Mahtab Niroomand M D Assistant Professor of Endocrinology

Mahtab Niroomand M. D. Assistant Professor of Endocrinology SBMU Research Institute of Endocrine Sciences June, 2013 BMD Monitoring

Outline �BMD monitoring in osteoporotic patients �BMD monitoring in non-Osteoporotic patients �Preferred Site for Monitoring �Guidelines

Introduction �DXA- based BMD is the standard tool for diagnosing osteoporosis �BMD measured by DXA is a strong predictor of fragility fractures in both sexes and different ethnicity Arch Intern Med. 2007; 167: 155 -160

BMD monitoring in osteoporotic patients q. Why? q. When ? q How to interpret?
BMD monitoring in osteoporotic patients , Why? q Serial measurements of DXA are performed to: q Main objective : detect patients with significant loss of BMD despite treatment (efficacy of treatment) q Improve adherence to treatment (few data to support that monitoring improves adherence). Journal of Clinical Densitometry, vol. 5, Supplement, S 29–S 38, 2002

BMJ 2009; 338: b 2266

Methods �Objective: To assess the value of monitoring response to bisphonate treatment by means of measuring BMD �Method: analysis data from the FIT study (RCT that compared the effects of alendronate with placebo in 6459 postmenopausal women with low BMD(≤ 0. 68 g/cm 2 at baseline) �BMD was measured at the hip and PA spine on all participants at baseline and at yearly intervals after randomization

Methods �Main outcome: measures Between-person (treatment related) variation and within person (measurement related) variation in hip and spine bone mineral density

Results �The mean effect of three years’ treatment with alendronate was to increase hip BMD by 0. 030 g/cm 2. �There was some between-person variation in the effects of alendronate, but this was small in size compared within-person variation. �Alendronate treatment is estimated to result in increases in hip bone density ≥ 0. 019 g/cm 2 in 97. 5% of patients
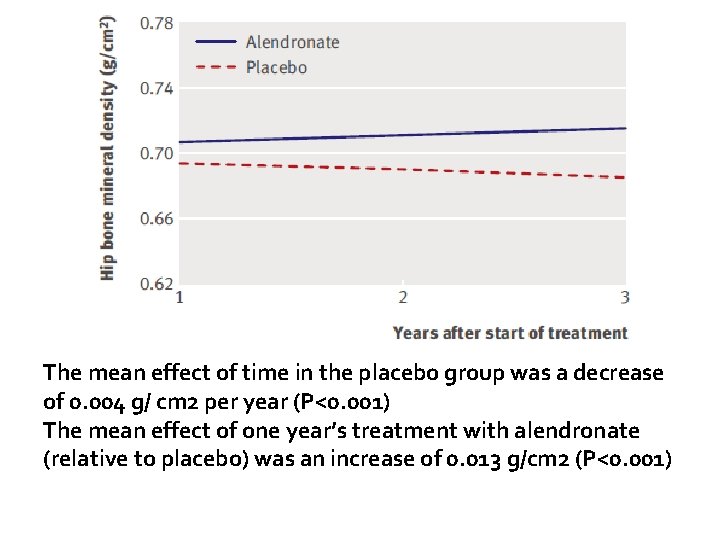
The mean effect of time in the placebo group was a decrease of 0. 004 g/ cm 2 per year (P<0. 001) The mean effect of one year’s treatment with alendronate (relative to placebo) was an increase of 0. 013 g/cm 2 (P<0. 001)


Results �There was considerable variation between patients in the placebo group at one year (P<0. 001) �In addition, there was variation between individuals in how their bone mineral density changed over time (P<0. 001)

Conclusion �Bone density increases sufficient to continue therapy unaltered occurred in virtually all osteoporotic women treated with a potent oral bisphonate for three years. �Monitoring BMD in this early period after starting treatment is unnecessary, and, because of the potential to mislead, it is best avoided.

How to interpret BMD monitoring?

Treatment Failure in Osteoporosis �For anti-resorptive treatment, efficacy is assumed by a significant reduction in fracture risk supported by an increase in BMD and decreases in Bone markers �Question? Whether these treatment are effective in all patients who adhere to treatment regimen? Osteoporosis Int 2012 , 23: 2769 -2774

Treatment Failure (cont’d) �An effective intervention decreases the risk of fracture but dos not eliminate the risk. � Systematic review: comparative effectiveness of treatments to prevent fractures in men and women with low bone density or osteoporosis. Risk reductions: ▪ Vertebral fractures: 30 -70% ▪ Hip fractures: 40 -50% ▪ Non- vertebral fractures: 15 -20% Ann Intern Med 2008, 148: 197 -213

Treatment Failure (cont’d) �In several studies: �Treatment seams to be equally effective irrespective of increment induced in BMD National Institute for Health and Clinical Excellence (NICE, London)2010 �Patients that lose bone under treatment are reported to have a lower fracture risk compared to control patients that lose bone. The fracture Intervention Trial. Osteoprosis Int, 2005 16: 842 -848 MORE investigators. JAMA 1999, 282: 637 -645

Treatment Failure (cont’d) �Committee of Scientific Advisors (CSA) of IOF recommendation: �The response to treatment can be assessed using: Incident Fracture Changes in BMD Changes in Bone turnover markers Osteoporosis Int 2012 , 23: 2769 -2774

1 - Incident Fracture � Sustaining a fracture is always an undesirable outcome, but treatment don’t eliminate fracture risk, they reduce it. � In clinical trial, a second or third fracture during therapy is markedly reduced by 80 -90%in comparison to the placebo group � The natural history of fracture events after index fracture decreases progressively with time �IOF recommendation: The occurrence of a second fragility fracture be used to infer that treatment has failed Osteoporosis Int 2012 , 23: 2769 -2774

2 - BMD �Osteoporosis is characterized by progressive loss of bone and BMD is a predictor of fracture risk �An increase in BMD represent a favorable response to treatment, and decrease in BMD during the treatment is a sign of failure of treatment �The principle problem : rate of bone loss or gain are most often modest compared to the errors incurred in the measurement of BMD Osteoporosis Int 2012 , 23: 2769 -2774

Basic principle �Precision: reflects the reproducibility of a measurement when performed under identical circumstances in the setting of no real biologic change �Precision error: Random error (non-biological) that is inherent in all quantitative medical testing (BMD) Precision error is Important because it allows LSC to be calculated

Basic principle (cont’d) �LSC: The smallest detectable change considered clinically significant due to biologic change � To compare follow- up BMD results with baseline, one must be able to determine whether change over time represents biologic change or instrument noise o LSC depends on: o The precision error of the technique o Confidence needed assume a change Osteoporosis Int 2012 , 23: 2769 -2774

2 - BMD (cont’d) q. In clinical research: q 95% confidence: q LSC=2. 77 x precision error (two-sided test) q LSC=2. 33 x precision error (one-sided test) q. In clinical practice: q 80% confidence: q. LSC=1. 81 x precision error (two sided test) q. LSC=1. 19 x precision error (one-sided test) Osteoporosis Int 2012 , 23: 2769 -2774

2 - BMD (cont’d) �In clinical practice: PE : Lumbar spine : 2% and Hip: 1. 6% � 95% confidence LSC= 4 -5% �IOF Recommendation: Decease in BMD > LSC at 95% confidence is considered as an indicator of failure to respond to treatment Osteoporosis Int 2012 , 23: 2769 -2774

3 - Markers of Bone Turnover �IOF Recommendation: �Decrease in bone markers (CTX and PINP) < LSC at 95% confidence (25%)is considered as an indicator of failure to respond to treatment with antiresorptive agent Osteoporosis Int 2012 , 23: 2769 -2774

Treatment Failure (cont’d) �If these response criteria are not fulfilled within a year of starting treatment: Review of adherence (most likely reason) Search for occult secondary cause of osteoporosis �If these cause are exclude: IOF recommends that treatment be changed Osteoporosis Int 2012 , 23: 2769 -2774

When monitor BMD?

BMD monitoring: When �Monitoring Time interval (MTI): MTI=LSC/ expected rate of change per year �MTI: minimum time during which more than 50% of the patients will show an increase in BMD that exceeds the LSC � MTI is influenced by both: q The LSC q. The magnitude of response to therapy

Official positions of the International Society for Clinical Densitometry and Executive Summary of the 2005 Position Development Conference Journal of clinical densitometry 2006; 9: 4

ISCD-2005 Recommendation q Follow-up BMD testing (DXA spine and hip) when the expected change in BMD equals or exceeds the LSC , which is typically one to two years after initiation or change of therapy, with longer intervals once therapeutic effect is established. J Clin Densitom 2006; 9: 4

ISCD-2005 Recommendation q In conditions associated with rapid bone loss, such as glucocorticoid therapy, testing more frequently is appropriate q Intervals between BMD testing should be determined according to each patient clinical status J Clin Densitom 2006; 9: 4

BMD monitoring in non osteoporotic patients

BMD monitoring in non osteoporotic patients q why? Monitoring is acceptable for determining when therapy is indicated q When?

When? �Although BMD testing to screen for osteoporosis is recommended for women 65 years of age or older, there are few data to guide decisions about the interval between BMD tests


Method q objective: q Whether repeat BMD measurement adds benefit beyond the initial BMD measurement in predicting fractures in older women? q Design: q A prospective cohort study q. Subjects: q 4124 women aged 65 or older from 4 US regions

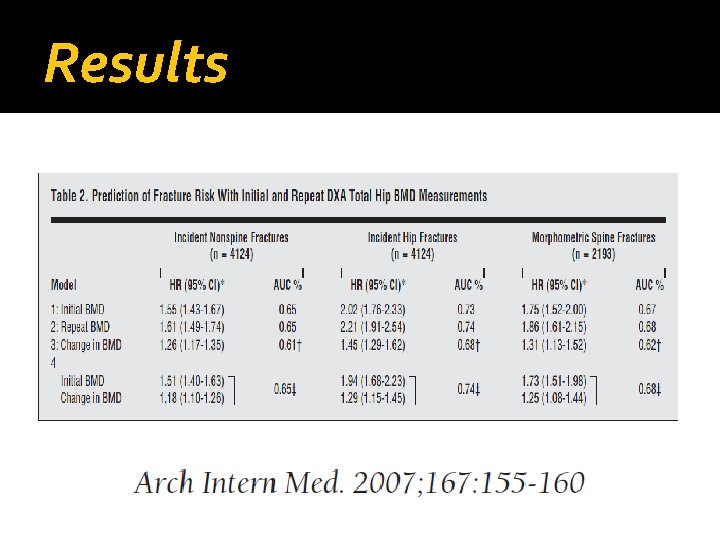
Results

Conclusions �Although change in BMD was an independent predictor of all fracture types, it was a weaker predictor than either initial or F/U BMD measure alone � In healthy, older, postmenopausal women who has not yet developed a fracture, repeating a measurement of BMD up to 8 years later provides little additional value besides the initial BMD measurement for predicting incident fractures


�Objective: For an individual (man or woman) without osteoporosis, given their present BMD level, what is the risk of developing osteoporosis and/or fracture, and when is the optimal time to repeat their BMD measurement? �Design: Part of the ongoing longitudinal Dubbo Osteoporosis Epidemiology study in Australia

Methods q. Subjects: q 1008 women and 750 men over the age of 60 (visit q 2 years to have BMD remeasured) q Primary endpoint: q The time to reach osteoporosis or an incident (low-trauma) fragility fracture Focus on femoral neck BMD q. Average follow-up period: q 7 years (maximum of 15 years)
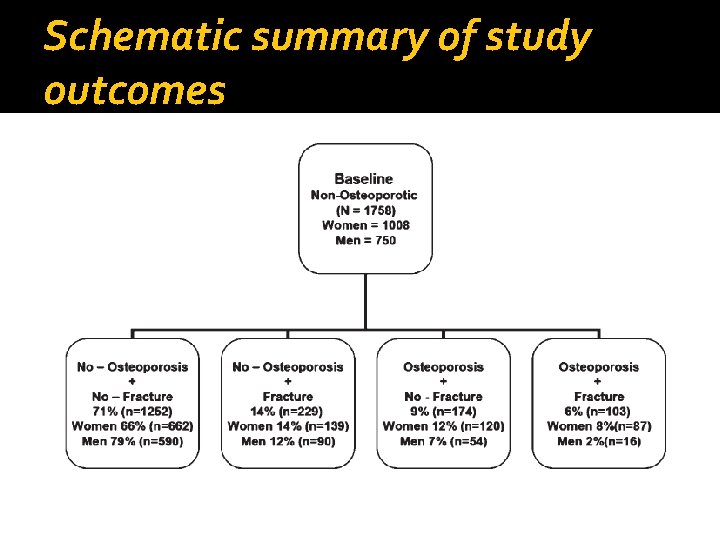
Schematic summary of study outcomes
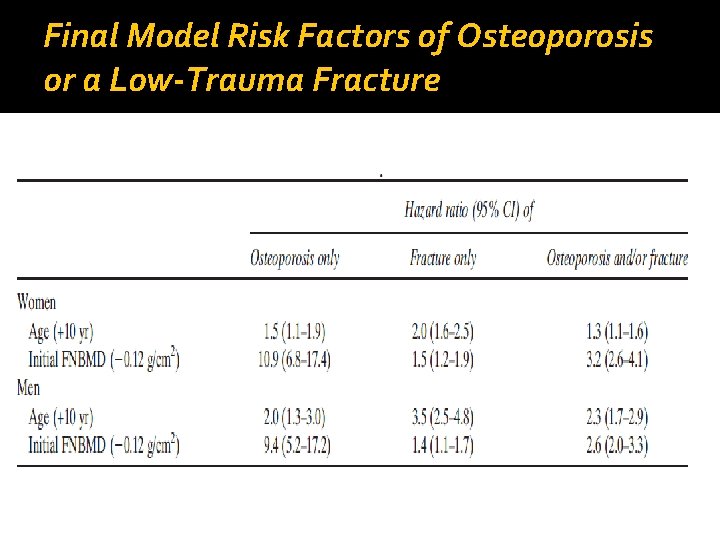
Final Model Risk Factors of Osteoporosis or a Low-Trauma Fracture

Conclusion Based on an individual current age and BMD Tscore at the femoral neck, it is possible to estimate the optimal time to repeat BMD testing for the individual q Some potential limitations: q q The model did not include comorbidities… q There is a large variation in background risk of fracture among populations

N Engl J Med 2012; 366: 225 -33

Methods q Longitudinal follow-up SOF study q Primary outcomes: The estimated intervals for 10% of participants to make the transition from normal BMD or osteopenia at baseline to osteoporosis before a hip or clinical vertebral fracture occurrence and before initiation of OP treatment

Methods q Study participants: 4957 women aged 67 or older with normal or osteopenic BMD (due to lowest T-score at femoral neck or total hip) and with no history of fracture or of treatment for OP q Follow-up duration: 15 years

Methods �The participants were stratified into four groups (according to lowest T score at femoral neck or total hip): Normal BMD : T score≥− 1. 00 Mild osteopenia : -1. 01 ≤ T score≤− 1. 49 Moderate osteopenia : − 1. 50 ≤ T-score≤− 1. 99 Advanced osteopenia : − 2. 00 ≤ T-score≤− 2. 49
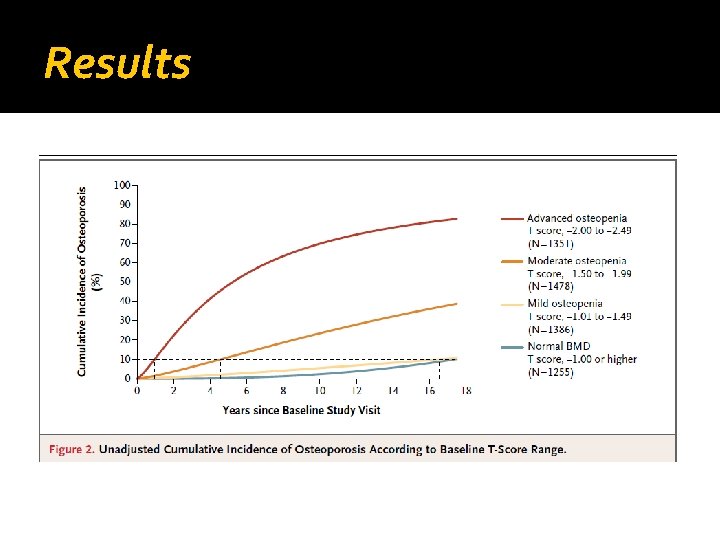
Results

Results q For women with osteopenia at baseline, T-score group, age, BMI, current estrogen use and the interaction of T-score group by BMI were significant predictors in the final model (P<0. 02) q During the 15 -year study period, less than 1% of women with normal BMD and 5% of women with mild osteopenia made the transition to OP

Results q The adjusted estimated time for 2% of women to have a hip or clinical vertebral fracture was: Ø more than 15 years for women with normal BMD or mild osteopenia Ø 5 years for those with moderate or advanced osteopenia. q Within a given T-score range, the estimated time for the transition from osteopenia to OP was longer with younger age.
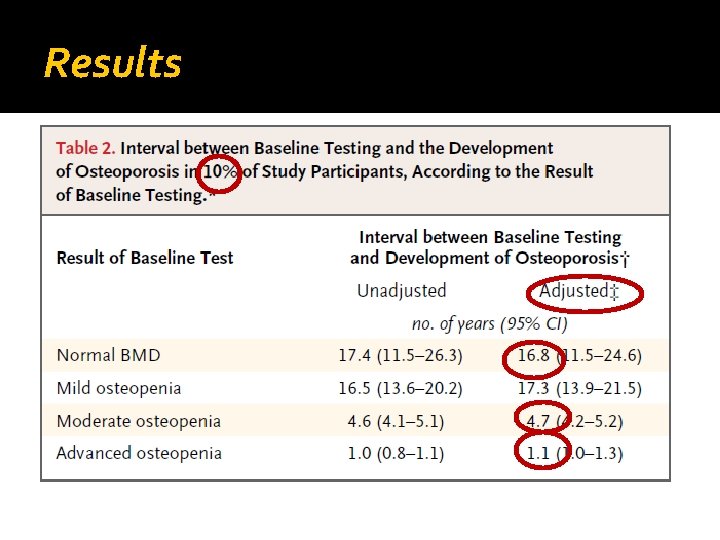
Results




Limitation of NEJM Repots �The study cohort was restricted to preselected women 67 years of age and did not include men or younger postmenopausal women �Only clinical vertebral fractures were considered in the analysis, although undiagnosed morphometric vertebral fractures are common in patients with densitometric evidence of osteopenia and are associated with high morbidity

Limitation of NEJM Repots �With its singular focus on BMD, the study did not capture those patients with osteopenia who by FRAX fracture risk assessment would have been at high risk for fracture and therefore warrant drug therapy.

Limitation of NEJM Repots �Lumbar spine T-score may be ≤-2. 5 even if the femoral neck or total hip T-score >-2. 5. Without tracking lumbar spine BMD, Gourlay and colleagues may have underestimated the number of individuals who progressed to osteoporosis during the study �In reality, overtesting with DXA is not a problem. The real problem is that far too few patients are being screened for osteoporosis

Limitation of NEJM Repots �Recent Medicare claims analysis during the 7 - year (2002 to 2008) demonstrated that: 48% of elderly women had not had a single DXA study 25% had one test 15% had two tests 8% had three tests 2% had four tests <1% had five or more tests.

Limitation of NEJM Repots �Despite the availability of DXA to diagnose osteoporosis and the use of FRAX to assess fracture risk, osteoporosis remains a disease that is under-diagnosed. � Although FDA-approved therapies that are proven to reduce fracture risk are widely available, the disease is still, in 2012, undertreated.

Preferred Site for Monitoring

Preferred Site for Monitoring �PA spine: preferred site for monitoring patients using DXA, because: q It has the best precision q Shows the greatest increases in BMD in treated patients q Show the greatest decreases in BMD in untreated patients � Total hip region : When PA spine BMD is not measureable because: q Total hip has both better precision q More therapy-responsive trabecular bone than the femoral neck.

Guideline Recommendation

AACE-2010 q. For patients receiving treatment or approaching an intervention threshold, retesting every 1 to 2 years is often appropriate q. For those who have borderline low results of BMD, retesting every 3 to 5 years is usually sufficient q. Patients who are comfortably above an intervention threshold may not need to undergo reassessment for 5 to 10 years or ever, unless there is some new indication Endocrine Practice Vol 16 (suppl 3)2010

NAMS 2010 In most cases, repeat DXA testing in untreated postmenopausal women is not useful until 2 to 5 years have passed q For women receiving OP therapy, BMD monitoring may not provide clinically useful information until after 1 to 2 years of treatment q Menopause : The Journal of The North American Menopause Society. Vol. 17, No. 1, pp. 25 -54

NOF -2010 �NOF recommends that repeat BMD assessments generally agree with Medicare guidelines of every 2 years, but recognizes that testing more frequently may be warranted in certain clinical situations

USPSTF 2011 Evidence is lacking about optimal intervals for repeated screening q A minimum of 2 years may be needed to reliably measure a change in BMD; however longer intervals may be necessary to improve fracture risk prediction q US. preventive services task force, Ann Intern Med. 2011; 154: 356 -364

Thanks for your attention
- Slides: 69