Managed Care Innovation Value Based Reimbursement in the

Managed Care Innovation Value Based Reimbursement in the Ohio Medicaid Program 6/29/2018 | Presented by: Holly Saelens, Vice President of Government Contracts
The Molina Mission Our Vision Our Mission Core Values We envision a future where everyone receives quality health care. To provide quality health care to persons receiving government assistance. Caring Enthusiastic Respectful Focused Thrifty Accountable Feedback One Molina
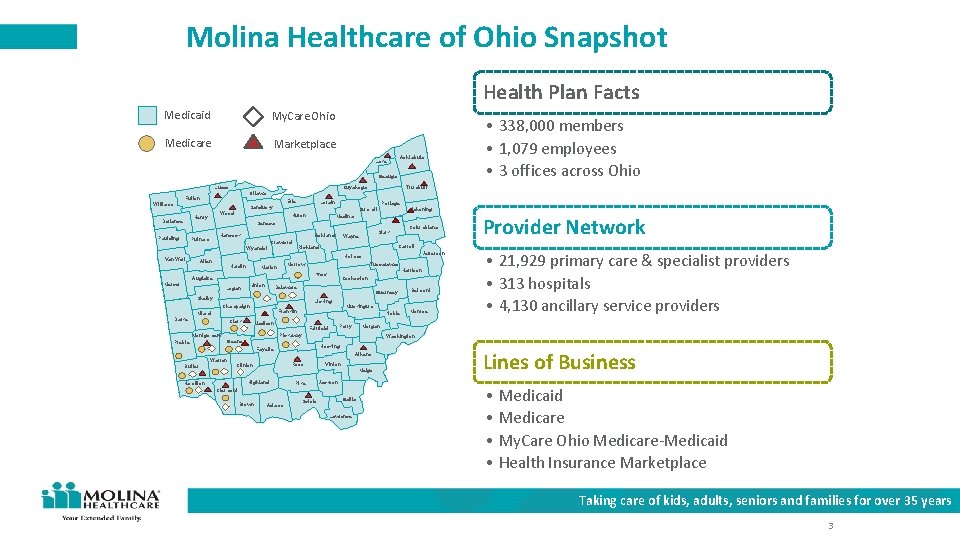
Molina Healthcare of Ohio Snapshot Health Plan Facts Medicaid My. Care Ohio Medicare Marketplace Ashtabula Lake Geauga Lucas Trumbull Cuyahoga Ottawa Fulton Erie Williams Lorain Sandusky Portage Summit Wood Henry Defiance Huron Mahoning Medina Seneca Paulding Hancock Putnam Ashland Crawford Hardin Morrow Marion Union Logan Guernsey Licking Champaign Clark Muskingum Franklin Miami Noble Madison Montgomery Perry Fairfield Warren Athens Vinton Meigs Highland Hamilton Pike Jackson Clermont Brown Adams Monroe Washington Hocking Ross Clinton Belmont • 21, 929 primary care & specialist providers • 313 hospitals • 4, 130 ancillary service providers Morgan Pickaway Greene Fayette Butler Harrison Coshocton Delaware Shelby Preble Jefferson Tuscarawas Knox Mercer Provider Network Carroll Holmes Allen Auglaize Darke Columbiana Stark Wayne Richland Wyandot Van Wert • 338, 000 members • 1, 079 employees • 3 offices across Ohio Scioto Gallia Lawrence Lines of Business • Medicaid • Medicare • My. Care Ohio Medicare-Medicaid • Health Insurance Marketplace Taking care of kids, adults, seniors and families for over 35 years 3

Managed Care Drives Innovation Value-based Purchasing Well structured, value-based agreements increase access to care, raise health awareness, promote early detection, improve outcomes and reduce cost. Through these initiatives, providers are eligible to receive additional payments when they achieve a quality goal as outlined in their contract. While metrics may vary amongst plans, most MCPs apply similar metrics related to primary and preventive care and often utilize national quality standards. By 2020, all Medicaid managed care plans must link 50 percent of provider payment to value. Taking care of kids, adults, seniors and families for over 35 years

Ohio SIM - Paying for Value Ohio brings a team together: • Focus on paying for value instead of volume. • Partnership and standardization to include ODM, MCPs and private sector partners. • Partners agree to align on 2 value models: Episodes of Care + Ohio CPC Align 50% of Molina’s Medicaid claims payment to value-oriented programs by 2020 Taking care of kids, adults, seniors and families for over 35 years 5

Ohio SIM - Paying for Value Episodes of Care + Ohio CPC Episodes of Care Retrospective Model Episodes growing in variety Upside-downside incentive payments 3 episodes in CY 2016 o 17 providers penalized $134 to $29, 036 o 29 providers rewarded $193 to $43, 451 • 43 episodes starting CY 2018 • • + Ohio Comprehensive Primary Care • Launched 1/1/2017 • Voluntary, population health focused • PCPs must meet activity, efficiency and clinical metrics • PMPM + Shared Savings • Over 30% of Medicaid members impacted, nearing 50% by 1/1/2018 • 111 Practices participating with up to 91 additional in 2018 Taking care of kids, adults, seniors and families for over 35 years 6
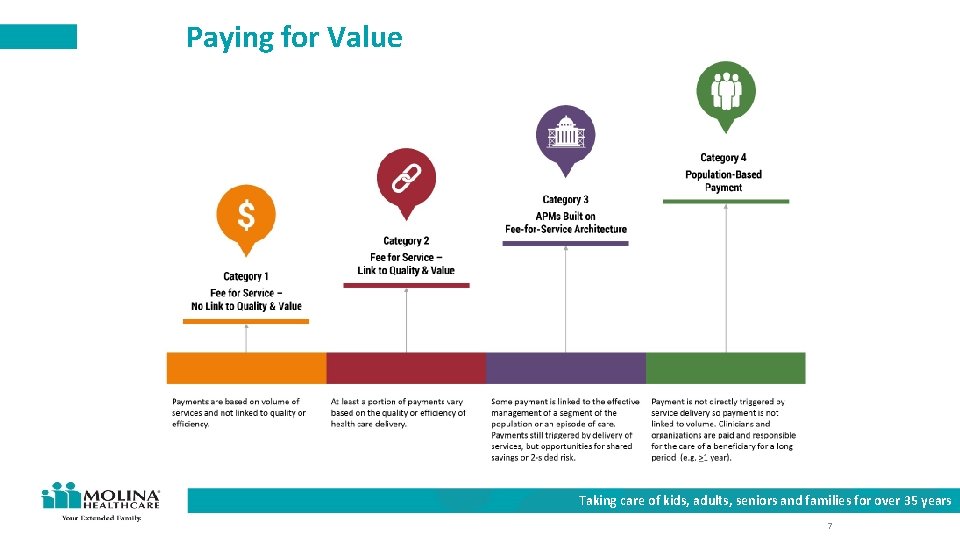
Paying for Value Taking care of kids, adults, seniors and families for over 35 years 7

Managed Care Plan Performance Quality Withhold Program The Kasich Administration established a Quality Withhold Program in HB 49 to replace the P 4 P program. ODM will withhold 2% of the MCPs capitation and delivery payments beginning April 2018. ODM will use Quality Indices to calculate the amount of the withhold payout. Quality Indices are comprised of multiple performance measures related to the index topic. Quality Indices measure the effectiveness of the MCP’s population health management strategy and quality improvement programs to impact population health outcomes. Performance will be assessed on four equally weighted Quality Indices. The Quality Indices used in the Quality Withhold program for SFY 2019 (measurement year 2018) are: • • Chronic Condition: Cardiovascular Disease Chronic Condition: Diabetes • • Behavioral Healthy Children Each index is composed of multiple quality measures which are assigned different weights. Taking care of kids, adults, seniors and families for over 35 years

CICIP- Overview for Managed Care Projected launch date July 1, 2018 (pending CMS approval) • • • Purpose - to increase alignment of quality improvement strategies between ODM, MCP, and public/nonprofit hospital agencies. Focus - improve healthcare and coordination of care for members with opioid or other substance use disorders. Participants will receive a quality measure incentive for meeting the following metrics: Taking care of kids, adults, seniors and families for over 35 years © 2016 MOLINA HEALTHCARE, INC. – INTERNAL USE ONLY 9

CICIP - Overview for Managed Care Taking care of kids, adults, seniors and families for over 35 years © 2016 MOLINA HEALTHCARE, INC. – INTERNAL USE ONLY 10
- Slides: 10