Male Reproductive System bladder seminal vesicle prostate gland
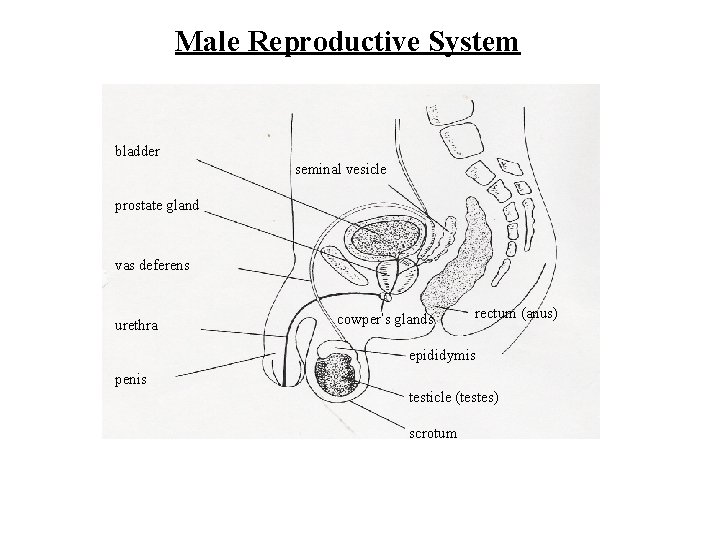
Male Reproductive System bladder seminal vesicle prostate gland vas deferens urethra cowper’s glands rectum (anus) epididymis penis testicle (testes) scrotum
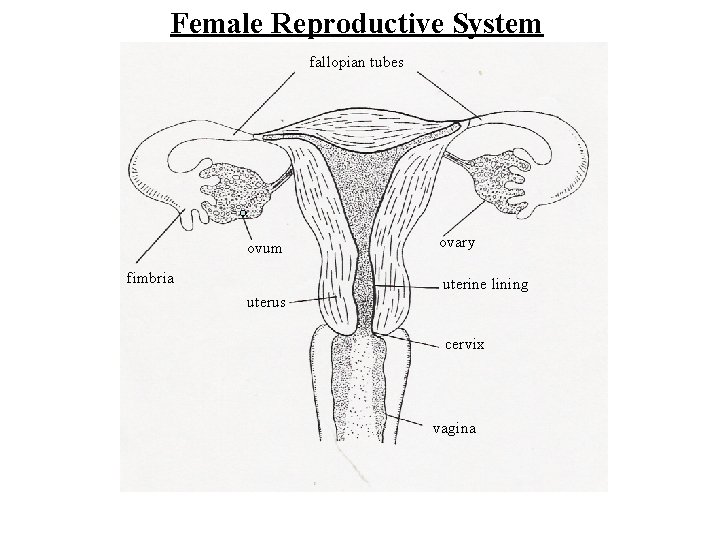
Female Reproductive System fallopian tubes ovum fimbria ovary uterine lining uterus cervix vagina

No Risk (no potential, no evidence) • • • abstinence masturbation hugging, kissing, casual contact sitting on toilet seats coughing & sneezing mosquitoes & other animals

Minimal Risk (some potential, no evidence) • giving/receiving oral sex with barrier • sharing toothbrushes or razors • using drugs with shared pipe or straw Note: • Transmission is unlikely, but possible. • Hepatitis C and HIV can live on these surfaces.

Low Risk (potential & some evidence) • anal or vaginal sex with a latex condom • oral sex on a woman • oral sex on a man, taking semen in one’s mouth or swallowing it Note: • Condoms are not 100% effective (break, misused). • Oral sex has fluids involved (semen, vaginal). • Risk increases with if have mouth/throat infections or cuts (possible entry into blood stream).

High Risk (potential & evidence) • anal or vaginal sex without a condom • sharing needles & drug injection equipment • sharing piercing/tattooing needles Note: • • Exchange of fluids (semen, vaginal, anal). Greater risk of infection. Use new condom on toys when sharing. Syringes or other equipment can have [infected] blood remain in barrel and tip. • HIV only lives for a short time outside body when exposed to oxygen (30 -60 seconds). • Hepatitis C can live up to 2 weeks on a surface. • Tattoo shops are regulated by Health Unit. See certificates!

ABSTINENCE Means not having vaginal, anal or oral sex. Also includes skin to skin sexual activity without penetration. • • • Avoid STI’s Early sexual activity is linked to cervical cancers No risk of pregnancy Sexual activity can change friendships and relationships Abstaining can have a positive impact on your future (education, career, ability to have children, quality of life and a healthy lifestyle, etc. ) • Positive self-esteem

Masturbation - Fact or Fiction Yes ____ It is common and a personal choice for males and females. Is masturbation normal? No ____ Is masturbation harmful? There is no evidence to say‘yes’. No ____ Can I get an STI from masturbation? ____ Can I get pregnant from masturbation? No Masturbation is the self-stimulation of the genitals to achieve sexual arousal and pleasure, usually to the point of orgasm (sexual climax).

Oral Sex - Fact or Fiction Yes Is oral sex actually sex? ____ Yes Is it okay to use a condom during oral sex? Yes Can I get an STI from having oral sex? ____ No Can I get pregnant from oral sex (swallow sperm)? ____ No Is oral sex only something a guy has done to him? ____ Oral sex is the stimulation of the external genitals (sex organs) by the mouth (sucking or licking). Cunnilingus (eating out, licking out) is the oral stimulation of the clitoris or vagina. Fellatio (giving head, blowjob) is the oral stimulation of the penis.

Oral Sex - The Facts How risky is oral sex? • Oral sex is a low risk sexual activity. • Sexually transmitted infections (STIs) such as gonorrhea, chlamydia, herpes, syphilis and HIV can all be transmitted through oral sex. • STIs are transmitted when fluids are exchanged: – Having small cuts in your mouth, even when you do not know it (e. g. , dental work, brushing or flossing, eating sharp foods). – Skin torn on genitals, even if it you do not know it (e. g. , before or during oral sex). – If your partner is menstruating (having her period). – Holding infected fluids such as semen, vaginal fluids or menstrual blood in your mouth for a long time or swallowing it. • You cannot get pregnant from having oral sex.

How can Oral Sex be done in a safer manner? • · · · Use a condom for oral sex on men Use a dental dam for oral sex on women Do not use saran wrap Try to avoid getting fluids such as semen, vaginal fluids or menstrual blood in your mouth Do not have oral sex right after brushing or flossing your teeth (wait about 30 minutes) Use anti-bacterial mouthwash after oral sex
Bacterial Chlamydia An often-asymptomatic infection That can lead to reproductive complications What is it? • Most common bacterial sexually transmitted infection. • Greatest number of infections found in people 15 to 24 years old. • Can affect the cervix and urethra, and occasionally the rectum, throat, and eyes. How is chlamydia transmitted? • Unprotected oral, vaginal or anal sex with an infected partner. • Penetration and ejaculation are not required for transmission. • It can be passed from an infected mother to her infant during birth, causing lung and/or eye infections. www. sexualityandu. ca
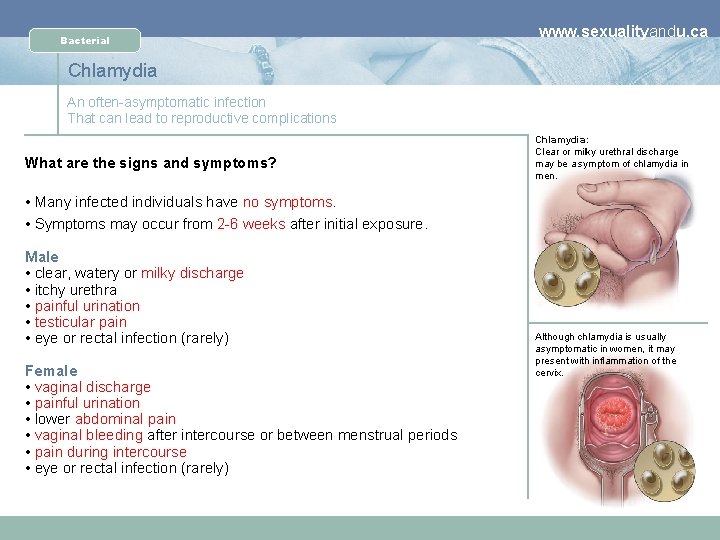
Bacterial www. sexualityandu. ca Chlamydia An often-asymptomatic infection That can lead to reproductive complications What are the signs and symptoms? Chlamydia: Clear or milky urethral discharge may be a symptom of chlamydia in men. • Many infected individuals have no symptoms. • Symptoms may occur from 2 -6 weeks after initial exposure. Male • clear, watery or milky discharge • itchy urethra • painful urination • testicular pain • eye or rectal infection (rarely) Female • vaginal discharge • painful urination • lower abdominal pain • vaginal bleeding after intercourse or between menstrual periods • pain during intercourse • eye or rectal infection (rarely) Although chlamydia is usually asymptomatic in women, it may present with inflammation of the cervix.

Bacterial www. sexualityandu. ca Chlamydia An often-asymptomatic infection That can lead to reproductive complications Considerations and possible complications: • Chlamydia is often associated with other undetected or untreated infections. • Increased risk of contracting and transmitting HIV. Male • Inflammation of the testicles, prostate and scrotum • Rashes, sores and joint pain • Infertility (in rare cases) Female • Infection spreading to the uterus and fallopian tubes (pelvic inflammatory disease) • Rashes, sores and joint pain • Infertility • Chronic pelvic pain
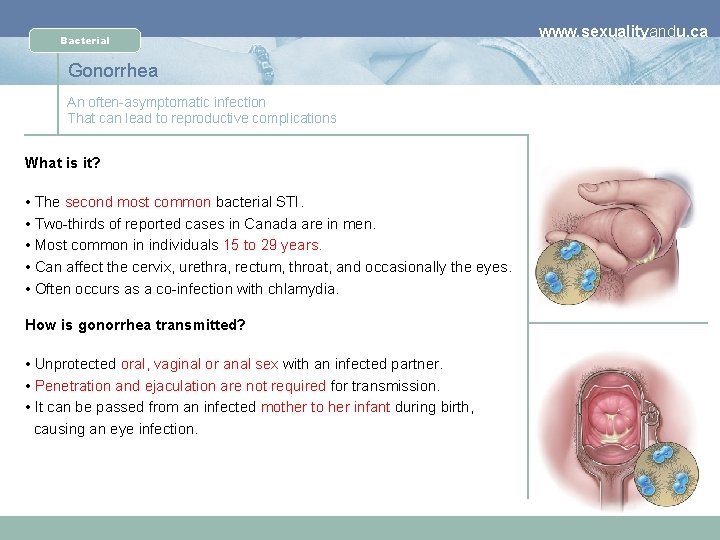
Bacterial Gonorrhea An often-asymptomatic infection That can lead to reproductive complications What is it? • The second most common bacterial STI. • Two-thirds of reported cases in Canada are in men. • Most common in individuals 15 to 29 years. • Can affect the cervix, urethra, rectum, throat, and occasionally the eyes. • Often occurs as a co-infection with chlamydia. How is gonorrhea transmitted? • Unprotected oral, vaginal or anal sex with an infected partner. • Penetration and ejaculation are not required for transmission. • It can be passed from an infected mother to her infant during birth, causing an eye infection. www. sexualityandu. ca
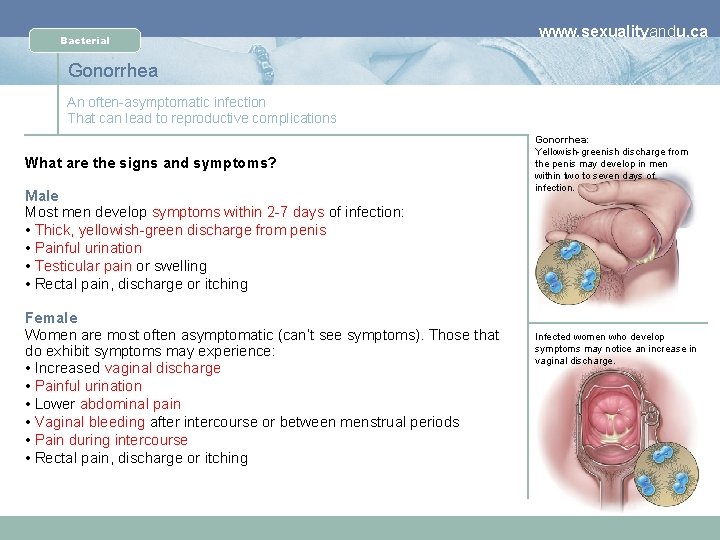
Bacterial www. sexualityandu. ca Gonorrhea An often-asymptomatic infection That can lead to reproductive complications What are the signs and symptoms? Male Most men develop symptoms within 2 -7 days of infection: • Thick, yellowish-green discharge from penis • Painful urination • Testicular pain or swelling • Rectal pain, discharge or itching Female Women are most often asymptomatic (can’t see symptoms). Those that do exhibit symptoms may experience: • Increased vaginal discharge • Painful urination • Lower abdominal pain • Vaginal bleeding after intercourse or between menstrual periods • Pain during intercourse • Rectal pain, discharge or itching Gonorrhea: Yellowish-greenish discharge from the penis may develop in men within two to seven days of infection. Infected women who develop symptoms may notice an increase in vaginal discharge.

Bacterial www. sexualityandu. ca Gonorrhea An often-asymptomatic infection That can lead to reproductive complications Considerations and possible complications • Gonorrhea is often associated with other undetected or untreated infections. • Increased risk of contracting and transmitting HIV. Male • Inflammation of the testicles • Rashes, sores and joint pain • Infertility (in rare cases) Female • Infection spreading to the uterus and fallopian tubes (pelvic inflammatory disease) • Chronic pelvic pain • Infertility • Risk of ectopic pregnancy (fetus grows outside uterus cavity - e. g. , fallopian tube)
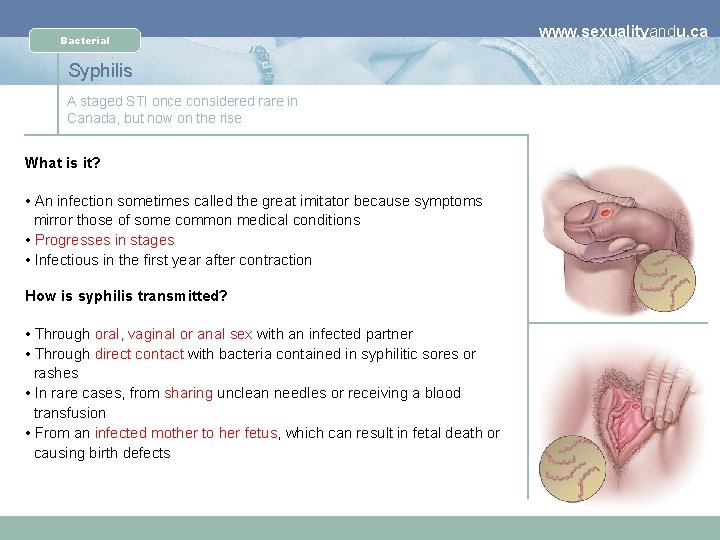
Bacterial Syphilis A staged STI once considered rare in Canada, but now on the rise What is it? • An infection sometimes called the great imitator because symptoms mirror those of some common medical conditions • Progresses in stages • Infectious in the first year after contraction How is syphilis transmitted? • Through oral, vaginal or anal sex with an infected partner • Through direct contact with bacteria contained in syphilitic sores or rashes • In rare cases, from sharing unclean needles or receiving a blood transfusion • From an infected mother to her fetus, which can result in fetal death or causing birth defects www. sexualityandu. ca
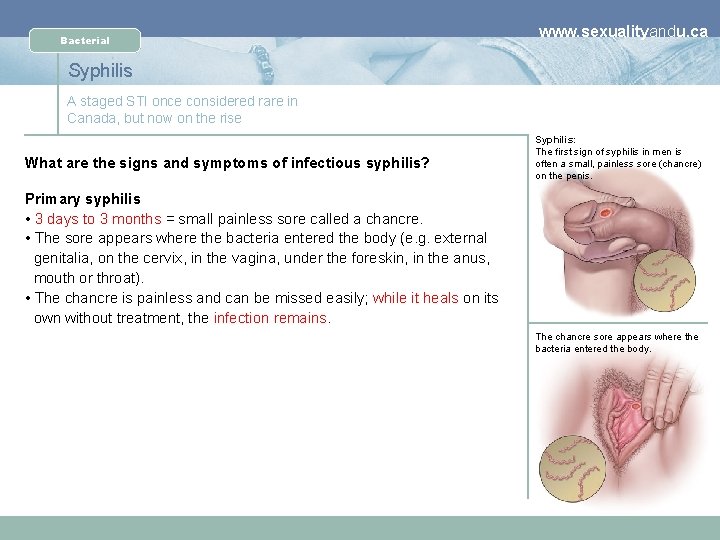
Bacterial www. sexualityandu. ca Syphilis A staged STI once considered rare in Canada, but now on the rise What are the signs and symptoms of infectious syphilis? Syphilis: The first sign of syphilis in men is often a small, painless sore (chancre) on the penis. Primary syphilis • 3 days to 3 months = small painless sore called a chancre. • The sore appears where the bacteria entered the body (e. g. external genitalia, on the cervix, in the vagina, under the foreskin, in the anus, mouth or throat). • The chancre is painless and can be missed easily; while it heals on its own without treatment, the infection remains. The chancre sore appears where the bacteria entered the body.
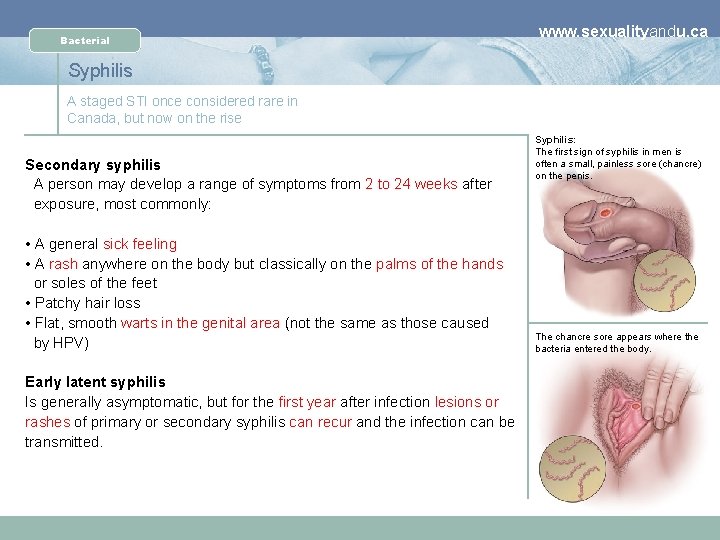
Bacterial www. sexualityandu. ca Syphilis A staged STI once considered rare in Canada, but now on the rise Secondary syphilis A person may develop a range of symptoms from 2 to 24 weeks after exposure, most commonly: • A general sick feeling • A rash anywhere on the body but classically on the palms of the hands or soles of the feet • Patchy hair loss • Flat, smooth warts in the genital area (not the same as those caused by HPV) Early latent syphilis Is generally asymptomatic, but for the first year after infection lesions or rashes of primary or secondary syphilis can recur and the infection can be transmitted. Syphilis: The first sign of syphilis in men is often a small, painless sore (chancre) on the penis. The chancre sore appears where the bacteria entered the body.
Bacterial Syphilis A staged STI once considered rare in Canada, but now on the rise Considerations and possible complications • Syphilis increases the risk of transmitting or becoming infected with HIV. Untreated syphilis may lead to tertiary syphilis, which can damage: • The cardiovascular system (heart and blood vessels) • The nervous system • Other major organs of the body • Death www. sexualityandu. ca

Viral Genital Herpes A very common viral infection that can cause genital and anal sores What is it? • Herpes simplex virus (two types: HSV-1, traditionally associated with cold sores, and HSV-2, traditionally associated with anogenital herpes) • May cause a single outbreak or recurrences over time Recurrences may be triggered by: • The menstrual cycle in women • Emotional stress • Illness (especially fever) • Sexual intercourse • Surgery • Exposure to sun (including tanning beds) • Use of certain medications www. sexualityandu. ca

Viral www. sexualityandu. ca Genital Herpes A very common viral infection that can cause genital and anal sores How is genital herpes transmitted? • Through direct vaginal, oral or anal sexual contact with an infected partner • By receiving oral sex from a partner with a history of cold sores • Transmission of the virus when there are no symptoms or lesions • From an infected woman to her infant during pregnancy or birth • Less commonly through contact with contaminated objects such as towels Condoms have limited effectiveness at preventing infection as they do not cover the entire genital area. Genital herpes: During a herpes outbreak, blister-like sores often occur, surrounded by redness and inflammation. Herpes sores may develop on the vulva.

Viral www. sexualityandu. ca Genital Herpes A very common viral infection that can cause genital and anal sores What are the signs and symptoms? • Not all infected people develop symptoms • Symptoms may emerge 2 -21 days after initial infection; usually after six • Prior to an outbreak, the infected person may feel a tingling or burning sensation where the virus first entered the skin or in the case of a recurrence, where there were lesions During an outbreak: • Painful sores (external or internal) • Inflammation and redness • Fever • Muscular pain • Tender lymph nodes An outbreak resolves in 17 days for men and 23 days for women, on average. Atypical signs and symptoms (without lesions) • Genital pain, urethritis, aseptic meningitis or cervicitis. Possible complications • Increased risk of transmitting or becoming infected with HIV

Viral www. sexualityandu. ca Genital Herpes A very common viral infection that can cause genital and anal sores Considerations • Avoid sexual activity from the start of burning/tingling symptoms until all lesions have completely healed • Pay attention to personal hygiene to avoid transmission by contaminated clothing/towels • Be aware of the potential for recurrences; watch for signs and symptoms as they may not be obvious • Condoms and drug therapy can reduce but not eliminate the risk of transmission • Though chronic in nature, herpes is a manageable infection. Counselling may be useful to help with relationship issues • Advise your gynecologist of your history of infection; precautions can be taken during pregnancy and delivery to minimize risk of transmission to the baby

Viral Hepatitis B A vaccine-preventable viral infection that affects the liver What is it? • A virus that affects the liver • A virus found in blood and body fluids including the vaginal secretions, semen, breast milk and saliva of infected individuals • Most infected people (90%) naturally produce antibodies to fight the disease, but some develop chronic hepatitis B; they carry the virus all their lives and are infectious for life • Chronic infection can significantly damage the liver • Most common in developing countries How is hepatitis B transmitted? • Through anal, vaginal or oral sex with an infected person • Through exposure to infected blood or blood products (e. g. injection drug use with shared equipment, accidental exposure, needlestick) • Occasionally from contact with shared household items (such as toothbrushes or razors) • During childbirth (transmission from mother to infant) www. sexualityandu. ca
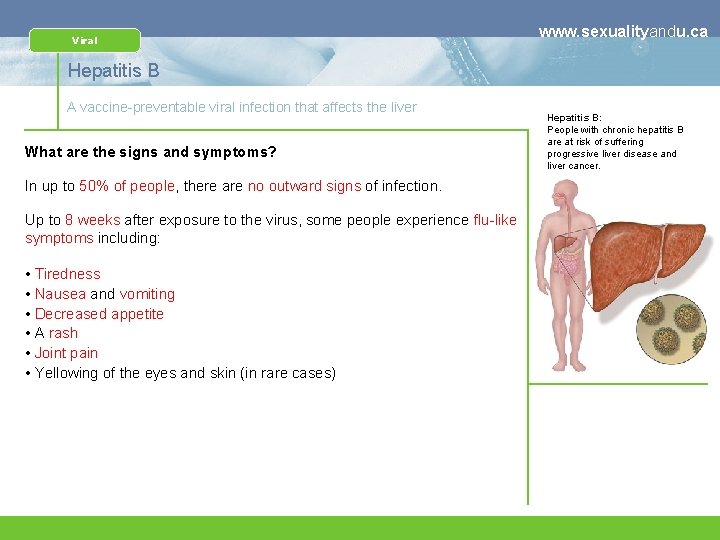
Viral www. sexualityandu. ca Hepatitis B A vaccine-preventable viral infection that affects the liver What are the signs and symptoms? In up to 50% of people, there are no outward signs of infection. Up to 8 weeks after exposure to the virus, some people experience flu-like symptoms including: • Tiredness • Nausea and vomiting • Decreased appetite • A rash • Joint pain • Yellowing of the eyes and skin (in rare cases) Hepatitis B: People with chronic hepatitis B are at risk of suffering progressive liver disease and liver cancer.

Viral www. sexualityandu. ca Hepatitis B A vaccine-preventable viral infection that affects the liver Considerations and possible complications • All sexual and household contacts of people with hepatitis B should be advised to be vaccinated to prevent infection • Chronic hepatitis B can lead to severe liver damage including cirrhosis (scarring of the liver) and cancer • Individuals who develop chronic hepatitis B infection require liver-function monitoring and may benefit from treatment with interferon or an anti-viral medication • Babies born to mothers with hepatitis B are at a high risk of becoming chronic carriers. They should receive an injection of antibodies immediately after birth, followed by the vaccine

Viral Genital Warts / HPV (Human Papilloma virus) A very common viral infection that can cause anogenital warts and cervical cancer What is it? • One of the most common sexually transmitted infections • There are over 100 types of HPV; 40 can cause anogenital infection • It is estimated that 75% of the adult population will have at least one HPV infection during their lifetime • Low-risk HPV types cause anogenital warts and other benign lesions • High-risk HPV types are associated with cancer (mainly of the cervix) • Vaccination is available to prevent certain types of HPV • Most HPV infections clear on their own within one to two years How is HPV transmitted? • Through direct sexual contact (primarily vaginal and anal sex, but oral sex is also a risk) • Other sexual activity with intimate contact (genital rubbing or activity causing friction) • To an infant during delivery (rare) www. sexualityandu. ca
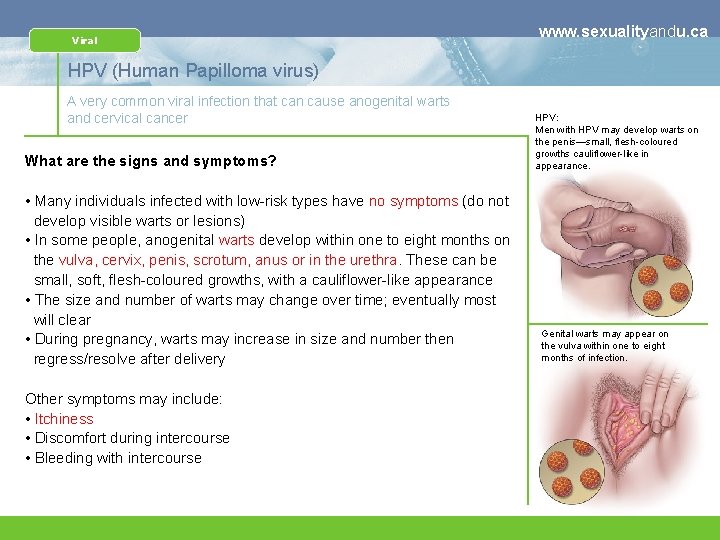
Viral www. sexualityandu. ca HPV (Human Papilloma virus) A very common viral infection that can cause anogenital warts and cervical cancer What are the signs and symptoms? • Many individuals infected with low-risk types have no symptoms (do not develop visible warts or lesions) • In some people, anogenital warts develop within one to eight months on the vulva, cervix, penis, scrotum, anus or in the urethra. These can be small, soft, flesh-coloured growths, with a cauliflower-like appearance • The size and number of warts may change over time; eventually most will clear • During pregnancy, warts may increase in size and number then regress/resolve after delivery Other symptoms may include: • Itchiness • Discomfort during intercourse • Bleeding with intercourse HPV: Men with HPV may develop warts on the penis—small, flesh-coloured growths cauliflower-like in appearance. Genital warts may appear on the vulva within one to eight months of infection.
Parasitic/Fungal Candidiasis (Yeast Infection) A common fungal infection caused by overgrowth of the naturally occurring yeast Candida What is it? • 75% of women develop vaginal candidiasis at least once in their lifetime • Candida can also affect the mouth, esophagus, skin or blood. • Yeast is normally found in a woman’s vagina. When the fungus begins to grow in excess, it may develop into candidiasis. Causes of overgrowth include: • Pregnancy • Recent or current use of antibiotics and certain other prescription medications • Sexual activity • Poorly controlled diabetes • A weakened immune system • Genital moisture retention caused by tight-fitting clothing www. sexualityandu. ca
Parasitic/Fungal Candidiasis (Yeast Infection) A common fungal infection caused by overgrowth of the naturally occurring yeast Candida How is a yeast infection transmitted? While yeast infection can be transmitted sexually, it is not generally considered an STI. Men sometimes develop signs of a yeast infection on the head (glans) of the penis after having intercourse with a woman with vaginal candidiasis. (She may have no symptoms. ) www. sexualityandu. ca
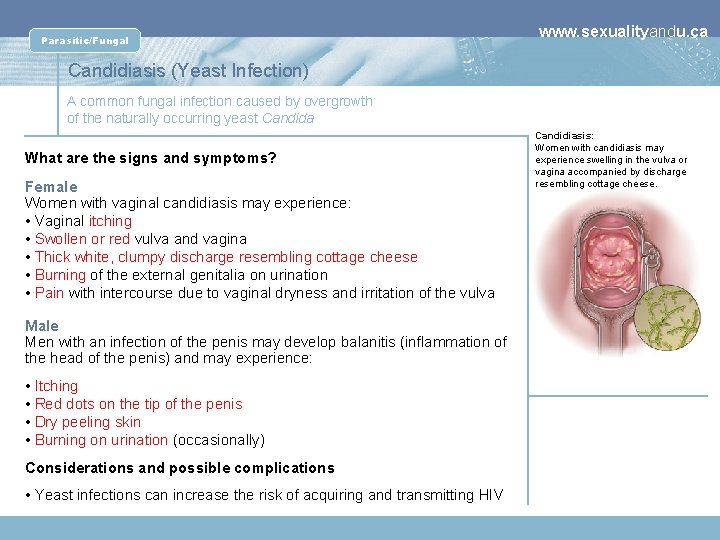
Parasitic/Fungal www. sexualityandu. ca Candidiasis (Yeast Infection) A common fungal infection caused by overgrowth of the naturally occurring yeast Candida What are the signs and symptoms? Female Women with vaginal candidiasis may experience: • Vaginal itching • Swollen or red vulva and vagina • Thick white, clumpy discharge resembling cottage cheese • Burning of the external genitalia on urination • Pain with intercourse due to vaginal dryness and irritation of the vulva Male Men with an infection of the penis may develop balanitis (inflammation of the head of the penis) and may experience: • Itching • Red dots on the tip of the penis • Dry peeling skin • Burning on urination (occasionally) Considerations and possible complications • Yeast infections can increase the risk of acquiring and transmitting HIV Candidiasis: Women with candidiasis may experience swelling in the vulva or vagina accompanied by discharge resembling cottage cheese.
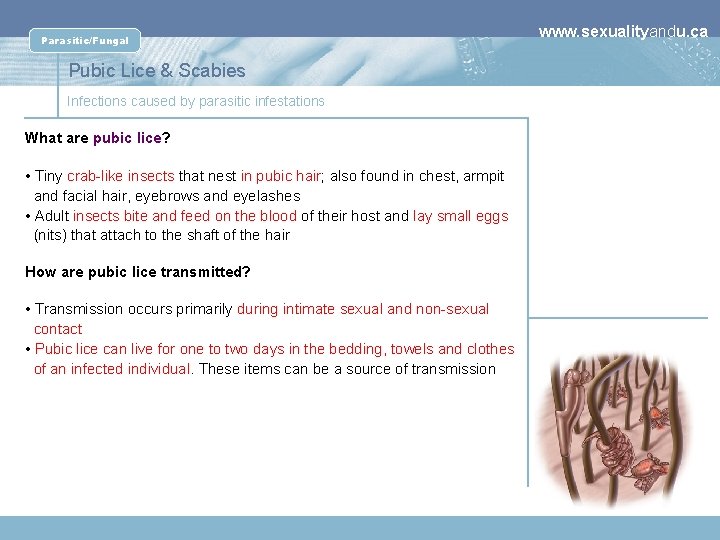
Parasitic/Fungal Pubic Lice & Scabies Infections caused by parasitic infestations What are pubic lice? • Tiny crab-like insects that nest in pubic hair; also found in chest, armpit and facial hair, eyebrows and eyelashes • Adult insects bite and feed on the blood of their host and lay small eggs (nits) that attach to the shaft of the hair How are pubic lice transmitted? • Transmission occurs primarily during intimate sexual and non-sexual contact • Pubic lice can live for one to two days in the bedding, towels and clothes of an infected individual. These items can be a source of transmission www. sexualityandu. ca

Parasitic/Fungal www. sexualityandu. ca Pubic Lice & Scabies Infections caused by parasitic infestations What are the signs and symptoms? Pubic lice and nits are small and can be difficult to spot. Infected individuals may experience: • Skin irritation and inflammation accompanied by itchiness and redness • Small blue spots on the skin where lice have bitten • Louse feces (fine black particles) in the infected person’s undergarments Considerations and possible complications • Persistent scratching of irritated skin cause a secondary bacterial infection • All sexual partners who have had contact with the infected person in the month before diagnosis should be treated to help prevent reinfestation • Clothes, bedding and other possible contaminated items should be washed or dry-cleaned, or bagged for a week. Items that cannot be washed or bagged should be vacuumed Pubic lice: The insects bite their host to feed on blood.
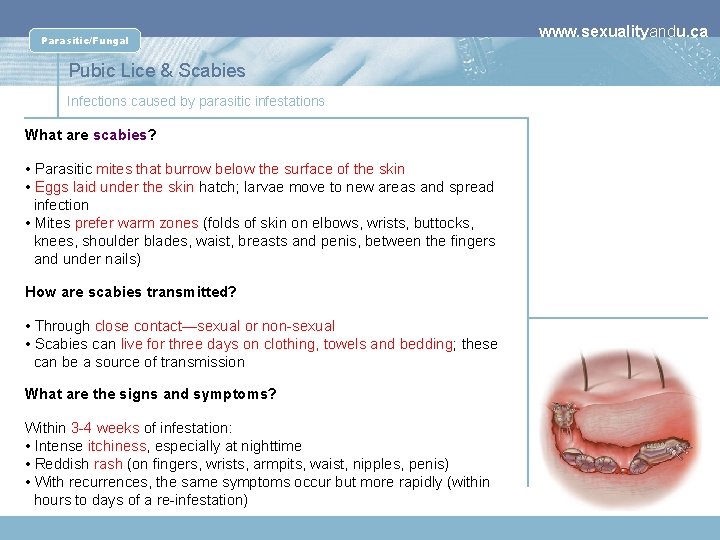
Parasitic/Fungal Pubic Lice & Scabies Infections caused by parasitic infestations What are scabies? • Parasitic mites that burrow below the surface of the skin • Eggs laid under the skin hatch; larvae move to new areas and spread infection • Mites prefer warm zones (folds of skin on elbows, wrists, buttocks, knees, shoulder blades, waist, breasts and penis, between the fingers and under nails) How are scabies transmitted? • Through close contact—sexual or non-sexual • Scabies can live for three days on clothing, towels and bedding; these can be a source of transmission What are the signs and symptoms? Within 3 -4 weeks of infestation: • Intense itchiness, especially at nighttime • Reddish rash (on fingers, wrists, armpits, waist, nipples, penis) • With recurrences, the same symptoms occur but more rapidly (within hours to days of a re-infestation) www. sexualityandu. ca
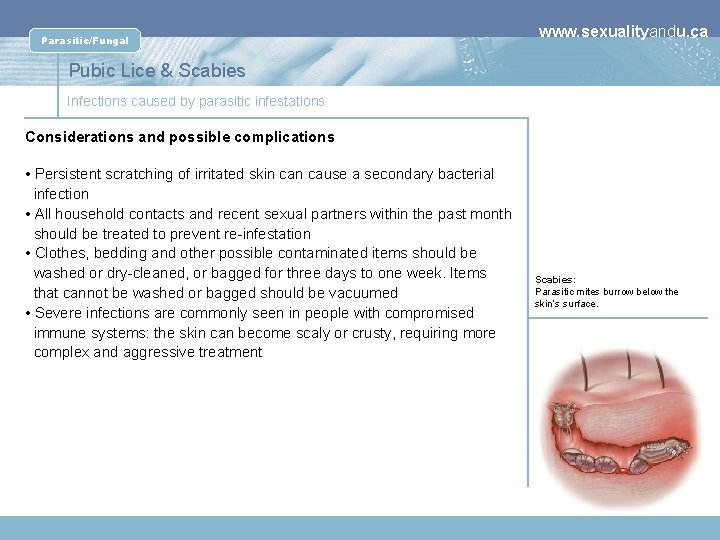
Parasitic/Fungal www. sexualityandu. ca Pubic Lice & Scabies Infections caused by parasitic infestations Considerations and possible complications • Persistent scratching of irritated skin cause a secondary bacterial infection • All household contacts and recent sexual partners within the past month should be treated to prevent re-infestation • Clothes, bedding and other possible contaminated items should be washed or dry-cleaned, or bagged for three days to one week. Items that cannot be washed or bagged should be vacuumed • Severe infections are commonly seen in people with compromised immune systems: the skin can become scaly or crusty, requiring more complex and aggressive treatment Scabies: Parasitic mites burrow below the skin’s surface.
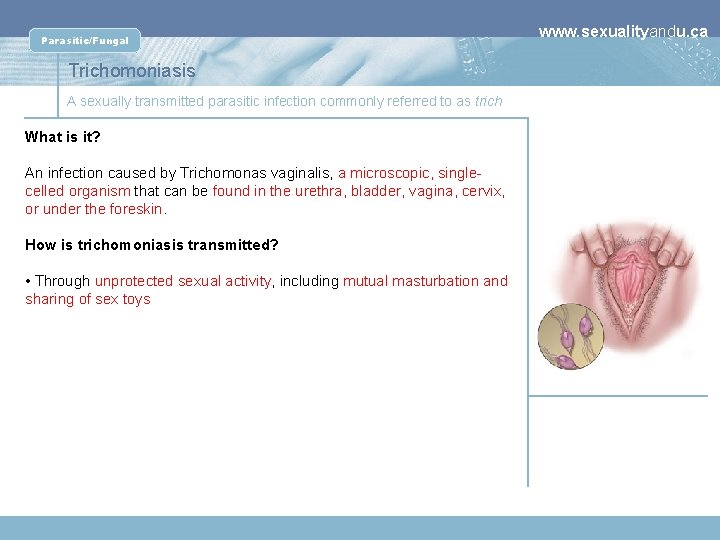
Parasitic/Fungal Trichomoniasis A sexually transmitted parasitic infection commonly referred to as trich What is it? An infection caused by Trichomonas vaginalis, a microscopic, singlecelled organism that can be found in the urethra, bladder, vagina, cervix, or under the foreskin. How is trichomoniasis transmitted? • Through unprotected sexual activity, including mutual masturbation and sharing of sex toys www. sexualityandu. ca
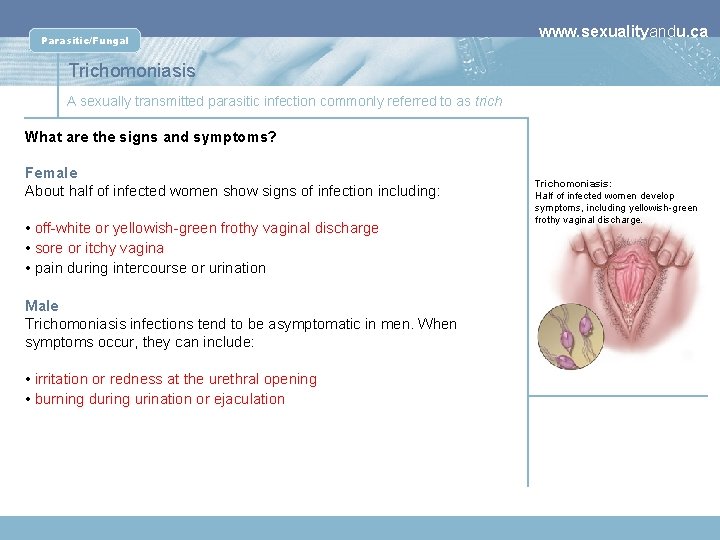
Parasitic/Fungal www. sexualityandu. ca Trichomoniasis A sexually transmitted parasitic infection commonly referred to as trich What are the signs and symptoms? Female About half of infected women show signs of infection including: • off-white or yellowish-green frothy vaginal discharge • sore or itchy vagina • pain during intercourse or urination Male Trichomoniasis infections tend to be asymptomatic in men. When symptoms occur, they can include: • irritation or redness at the urethral opening • burning during urination or ejaculation Trichomoniasis: Half of infected women develop symptoms, including yellowish-green frothy vaginal discharge.
Parasitic/Fungal www. sexualityandu. ca Trichomoniasis A sexually transmitted parasitic infection commonly referred to as trich Considerations and possible complications • Trichomoniasis infections can increase the risk of acquiring and transmitting HIV • Trich may occur in conjunction with other STIs, such as gonorrhea, chlamydia, syphilis, HIV and hepatitis B • In pregnancy, trichomoniasis infection may increase the risk of pre-term delivery and low birth weight
Testing/Screening Importance and Timing The early detection and treatment of STIs is critical to prevent further spread of infections Decreasing the risks Early identification and treatment of an STI can help decrease the possibility of complications, both for an infected individual and their sexual partner(s). This is especially true for women, as undetected and untreated infections can lead to pelvic inflammatory disease, ectopic pregnancy, chronic pelvic pain and even infertility. www. sexualityandu. ca
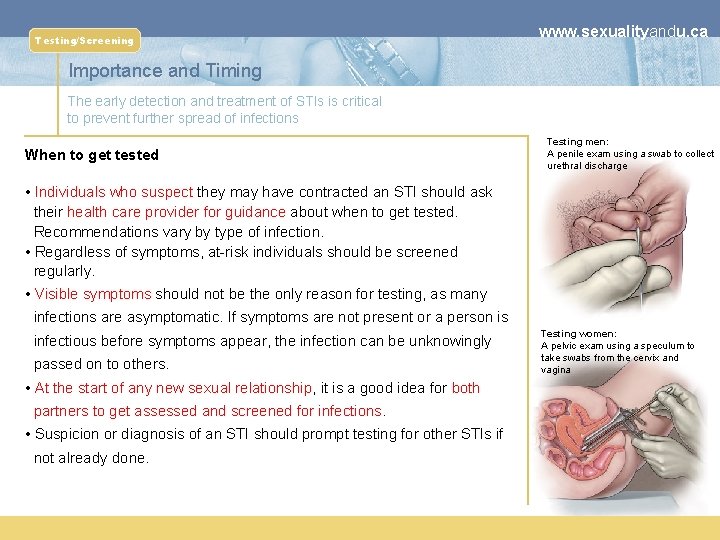
Testing/Screening www. sexualityandu. ca Importance and Timing The early detection and treatment of STIs is critical to prevent further spread of infections When to get tested Testing men: A penile exam using a swab to collect urethral discharge • Individuals who suspect they may have contracted an STI should ask their health care provider for guidance about when to get tested. Recommendations vary by type of infection. • Regardless of symptoms, at-risk individuals should be screened regularly. • Visible symptoms should not be the only reason for testing, as many infections are asymptomatic. If symptoms are not present or a person is infectious before symptoms appear, the infection can be unknowingly passed on to others. • At the start of any new sexual relationship, it is a good idea for both partners to get assessed and screened for infections. • Suspicion or diagnosis of an STI should prompt testing for other STIs if not already done. Testing women: A pelvic exam using a speculum to take swabs from the cervix and vagina
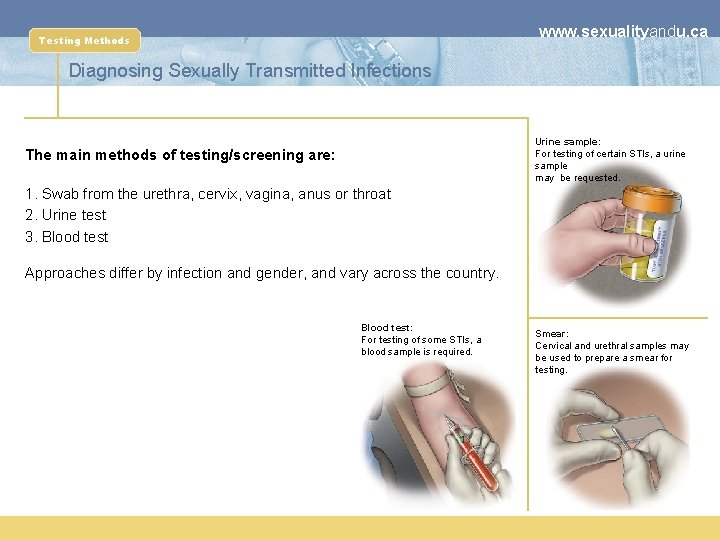
www. sexualityandu. ca Testing Methods Diagnosing Sexually Transmitted Infections Urine sample: For testing of certain STIs, a urine sample may be requested. The main methods of testing/screening are: 1. Swab from the urethra, cervix, vagina, anus or throat 2. Urine test 3. Blood test Approaches differ by infection and gender, and vary across the country. Blood test: For testing of some STIs, a blood sample is required. Smear: Cervical and urethral samples may be used to prepare a smear for testing.
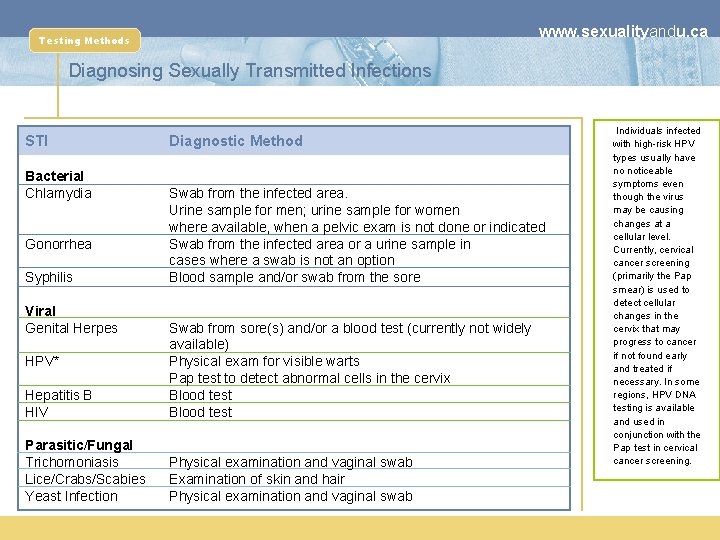
www. sexualityandu. ca Testing Methods Diagnosing Sexually Transmitted Infections STI Bacterial Chlamydia Gonorrhea Syphilis Viral Genital Herpes Diagnostic Method Swab from the infected area. Urine sample for men; urine sample for women where available, when a pelvic exam is not done or indicated Swab from the infected area or a urine sample in cases where a swab is not an option Blood sample and/or swab from the sore Hepatitis B HIV Swab from sore(s) and/or a blood test (currently not widely available) Physical exam for visible warts Pap test to detect abnormal cells in the cervix Blood test Parasitic/Fungal Trichomoniasis Lice/Crabs/Scabies Yeast Infection Physical examination and vaginal swab Examination of skin and hair Physical examination and vaginal swab HPV* Individuals infected with high-risk HPV types usually have no noticeable symptoms even though the virus may be causing changes at a cellular level. Currently, cervical cancer screening (primarily the Pap smear) is used to detect cellular changes in the cervix that may progress to cancer if not found early and treated if necessary. In some regions, HPV DNA testing is available and used in conjunction with the Pap test in cervical cancer screening.
Prevention www. sexualityandu. ca Barrier Methods Prevention approaches are important to decrease the transmission of STIs Blocking transmission Barrier methods are very effective in the prevention of many sexually transmitted infections (STIs). Male and female condoms made of latex and polyurethane offer the best protection. Note: Latex and polyurethane condoms may not fully protect against herpes and HPV, as the viruses can be found in areas not protected by a condom. Dental dams are an effective option for oral sex. Proper use of barrier methods is critical. Illustrations: © 2007 GCT II Solutions and Enterprises Ltd. � • Male condom • Female condom • Dental dam

Prevention www. sexualityandu. ca Barrier Methods Prevention approaches are important to decrease the transmission of STIs Male condom: A male condom prevents the exchange of fluids during intercourse. A male condom is a sheath placed on an erect penis to prevent the exchange of fluids between partners during intercourse or oral sex. Polyurethane condoms are also highly effective, but are more prone to breakage. Condoms made from sheep membrane are not effective barriers. Illustrations: © 2007 GCT II Solutions and Enterprises Ltd. � Latex condoms offer protection against the transmission of many (not all) STIs.

Prevention www. sexualityandu. ca Barrier Methods Prevention approaches are important to decrease the transmission of STIs Male condom: A male condom prevents the exchange of fluids during intercourse. • Found in many stores. • Available without doctor prescription. • Inexpensive. • Protects against most STIs. • Allows male partner to assume some responsibility. DISADVANTAGES • Must be available at time is sexual activity. • May slip or break. • Must be stored and handled properly. • Does not protect against all STIs (e. g. , craps, herpes). • Expiry date. Illustrations: © 2007 GCT II Solutions and Enterprises Ltd. � ADVANTAGES

How To Use A Male Condom 1. Check expiry date. Open package carefully so don’t rip the condom. 2. Make sure tip of condom points through the ring. 3. Pinch end to remove air. 4. Place on tip of penis leaving 1/2 inch space at end for semen collection. 5. Unroll over erect penis right down to the base. (Uncircumcised men should put back foreskin. ) 6. After ejaculation (and before soft) hold condom against penis as slide the condom off. 7. Discard into trash. Demo

Prevention www. sexualityandu. ca Barrier Methods Prevention approaches are important to decrease the transmission of STIs Female condom A female condom is a polyurethane sheath worn inside the vagina during sexual intercourse. It should not be used with a male condom. Female condom: The female condom is inserted into the vagina prior to entry by the penis. Illustrations: © 2007 GCT II Solutions and Enterprises Ltd. � It has two rings, an inner one at the closed end, used to insert the condom and hold it in place behind the pubic bone; and an outer ring that remains outside the vagina.
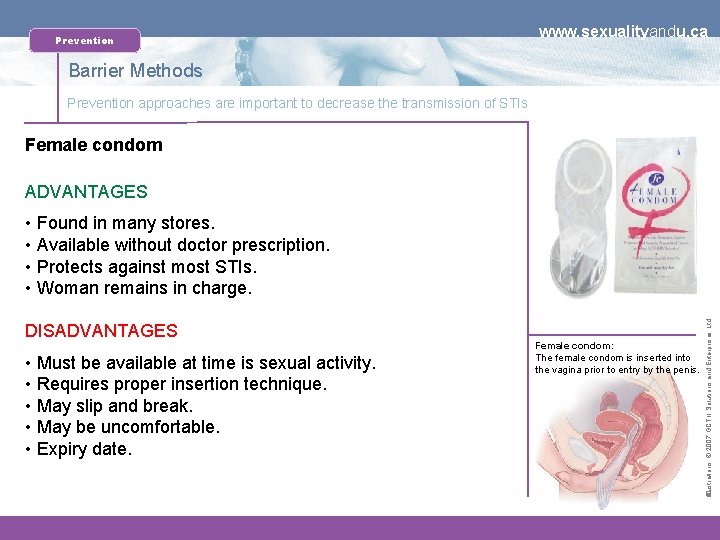
Prevention www. sexualityandu. ca Barrier Methods Prevention approaches are important to decrease the transmission of STIs Female condom ADVANTAGES DISADVANTAGES • Must be available at time is sexual activity. • Requires proper insertion technique. • May slip and break. • May be uncomfortable. • Expiry date. Female condom: The female condom is inserted into the vagina prior to entry by the penis. Illustrations: © 2007 GCT II Solutions and Enterprises Ltd. � • Found in many stores. • Available without doctor prescription. • Protects against most STIs. • Woman remains in charge.

How To Use A Female Condom 1. Check expiry date. Open package carefully so don’t rip the condom. 2. Inner ring should be far in the vagina. 3. Outer ring should be outside the vagina. 4. Guide penis into condom. 5. NOT to be used with a male condom. 6. After intercourse, remove condom by pulling it out gently. 7. Discard into trash.

www. sexualityandu. ca Prevention Barrier Methods Prevention approaches are important to decrease the transmission of STIs A dental dam is a thin square of latex that can be used as a shield during oral sex. The dam is placed over a woman’s vulva, acting as a barrier between her genitals and her partner’s mouth. Dams are for sale in some pharmacies and sexual-health clinics, but can also be made using a condom. Simply unroll the condom, cut off the tip and base and cut down the length of the tube. Then unroll the condom into a rectangular sheet. Cutting a condom to make a dental dam 1 2 3 Illustrations: © 2007 GCT II Solutions and Enterprises Ltd. � Dental dam

What does HIV stand for? H uman I mmunodeficiency V irus

What does AIDS stand for? A cquired I mmune D eficiency S yndrome
Viral HIV (Human Immunodeficiency Virus) A virus that attacks the body’s immune system, leaving infected individuals unable to ward off other illnesses What is it? • Virus that destroys cells critical to a person’s immune system, robbing the body of its ability to fight other infections and illnesses. • Weakens the immune system over time (months to years) until other infections occur and Acquired Immunodeficiency Syndrome or AIDS (the fatal stage of HIV infection) develops. www. sexualityandu. ca
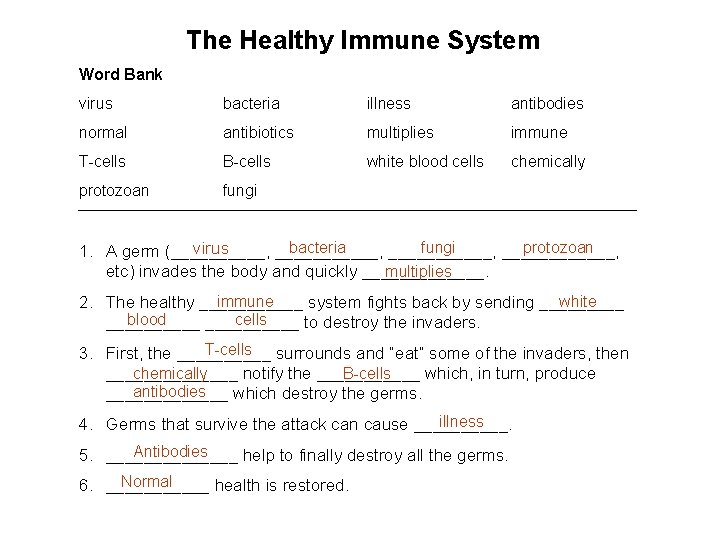
The Healthy Immune System Word Bank virus bacteria illness antibodies normal antibiotics multiplies immune T-cells B-cells white blood cells chemically protozoan fungi bacteria fungi protozoan virus 1. A germ (__________, ______, etc) invades the body and quickly _______. multiplies immune white 2. The healthy ______ system fights back by sending _____ blood cells __________ to destroy the invaders. T-cells surrounds and “eat” some of the invaders, then 3. First, the ______________ notify the ______ which, in turn, produce chemically B-cells antibodies _______ which destroy the germs. illness 4. Germs that survive the attack can cause _____. Antibodies 5. _______ help to finally destroy all the germs. Normal 6. ______ health is restored.

AIDS-Infected Immune System Word Bank Kaposi’s B-cells factories attaches T-cells HIV cannot antibodies destroyed die pneumonia opportunistic dementia HIV 1. The _______ invades the body and quickly multiplies. The immune system tries to fight back by sending white blood cells to destroy the invaders. T-cells 2. _____ surround attempt to “eat” the HIV but the HIV attaches ______ itself to the T-cells causing them to become HIV-producing _______. factories cannot B-cells 3. The T-cells _______ chemically notify the _____, and therefore, the _____ cannot produce _______. B-cells antibodies destroyed 4. The immune system is _______ and the person is susceptible to opportunistic many ________ diseases, such as: pneumonia Kaposi’s sarcoma, and AIDS pneumocystis carinii _______, _____________ complex. These diseases usually cause the person to dementia ______. die

Viral HIV (Human Immunodeficiency Virus) A virus that attacks the body’s immune system, leaving infected individuals unable to ward off other illnesses How is HIV transmitted? When the body fluids of an infected person (blood, semen, pre-semen, vaginal secretions, breast milk) enter the blood stream of another individual—specifically, from: • Unprotected vaginal, oral or anal sex • Shared needles or other drug equipment (i. e. water, cookers, crack pipes) • HIV-infected blood or blood products • Household items such as toothbrushes and razors that have touched infected blood • Transmission during pregnancy, childbirth or breastfeeding (transmission from mother to child) • HIV cannot be transmitted by mosquitoes or other insects that have made contact with infected blood, nor can it be transmitted through saliva, sweat, tears, urine or feces of infected individuals, unless blood is present. www. sexualityandu. ca
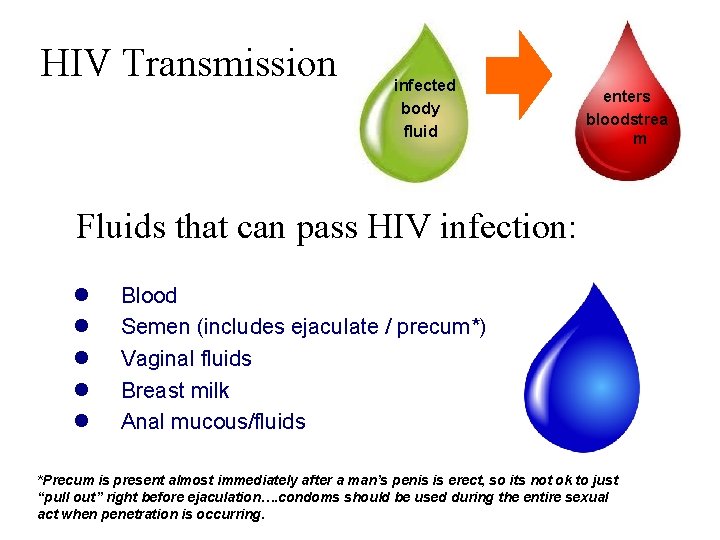
HIV Transmission infected body fluid enters bloodstrea m Fluids that can pass HIV infection: l l l Blood Semen (includes ejaculate / precum*) Vaginal fluids Breast milk Anal mucous/fluids *Precum is present almost immediately after a man’s penis is erect, so its not ok to just “pull out” right before ejaculation…. condoms should be used during the entire sexual act when penetration is occurring.
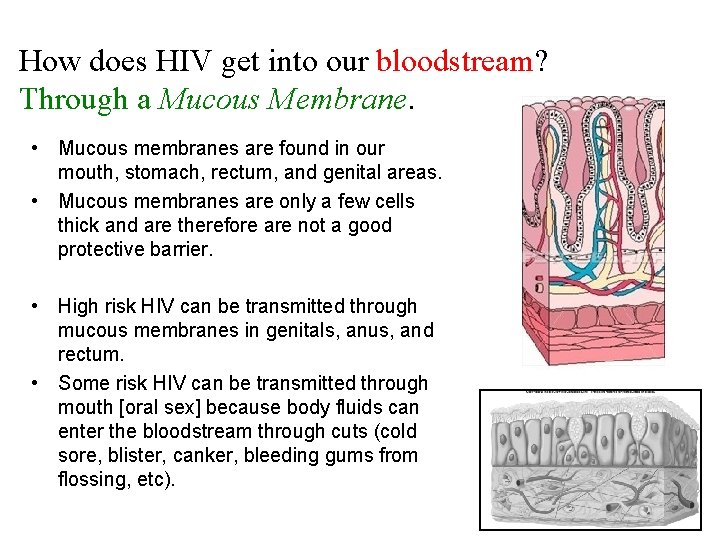
How does HIV get into our bloodstream? Through a Mucous Membrane. • Mucous membranes are found in our mouth, stomach, rectum, and genital areas. • Mucous membranes are only a few cells thick and are therefore are not a good protective barrier. • High risk HIV can be transmitted through mucous membranes in genitals, anus, and rectum. • Some risk HIV can be transmitted through mouth [oral sex] because body fluids can enter the bloodstream through cuts (cold sore, blister, canker, bleeding gums from flossing, etc).

These are MYTHS. AIDS is not transmitted by: • Insects or animals • Coughing or sneezing • Casual body contact (shaking hands, hugging) • Food • Dishes or glasses • Pools or saunas You might want to write a few of these down (wink). • Toilet seats • Playground equipment • Drinking fountains • Telephones • Artificial insemination (using a sperm bank to become pregnant) AIDS IS NOT AN EASY DISEASE TO GET!

Viral www. sexualityandu. ca HIV (Human Immunodeficiency Virus) A virus that attacks the body’s immune system, leaving infected individuals unable to ward off other illnesses What are the signs and symptoms? 2 -4 weeks after exposure, some infected individuals may experience mild flu-like symptoms that last a few weeks then disappear. HIV: An individual who is diagnosed with HIV requires regular medical consultation. For most people, symptoms don’t emerge until years after exposure. Once the immune system is weakened, the following may develop: • Frequent fever or sweats • Joint or muscle pain • Persistent skin rashes • Swollen glands • Sore throat • Fatigue or lack of energy • Headaches • Rapid, unexplained weight loss • Nausea, vomiting, or diarrhea A blood test to check for HIV antibodies is the only way to detect HIV infection. It may take up to three months for an infection to be detectable. Anyone at high risk who tests negative initially should retest three months later for certainty. HIV destroys cells critical to the immune system, leaving carriers susceptible to other infections.

Symptoms of HIV infection: • Flu-like (prolonged); fever, loss of appetite, sore throat, etc. • Swollen lymph nodes. • Can take up to 4 weeks for “seroconversion” to occur (antibodies are detected in blood). • After initial symptoms, any others may not occur for months/years. • Differs from 1 person to the next person.

Mark has a friend who can do cheap tattoos and piercing, should he have it done? Answer : Maybe. . . Only have tattooing and piercing done at a certified establishment. Equipment that has not been properly cleaned can transmit HIV, Hepatitis and bacterial skin infections.

Tattooing and Piercing Get Good Clean Art What are the risks? § Blood-borne infections § Skin disorders § Allergic reactions Be a smart consumer. Take your time. Think about it. ü Go to an Expert Artist in an Inspected Shop

Here's a checklist of what the artist must provide for your safety: ü Clean Hands ü New Sterile Needles ü Clean and Sterilized Equipment ü Clean Skin ü No Double Dipping ü Quality Jewelry ü Gun Control ü After Care Instructions

HIV Testing in Waterloo Region 1. Family doctor 2. Anonymous testing available at the Waterloo Regional Community Health Department 3. Confidential HIV testing available at the Waterloo Regional Community Health Department STD clinics in Waterloo and Cambridge *The fastest growing HIV positive age group, including teenagers, is the 15 -24 year old age group!!!

Aids Information Video Click the above hyperlink to access the video http: //teachaids. org/flash/english/

AIDS: Answers for Young People Video 11559 - 19 mins. doubling Among teenagers in the U. S. , AIDS is more than ______ every two years! The progress 5 -10 of AIDS is slow. It’s often _____ years before you get sick. acquired AIDS stands for A-_________ immune I-__________ deficiency D-_________ syndrome S-_________ skin The first line of defense against AIDS is the ____ and mucous membranes. The second immune system line of defense is the ______. This immune system manufactures white T B blood cells which help fight disease. The ___-cells send out an alarm to the ___-cells which are the fighters that attack any invading organism. Together the T-cells and B-cells help fight off sickness and disease. When the AIDS virus, known as HIV (Human Immunodeficiency Virus), enters the body it T attacks the ___-cells. Once it takes over the T-cells, the virus will multiply and take over the Tcell. This T-cell will weaken and break therefore exposing other T-cells in the body to the virus. B Eventually the T-cells will no longer be able to activate the fighter ___-cells which means the immune system can no longer do its job. This means that the body can’t fight off disease.

AIDS: Answers for Young People continued infected sick Primary Stage- You become ______ with the HIV virus but you don’t feel ____. years Virus takes _____ to damage the immune system enough to make you feel sick. You carrier become a _____ of the AIDS virus during this stage. protect Middle Stage- Your immune system doesn’t ______ you and you will start to notice sweats symptoms such as: swollen glands, mouth sores, night ______, bad coughs, rashes, flu chronic diarrhea, unexplained weight loss, and _______-like symptoms that don’t go away. Full blown Final Stage-____ - ______ AIDS. During this stage serious diseases like lungs cancer pneumonia in the _____, and _____ that causes bleeding under the skin and inside the body can occur. The _____ and nervous system are also attacked during this stage. brain cure drugs There is no _____ for AIDS. Modern _____ have helped extend the life expectancy of AIDS patients. The AIDS virus is transmitted through blood, ______, and _______ semen fluid. vaginal Obviously sex and any activities where blood could be exchanged need to be avoided. Don’t share needles, razors, and don’t become blood brothers or sisters with anybody. Tattooing and any body _____piercing should be done by professionals. The AIDS virus can also transmitted from mother to baby. Since ____, they’ve been able to test blood for the AIDS 1985 virus and so there’s very little risk of getting AIDS from blood transfusions. There’s a _____ denial amongst teenagers about the possibility of getting AIDS. _____pressure often Peer influences teen to become sexually active before they are ____. The best way to ready avoid abstinence getting AIDS is by ______. The bottom line is “Be smart and be _______!” careful Avoid _______ and drinking taking ______ as they drugs can impair your common sense. Get _______ and live! educated
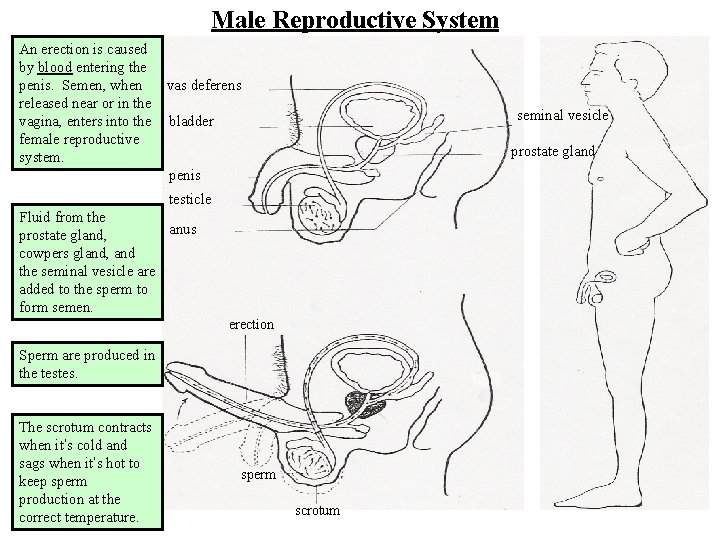
Male Reproductive System An erection is caused by blood entering the penis. Semen, when released near or in the vagina, enters into the female reproductive system. vas deferens seminal vesicle bladder prostate gland penis testicle Fluid from the anus prostate gland, cowpers gland, and the seminal vesicle are added to the sperm to form semen. erection Sperm are produced in the testes. The scrotum contracts when it’s cold and sags when it’s hot to keep sperm production at the correct temperature. sperm scrotum
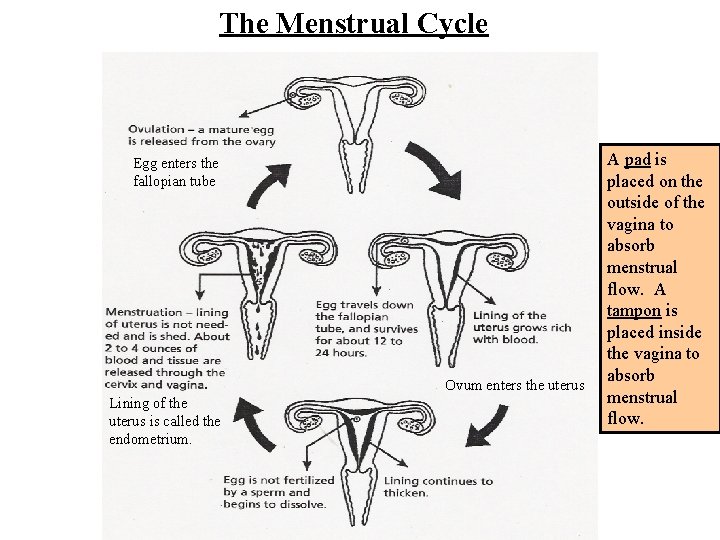
The Menstrual Cycle Egg enters the fallopian tube Ovum enters the uterus Lining of the uterus is called the endometrium. A pad is placed on the outside of the vagina to absorb menstrual flow. A tampon is placed inside the vagina to absorb menstrual flow.
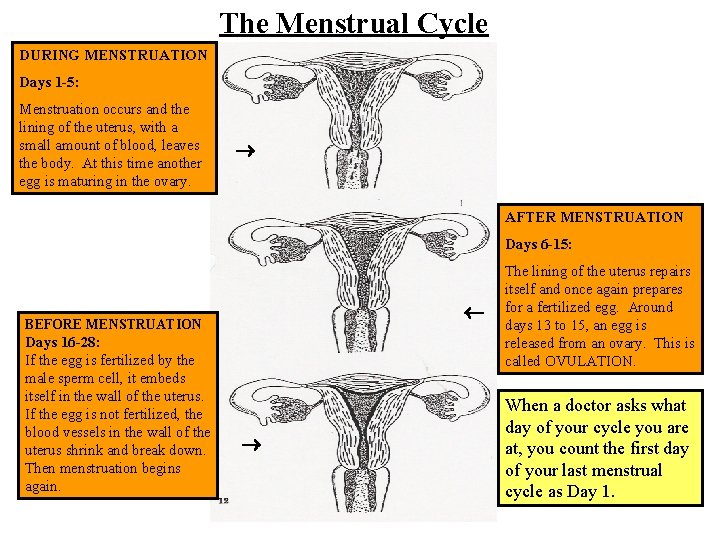
The Menstrual Cycle DURING MENSTRUATION Days 1 -5: Menstruation occurs and the lining of the uterus, with a small amount of blood, leaves the body. At this time another egg is maturing in the ovary. AFTER MENSTRUATION Days 6 -15: BEFORE MENSTRUATION Days 16 -28: If the egg is fertilized by the male sperm cell, it embeds itself in the wall of the uterus. If the egg is not fertilized, the blood vessels in the wall of the uterus shrink and break down. Then menstruation begins again. The lining of the uterus repairs itself and once again prepares for a fertilized egg. Around days 13 to 15, an egg is released from an ovary. This is called OVULATION. When a doctor asks what day of your cycle you are at, you count the first day of your last menstrual cycle as Day 1.
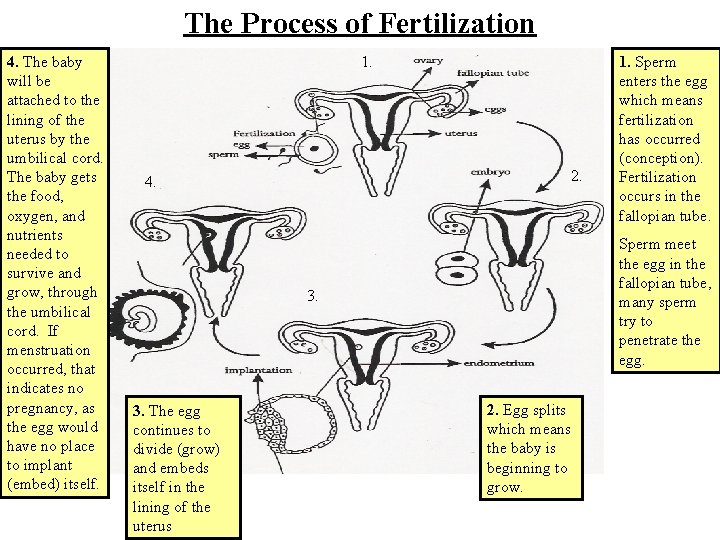
The Process of Fertilization 4. The baby will be attached to the lining of the uterus by the umbilical cord. The baby gets the food, oxygen, and nutrients needed to survive and grow, through the umbilical cord. If menstruation occurred, that indicates no pregnancy, as the egg would have no place to implant (embed) itself. 1. 2. 4. Sperm meet the egg in the fallopian tube, many sperm try to penetrate the egg. 3. The egg continues to divide (grow) and embeds itself in the lining of the uterus 1. Sperm enters the egg which means fertilization has occurred (conception). Fertilization occurs in the fallopian tube. 2. Egg splits which means the baby is beginning to grow.
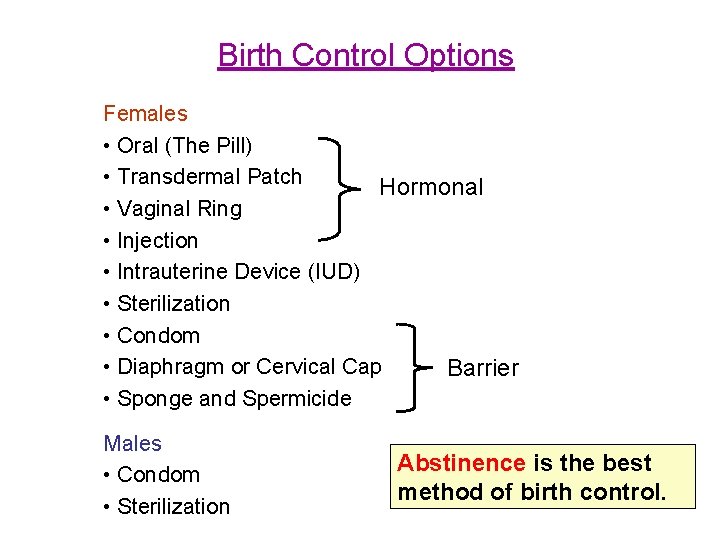
Birth Control Options Females • Oral (The Pill) • Transdermal Patch Hormonal • Vaginal Ring • Injection • Intrauterine Device (IUD) • Sterilization • Condom • Diaphragm or Cervical Cap Barrier • Sponge and Spermicide Males • Condom • Sterilization Abstinence is the best method of birth control.

Oral Contraceptives sexualityandu. ca What are they? • Prescription tablets taken once a day • There are two main types: 1. Combination pill which contains two female hormones similar to the body’s own estrogen and progesterone 2. Progestin-only pill (or mini-pill) which does not contain estrogen • Available under a variety of brand names with various strengths and formulations How do they work? • Stop the release of a mature egg • Thicken the cervical mucus making it difficult for sperm to get to the egg • Change the lining of the uterus making implantation difficult Failure rate: 80 per 1000 women per year (8%)

Oral Contraceptives sexualityandu. ca What are the advantages? 1. One of the most effective reversible birth control methods when taken consistently and reliably 2. Simple and easy to use 3. Regulates menstrual cycle and reduces cramps 4. Does not interfere with intercourse 5. Decreases acne 6. Reduces the risks of endometrial and ovarian cancer 7. May reduce perimenopausal symptoms

Oral Contraceptives sexualityandu. ca What are the disadvantages? 1. Must be taken every day. The progestin-only pill must be taken at the same time every day 2. May cause irregular bleeding or spotting 3. Effectiveness may be reduced by other medications 4. Should not be used by women over the age of 35 who smoke 5. May increase the risk of blood clots, particularly in women who have certain blood disorders or a family history of blood clots 6. Does not protect against STIs 7. May increase the number of headaches 8. May not be suitable for breastfeeding women
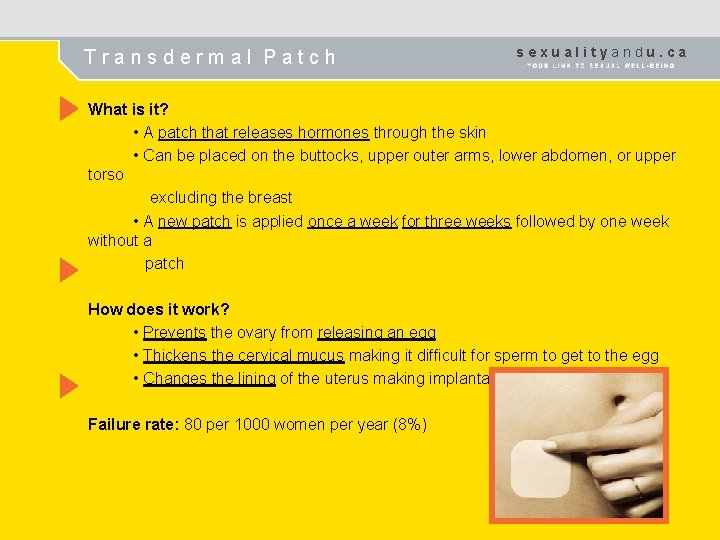
Transdermal Patch sexualityandu. ca What is it? • A patch that releases hormones through the skin • Can be placed on the buttocks, upper outer arms, lower abdomen, or upper torso excluding the breast • A new patch is applied once a week for three weeks followed by one week without a patch How does it work? • Prevents the ovary from releasing an egg • Thickens the cervical mucus making it difficult for sperm to get to the egg • Changes the lining of the uterus making implantation difficult Failure rate: 80 per 1000 women per year (8%)

Transdermal Patch sexualityandu. ca What are the advantages? 1. A reversible and highly effective birth control method 2. Once-a-week regimen; no daily contraceptive routine required 3. Simple and easy to use 4. Regulates menstrual cycle and reduces cramps 5. Does not interfere with intercourse 6. Expected to provide other benefits similar to oral contraceptives; research is needed

Transdermal Patch sexualityandu. ca What are the disadvantages? 1. May cause irregular bleeding or spotting 2. May cause breast sensitivity or headache 3. Does not protect against STIs 4. Patch may detach from skin (less than 2%) 5. Possible skin irritation at the application site

Vaginal Ring sexualityandu. ca What is it? • A flexible, nearly transparent ring that measures 54 mm (about 2 inches) across • The ring releases a continuous dose of hormones for three weeks while it is in the vagina How does it work? • Prevents the ovary from releasing an egg • Thickens the cervical mucus making it difficult for sperm to reach the egg • Changes the lining of the uterus making implantation difficult Failure rate: 80 per 1000 women per year (8%)

Vaginal Ring sexualityandu. ca What are the advantages? 1. A reversible and highly effective birth control method 2. Once-a-month regimen; no daily contraceptive routine required 3. Regulates menstrual cycles 4. Does not interfere with intercourse 5. Does not require daily attention 6. Expected to provide other benefits similar to oral contraceptives; research is needed

Vaginal Ring sexualityandu. ca What are the disadvantages? 1. Does not protect against STIs 2. May cause irregular bleeding or spotting 3. May cause side effects such as headache, nausea, or breast tenderness 4. May cause vaginal discomfort 5. The ring may be expelled from the vagina but this is uncommon

Injectable Contraceptive sexualityandu. ca What is it? • It contains a hormone called progesterone; it does not contain estrogen • The injection is given in the upper arm or buttocks every 12 to 13 weeks (four times a year) How does it work? • Prevents the ovary from releasing an egg • Thickens the cervical mucus making it difficult for sperm to get to the egg • Changes the lining of the uterus making implantation difficult Failure rate: 30 per 1000 women per year (3%)

Injectable Contraceptive sexualityandu. ca What are the advantages? 1. One of the most effective reversible birth control methods available 2. Does not contain estrogen 3. No daily contraceptive routine required; 1 injection lasts for 3 months 4. Effectiveness is not reduced by other common medications 5. May be suitable for breastfeeding women or women who smoke 6. With continued use, menstrual cycles cease in over half of users after the first year, and two-thirds of users after two years of use 7. Improves symptoms of endometriosis 8. Reduces the risk of endometrial cancer 9. Effective immediately when given during the first 5 days of a normal menstrual period

Injectable Contraceptive sexualityandu. ca What are the disadvantages? 1. Initially, irregular bleeding is the most common side effect 2. Decrease in bone mineral density which may be reversible when a woman stops taking the injection. Calcium supplementation is advised. 3. May be associated with weight gain in some women 4. Takes an average of nine months after the last injection for the ovaries to start releasing eggs again 5. Does not protect against STIs 6. The lack of a monthly period may be bothersome for some women

sexualityandu. ca Side-Effects of Hormonal Contraception Side effects that may occur during the first few months on hormonal contraception include : § § § irregular bleeding, spotting nausea mood swings bloating breast tenderness headaches

sexualityandu. ca Side-Effects of Hormonal Contraception Reason: § § Your body is getting used to birth control Fluctuating hormone levels when you start - When will it stop? § Most symptoms are normal and will decrease or stop in the first 2 -3 months. If they bother you or don’t get better: § Talk to your healthcare provider § There might be a method that’s better suited for you.

sexualityandu. ca Myths and Misconceptions about Hormonal Contraception Common myths and misconceptions § § § § Causes weight gain Causes acne Causes infertility Causes birth defects Should take a break from time to time Smokers should not be taking it Women over age 35 should not take the Pill No need for condoms if you’re on the Pill
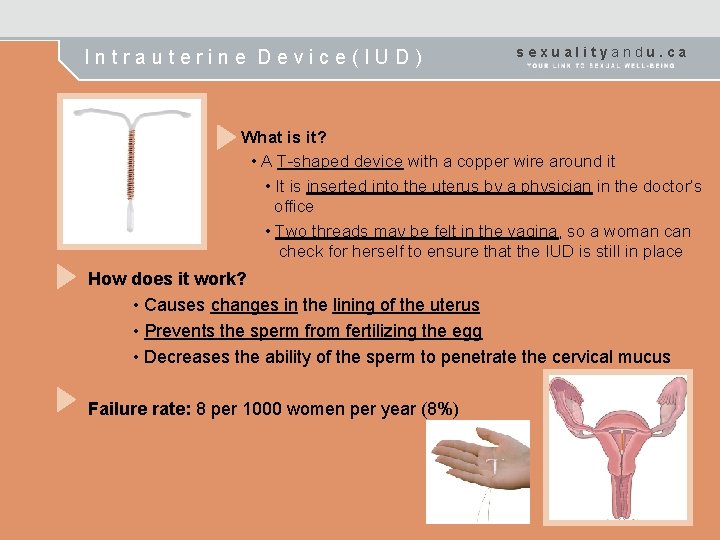
Intrauterine Device(IUD) sexualityandu. ca What is it? • A T-shaped device with a copper wire around it • It is inserted into the uterus by a physician in the doctor’s office • Two threads may be felt in the vagina, so a woman check for herself to ensure that the IUD is still in place How does it work? • Causes changes in the lining of the uterus • Prevents the sperm from fertilizing the egg • Decreases the ability of the sperm to penetrate the cervical mucus Failure rate: 8 per 1000 women per year (8%)

Intrauterine Device(IUD) sexualityandu. ca What are the advantages? 1. Long-acting contraceptive; can be left in place for up to five years 2. No daily contraceptive routine required; device provides five years of contraception 3. Does not contain estrogen 4. Does not interfere with intercourse 5. May reduce the risk of endometrial cancer 6. May be suitable for women who are breastfeeding

Intrauterine Device(IUD) sexualityandu. ca What are the disadvantages? 1. Possible side effects include irregular bleeding or spotting in the first months after insertion 2. Perforation of the uterus may occur at the time of insertion but this is rare 3. May increase menstrual bleeding or menstrual cramping 4. May be expelled from the uterus. This happens in 2– 10% of users 5. Does not protect against STIs

Female Sterilization sexualityandu. ca Tubal occlusion “Having your tubes tied” Sites of Sterilization What is it? • A surgical procedure to close or block the fallopian tubes Techniques include: • Laparoscopy – special instruments are inserted through two tiny incisions (less than 1 cm long) in the abdomen • Mini-laparotomy – also requires a small cut in the abdomen • Hysteroscopy – use of a thin telescope inserted into the uterus Fallopian tubes may be blocked by using one of the following: • A clip or a ring • Cautery (an electric current) • Removing a small piece of each tube • Hysteroscopy for the insertion of tubal plugs (Essure) How does it work? • The fallopian tube is blocked and therefore the sperm and egg cannot meet Failure rate: 5 per 1000 women per year (5%) Essure Ligation Clips Cauterization

Female Sterilization sexualityandu. ca What are the advantages? 1. No daily contraceptive routine required; nothing to remember 2. Private 3. Does not interfere with intercourse 4. No significant long term side effects

Female Sterilization sexualityandu. ca What are the disadvantages? 1. Usually permanent and difficult to have reversed 2. Possible post-sterilization regret 3. Possible short-term surgery-related complications: abdominal discomfort; bruising, bleeding, or infection at the incision site; reaction to anesthesia 4. If pregnancy occurs, there is a higher chance that it will be an ectopic pregnancy 5. Does not protect against STIs
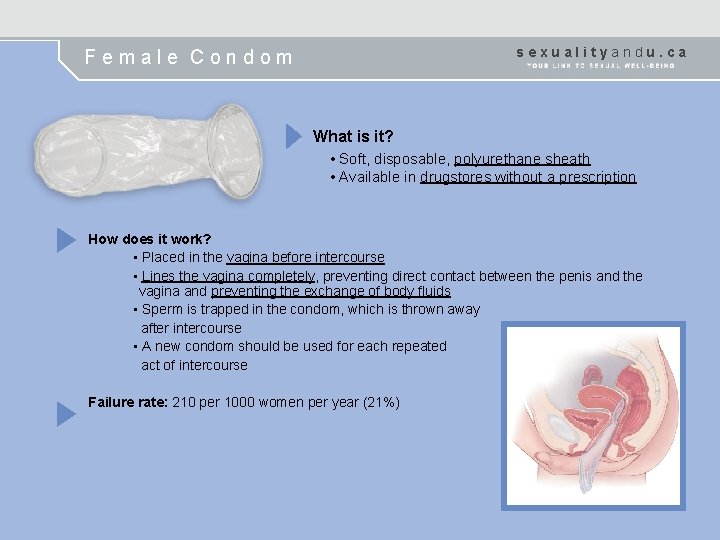
sexualityandu. ca Female Condom What is it? • Soft, disposable, polyurethane sheath • Available in drugstores without a prescription How does it work? • Placed in the vagina before intercourse • Lines the vagina completely, preventing direct contact between the penis and the vagina and preventing the exchange of body fluids • Sperm is trapped in the condom, which is thrown away after intercourse • A new condom should be used for each repeated act of intercourse Failure rate: 210 per 1000 women per year (21%)

Female Condom sexualityandu. ca What are the advantages? 1. Available widely without a prescription 2. No daily contraceptive routine or continued use required 3. Woman remains in charge of placement and use 4. Protects against some STIs
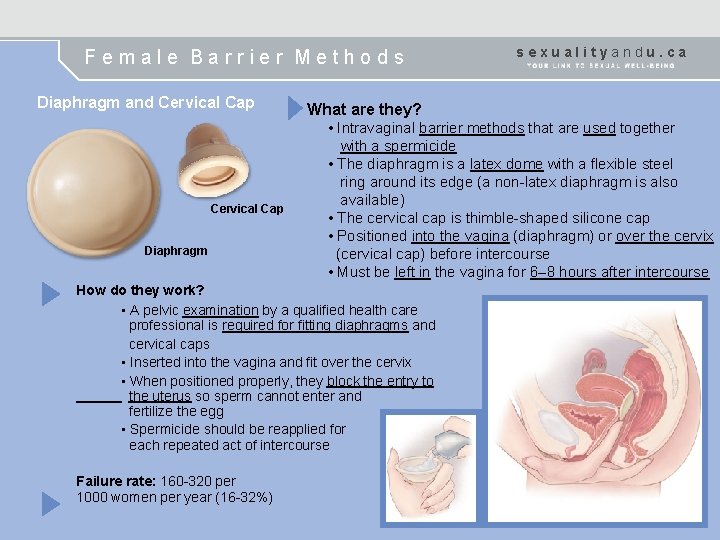
Female Barrier Methods Diaphragm and Cervical Cap Diaphragm What are they? • Intravaginal barrier methods that are used together with a spermicide • The diaphragm is a latex dome with a flexible steel ring around its edge (a non-latex diaphragm is also available) • The cervical cap is thimble-shaped silicone cap • Positioned into the vagina (diaphragm) or over the cervix (cervical cap) before intercourse • Must be left in the vagina for 6– 8 hours after intercourse How do they work? • A pelvic examination by a qualified health care professional is required for fitting diaphragms and cervical caps • Inserted into the vagina and fit over the cervix • When positioned properly, they block the entry to the uterus so sperm cannot enter and fertilize the egg • Spermicide should be reapplied for each repeated act of intercourse Failure rate: 160 -320 per 1000 women per year (16 -32%) sexualityandu. ca

Female Barrier Methods sexualityandu. ca What are the advantages? 1. Does not contain hormones 2. Can be used by women who are breastfeeding 3. Some protection against certain STIs

Female Barrier Methods sexualityandu. ca What are the disadvantages? 1. Must be available at time of intercourse 2. Requires proper insertion technique 3. Does not protect against certain STIs 4. Cannot be used by people who are allergic to spermicides 5. Diaphragm may increase the risk of persistent urinary tract infection 6. Cervical cap should not be used during menstruation 7. May become dislodged during intercourse 8. Cervical cap may cause vaginal odour and discharge

Female Barrier Methods sexualityandu. ca Sponge and Spermicides What are they? • The sponge is a soft, disposable, polyurethane foam device impregnated with a spermicide • Spermicides disable sperm and come in several forms, including creams, jellies, tablets, suppositories, foams, and film How do they work? Sponge • Fits over the cervix • Traps and absorbs sperm to augment effect of spermicide • Spermicide in the sponge disables the sperm • Effective for up to 12 hours Spermicides • Contain an ingredient that disables sperm • Should be used together with another form of contraception Failure rate: 160 -320 per 1000 women per year (16 -32%)

Female Barrier Methods sexualityandu. ca What are the advantages? 1. Does not contain hormones 2. Can be used by women who are breastfeeding 3. Can be used by women who smoke 4. Spermicide may provide added lubrication

Female Barrier Methods sexualityandu. ca What are the disadvantages? 1. Must be available at time of intercourse 2. Does not protect against certain STIs 3. Cannot be used by people who are allergic to spermicides 4. Requires proper insertion technique 5. Sponge users may experience vaginal irritation or infection 6. Spermicide must be inserted into the vagina in advance (time depends on product) 7. If left in the vagina in excess of the recommended time, symptoms of toxic shock syndrome may appear
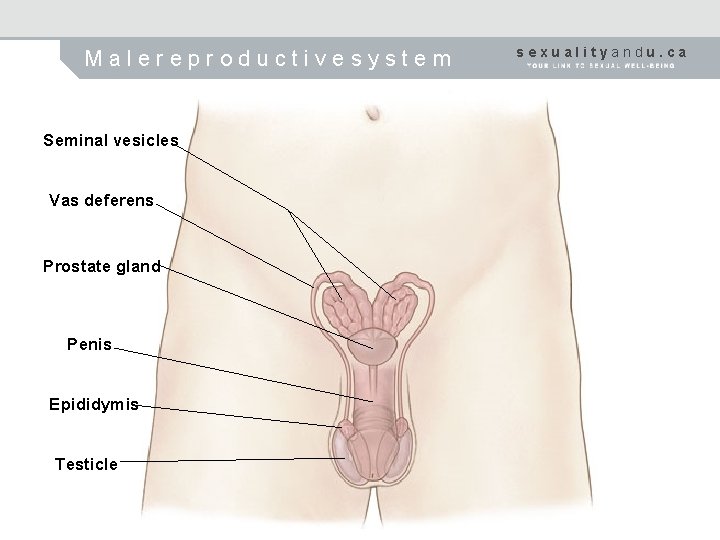
Malereproductivesystem Seminal vesicles Vas deferens Prostate gland Penis Epididymis Testicle sexualityandu. ca
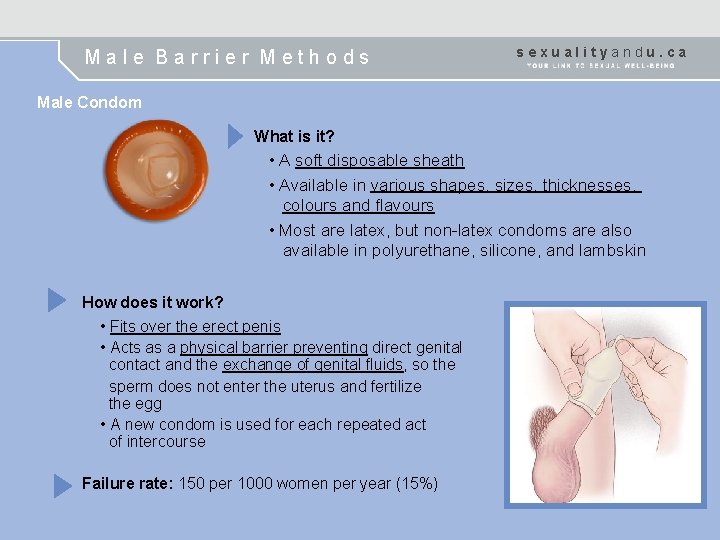
Male Barrier Methods sexualityandu. ca Male Condom What is it? • A soft disposable sheath • Available in various shapes, sizes, thicknesses, colours and flavours • Most are latex, but non-latex condoms are also available in polyurethane, silicone, and lambskin How does it work? • Fits over the erect penis • Acts as a physical barrier preventing direct genital contact and the exchange of genital fluids, so the sperm does not enter the uterus and fertilize the egg • A new condom is used for each repeated act of intercourse Failure rate: 150 per 1000 women per year (15%)

Male Barrier Methods sexualityandu. ca What are the advantages? 1. Available widely without a prescription 2. Inexpensive 3. Latex condoms protect against STIs 4. Allows the male partner to assume some responsibility for birth control 5. Both partners can participate in their use 6. May help the wearer avoid premature ejaculation

Male Barrier Methods sexualityandu. ca What are the disadvantages? 1. Must be available at time of intercourse 2. May slip or break during intercourse 3. Must be stored and handled properly 4. People with latex allergies cannot use latex condoms, but may be able to use non-latex condoms 5. May reduce sensitivity for either partner 6. May interfere with the maintenance of an erection 7. May reduce spontaneity 8. Lambskin condoms do not protect against STIs
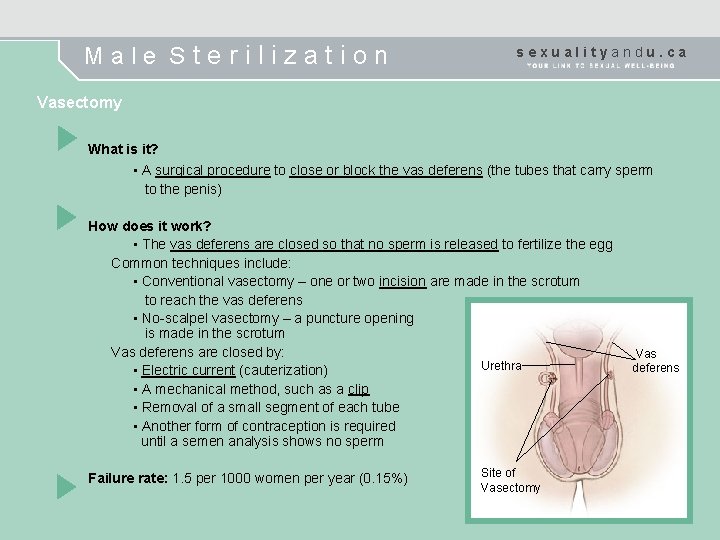
Male Sterilization sexualityandu. ca Vasectomy What is it? • A surgical procedure to close or block the vas deferens (the tubes that carry sperm to the penis) How does it work? • The vas deferens are closed so that no sperm is released to fertilize the egg Common techniques include: • Conventional vasectomy – one or two incision are made in the scrotum to reach the vas deferens • No-scalpel vasectomy – a puncture opening is made in the scrotum Vas deferens are closed by: Urethra • Electric current (cauterization) • A mechanical method, such as a clip • Removal of a small segment of each tube • Another form of contraception is required until a semen analysis shows no sperm Failure rate: 1. 5 per 1000 women per year (0. 15%) Site of Vasectomy Vas deferens

Male Sterilization sexualityandu. ca What are the advantages? 1. No contraceptive routine required; nothing to remember 2. Private 3. Does not interfere with intercourse 4. No significant long-term side effects 5. Simple procedure 6. Less invasive and more cost-effective than tubal ligation for women 7. Allows the male partner to assume some responsibility for birth control

Male Sterilization sexualityandu. ca What are the disadvantages? 1. Difficult to have reversed 2. Possible post-sterilization regret 3. Possible short-term surgery-related complications: pain and swelling; vasovagal reaction; infection at the incision site 4. Does not protect against STIs 5. Not effective immediately. Must do a follow-up sperm analysis that shows no sperm are present in the semen

STI Prevention sexualityandu. ca Dental dams and gloves A dental dam is a small piece of latex similar to the material used for latex condoms. • It can be used during oral sex. The dental dam is stretched across a woman’s vagina to prevent the exchange of bodily fluids. • It can also be used in other activities where a barrier is desired. • Latex surgical gloves can also be used in activities where a barrier is desired. General tips • When using latex dental dams, gloves, or condoms, apply only water- based lubricants. They are available at drugstores. • Use new dental dams, gloves, or condoms for each partner. • Do not re-use latex barriers or turn them over and use the other side.

STI Prevention sexualityandu. ca Cutting a condom to make a dental dam • When a dental dam is not available, a latex condom can be cut to create a latex barrier. 1. Unroll a new condom. 2. Using scissors, cut off both ends of the condom, removing the closed tip and the round loop at the base. 3. Cut the condom lengthwise so that it opens up into a rectangle. • If you are going to use the barrier for oral sex, you may wish to select a condom without spermicide or lubrication. A flavoured condom may be a good choice. 1 2 3
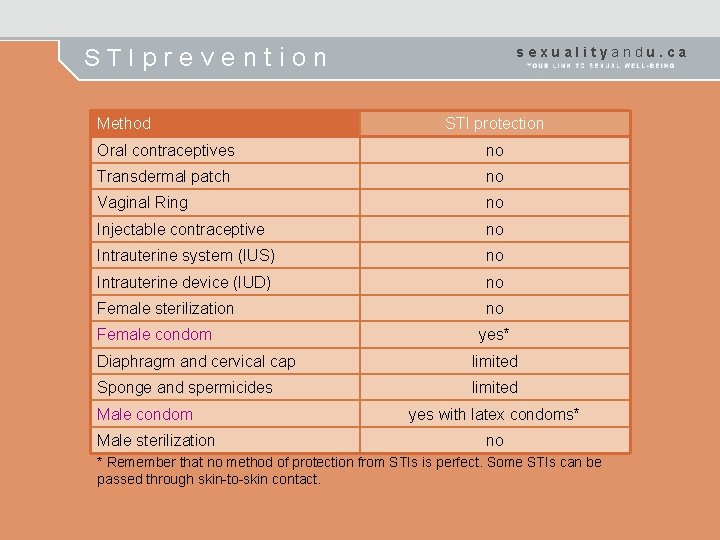
STIprevention Method sexualityandu. ca STI protection Oral contraceptives no Transdermal patch no Vaginal Ring no Injectable contraceptive no Intrauterine system (IUS) no Intrauterine device (IUD) no Female sterilization no Female condom yes* Diaphragm and cervical cap limited Sponge and spermicides limited Male condom Male sterilization yes with latex condoms* no * Remember that no method of protection from STIs is perfect. Some STIs can be passed through skin-to-skin contact.

Birth Control: Myths and Methods + 50 million 1. How many sperm are contained in semen when a man ejaculates? ________ one 2. How many sperm does it take for a female’s egg to become fertilized? _______ Some semen 3. Why is “pulling” or “withdrawal” not considered a method of birth control? ______ is released prior to ejaculation, therefore pregnancy can occur. ____________________________________ 5 4. Sperm can live in the female’s body for up to ______ days. 5. Before using any method of birth control, it is always important to read the directions/instructions ________________. No 6. Does ovulation always occur on the 14 th day of a woman’s menstrual cycle? ____ 7. Douching and feminine deodorants are ____ methods of birth control. not 8. In a relationship, who is responsible for providing the birth control? Explain. Both partners are equally responsible to ensure that pregnancy and STI’s are avoided. _________________________________________________________________________ kill 9. Foams, film, gels and suppositories (spermicides) ____ sperm at the entrance to the cervix _______. spermicide 10. The sponge contains ___________ and is activated with water. It also traps blocks _____ and absorbs the sperm. It also _____ sperm at the cervix.

Birth Control: Myths and Methods continued prevents 11. The male condom __________ sperm from entering the vagina and helps to prevent STI’s. prevents 12. The female condom __________ sperm from entering the vagina and helps to prevent STI’s. egg 13. The pill prevents the _____ from being released from the ovary. It thickens cervical mucous and decreases the lining of the uterus so an egg can’t implant if it was released. No egg=no pregnancy. spermicide 14. The diaphragm is used with _________ which is placed inside the diaphragm and on the rim to block sperm from entering the cervix. spermicide 15. The cervical cap is used with __________ which is placed inside the cap and on the rim to block sperm from entering the cervix. It’s smaller than the diaphragm and uses suction to adhere to the cervix. Pinching the cap with the fingers causes the suction. hormones 16. IUD has two types. The IUS releases __________ and thickens cervical mucous making it hard for the sperm to travel and it changes the uterine lining to prevent the egg copper from implanting. The IUD is _________ wire and it thickens the cervical mucous and changes the uterine lining and prevents the egg from implanting. It is not meant for those less than 25 years of age or those who have never been pregnant. 17. Norplant is 6 hormone implants put into an _______ in the upper arm. These incision hormones prevent the release of an egg. It is good for 5 years. It is no longer available in Canada.

Birth Control: Myths and Methods continued injection every 3 months, which also prevents the 18. Depo-provera is a liquid hormone ______ release of an egg. 19. The rhythm (calendar) method involves the couple planning to have sex at a time when the egg _____ is not in the fallopian tube. vas deferens 20. A vasectomy is when the ____________ are cut and sealed so that sperm are not able to get to the semen and therefore no sperm are in the semen that is released from the male. fallopian tubes 21. A tubal ligation is when the _____________ are cut and sealed so that sperm can’t make it to the egg. abstinence 22. ____________ is the only method of birth control that is guaranteed to be 100% effective.

It’s OK to have sex if you have been drinking or doing drugs? Answer : Maybe… • A person can not consent to sex if that person is high on drugs or alcohol and this could constitute sexual abuse If this happened to you or your friend who would you go to for help?

Basic Facts About AIDS 1. AIDS is fatal. 2. It is not spread by casual contact. 3. It is spread by sex, contaminated blood and needles. 4. It can pass from mother to the unborn child. 5. Reduce your number of sexual partners and remember one partner is safer (monogamy). 6. Latex condoms are your best protection if you become sexually active. 7. Someone can look healthy and still spread infection.

Tips to Reduce RISKS! l l l l l Practice abstinence (no sex) Practice monogamy (one partner) if becoming sexually active Get tested (annually) Comfortable sharing sexual history with partner Using, storing, disposing of latex condoms properly Lubricant is a good choice Use dental dams Don’t use illegal drugs or share needles Don’t share objects that get blood on them such as razors or toothbrushes.
- Slides: 120