Macrominerals Phosphorus Dr Sherin Bakhashab Phosphorus Sources 1

Macrominerals Phosphorus Dr. Sherin Bakhashab

Phosphorus Sources: 1. Milk and milk products (the richest sources) 2. Fish, meat, liver and kidney 3. Leafy vegetables and egg yolk Requirements: 1. Adult men and women: 800 mg/ day 2. Children, pregnant and lactating women: 800 – 1200 mg/day Excretion: Mostly 90% is excreted in urine.
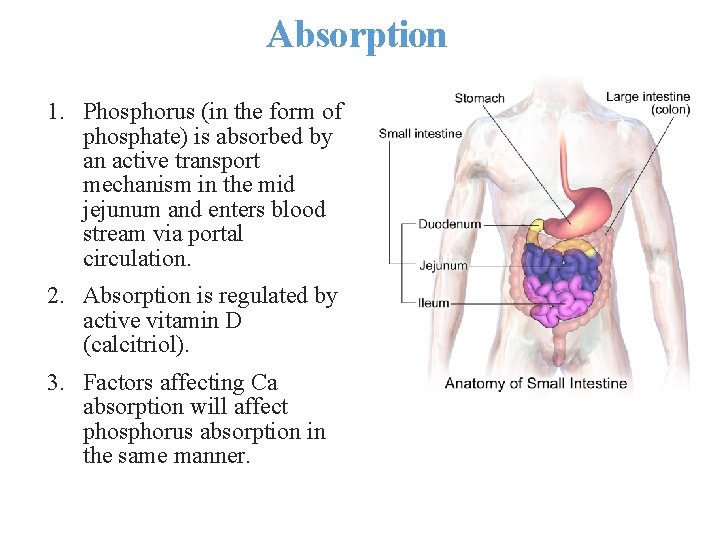
Absorption 1. Phosphorus (in the form of phosphate) is absorbed by an active transport mechanism in the mid jejunum and enters blood stream via portal circulation. 2. Absorption is regulated by active vitamin D (calcitriol). 3. Factors affecting Ca absorption will affect phosphorus absorption in the same manner.

Body Phosphorus 1. Total body phosphorus is about 800 g. 2. Most of the phosphorus (80%) is present in the skeleton (bones and teeth). 3. The other 20% is present in other tissues (mostly intracellular) and body fluids.

Blood Phosphorus 1. Normal plasma inorganic phosphorus between 3 -5 mg/dl. 2. Other forms are present: a) In plasma: phospholipids b) In red blood cells (RBCs): organic phosphate, e. g. ATP, glucose-6 -phosphate.

Factors Affecting Blood Phosphorus § Parathyroid hormone: Decreases phosphorus by stimulating its excretion through inhibiting the renal tubular reabsorption of phosphate. § Active vitamin D (calcitriol) a) Hypophosphataemia stimulates directly the renal hydroxylation of 25(OH)D 3. b) Calcitriol increases blood phosphorus through stimulation of: 1. 2. 3. Absorption of phosphorus from the intestine. Bone resorption, i. e. , mobilization of phosphorus from bones. Renal reabsorption by renal tubules.
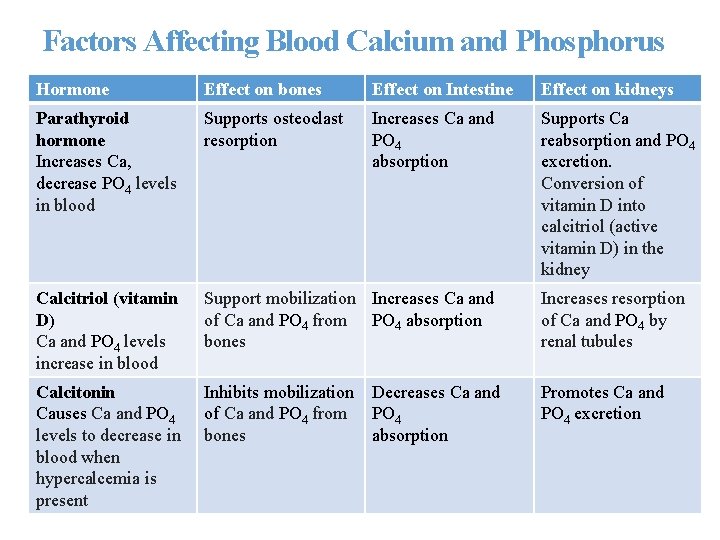
Factors Affecting Blood Calcium and Phosphorus Hormone Effect on bones Effect on Intestine Effect on kidneys Parathyroid hormone Increases Ca, decrease PO 4 levels in blood Supports osteoclast resorption Increases Ca and PO 4 absorption Supports Ca reabsorption and PO 4 excretion. Conversion of vitamin D into calcitriol (active vitamin D) in the kidney Calcitriol (vitamin D) Ca and PO 4 levels increase in blood Support mobilization Increases Ca and of Ca and PO 4 from PO 4 absorption bones Increases resorption of Ca and PO 4 by renal tubules Calcitonin Causes Ca and PO 4 levels to decrease in blood when hypercalcemia is present Inhibits mobilization of Ca and PO 4 from bones Promotes Ca and PO 4 excretion Decreases Ca and PO 4 absorption

Functions of Phosphorus Ø It comprises the structure of bones and teeth. Ø It enters in the structure of the following cellular components: a) b) c) d) e) Nucleic acids: DNA, RNAs. Phospholipids: e. g. lecithin, cephalin. Phosphoproteins Coenzymes: e. g. NAD, NADP. High energy phosphate compounds: e. g. ATP, GTP, creatine phosphate. f) Cyclic AMP, GMP g) Carbohydrate intermediates: e. g. glucose-6 -phosphate, fructose-1 -phosphate.

Functions of Phosphorus Ø It enters in the formation of blood buffers. Phosphate buffer system: dihydrogen phosphate (H 2 PO 4 -) and monohydrogen phosphate (HPO 42 -) are the ions used in this system. H 2 PO 4 - acts as a weak acid:
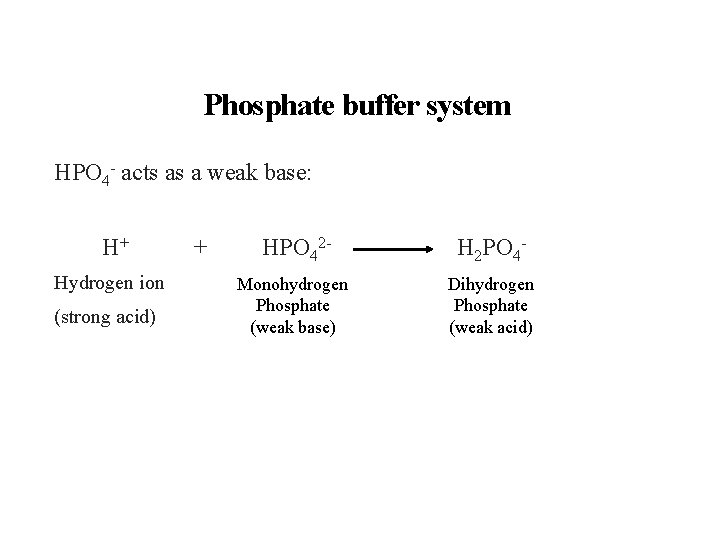
Phosphate buffer system HPO 4 - acts as a weak base: H+ Hydrogen ion (strong acid) + HPO 42 - H 2 PO 4 - Monohydrogen Phosphate (weak base) Dihydrogen Phosphate (weak acid)
- Slides: 10