Maine Care Accountable Communities Initiative SIM Payment Reform

Maine. Care Accountable Communities Initiative SIM Payment Reform Subcommittee November 12, 2013 http: //www. maine. gov/dhhs/oms/vbp/accountable. html

Accountable Communities Timeline Sep 2013 Oct 2013 Dec 2013 Winter 2014 Spring 2014 • Public Forums • Release of Request for Applications (RFA) • Eligible Accountable Communities Notified • Contract Negotiations • Implementation 1

Strategy to Achieve the Triple Aim Accountable Communities will achieve the triple aim of better care for individuals, better population health, and lower cost through four overarching strategies: Shared savings based on quality performance Coordination across the continuum of care Practice-level transformation Community-led innovation 2

Maine. Care Accountable Communities • Open to any willing and qualified providers statewide – Participation not required – Qualified providers will be determined through a Request for Application (RFA) process – Accountable Communities will not be limited by geographical area • Members retain choice of providers • Alignment with aspects of other emerging ACOs in the state wherever feasible and appropriate • Maintains fee for service system with the potential for retrospective shared savings payment 3
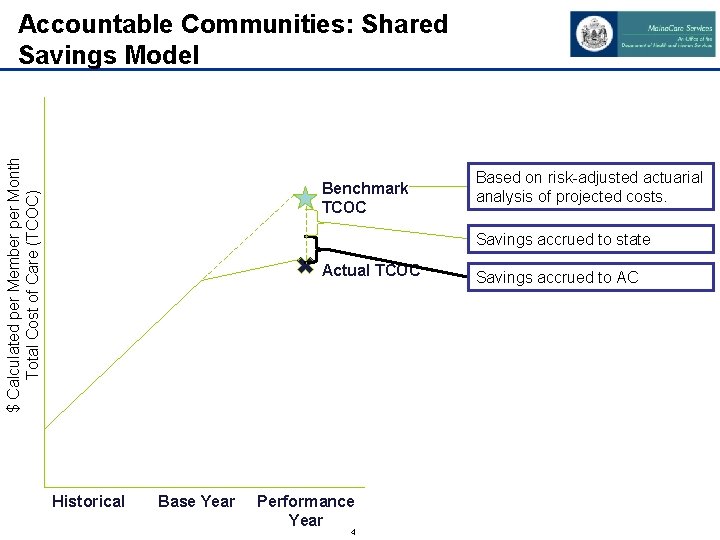
$ Calculated per Member per Month Total Cost of Care (TCOC) Accountable Communities: Shared Savings Model Benchmark TCOC Based on risk-adjusted actuarial analysis of projected costs. Savings accrued to state Actual TCOC Historical Base Year Performance Year 4 Savings accrued to AC

Who Can be an Accountable Community? • One or multiple provider organizations represented by a Lead Entity • Providers must be Maine. Care providers • Include providers that directly deliver primary care services • Have partnerships to leverage DHHS care coordination resources • Demonstrate collaboration with the larger community 5

Lead Entity Requirements Legal Entity will contract with the Department • Receive and distribute any payments • Hold contractual agreements with other providers sharing in savings/ loss under the AC • Ensure the delivery of Primary Care Case Management (PCCM) services (1905(t)(1) of the Social Security Act – Primary Care Providers that “Locate, coordinate and monitor” health care services – 24 hour availability of information, referral and treatment in emergencies 6

Governance • Structure, roles, processes • Transparency • Includes two Maine. Care members 7
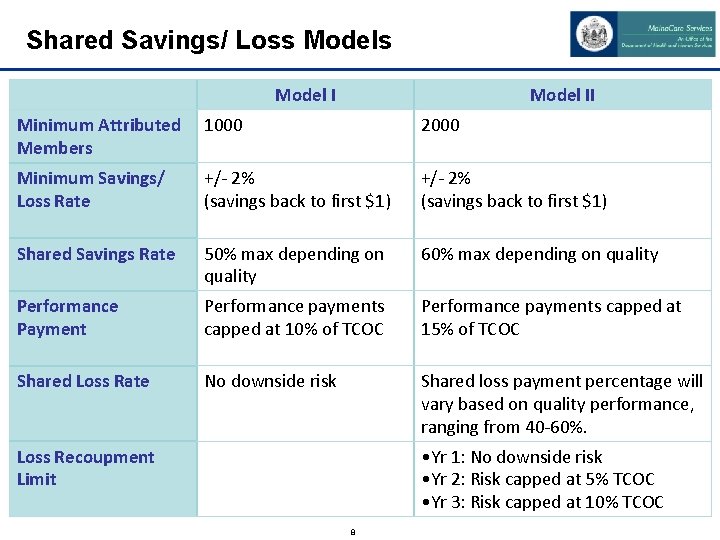
Shared Savings/ Loss Model II Minimum Attributed Members 1000 2000 Minimum Savings/ Loss Rate +/- 2% (savings back to first $1) Shared Savings Rate 50% max depending on quality 60% max depending on quality Performance Payment Performance payments capped at 10% of TCOC Performance payments capped at 15% of TCOC Shared Loss Rate No downside risk Shared loss payment percentage will vary based on quality performance, ranging from 40 -60%. • Yr 1: No downside risk • Yr 2: Risk capped at 5% TCOC • Yr 3: Risk capped at 10% TCOC Loss Recoupment Limit 8
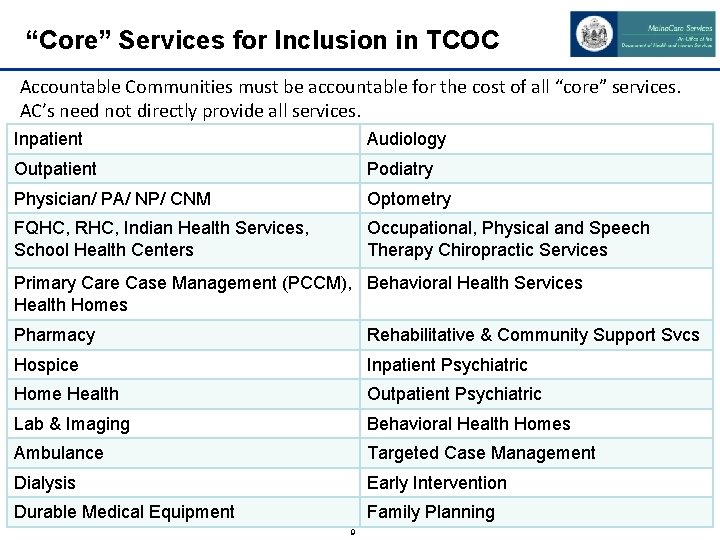
“Core” Services for Inclusion in TCOC Accountable Communities must be accountable for the cost of all “core” services. AC’s need not directly provide all services. Inpatient Audiology Outpatient Podiatry Physician/ PA/ NP/ CNM Optometry FQHC, RHC, Indian Health Services, School Health Centers Occupational, Physical and Speech Therapy Chiropractic Services Primary Care Case Management (PCCM), Behavioral Health Services Health Homes Pharmacy Rehabilitative & Community Support Svcs Hospice Inpatient Psychiatric Home Health Outpatient Psychiatric Lab & Imaging Behavioral Health Homes Ambulance Targeted Case Management Dialysis Early Intervention Durable Medical Equipment Family Planning 9
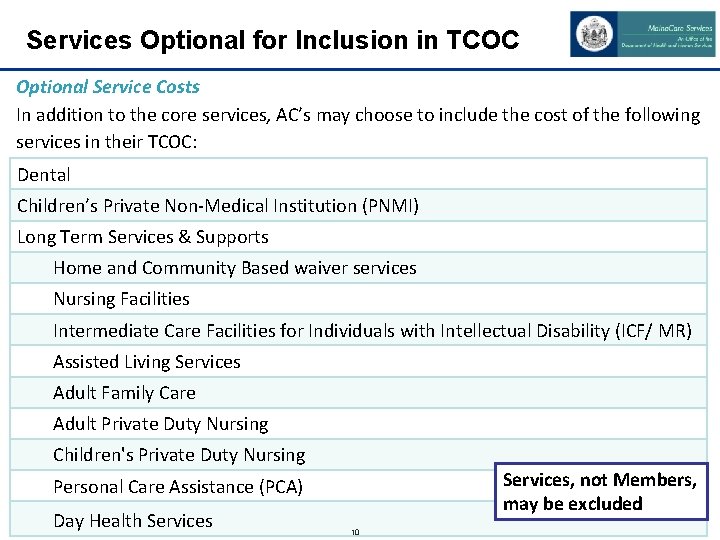

Services Optional for Inclusion in TCOC Optional Service Costs In addition to the core services, AC’s may choose to include the cost of the following services in their TCOC: Dental Children’s Private Non-Medical Institution (PNMI) Long Term Services & Supports Home and Community Based waiver services Nursing Facilities Intermediate Care Facilities for Individuals with Intellectual Disability (ICF/ MR) Assisted Living Services Adult Family Care Adult Private Duty Nursing Children's Private Duty Nursing Services, not Members, may be excluded Personal Care Assistance (PCA) Day Health Services 10
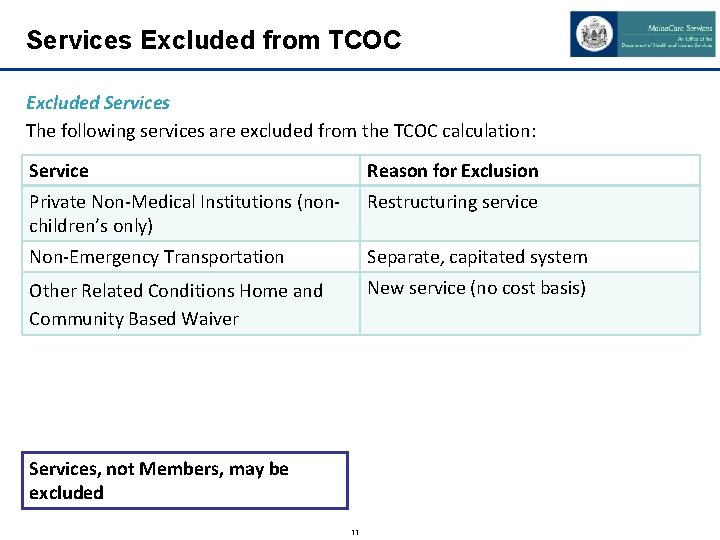
Services Excluded from TCOC Excluded Services The following services are excluded from the TCOC calculation: Service Reason for Exclusion Private Non-Medical Institutions (nonchildren’s only) Restructuring service Non-Emergency Transportation Separate, capitated system Other Related Conditions Home and Community Based Waiver New service (no cost basis) Services, not Members, may be excluded 11

Stepwise Attribution Methodology 1. Member has 6 mo continuous eligibility or 9 mo non-continuous eligibility ? YES 2. NO Member enrolled in a Health Home practice that is part of an AC? NO YES 3. Member has a plurality of primary care visits with a primary care provider that is part of an AC? – Evaluation and Management, preventive, and wellness services, Federally Qualified Health Centers, Rural Health Centers NO YES 4. Member has 3 or more ED visits with a hospital that is part of an AC? YES NO Attributed to AC NOT Attributed to AC 12
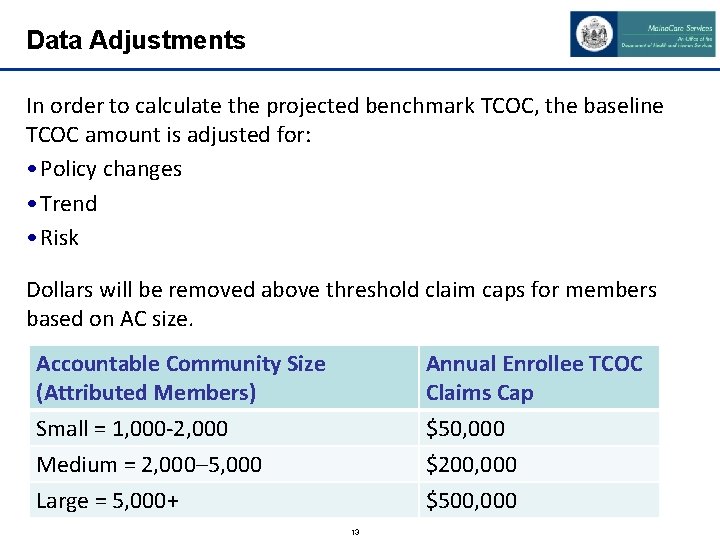
Data Adjustments In order to calculate the projected benchmark TCOC, the baseline TCOC amount is adjusted for: • Policy changes • Trend • Risk Dollars will be removed above threshold claim caps for members based on AC size. Accountable Community Size (Attributed Members) Annual Enrollee TCOC Claims Cap Small = 1, 000 -2, 000 Medium = 2, 000– 5, 000 Large = 5, 000+ $50, 000 $200, 000 $500, 000 13

Data Feedback to Providers Reports to Accountable Community providers will include the following: Utilization report for high risk members (monthly) Attributed member roster (quarterly) Actual TCOC compared to benchmark (quarterly) Claims-based quality performance measures for attributed population (quarterly) Under the State Innovations Model (SIM) grant, Health. Info. Net will be providing real-time notifications of Members’ Emergency Department visits and inpatient admissions to provider care managers. 14

Quality Framework Team • DHHS – Maine. Care – Office of Continuous Quality Improvement – SAMHS • Health. Info. Net • Maine Quality Counts • Maine Health Management Coaltion – Pathways to Excellence (PTE) – Accountable Care Implementation (ACI) • Aligning Forces for Quality • Muskie – Improving Health Outcomes for Children 15

Criteria for Metric Selection 1. Reflective of Medicaid population 2. Alignment with other measures (Health Homes, Medicare ACO, Improving Health Outcomes for Children (IHOC)) 3. Ease of reporting/ pay for performance vs pay for reporting 4. Current performance on measure 16

Quality Domains • Patient Experience (10%) • Care Coordination/ Patient Safety (30%) • Preventive Health (30%) • At Risk Populations (30%) Selection of Measures: All AC’s will be scored on the same set of 15 core measures. In addition, each AC must select 4 elective measures (out of 7 possible). Additional measures will be used for monitoring and evaluation purposes only. 17
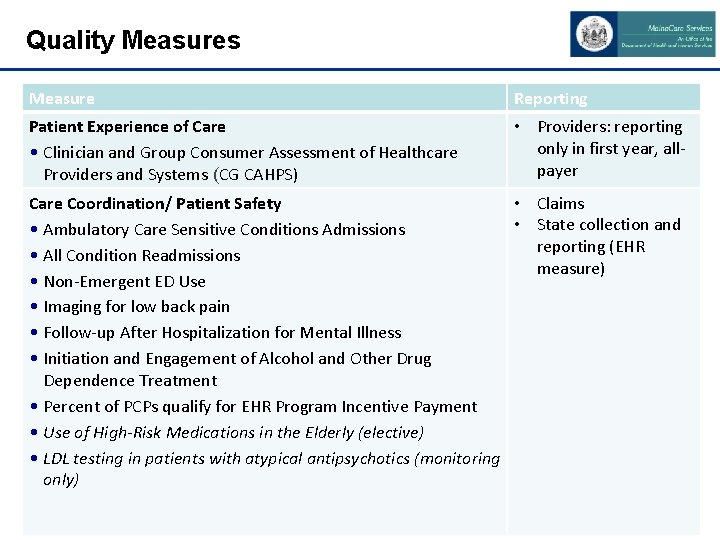

Quality Measures Measure Reporting Patient Experience of Care • Clinician and Group Consumer Assessment of Healthcare Providers and Systems (CG CAHPS) • Providers: reporting only in first year, allpayer Care Coordination/ Patient Safety • Claims • State collection and • Ambulatory Care Sensitive Conditions Admissions reporting (EHR • All Condition Readmissions measure) • Non-Emergent ED Use • Imaging for low back pain • Follow-up After Hospitalization for Mental Illness • Initiation and Engagement of Alcohol and Other Drug Dependence Treatment • Percent of PCPs qualify for EHR Program Incentive Payment • Use of High-Risk Medications in the Elderly (elective) • LDL testing in patients with atypical antipsychotics (monitoring only) 18
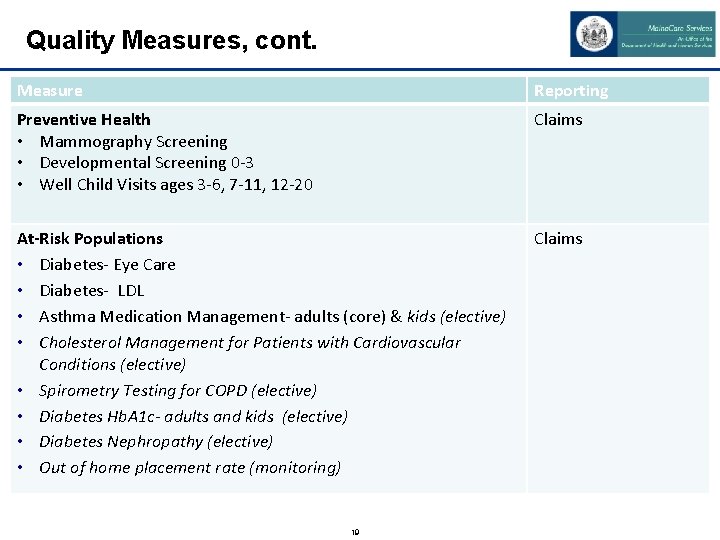
Quality Measures, cont. Measure Reporting Preventive Health • Mammography Screening • Developmental Screening 0 -3 • Well Child Visits ages 3 -6, 7 -11, 12 -20 Claims At-Risk Populations • Diabetes- Eye Care • Diabetes- LDL • Asthma Medication Management- adults (core) & kids (elective) • Cholesterol Management for Patients with Cardiovascular Conditions (elective) • Spirometry Testing for COPD (elective) • Diabetes Hb. A 1 c- adults and kids (elective) • Diabetes Nephropathy (elective) • Out of home placement rate (monitoring) Claims 19
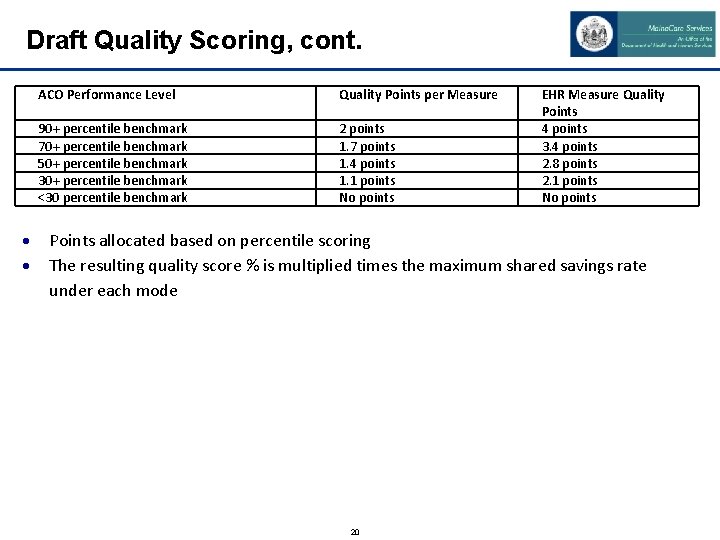
Draft Quality Scoring, cont. ACO Performance Level Quality Points per Measure 90+ percentile benchmark 70+ percentile benchmark 50+ percentile benchmark 30+ percentile benchmark <30 percentile benchmark 2 points 1. 7 points 1. 4 points 1. 1 points No points EHR Measure Quality Points 4 points 3. 4 points 2. 8 points 2. 1 points No points Points allocated based on percentile scoring The resulting quality score % is multiplied times the maximum shared savings rate under each mode 20

Thank you! michelle. probert@maine. gov https: //www. maine. govdhhsomsvbp
- Slides: 22