Management of Cervical Spine Disease in Downs Syndrome





































- Slides: 70

Management of Cervical Spine Disease in Down's Syndrome: A Neurosurgical perspective Dominic Thompson Department of Paediatric Neurosurgery Great Ormond Street London

Flemish (1515) Anon Am J Med Genetics

Cervical spinal pathology in Downs syndrome -The controversies • • Aetiology Diagnosis Screening Treatment

Aetiology

Aetiology • Primary features • Ligamentous laxity • Hypotonia • Hypermobility

Aetiology • Primary features • Skeletal consequences • Ligamentous laxity • Hypotonia • Hypermobility • • Craniovertebral instability Scoliosis Hip instability Patellar instability

Cervical spinal pathology in Downs syndrome • • Occipito-atlantal subluxation Atlantoaxial subluxation Os Odontoideum Incomplete C 1 ring Cervical stenosis Segmentation anomaly Premature cervical spondylarthrotic myelopathy

Cervical spinal pathology in Downs syndrome • • Occipito-atlantal subluxation Atlantoaxial subluxation Os Odontoideum Incomplete C 1 ring Cervical stenosis Segmentation anomaly Premature cervical spondylarthrotic myelopathy

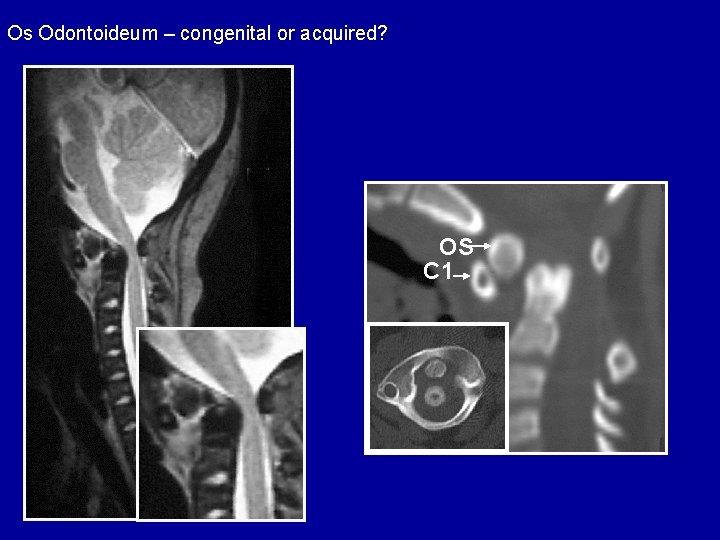
Os Odontoideum – congenital or acquired? OS C 1

Os odontoideum – developmental anatomy • Sclerotomes cranial and caudal moieties – scleromites Cranial – hypocentrum - disc Caudal – centrum - body

Os odontoideum – developmental anatomy • Sclerotomes cranial and caudal moieties – scleromites Cranial – hypocentrum - disc Caudal – centrum - body

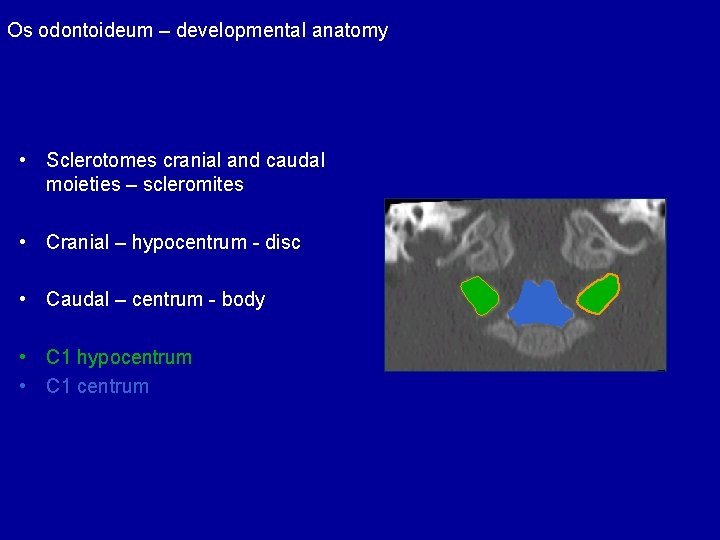
Os odontoideum – developmental anatomy • Sclerotomes cranial and caudal moieties – scleromites • Cranial – hypocentrum - disc • Caudal – centrum - body • C 1 hypocentrum • C 1 centrum

Os odontoideum – developmental anatomy • Sclerotomes cranial and caudal moieties – scleromites • Cranial – hypocentrum - disc • Caudal – centrum - body • C 2 hypocentrum -regresses • C 2 centrum

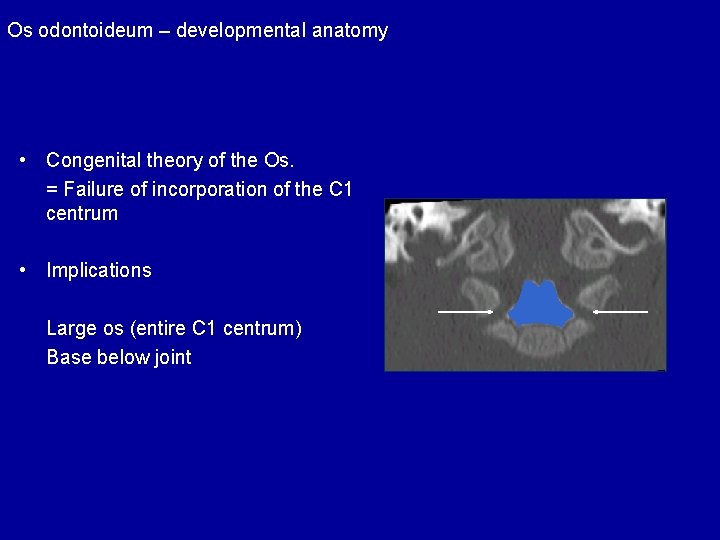
Os odontoideum – developmental anatomy • Congenital theory of the Os. = Failure of incorporation of the C 1 centrum • Implications Large os (entire C 1 centrum) Base below joint

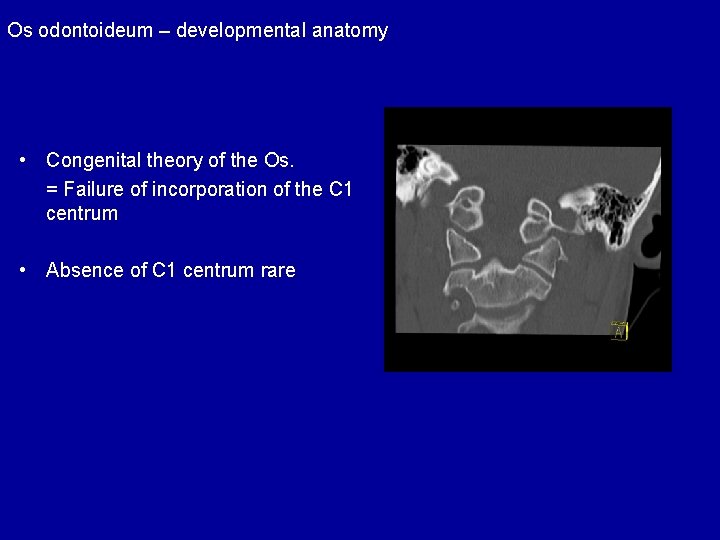
Os odontoideum – developmental anatomy • Congenital theory of the Os. = Failure of incorporation of the C 1 centrum • Absence of C 1 centrum rare

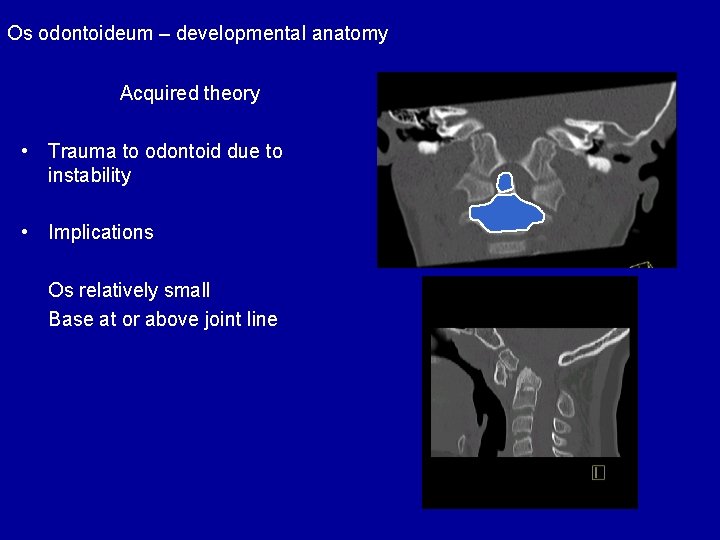
Os odontoideum – developmental anatomy Acquired theory • Trauma to odontoid due to instability • Implications Os relatively small Base at or above joint line

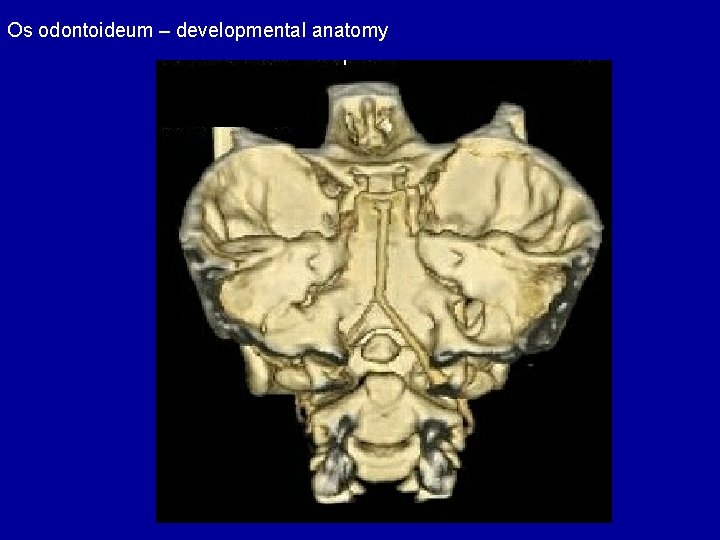
Os odontoideum – developmental anatomy

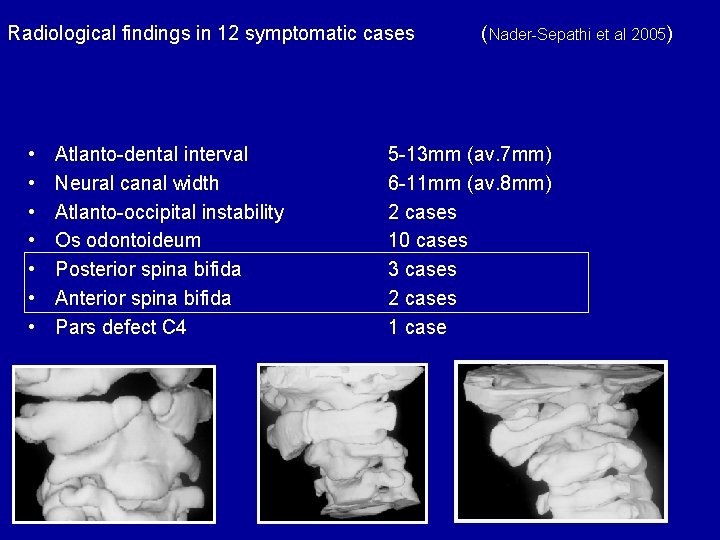
Radiological findings in 12 symptomatic cases • • Atlanto-dental interval Neural canal width Atlanto-occipital instability Os odontoideum Posterior spina bifida Anterior spina bifida Pars defect C 4 (Nader-Sepathi et al 2005) 5 -13 mm (av. 7 mm) 6 -11 mm (av. 8 mm) 2 cases 10 cases 3 cases 2 cases 1 case

Radiological findings in 12 symptomatic cases • • Atlanto-dental interval Neural canal width Atlanto-occipital instability Os odontoideum Posterior spina bifida Anterior spina bifida Pars defect C 4 (Nader-Sepathi et al 2005) 5 -13 mm (av. 7 mm) 6 -11 mm (av. 8 mm) 2 cases 10 cases 3 cases 2 cases 1 case

Radiological findings in 12 symptomatic cases • • Atlanto-dental interval Neural canal width Atlanto-occipital instability Os odontoideum Posterior spina bifida Anterior spina bifida Pars defect C 4 (Nader-Sepathi et al 2005) 5 -13 mm (av. 7 mm) 6 -11 mm (av. 8 mm) 2 cases 10 cases 3 cases 2 cases 1 case

Craniovertebral instability Os Odontoideum Delayed Atlantal ossification

Diagnosis

Diagnosis of craniovertebral instability in Downs Syndrome Aims • To identify children with or at risk of spinal cord damage due to craniovertebral instability • To instigate effective treatment

What to measure?

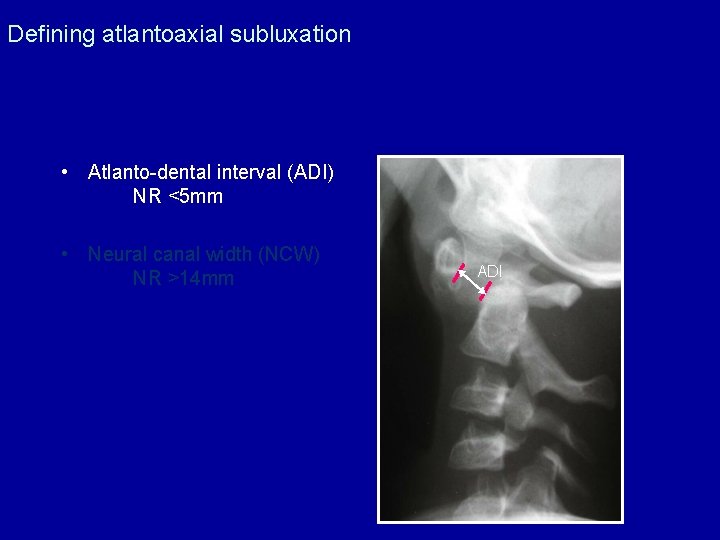
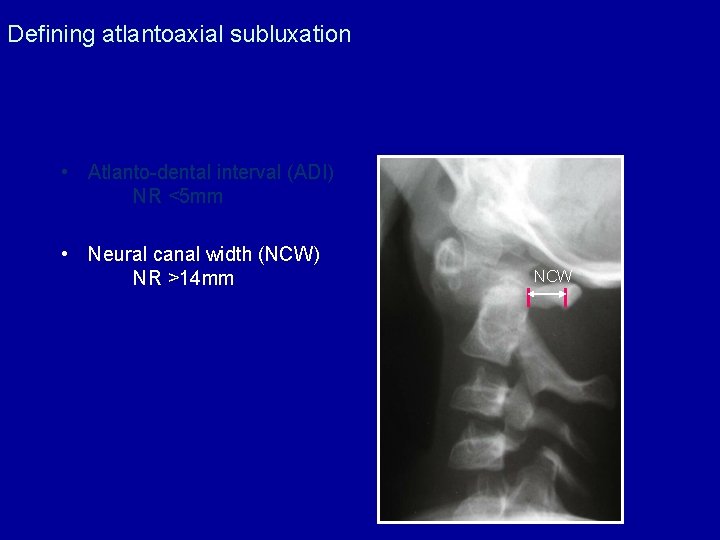
Defining atlantoaxial subluxation • Atlanto-dental interval (ADI) NR <5 mm • Neural canal width (NCW) NR >14 mm ADI

Defining atlantoaxial subluxation • Atlanto-dental interval (ADI) NR <5 mm • Neural canal width (NCW) NR >14 mm NCW

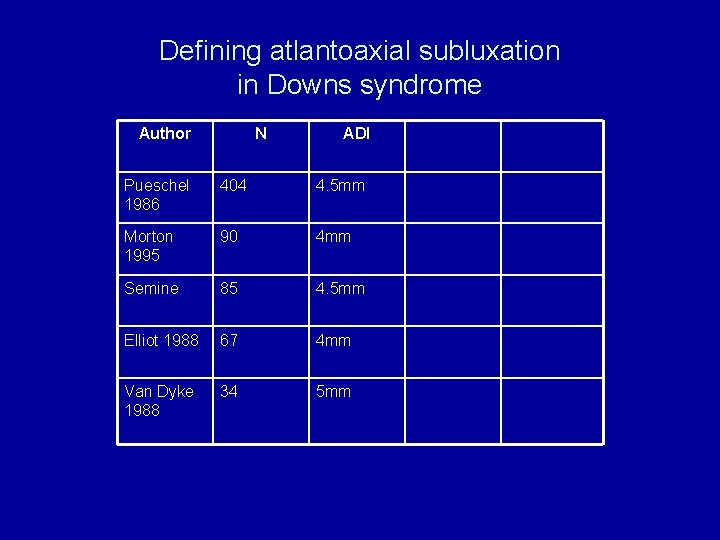
Defining atlantoaxial subluxation in Downs syndrome Author N ADI Pueschel 1986 404 4. 5 mm Morton 1995 90 4 mm Semine 85 4. 5 mm Elliot 1988 67 4 mm Van Dyke 1988 34 5 mm

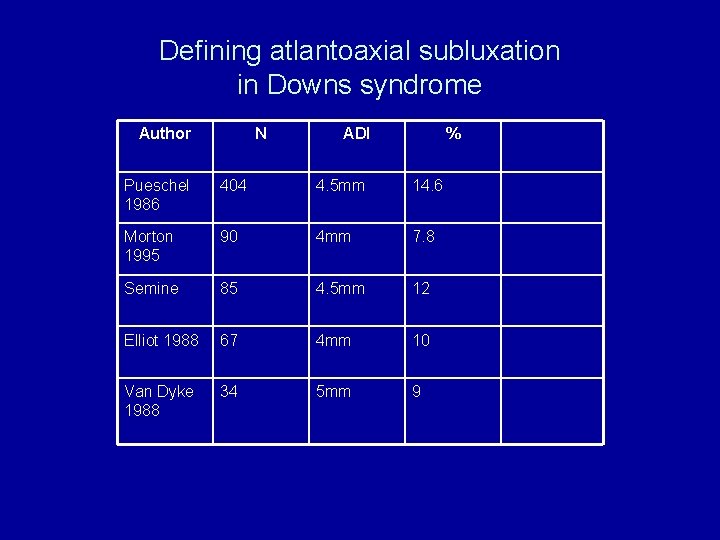
Defining atlantoaxial subluxation in Downs syndrome Author N ADI % Pueschel 1986 404 4. 5 mm 14. 6 Morton 1995 90 4 mm 7. 8 Semine 85 4. 5 mm 12 Elliot 1988 67 4 mm 10 Van Dyke 1988 34 5 mm 9

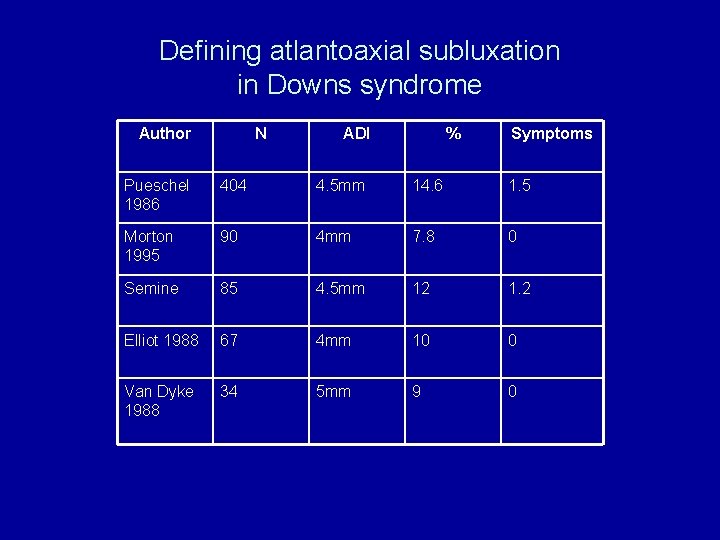
Defining atlantoaxial subluxation in Downs syndrome Author N ADI % Symptoms Pueschel 1986 404 4. 5 mm 14. 6 1. 5 Morton 1995 90 4 mm 7. 8 0 Semine 85 4. 5 mm 12 1. 2 Elliot 1988 67 4 mm 10 0 Van Dyke 1988 34 5 mm 9 0

Acute vs chronic deterioration • Nader-Sepathi et al 2005 • 5/12 acute deterioration • Preceeding symptoms in 4 • Davidson 1988 • 31 Downs with neurological symptoms/signs • 29 symptoms for >1 mnth

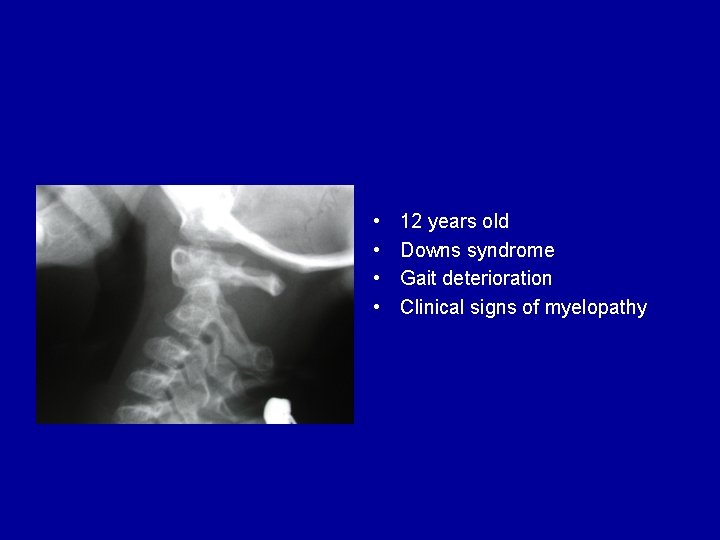
• • 12 years old Downs syndrome Gait deterioration Clinical signs of myelopathy

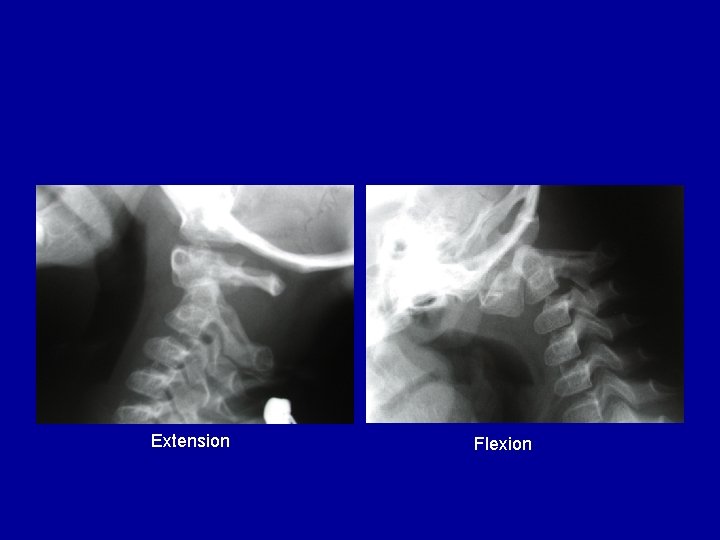
Extension Flexion

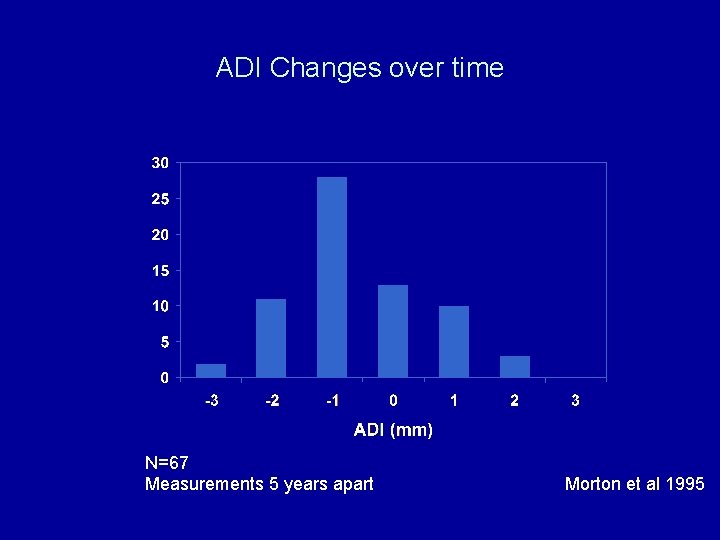
ADI Changes over time N=67 Measurements 5 years apart Morton et al 1995

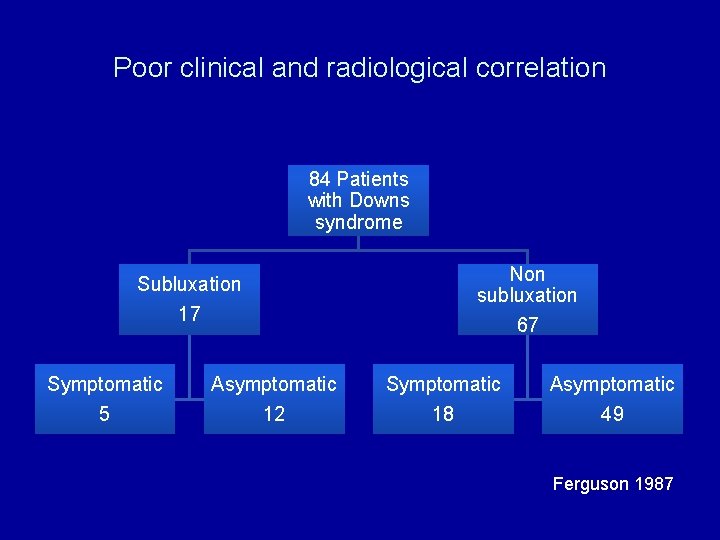
Poor clinical and radiological correlation 84 Patients with Downs syndrome Subluxation 17 Symptomatic 5 Asymptomatic 12 Non subluxation 67 Symptomatic 18 Asymptomatic 49 Ferguson 1987

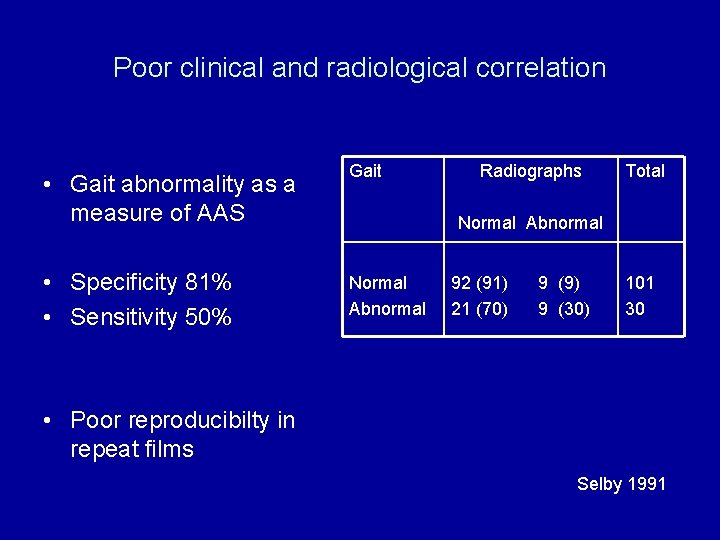
Poor clinical and radiological correlation • Gait abnormality as a measure of AAS • Specificity 81% • Sensitivity 50% Gait Radiographs Total Normal Abnormal 92 (91) 21 (70) 9 (9) 9 (30) 101 30 Selby 1991

Poor clinical and radiological correlation • Gait abnormality as a measure of AAS • Specificity 81% • Sensitivity 50% Gait Radiographs Total Normal Abnormal 92 (91) 21 (70) 9 (9) 9 (30) 101 30 • Poor reproducibilty in repeat films Selby 1991

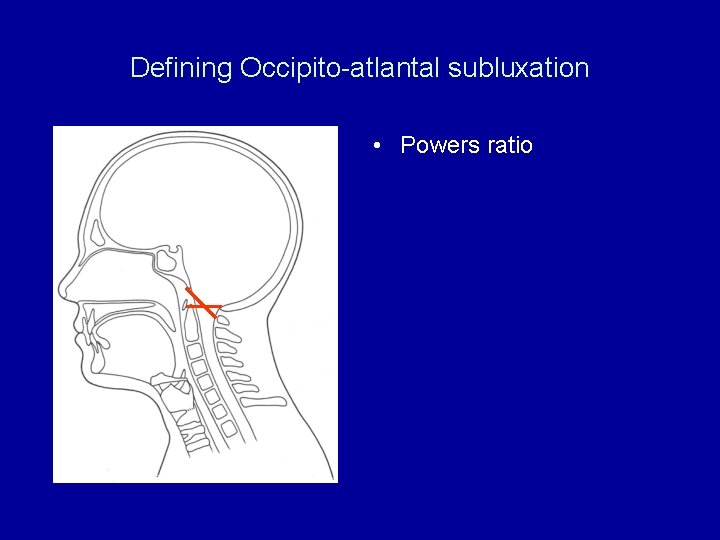
Defining Occipito-atlantal subluxation • Coexisting occipitoatlantal instability is common 40 -50% • Treadwell 1990 • Taggart 2000 • Difficult to diagnose

Defining Occipito-atlantal subluxation • Powers ratio

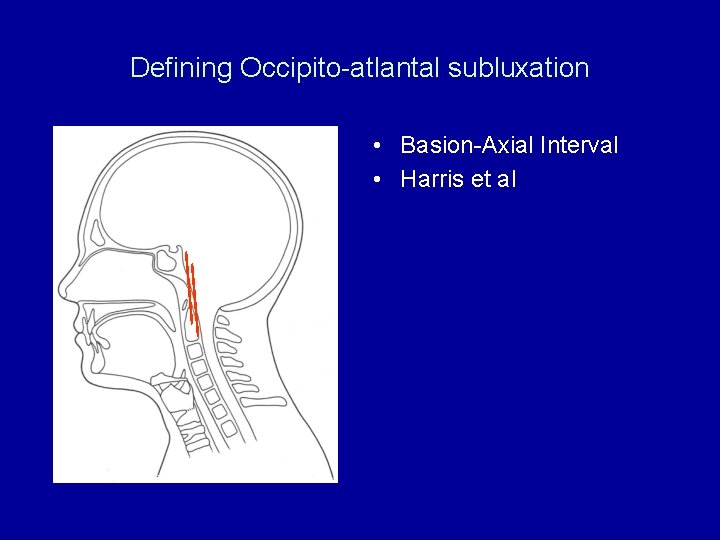
Defining Occipito-atlantal subluxation • Basion-Axial Interval • Harris et al

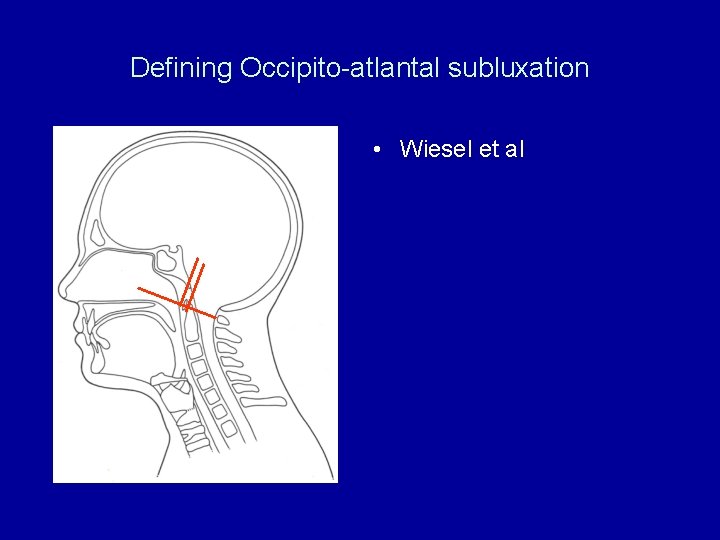
Defining Occipito-atlantal subluxation • Wiesel et al

Defining Occipito-atlantal subluxation • “Measurement of atlantooccipital translation by any of these methods is not reproducible” • Lori et al 1996

Limitations of Radiographic Measurements in Downs Syndrome • • ADI No consensus on measurement Poor reproducibility Poor correlation with symptoms O-C instability, present but difficult to measure

Screening

Should Children With Down Syndrome be Screened for Atlantoaxial Instability?

Should Children With Down Syndrome be Screened for Atlantoaxial Instability? • Special Olympics 1983 – All patients with Downs syndrome should have lateral cervical spine X rays – ADI>4. 5 mm mandates exclusion from high risk sporting activities • American Academy of Pediatrics 1984 • Department of Health Standing Medical Advisory Committee 1986

Should Children With Down Syndrome be Screened for Atlantoaxial Instability? • Special Olympics 1983 – All patients with Downs syndrome should have lateral cervical spine X rays – ADI>4. 5 mm mandates exclusion from high risk sporting activities • American Academy of Pediatrics 1984 • Department of Health Standing Medical Advisory Committee 1986

Screening • Incidence must be common • Screening test should be sensitive and specific • Asymptomatic AAS must be a risk factor for symptomatic AAS • A safe and effective intervention should be available

British Guidelines 2009 Downs Medical Interest Group of UK Cervical spine X rays are not recommended for the asymptomatic child with Downs syndrome , Medical personnel and carers need to be aware of the potential for neurological symptoms to develop

British Guidelines 2009 Downs Medical Interest Group of UK Warning Signs Neck pain, Abnormal head posture, Torticollis, (Wry neck) Reduced neck movements, Deterioration of gait and/or frequent falls Increasing fatigability on walking, Deterioration of manipulative skills,

British Guidelines 2009 Downs Medical Interest Group of UK Action Full physical and neurological examination Specialist Referral

British Gymnastics Association • Guidelines for the participation of individuals with Downs syndrome in gymnastics and trampolining • For all applicants to: – Registered clubs – Competitive events • Screening by medical practitioner • Approved by • • British Gymnastics Medical Commission Gymnastics and movement for people with disabilities Technical Committee

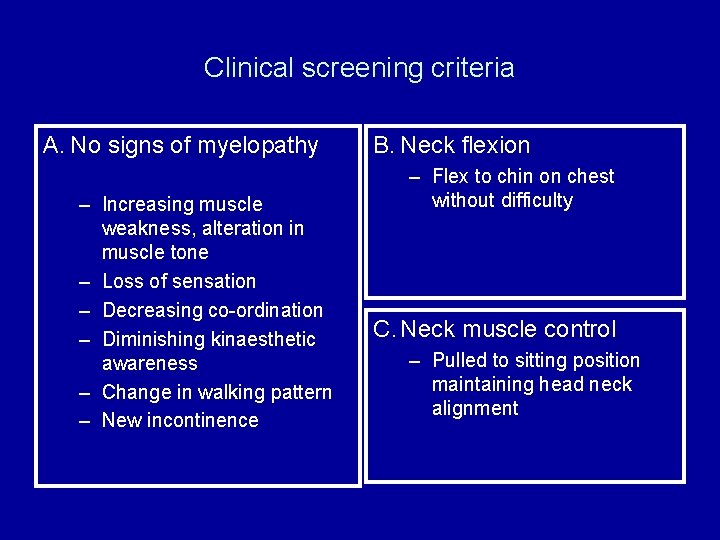
Clinical screening criteria A. No signs of myelopathy – Increasing muscle weakness, alteration in muscle tone – Loss of sensation – Decreasing co-ordination – Diminishing kinaesthetic awareness – Change in walking pattern – New incontinence B. Neck flexion – Flex to chin on chest without difficulty C. Neck muscle control – Pulled to sitting position maintaining head neck alignment

Results • 1995 -2009 • 399 applications from Individuals with Down syndrome • 6 positive responses – 4 Poor head neck muscle control – 2 Flex to chin on chest without difficulty – No further follow up

Results • 393 granted membership • No injuries referable to the cervical spine reported during the time period • 3 in National Squad

Treatment

Treatment • “A safe an effective intervention should be available”

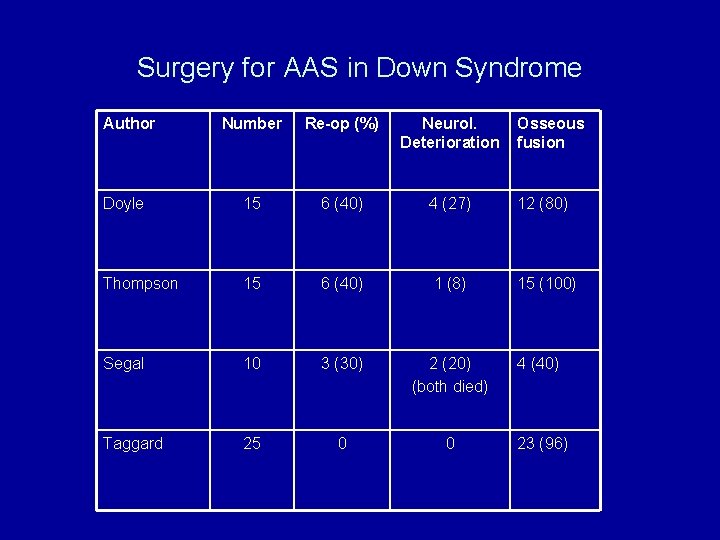
Surgery for AAS in Down Syndrome Author Number Re-op (%) Neurol. Deterioration Osseous fusion Doyle 15 6 (40) 4 (27) 12 (80) Thompson 15 6 (40) 1 (8) 15 (100) Segal 10 3 (30) 2 (20) (both died) 4 (40) Taggard 25 0 0 23 (96)

Reasons for failure N=15, 6 failures • • Inadequate immobilisation Inadequate reduction Inadequate fixation Inadequate age

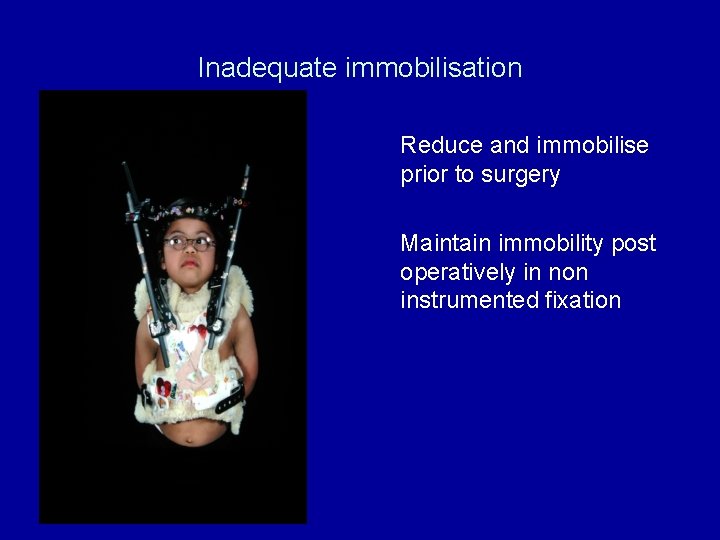
Inadequate immobilisation Reduce and immobilise prior to surgery Maintain immobility post operatively in non instrumented fixation

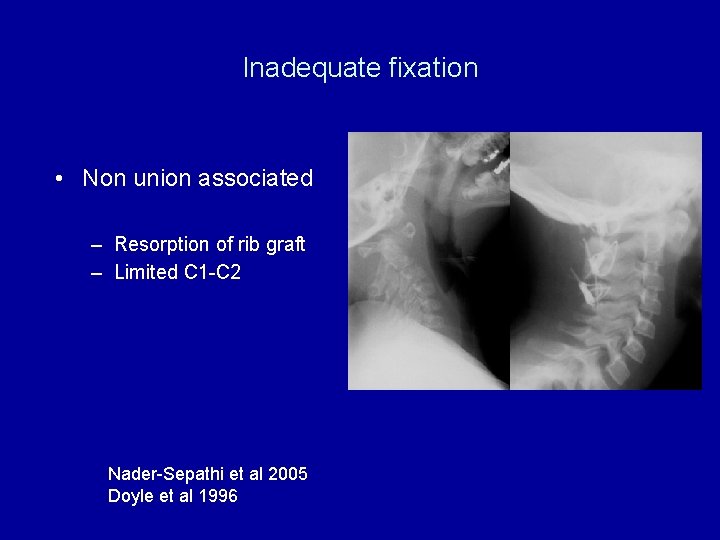
Inadequate fixation • Non union associated – Resorption of rib graft – Limited C 1 -C 2 Nader-Sepathi et al 2005 Doyle et al 1996

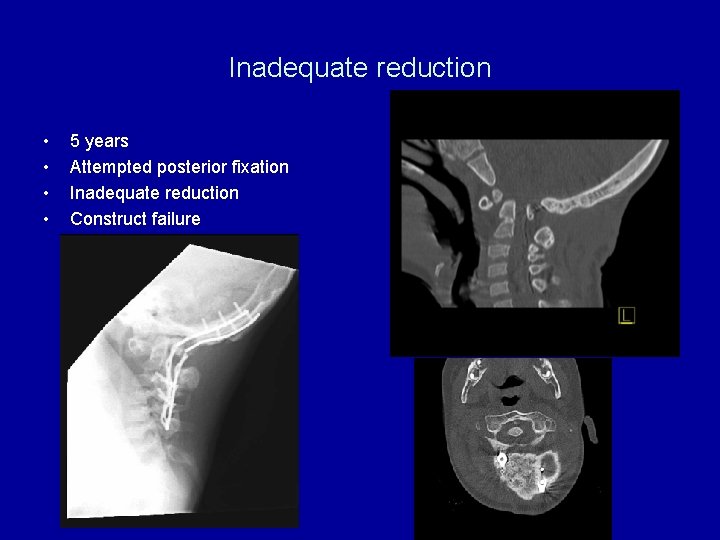
Inadequate reduction • • 5 years Attempted posterior fixation Inadequate reduction Construct failure

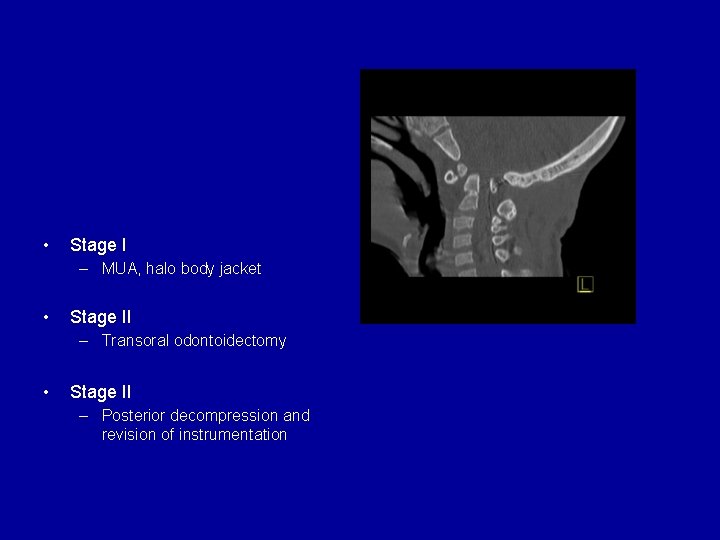
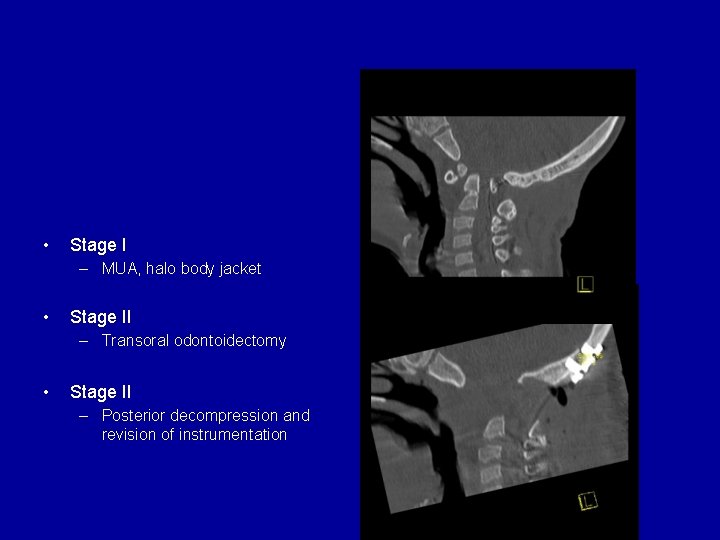
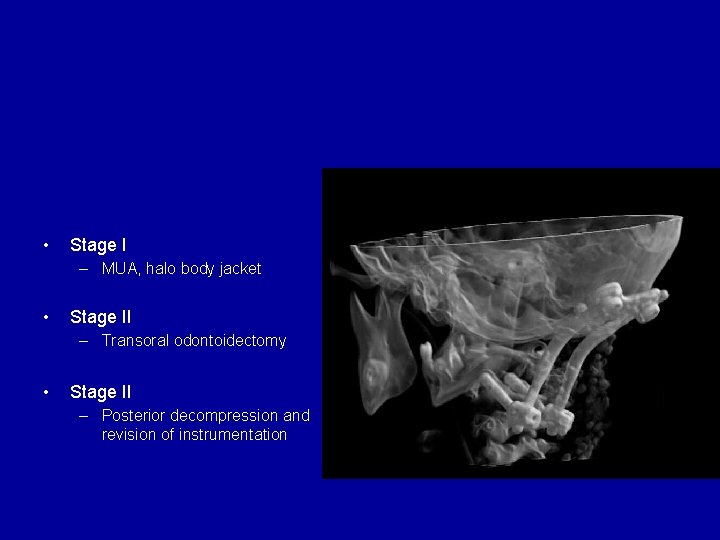
• Stage I – MUA, halo body jacket • Stage II – Transoral odontoidectomy • Stage II – Posterior decompression and revision of instrumentation

Case 1: Downs syndrome • Stage I – MUA, halo body jacket • Stage II – Transoral odontoidectomy • Stage II – Posterior decompression and revision of instrumentation

Case 1: Downs syndrome • Stage I – MUA, halo body jacket • Stage II – Transoral odontoidectomy • Stage II – Posterior decompression and revision of instrumentation

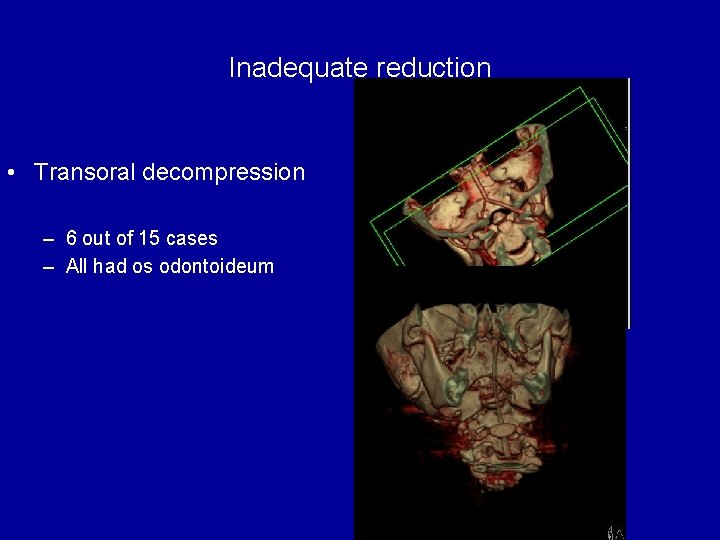
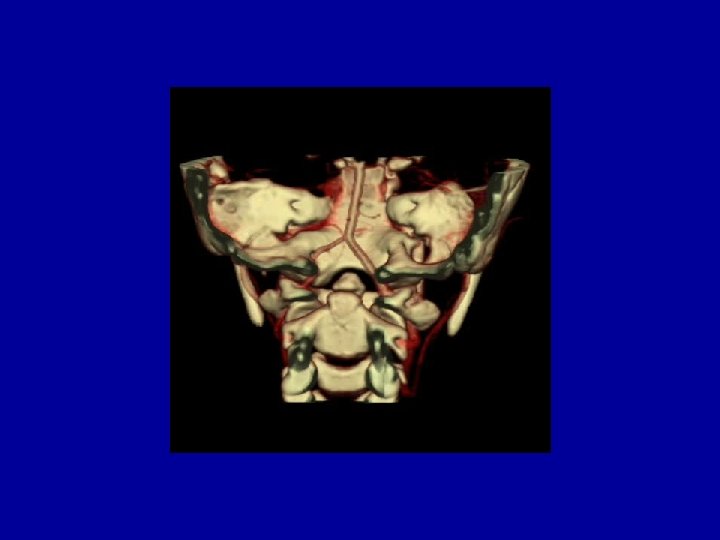
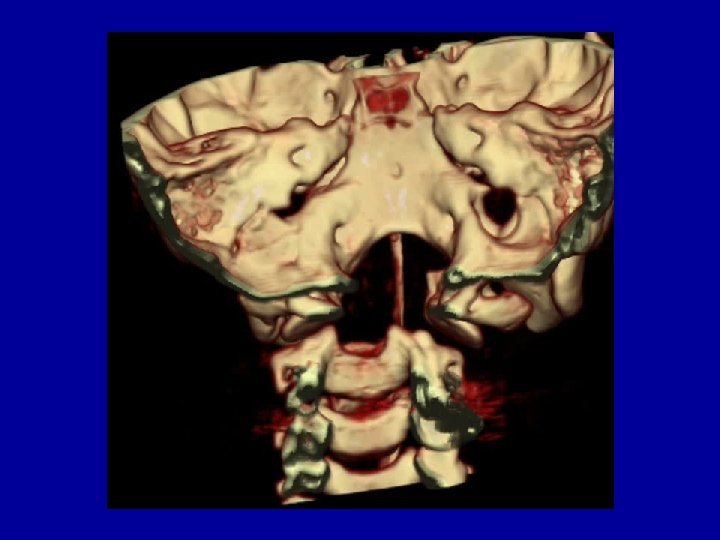
Inadequate reduction • Transoral decompression – 6 out of 15 cases – All had os odontoideum



Conclusions • Osseous anomalies at the CCJ may be consequence rather than cause of instability • Morphometric measures of AAI and OCI lack sufficient sensitivity and specificity to justify screening • Education rather than screening

Conclusions • Early investigation and treatment of symptomatic patients • Beware the child with Downs! • Ensure – Effective immobilisation – Adequate reduction – Rigid fixation
