Management of Neuropsychological Issues in Concussion Rehabilitation Role

Management of Neuropsychological Issues in Concussion Rehabilitation

Role of Case Management in m. TBI Treatment Bill Kerrigan, LGSW, CBIS Case Manager Department of Physical Medicine & Rehabilitation

Disclosures • I have no conflicts to disclose

Objectives At the end of this session, participants will be able to: • Define mild traumatic brain injury (m. TBI) • Describe psychosocial stressors associated with m. TBI and their potential impact on recovery • Describe critical role of case management in care plan of a person with m. TBI

Concussion: Myths and Truths True or False? • Cognitive complaints associated with concussion are common 3 months after injury • A concussion can occur without a direct blow to the head or loss of consciousness • Stress can negatively affect concussion recovery

Concussion: Myths and Truths True or False? • When individuals present with chronic complaints, abnormal scores on neuropsychological testing, or both, these findings are most likely caused by factors other than concussion • Terms “concussion” and “mild traumatic brain injury” are synonymous

Defining Concussion/m. TBI • Concerns – Multiple definitions across medical literature – Public misconceptions in defining concussion. – Merriam-Webster: a stunning, damaging, or shattering effect from a hard blow; especially: a jarring injury of the brain resulting in disturbance of cerebral function

VA/Do. D Clinical Practice Guideline A traumatic brain injury (TBI) is defined as a traumatically induced structural injury and/or physiologic disruption of brain function as a result of an external force. External forces may include any of the following events: – the head being struck by an object – the head striking an object – the brain undergoing acceleration/deceleration movement without direct external trauma to the head – a foreign body penetrating the brain – forces generated from events such as a blast or explosion, or other forces
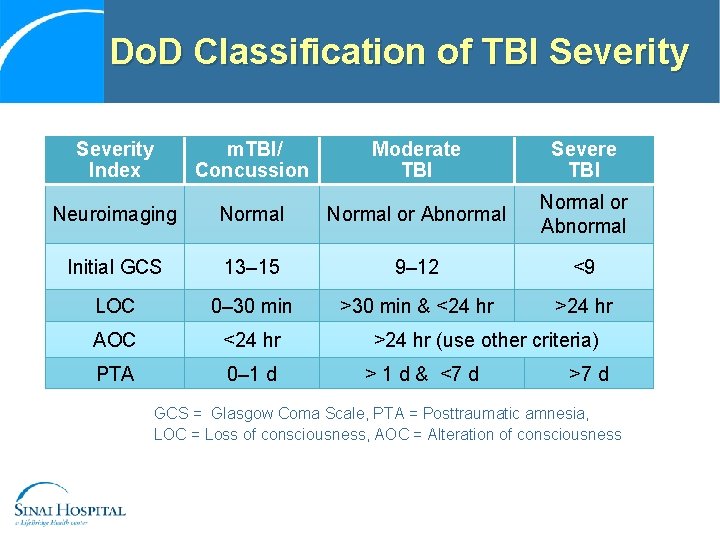

Do. D Classification of TBI Severity Index m. TBI/ Concussion Moderate TBI Severe TBI Neuroimaging Normal or Abnormal Initial GCS 13– 15 9– 12 <9 LOC 0– 30 min >30 min & <24 hr >24 hr AOC <24 hr PTA 0– 1 d >24 hr (use other criteria) > 1 d & <7 d >7 d GCS = Glasgow Coma Scale, PTA = Posttraumatic amnesia, LOC = Loss of consciousness, AOC = Alteration of consciousness

Benefits of the Case Management Model • Every patient in the Mild Brain Injury Program (MBIP) at Life. Bridge is assigned a case manager • Serve as primary contact/advocate for patients • Set positive tone for treatment • Provide education and information to patients, families, and funders • Assist individuals in navigating rehabilitation process • Provide documentation for work and academic accommodations as needed

Initial Case Management Intake • Introduction, explain the role of case management • Obtain demographic information • Obtain information related to the injury • Discuss current symptoms and obtain relevant medical history
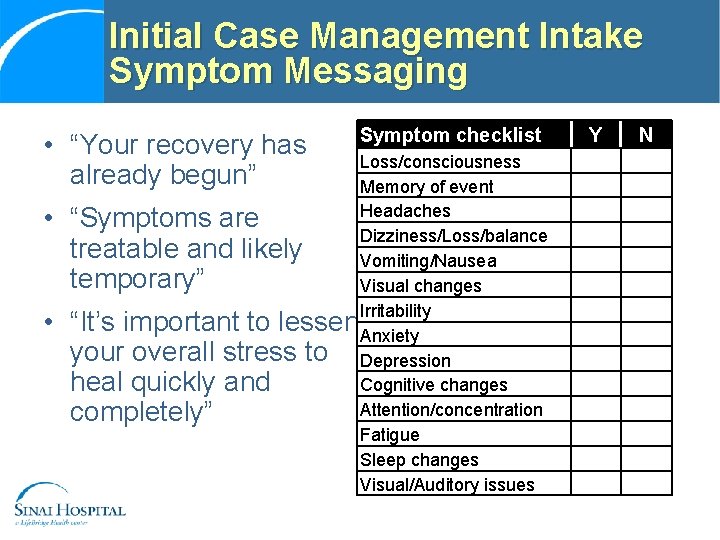
Initial Case Management Intake Symptom Messaging • “Your recovery has already begun” • • Symptom checklist Loss/consciousness Memory of event Headaches “Symptoms are Dizziness/Loss/balance treatable and likely Vomiting/Nausea temporary” Visual changes “It’s important to lessen Irritability Anxiety your overall stress to Depression heal quickly and Cognitive changes Attention/concentration completely” Fatigue Sleep changes Visual/Auditory issues Y N
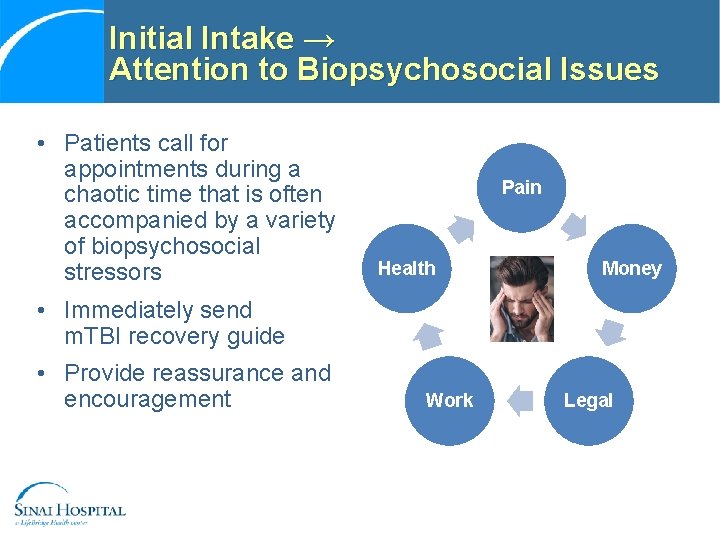
Initial Intake → Attention to Biopsychosocial Issues • Patients call for appointments during a chaotic time that is often accompanied by a variety of biopsychosocial stressors Pain Health Money • Immediately send m. TBI recovery guide • Provide reassurance and encouragement Work Legal

Understanding Patient Population • As of October 1, 2017, intakes completed on 715 patients • Average age: 37. 3 • Gender: 59% female; 41% male • Injury acuity: 45% <28 days after injury 55% >28 days after injury
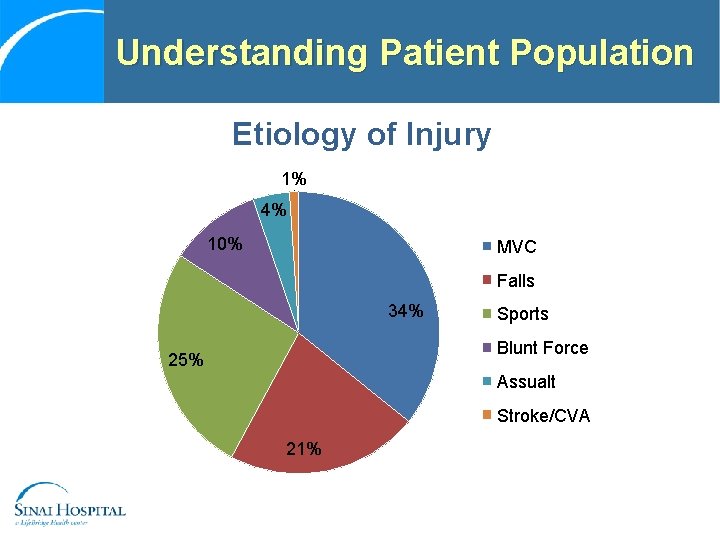
Understanding Patient Population Etiology of Injury 1% 4% 10% MVC Falls 34% Sports Blunt Force 25% Assualt Stroke/CVA 21%

Today’s Case Study You remember John Date of Birth 10/22/76 Age 40 Primary Insurance Work Comp Carrier Injury History Injury Date: Treatment Sought: Urgent Care December 2017 Injury Type: Member ID Specifics: Source One Comp Symptom Immediate FALL ly Labc-Onset: Patient was driven to urgent care – Q 119993393 no ambulance Injury Notes: Patient had a fall while on a job site, no LOC. Patient slipped on a wet floor and struck the back of his head on concrete. Attempted to return to work a few days following the fall – was not successful due to increase in symptoms.

Case Study- Symptom checklist Y N Loss/consciousness Memory of event Headaches Dizziness/Loss/balance Vomiting/Nausea Visual changes Irritability Anxiety Depression Cognitive changes Attention/concentration Fatigue Sleep changes Visual/Auditory issues X X X X X Psychosocial Notes: Patient has increased financial stress; has not returned to work. Short-term disability will soon expire. Case has recently been accepted by workers comp carrier. Patient has been sleeping more and states since not working has increased consumption of alcohol.

Details from John’s Intake • 40 y/o male, fell while working on the job (Work Comp Case) • Initially seen at Express Care, diagnosed with a concussion Was referred to MBIP but decided not to pursue • Tried returning to work a few days after fall, was not successful • No care for a few weeks following fall; sleeps in often and has increased Et. OH • 3 months after injury, connects with case manager at m. TBI program

Comprehensive Management of Mild TBI

Disclosures • I have no conflicts to disclose

Objectives At the end of this session, participants will be able to: • Describe natural history of m. TBI recovery • Differentiate various factors that can cause persistent symptoms • Summarize components of a thorough m. TBI medical evaluation • To understand the interplay between symptoms after concussion • To recognize circumstances in which referral for health and behavior intervention, neuropsychological testing, or neuropsychiatric consultation would be appropriate

TRAUMATIC IMPACT m. TBI-Causes TRAUMATIC INERTIAL Brain moves within skull § § § Falls Vehicular accidents Sports-related accidents Primary Causes – Acceleration-deceleration – Striking head against hard surface – Blasts or explosions 3/12/2018 Contact Injury Head struck by or against an object § § Blast-related assaults Falls Vehicular accidents Sports accidents
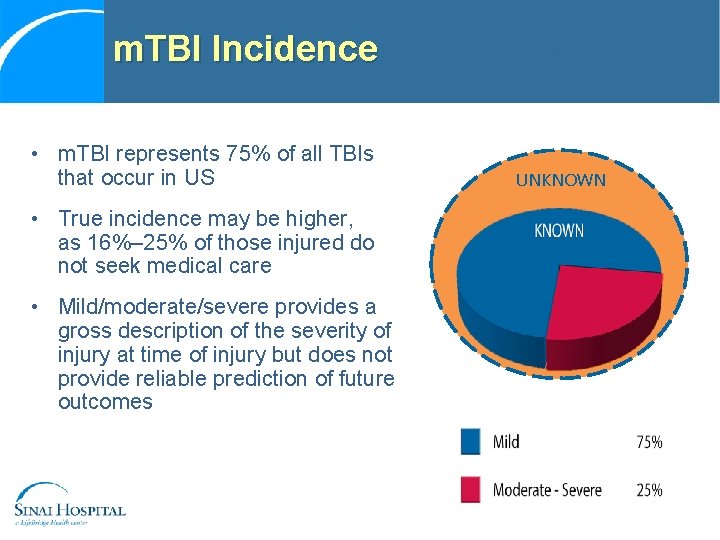
m. TBI Incidence • m. TBI represents 75% of all TBIs that occur in US • True incidence may be higher, as 16%– 25% of those injured do not seek medical care • Mild/moderate/severe provides a gross description of the severity of injury at time of injury but does not provide reliable prediction of future outcomes UNKNOWN

Physiology & Biochemistry Natural History of Concussion & Expected Course of Recovery
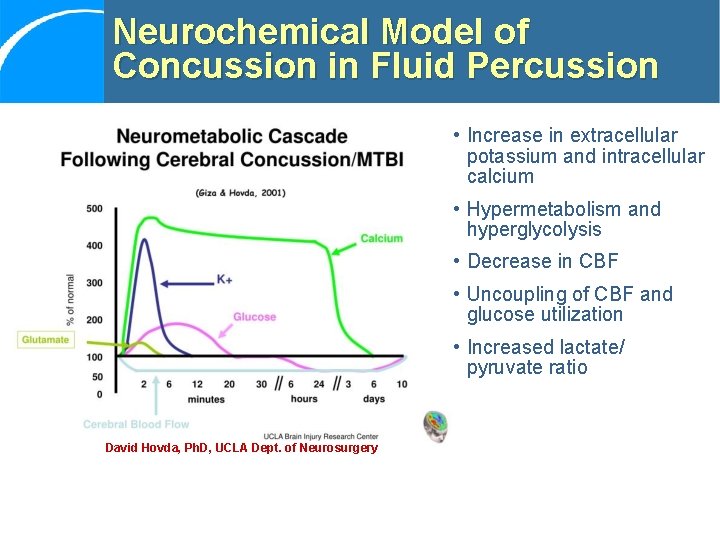
Neurochemical Model of Concussion in Fluid Percussion • Increase in extracellular potassium and intracellular calcium • Hypermetabolism and hyperglycolysis • Decrease in CBF • Uncoupling of CBF and glucose utilization • Increased lactate/ pyruvate ratio David Hovda, Ph. D, UCLA Dept. of Neurosurgery

Biochemical Cascade
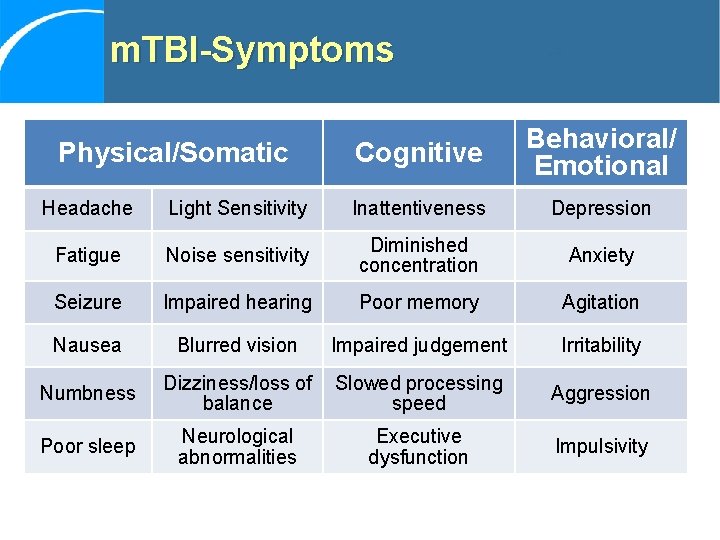
m. TBI-Symptoms Physical/Somatic Cognitive Behavioral/ Emotional Headache Light Sensitivity Inattentiveness Depression Fatigue Noise sensitivity Diminished concentration Anxiety Seizure Impaired hearing Poor memory Agitation Nausea Blurred vision Impaired judgement Irritability Numbness Poor sleep Dizziness/loss of Slowed processing balance speed Neurological abnormalities Executive dysfunction Aggression Impulsivity

m. TBI-Initial Symptoms • Most symptoms resolve in 2– 4 weeks – Only 10 -15% of people experience persistent problems after one month Symptoms are considered nonspecific § Cognitive changes may be subtle §

Patient Assessment

Patient Assessment • History of Present Illness • Accident background Ø Ø Mechanism of injury Loss of consciousness and its duration Posttraumatic amnesia and its duration Initial treatment and imaging • Pertinent medical and social history • Current symptoms • Physical

Our Patient, John • Mr. Smith is a 40 yo male who sustained a fall 2 months prior to visit while going down a flight of stairs at work, causing him to hit the back of his head • No loss of consciousness • No posttraumatic amnesia • Did note initial confusion/alteration of consciousness • Presented to the ED and underwent head CT, which was negative

Take-Home Point John’s injury would be classified as at least moderate traumatic brain injury moderate if any positive structural imaging findings were identified

John’s Treatment Since Injury, Prior to 1 st Visit • Attempted to return to work a few days after injury, which resulted in increased symptoms (which we will discuss) • Has seen his PCP, who provided a note to be off work • Was prescribed Vicodin and cyclobenzaprine, which he is taking 3 x/day, resulting in his being sleepy most of the day

Pertinent History Past Medical/Surgical History Family History Social History

Pertinent History Past medical and surgical history • Any prior TBIs • History of psychiatric disorders • Headaches • Learning disorder such as ADHD Family history • Migraine headaches or neurological or psychological issues

Pertinent History Social History • Substance use • Home situation • Occupation • Level of education • Hobbies • Social support

John’s History Past medical/past surgical history • “low mood” • Hypertension Family history • Migraine headaches

John’s History Social history • Drinks alcohol socially, but has been drinking daily now • Works as an accountant and completed a master’s degree • Lives with his spouse, who works during the day in a multilevel home • Is an avid runner and has completed Iron. Man triathlons

Current Symptoms Self-Report Forms Interview

Neurobehavioral Symptom Inventory Cicerone KD, Kalmar K. Persistent postconcussion syndrome: The structure of subjective complaints after mild traumatic brain injury. J Head Trauma Rehab, 1995 Please rate the following symptoms with regard to how much they have disturbed you IN THE LAST 2 WEEKS. 0 = None – Rarely if ever present; not a problem at all 1 = Mild – Occasionally present, but it does not disrupt my activities; I can usually continue what I’m doing; doesn’t really concern me 2 = Moderate – Often present, occasionally disrupts my activities; I can usually continue what I’m doing with some effort; I feel somewhat concerned 3 = Severe – Frequently present and disrupts activities; I can only do things that are fairly simple or take little effort; I feel I need help 4 = Very Severe – Almost always present, and I have been unable to perform at work, school, or home due to this problem; I probably cannot function without help
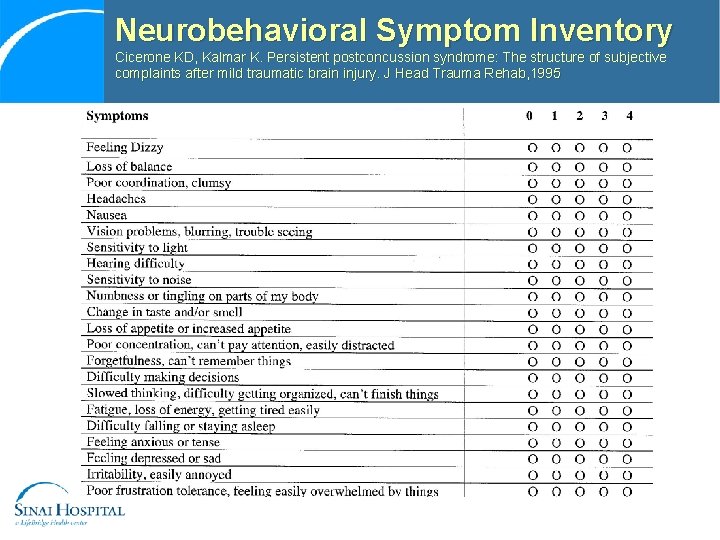
Neurobehavioral Symptom Inventory Cicerone KD, Kalmar K. Persistent postconcussion syndrome: The structure of subjective complaints after mild traumatic brain injury. J Head Trauma Rehab, 1995

Neurobehavioral Symptom Inventory Cicerone KD, Kalmar K. Persistent postconcussion syndrome: The structure of subjective complaints after mild traumatic brain injury. J Head Trauma Rehab, 1995 Vestibular/Somatic Symptoms ● Feeling dizzy ● Loss of balance ● Poor coordination, clumsy

Neurobehavioral Symptom Inventory Cicerone KD, Kalmar K. Persistent postconcussion syndrome: The structure of subjective complaints after mild traumatic brain injury. J Head Trauma Rehab, 1995 Somatic Symptoms ● ● ● ● ● Headaches Nausea Vision problems, blurring, trouble seeing Sensitivity to light Hearing difficulty Sensitivity to noise Numbness or tingling on part of my body Change in taste and/or smell Loss of appetite or increased appetite

Neurobehavioral Symptom Inventory Cicerone KD, Kalmar K. Persistent postconcussion syndrome: The structure of subjective complaints after mild traumatic brain injury. J Head Trauma Rehab, 1995 Cognitive Symptoms ● Poor concentration, can’t pay attention, easily distracted ● Forgetfulness, can’t remember things ● Difficulty making decisions ● Slowed thinking, difficulty getting organized, can’t finish things

Neurobehavioral Symptom Inventory Cicerone KD, Kalmar K. Persistent postconcussion syndrome: The structure of subjective complaints after mild traumatic brain injury. J Head Trauma Rehab, 1995 Affective Symptoms ● ● ● Fatigue, loss of energy, getting tired easily Difficulty falling or staying asleep Feeling anxious or tense Irritability, easily annoyed Poor frustration tolerance, feeling easily overwhelmed by things
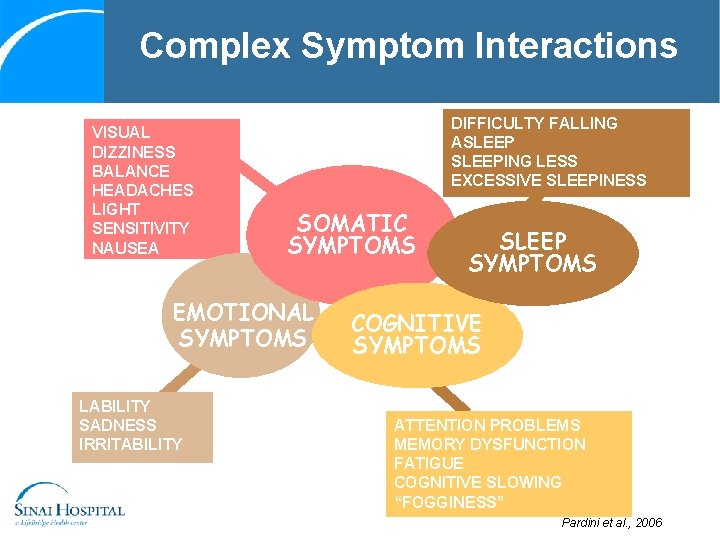
Complex Symptom Interactions VISUAL DIZZINESS BALANCE HEADACHES LIGHT SENSITIVITY NAUSEA PAIN DIFFICULTY FALLING ASLEEPING LESS EXCESSIVE SLEEPINESS SOMATIC SYMPTOMS EMOTIONAL SYMPTOMS LABILITY SADNESS IRRITABILITY SLEEP SYMPTOMS COGNITIVE SYMPTOMS ATTENTION PROBLEMS MEMORY DYSFUNCTION FATIGUE COGNITIVE SLOWING “FOGGINESS” Pardini et al. , 2006

Key Look for the codes listed below that indicate circumstances in which the following referrals could be appropriate: H&B NP NT — — — Health and behavior intervention Neuropsychiatry Neuropsychological testing
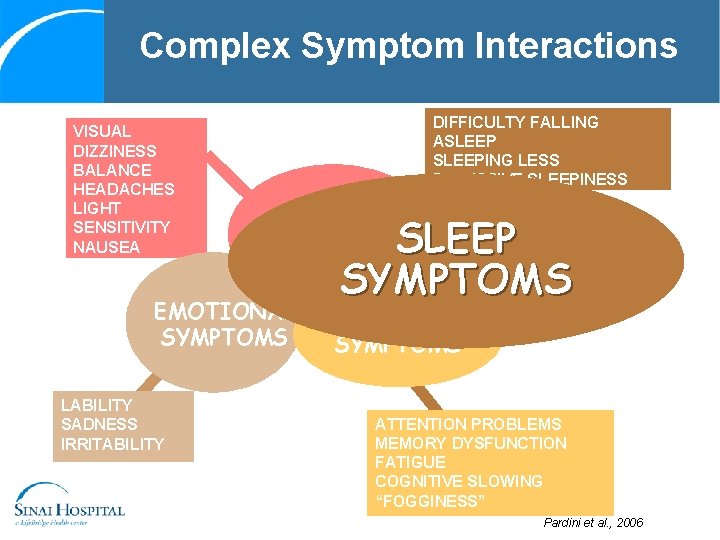
Complex Symptom Interactions VISUAL DIZZINESS BALANCE HEADACHES LIGHT SENSITIVITY NAUSEA PAIN DIFFICULTY FALLING ASLEEPING LESS EXCESSIVE SLEEPINESS SOMATIC SYMPTOMS EMOTIONAL SYMPTOMS LABILITY SADNESS IRRITABILITY SLEEP SYMPTOMS COGNITIVE SYMPTOMS ATTENTION PROBLEMS MEMORY DYSFUNCTION FATIGUE COGNITIVE SLOWING “FOGGINESS” Pardini et al. , 2006

Sleep • Sleep initiation • Sleep maintenance • Naps • Reasons for interrupted sleep • Apneic episodes

Epworth Sleepiness Scale • 0– 5: Lower normal daytime sleepiness • 6– 10: Higher normal daytime sleepiness • 11– 12: Mild excessive daytime sleepiness • 13– 15: Moderate excessive daytime sleepiness • 16– 24: Severe excessive daytime sleepiness http: //epworthsleepinessscale. com/

Sleep Disturbances: John • It takes him 2 hr to fall asleep because he re-lives the injury (H&B) and has persistent neck pain and headaches • Wakes up multiples times throughout the night because of nightmares (NP)(H&B) • Takes two 3 -hr naps during the day, because of grogginess from his medication (H&B)
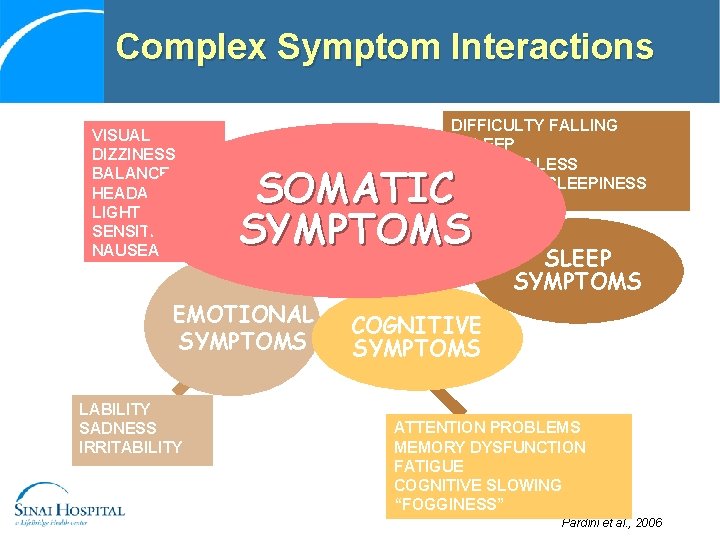
Complex Symptom Interactions VISUAL DIZZINESS BALANCE HEADACHES LIGHT SENSITIVITY NAUSEA PAIN SOMATIC SYMPTOMS EMOTIONAL SYMPTOMS LABILITY SADNESS IRRITABILITY DIFFICULTY FALLING ASLEEPING LESS EXCESSIVE SLEEPINESS SLEEP SYMPTOMS COGNITIVE SYMPTOMS ATTENTION PROBLEMS MEMORY DYSFUNCTION FATIGUE COGNITIVE SLOWING “FOGGINESS” Pardini et al. , 2006

Somatic Symptoms Pain (OPQRST) • O: onset • P: provocation and palliation • Q: quality • R: region and radiation • S: severity • T: timing

Somatic Symptoms • Dizziness • Light headed • Balance disturbance • Numbness/tingling/weakness • Vision: blurred and/or double • Light sensitivity • Sound sensitivity • Tinnitus or hearing loss

Somatic Symptoms: John Headaches and neck pain • Started the day of accident • Worse with physical and cognitive activity • Better with rest • Described as pressure • Located along occipital region/upper cervical region and radiates to forehead

Somatic Symptoms: John • Poor balance and dizziness with quick movements and when walking down busy hallway, which makes him fearful that he will fall again, causing him to eliminate all activity (H&B) • Light and sound sensitivity • Bilateral tinnitus • Blurred and double vision worse when looking at screens
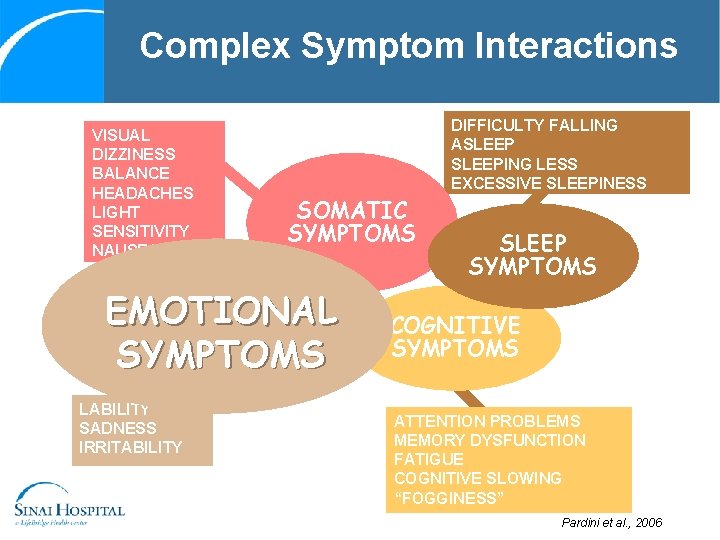
Complex Symptom Interactions VISUAL DIZZINESS BALANCE HEADACHES LIGHT SENSITIVITY NAUSEA PAIN DIFFICULTY FALLING ASLEEPING LESS EXCESSIVE SLEEPINESS SOMATIC SYMPTOMS EMOTIONAL SYMPTOMS LABILITY SADNESS IRRITABILITY SLEEP SYMPTOMS COGNITIVE SYMPTOMS ATTENTION PROBLEMS MEMORY DYSFUNCTION FATIGUE COGNITIVE SLOWING “FOGGINESS” Pardini et al. , 2006

Emotional Symptoms • • Anxiety Depression Emotional lability Panic attacks Irritability Avoiding activity and isolation Perseveration on symptoms
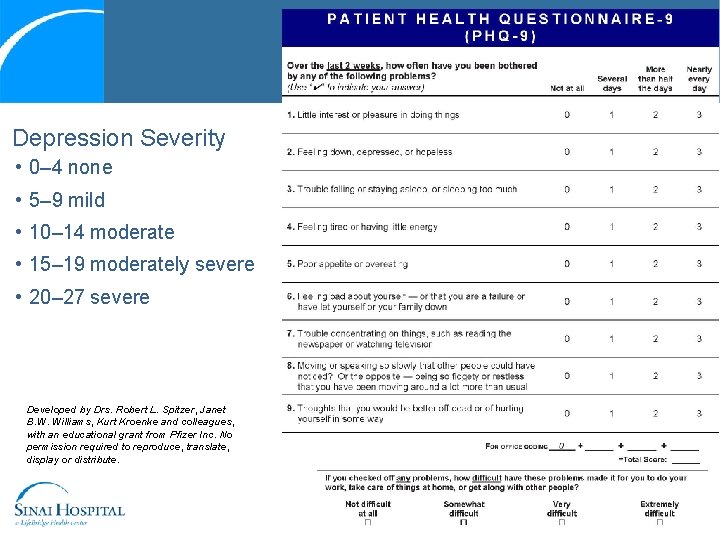
Depression Severity • 0– 4 none • 5– 9 mild • 10– 14 moderate • 15– 19 moderately severe • 20– 27 severe Developed by Drs. Robert L. Spitzer, Janet B. W. Williams, Kurt Kroenke and colleagues, with an educational grant from Pfizer Inc. No permission required to reproduce, translate, display or distribute.

Emotional Symptoms: John • Has history of “low mood, ” which has gotten worse since the accident (NP) • Is anxious about falling again and is only staying on first level of his home to avoid using stairs (H&B) • Spouse reports that he is more irritable than normal and will shout for seemingly no reason (H&B) • Is fearful that he will never get better (H&B)
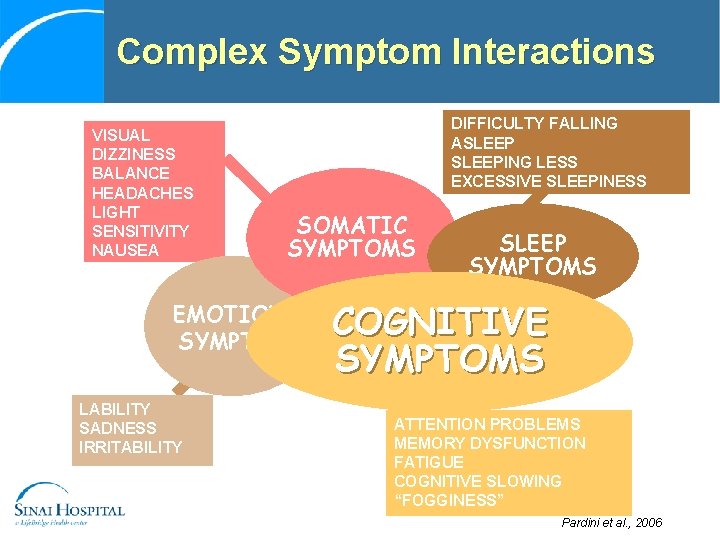
Complex Symptom Interactions VISUAL DIZZINESS BALANCE HEADACHES LIGHT SENSITIVITY NAUSEA PAIN DIFFICULTY FALLING ASLEEPING LESS EXCESSIVE SLEEPINESS SOMATIC SYMPTOMS EMOTIONAL SYMPTOMS LABILITY SADNESS IRRITABILITY SLEEP SYMPTOMS COGNITIVE SYMPTOMS ATTENTION PROBLEMS MEMORY DYSFUNCTION FATIGUE COGNITIVE SLOWING “FOGGINESS” Pardini et al. , 2006

Cognitive Symptoms • Concentration • Memory • Cognitive “fog” • Fatigue • Mental processing speed • Difficulty completing tasks

Cognitive Symptoms: John • Poor concentration and decreased mental processing speed (NT) • Made multiple mistakes at work and was confronted by his boss (NT) • Misplaces keys and one time accidentally put them in trashcan • Notes word-finding difficulty (NT) • Feels like he is in a mental “fog”

Physical Exam

Physical Exam • General appearance • Affect • Neurological Exam • Vestibular ocular motor screen test • Head Impulse Test • Balance • DON’T FORGET TO LOOK AT THE NECK

Physical Exam • Neurological Exam – Cranial Nerves – Manual muscle testing – Sensory exam – Reflexes
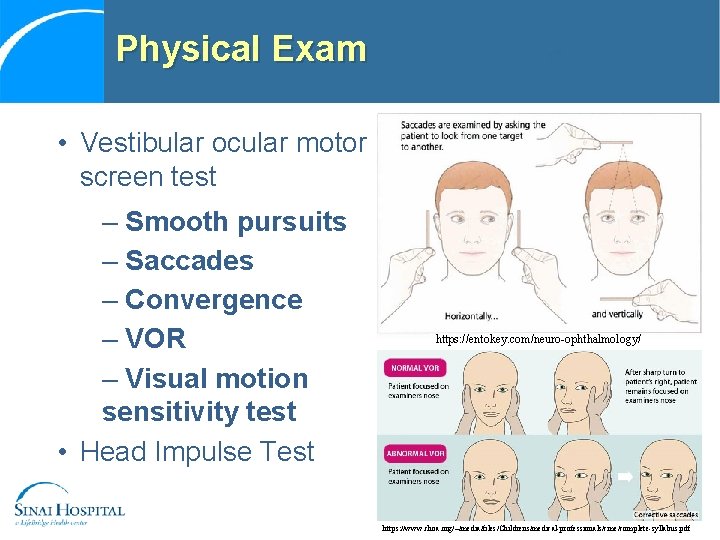
Physical Exam • Vestibular ocular motor screen test – Smooth pursuits – Saccades – Convergence – VOR – Visual motion sensitivity test • Head Impulse Test https: //entokey. com/neuro-ophthalmology/ https: //www. choa. org/~/media/files/Childrens/medical-professionals/cme/complete-syllabus. pdf
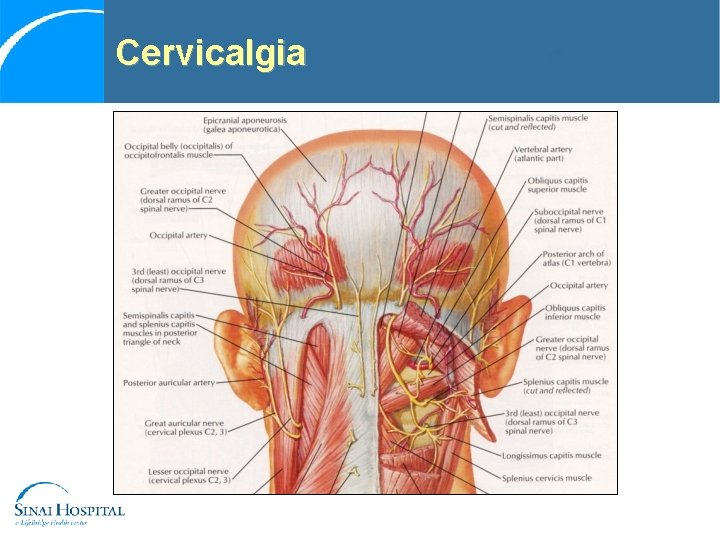
Cervicalgia

Take-Home Point Interplay among symptoms is complex interplay Health and behavior intervention, neuropsychological testing, and neuropsychiatric consultation are essential to help disentangle the interplay
- Slides: 69