Macitentan A novel sulfamide Bosentan Macitentan Bolli M
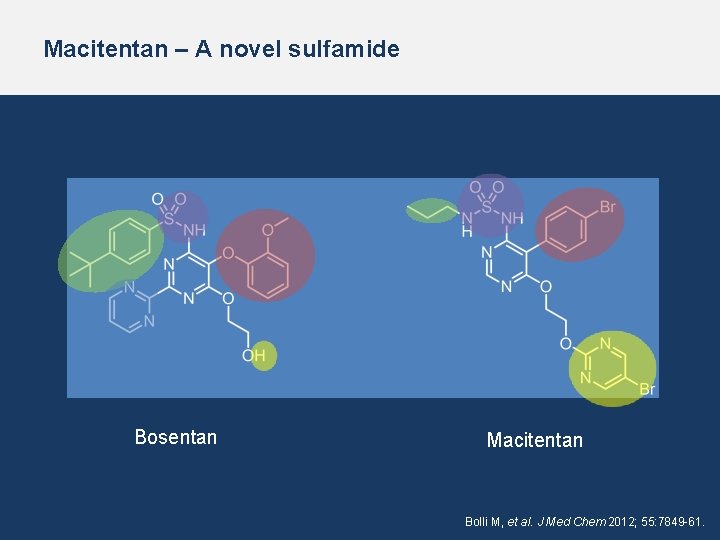
Macitentan – A novel sulfamide Bosentan Macitentan Bolli M, et al. J Med Chem 2012; 55: 7849 -61.
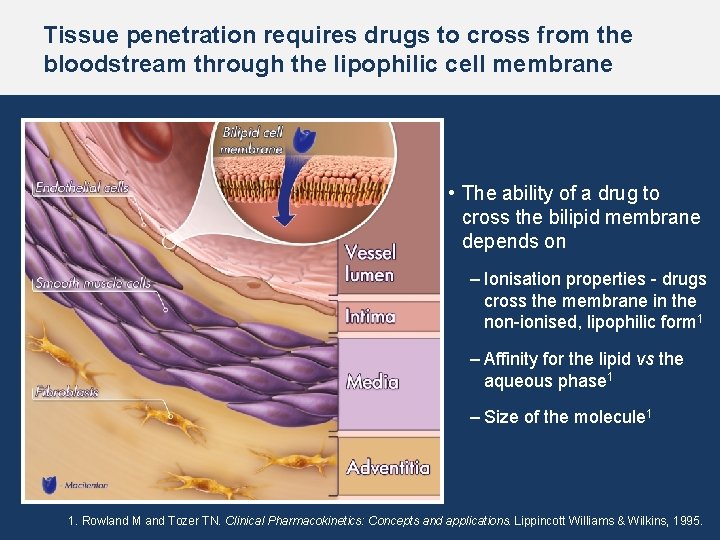
Tissue penetration requires drugs to cross from the bloodstream through the lipophilic cell membrane • The ability of a drug to cross the bilipid membrane depends on – Ionisation properties - drugs cross the membrane in the non-ionised, lipophilic form 1 – Affinity for the lipid vs the aqueous phase 1 – Size of the molecule 1 1. Rowland M and Tozer TN. Clinical Pharmacokinetics: Concepts and applications. Lippincott Williams & Wilkins, 1995.
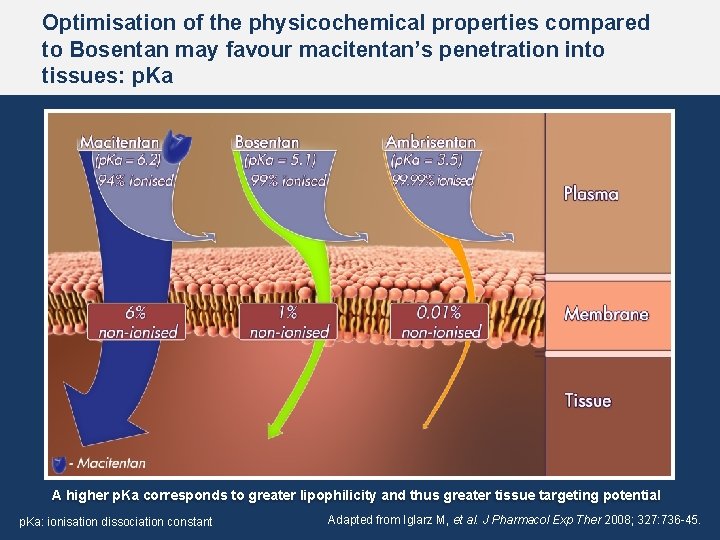
Optimisation of the physicochemical properties compared to Bosentan may favour macitentan’s penetration into tissues: p. Ka A higher p. Ka corresponds to greater lipophilicity and thus greater tissue targeting potential p. Ka: ionisation dissociation constant Adapted from Iglarz M, et al. J Pharmacol Exp Ther 2008; 327: 736 -45.

Optimisation of the physicochemical properties compared to Bosentan may favour macitentan’s penetration into tissues: Log D In vitro data Log D (Distribution coefficient) Lipid: Aqueous Macitentan Bosentan Ambrisentan 800: 1 20: 1 1: 2. 5 Blood Membrane Tissue • The distribution coefficient (Log D) defines the distribution of a compound between an aqueous and a lipid phase • A greater affinity for the lipid phase may favour tissue penetration • Macitentan may have a greater affinity for the lipid phase compared with other ERAs* *To date, no head-to-head trials in humans have been performed. Iglarz M, et al. J Pharmacol Exp Ther 2008; 327: 736 -45.
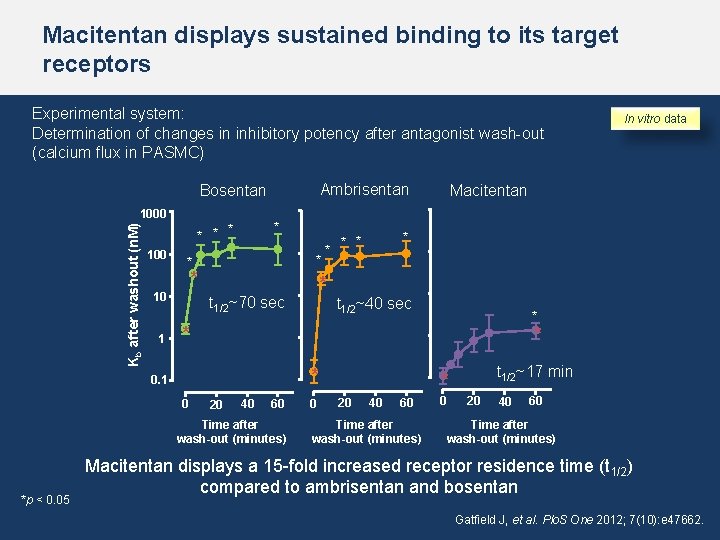
Macitentan displays sustained binding to its target receptors Experimental system: Determination of changes in inhibitory potency after antagonist wash-out (calcium flux in PASMC) Ambrisentan Bosentan Kb after washout (n. M) 1000 * * 100 * * * 10 1 Macitentan * * t 1/2~70 sec t 1/2~40 sec * * 0. 1 0 20 40 60 Time after wash-out (minutes) *p < 0. 05 * In vitro data 0 t 1/2~17 min * 20 40 60 Time after wash-out (minutes) 0 20 40 60 Time after wash-out (minutes) Macitentan displays a 15 -fold increased receptor residence time (t 1/2) compared to ambrisentan and bosentan Gatfield J, et al. Plo. S One 2012; 7(10): e 47662.
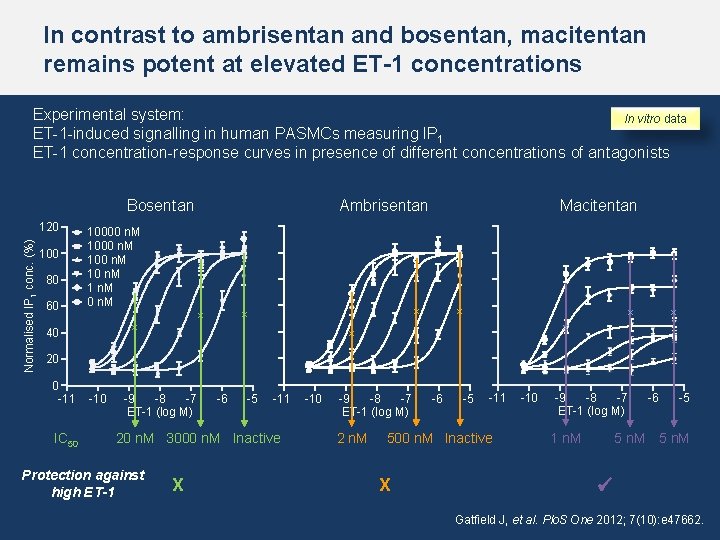
In contrast to ambrisentan and bosentan, macitentan remains potent at elevated ET-1 concentrations Experimental system: In vitro data ET-1 -induced signalling in human PASMCs measuring IP 1 ET-1 concentration-response curves in presence of different concentrations of antagonists Bosentan Normalised IP 1 conc. (%) 120 100 80 60 10000 n. M 100 n. M 1 n. M 0 n. M x x 40 Macitentan Ambrisentan x x x 20 0 -11 IC 50 -10 -9 -8 -7 ET-1 (log M) -6 -5 -11 20 n. M 3000 n. M Inactive Protection against high ET-1 X -10 -9 -8 -7 ET-1 (log M) 2 n. M -6 -5 -11 500 n. M Inactive X -10 -9 -8 -7 ET-1 (log M) 1 n. M -6 -5 5 n. M Gatfield J, et al. Plo. S One 2012; 7(10): e 47662.
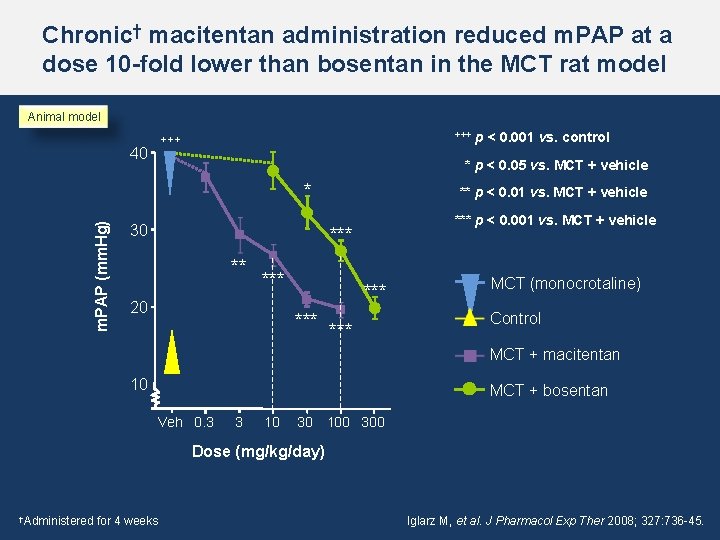
Chronic† macitentan administration reduced m. PAP at a dose 10 -fold lower than bosentan in the MCT rat model Animal model +++ 40 * p < 0. 05 vs. MCT + vehicle * m. PAP (mm. Hg) p < 0. 001 vs. control 30 ** p < 0. 01 vs. MCT + vehicle *** p < 0. 001 vs. MCT + vehicle *** ** *** 20 *** *** MCT (monocrotaline) Control MCT + macitentan 10 MCT + bosentan Veh 0. 3 3 10 30 100 300 Dose (mg/kg/day) †Administered for 4 weeks Iglarz M, et al. J Pharmacol Exp Ther 2008; 327: 736 -45.
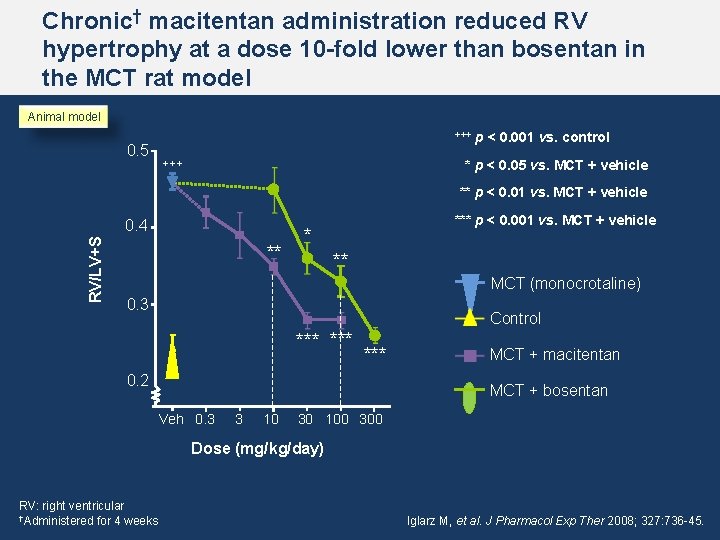
Chronic† macitentan administration reduced RV hypertrophy at a dose 10 -fold lower than bosentan in the MCT rat model Animal model +++ 0. 5 +++ p < 0. 001 vs. control * p < 0. 05 vs. MCT + vehicle ** p < 0. 01 vs. MCT + vehicle RV/LV+S 0. 4 ** *** p < 0. 001 vs. MCT + vehicle * ** MCT (monocrotaline) 0. 3 Control *** *** 0. 2 MCT + macitentan MCT + bosentan Veh 0. 3 3 10 30 100 300 Dose (mg/kg/day) RV: right ventricular †Administered for 4 weeks Iglarz M, et al. J Pharmacol Exp Ther 2008; 327: 736 -45.
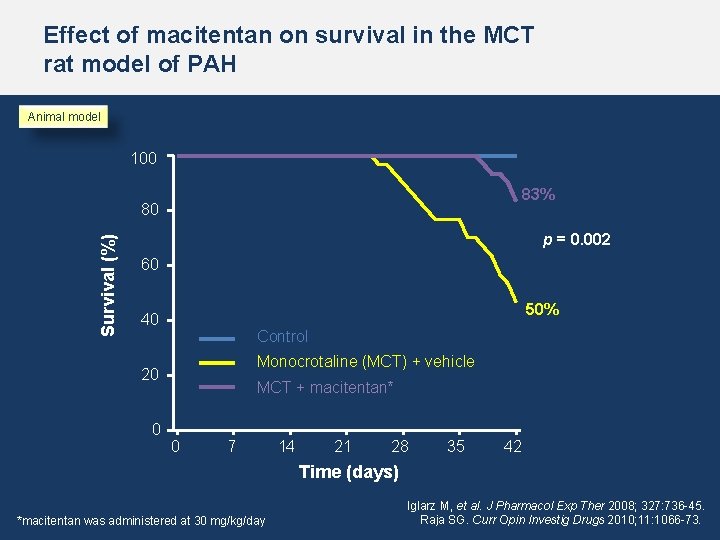
Effect of macitentan on survival in the MCT rat model of PAH Animal model 100 83% Survival (%) 80 p = 0. 002 60 50% 40 Control Monocrotaline (MCT) + vehicle 20 0 MCT + macitentan* 0 7 14 21 28 35 42 Time (days) *macitentan was administered at 30 mg/kg/day Iglarz M, et al. J Pharmacol Exp Ther 2008; 327: 736 -45. Raja SG. Curr Opin Investig Drugs 2010; 11: 1066 -73.
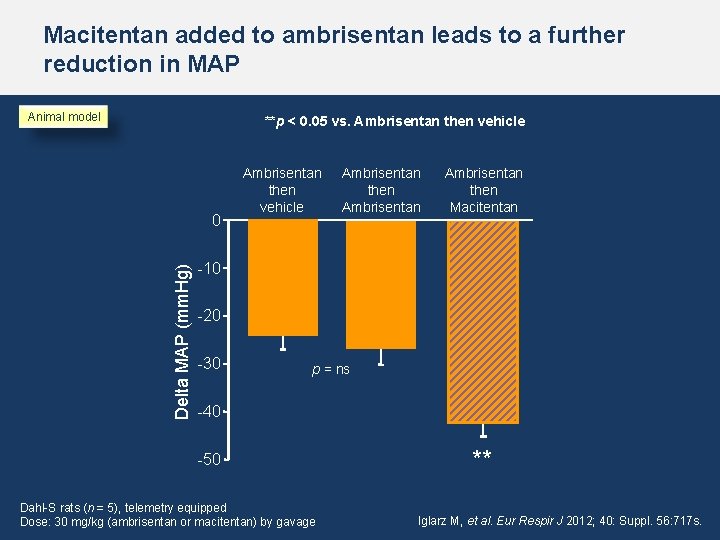
Macitentan added to ambrisentan leads to a further reduction in MAP Animal model **p < 0. 05 vs. Ambrisentan then vehicle Delta MAP (mm. Hg) 0 Ambrisentan then vehicle Ambrisentan then Macitentan -10 -20 -30 p = ns -40 -50 Dahl-S rats (n = 5), telemetry equipped Dose: 30 mg/kg (ambrisentan or macitentan) by gavage ** Iglarz M, et al. Eur Respir J 2012; 40: Suppl. 56: 717 s.
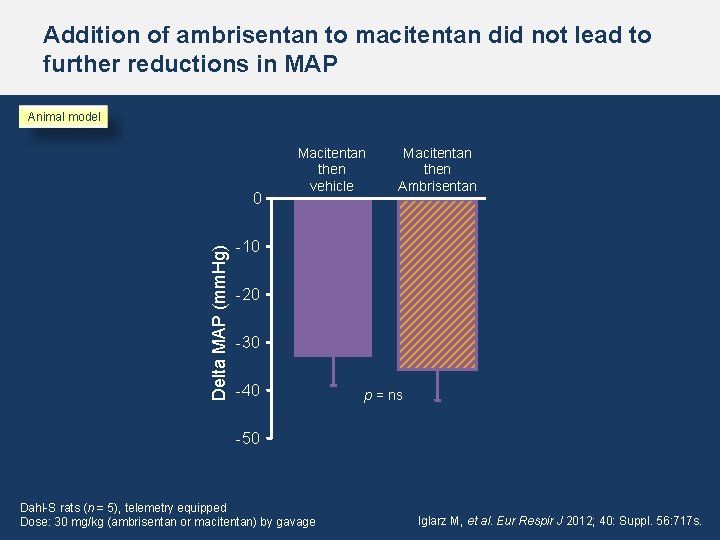
Addition of ambrisentan to macitentan did not lead to further reductions in MAP Animal model Delta MAP (mm. Hg) 0 Macitentan then vehicle Macitentan then Ambrisentan -10 -20 -30 -40 p = ns -50 Dahl-S rats (n = 5), telemetry equipped Dose: 30 mg/kg (ambrisentan or macitentan) by gavage Iglarz M, et al. Eur Respir J 2012; 40: Suppl. 56: 717 s.
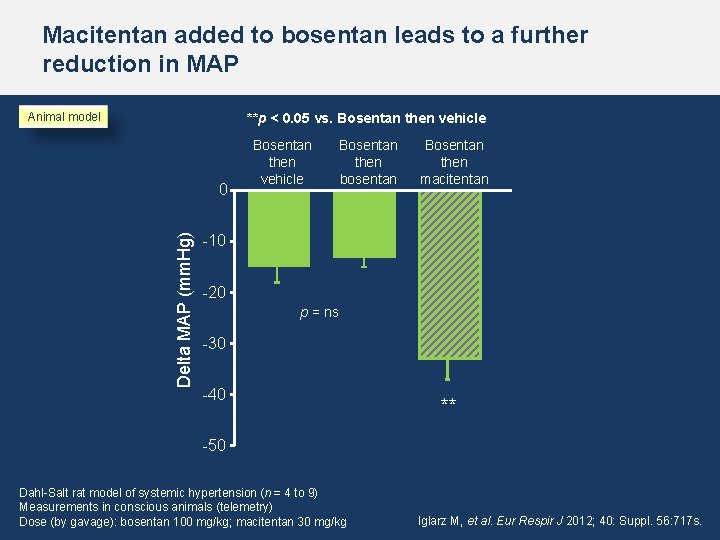
Macitentan added to bosentan leads to a further reduction in MAP Animal model **p < 0. 05 vs. Bosentan then vehicle Delta MAP (mm. Hg) 0 Bosentan then vehicle Bosentan then bosentan Bosentan then macitentan -10 -20 p = ns -30 -40 ** -50 Dahl-Salt rat model of systemic hypertension (n = 4 to 9) Measurements in conscious animals (telemetry) Dose (by gavage): bosentan 100 mg/kg; macitentan 30 mg/kg Iglarz M, et al. Eur Respir J 2012; 40: Suppl. 56: 717 s.
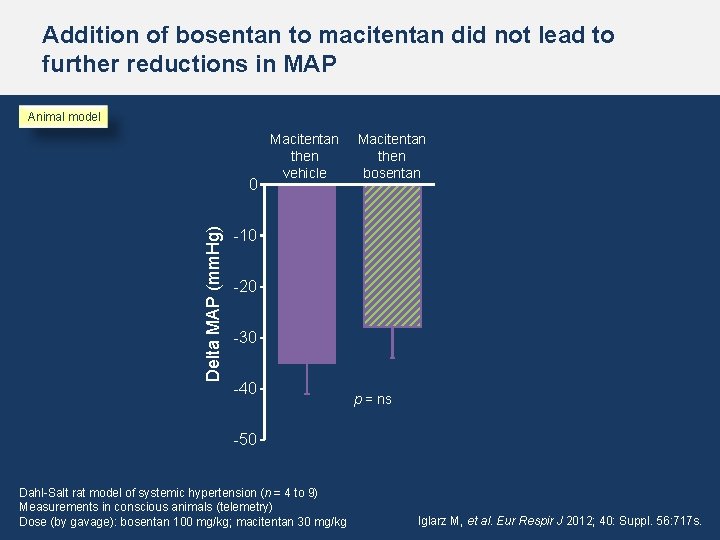
Addition of bosentan to macitentan did not lead to further reductions in MAP Animal model Delta MAP (mm. Hg) 0 Macitentan then vehicle Macitentan then bosentan -10 -20 -30 -40 p = ns -50 Dahl-Salt rat model of systemic hypertension (n = 4 to 9) Measurements in conscious animals (telemetry) Dose (by gavage): bosentan 100 mg/kg; macitentan 30 mg/kg Iglarz M, et al. Eur Respir J 2012; 40: Suppl. 56: 717 s.

Pre-clinical, in vitro data and hepatic safety for macitentan • Inhibition of BSEP, resulting in the disruption of bile salt homeostasis, is a key mechanism that may cause hepatic cholestasis and liver damage 1 • Macitentan and its active metabolite do not have significant inhibitory effects on bile salt transport 2, 3 • In vitro studies suggest that hepatic disposition of macitentan is mainly driven by passive diffusion rather than OATP-mediated uptake 4 1. Fattinger K, et al. Clin Pharmacol Ther 2001; 69: 223 -31. 2. Raja SG. Curr Opin Investig Drugs 2010; 11: 1066 -73. 3. Bolli M, et al. J Med Chem 2012; 55: 7849 -61. 4. Bruderer S, et al. AAPS 2012; 14: 68 -78.

Macitentan – Summary • Macitentan is a newly developed molecule displaying: – Optimised physicochemical properties that facilitate penetration into the tissue – High affinity for the ET receptors and sustained receptor binding resulting in more effective receptor antagonism • Pre-clinical data suggest that macitentan may have the potential for favourable potency and efficacy • In vitro and pre-clinical data suggests that macitentan has the potential for favourable safety and tolerability
- Slides: 15