Management of bronchial asthma The aims of treatment

Management of bronchial asthma The aims of treatment are to: Ø abolish symptoms Ø restore normal or best possible lung function Ø reduce the risk of severe attacks Ø enable normal growth to occur in children Ø minimize absence from school or employment.

Drugs used in asthma • Short-acting relievers Inhaled β 2 agonists (e. g. salbutamol, terbutaline) • Long-acting relief/disease controllers Inhaled long-acting β 2 agonists (e. g. salmeterol, formoterol) • Inhaled corticosteroids (e. g. beclometasone, budesonide, fluticasone) • Compound inhaled salmeterol & fluticasone • Sodium cromoglicate • Leukotriene modifiers (e. g. montelukast) Other agents with bronchodilator activity: • Inhaled antimuscarinic (e. g. ipratropium) • Theophylline preparations • Oral corticosteroids (e. g. prednisolone 40 mg daily) • Steroid-sparing agents Methotrexate Ciclosporin • Intravenous immunoglobulin • Anti-Ig. E monoclonal antibody – omalizumab Etanercept

Step-wise approach to asthma therapy according to the severity of asthma and ability to control symptoms SABA: short acting B. agonist, ICS, inhaled corticosteroid; LABA, long-acting β 2 agonists; OCS, oral corticosteroid 1 2 SABA ICS Low dose 3 LABA ICS Low dose 4 LABA ICS High dose 5 OCS LABA ICS High dose Short-acting β 2 -agonist as required for symptom relief Mild intermittent Mild persistent Moderate persistent Severe persistent Very severe persistent
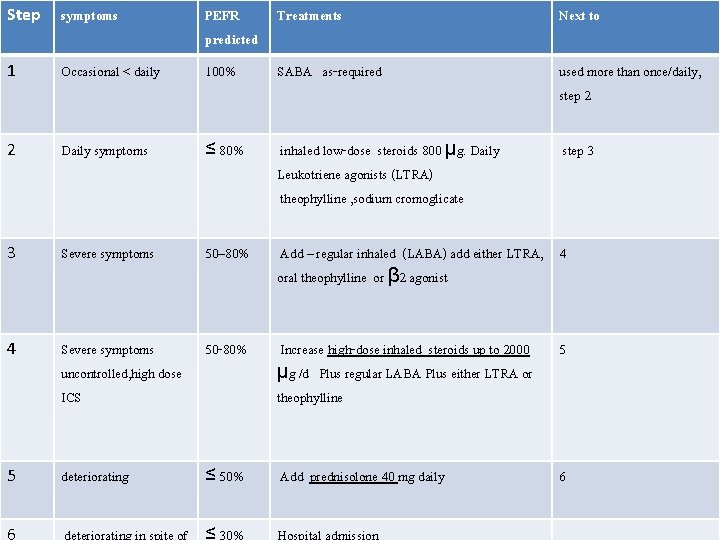
Step symptoms PEFR Treatments predicted Next to 1 Occasional < daily 100% SABA as-required used more than once/daily, step 2 2 Daily symptoms ≤ 80% inhaled low-dose steroids 800 μg. Daily Leukotriene agonists (LTRA) theophylline , sodium cromoglicate step 3 3 Severe symptoms 50– 80% Add – regular inhaled (LABA) add either LTRA, 4 oral theophylline or β 2 agonist 4 Severe symptoms uncontrolled, high dose ICS 50 -80% Increase high-dose inhaled steroids up to 2000 μg /d Plus regular LABA Plus either LTRA or theophylline 5 5 deteriorating ≤ 50% Add prednisolone 40 mg daily 6 6 deteriorating in spite of ≤ 30% Hospital admission
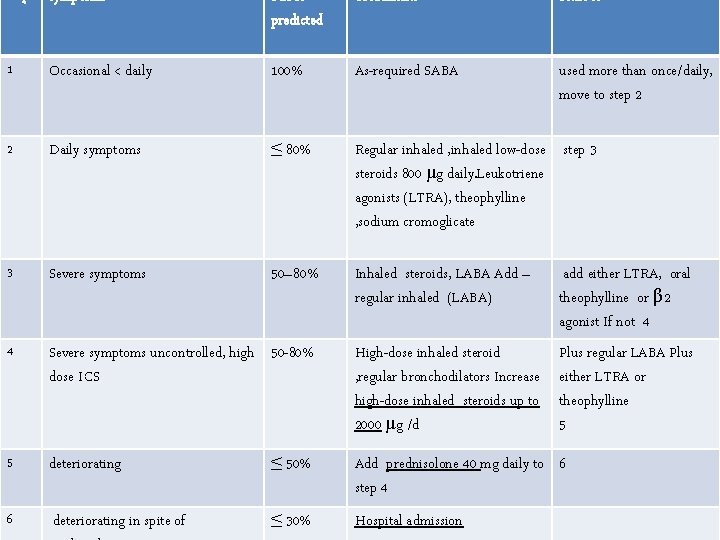
symptoms PEFR predicted Treatments Next to 1 Occasional < daily 100% As-required SABA used more than once/daily, move to step 2 2 Daily symptoms ≤ 80% Regular inhaled , inhaled low-dose step 3 steroids 800 μg daily. Leukotriene agonists (LTRA), theophylline , sodium cromoglicate 3 Severe symptoms 50– 80% Inhaled steroids, LABA Add – regular inhaled (LABA) add either LTRA, oral theophylline or β 2 agonist If not 4 4 Severe symptoms uncontrolled, high 50 -80% dose ICS High-dose inhaled steroid , regular bronchodilators Increase high-dose inhaled steroids up to 2000 μg /d Plus regular LABA Plus either LTRA or theophylline 5 5 deteriorating ≤ 50% Add prednisolone 40 mg daily to 6 step 4 6 deteriorating in spite of ≤ 30% Hospital admission

Acute severe asthma • ‘status asthmaticus’ defined as asthma that had failed to resolve with therapy in 24 hours. replaced by • ‘acute severe asthma’, i. e. severe asthma that has not been controlled by the patient’s use of medication.

Patients with acute severe asthma typically have: inability to complete a sentence in one breath respiratory rate ≥ 25 breaths per minute tachycardia ≥ 110 beats/min (pulsus paradoxus, in 45% of cases) PEFR < 33 -50% of predicted normal or best ( < 200 L/M. )

LAB. Features suggesting very severe life-threatening attacks: normal or high Paco 2 > 6 k. Pa severe hypoxaemia, Sp. O 2 < 92% or Pa. O 2 < 8 k. Pa (60 mm. Hg) despite treatment with oxygen low and falling arterial p. H.
Features of life-threatening attacks are: silent chest, cyanosis feeble respiratory effort exhaustion, confusion or coma bradycardia or hypotension PEFR < 33% of predicted (100 L/M)

Near-fatal asthma • Raised Pa. CO 2 and/or requiring mechanical • Arterial blood gases should ventilation with • raised inflation pressures always be measured in asthmatic patients requiring admission to hospital.

Treatment of severe asthma 1. 2. 3. 4. 5. 6. Oxygen 40– 60% Nebulized salbutamol 5 mg or terbutaline 10 mg is repeated 4 -hourly. Add nebulized ipratropium bromide 0. 5 mg Hydrocortisone 200 mg i. v. is given 4 -hourly for 24 hours. Prednisolone is continued at 60 mg orally daily for 2 weeks. Arterial blood gases are measured; if the Paco 2 is greater than 7 k. Pa, ventilation should be considered. 7. A chest X-ray , to exclude pneumothorax. 8. One of the following intravenous infusions is given if no improvement is seen: salbutamol 3– 20 μg/min, or terbutaline 1. 5– 5. 0 μg/min, or magnesium sulphate 1. 2– 2 g over 20 min

Hospital stay • Kept patients in hospital for at least 5 days, sudden deaths occur 2– 5 days after admission. • oxygen saturation monitored by oximetry. • Oral prednisolone can be reduced from 60 mg to 30 mg once improvement occurs • Further reduction should be gradual on an outpatient basis until an appropriate maintenance dose or substitution by inhaled corticosteroid aerosols can be achieved.

Recent advance bronchial thermoplasty: • A recent approach for moderate to severe persistent asthma • This bronchoscopic procedure reduces the mass of airway smooth muscle, reducing bronchoconstriction, and is being evaluated.
- Slides: 13