Management of Adult Fever and Sepsis MLP EM













- Slides: 14

Management of Adult Fever and Sepsis MLP EM Education Curriculum Dave Markel September 15, 2015

What will be covered • Basic concepts and definitions • Initial management • Septic shock • Pearls and pitfalls

What will not be covered • Pediatric fever (Scheduled for May 2017, Dr. Justice) • Febrile seizures • Hyperthermia • Environmental • Drug-induced

Basic concepts and definitions • Fever: temp > 37. 8 C = 100 F (CDC definition) • Not “I’m usually at 96 degrees so 98. 6 is a fever for me” • Not “It feels kinda warm in here” • Not “I had a chill the other day” • Most reliable way of checking the temperature? • No axillary temps, please!

Basic concepts and definitions • Systemic inflammatory response syndrome (SIRS) • At least 2 of the following: • • Oral temperature > 38 or < 35 C Respiratory rate > 20 or Pa. CO 2 < 32 mm. Hg (requires ABG) Heart rate > 90 Leukocytes > 12, 000 or < 4, 000 or >10% bands • Sepsis: + microbial source • Severe sepsis: + organ dysfunction • Septic shock: + hypotension unresponsive to fluids • Multiple organ dysfunction syndrome (MODS)

Sick vs Not Sick • Patients with any of the following need IMMEDIATE intervention • • Altered mental status Respiratory distress Cardiovascular instability Prolonged temp > 41 C = 105. 8 F

Most aren’t critically ill… take a history! • Localizing symptoms • Atypical symptoms • Fever patterns • Tubes, lines, drains (incl. pacemakers, heart valves, PICC lines, etc) • Living situation (nursing home, dorm, jail, etc) • Recent hospitalizations

Never trust the elderly • Symptoms are often atypical • May not even mount a fever response • Abdominal exam often deceptively benign • 3 critical things to do when evaluating fever in the elderly • Completely undress and examine skin • Chest x-ray (2 -view if possible) • Urinalysis (straight cath if possible)

Sepsis: a problem with perfusion • For MIS: sepsis is caused by a complex disarray of pro-inflammatory and anti-inflammatory mediators which are triggered by infection, leading to tissue ischemia, direct tissue injury, alterations in apoptosis • For us: sepsis = poor perfusion… fix it • • Hypotension Elevated lactate Tachycardia Decreased urine output

How to fix the perfusion problem • IV fluids • Initial choice: 0. 9% NS • Optimal volume unknown… usually will get 3 -5 liters over first 6 hours • Watch for pulmonary edema • Vasopressors • Initial choice: norepinephrine (Levophed) • Consider phenylephrine if tachycardia or dysrhythmias

Targets: first 6 hours •

Pro. CESS, 2014: “In a multicenter trial conducted in the tertiary care setting, protocol-based resuscitation of patients in whom septic shock was diagnosed in the emergency department did not improve outcomes. ” ARISE, 2014: “In critically ill patients presenting to the emergency department with early septic shock, EGDT did not reduce all-cause mortality at 90 days. ” Pro. MISe, 2015: “In patients with septic shock who were identified early and received intravenous antibiotics and adequate fluid resuscitation, hemodynamic management according to a strict EGDT protocol did not lead to an improvement in outcome. ”

Bonus: empiric abx (if source unknown) • Gram-positives and MRSA: vancomycin • Gram-negatives: 3 rd- or 4 th generation cephalosporin (eg, ceftriaxone) • Pseudomonas: zosyn, ceftazidime

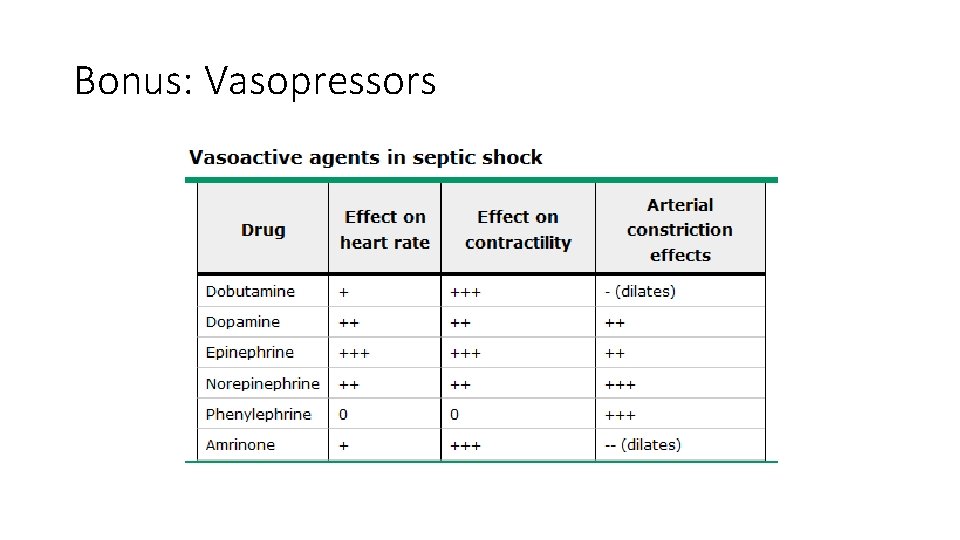
Bonus: Vasopressors