MALNUTRITION EnergyYielding Nutrients Carbohydrates1 gr4 kcal Proteins1 gr4



MALNUTRITION
Energy_Yielding Nutrients Carbohydrates(1 gr=4 kcal) Proteins(1 gr=4 kcal) Fat(lipids)(1 gr=9 kcal)


MALNUTRITION CLAUDE PICHARD. 2009


Malnutrition is associated with; Increased morbidity and mortality Delayed wound healing Increased length of hospitalization Increased complications Immunosuppression Organ impairment
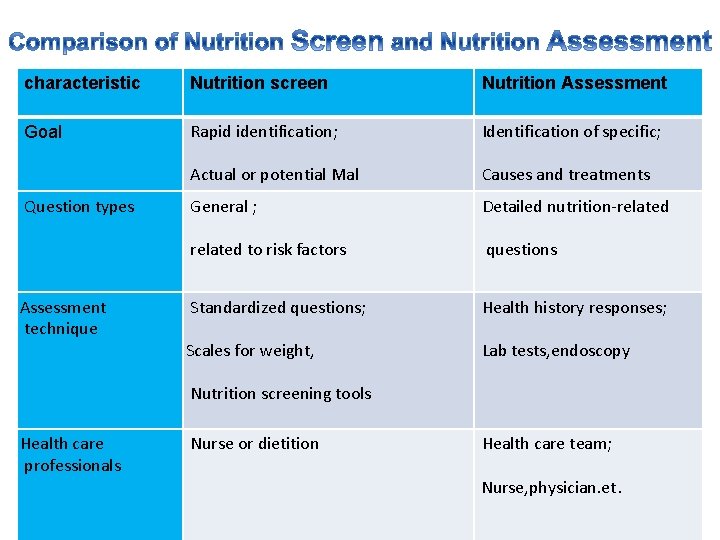
characteristic Nutrition screen Nutrition Assessment Goal Rapid identification; Identification of specific; Actual or potential Mal Causes and treatments General ; Detailed nutrition-related to risk factors questions Standardized questions; Health history responses; Scales for weight, Lab tests, endoscopy Question types Assessment technique Nutrition screening tools Health care professionals Nurse or dietition Health care team; Nurse, physician. et.

Features of the Admission Nutrition Screening Tool A. Diagnosis If the client has one or more of the following condition, circle it, proceed to section E and consider the client AT NUTRITIONAL RISK. If the client has none of these condition, proceed to section B. ●Anorexia nervosa /bulimia nervosa ●Cachexia (temporal wasting, muscle wasting, cancer, cardiac disease) ●Coma ●Diabetes ●End_stage liver disease ●End- stage renal disease ●Malabsorption (celiac sprue, ulcerative colitis, crohn’s disease, shortbowel syndrome) ●Major gastrointestinal surgery within the past year ●Multiple trauma(closed-head injury, penetrating trauma, multiple fractures) ●Pressure ulcers ●Nonhealing wounds

B. Nutrition Intake Historory If the client has one or more of the following manifestations, circle it, proceed to section E, and consider the client AT NUTRITIONAL RISK. If the client has none of these manifestations, proceed to section C. ●Diarrhea(>500 ml for 2 days) ●Vomiting(>5 days) ●Reduced intake(1/2 normal intake for more than 5 days) C. Ideal body weight standards Compare the client’s current weight for height to a chart of ideal body weight. If the client weighs less than 80%of ideal body weight, proceed to section E and consider the client AT NUTRITIONAL RISK. If the client weighs more than 80% of ideal body weight, proceed to section D.
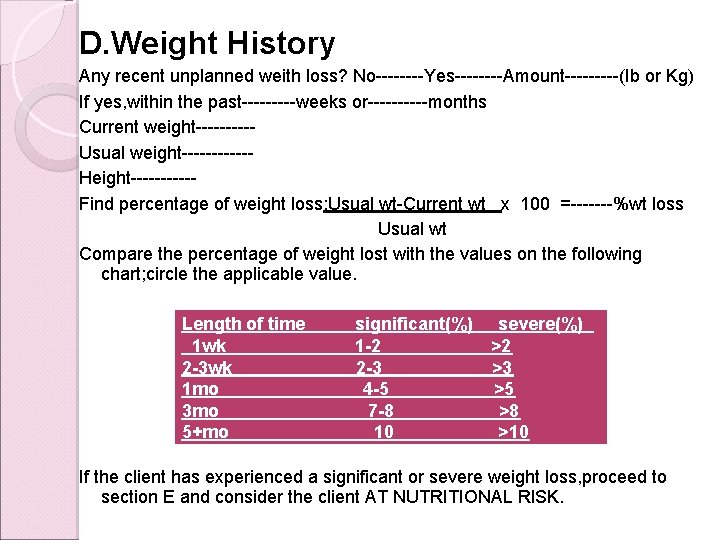

D. Weight History Any recent unplanned weith loss? No----Yes----Amount-----(Ib or Kg) If yes, within the past-----weeks or-----months Current weight-----Usual weight------Height-----Find percentage of weight loss: Usual wt-Current wt x 100 =-------%wt loss Usual wt Compare the percentage of weight lost with the values on the following chart; circle the applicable value. Length of time 1 wk 2 -3 wk 1 mo 3 mo 5+mo significant(%) severe(%) 1 -2 >2 2 -3 >3 4 -5 >5 7 -8 >8 10 >10 If the client has experienced a significant or severe weight loss, proceed to section E and consider the client AT NUTRITIONAL RISK.

E. Nurse Assessment Using the above criteria, what is this client’s nutritional risk? (check one) -----------LOW NUTRITIONAL RISK -----------AT NUTRITIONAL RISK

Assessing nutritional status Collection of four types of information; ♠Anthropometric measurements (weight, height) ♠Biochemical data (hb, hct, Alb, pre. Alb, Transferin, lymp) ♠Clinical signs(physical examination) ♠Diet and health history
![BMI=WEIGHT÷HEIGHT² For men; height=6419 -(0. 04×age in years)+(2. 02×knee height[cm]) For women; height=84. 88 BMI=WEIGHT÷HEIGHT² For men; height=6419 -(0. 04×age in years)+(2. 02×knee height[cm]) For women; height=84. 88](http://slidetodoc.com/presentation_image/565b2b9aa5bac4eea3070288da0d6a7e/image-15.jpg)
BMI=WEIGHT÷HEIGHT² For men; height=6419 -(0. 04×age in years)+(2. 02×knee height[cm]) For women; height=84. 88 -(0. 24×age in years)+(1. 83×knee height[cm])
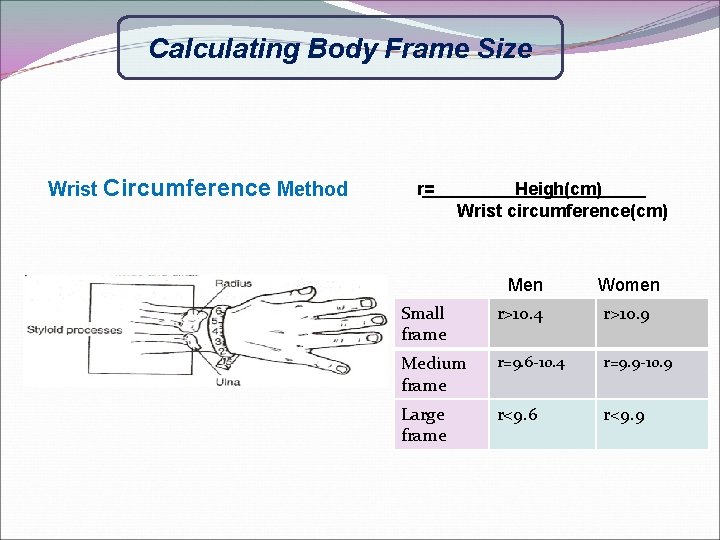
Calculating Body Frame Size Wrist Circumference Method r= Heigh(cm) Wrist circumference(cm) Men Women Small frame r>10. 4 r>10. 9 Medium frame r=9. 6 -10. 4 r=9. 9 -10. 9 Large frame r<9. 6 r<9. 9
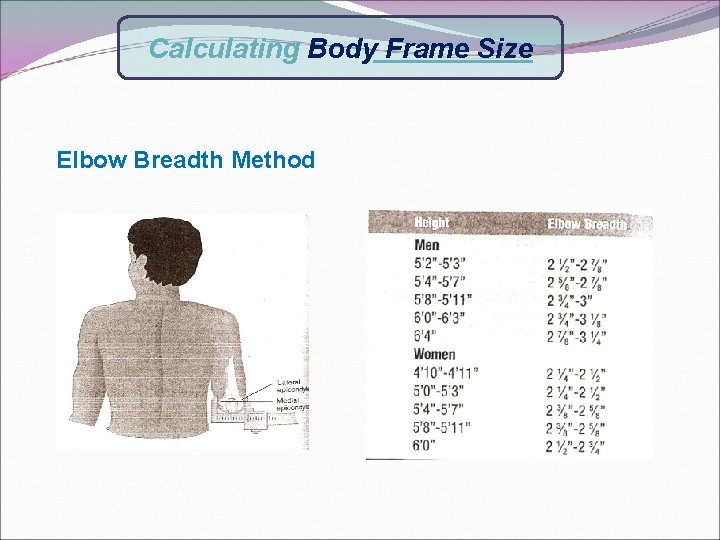
Calculating Body Frame Size Elbow Breadth Method
Nutrition and cardiovascular alterations A ♣Overweight or obsity; underweight ♣Abdominal fat B ♣Elevated serum chol, l. Dl, Tig C ♣Wasting of muscle and subcutaneous fat

D ♣Sedentary lifestyle ♣Excessive intake of saturated fat, chol, alcohol, Na ♣Angina, respiratory difficulty, or fatigue during eating medication that impair appetite (e. g. , digitalis, quinidin)
Nutrition and pulmonary alterations A ♣Underweight. Slide 14 B ♣Elevated pco 2 related to overfeeding C ♣Edema, dyspnea, signs of PE related to fluid volume excess

D ♣Poor food intake related to dyspena, unpleasant taste in the mouth from sputum production or bronchodilator therapy; endotracheal intubation preventing oral intake
Nutrition and neurologic alterations A ♣Underweight B ♣Hyperglycemia(with corticosteroid use) C ♣Wasting of muscle and subcutaneous fat related to disuse or to poor food intake

D ♣Poor food intake related to altered state of consciousness, dysphagia or other chewing or swallowing difficulties, ileus resulting from spinal cord injury or use of pentobarbital ♣Hypermetabolism resulting from head injury ♣pressure ulcers
Nutrition and renal alteration A ♣Underwight(may be masked by edema) B ♣Electrolyte imbalances ♣Hpo. Alb related to protein restriction and aminoacid losses in dialysis ♣Anemia ♣Hypertriglyceridemia

C ♣Wasting of muscle and subcutaneus tissue D ♣Poor dietary intake related to protein and electrolyte restrictions and alterations in taste

Nutrition and gastrointestinal alterations A ♣Underweight related to malabsorption, anorexia, or poor intake B ♣Hypo. Albuminemia ♣Hypomagnesemia ♣Anemia

C ♣Wasting of muscle and subcutaneus ♣Confusion, nystagmus, and/or peripheral neuropthy related to thiamine deficiency (alcohol abuse) D ♣Steatorrhea
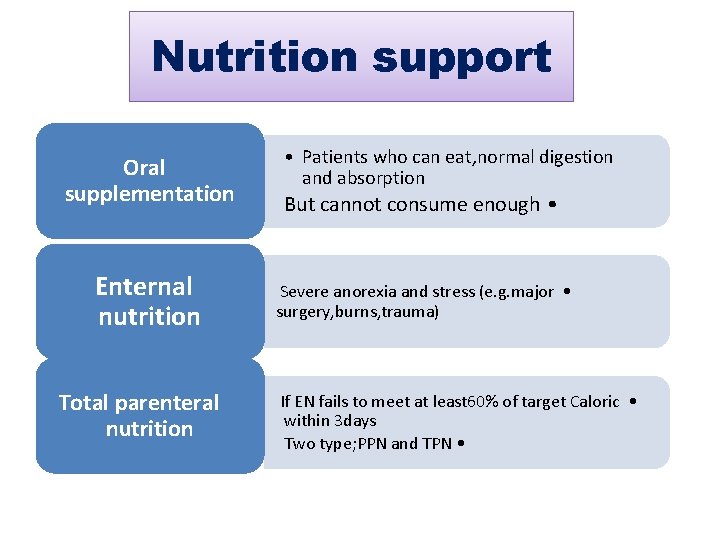
Nutrition support Oral supplementation Enternal nutrition Total parenteral nutrition • Patients who can eat, normal digestion and absorption But cannot consume enough • Severe anorexia and stress (e. g. major • surgery, burns, trauma) If EN fails to meet at least 60% of target Caloric • within 3 days Two type; PPN and TPN •
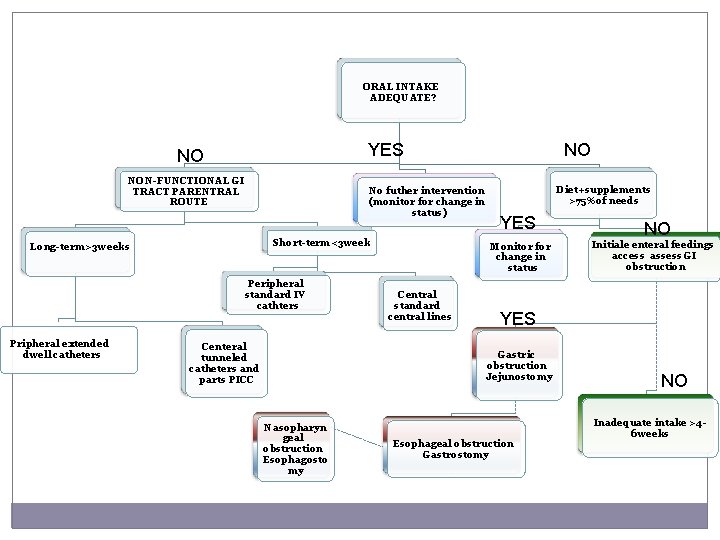
ORAL INTAKE ADEQUATE? YES NO NON-FUNCTIONAL GI TRACT PARENTRAL ROUTE No futher intervention (monitor for change in status) Short-term<3 week Long-term>3 weeks Peripheral standard IV cathters Pripheral extended dwell catheters Centeral tunneled catheters and parts PICC NO Diet+supplements >75%of needs YES Monitor for change in status Central standard central lines Initiale enteral feedings access assess GI obstruction YES Gastric obstruction Jejunostomy Nasopharyn geal obstruction Esophagosto my NO Esophageal obstruction Gastrostomy NO Inadequate intake >46 weeks
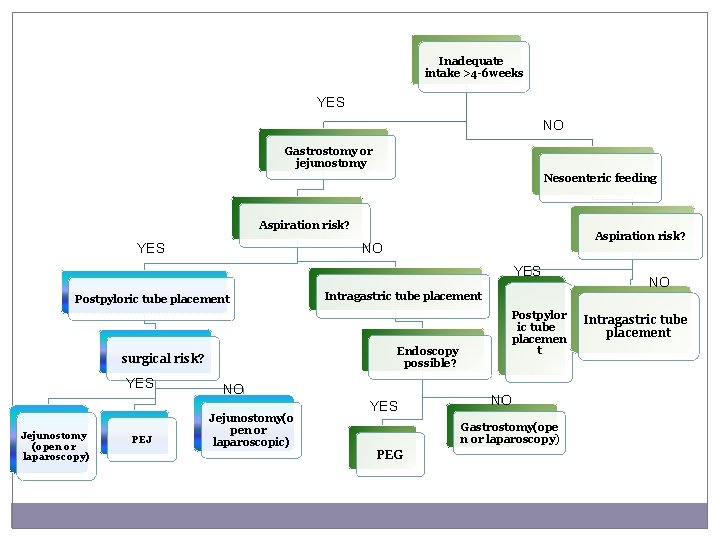
Inadequate intake >4 -6 weeks YES NO Gastrostomy or jejunostomy Nesoenteric feeding Aspiration risk? YES Aspiration risk? NO YES Postpyloric tube placement Endoscopy possible? surgical risk? YES Jejunostomy (open or laparoscopy) PEJ Intragastric tube placement NO Jejunostomy(o pen or laparoscopic) YES Postpylor ic tube placemen t NO Gastrostomy(ope n or laparoscopy) PEG NO Intragastric tube placement
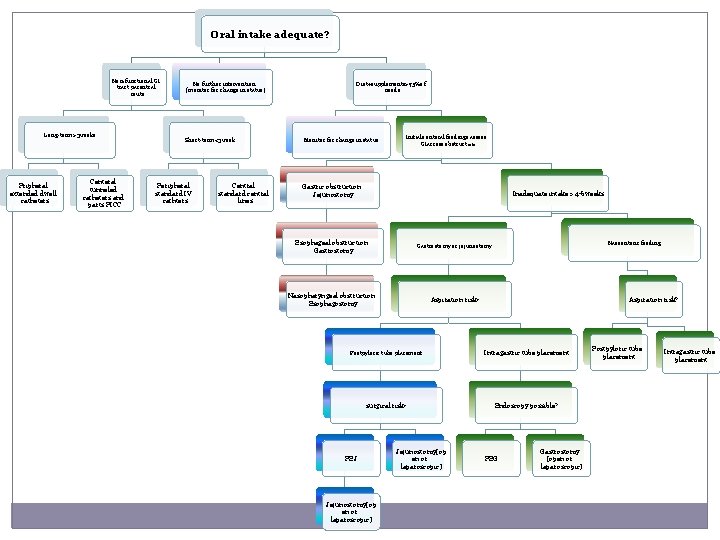
Oral intake adequate? Non-functional GI tract parentral route Long-term>3 weeks Pripheral extended dwell catheters Centeral tunneled catheters and parts PICC No further intervention (monitor for change in status ) Short-term<3 week Peripheral standard IV cathters Central standard central lines Diet+supplements>75%of needs Monitor for change in status Initiale enteral feedings assess GIaccess obstruct ion Gastric obstruction Jejunostomy Inadequate intake >4 -6 weeks Esophageal obstruction Gastrostomy or jejunostomy Nasopharyngeal obstruction Esophagostomy Aspiration risk? Nasoenteric feeding Aspiration risk? Postpyloric tube placement Intragastric tube placement surgical risk? Endoscopy possible? PEJ Jejunostomy(op en or laparoscopic) PEG Gastrostomy (open or laparoscopic) Postpyloric tube placement Intragastric tube placement


☻Anthropometric measurements(daily weights, I&O) ☻ Biochemical evaluation(serum levels of BUN, electrolytes, BS, Ca, Ph, Alb, Tig, …) ☻ Physical examination
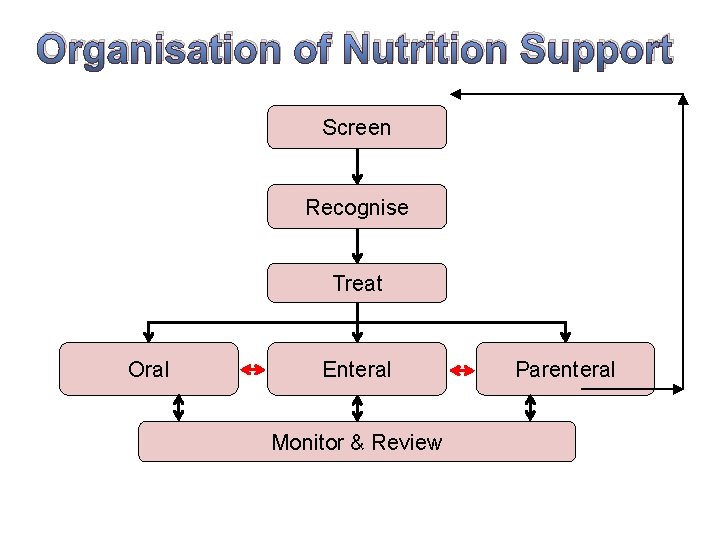
Organisation of Nutrition Support Screen Recognise Treat Oral Enteral Monitor & Review 3. NICE Guidelines for Nutrition Support in Adults 2006 Parenteral

Reference 1 pichard. C, Thibault. R, Heidegger. C, Genton. L; Enternal and parenteral nutrition for critically ill patients; Alogical combination to optimize nutritional support. Clinical Nutrition Suplements 2009; 4: 3 -7. 2. Urden. L, stacy. K, E. lough. M. Thelan’s critical care Nursing. 5 th edition; Mosby; 2008. pp: 94 -119 3. Morton. P, Fontaine. D. Critical Care Nursing: A holistic Approch. 9 th edition; Wolters Kluwer, lippincott Wilkins; 2008. pp: 1015 -1017 4. Black. J, Hawks. J. Medical Sergical Nursing. 7 th edition; Elsevier; 2005. pp: 670700 5. Bockenkamp. B, Jouvet. P, Arsenault. V, Beausejour. M, Annepelletier. V; Assessment of caloriec prescribed and delivered to critically ill children. e-spen, the European e-Journal of clinical Nutrition and Metabolism 2009; 4: e 172 -e 175

THANK YOU
- Slides: 36