12 Refer No FU Re scan 3/12 Refer
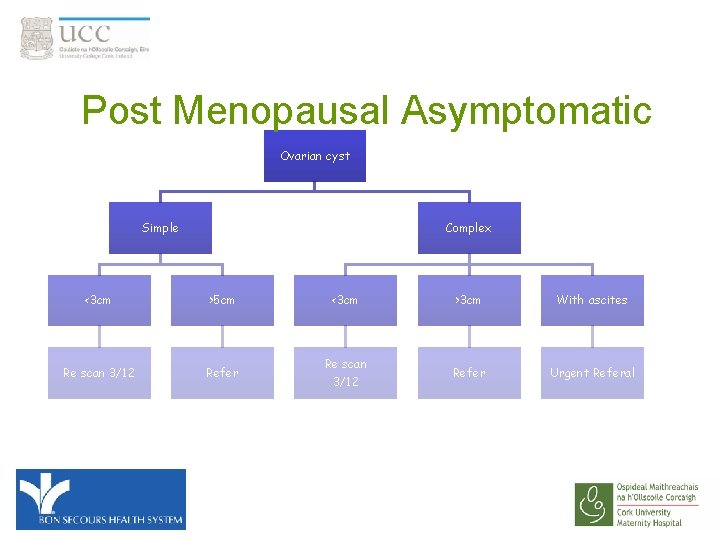
Post Menopausal Asymptomatic Ovarian cyst Simple Complex <3 cm >5 cm Re scan 3/12 Refer <3 cm Re scan 3/12 >3 cm With ascites Refer Urgent Referal
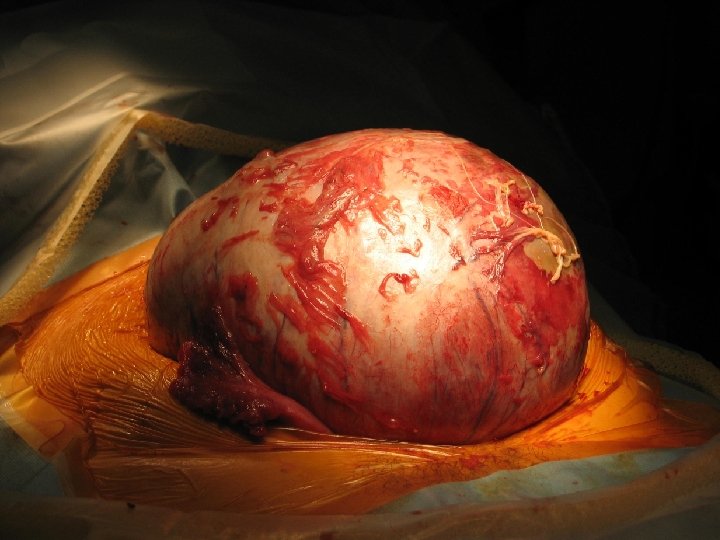
Thank you
- Slides: 15