Management of Lower Urinary Tract Trauma A Practical













































- Slides: 49

Management of Lower Urinary Tract Trauma – A Practical Perspective Jeremy Grummet St Vincent’s Hospital Melbourne


Scenario 1 l Called l Male, to ED at 2 am to see Mr F-W 30 l Buck’s night for mate at Amanda’s Steak and Grill

Scenario 1 l Decided to drive home thinking only had 6 beers in 4 hrs l Forgot about Depth Charges in each one l Mistook phone booth for freeway entrance

Scenario 1 l Slight confusion (shaving cream and cups) l Stable: BP 110/70, HR 100 l Suprapubic pain, tender D

Scenario 1 l IDC had been inserted by ED staff l Gross l PXR haematuria in bag shows stable pelvic #

Scenario 1 l Suspect LUT injury Order cystogram l Radiology reg: Cystogram NAD, presumed bladder contusion l Admit for observation

Scenario 1 l 3 days later, more generalised abdo pain l Continued gross haematuria l Febrile l Rigid abdomen l Exploratory laparotomy

Scenario 1 l Intraperitoneal bladder rupture l Infected urine l Repaired l SPC l No other injury found

Scenario 1 l IV AB l Prolonged ileus l TPN l D/C 3 weeks later

Issues Raised Initial assessment l Investigation l Treatment

Initial Assessment l When suspect LUT trauma, must bear in mind: l Risk of multiple trauma l Anatomical sites l Mechanism of injury l Physical signs l Safety of catheterisation

Risk of Multiple Trauma l Bladder trauma series of 51 pts: l Mortality 22% (Carroll 1984) l None due to bladder injury itself l Must suspect other life-threatening injuries l E. g. Massive haemorrhage 2° to unstable pelvic #

Anatomical Sites l Bladder l Posterior l Anterior urethra (prostatic/membranous) urethra (distal to urogenital diaphragm)

Mechanism of Injury l Blunt vs Penetrating l Implications for further assessment l Blunt far more common – 66 -88% in US bladder studies (Carroll 1984, Cass 1987) – Likely more so in Australia (100% - small series) (Chan 1994)

Blunt Bladder Trauma Mechanism l 85 -90% bladder rupture pelvic # (Morey 2001) l Usu. burst or shear (intra- and extraperitoneal (Corriere 1988) l Occ. 2° to spicules from pelvic # if extraperitoneal l MVA, esp. if been drinking l Fall from height

Posterior Urethra Trauma Mechanism l Blunt pelvic # l Membranous urethra passes through urogenital diaphragm attached to pubic rami l Shear usu. at prostatomembranous junction

Anterior Urethra Trauma Mechanism l More common than posterior urethra trauma l Straddle injuries, e. g. fall off bicycle l “Common in Texas if pt is kicked with the toe of a boot” (Campbell’s Urology) l Urethra crushed against inf. symphysis

LUT Physical Signs l Gross haematuria l Pelvic # – 15% all pelvic # bladder/urethra injury l Inability to void l Suprapubic tenderness

LUT Physical Signs l Blood at meatus l Perineal l High swelling/haematoma riding prostate or indistinct landmarks on PR exam

LUT Physical Signs l Problems (not covered well in texts): l Signs alert you to LUT injury, but do not differentiate well between bladder and urethra l E. g. Inability to void

LUT Physical Signs l Absence of a sign does not always exclude LUT injury l E. g. Does pt with pelvic # and unable to void but no other signs have urethral injury?

LUT Physical Signs l Cannot determine ability to void when pt obtunded – head trauma – intoxication l How to assess for haematuria in such a pt?

Catheterisation l Often not a priority in trauma setting l Risk: Conversion of partial urethral tear to complete l When safe if suspect LUT trauma?

Catheterisation l When NOT safe: l Blood at meatus l Pelvic # + gross haematuria/unable to void/perineal haematoma (Chan 1994)

Investigations l CXR, l RUG PXR indicated when catheterisation unsafe l 20 -30 ml water-soluble contrast

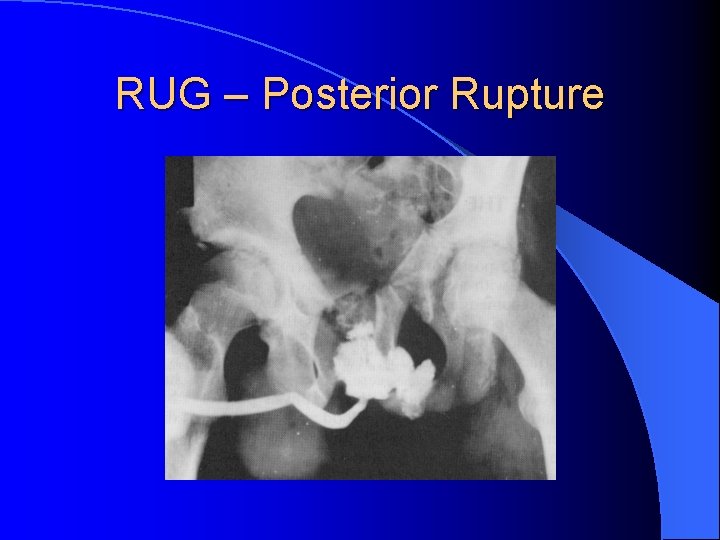
RUG – Posterior Rupture

RUG – Disrupted Diaphragm

Cystography l Performed retrograde l Commonly preceded by RUG l Indications controversial l A former recommendation: all trauma pts with macro- or micro-haematuria (Cass 1987)

Cystography l Problems: – Pts in series not stratified to blunt vs penetrating – Not stratified by degree of haematuria – 2/3 pts had bladder contusion only – Expensive

Cystography l More recent studies show that in pts with pelvic #, risk of bladder rupture if: – Gross haematuria: 13 -55% – Microscopic haematuria: 0 -1% l (True for blunt trauma, but lower threshold if penetrating)

Cystography l Current absolute indication for blunt trauma cystography: pelvic # + gross haematuria (Morey 2001) l Softer indications: e. g. micro-haematuria in combination with suprapubic tenderness and inability to void

Cystography l Technique crucial l Papers advise at least 250 -300 ml contrast l Less may not expand bladder enough to open up tear l Post-drainage film l Filling film may obscure extravasation

Types of Bladder Rupture l As mentioned before, intra-and extraperitoneal l Extra-peritoneal l Occ. combined twice as common

Extra-peritoneal Rupture

Extra-peritoneal Rupture

Intra-peritoneal Rupture

CT Cystography l Appears to be as good as cystography l Indicated when injury to other abdominal organs also suspected l Again, must ensure adequate distension with contrast l Conventional cystography still preferred when only looking for bladder rupture

IVP l When unable to perform cystography due to urethral injury l Still need to exclude concomitant bladder trauma IVP

Treatment – Intraperitoneal Bladder Rupture l Surgery l Transperitoneal l Keep l Use repair suprapubic cystostomy extraperitoneal absorbable sutures

Treatment - Extraperitoneal Bladder Rupture l Controversial l Proponents of surgical repair: l Avoid pelvic haematoma l Repair intravesically – midline incision l Peritoneotomy

Treatment - Extraperitoneal Bladder Rupture l Other option is catheterisation only l Only if uninfected urine and no other reason for exploratory surgery l Series of 41 extraperitoneal ruptures l Healing in all pts with no complications (Corriere 1988)

Treatment – Posterior Urethral Injury l Highly controversial l Range from immediate repair to suprapubic cystostomy and delayed repair l In between, immediate urethral catheter railroading and delayed repair good results (Devine 1989) l Need urologist experienced in urethral reconstruction

Treatment – Anterior Urethral Injury l Suprapubic l Any cystostomy catheter strictures usu. not severe enough to warrant surgical reconstruction

Mr F-W l Similar presentation: l Haemodynamically stable l Too concussed/drunk to void l Tender suprapubically l Pelvic # on PXR

Mr F-W l You arrive before a catheter has been inserted l After l ABCs, how would you manage pt? Panel

Conclusions l Think of LUT trauma in the trauma pt l Conversely, suspect other more lifethreatening injuries in pt with LUT trauma, and manage accordingly

Conclusions l Never catheterise before obtaining a negative RUG when blood at meatus l Think carefully before catheterising when NO blood at meatus l Ensure proper cystography or CT cystography technique

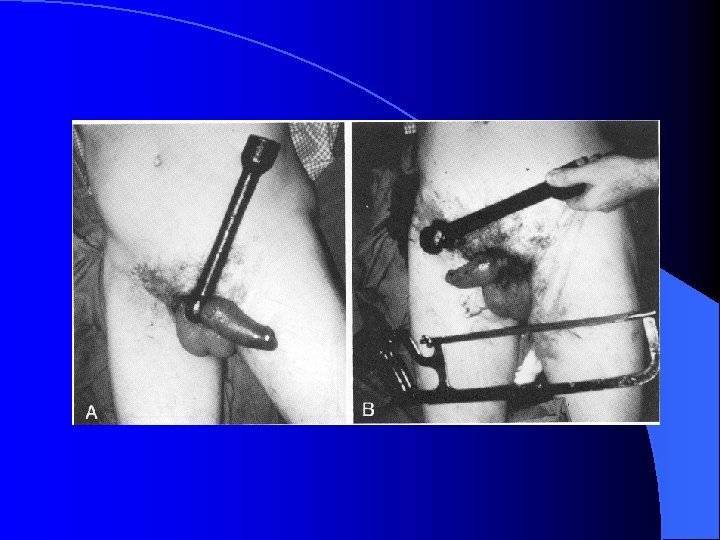
Conclusions l Refer to urologist preferably once LUT injury suspected, certainly for treatment l As a general rule, avoid instruments as shown at beginning of presentation