Management of Hyperglycemia in Type 2 Diabetes A

Management of Hyperglycemia in Type 2 Diabetes: A Patient-Centered Approach Position Statement of the American Diabetes Association (ADA) and the European Association for the Study of Diabetes (EASD) Diabetes Care 2012; 35: 1364– 1379 Diabetologia 2012; 55: 1577– 1596

Writing Group American Diabetes Association European Assoc. for the Study of Diabetes Richard M. Bergenstal MD Michaela Diamant MD, Ph. D John B. Buse MD, Ph. D Ele Ferrannini MD Anne L. Peters MD Michael Nauck MD Richard Wender MD Apostolos Tsapas MD, Ph. D Silvio E. Inzucchi MD (co-chair) David R. Matthews MD, DPhil (co-chair) Int’l Diabetes Center, Minneapolis, MN University of North Carolina, Chapel Hill, NC Univ. of Southern California, Los Angeles, CA Thomas Jefferson University, Philadelphia, PA Yale University, New Haven, CT VU University, Amsterdam, The Netherlands University of Pisa, Italy Diabeteszentrum, Bad Lauterberg, Germany Aristotle University, Thessaloniki, Greece Oxford University, Oxford, UK

ADA-EASD Position Statement: Management of Hyperglycemia in T 2 DM: A Patient-Centered Approach 1. PATIENT-CENTERED APPROACH 2. BACKGROUND • Epidemiology and health care impact • Relationship of glycemic control to outcomes • Overview of the pathogenesis of Type 2 diabetes 3. ANTI-HYPERGLYCEMIC THERAPY • Glycemic targets • Therapeutic options - Lifestyle - Oral agents & non-insulin injectables - Insulin Diabetes Care 2012; 35: 1364– 1379 Diabetologia 2012; 55: 1577– 1596

ADA-EASD Position Statement: Management of Hyperglycemia in T 2 DM: A Patient-Centered Approach 3. ANTIHYPERGLYCEMIC THERAPY • Implementation Strategies - Initial drug therapy - Advancing to dual combination therapy - Advancing to triple combination therapy - Transitions to and titrations of insulin 4. OTHER CONSIDERATIONS • • Age Weight Sex/racial/ethnic/genetic differences Comorbidities (Coronary artery disease, Heart failure, Chronic kidney disease, Liver dysfunction, Hypoglycemia) 5. FUTURE DIRECTIONS / RESEARCH NEEDS Diabetes Care 2012; 35: 1364– 1379 Diabetologia 2012; 55: 1577– 1596

ADA-EASD Position Statement: Management of Hyperglycemia in T 2 DM 1. Patient-Centered Approach “. . . providing care that is respectful of and responsive to individual patient preferences, needs, and values - ensuring that patient values guide all clinical decisions. ” • Gauge patient’s preferred level of involvement. • Explore, where possible, therapeutic choices. • Utilize decision aids. • Shared decision making – final decisions re: lifestyle choices ultimately lie with the patient. Diabetes Care 2012; 35: 1364– 1379 Diabetologia 2012; 55: 1577– 1596

ADA-EASD Position Statement: Management of Hyperglycemia in T 2 DM 2. BACKGROUND • Epidemiology and health care impact Diabetes Care 2012; 35: 1364– 1379 Diabetologia 2012; 55: 1577– 1596
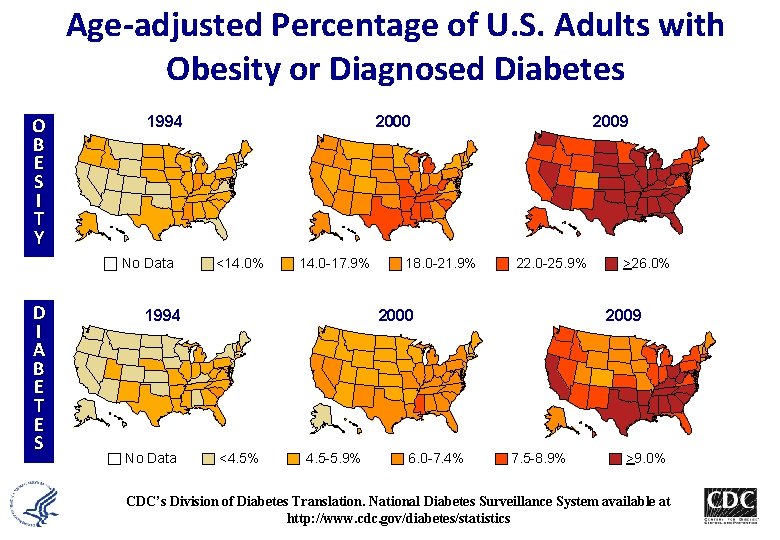
Age-adjusted Percentage of U. S. Adults with Obesity or Diagnosed Diabetes Obesity (BMI ≥ 30 kg/m 2) 1994 O 2000 2009 B E S I T Y No Data Diabetes D I A B E T E S <14. 0% 14. 0 -17. 9% 1994 No Data 18. 0 -21. 9% 22. 0 -25. 9% 2000 <4. 5% 4. 5 -5. 9% 6. 0 -7. 4% >26. 0% 2009 7. 5 -8. 9% >9. 0% CDC’s Division of Diabetes Translation. National Diabetes Surveillance System available at http: //www. cdc. gov/diabetes/statistics

The Diabetes Epidemic: Global Projections, 2010– 2030 IDF. Diabetes Atlas 5 th Ed. 2011

ADA-EASD Position Statement: Management of Hyperglycemia in T 2 DM 2. BACKGROUND • Relationship of glycemic control to outcomes Diabetes Care 2012; 35: 1364– 1379 Diabetologia 2012; 55: 1577– 1596
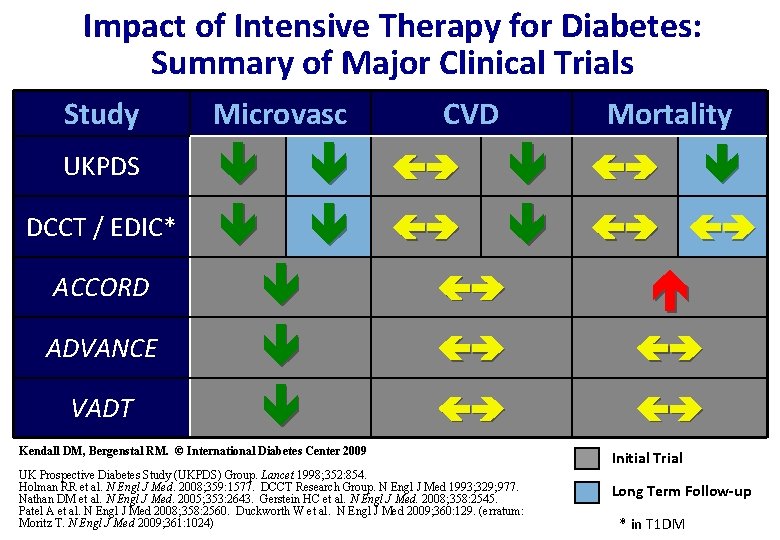
Impact of Intensive Therapy for Diabetes: Summary of Major Clinical Trials Study Microvasc UKPDS DCCT / EDIC* ACCORD ADVANCE VADT CVD Mortality Kendall DM, Bergenstal RM. © International Diabetes Center 2009 UK Prospective Diabetes Study (UKPDS) Group. Lancet 1998; 352: 854. Holman RR et al. N Engl J Med. 2008; 359: 1577. DCCT Research Group. N Engl J Med 1993; 329; 977. Nathan DM et al. N Engl J Med. 2005; 353: 2643. Gerstein HC et al. N Engl J Med. 2008; 358: 2545. Patel A et al. N Engl J Med 2008; 358: 2560. Duckworth W et al. N Engl J Med 2009; 360: 129. (erratum: Moritz T. N Engl J Med 2009; 361: 1024) Initial Trial Long Term Follow-up * in T 1 DM

ADA-EASD Position Statement: Management of Hyperglycemia in T 2 DM 2. BACKGROUND • Overview of the pathogenesis of T 2 DM - Insulin secretory dysfunction - Insulin resistance (muscle, fat, liver) - Increased endogenous glucose production - Deranged adipocyte biology - Decreased incretin effect Diabetes Care 2012; 35: 1364– 1379 Diabetologia 2012; 55: 1577– 1596
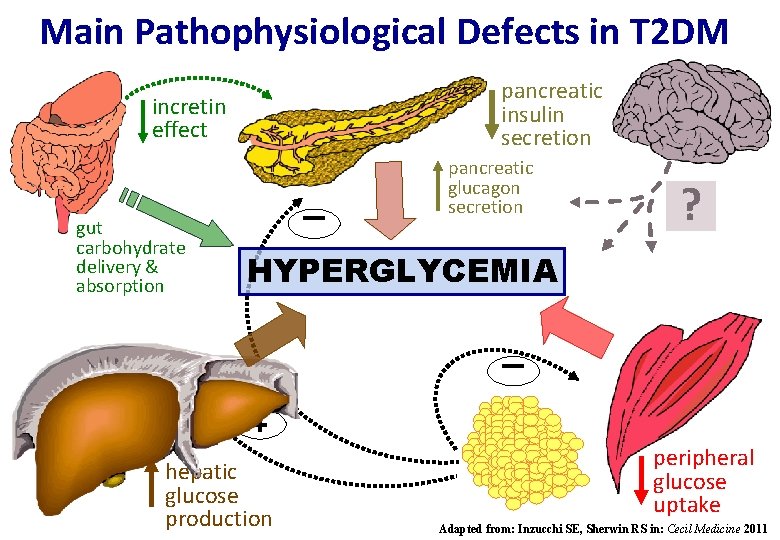
Main Pathophysiological Defects in T 2 DM pancreatic insulin secretion incretin effect - gut carbohydrate delivery & absorption pancreatic glucagon secretion ? HYPERGLYCEMIA + hepatic glucose production peripheral glucose uptake Adapted from: Inzucchi SE, Sherwin RS in: Cecil Medicine 2011

ADA-EASD Position Statement: Management of Hyperglycemia in T 2 DM 3. ANTI-HYPERGLYCEMIC THERAPY • Glycemic targets - Hb. A 1 c < 7. 0% (mean PG 150 -160 mg/dl [8. 3 -8. 9 mmol/l]) - Pre-prandial PG <130 mg/dl (7. 2 mmol/l) - Post-prandial PG <180 mg/dl (10. 0 mmol/l) - Individualization is key: Ø Tighter targets (6. 0 - 6. 5%) - younger, healthier Ø Looser targets (7. 5 - 8. 0%+) - older, comorbidities, hypoglycemia prone, etc. - Avoidance of hypoglycemia PG = plasma glucose Diabetes Care 2012; 35: 1364– 1379 Diabetologia 2012; 55: 1577– 1596

Figure 1 Diabetes Care 2012; 35: 1364– 1379 Diabetologia 2012; 55: 1577– 1596 (Adapted with permission from: Ismail-Beigi et al. Ann Intern Med 2011; 154: 554)

ADA-EASD Position Statement: Management of Hyperglycemia in T 2 DM 3. ANTI-HYPERGLYCEMIC THERAPY • Therapeutic options: Lifestyle - Weight optimization - Healthy diet - Increased activity level Diabetes Care 2012; 35: 1364– 1379 Diabetologia 2012; 55: 1577– 1596

ADA-EASD Position Statement: Management of Hyperglycemia in T 2 DM 3. ANTI-HYPERGLYCEMIC THERAPY • Therapeutic options: Oral agents & non-insulin injectables - Metformin - Sulfonylureas - Thiazolidinediones - DPP-4 inhibitors - GLP-1 receptor agonists - Meglitinides - a-glucosidase inhibitors - Bile acid sequestrants - Dopamine-2 agonists - Amylin mimetics Diabetes Care 2012; 35: 1364– 1379 Diabetologia 2012; 55: 1577– 1596

Class Mechanism Advantages Biguanides (Metformin) • Activates AMP-kinase • Hepatic glucose production • Extensive experience • No hypoglycemia • Weight neutral • ? CVD events • Gastrointestinal • Lactic acidosis • B-12 deficiency • Contraindications Low SUs / Meglitinides • Closes KATP channels • Insulin secretion • Extensive experience • Microvascular risk • Hypoglycemia • Weight gain • Low durability • ? Ischemic preconditioning Low TZDs • Activates PPAR-g • Insulin sensitivity • No hypoglycemia • Durability • TGs, HDL-C • ? CVD events (pio) • Weight gain • Edema / heart failure • Bone fractures • ? MI (rosi) • ? Bladder ca (pio) High a-GIs • Inhibits a-glucosidase • Slows carbohydrate absorption • No hypoglycemia • Gastrointestinal • Nonsystemic • Dosing frequency • Post-prandial glucose • Modest A 1 c • ? CVD events Table 1. Properties of anti-hyperglycemic agents Disadvantages Cost Mod. Diabetes Care 2012; 35: 1364– 1379 Diabetologia 2012; 55: 1577– 1596
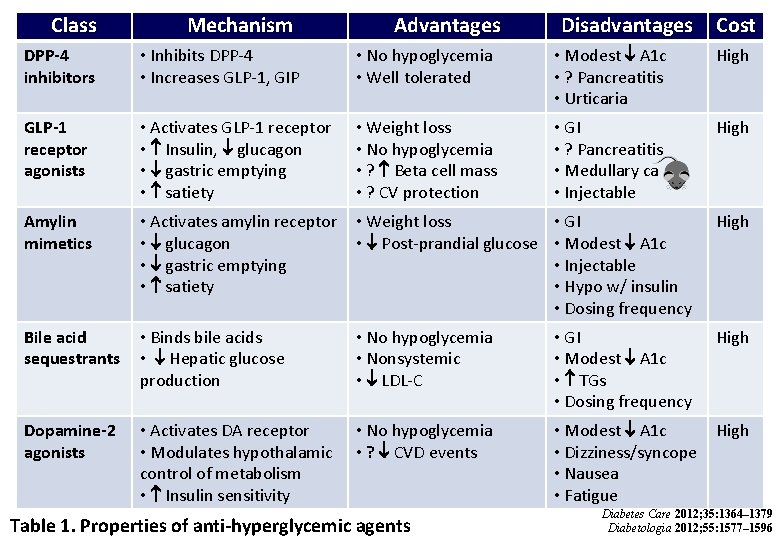
Class Mechanism Advantages Disadvantages Cost DPP-4 inhibitors • Inhibits DPP-4 • Increases GLP-1, GIP • No hypoglycemia • Well tolerated • Modest A 1 c • ? Pancreatitis • Urticaria High GLP-1 receptor agonists • Activates GLP-1 receptor • Insulin, glucagon • gastric emptying • satiety • Weight loss • No hypoglycemia • ? Beta cell mass • ? CV protection • GI • ? Pancreatitis • Medullary ca • Injectable High Amylin mimetics • Activates amylin receptor • glucagon • gastric emptying • satiety • Weight loss • GI • Post-prandial glucose • Modest A 1 c • Injectable • Hypo w/ insulin • Dosing frequency High Bile acid sequestrants • Binds bile acids • Hepatic glucose production • No hypoglycemia • Nonsystemic • LDL-C • GI • Modest A 1 c • TGs • Dosing frequency High Dopamine-2 agonists • Activates DA receptor • Modulates hypothalamic control of metabolism • Insulin sensitivity • No hypoglycemia • ? CVD events • Modest A 1 c High • Dizziness/syncope • Nausea • Fatigue Table 1. Properties of anti-hyperglycemic agents Diabetes Care 2012; 35: 1364– 1379 Diabetologia 2012; 55: 1577– 1596
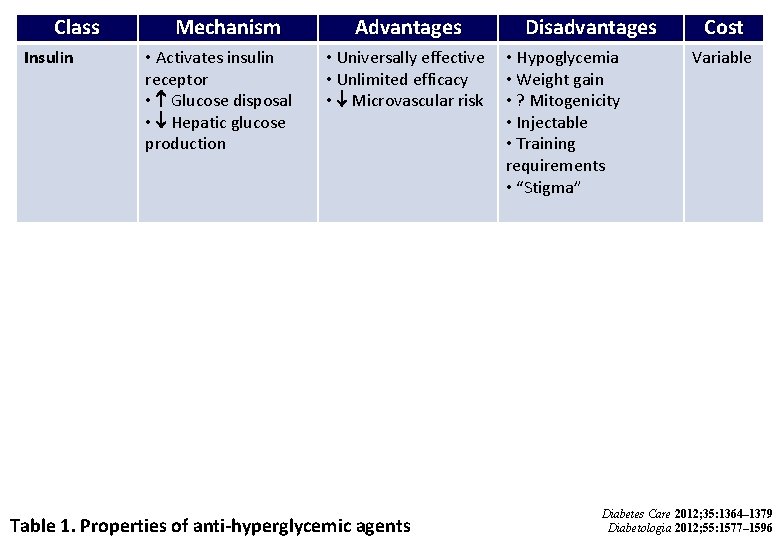
Class Insulin Mechanism • Activates insulin receptor • Glucose disposal • Hepatic glucose production Advantages • Universally effective • Unlimited efficacy • Microvascular risk Table 1. Properties of anti-hyperglycemic agents Disadvantages • Hypoglycemia • Weight gain • ? Mitogenicity • Injectable • Training requirements • “Stigma” Cost Variable Diabetes Care 2012; 35: 1364– 1379 Diabetologia 2012; 55: 1577– 1596

ADA-EASD Position Statement: Management of Hyperglycemia in T 2 DM 3. ANTI-HYPERGLYCEMIC THERAPY • Therapeutic options: Insulin - Human Neutral protamine Hagedorn (NPH) - Human Regular - Basal analogues (glargine, detemir) - Rapid analogues (lispro, aspart, glulisine) - Pre-mixed varieties Diabetes Care 2012; 35: 1364– 1379 Diabetologia 2012; 55: 1577– 1596

ADA-EASD Position Statement: Management of Hyperglycemia in T 2 DM 3. ANTI-HYPERGLYCEMIC THERAPY • Therapeutic options: Insulin level Rapid (Lispro, Aspart, Glulisine) Short (Regular) Intermediate (NPH) Long (Detemir) Long (Glargine) 0 2 4 6 8 Hours 10 12 14 16 Hours after injection 18 20 22 24

ADA-EASD Position Statement: Management of Hyperglycemia in T 2 DM 3. ANTI-HYPERGLYCEMIC THERAPY • Implementation strategies: - Initial therapy - Advancing to dual combination therapy - Advancing to triple combination therapy - Transitions to & titrations of insulin Diabetes Care 2012; 35: 1364– 1379 Diabetologia 2012; 55: 1577– 1596
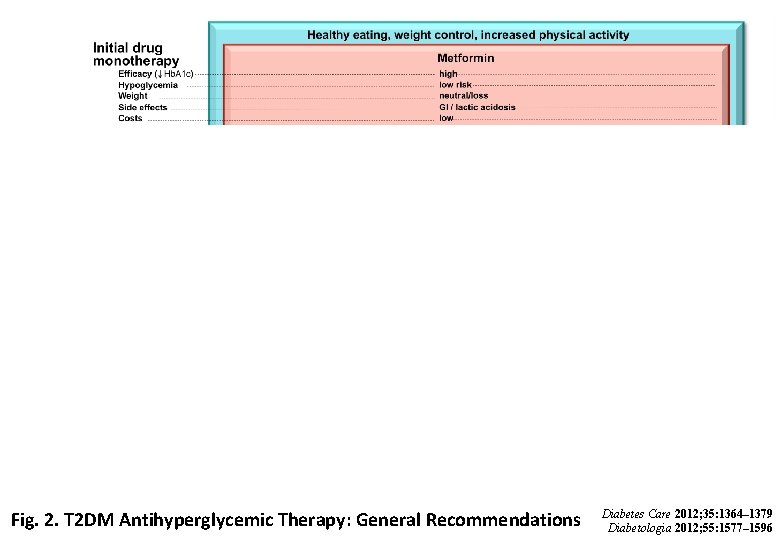
Fig. 2. T 2 DM Antihyperglycemic Therapy: General Recommendations Diabetes Care 2012; 35: 1364– 1379 Diabetologia 2012; 55: 1577– 1596

Fig. 2. T 2 DM Antihyperglycemic Therapy: General Recommendations Diabetes Care 2012; 35: 1364– 1379 Diabetologia 2012; 55: 1577– 1596
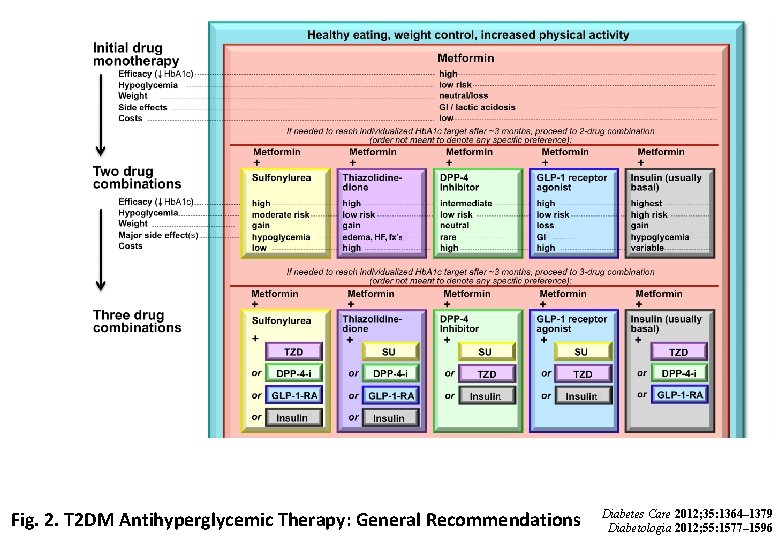
Fig. 2. T 2 DM Antihyperglycemic Therapy: General Recommendations Diabetes Care 2012; 35: 1364– 1379 Diabetologia 2012; 55: 1577– 1596
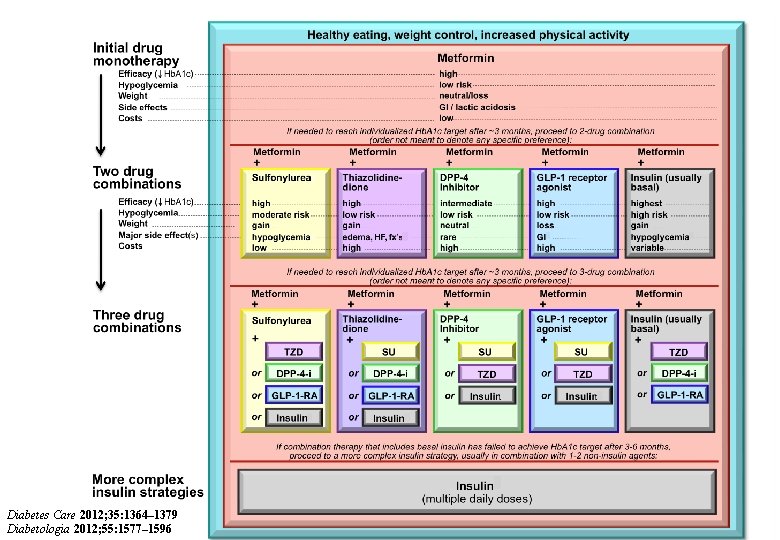
Diabetes Care 2012; 35: 1364– 1379 Diabetologia 2012; 55: 1577– 1596
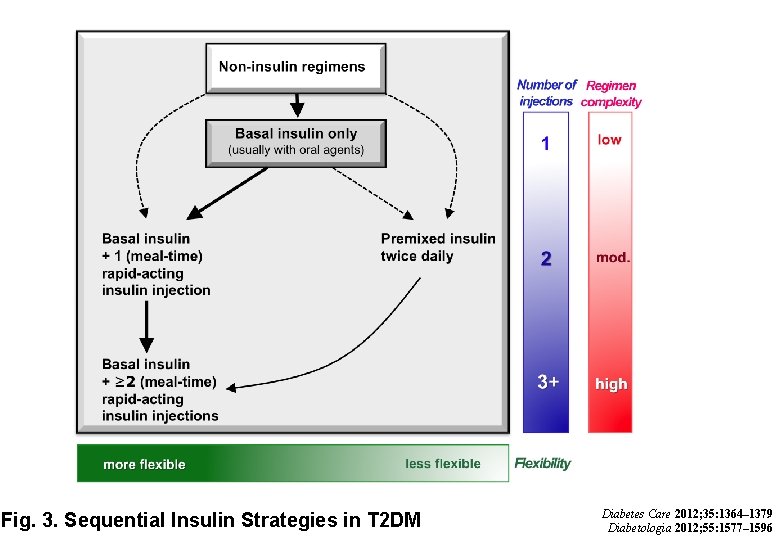
Fig. 3. Sequential Insulin Strategies in T 2 DM Diabetes Care 2012; 35: 1364– 1379 Diabetologia 2012; 55: 1577– 1596

ADA-EASD Position Statement: Management of Hyperglycemia in T 2 DM 4. OTHER CONSIDERATIONS • • Age Weight Sex / racial / ethnic / genetic differences Comorbidities - Coronary artery disease Heart Failure Chronic kidney disease Liver dysfunction Hypoglycemia Diabetes Care 2012; 35: 1364– 1379 Diabetologia 2012; 55: 1577– 1596

ADA-EASD Position Statement: Management of Hyperglycemia in T 2 DM 4. OTHER CONSIDERATIONS • Age: Older adults - Reduced life expectancy Higher CVD burden Reduced GFR At risk for adverse events from polypharmacy More likely to be compromised from hypoglycemia üLess ambitious targets üHb. A 1 c <7. 5– 8. 0% if tighter targets not easily achieved üFocus on drug safety Diabetes Care 2012; 35: 1364– 1379 Diabetologia 2012; 55: 1577– 1596

ADA-EASD Position Statement: Management of Hyperglycemia in T 2 DM 4. OTHER CONSIDERATIONS • Weight - Majority of T 2 DM patients overweight / obese Intensive lifestyle program Metformin GLP-1 receptor agonists ? Bariatric surgery Consider LADA in lean patients Diabetes Care 2012; 35: 1364– 1379 Diabetologia 2012; 55: 1577– 1596

T 2 DM Anti-hyperglycemic Therapy: General Recommendations Diabetes Care 2012; 35: 1364– 1379 Diabetologia 2012; 55: 1577– 1596
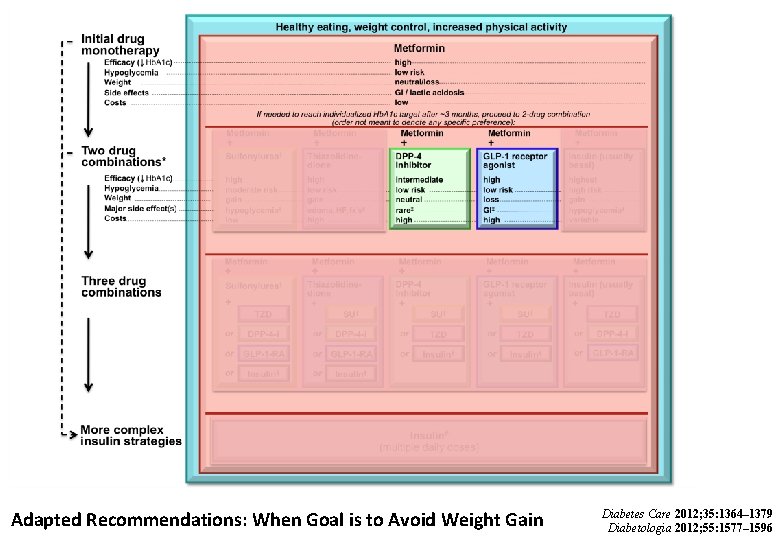
Adapted Recommendations: When Goal is to Avoid Weight Gain Diabetes Care 2012; 35: 1364– 1379 Diabetologia 2012; 55: 1577– 1596

ADA-EASD Position Statement: Management of Hyperglycemia in T 2 DM 4. OTHER CONSIDERATIONS • Sex/ethnic/racial/genetic differences - Little is known MODY & other monogenic forms of diabetes Latinos: more insulin resistance East Asians: more beta cell dysfunction Gender may drive concerns about adverse effects (e. g. , bone loss from TZDs) Diabetes Care 2012; 35: 1364– 1379 Diabetologia 2012; 55: 1577– 1596

ADA-EASD Position Statement: Management of Hyperglycemia in T 2 DM 4. OTHER CONSIDERATIONS • Comorbidities Ø Metformin: CVD benefit (UKPDS) - Coronary Disease Ø Avoid hypoglycemia - Heart Failure Ø ? SUs & ischemic preconditioning - Renal disease - Liver dysfunction Ø ? Pioglitazone & CVD events Ø ? Effects of incretin-based therapies - Hypoglycemia Diabetes Care 2012; 35: 1364– 1379 Diabetologia 2012; 55: 1577– 1596

ADA-EASD Position Statement: Management of Hyperglycemia in T 2 DM 4. OTHER CONSIDERATIONS • Comorbidities - Coronary Disease - Heart Failure - Renal disease - Liver dysfunction Ø Metformin: May use unless condition is unstable or severe Ø Avoid TZDs Ø ? Effects of incretin-based therapies - Hypoglycemia Diabetes Care 2012; 35: 1364– 1379 Diabetologia 2012; 55: 1577– 1596

ADA-EASD Position Statement: Management of Hyperglycemia in T 2 DM 4. OTHER CONSIDERATIONS • Comorbidities - Coronary Disease - Heart Failure Ø Increased risk of hypoglycemia - Renal disease Ø Metformin & lactic acidosis - Liver dysfunction - Hypoglycemia § US: stop @SCr ≥ 1. 5 (1. 4 women) § UK: half-dose @GFR < 45 & stop @GFR < 30 Ø Caution with SUs (esp. glyburide) Ø DPP-4 -i’s – dose adjust for most Ø Avoid exenatide if GFR < 30 Diabetes Care 2012; 35: 1364– 1379 Diabetologia 2012; 55: 1577– 1596

ADA-EASD Position Statement: Management of Hyperglycemia in T 2 DM 4. OTHER CONSIDERATIONS • Comorbidities - Coronary Disease - Heart Failure - Renal disease - Liver dysfunction - Hypoglycemia Ø Most drugs not tested in advanced liver disease Ø Pioglitazone may help steatosis Ø Insulin best option if disease severe Diabetes Care 2012; 35: 1364– 1379 Diabetologia 2012; 55: 1577– 1596

ADA-EASD Position Statement: Management of Hyperglycemia in T 2 DM 4. OTHER CONSIDERATIONS • Comorbidities - Coronary Disease - Heart Failure - Renal disease - Liver dysfunction - Hypoglycemia Ø Emerging concerns regarding association with increased morbidity / mortality Ø Proper drug selection is key in the hypoglycemia prone Diabetes Care 2012; 35: 1364– 1379 Diabetologia 2012; 55: 1577– 1596
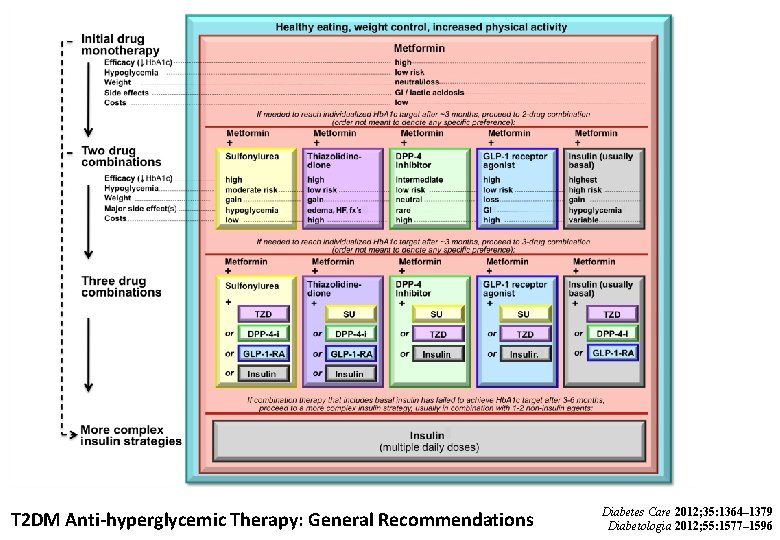
T 2 DM Anti-hyperglycemic Therapy: General Recommendations Diabetes Care 2012; 35: 1364– 1379 Diabetologia 2012; 55: 1577– 1596
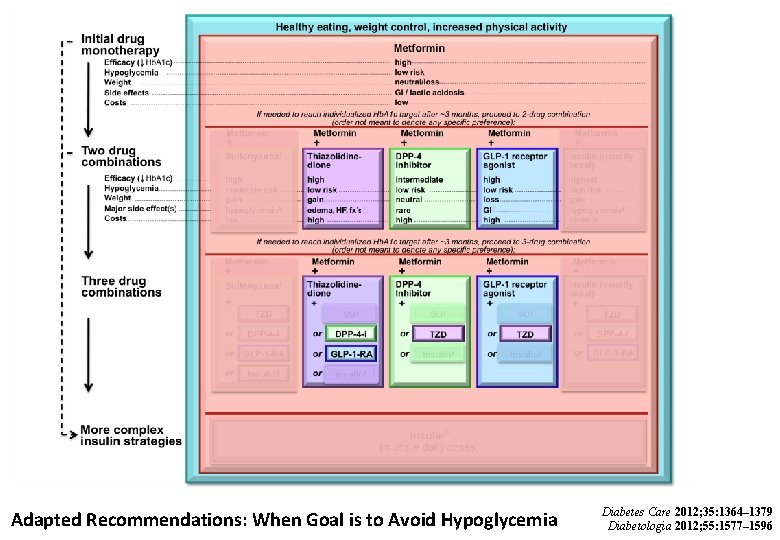
Adapted Recommendations: When Goal is to Avoid Hypoglycemia Diabetes Care 2012; 35: 1364– 1379 Diabetologia 2012; 55: 1577– 1596
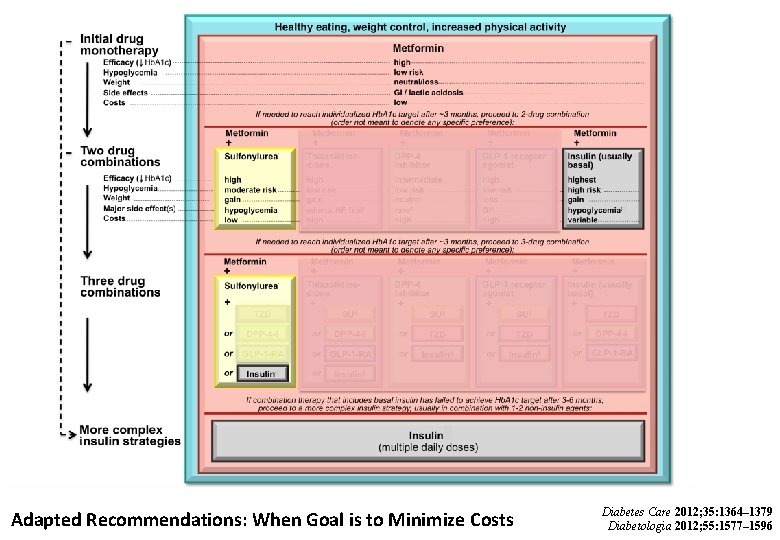
Adapted Recommendations: When Goal is to Minimize Costs Diabetes Care 2012; 35: 1364– 1379 Diabetologia 2012; 55: 1577– 1596
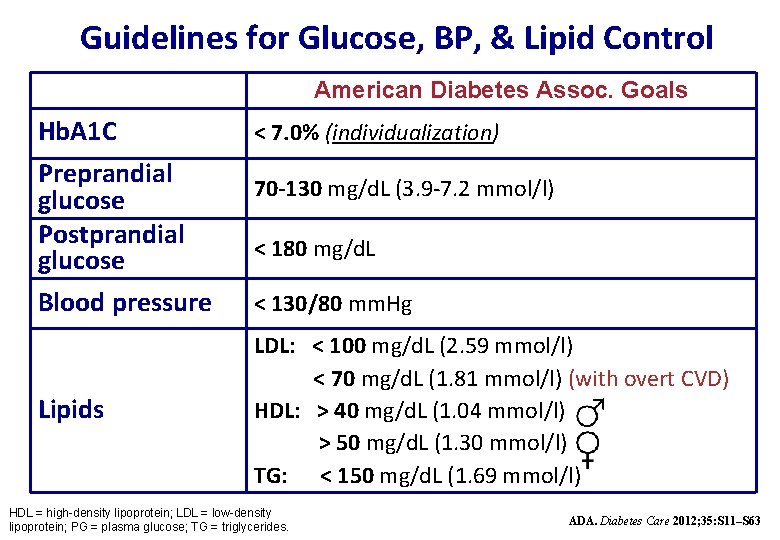
Guidelines for Glucose, BP, & Lipid Control American Diabetes Assoc. Goals Hb. A 1 C Preprandial glucose Postprandial glucose Blood pressure Lipids < 7. 0% (individualization) 70 -130 mg/d. L (3. 9 -7. 2 mmol/l) < 180 mg/d. L < 130/80 mm. Hg LDL: < 100 mg/d. L (2. 59 mmol/l) < 70 mg/d. L (1. 81 mmol/l) (with overt CVD) HDL: > 40 mg/d. L (1. 04 mmol/l) > 50 mg/d. L (1. 30 mmol/l) TG: < 150 mg/d. L (1. 69 mmol/l) HDL = high-density lipoprotein; LDL = low-density lipoprotein; PG = plasma glucose; TG = triglycerides. ADA. Diabetes Care 2012; 35: S 11–S 63

ADA-EASD Position Statement: Management of Hyperglycemia in T 2 DM 4. FUTURE DIRECTIONS / RESEARCH NEEDS • Comparative effectiveness research Ø Focus on important clinical outcomes • Contributions of genomic research • Perpetual need for clinical judgment! Diabetes Care 2012; 35: 1364– 1379 Diabetologia 2012; 55: 1577– 1596

ADA-EASD Position Statement: Management of Hyperglycemia in T 2 DM KEY POINTS • Glycemic targets & BG-lowering therapies must be individualized. • Diet, exercise, & education: foundation of any T 2 DM therapy program • Unless contraindicated, metformin = optimal 1 st-line drug. • After metformin, data are limited. Combination therapy with 1 -2 other oral / injectable agents is reasonable; minimize side effects. • Ultimately, many patients will require insulin therapy alone / in combination with other agents to maintain BG control. • All treatment decisions should be made in conjunction with the patient (focus on preferences, needs & values. ) • Comprehensive CV risk reduction - a major focus of therapy. Diabetes Care 2012; 35: 1364– 1379 Diabetologia 2012; 55: 1577– 1596

ADA-EASD Position Statement: Management of Hyperglycemia in T 2 DM Invited Reviewers James Best, The University of Melbourne, Australia Ilias Migdalis, NIMTS Hospital, Athens, Greece Henk Bilo, Isala Clinics, Zwolle, Netherlands Donna Miller, Univ of So California, LA, CA John Boltri, Wayne State University, Detroit, MI Robert Ratner, Med. Star/Georgetown Univ, DC Thomas Buchanan, Univ of So California, LA, CA Julio Rosenstock, Dallas Diab/Endo Ctr, Dallas, TX Paul Callaway, University of Kansas, Wichita, KS Bernard Charbonnel, University of Nantes, France Stephen Colagiuri, The University of Sydney, Australia Samuel Dagogo-Jack, Univ of Tenn, Memphis, TN Margo Farber, Detroit Medical Center, Detroit, MI Cynthia Fritschi, University of Illinois, Chicago, IL Guntram Schernthaner, Rudolfstiftung Hosp, Vienna, Austria Robert Sherwin, Yale University, New Haven, CT Jay Skyler, University of Miami, FL Geralyn Spollett, Yale University, New Haven, CT Ellie Strock, Int’l Diabetes Center, Minneapolis, MN Rowan Hillson, Hillingdon Hospital, Uxbridge, U. K. Agathocles Tsatsoulis, University of Ioannina, Greece Faramarz Ismail-Beigi, CWR Univ, Cleveland, OH Andrew Wolf, Univ of Virginia Charlottesville, VA Devan Kansagara, Oregon H&S Univ, Portland, OR Bernard Zinman, University of Toronto, Ontario, Canada Professional Practice Committee, American Diabetes Association Panel for Overseeing Guidelines and Statements, European Association for the Study of Diabetes American Association of Diabetes Educators The Endocrine Society American College of Physicians
- Slides: 45