Makati Medical Center Department of Medicine Medical Grandrounds










































- Slides: 57

Makati Medical Center Department of Medicine Medical Grandrounds July 12, 2007 8: 15 Am, Ledesma Hall MARIZEN L. LIM, MD

Learning Objectives To present a case of SLE with lupus nephrtis To present updates on the treatment of lupus nephritis

Idenifying Data ER 43 -y/0 female Chief Complaint: Persistently elevated BP

History of the Present Illness 20 years PTA malar rash photosensitivity polyarthralgia 3 x spontaneous abortions 1 month PTA severe throbbing headache, vomiting, dizziness, dyspnea on exertion BP: 200/100 consult u/a: +3 alb, 60 rbc, hyaline & coarse granular casts; crea 0. 9

History of the Present Illness Metoprolol 50 mg OD & Felodipine 2. 5 mg OD BP remained uncontrolled Beta blocker calcium channel blocker ACE inhibitor Angiotensin II receptor blocker BP persistently elevated

History of the Present Illness 1 week PTA progressive dyspnea, periorbital, facial, pitting bipedal edema , noted ↓ urine output Consult Leukopenia w/ thrombocytopenia; +3 albumin, 12 wbc, fine granular casts; crea 1. 2 from 0. 9; K 5. 7 Nephrology Admitted

Review of Systems (-) fever (+) headache (+) nausea (+) body malaise (+) anorexia (-) easy bruisability (-) chest pain/palpitation (-) pleurisy (-) abdominal pain (-) dysuria (-) depression/mania

Past Medical, Social and Personal, Family History (-) DM (-) BA (-) allergies Non smoker Non alcoholic beverage drinker Officer worker (+) HPN (-) DM (-) connective tissue disease

Physical Examination General Survey: conscious, coherent, oriented, not in cardiorespiratory distress Vital Signs: BP: 160/100 CR: 68/min, regular RR: 18/min Temp: 36. 2°C HEENT: no alopecia, no head lesions, anicteric sclera, slightly pale palpebral conjunctivae, no abnormal discharges, no oral or nasopharyngeal ulcers, no tonsillopharyngeal wall congestion, no cervical lymphadenopathy, flat neck veins Skin: no pallor, no jaundice, no rashes, (-) petechiae/hematoma

Physical Examination Cardiovascular: adynamic precordium, distinct S 1 and S 2, normal rate, regular rhythm, no murmur Respiratory: symmetrical chest expansion, no intercostals/subcostal retractions, clear breath sounds Abdomen: flabby, normoactive bowel sounds, soft, no tenderness, no organomegaly, no palpable masses Extremities: (+) grade 3 pitting bipedal edema, no cyanosis, full and equal pulses

Salient Features 43 y/o female ↑ BP History of malar rash, photosensitivity, arthralgia, 3 x miscarriages Decreased urine output Pitting bipedal edema Proteinuria, hematuria, casts Increasing creatinine 0. 9 1. 2

Differential Diagnoses ARF Prerenal RPGN Immune Complex GN Postrenal Low C 3 Post infectious GN Normal C 3 Lupus nephritis

Admitting Diagnosis Acute renal failure, probably rapidly progressive glomerulonephritis, probably immune-mediated Hypertension, poorly controlled, probably secondary to a renal pathology Connective tissue disease t/c systemic lupus erythematosus

Course in the Wards On admission CBC: H 11. 6, H 33. 6, wbc 5990 (s 65, L 22, M 11, E 2) K: 6. 6↑ Crea: 1. 7 ↑ U/A: (protein +3, rbc 3. 8, wbc 23. 1, e. c. 20. 3, bact 1784, fine granular casts 5 -10/lpf) Meropenem 500 mg IV q 12 hrs

Course in the Wards Elevated ESR: 74 (n. v. 0 -20) ANA and C 3 beta complement ABG: 100/7. 36/34. 1/18. 8/97. 5/+5. 7/19. 9 Hyperkalemia regimen: (Furosemide 40 mg IV q 8; Kalimate QID; Salbutamol neb q 6; Na. HCO 3 drip) Methylprednisolone (Solumedrol) 1 gm in D 5 W 100 cc slow IV push x 3 days Crea: 1. 7 1. 8 K: 5. 1 6. 6

Course in the Wards 2 nd Hospital day: Hyponatremia: 134 Crea: 1. 3 1. 7 1. 8 BUN: 49↑ 24 -hour urine protein: 864. 5 mg/24 hrs ↑ 24 -hour urine crea: 551. 85 mg/24° estimated crea clearance: 29. 48 ml/min 24 hour urine vol: 650 cc

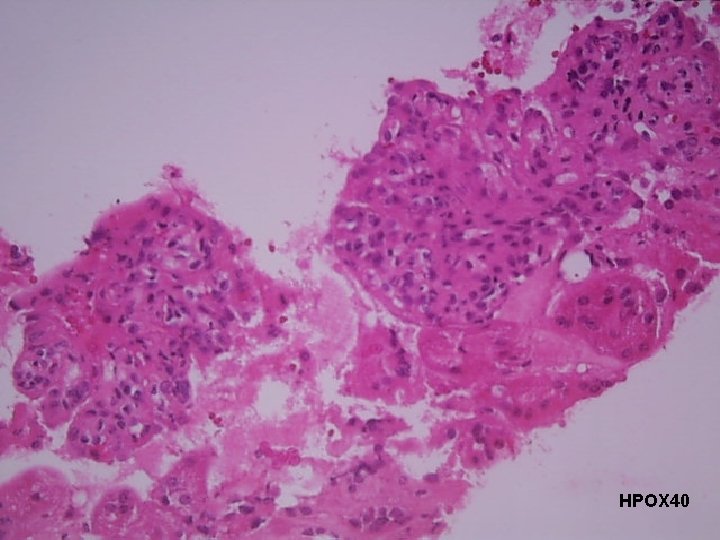
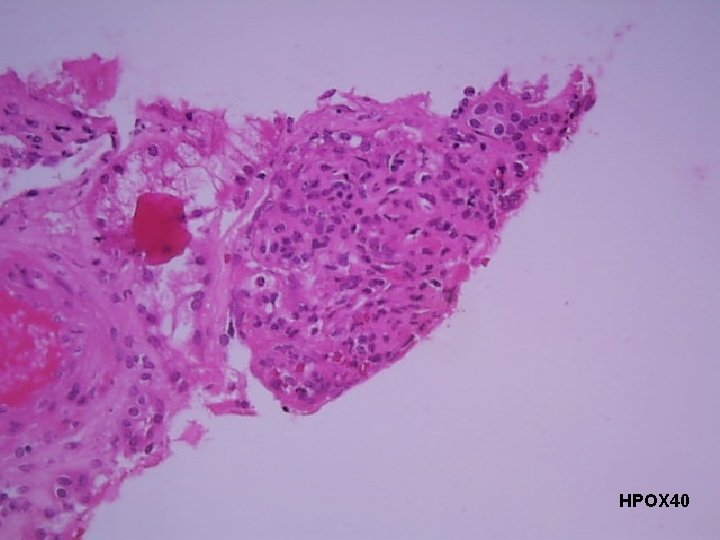
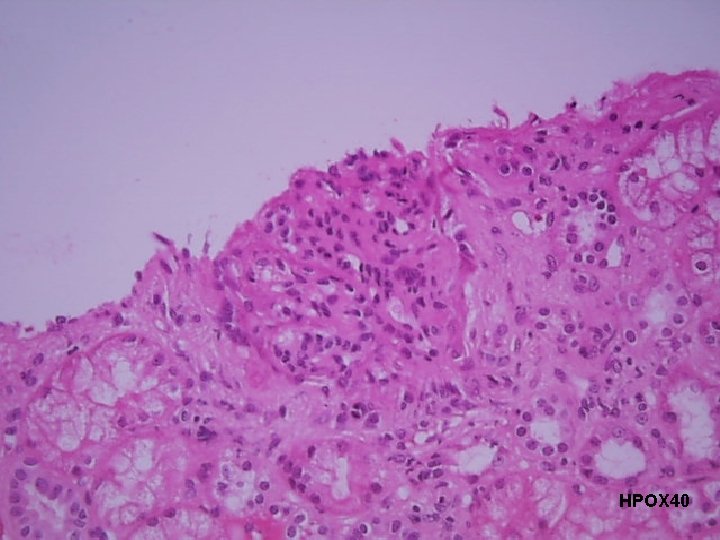
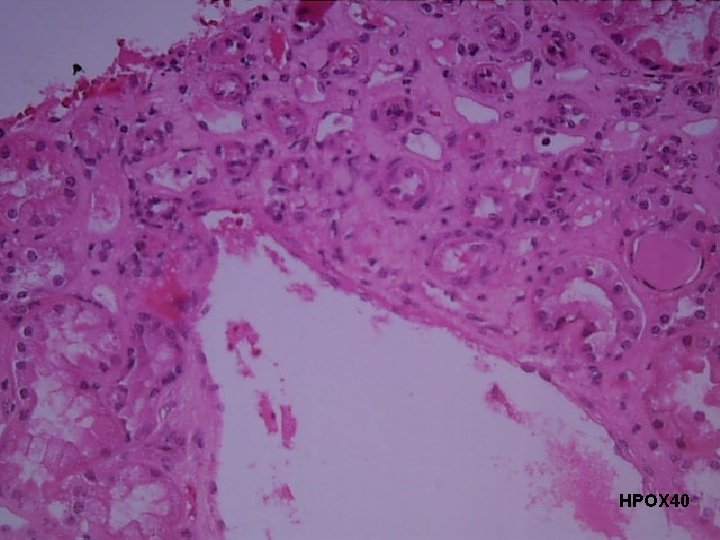
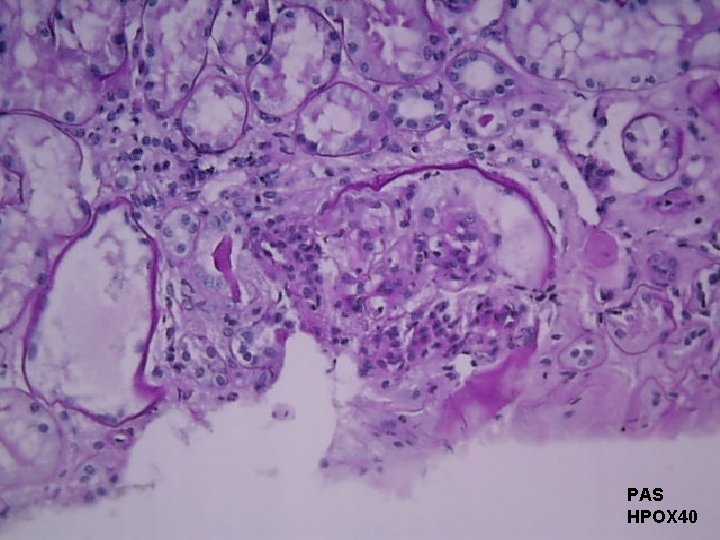
Course in the Wards 3 rd Hospital Day: s/p utz-guided kidney biopsy Result: Lupus Nephritis Class III

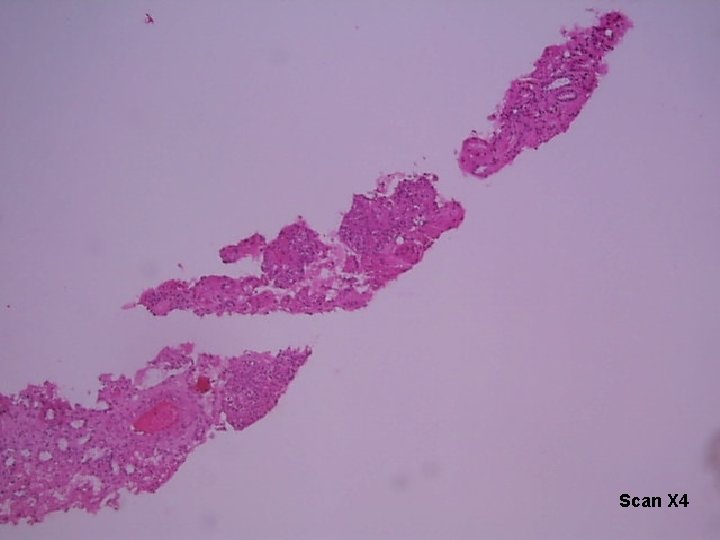
RENAL BIOPSY Specimen consists of a strip of brown tissue measuring 1. 1 cm Block all

Scan X 4

HPOX 40

HPOX 40

HPOX 40

HPOX 40

HPOX 40

PAS HPOX 40

Trichrome Scan X 4

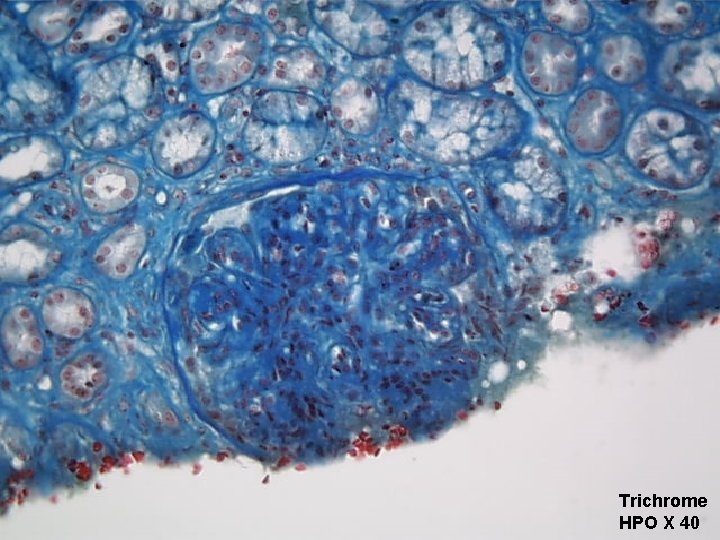
Trichrome HPO X 40

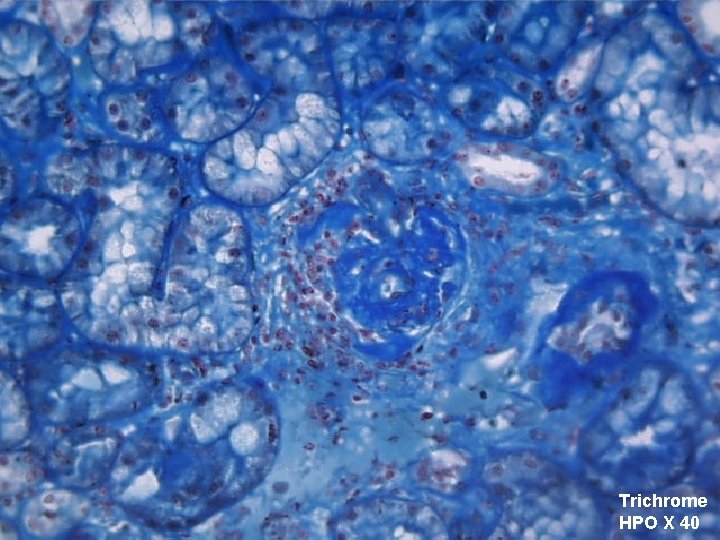
Trichrome HPO X 40

Final Diagnosis RENAL BIOPSY: Clinically diagnosed Systemic Lupus Erythematosus (SLE) with proteinuria Lupus Nephritis Class III

Course in the Wards Anemia Hgb: 9. 7 ↓ Hct: 27. 4 ↓ Kidney UTZ: no hematoma 4 th Hospital day: ANA: positive up to 1: 320 serum dilution; speckled pattern C 3 beta complement: 23. 80 mg% ↓(N. V. 79152)

Course in the Wards Rheumatology Anti-cardiolipin Ab: 11 GPL (N. V. <15) Full Lupus Panel: ANA (+) up to 1: 320 dilution, speckled pattern anti-DNA: (+) anti-SSA(Ro): (+) anti-Sm: (+) anti-SSB(La): (+) anti-RNP: (-) anti-Jo 1: (-)

Course in the Wards Progression of anemia: Hgb: 9. 4 9. 7 Hct: 27. 9 EPO (Renogen) 8000 u IV OD Crea: 2 1. 3

Course in the Wards Prednisone 30 mg PO AM, 20 mg PO PM (on full stomach) Ca. CO 3 500 mg OD Urine CS: E. coli sensitive to Ertapenem & Cefuroxime: Meropenem Cefuroxime 250 mg PO BID Losartan 50 mg PO OD

Course in the Wards 5 th Hospital day: Cyclophosphamide (CYC) IV pulsed therapy CYC 700 mg in D 5 W 500 cc x 2 hours Crea: 1. 4 2 Prednisone

Course in the Wards 6 th Hospital day: Discharged stable and improved THM: 1. EPO (Recormon) 5000 U SC, T-Th-Sat 2. Esomeprazole 40 mg OD 3. Clonidine 75 mcg SL TID 4. Losartan 50 mg OD 5. Cefuroxime 250 mg BID x 7 days 6. Prednisone 5 mg/tab, 30 mg in AM, 20 mg in PM w/ meals 7. Ca. Co 3 500 mg PO OD

Final Diagnoses Systemic lupus erythematosus, lupus nephritis Class III, ARF 2°, s/p kidney biopsy Hypertension stage II, secondary to lupus nephritis Urinary tract infection, on treatment

Discussion

Lupus Nephritis 50% of lupus patients will develop clinically relevant nephritis at some time in the course of their illness 1 Varies from isolated abnormalities of the urinary sediment to full-blown nephritic or nephrotic syndrome or chronic renal failure Formation of immune complexes w/in glomerular capillary wall Diagnosed by renal biopsy 1 http: //www. cerebrel. com/lupus/nephritis. php

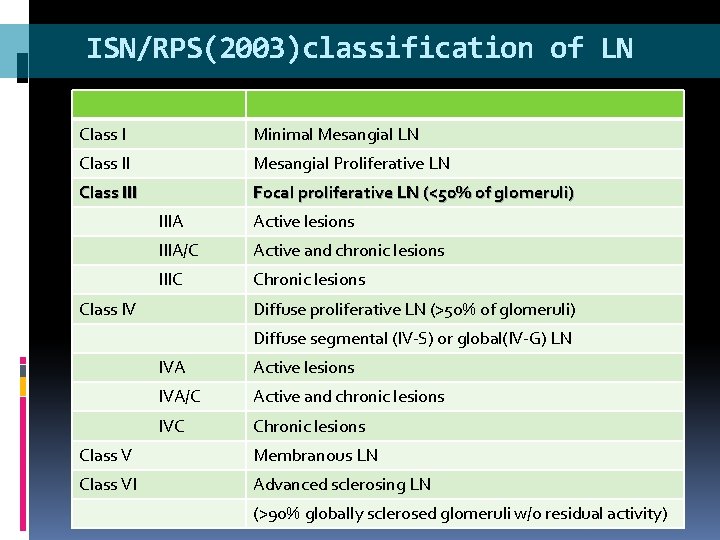
ISN/RPS(2003)classification of LN Class I Minimal Mesangial LN Class II Mesangial Proliferative LN Class III Focal proliferative LN (<50% of glomeruli) IIIA Active lesions IIIA/C Active and chronic lesions IIIC Chronic lesions Class IV Diffuse proliferative LN (>50% of glomeruli) Diffuse segmental (IV-S) or global(IV-G) LN IVA Active lesions IVA/C Active and chronic lesions IVC Chronic lesions Class V Membranous LN Class VI Advanced sclerosing LN (>90% globally sclerosed glomeruli w/o residual activity)

Corticosteroids Mainstay of tx for any inflammatory lifethreatening or organ-threatening manifestations of SLE (proliferative LN) High dose IV glucocorticoid pulses given slowly over a 3 -4 hour period, monthly for 6 months with 0. 5 - 1 mg of oral prednisone per kg between pulses, to control both renal and extrarenal manifestations

Pulse steroids: How much is enough? Giovanni Franchin, and Betty Diamond Columbia University, Department of Medicine, Division of Rheumatology, 1130 St. Nicholas Ave. , Audubon III Room 923, New York, NY 10032, USA Available online 29 August 2005. High dose pulse intravenous steroids with 1 g of methylprednisolone (MEP) given daily, usually for three days, is an accepted practice to treat severe manifestations of systemic lupus erythematosus (SLE) or systemic vasculitides, despite the lack of definitive data.

Adverse Effects of Steroids Weight gain Hirsutism Acne Infection Glucose intolerance Osteopenia/ osteonecrosis Glaucoma PUD

Cytotoxic drugs Used in severe corticosteroid-resistant disease or in the context of unacceptable steroid side effects Cyclophosphamide has been shown to reduce progression of scarring in the kidney & reduce risk for end-stage renal failure

Cyclophosphamide An alkylating agent; Cyclophosphamide given intravenously for prolonged periods is the current gold standard. National Institution of Health Protocol: Cyclophosphamide 1 gm/m 2 every month for 6 months (Induction phase) Cyclophosphamide 1 gm/m 2 every 3 months for 2 years (Maintainance phase)

Adverse effects of Cyclophosphamide Nausea and vomiting Alopecia Ovarian failure or azoospermia Hemorrhagic cystitis, bladder fibrosis, bladder transitional or squamous CA

Monitoring for patients on CTX Regular and frequent lab evaluations to screen for: bone marrow toxicity: CBC monitor renal function: BUN, crea, electrolytes avoid major drug-induced bladder complications: urinalysis

Other treatment options Azathioprine Long-term efficacy of azathioprine treatment for proliferative lupus nephritis H. C. Nossent and W. Koldingsnes Department of Rheumatology, University Hospital Tromsø, Norway Plasmapheresis The Lupus Nephritis Collaborative Study: A randomized, controlled, multicenter clinical trial (John M. Lachin, Sc. D. )

Mycophenolate mofetil A new immunosuppressive drug May be more effective in inducing remission than standard regimen of IV cyclophosphamide Produces fewer complications than Cyclophosphamide like the loss of childbearing ability

Updates

Long-Term Study of Mycophenolate Mofetil as Continuous Induction and Maintenance Treatment for Diffuse Proliferative Lupus Nephritis (Tak. Mao Chan, et al; Feb. 23, 2005) Background: Mycophenolate mofetil (MMF) and the sequential use of cyclophosphamide followed by azathioprine (CTX-AZA) demonstrate similar short-term efficacy in the treatment of diffuse proliferative lupus nephritis (DPLN), but MMF is associated with less drug toxicity Materials and Methods: Thirty-three patients were randomized to receive MMF, and 31 were randomized to the CTX-AZA treatment arm, both in combination with prednisolone.

RESULTS: >90% in each group responded favorably (complete or partial remission) to induction treatment. Serum creatinine in both groups remained stable and comparable over time. Creatinine clearance increased significantly in the MMF group, but the between-group difference was insignificant. Improvements in serology and proteinuria were comparable between the two groups. A total of 6. 3% in the MMF group and 10. 0% of CTX-AZA–treated patients showed doubling of baseline creatinine during follow-up (P = 0. 667).

Both the relapse-free survival and the hazard ratio for relapse were similar between MMFand CTX-AZA–treated patients (11 and nine patients relapsed, respectively) and between those with MMF treatment for 12 or 24 mo. MMF treatment was associated with fewer infections and infections that required hospitalization (P = 0. 013 and 0. 014, respectively). Four patients in the CTX-AZA group but none in the MMF group reached the composite end point of end-stage renal failure or death (P = 0. 062 by survival analysis).

CONCLUSION: MMF and prednisolone constitute an effective continuous inductionmaintenance treatment for DPLN in Chinese patients. MMF-based induction-maintenance regimen has comparable long-term efficacy regarding renal preservation and the prevention of relapse as the sequential CTX-AZA regimen but is associated with significantly reduced unfavorable outcomes, in particular infection and amenorrhea

Prognosis of Lupus Nephritis has dramatically increased over the last several decades (40% at five years in the 1950 s to current survival rates of approx. 90% at 10 years)

Prognosis is Good due to: earlier and better disease recognition with more sensitive diagnostic tests earlier treatment the inclusion of milder cases increasingly judicious therapy and prompt treatment of complications

Prognosis Many patients go into remission and require no treatment. In one study of 667 patients, approx. 25% had remission lasting for at least a year. Remission occurred in 50% of those with disease over 18 years duration, and in 75 % of those with disease over 30 years duration Remission was even seen in some patients who had severe kidney disease http: //patients. uptodate. com/topic. asp? file=arth_rhe/6415

THANK YOU!
 Makati medical center charity program
Makati medical center charity program Iakentro athens
Iakentro athens Bureau of fire protection makati
Bureau of fire protection makati Digmaang moro kahulugan
Digmaang moro kahulugan Meritus medical center family medicine residency
Meritus medical center family medicine residency Greater baltimore medical center medical records
Greater baltimore medical center medical records Torrance memorial hospital medical records
Torrance memorial hospital medical records Cartersville medical center medical records
Cartersville medical center medical records Department of medicine solna
Department of medicine solna Department of medicine mcgill
Department of medicine mcgill Af williams clinic
Af williams clinic Emdec navy
Emdec navy National center for disaster medicine and public health
National center for disaster medicine and public health Center for individualized medicine
Center for individualized medicine A fire department communication center functions
A fire department communication center functions Tracer card medical record
Tracer card medical record Medical education and drugs department
Medical education and drugs department Wyndham+houston+medical+center
Wyndham+houston+medical+center Umass memorial nurse residency program
Umass memorial nurse residency program Kuwait medical association training center
Kuwait medical association training center Jacobi medical center building 1
Jacobi medical center building 1 Queens medical center internship
Queens medical center internship Berkshire medical center program
Berkshire medical center program Durham va pharmacy
Durham va pharmacy Vanderbilt epilepsy monitoring unit
Vanderbilt epilepsy monitoring unit Empp university medical center
Empp university medical center Duke medical library
Duke medical library Ospital ng maynila directory
Ospital ng maynila directory Chinle indian health service
Chinle indian health service Assarts farm medical centre
Assarts farm medical centre Slowenien university medical center
Slowenien university medical center Anchorage va medical center
Anchorage va medical center Ku medical center histology slides
Ku medical center histology slides Outpatient medical center tallulah la
Outpatient medical center tallulah la Columbia university medical center
Columbia university medical center Mercy regional medical center lorain
Mercy regional medical center lorain Suhail medical center philippines
Suhail medical center philippines Columbia university medical center
Columbia university medical center Suny downstate medical center
Suny downstate medical center Suhail allaqaband
Suhail allaqaband Global east asia medical center
Global east asia medical center Arden medical center
Arden medical center Tufts anesthesia residency
Tufts anesthesia residency Islamic medical center kuwait
Islamic medical center kuwait Joint special operations medical training center
Joint special operations medical training center Woodlane medical centre
Woodlane medical centre Unm sandoval regional medical center billing
Unm sandoval regional medical center billing Physicians in north central washington
Physicians in north central washington Doctors license number
Doctors license number Hepburn osteometric board
Hepburn osteometric board Who traditional medicine strategy 2014–23
Who traditional medicine strategy 2014–23 Lt lead time
Lt lead time Babesuniversity
Babesuniversity Nmis nuclear medicine software
Nmis nuclear medicine software Use of polynomials in medicine
Use of polynomials in medicine Unm internal medicine residency
Unm internal medicine residency Typhoid medicine course
Typhoid medicine course Tir in medicine
Tir in medicine