MALIGNANT TUMOURS OF THE BREAST BY DR HOSAM

MALIGNANT TUMOURS OF THE BREAST BY DR. HOSAM ELSROGY

SARCOMA Incidence Pathology 1. General incidence: rare (0. 5 -1% of malignant tumors of the breast). 2. Age incidence: the commonest age ranges between 30 & 40 years. It may develop de novo or o top of soft fibroadenoma. 1. It includes fibrosarcoma, liposarcoma, rhabdomyosarcoma & angiosarcoma. 2. M. P: Spindle cell sarcoma (the commonest type), round cell sarcoma, or mixed cell sarcoma. Clinical Picture The tumor forms a fleshy massive swelling, which infiltrates the breast, does not fix (usually) to the underlying structures but fungates through the skin & disseminates to lungs & viscera. 1. The swelling is highly vascular with variable consistency. The skin becomes stretched & shows dilated veins. Lymph nodes are characteristically not necessarily enlarged.

Differential Diagnosis: 1. Breast Abscess Severe throbbing pain Fired skin Firing edema Temperature 39 -40°C Leucocytosis Pus on aspiration Sarcoma Mild pain. Dusky red skin Non-pitting edema Temperature 37 -3 8°C No pus on No leucocytosis aspiration 2. Encephaloid carcinoma (areas of cystic degeneration are usually suggestive of sarcoma). 3. Cystosarcoma phylloides Treatment: A multimodality treatment: Simple mastectomy + Radiotherapy + Chemotherapy. Prognosis: Prognosis is usually very poor.

CARCINOMA INCIDENCE : General Incidence Age Sex Race Site ETIOLOGY / RISK FACTORS Reproductive Experience Ovarian Activity Hormonal Factors Age Sex Race Genetic predisposition Multiple 1 ry cancers Diet & Obesity Precancerous conditions& carcinogens

INCIDENCE: General Incidence: It is the commonest malignant tumor in women (= 25% of all female cancers). Age: Any age after puberty can be affected with a maximum incidence at 40 -50 Y (till menopause). There may be two peaks of incidence; at 45 & 65 years of age. Sex (Gender): Female to male ratio is 99: 1. Race: It affects white races > black races. It is more common in USA & Europe than in Japan. Site: The upper outer quadrant (containing the axillary tail) is the commonest site & the lower inner quadrant is the least affected , tubular carcinoma has special characteristics ; multicentricity & bilaterality

PATHOLOGY Gross appearance Histological types 1 -Foot & stewart classification . Paget`s disease . carcinoma of duct origin . carcinoma of lobular origin 2 -Ackermann classification . neoplasms of mamary tissue . malignant mesenchymal neoplasm . malignant neoplasm of skin & skin adnexa . metastatic neoplasms

Gross appearance 1. A hard, poorly defined, grayish white mass with areas of hemorrhage and necrosis ± calcification. 2. Ramifying processes are seen extending from the tumor to the surrounding tissue. 3. Extension of the tumor through the fascia and muscles leads to its fixation. 4. The skin may be involved leading to ulceration or nodule formation. 5. Lymph nodes may be involved. They become enlarged, hard and may be matted. A cut section shows grayish yellow areas due to metastatic deposits. Histological types

I. Foote & Stewart Classification 1. Paget's disease of Nipple 2. Carcinoma of Duct Origin A. Non-infiltrating (in-situ, intraductal) B. Infiltrating: a) Scirrhous (carcinoma simplex). b) Medullary. c) Colloid. d) Comedo. 1. Papillary. 2. Tubular. 3. Carcinoma of Lobular Origin A. Non-infiltrating (in-situ). B. Infiltrating:

2 -Ackermann classification neoplasmes of mammary tissue; A. . neoplasmes of lobular epithelial origin: 1. lobular carcinoma in situ 2. lobular carcinoma invasive B neoplasmes of ductal epithelial origin 1. non infiltrating carcinoma a. intraductal carcinoma, non invasive b. intracystic papillary carcinoma, non invasive 2. infiltrating ductal carcinoma: a)carcinoma simplex = non-otherwise specified b) special types. scirrhous. medullary. colloid (mucoid, mucinous). comedo. papillary. cribriform. secretory C. unusual presintations: 1. inflamatory carcinoma 2. pagets disease of the nipple& areola

MALIGNANT NEOPLASMES OF MESENCHYMAL ORIGIN; 1. SARCOMA 2. LYMPHOMA MALIGNANT NEOPLASMES OF SKIN& SKIN ADNEXA: skin neoplasmes: squamous cell carcinoma, basal cell carcinoma. Skin adnexa neoplasmes; carcinoma of sweat or sebaceous glands METASTATIC NEOPLASMES: 1. FEMALES; adults: from melanoma, other breast, endocrinal tumors children: from hemopoitic tumors rabdomyosarcoma 2. MALES: from prostatic carcinoma
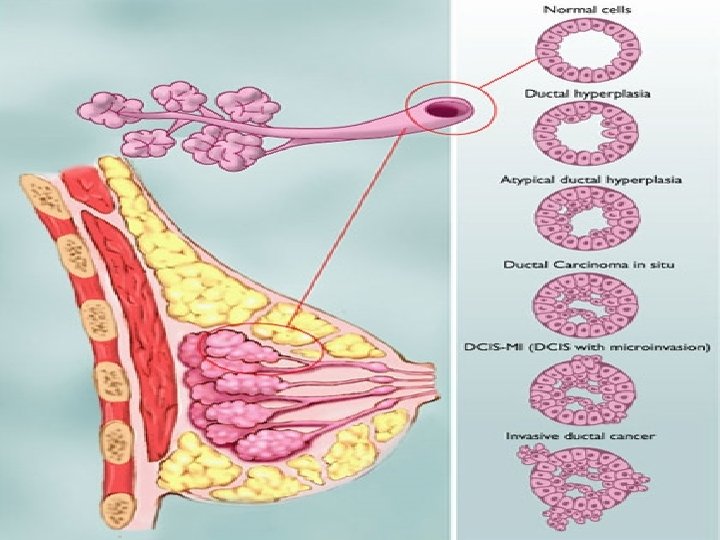
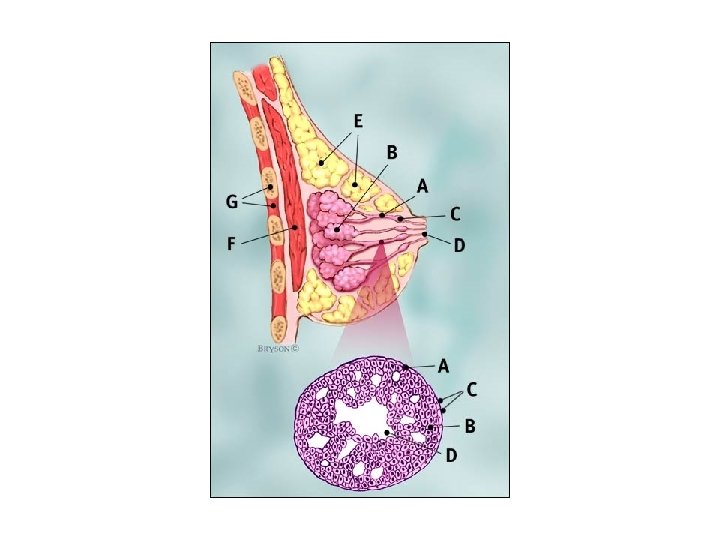

A. Lobular Carcinoma 1. Carcinoma originating in the terminal ductules of the lobules. It is often bilateral & family history may be positive. It is either non-invasive (msitu) or invasive. 2. M. P: Terminal lobules are packed with small, hyperplastic, uniform cells, often arranged in rows or beads with mitoses, hyperchromatism & nuclear anaplasia.

B. Ductal Carcinoma 1. Non-infiltrating (Ductal Carcinoma in-situ = DCIS): The cells have the microscopic characteristics of malignancy but do not invade the basement membrane of the ductal epithelium. Multicentricity within the same (ipsilateral) breast is common. 2. Infiltrating Duct Carcinoma (IDC): a) Scirrhous Carcinoma (simplex = IDC with productive fibrosis): 1. It is the commonest variety constituting about 75 -80% of invasive carcinomas. 2. It is so called because of its hard consistency & occurs typically in middle-aged females. NEA: The tumour is rather small in size and may be fixed firmly within the breast substance, and lies most often in the upper outer quadrant (UOQ). When sectioned with a knife, the cut surface: Gives a gritty sensation (due to small spiules of calcification). Becomes concave due to its retraction. Has a gray color with yellow specks of necrotic tissue. Has an infiltrating edge without any form of capsule.

M. P: Irregular groups and columns of spheroidal cells in a dense fibrous tissue stroma. There is a great variation in cellularity; in some cases the malignant cells are relatively scanty, presenting finger-like processes in the copious stroma; in others there are solid masses of tumor cells with relatively little connective tissue. Mitotic figures are present only in small numbers, because the tumor grows slowly & cell division is infrequent. b) Medullary (Encephaloid) Carcinoma: 1. It occurs typically in well-developed breasts of young women, in the form of a rapidly growing large fleshy mass which infiltrates widely & disseminates early 2. NEA: brain-like cut surface (encephaloid) with areas of hemorrhages & necrosis. M. P: Masses of highly malignant cells with marked lymphocytic infiltration supported in a delicate vascular stroma.

c) Mucoid Carcinoma (Colloid or Mucinous Adenocaricnoma): 1. A rare type (1%) in the form of a bulky soft well-demarcated though noncapsulated mass with areas of mucoid degeneration & necrosis. It may reach an enormous size, but grows slowly & disseminates late so that the prognosis after operation is favorable. MP: the mucoid material distends the cells to form signet-ring shaped cells & may be set free in the intercellular stroma. d) Comedo Carcinoma: It has characteristic plugs of pasty material expressible from the surface of the neoplasm. NEA: Well-circumscribed, firm, grayish mass. M. P: Cores of highly cellular epithelial tissue with focal calcifications occluding the ducts.

e) Papillary Carcinoma: It has the lowest frequency of axillary nodal involvement with the best 5 year survival. It typically appears in younger age groups (35 -40 y). Nipple discharge (bloody) is common. NEA: Bulky mass, centrally located. M. P: Large sheets of cells with papillary formation. Cells show numerous mitoses, hyperchromatism, and loss of polarity f) Tubular Carcinoma: A rare (1%) well-differentiated ductal lesion that forms tubules. It has a relatively good prognosis.
C. Carcinomas with Unusual Presentation 1. Acute Inflammatory Carcinoma (Mastitis Carcinomatosa): 1. It is the most malignant form, but represents <3% of all cases. It is called inflammatory or lactational carcinoma as it usually occurs in the lactating hypertrophied breast. 2. The breast becomes diffusely swollen, painful, tender & hot on palpation, with dilated veins on the overlying skin so that the condition is often mistaken for acute mastitis. However, there is no pyrexia, no leucocytosis, no response to antibiotics, no tender lymph nodes (though enlarged), besides it is a rapidly growing & spreading tumor. 3. M. P: Very rapid proliferation of anaplastic cells with very little fibrous reaction so that the turnpr may resemble a sarcoma. The inflammatory changes are caused by carcinomatous invasion of the dermal lymphatics resulting in edema & hyperemia.
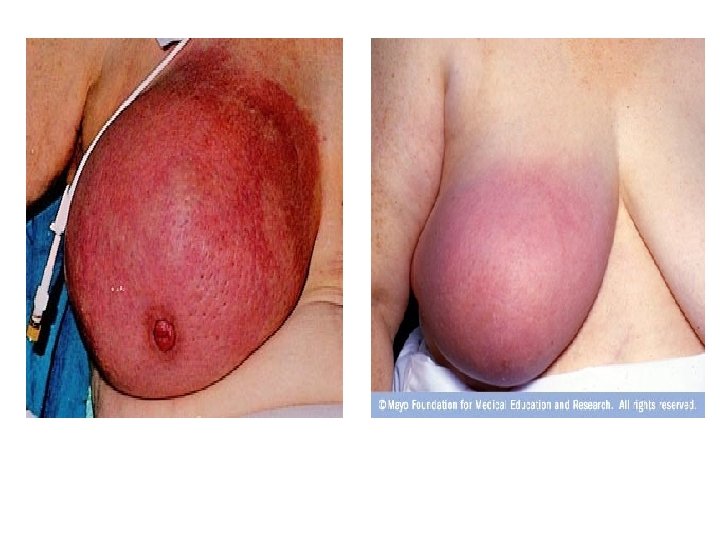
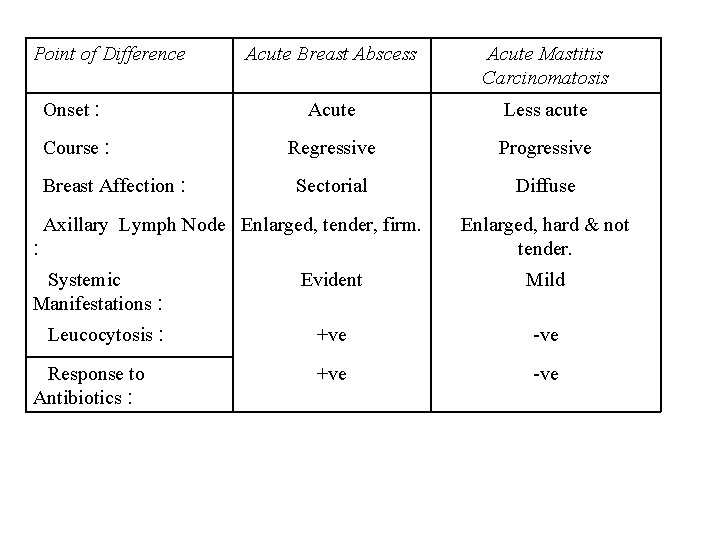
Point of Difference Acute Breast Abscess Acute Mastitis Carcinomatosis Onset : Acute Less acute Course : Regressive Progressive Sectorial Diffuse Breast Affection : Axillary Lymph Node Enlarged, tender, firm. : Systemic Manifestations : Leucocytosis : Response to Antibiotics : Enlarged, hard & not tender. Evident Mild +ve -ve

2. Paget's Disease: It is a rare disease (1%), of middle aged & elderly women. It begins as a malignant eczema (due to intradermal lymphatic obstruction, epitheliosis & invasion of dermis by Paget's cells. It erodes the nipple & spreads peripherally for about 2 years by which time a scirrhous carcinoma appears within the breast. It is believed to arise in the terminal ducts as an intraductal cancer, which spreads both, outvards to affect the nipple & skin, and inwards to produce the underlying carcinoma. M. P: by hyperplasia of all layers of epidermis with the presence of large vacuolated cells with small deeply stained nuclei in the deeper layers of the epidermis (Paget's cells) + epidermoid hypertrophy + subdermal round cell infiltration. N. B. Paget's disease may be extra-mammary affecting the axilla, groin, umbilicus, and perianal region.
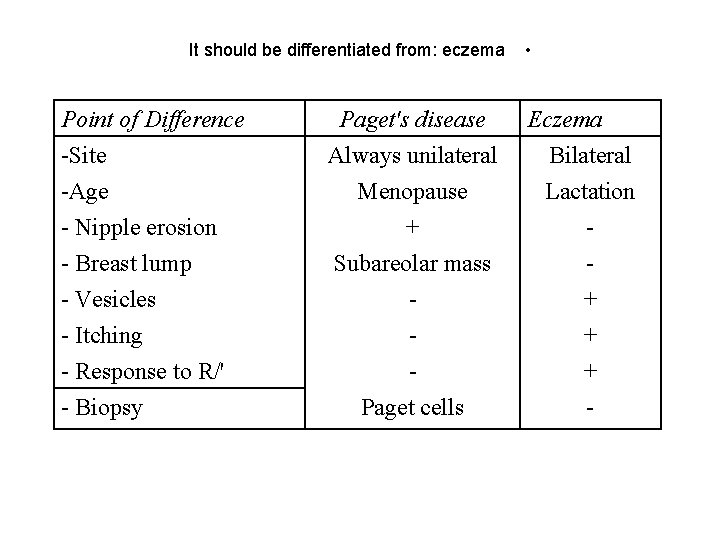
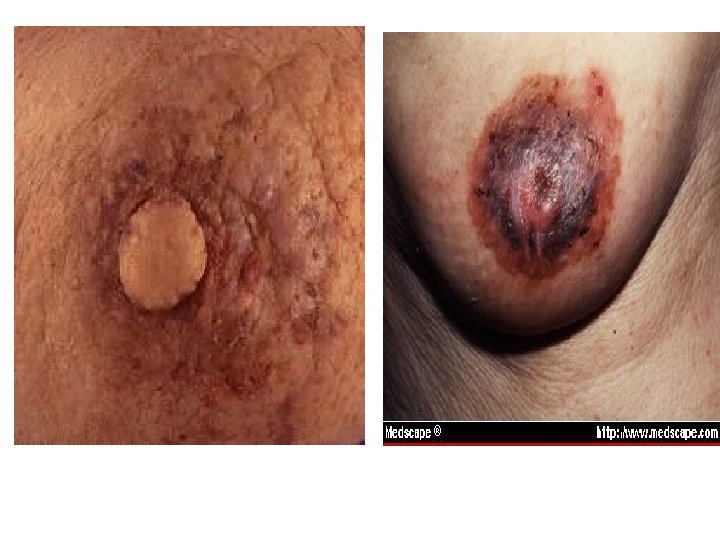
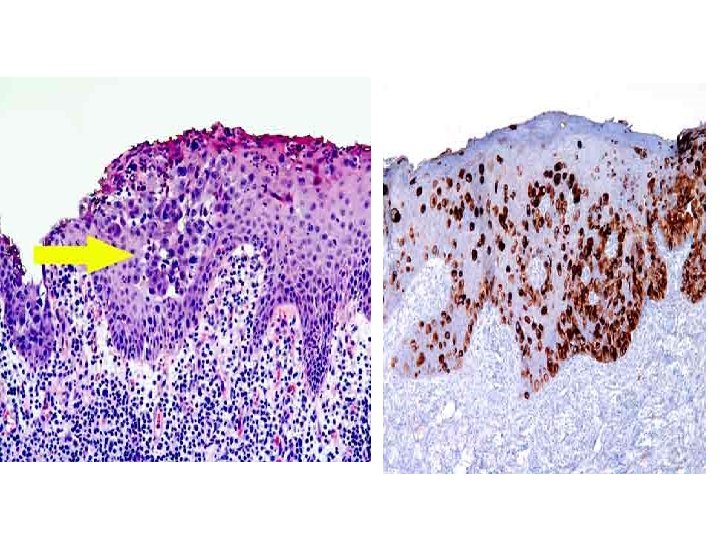

It should be differentiated from: eczema • Point of Difference -Site -Age - Nipple erosion Paget's disease Always unilateral Menopause + - Breast lump - Vesicles - Itching - Response to R/' - Biopsy Subareolar mass Paget cells Eczema Bilateral Lactation + + + -
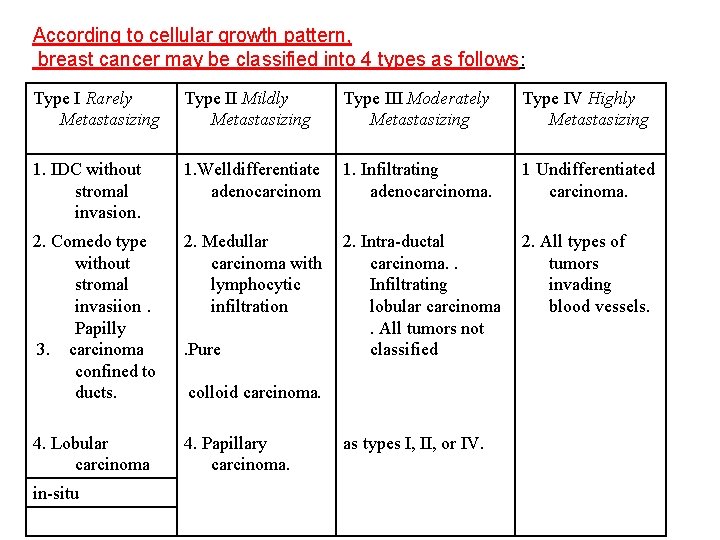
According to cellular growth pattern, breast cancer may be classified into 4 types as follows: Type I Rarely Metastasizing Type II Mildly Metastasizing Type III Moderately Metastasizing Type IV Highly Metastasizing 1. IDC without stromal invasion. 1. Welldifferentiate adenocarcinom 1. Infiltrating adenocarcinoma. 1 Undifferentiated carcinoma. 2. Comedo type without stromal invasiion. Papilly 3. carcinoma confined to ducts. 2. Medullar carcinoma with lymphocytic infiltration 2. Intra-ductal carcinoma. . Infiltrating lobular carcinoma. All tumors not classified 2. All types of tumors invading blood vessels. 4. Lobular carcinoma 4. Papillary carcinoma. in-situ . Pure colloid carcinoma. as types I, II, or IV.

SPREAD OF BREAST CANCER; 1. Direct (Local) Spread: 1. From the site of origin, malignant cells invade the surrounding "corpus mammae" & adjacent soft tissue & then spread to involve the overlying skin in various ways (dimpling, peau d'orange, nodules. . . etc). 2. In late cases, the tumor invades also deeply to involve the deep fascia & chest wall. 2. Lymphatic Spread: 1. The main drainage from the breast is towards the axilla. Usually the first L. Ns to be affected are those in the pectoral group, later the central & finally the apical group. In 5 -10% of unselected cases, the internal mammary L. Ns. are involved before the axillary L. Ns. 2. Once the tumor invades the lymph vessels, it spreads by permeation & embolization to the L. Ns, which become full with malignant cells & enlarge significantly. By permeation & embolization, malignant cells reach the subareolar & fascial pectoral plexuses, and then along other pathways: 3. Laterally —> axillary L. Ns (pectoral, central & apical) & then —> supraclaviculai L. Ns. 4. Medially -> internal mammary & mediastinal L. Ns. then -» opposite breast & axilla. 5. Upwards —> supraclavicular L. Ns directly. 6. Downwards -> rectus sheath, falciform ligament, liver & peritoneum. 7. Deeply —> infraclavicular L. Ns & then —> Apical axillary L. Ns by piercing the fascia. • Virchow 's L. Ns (left supraclavicular) are involved (=Trousier sign) via mediastinal L. Ns & thoracic duct.

3. Blood Spread: 1. Blood bome emboli are carried to the lungs first, and then through the pulmonary capillary bed to other sites (bones, brain, liver). 2. Bone metastases may occur without lung metastasis via vertebral veins where emboli pass via the intercostal veins to the vertebral system. The most common sites affected are the ribs, spine, skull, pelvis, and upper ends of femur & humerus. Bone metastases are almost always osteolytic wherever they occur; however, they may be osteosclerotic if the 1™ was of the scirrhous type. 3. Voluntary muscles are practically never involved (due to their metabolic property or because by contracting they expel the malignant cells before having time to engraft). 4. The spleen also, is rarely affected (it is not properly understood why? ) 4. Transcelomic Spread: 1. Spread reaches the peritoneum first, then the liver, pelvic organs & Douglas pouch (Plummer's shelf or Sheraton's shelf). Recently, involvement of the ovary (Krukenburg tumor (is believed to be by blood spread & not transcelomic because the outer surface of the ovary is almost always free

CLINICAL FEATURES; I. (Complaints) Symptoms A. Main Complaints: 1. Lump in the breast. 2. Pain (usually in late stages, except in mastitis carcinomatosa). 3. Discharge (blood-stained). It may be the first symptom as in duct carcinoma. B. Symptoms due to Spread: 1. Direct: skin, nipple & areola manifestations. 2. Lymphatic: Lump in the axilla (Lymph node enlargement). 3. Blood: Respiratory distress & hemoptysis (lungs), bone ache, pathological fractures (bones), malignant ascites or metastatic lumps (nodules) anywhere in the body.

II. Signs (Clinical Examination) General Examination: 1. Chest: Pleural effusion, pulmonary deposits & enlarged mediastinal L. Ns. 2. Abdomen: Hepatomegaly, malignant ascites & peritoneal deposits. 3. Pelvis: PV & PR examination to detect secondaries in the ovaries (Krukenburg's disease). 4. Bones: Tenderness, weakness, deformity & pathological fractures. Local & Regional Examination: 1. Lump in the Breast: A malignant tumor can be differentiated from a B. T. by the following characteristics: It is felt by the flat of the hand than by fingertips. It is not tender. It is stony hard, irregular better in shape, with ill-defined borders & flat deep surface. It may be anchored in its bed. Fixation to skin or chest wall occurs late. 2. Nipple Changes: Depression, Destruction, Discharge, • Displacement, Deviation, and Discoloration Recent Retraction It results from neoplastic fibrosis & lactiferous duct invasion. It should be differentiated from other causes of nipple retraction i. e. congenital & chronic inflammation. • Erosion (Destruction): It results from malignant eczema or Paget's disease.

• Discharge: Usually there is no nipple discharge, but in duct carcinoma a bloody discharge is present, and in scirrhous carcinoma, a crystal clear discharge is rarely observed. 3. Breast Changes: (Fibrosis causes the following): • It becomes puckered & displaced. • It is pulled upward on raising arms above the head • It does not protrude freely when the patient leans forwards. 4. Skin Changes: • Dimpling: It is the earliest manifestation & results from contraction or pull of the ligament of Cooper. It is more evident on raising the arm or leaning forwards. • Puckering: It is due to tumor attachment to the skin & fibrosis with enfolding of the skin. • Dilated veins: Due to increased vascularity of the breast & block of the venous return.

• Peau d'orange: Edema of the skin due to dermal & subdermal lymphatic obstruction. Sites of hair follicles appear as pits on the edematous skin as they are more attached to the subcutaneous tissue They may also occur with chronic breast abscess or FCD. • Skin lymphedema: Due to obstruction of the lateral lymphatic trunk (drains the breast skin). • Fixation of the skin to the tumor: Due to growth of the tumor beneath the skin. • Cancerous nodules & satellites: Due to retrograde tumor spread to the skin. • Malignant ulceration or fungation due to extensive skin invasion. • Cancer-en-Cuirasse (late): Indurated thickening of the skin due to diffuse infiltration of the dermis (skin) by malignant cells in addition to lymphedema (obstruction of the deep lymphatics). It extends as a semirigid case around the chest and may involve the neck, arm & trunk. • Inflammatory Signs: In case of acute cancer of pregnancy & lactation. • Nipple & areola changes

5. Opposite Breast: 1. Metastases may be detected on careful palpation, but when seen early, it seems more probable that it should be regarded as independent 1 ry growth. 2. Since the two breasts are identical in structure, in function, and in their response to hormonal influence it is not surprising that the liability to cancer is also shared. 3. It seems that in such cases both breasts have been the site of FCD especially such types as lobular carcinoma in-situ which gives multifocal nodules of true invasive cancer. 6. Lymph Nodes (L. Ns): Axillary & supraclavicular L. Ns on both sides should be examined for enlargement, consistency, tenderness & mobility. They become enlarged, hard, not tender, mobile but fixed later. 7. The Arms: The arms are palpated for swelling, skin nodules or other abnormalities. In late cases of cancer, the arm may be swollen due to lyrnphedema or venous thrombosis

III. Special Clinical Situations of Breast Cancer A. Inflammatory Carcinoma: Clinically, there is a rapidly growing mass, sometimes painful. The overlying skin is erythematous, edematous & warm. Often there is no distinct mass when the tumors infiltrate the breast diffusely, It should be differentiated from acute breast abscess. Diagnosis should be put in mind if redness involves >l/3 of the skin over the breast & if there is no response to antibiotics within 1 -2 weeks. B. Paget's Disease: C/O: Burning sensation with itching & tenderness, and occasionally, bleeding per nipple. The surface of the nipple & areola is encrusted, scaly, hyperemic & may be eroded & destroyed. A palpable subareolar mass may be felt. It should be differentiated from eczema.

C. Breast Cancer During Pregnancy & Lactation: 1. About 1 -2% of breast cancer occurs during pregnancy & lactation. 2. The problems encountered by the physician are the following: 3. The tumor is in adverse circumstances: (1) Delayed diagnosis due to enlargement of the breast which may mask the tumor, (2) increased hormone levels, lymphatics & hyperemia, (3) Reduced immunity, and (4) most tumors (70%) are estrogen receptor negative. Weapons are lacking: radiotherapy, chemotherapy & hormonal therapy are all contraindicated. Surgery may induce abortion in the 1 SI trimester or premature labor in the last trimester. D. Bilateral Breast Cancer: Breast cancer may occur simultaneously in both breasts in about 1% of cases, and later on (metachronous) in 5 -8% of cases. Bilaterality is more common in women below 50 years of age, lobular or comedo carcinoma, and positive family history. 1. E. Breast Cancer in Children & Adolescents: 2. Breast Cancer, whether carcinoma, sarcoma, or metastases from other areas, is rare in childhood & adolescence. At most, 3 -4 cases of Iry breast cancer/ year occur in women below 20 years, in USA. 3. • Any unusual appearance of a breast lesion at children is an indication for biopsy.

INVESTIGATIONS: I. Laboratory Investigations 1. General Tests: Complete blood picture, bleeding time, coagulation time, Hb%, glucose level. . . etc. 2. Liver Functions Tests (LFT): Alkaline phosphatase, bilirubin, liver enzymes (AST, ALT). 3. Renal Function Tests: Serum urea & creatinine. 4. Cytological Examination of Nipple Discharge: As a rule, mammography or biopsy is required when nipple discharge (or cyst fluid) is bloody. 5. Biochemical Tumor Markers: 6. Urinary hydroxyproline (HYPRO): Massive spread, especially to the bone causes breakdown of collagen, which results in t excretion in urine as hydroxyproline (Normal level = 35 mg/dl). 7. Alkaline phosphatase (t in bone & liver metastases). 8. Hypercalcemia (Occurs in advanced breast cancer - Plasma Calcitonin (useful in staging). 9. Blood count (anemia or pancytopenia occurs with bone marrow involvement). 10. Others: ESR (may t in disseminated cancer), Serum ferretin, Alpha-feto protein (AFP), Carcino-embryonic antigen (CEA), Human chorionic gonadotrophin (HCG), and i. C-cassein.

II. Radiological Investigations (Breast Imaging Techniques) 1. Soft Tissue Mammography: 1. It is the only reliable means of detecting breast cancer before a mass can be palpated in the breast. Although false positive & false negative results occasionally occur, mammograms are correctly interpreted in over 90% of cases. 2. Mammography is never a substitute for biopsy because it may not reveal clinical cancer in a dense breast as in young women with mammary dysplasia. Also, it often fails to reveal medullary carcinoma. Mammographic features suspicious of malignancy ARE: • Punctate calcifications (similar to salt) in 30% of cases (i. e. clustered, irregular microcalcifications). • The lump shows a dense shadow with very irregular outlines against the softer shadow of the breast. • 2 RY breast changes (asymmtery, architectural distortion) & nipple retraction.

Mammographic features OF Benign Tumor Course calcification (fibroadenoma) in 30% of cases. The lump appears as a homogenous dense smooth lesion. A surrounding halo of a thin radiolucent layer of fat. Ultrasonography (US): 1. It can differentiate between solid & cystic lesions. 2. It cannot diagnose early cancer because it can neither detect lesion <0. 05 cm nor rmcrocalcifications, Computerized Tomography: Can be used for diagnosis of breast cancer but uses large doses of radiation Magnetic Resonance Imaging (MRI): Cannot detect microcalcifications & is still under evaluation
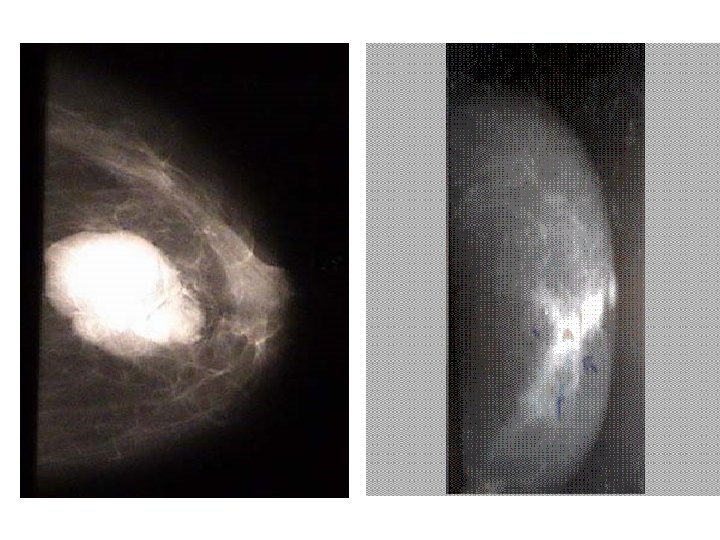

2. Xerography: 1. mammography made on a selenium plate producing positive It is a method of impression with accentuation of density differences. 2. Although xerography is very sensitive, yet ordinary film of mammography (film screen) is preferred because it is accomplished with a lower dose of irradiation. 3. Galactography: 1. The secreting duct is cannulated & sterile water-soluble contrast material is injected until the patient feels discomfort & then 2 projections of mammography are taken. 2. It is particularly valuable in cases of nipple discharge as it can show the nature, site and size of the underlying lesion especially when clinical examination & mammography are negative. 4. Thermography (Heat Map of the Breast): 1. General Rule: It is not essential for diagnosis (C/E & mammography are enough in 98% of cases). 2. Indications: {never for detection}, 3. Coupled with mammography in high-risk patients, it yields better surveillance of the other breast, 4. Follow-up of irradiated breast (persistent hyperthermic zone after irradiation is a bad sign) 5. Prognostic: The pattern of thermal changes varies according to the severity of the disease. 6. • Appearance Malignant Breast Lesions: Hyper-vascularization, hot spot > 3°C, diffuse t in temperature (> 2°C), edge sign (loss of convex margin of breast), and L. N secondaries (hotter if cancer is on the same side) especially supra & infraclavicular L. Ns.

III. Imaging Techniques for Metastases 1. Plain X-ray (PXR) of the chest & suspected bones. 2. Computerized Tomography (CT) of the liver & brain (when metastases are suspected). 1. Bone Scanning using ""Tc-labeled phophates is more sensitive than PXR in detecting bone metastases. Lymphsintigraphy: For detection of axillary L. Ns before being detected clini

IV. Breast Biopsy 1. Open Biopsy: • It provides enough tissue material of the tumor for: Histologic Diagnosis (type & grade of the tumor). 1. Hormone Receptor Estimation (estorgen & progesterone receptors): Receptor-positive tumors respond more to hormonal therapy & have a better prognosis than receptornegative tumors. 2. Flow Cytometry to determine if the tumor is diploid or aneuploid, and to determine the S-Phase Fraction. Aneuploid tumors with a large S-Phase Fraction have poor prognosis. • Methods: /. Paraffin-Section Biopsy: • Excisional Biopsy: It is the best method & could be done in the operating room under general anesthesia, or in the outpatient clinic under local anesthesia. • Incisional Biopsy : It is more appropriate in patients with large or deeply seated carcinomas.

2. Frozen-Section Biopsy: 1. A glance at the cut section intra-operatively often indicates the nature of the tumor, which should be confirmed by immediate histological examination by the frozen-section technique. If the tumor proves malignant, all instruments & towels are changed & the radical procedure is carried out. Limitations of frozen-section: (1) It needs an expert pathologist, (2) Few sections are usually done because of short time, (3) Freezing causes nuclear changes & may interfere with diagnosis.

3. Needle Biopsy: 1. If results are negative, it should be followed by an open biopsy because false negative results are obtained in about 15 -20% of cases. 1. Methods. a) Fine Needle Aspiration Cytology (FNAC): Advantages: (1) No need for local anesthesia, and (2) it does not cause dissemination. b) Core Biopsy: Under local anesthesia, through a small 2 mm incision a special needle is inserted ( Tru-cut needle).

DIAGNOSIS OF BREAST CANCER: A. Diagnosis of the Lump: 1. Clinical Assessment: 1. History Taking: Special notes should be made for breast cancer risk factors, relation of the mass to the menstrual cycle, previous breast problems, and any systemic complaint. 2. Examination: It should be performed with the patient sitting (arms at sides & then upwards overhead) and then when lying down. The upper outer quadrant is most commonly affected because it contains the largest volume of breast tissue. The smaller the size of the lump, the lesser the chance of lymph node metastases. 3. Biopsy: for confirmation of diagnosis of cancer & histological grading. 4. Breast Imaging Techniques (Mammography is the best). 5. Cytological Examination of nipple discharge. B. Diagnosis of Spread by Lymph Nodes: • Clinical Picture: Palpable lymph nodes (axillary, supraclavicular & internal mammary). • Chest X-ray (CXR): may show enlarged mediastinal lymph nodes. 1. Biopsy: Histological examination of L. Ns removed at surgery may show a 25% clinical error 2. Radioactive Isotope Scanning using "c Tm (Lymphsintigraphy). 3. C. Diagnosis of Systemic Spread:
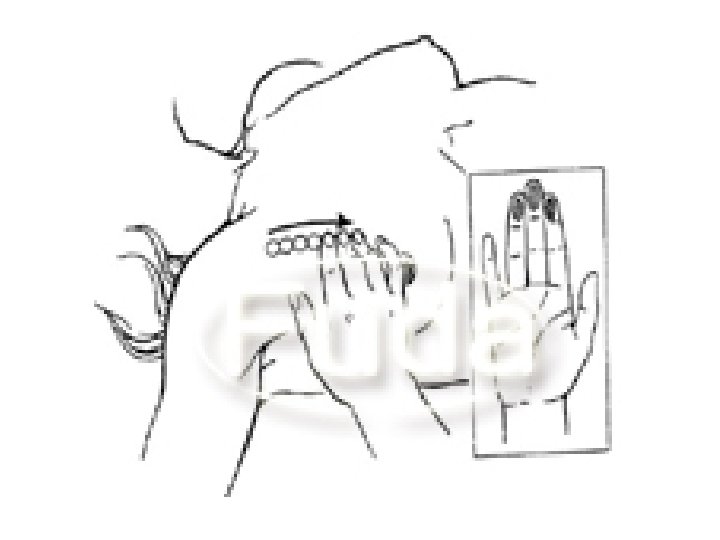
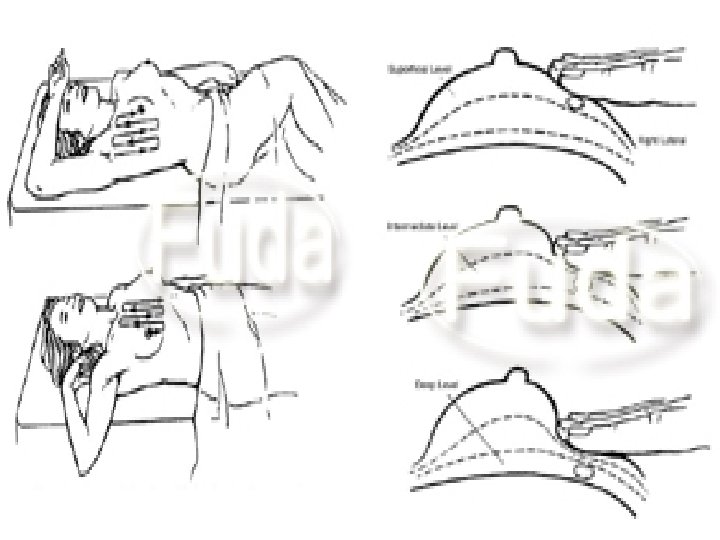

C. Diagnosis of Systemic Spread: 1. Clinical Criteria: a) Tumor size, skin affection & chest wall fixation. b) Axillary & supraclavicular lymph node enlargement. c) Distant metastases. 2. Investigations: Radiological: PXR (chest & bones), Isotope scanning (liver, bone and brain), US, CT, MRI. Biochemical : Anemia/pancytopenia (bone marrow), Urinary HYPRO (bone), AP (liver & bone), Hypercalcemia (bone), Serum ferretin, AFP, CEA, HCG.
STAGING OF BREAST CANCER: 1. Clinical Staging A. International Classification (Manchester); Stage Criteria Stage I • Mobile tumor confined to the breast, or Paget's disease with no mass. • Free axilla (no enlarged L. Ns) Stage II • Mobile tumor confined to the breast • Mobile axillary L, Ns on the same side(discrete=IIa, matted=IIb Stage III • Tumor fixed within the breast, to the underlying tissues or skin axillary Fixed L. Ns Stage IV * Wide dissemination to the opposite breast, chest, bone, liver. Supraclavicu. lar L. Ns

B. TNM Staging T (Tumor) N (Lymph Nodes) To = No demonstrable tumor. No = Not palpable (axillary L. Ns). T 1 = Tumor < 2 cm: Nl = Palpable (axillary T 1 a: No deep fixation. L. Ns). T 1 b: With deep fixation. Nla: clinically not malignant. NIb: clinically malignant. T 2 = Tumor 2 -5 cm: T 2 a: No deep fixation. T 2 b: With deep fixation. T 3 = Tumor 5 -10 cm: T 3 a: No deep fixation. T 3 b: With deep fixation. T 4 = Tumor of any size: T 4 a: Direct chest extension. T 4 b: Skin involvement. T 4 c: T 4 a + T 4 b. N 2 = Palpable axillary L. Ns (clinically malignant & fixed). N 3= Palpable homolateral supra- or infraclavicular L. Ns (malignant & fixed). M (Metastases) Mo = No known distant metastases. Ml = Positiye distant metastases.
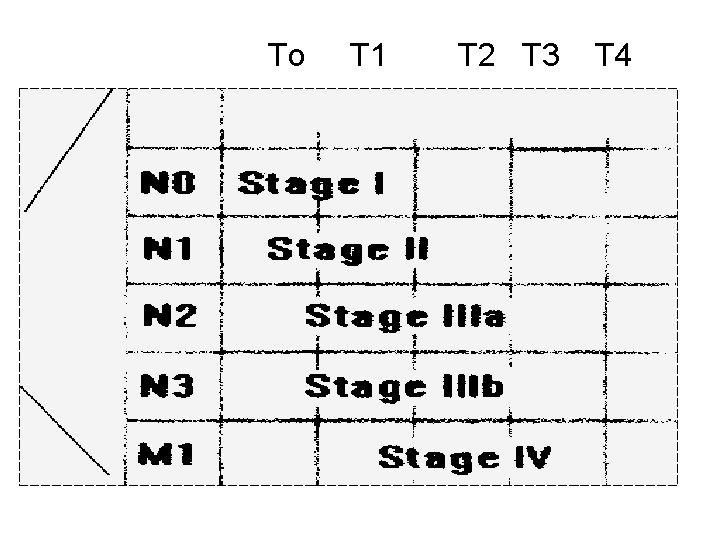
To T 1 T 2 T 3 T 4

C. Columbia Staging: Stage Criteria Stage A 1. No skin edema, ulceration or solid fixation of the tumor to the chest wall. 2. Axillary L. Ns not clinically involved. Stage B 1. No skin edema, ulceration or solid fixation of the tumor to the chest wall. 2. Axillary L. Ns are clinically involved, but <2. 5 cm in diameter & not Fixed. Stage C Presence of any of the 5 grave signs of locally advanced breast cancer: 1. Skin edema (<l/3 of the breast skin). 2. Skin ulceration. 3. Solid fixation of the tumor to the chest wall. 4. Massive involvement of axillary L. Ns: One L. N. or a group of L. Ns (2. 5 cm in diameter or more), or a chain of L. Ns extending high up in the axilla. 5. Fixation of axillary L. Ns (to overlying skin or deeper structure)

Stage D Criteria A combination of 2 or more of the signs of stage C. Extensive edema of the skin (>l/3). Satellite skin nodules. Inflammatory type of carcinoma. Supraclavicular L. Ns (clinically) or internal mammary L. Ns. Arm edema. Distant metastases. D. American Joint Committee (AJC) Staging: Similar to the TNM (UICC) but with some modifications as follows: Stage 1: Tl No Mo, Stage 2: T 2 No Mo, Stage 3: T 3 No/Nl. Mo, Stage 4: T 4 N 2/N 3 Ml

1. . Histological Staging (Grading) A. Broder's Classification: This is in fact "grading" of the tumor according to the % of differentiated cells: 75 -100 % = grade I, 50 -75% = Grade II, 25 -50% Grade III, 0 -25% (Grade IV). B. SBR Grading System (Scraff, Bloom and Richardson): The rumor is graded according to ductal forrnation, nuclear pleomorphism and number of mitosis each item is graded from 1 to 3, thus making a minimum total scor of 3 and a maximum of 9 as follow : grade I =score 3 -5. , Grade II = score 6 -7, Grade III = score 8 -9 1. 2. 3. 4. Degree of differentiation ductal formation: Generalized = 3 Moderate = 2. Absent = 1 I nuclear irregularity (pleomorphism) : Weak = 1. Moderate = 2. Dense = 3 number of mitosis (Maximum number : one field X 400 ) : <1 = 1 2 = 2 >3 = 3

DIFFERENTIAL DIAGNOSIS OF BREAST CANCER LUMP IN THE BREAST Hard Lump: 1. Traumatic: Traumatic fat necrosis (TFN), chronic calcified hematoma. 2. Inflammatory: Chronic abscess (non-specific), T. B. and $ (specific). 3. Interstitial Fibroadenosis. 4. Neoplastic: Hard fibroadenoma (benign), IDC (malignant). • Large (Huge) Lump : Giant soft fiobroadenoma, Encephaloid carcinoma. Sarcoma. • Large Breast: Pregnancy (physiological), acute mastitis, milk engorgement, inflammatory carcinoma. • Acute Lump: Acute mastitis, Acute breast abscess, Acute inflammatory carcinoma. Chronic Lump: • Traumatic: TFN, chronic hematoma. • Inflammatory: Chronic breast abscess (non-specific), TB & $ (specific). • Mammary Dysplasia (MDE). • Neoplastic: fibroadenoma, duct papilloma (benign), carcinoma, sarcoma (malignant). Painless Lump: Breast cysts, benign rumors (duct papilloma, fibroadenoma), malignant tumors (e. g. IDC). Bilateral Breast Lesions: • Fibroadenosis. • Tuberculosis • Lobular carcinoma. Secondary tumor from a primary in the other breast, or a second primary cancer

• Lumpy Axilla: • a) Physiological: obesity (always bilateral). b) Accessory Breast: presence of a nipple. c) Lipoma: No nipple. d) Enlarged Axillary lymph nodes. e) A Tumor in the axillary tail of Spence. PEAU D'ORANGE 1. Breast cancer. 2. Fibroadenosis. a) Chronic breast abscess. b)NIPPLE & AREOLA CHANGES c)Nipple Depression (Retraction): IDC, congenital (withdrawn nipple), chronic breast abscess. Nipple Deviation: To same side (IDC, chronic breast abscess), d) to opposite side (sarcoma). Nipple Destruction: Paget 's disease, eczema, Bowen's disease, malignant melanoma. e).

PROGNOSIS OF BREAST CANCER: A. Clinical Factors: 1. Stage: 2. Age (worse prognosis if <35 Y or >70 Y). 3. Sex : Prognosis is worse in males due to: In early stages, it is a 4 -quadrant carcinoma (stage III) due to small size of the male breast Blood spread is rapid (due to small breast also). Absent buffer pad of fat in males. Spread along lymphatics in the 4 directions. Radical surgery is hardly feasible due to soft tissue deficiency. 4. Site: Lower inner quadrant (LIQ) has the worst prognosis due to early spread to chest & abdomen, Upper inner quadrant (UIQ) comes next. The UOQ has the best prognosis (spread to axilla). 5. Pregnancy: Pregnancy exerts a bad influence on prognosis due to: Increased vascularity (hyperemia & increased lymphatics) Endocrinal influences (t hormones). Enlargement of the breast may mask the tumor & delay diagnosis. Reduction in the immunity of the body. About 70% of the tumors in pregnancy are estrogen receptor negative. Delay in diagnosis & treatment.

B. Pathological Factors: Tumor Type: Unfavorable Prognosis: Scirrhous, encephaloid & inflammatory carcinoma. Favorable Prognosis: Colloid & duct carcinoma (NOS). Tumor Grade (SBR): 5 -Y SR is 90% in Grade I, 70% in Grade II & 60% in grade III. Axillary Lymph Node Involvement: It reduces the 5 Y-SR by 50% (from 80% to 40%). Stromal Changes. Favorable Prognosis: Mucinous formation, lymphocytic infiltration, elastosis). Unfavorable Prognosis: Hemorrhage, necrosis, lymphatic & vascular invasion. • Biological Factors: 1. Receptors (ER & Prog) : Positivity : Receptor-positive tumors have better prognosis. Quantity of receptors: Highly positive tumors have better prognosis 2. Tumor Markers 3. DMA ploidy: Aneuploid tumors have a poor prognosis. 4. S-Fraction: Tumors with a large S-phase fraction have a poor prognosis.

Tumor Markers Urokinase Plasminogen Activator (u. PA) Plasminogen Activator Inhibitor (PAI-1) . These are measured with one test, called the u. PA + PAI-1 Tumor Marker Test These OTHER tumor marker tests are useful for only a small fraction of patients Cancer Antigen 15 -3 (CA 15 -3) Cancer Antigen 27. 29 (CA 27. 29) Ki-67 Labeling Index Carcinoembryonic Antigen (CEA) Other Diagnostic and Prognostic Tests: THESE ARE NOT TUMOR MARKER TESTS BUT ARE IMPORTANT IN MAKING DECISION ABOUT TREATMENT Estrogen (ER) and Progesterone Receptors (PR) Human Epidural Growth Factor 2 (HER 2/neu) tumors with over exprision of this poly peptide protein have poor prognosis
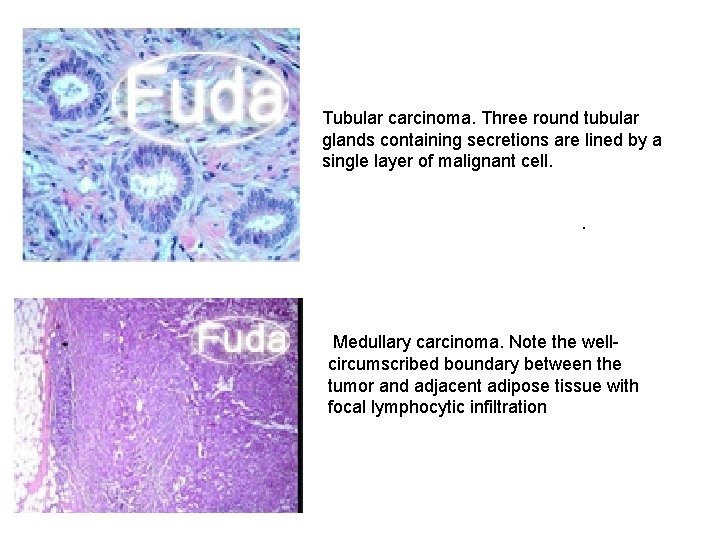
Tubular carcinoma. Three round tubular glands containing secretions are lined by a single layer of malignant cell. . Medullary carcinoma. Note the wellcircumscribed boundary between the tumor and adjacent adipose tissue with focal lymphocytic infiltration
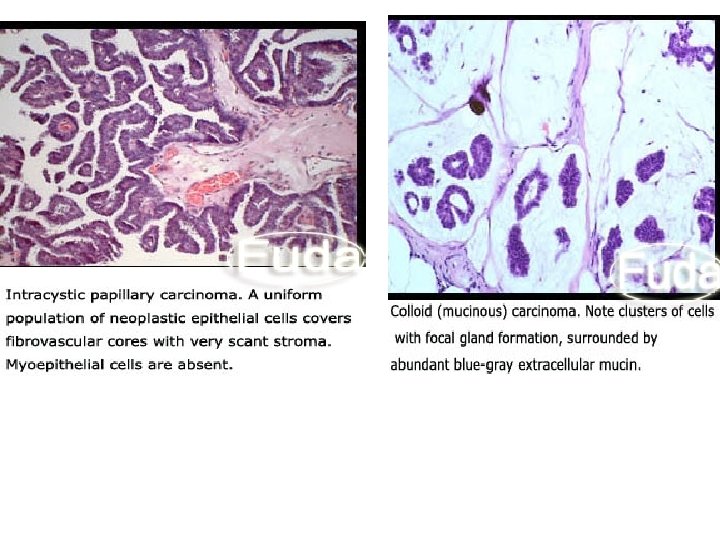
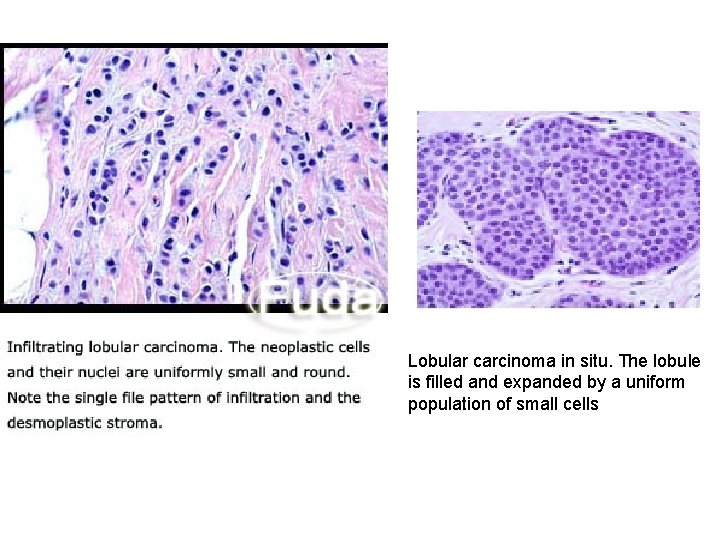
Lobular carcinoma in situ. The lobule is filled and expanded by a uniform population of small cells
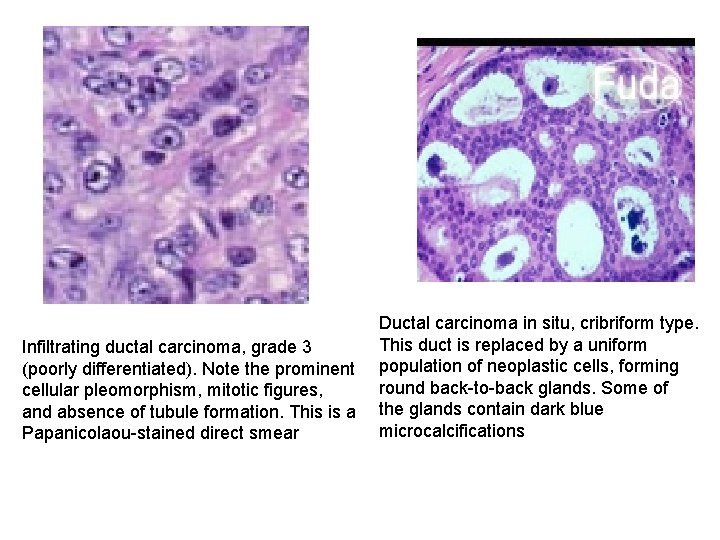
Infiltrating ductal carcinoma, grade 3 (poorly differentiated). Note the prominent cellular pleomorphism, mitotic figures, and absence of tubule formation. This is a Papanicolaou-stained direct smear Ductal carcinoma in situ, cribriform type. This duct is replaced by a uniform population of neoplastic cells, forming round back-to-back glands. Some of the glands contain dark blue microcalcifications

I- TREATMENT OF OPERABLE (EARLY) BREAST CANCER A. Treatment of Breast Carcinoma In-Situ Treatment of Iobular Carcinoma in-Situ (LCIS): All patients with LCIS are exclusively women; 90% are premenopausal (mean age = 45 years). The incidence of development of "invasive" cancer is 10 -35%. Characteristically, there are no micorcalcifications. Options of treatment include the following: 1. The old R, which consisted of "radical mastectomy is now obsolete; and the suggestion of just "observation" (i. e. follow-up by mammography) is very risky due to the possibility of tumor multicentricity & bilaterality in addition to being associated with an invasive carcinoma. 2. The routine R/ consists of "simple mastectomy" (routine axillary L. N. dissection is not justifiable because positive axillary nodes have been found in < 1% of cases only). 3. A contra-lateral biopsy of the other "normal" breast may be added to simple mastectomy. 4. If the condition is bilateral, then "bilateral simple mastectomy" should be performed.

Treatment of Ductal Carcinoma In-Situ (DCIS): About 75% of patients with DCIS are women with a mean age of 55 years (5% are men !!). The incidence of future development of an "invasive carcinoma" is 75%. Characteristically, miscrocalcifications are positive. Treatment options include the following: 1. Simple Mastectomy has been the routine R/ option for several decades (axillary L. N. dissection is not necessary in most cases). Factors favoring mastectomy are a palpable mass (> 2 cm), comedo type, multicentricity, high nuclear grade, negative receptors, aneuploid DNA, and young age. 2. Wedge resection yielded a survival rate similar to that of mastectomy. 3. Wide local excision + radiotherapy reduced the incidence of recurrence.

B. Treatment of Stages "I & II" Breast Cancer (up to T 2 N 1 ) Surgery (Which Operation)? : Radical Mastectomy: En block removal of the (1) whole breast (including nipple, areola & tumor with a wide margin of surrounding skin & tissues), (2) pectoralis major & minor muscles, and (3) axillary L. Ns. Modified Radical Mastectomy : Total (simple) mastectomy with axillary L. N. dissection i. e. en- block removal of the whole breast with the underlying pectoralis fascia (but not the pectoralis major muscle) & all axillary L. Ns. Some surgeons remove also the pectoralis minor muscle. Simple Mastectomy (Total Mastectomy): Removing the whole breast only (no L. N. dissection). Breast Conservative Techniques: Partial mastectomy (Segmental mastectomy, quadrantectomy, or lumpectomy) + complete clearance of the axilla, at the same sitting, through a separate incision.
Choice of the Surgical Procedure - Current Recommendations: The best initial R/ for most patients with a potentially curable carcinoma of the breast is: Modified Radical Mastectomy. OR Breast Conservation Technique (e. g. lumpectomy + axillary dissection + radiotherapy). Indications & contraindications are shown in the Table below: Selection Criteria for Breast Conservation 1. Tumor size: Small (<2 -4 cm). 2. Patient: should be motivated. . 3. Resection would not compromise cosmoses: a) Acceptable tumor to breast ratio b) Single lesion completely excisable c) Focal (non-diffuse) microcalcification Contraindications 1. Multiple primaries 2. large tumor in a small breast 3. gross residual tumor 4. diffuse microcalcification. 5. pregnancy 6. collagen vascular disease.

The Place for Adjuvant Therapy: Why Use Adjuvant Therapy? Adjuvant R/ after surgery for operable breast cancer has been recommended because of the following: 1. Systemic nature of the disease (micrometastases are present in >50% of cases at the time of diagnosis). 2. High recurrence rate (RR) after apparent adequate surgical treatment. Clinically undetectable disease after adequate surgery responds better to adjuvant therapy

Adjuvant Therapy - Which Regimen? A. Postoperative Radiotherapy (RT): Aim: Destruction of locally microscopic residual malignant cells. Indications: After modified radical mastectomy in large tumors (>5 cm i. e. T 3), or if the tumor is located in the central or medial portion of the breast. After breast conserving procedures. B. Postoperative Chemotherapy: Aim: Killing hidden malignant cells present anywhere inside the body (occult metastases responsible for late recurrences while they are microscopic & most vulnerable to anti-cancer agents. Indications: in pre-menopausal women, with involved lymph nodes (node positive), and tumors of any receptor status (+ve or -ve). Drugs Used: The most commonly used "combination chemotherapy" is the CMF regimen (Cyclophosphamide + methotrexate + 5 -FU). Effects: It prolongs survival & reduces RR; but has more toxic effects than hormonal therapy

C. Postoperative Hormonal Therapy: Postoperative Prophylactic Oophorectomy: Rationale: removing the source of estrogen in patients with intact ovaries. Not used anymore because of its questionable value, operative risk & introduction of anti-estrogens Post-operative Nolvadex = Tamoxifen (Anti-Estrogen): Indications (Candidacy): The NIH recommends its use in postmenopausal women, with node-positive, and receptor +ve tumors only. However, the NATO (Nolvadex Adjuvant Trial Organization) recommends its use in tumors of any receptor status in pre-menopausal women with involved axillary L. Ns & in post-menopausal women whether L. Ns are involved or not !! Dose: 10 mg twice/d for 1 -2 years (Long course of tamoxifen is better than short course. Some authors recommend it for 5 years because of its safety).

Management of Breast Cancer During Pregnancy: A biopsy + ER assay are done modified radical mastectomy, and if ER status is positive pregnancy should be terminated. If ER status is negative, pregnancy is terminated if the patient is in the first or second trimesters only, and continued if in the third trimester.

II- TREATMENT OF INOPERABLE (ADVANCED) BREAST CANCER Definition of Advanced Breast Cancer: 1. Stages III or locally advanced breast cancer (LABC) & IV (metastatic disease) i. e. >T 2 N| or M, 2. Recurrent local disease 1. Surgery - Simple Mastectomy (or excision of local recurrence): Effects (rationale) 1. To remove the turner reservoir (which should be biopsied). 2. To prevent complications e. g. ulceration, hemorrhage, infection and pain. 3. To facilitate the response to adjuvant therapy. 2. Radiotherapy: Indications: 1. To control LABC particularly radiosensitive tumors (encephaloid carcinoma, mastitis carcinomatosa). 2. To treat post-operative recurrences (lymph node recurrence or chest wall recurrence). 3. To control secondary deposits, particularly bone (pain) & brain deposits. 4. To control signs of mediastmal & spinal cord compression. 5. Following internal fixation of pathological fracture 2^ to bone metastases. 3. chemotherapy
Indications: 1. ER-negative tumors. 2. Rapidly growing ER-positive tumors & ER-positive tumors that failed to respond to hormonal R/. Types (Groups): Group Examples 1. Alkylating agents Nitrogen mustard, nitromin, endoxan, phenylalanine mustard. 2. Anti-metabolites Methotrexate, 5 -fluorouracil (5 -FU), 6 -mercaptopurine (6 -MP). 3. Vinca alkaloids Vincnstine sulfate (oncovin). 4. Antibiotics Adnamycin (Doxorubicin), actinomycin D, mitomycin Bone marrow depression, GIT disturbance, alopecia, cystitis (endoxan), cardiac toxicity (adriamycin), and neurological toxicity (vincristine). Intracavitary Chemotherapy: 1. Aspiration of pleura 1 effusions for symptomatic relief + installation of Thio-TEPA to prevent recurrence 2. Abdominal paracentesis + installation of chemotherapeutic agents (e. g the most recent, inactivated corynebacterium parvum organisms "coparvax" ) can similarly be used in malignant ascites. Neoadjuvant Chemotherapy: • Pre-operative chemotherapy (3 -4 cycles) for down-staging of the tumor has been recently introduced.

4. Hormonal Therapy: Indications - Patients likely to respond to hormone manipulation include those with: 1. Long disease-free interval. 2. Over 5 years after menopause at the time of presentation of the primary tumor. 3. Good response to previous hormonal therapy. 4. Advanced local disease without metastases. 5. Primarily osseous metastases rather than soft tissue metastases. 6. Estrogen receptor-positive tumors. Types: • Additive (androgens, estrogen, progesterone, cortisone). • Ablative (e. g. oophorectomy). 1. Competitive (Tamoxifen). 2. Inhibitive (Aminoglutathemide - it causes medical adrenalectomy).

Drugs: 1. Nolvadex (Tuinoxiji'n): It is the most commonly used drug. It antagonizes estrogen at the receptor level, and is given at a dose of 10 mg twice daily for 1 -2 years. Aminoglutethernide (Cytadren): It blocks the action of adrenal glands leading to remissions however, its side effects include skin rash, dizziness, somnolence & visual blurring. Androgen Therapy (Testosterone): In cases of failed remission or tumor reactivation following oophorectomy or estrogen therapy. It antagonizes estrogen & inhibits the pituitary gland; however, it causes virilism & hepatic dysfunction. Estrogen Therapy: In post-menopausal patients without evidence of estrogen secretion. Side effects include GIT disturbances, vaginal bleeding, and engorgement of the breast with pigmentation of the areola, lower limb edema & fluid retention with congestive heart failure. Progesterone Therapy (e. g. Megace. J: it is effective in 20 -30% of cases if used in massive doses Corticosteroid Therapy: Action: It potentiates the action of cytotoxic drugs, and stimulates hemopoiesis. Particular Indications: R/ of acute symptoms of hypercalcemia, brain, lung and hepatic secondaries. It is also of value in patients who do not respond to other hormonal therapy. 1. Side Effects : GIT bleeding, hyperacidity & PU, hypertension, acne, muscle wasting, T

Hormonal Ablation: 1. Minor Ablation - Oophorectomy (Ovarectomv): Indication: Used in the past in pre- & post-menopausal women up to 5 years after menopause, in order to remove the source of estrogen. It gives a remission for 612 months & is effective in about 50% of premenopausal women having metastases Methods: surgical, radiological (less effective), or more recently, chemical by LH/RH agonists e. g. Zoladex (one injection/month; effective but reversible). 2. Major Ablation: 1. Bilateral Adrenalectomy is now obsolete. Side effects include fluid & electrolyte problems & permanent deficient response to stress. 2. Hypophvsectomy (transcranial. transsphenoidal, or using isotope implantation js also obsolete. Side effects = meningitis, CSF rhinorrhea, visual field defects, & occulomotor paralysis.

5. Immunotherapy: It is not proved effective yet. Methods tried include the following: 1. Active Immunization: Specific (Immunization with attenuated living cells or cell-free tumor extract) - Non-specific (using BCG). 2. Passive Immunization: By cross immunization of another individual with tumor fragments & then blood is withdrawn from the immunized individual & the serum containing antibodies is then given to the patient. 3. Pharmacologic Immunothenipv: Levamizole administration: used in order to activate lymphocytes. 4. GP 2 poly peptide vaccein for patients having over exprision of HER 2/NEU

6. Management of Oncologic Emergencies due to Distant Metastases: A. Malignant Hypercalcemia: Etiology: It may occur due to bone secondaries or humoral substance secreted by the tumor and may be aggravated by anti-estrogen therapy (which should be discontinued). Diagnosis: It presents with marked t in bone ache, anorexia, nausea & vomiting, progressive weakness & lethargy, oliguric renal failure, deterioration of general condition & coma. Treatment: 1. Saline infusion (hydration & duiresis). 2. Corticosteroids (prednisone): 60 -80 mg/d —> response i. e. reduction in calcium level in 5 -10 days. 3. Calcitonin (calcium lowering agent): —> response in 2 -4 hours (safe but may cause allergy). 4. Diphosphonate. 5. Mithramycin (25 ug/Kg) —> response in 6 hours. It is a cytotoxic antibiotic, which preventsosteoclastic function by inhibiting RNA synthesis. B Unstable Bone Metastases: Internal fixation (for pathological fractures), total hip replacement. C. Spinal Cord compression: Laminectomy. D Brain Metastases: Whole head irradiation. E. Lung Metastases: Steroid therapy, brochodilators. F. Pleural Effusion: aspiration (may be repeated) + chest tube drainage with instillation of cytotoxins.

Early-stage breast cancer Surgery: Breast preservation with lumpectomy with radiation is the preferred treatment. Radiation: As a part of the breast-coserving treatment (lumpectomy), breast radiation is performed with 4 500 to 5 000 c. Gy boost to tumor-excision site. Systemic chemotherapy: Combination chemotherapy can reduce the annual risk of • death by 20%, and in 10 years produces an absolute improvement in survival of 7% to 11% in women younger than 50 years. Hormone therapy: Tamoxifen is a selective estrogen-receptor modulator (SERM), can decrease the risk of recurrence by 42% and the absolute risk of death by 22% in patients with ERpositive tumors. Combination of tamoxifen with chemotherapy can cause a 25%-30% reduction in recurrence, compared with chemotherapy alone.

Locally advanced breast cancer Initial surgery is only used to biopsy to confirm the diagnosis and to identify the receptor status. Resection operation is done after the best response to preoperative chemotherapy Neoadjuvant (primary) chemotherapy produces the tumor shrinks by 50% and allows surgical resection with clear margins in more than 65% of the women treated. Radiation to chest wall and supraclavicular area is done after surgery

Metastatic breast cancer. Surgery and /or radiation may be used for local control Hormone agents may be used as the first-line therapy in patient with positive hormone receptor. : Hormone agents used are. SERM with combined estrogen agonist and estrogen antagonist activity Tamoxifen (Nolvadex), 20 mg/day, p. o. Toremifene (Fareston), 60 mg/day p. o . Progestins Megestrol acetate (Megace), 40 mg/dose p. o. 4 times daily

Aromatase inhibitors Anastrozole(Arimidex), 1 mg/day p. o. Letrozole(femara), 2. 5 mg/day p. o. Aminoglutethimide, 250 mg/dose p. o. 4 times daily; hydrocortisone replacement to offset cortisol suppression associated with aminoglutethimide. LHRH agonist analogue in premenopausal women Goserelin (Zoladex), 3. 6 mg/dose, s. c. implant into the abdomen wall every 28 days Goserelin (Zoladex), 10. 8 mg/dose, s. c. implant into the abdomen wall every 12 weeks. Used in patients who have tumors that express either ER or PR receptors or both receptors

. Chemotherapy may be used as the initial treatment in hormone receptor-negative patients Commonly used chemotherapy regimens are ; (AC: Dororubicin, 60 mg/m 2 i. v. on day 1 (total dose/cycle, 60 mg/m Cyclophosphamide, 600 mg/m 2 i. v. , on day 1 Treatment cycles are repeated every 21 -28 days depending on hematology recovery. CMF: Cyclophosphamide, 100 mg/m 2 per day p. o. for 14 days, day 1 -14 Methotrexate (MTX), 40 mg/m 2 per dose i. v. for two doses, day 1 and 8 5 -FU, 600 mg/m 2 per dose i. v. for 2 doses, day 1 and 8 Treatment cycles are repeated every 28 days. AC-P: Dororubicin, 60 mg/m 2 i. v. on day 1 Cyclophosphamide, 600 mg/m 2 i. v. , on day 1′ 4 cycles Paclitaxel 175 mg/m 2 per dose i. v. over 3 hours every 3 weeks′ 4 cycles Treatment cycles are repeated every 21 days.

Recurrent breast cancer For local recurrence surgical excision and radiation are choice. Chemotherapy and hormone therapy are as for metastatic breast cancer. Trastuzumab (Herceptin. TM) Indication: metastatic breast cancer with tumor overexpresses HER 2/neu protein About 30% of the patients overexpress HER 2/neu. Regimen: Initial dosage is 4 mg/kg i. v. over 90 minutes, followed at weekly intervals by maintenance with 2 mg/kg i. v. over 30 minutes if the initial infusion rate was well . tolerated (High-dose chemotherapy (HDCT can overcome drug resistance and eradicate micrometastases. Breast cancer is a moderately chemosensitive tumor, and there is a dose-response correlation. Some trials showed promising results of this therapy.

Cryosurgery This therapy can be used for patients with local cancerous mass who can not tolerate operative intervention due to age and associated systemic diseases or dysfunction of important organs.

- Slides: 85