MACRA The Big Picture Legislative Hot Topics MARCH


MACRA: The Big Picture & Legislative Hot Topics MARCH 15, 2017

Overview
HHS VISION FFS Payments for Quality & Value Better Care Smarter Spending Healthier People
TRENDS MSSP Meaningful Use Medicare e. RX PQRI/PQRS Value-Based Payment Modifier Pioneer ACOs Bundled Payments
QUALITY PAYMENT PROGRAM MACRA QPP MIPS Advanced APMs
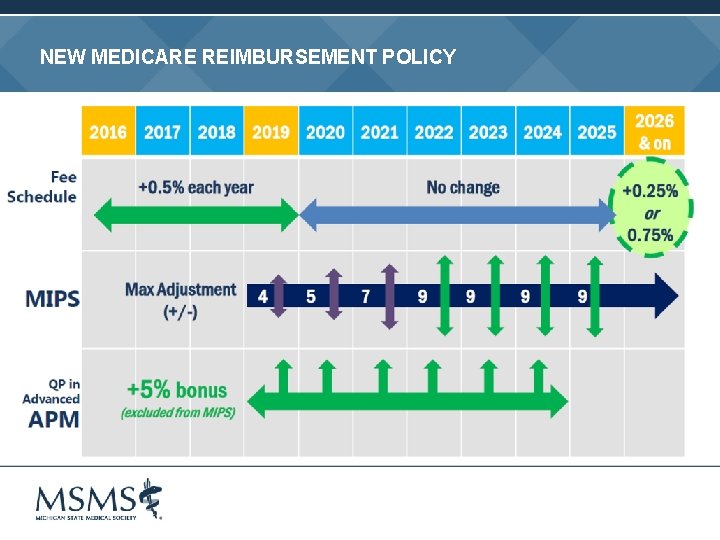
NEW MEDICARE REIMBURSEMENT POLICY

ELIGIBILITY Eligible Clinicians (ECs) • • • Physicians, Physician Assistants, Nurse Practitioners, Clinical Nurse Specialists, Certified Registered Nurse Anesthetists (in 2019 and 2020; list to be expanded in 2021) Participate as an individual or group In MIPS unless… o o o 1 st year in Medicare billing charges ≤ $30, 000 OR provide care to 100 or fewer Medicare patients in one year Certain participants in APMs

IMPLEMENTATION QPP Implementation Dates • • Payment adjustment year = 2019 Performance year = 2017 o o o “Pick Your Pace” options for 2017 only Start no later than October 2, 2017 Report performance data by March 31, 2018
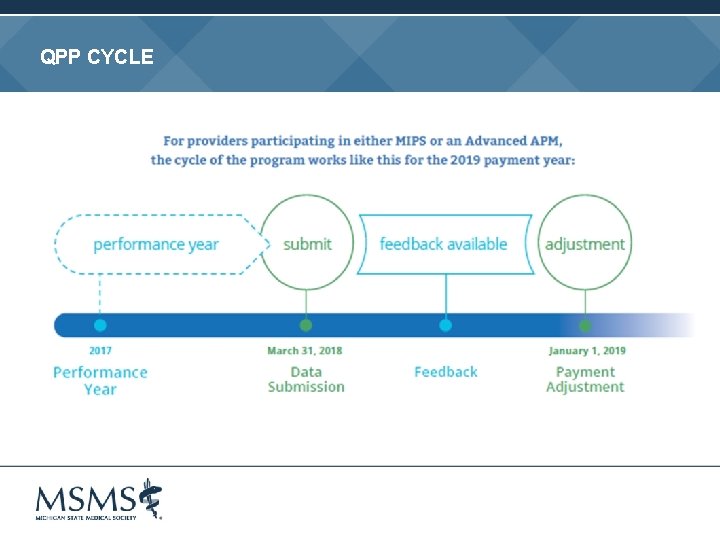
QPP CYCLE
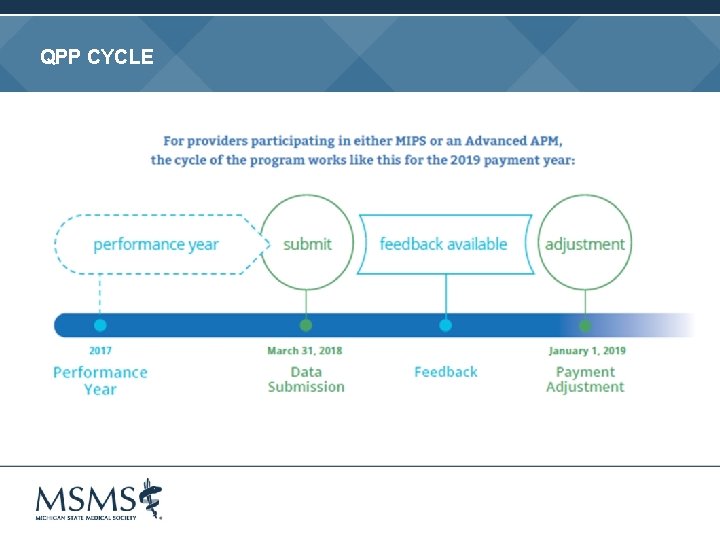
QPP CYCLE

“PICK YOUR PACE” Don’t participate = -4% payment adjustment Report at least one quality measure or improvement activity, or the advancing care information base component = no payment adjustment +/ - Submit at least 90 consecutive days of data = neutral or small positive payment adjustment Submit full year of data to Medicare = opportunity to earn maximum positive payment adjustment If you receive 25% of Medicare payments or see 20% of your Medicare patients through an Advanced APM in 2017, then you earn a 5% incentive payment in 2019

Merit-Based Incentive Program (MIPS)
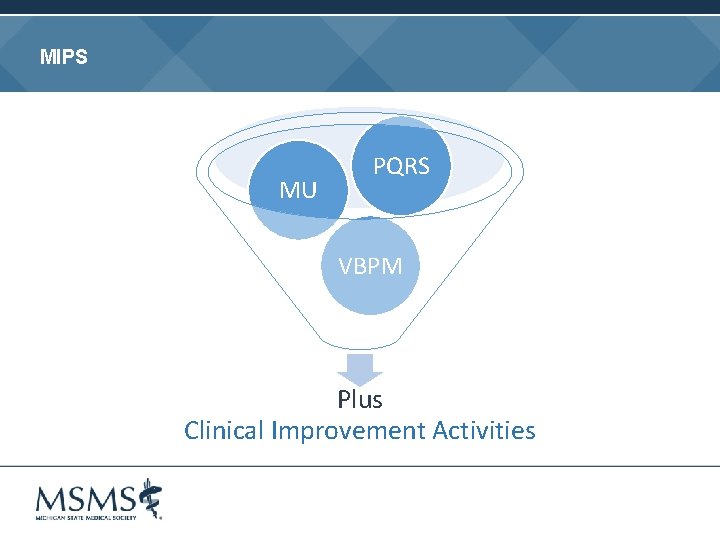
MIPS MU PQRS VBPM Plus Clinical Improvement Activities
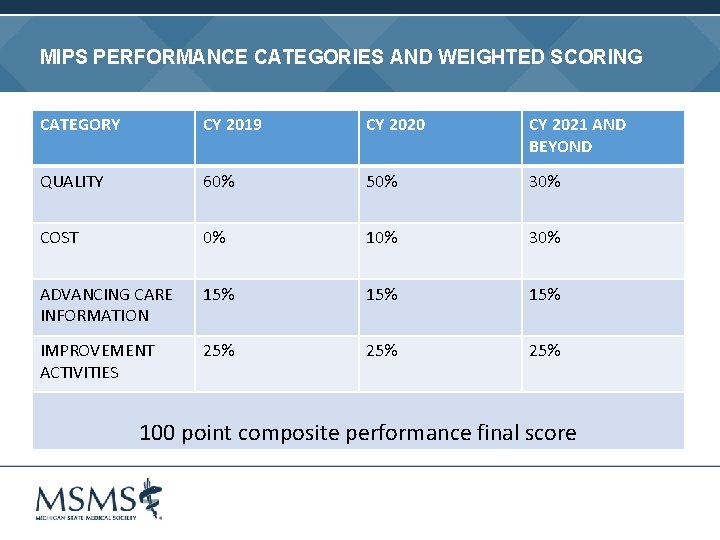
MIPS PERFORMANCE CATEGORIES AND WEIGHTED SCORING CATEGORY CY 2019 CY 2020 CY 2021 AND BEYOND QUALITY 60% 50% 30% COST 0% 10% 30% ADVANCING CARE INFORMATION 15% 15% IMPROVEMENT ACTIVITIES 25% 25% 100 point composite performance final score
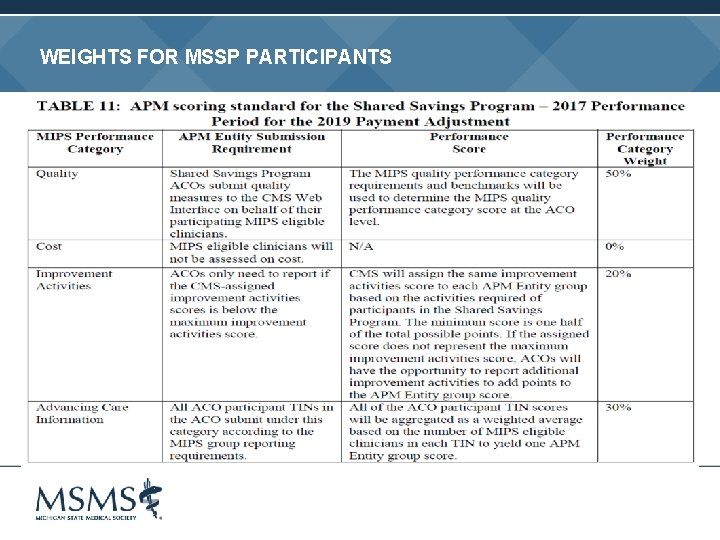
WEIGHTS FOR MSSP PARTICIPANTS

OTHER CONSIDERATIONS Modified participation requirements for some MIPS ECs • • • Non-patient facing physicians Hospital-based physicians Small practices and practices in rural or geographic health professional shortage areas Performance data will be posted on Physician Compare
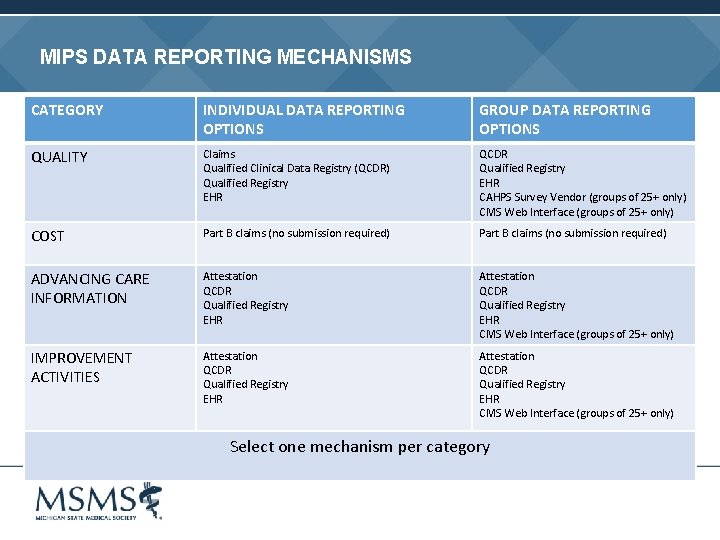
MIPS DATA REPORTING MECHANISMS CATEGORY INDIVIDUAL DATA REPORTING OPTIONS GROUP DATA REPORTING OPTIONS QUALITY Claims Qualified Clinical Data Registry (QCDR) Qualified Registry EHR QCDR Qualified Registry EHR CAHPS Survey Vendor (groups of 25+ only) CMS Web Interface (groups of 25+ only) COST Part B claims (no submission required) ADVANCING CARE INFORMATION Attestation QCDR Qualified Registry EHR CMS Web Interface (groups of 25+ only) IMPROVEMENT ACTIVITIES Attestation QCDR Qualified Registry EHR CMS Web Interface (groups of 25+ only) Select one mechanism per category

What is meant by quality, cost, advancing care information, and improvement activities?

QUALITY Are you currently participating in PQRS? • • Do you regularly document medications? Do you inquire about flu immunization? Is tobacco use screened? Do you receive specialist reports for the patients whom you refer? Do you screen for high blood pressure? Are you participating in the “Million Hearts” Campaign? Do you calculate and document BMI? Do you participate in your specialty’s qualified clinical data registry (QCDR) or a multi-specialty QCDR?

QUALITY Requirements • Final measures list to be published annually • Select 6 measures or 1 specialty measure set o At least 1 outcomes measure (or high priority measure) o 50% scoring threshold in 2017; 60% in 2018 o Partial credit vs pass/fail • Groups using the web interface – report 15 quality measures • MIPS APMs (e. g. , MSSP Track 1) – report through the APM • For groups of 16 or more ECs, CMS will include an allcause hospital readmission measure

QUALITY Performance scoring • Each measure earns up to 10 points • Based upon the percentile-basis performance of the measure • 3 points minimum for reporting a measure • Zero points for measures not reported • Opportunity to earn bonus points • Maximum 60 points

Cost

COST Getting a handle on cost • Have you reviewed your Quality and Resource Use Report (QRUR)? • Are you receiving a negative adjustment under the VBPM? • Are you receiving a positive adjustment under the VBPM? • Do you track or receive ADT information?

COST Criteria • In 2017, weight is zero • Score based on Medicare claims o No reporting necessary • Performance feedback will be given o Total per capita costs for all attributed beneficiaries o Medicare spending per beneficiary o 10 episode-based measures • Risk-adjusted

Advancing Care Information

ACI Utilizing technology • Do you e-Prescribe? • Are you sharing summaries of care electronically when you refer a patient? Or, have you received such information electronically? • Have you performed a security risk analysis as required by HIPAA? • Do you have a patient portal? • Is your EHR certified to 2014 or 2015 standards? • Do you provide education information to your patients? • Do you report to MCIR?

ACI Criteria • Emphasis is on interoperability, secure information exchange, and patient engagement • Scoring is comprised of a base score, optional performance score, and bonus points o 5 measures comprise the base score (50 points) § Security risk analysis, e-Prescribing, patient access, sending summary of care, requesting/accepting summary of care o 9 measures are optional (up to 90 points) o Bonus for reporting to public health or clinical data registries and for utilizing CEHRT for improvement activities (up to 15 points) o Earn 100 points or more for full credit

Improvement Activities

IMPROVEMENT ACTIVITIES Engaging in improvement activities • Do you offer 24/7 access? • Do you use MAPS? • Are you participating in the Transforming Clinical Practice Initiative? • Do you accept new and follow-up Medicaid patients in a timely manner? • Are you a PCMH? • Are you participating in a MIPS APM? • Are you a participant in a Quality Improvement Organization (e. g. MPRO/Lake Superior Quality Innovation Network) initiative? • Have you completed any of the AMA STEPSForward™ modules? • Do you use Choosing Wisely tools or resources?

IMPROVEMENT ACTIVITIES Criteria • Focus is on care coordination, shared decision-making, beneficiary engagement, health equity, population management, and patient safety • Credit given for engaging in clinical practice improvement activities • 90+ activities weighted as “high” (20 points) or “medium” (10 points) • Zero score if not engaged in at least one activity • 40 points* for maximum score • Full credit for PCMH designation • Minimum half credit for APM participation • Bonus points for utilizing EHR technology *20 points for MIPS ECs who are non-patient facing or who are in small practices or practices in rural or health professional shortage areas
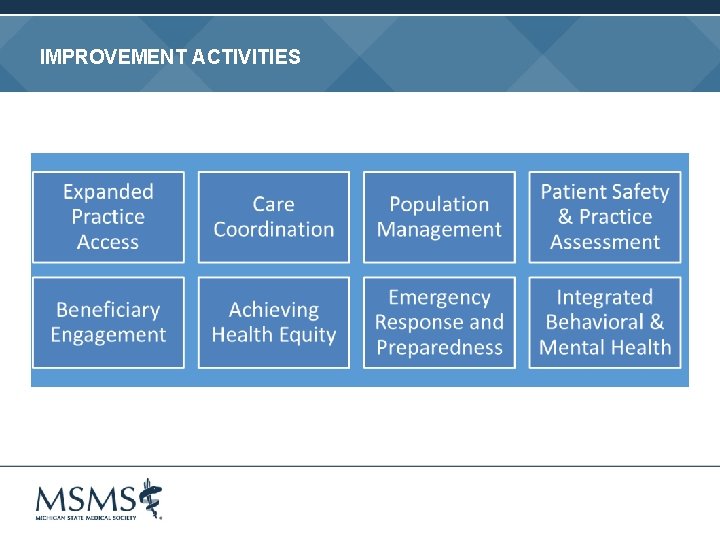
IMPROVEMENT ACTIVITIES
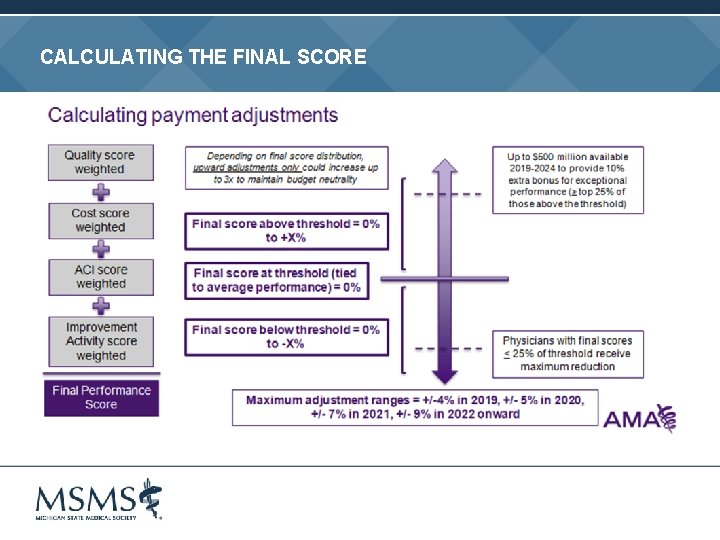
CALCULATING THE FINAL SCORE

Alternative Payment Models (APMs)

APMs Alternative Payment Model • Payment approach designed to incentivize high-quality and cost-efficient care • Can apply to a specific clinical condition, a care episode, or a population • As defined in the final rule… o CMS Innovation Center Model (other than a Health Care Innovation Award) o Medicare Shared Savings Program ACOs o Demonstrations under the Health Care Quality Demonstration Program o Demonstrations required by federal law

APMs Advanced APMs • • • Subset of APMs Share rewards Share nominal financial risk Utilize electronic health record technology Base payment on quality measures comparable to MIPS QMs • CMS designated • Includes medical home models expanded under the CMS Innovation Center

APMs 2017 Advanced APMs • • Medicare Shared Savings Program (Tracks 2 and 3) Next Generation ACOs Comprehensive Primary Care Plus Comprehensive ESRD Care (LDO and non-LDO arrangements) • Oncology Care Model (two-sided risk arrangement) 2018 and beyond • Could include a new MSSP ACO Track 1+, bundled payment models, other payer ACOs, physician-focused payment models, etc.

APM INCENTIVES MACRA provides incentives for qualifying professionals in Advanced APMs • Lump sum bonus payment of 5% of Part B payments for professional services • Exemption from MIPS reporting requirements • Higher base rates beginning in 2026
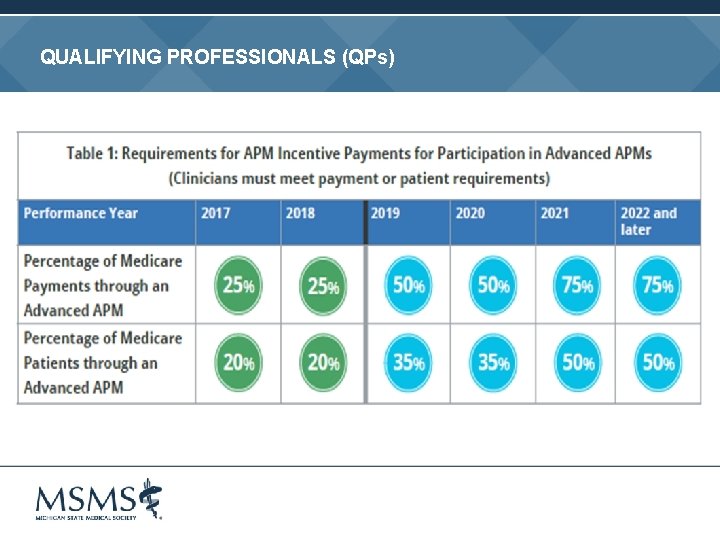
QUALIFYING PROFESSIONALS (QPs)
APMs QPs Partially Qualified APM Participants Advanced APM MIPS APM

What Happens Now?

STRATEGIES FOR SUCCESS “Just breathe” • Much of this will be familiar if you’re currently participating in PQRS, MU, specialty or other professional quality improvement activities Determine pathway that makes sense for your situation • Status • • o AMA’s Payment Model Evaluator - https: //apps. ama-assn. org/pme/#/ Individual vs. group vs. MIPS APM reporting How to report Identify exceptions and preferential scoring opportunities ROI
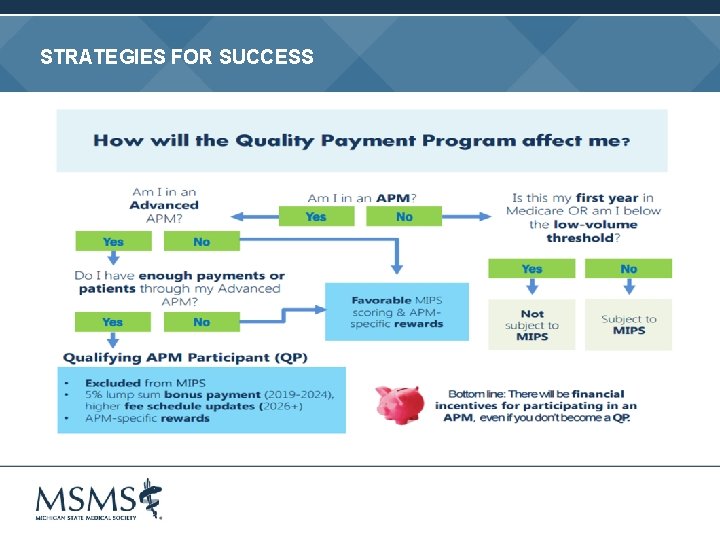
STRATEGIES FOR SUCCESS

STRATEGIES FOR SUCCESS Review Quality and Resource Use Reports (QRURs) • Download at https: //portal. cms. gov • See directions on how to obtain your QRUR at https: //www. cms. gov/Medicare-Fee-for-Service. Payment/Physician. Feedback. Program/2014 QRUR. html#2014 -annual-qrur • QRURs with 2015 data released last fall

STRATEGIES FOR SUCCESS Identify and target gaps and areas of strength • Current PQRS measures that are meaningful • Improve administrative processes and performance measurements under PQRS and VBPM • Patient data entered consistently and accurately • HIT that works for you o Opportunities for efficiencies , patient engagement, analytics, etc. o Leverage data registries

STRATEGIES FOR SUCCESS Identify current practice improvement activities • Align quality measures • Easily accomplished • Future opportunities (e. g. , telehealth, expanded access, AMA Steps. Forward™ modules, etc. ) • Review internal workflow processes related to patient engagement and data exchange Evaluate staffing needs and resources

STRATEGIES FOR SUCCESS Examine where best to focus efforts • Chronic disease management patients • Referrals and transitions of care • High treatment costs without sacrificing quality Emphasize need for accurate documentation and coding to ensure claims reflect complexity of patient population • Ensure physicians and billers/coders are speaking the same language • Co-morbidities that are considered for treatment or medical decision-making should be documented and included on the claim

STRATEGIES FOR SUCCESS Evaluate readiness of your EHR system and vendors • Certified edition 2014 or 2015? • Support Medicare quality reporting? • Help with optimization? Utilize MSMS, AMA, specialty societies, physician organizations, etc. for resources and education opportunities and to help you sort through the details

STRATEGIES FOR SUCCESS MSMS MACRA Plan • • • Jan/Feb ‘ 17 Michigan Medicine http: //msms. org/MACRA Two full-day conferences May 5, 2017 (Friday before the MSMS HOD) October 24, 2017 (Tuesday before the ASM) Series of free Lunch & Learn webinars On-demand education modules Video updates MSMS communication channels

Resources

RESOURCES • CMS MACRA QPP Web Site - https: //qpp. cms. gov/ • MSMS – http: //msms. org/MACRA • AMA - http: //www. ama-assn. org/ama/pub/advocacy/topics/medicarephysician-payment-reform. page • QRURs - https: //www. cms. gov/Medicare-Fee-for-Service. Payment/Physician. Feedback. Program/Obtain-2013 -QRUR. html • Office of the National Coordinator CEHRT List https: //chpl. healthit. gov/#/search • MGMA – https: //www. mgma. com • Lake Superior Quality Innovation Network (QIN)- https: //www. lsqin. org

RESOURCES Quality Payment Program Service Center • 1 -866 -288 -8292 (TTY 1 -877 -715 -6222) • qpp@cms. hhs. gov National Provider Calls • http: //www. cms. gov/Medicare/Quality-Initiatives-Patient. Assessment-Instruments/PQRS/CMSSponsored. Calls. html FFS Provider Listserv • https: //list. nih. gov/cgi-bin/wa. exe? A 0=PHYSICIANS-L

State Legislative Issues • -State Budget • -Scope of Practice • -Auto No-Fault • -Maintenance of Certification

State Budget -State should be finished by the beginning of June -The biggest factors that impact physicians are Medicaid and GME funding -MSMS does not currently expect any cuts from the state to current funding for either of these items, but could be impacted by any changes to federal funding

Scope of Practice -Every legislative session, legislation is introduced that would expand the scope of practice for non-physicians -MSMS believes in a physician led health care team -In the last legislative session, MSMS narrowly defeated SB-320, legislation that would have expanded the scope of practice for certified nurse anesthetists and allowed them to practice without oversight by an anesthesiologist -While this legislation was defeated, we do expect it to be reintroduced for this legislative session

Auto No-Fault -Michigan is the last state with a true auto no-fault system -The cost of insurance is slightly higher than other states, but people who are injured do receive care without ultimately being put on Medicaid -The Governor and other legislative leaders have been pushing to completely alter auto no-fault in ways that would lower reimbursement for physicians and other healthcare providers, potentially leave consumers with too little coverage, and provide little in the way of guaranteed savings for consumers -MSMS does expect for some sort of compromise to be reached on this legislation, ideally with no impact on physicians

Maintenance of Certification (MOC) -Since the beginning of the last legislative session, MSMS has been championing legislation that would free physicians from burdensome MOC requirements -These bills would prohibit either hospitals or health plans from requiring MOC to serve on a panel or receive privileges -Michigan already has the highest CME requirements for licensing in the country and no data exists that physicians who maintain MOC provide higher quality care -More information can be found at www. right 2 care. org

Thank you! Joshua C. Richmond Director, Membership & Physician Engagement Michigan State Medical Society (517) 336 -5788 jrichmond@msms. org
- Slides: 58