MALARIA Malaria A protozoan infection characterized by paroxysms
MALARIA
Malaria • A protozoan infection characterized by paroxysms of chills, fever, and sweating, and by anemia, splenomegaly, and a chronic relapsing course.
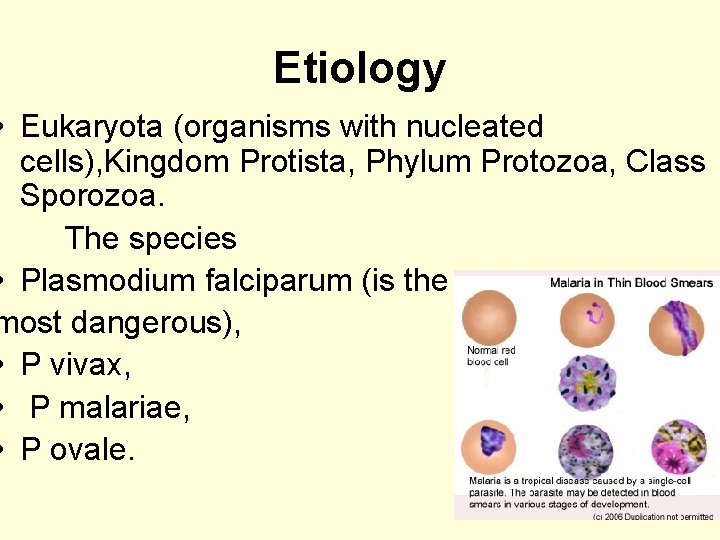
Etiology • Eukaryota (organisms with nucleated cells), Kingdom Protista, Phylum Protozoa, Class Sporozoa. The species • Plasmodium falciparum (is the most dangerous), • P vivax, • P malariae, • P ovale.
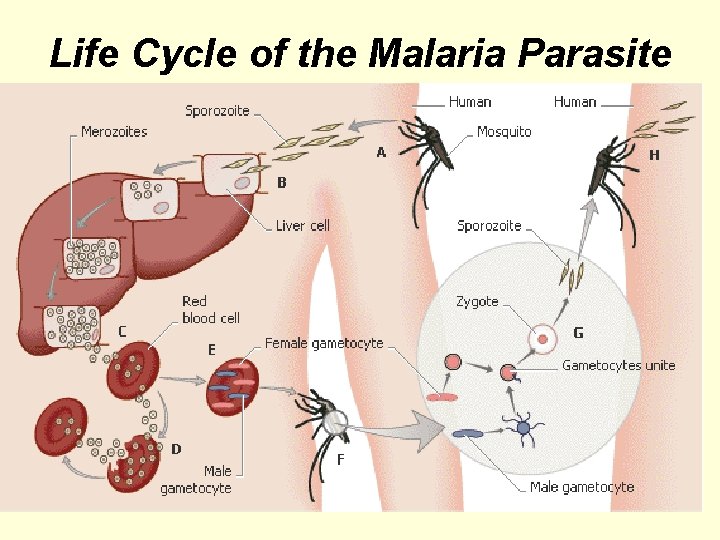
Life Cycle of the Malaria Parasite
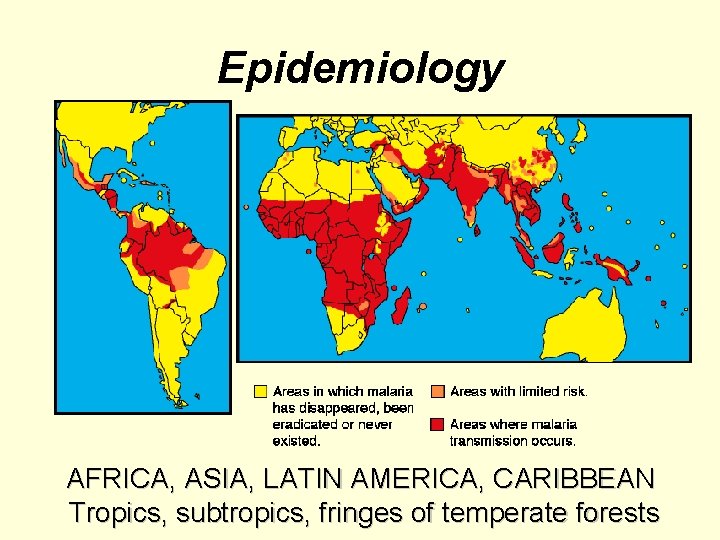
Epidemiology AFRICA, ASIA, LATIN AMERICA, CARIBBEAN Tropics, subtropics, fringes of temperate forests

Transmission • Man is the only important reservoir • Vector is female Anopheles mosquito ® Transmission also possible through: 1. Blood transfusion 2. Contaminated needle 3. Organ transplant 4. Congenital

Pathogenesis • The fever and chills of malaria are associated with the rupture of erythrocyticstage schizonts. • In severe falciparum malaria, parasitized red cells may obstruct capillaries and postcapillary venules, leading to local hypoxia and the release of toxic cellular products. • Obstruction of the microcirculation in the brain (cerebral malaria) and in other vital organs is thought to be responsible for severe complications

The incubation period is usually 10 to 35 days. • Incubation period (the time from the initial malaria infection until symptoms appear) generally ranges from: • 9 to 14 days for P. falciparum • 12 to 18 days for P. vivax and P. ovale • 18 to 40 days for P. malariae

Acute Symptoms • Classical cyclic paroxysm: – Cold stage: chills and shaking – Hot stage: warm, headache, vomiting – Sweating stage: weakness – Feel well for period of time, then cycle repeats itself
• The three stages are often repeated the following day, two days later, or at some later time. In many cases, a person experiences a repetition of the stages again and again during their lifetime. Some people go many years before the symptoms repeat.
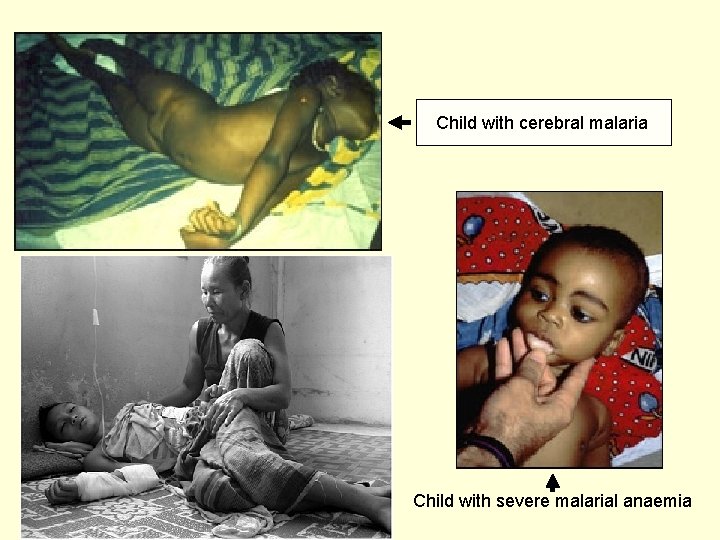
Child with cerebral malaria Child with severe malarial anaemia

Presentation • • Fever Chills Headache Muscle Pain Palpable liver Palpable Spleen Nausea or vomiting Abdominal pain/diarrhea 96% 79% 60% 33% 28% 23% 6%

DIAGNOSIS 1. microscopic examination of the blood Giemsa-stained thick and thin peripheral blood smears 2. CBC (complete blood count) – anemia 3. Polymerase chain reaction
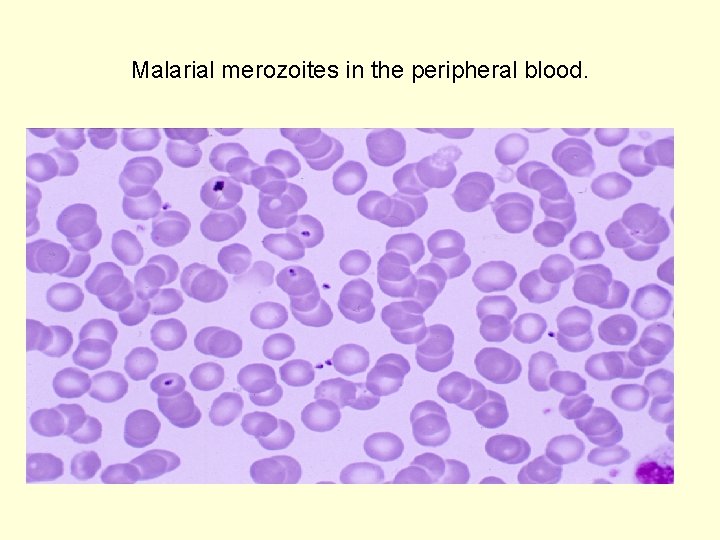
Malarial merozoites in the peripheral blood.

This micrograph illustrates the trophozoite form, or immature-ring form, of the malarial parasite within peripheral erythrocytes.
Treatment • CHLOROQUINE • Quinine and DOXYCYCLINE • MEFLOQUINE • PRIMAQUINE

Points of Attack 1. Attack the parasite in the human host 2. Reduce contact between humans and mosquitoes 3. Decrease mosquito population

Attack The Parasite In The Human Host • Treat malaria infections with effective medications • Use prophylactic drugs to prevent illness and/or infection

Attack The Parasite In The Human Host • Chemoprophylaxis is based on current drug resistance patterns • MEFLOQUINE first line prophylaxis – Mefloquine 250 mg po q week, 1 -2 wks prior to 4 wks after • DOXYCYCLINE as second line drug – Doxy 100 mg po qd, 2 days prior to 4 wks after • PRIMAQUINE – 30 mg* po qd x 14 days terminal prophylaxis *15 mg per FDA and drug product information insert

Reduce Contact Between Humans And Mosquitoes • Personal protective measures – Proper wearing of uniform – PERMETHRIN – Bed nets

Decrease Mosquito Population • • • Surveillance of mosquito populations Identify and eliminate breeding sites Proper insecticide application – Attack larval stages – Attack adult mosquito
- Slides: 21