Maastricht Classification of DCD Definition I Where Dead















- Slides: 30

Maastricht Classification of DCD Definition I Where Dead on arrival Spain, France, Italy II Unsuccessful resuscitation III Cardiac arrest awaited after withdrawal of life support in patients who are not brain dead IV Cardiac arrest after brain death MC I, II, uncontrolled MC III, IV: controlled 18 th TPM course, November 2012 Belgium, United Kingdom, Netherlands, Australia, USA, New Zealand

An Introduction to Maastricht Category III DCD Dr Paul Murphy National Lead for Organ Donation NHS Blood and Transplant, UK 18 th TPM course, November 2012

Controlled DCD – the donation process Objectives for the session – to understand • Definition of category III DCD • Key elements of the category III DCD pathway • Obstacles to DCD donation – Family approach and conflict of interest – Who can donate: prediction of asystole – Limitation of ischaemic injury – Diagnosis of death and post mortem interventions • Outcomes – Contribution to transplantation in UK 18 th TPM course, November 2012

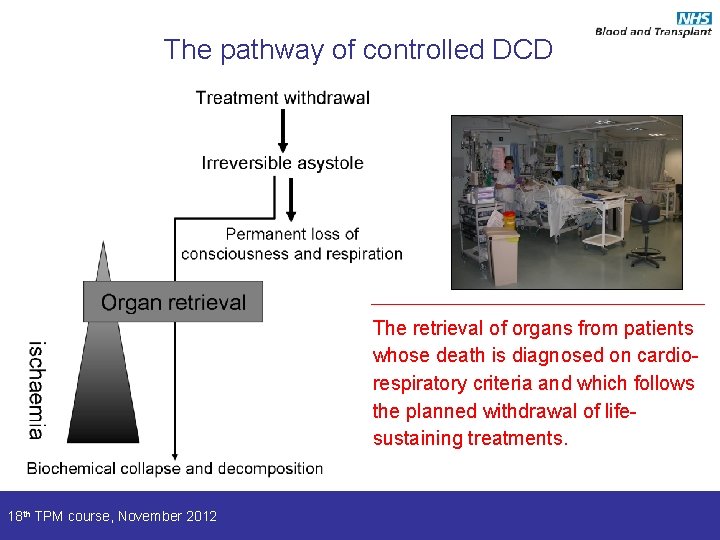
The pathway of controlled DCD The retrieval of organs from patients whose death is diagnosed on cardiorespiratory criteria and which follows the planned withdrawal of lifesustaining treatments. 18 th TPM course, November 2012

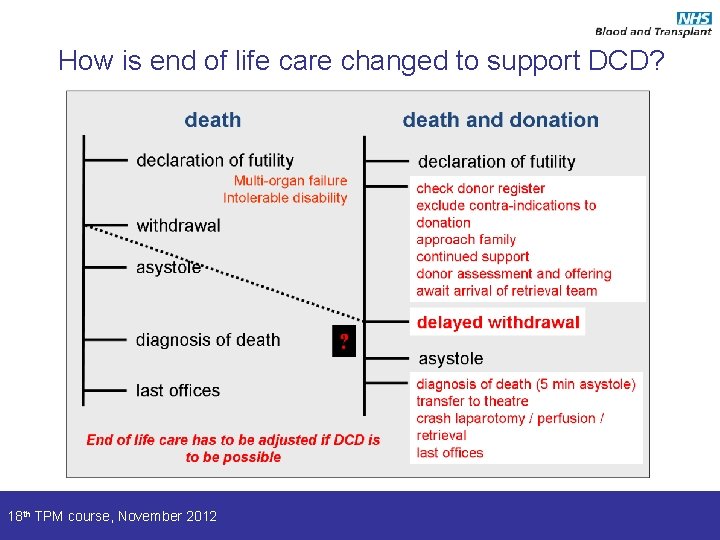
How is end of life care changed to support DCD? 18 th TPM course, November 2012

DCD as part of end of life care Key considerations General overview • Donation considered before death • Withdrawal delayed by several hours – Physiological instability • Altered management of death – ? Withdrawal in anaesthetic room – Diagnosis of death after 5 minutes of asystole – Rapid transfer to theatre • Organ ischaemia and graft outcomes • Stand down • Substitution 18 th TPM course, November 2012 We view DCD as part of the care we give patients when they die – offered, not imposed

DCD as part of end of life care Key considerations General overview • Donation considered before death • Withdrawal delayed by several hours – Physiological instability • Altered management of death – ? Withdrawal in anaesthetic room – Diagnosis of death after 5 minutes of asystole – Rapid transfer to theatre • Organ ischaemia and graft outcomes • Stand down • Substitution 18 th TPM course, November 2012 40% of DCD retrievals in the UK are stood down.

Family approach and conflict of interest • Decision making around withdrawal of treatments should be transparent and consistent – All ICUs and EDs should have explicit local policies based upon national guidance – Multi-disciplinary • Donation should only be raised after a family have understood and accepted their loss – presented as an end of life care option 18 th TPM course, November 2012 “You should be prepared to follow any national procedures for identifying

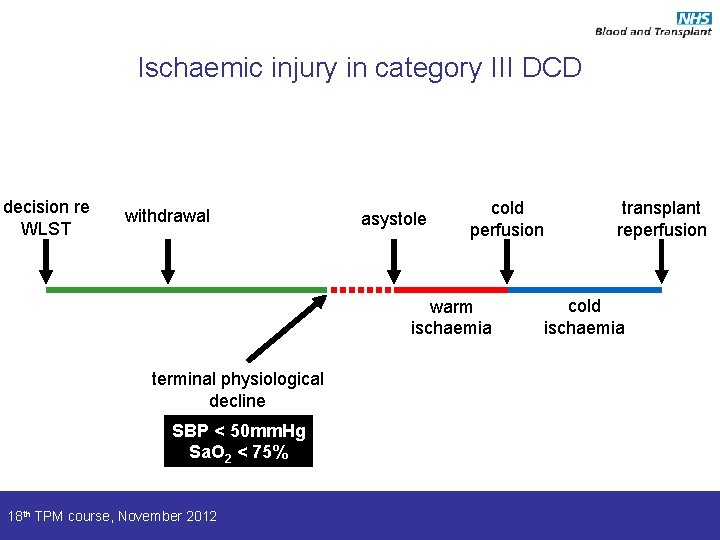
Ischaemic injury in category III DCD decision re WLST withdrawal asystole cold perfusion warm ischaemia terminal physiological decline SBP < 50 mm. Hg Sa. O 2 < 75% 18 th TPM course, November 2012 transplant reperfusion cold ischaemia

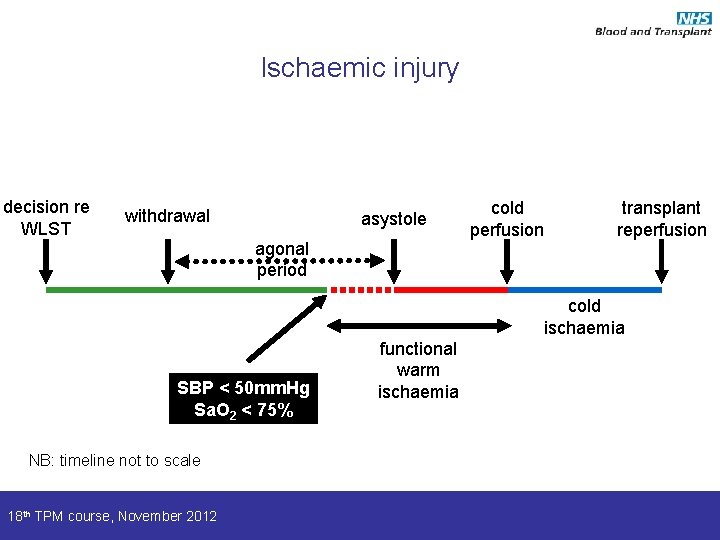
Ischaemic injury decision re WLST withdrawal asystole agonal period cold perfusion transplant reperfusion cold ischaemia SBP < 50 mm. Hg Sa. O 2 < 75% NB: timeline not to scale 18 th TPM course, November 2012 functional warm ischaemia

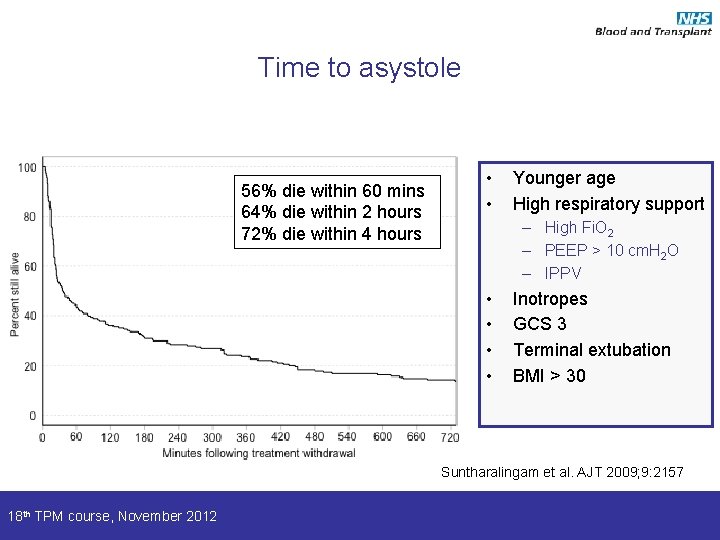
Time to asystole 56% die within 60 mins 64% die within 2 hours 72% die within 4 hours • • Younger age High respiratory support – High Fi. O 2 – PEEP > 10 cm. H 2 O – IPPV • • Inotropes GCS 3 Terminal extubation BMI > 30 Suntharalingam et al. AJT 2009; 9: 2157 18 th TPM course, November 2012

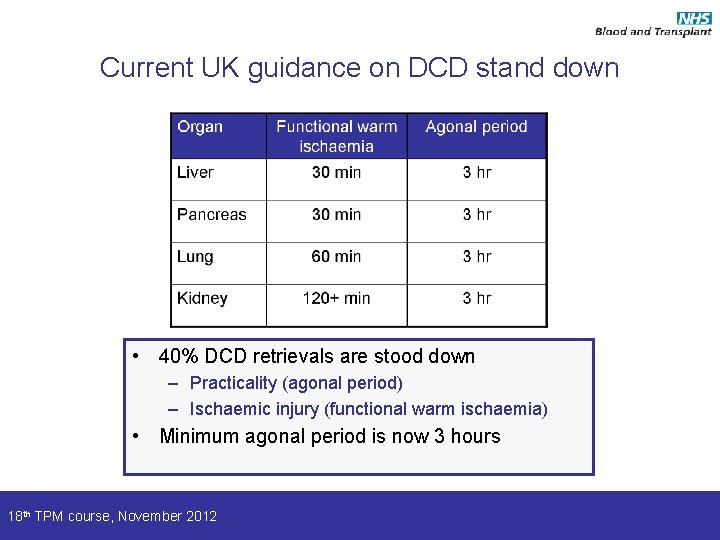
Current UK guidance on DCD stand down • 40% DCD retrievals are stood down – Practicality (agonal period) – Ischaemic injury (functional warm ischaemia) • Minimum agonal period is now 3 hours 18 th TPM course, November 2012

Solutions to ischaemic injury • Ante-mortem – Tissue typing and virological screening – Steroids, heparin, vasodilators – Femoral cannulation • Management at time of death – Withdrawal in theatre t = 2 min – Expedient diagnosis of death • Post-mortem reperfusion – In situ – Ex situ 18 th TPM course, November 2012 Medical Centre University of Pittsburgh USA

Process of treatment withdrawal • Manner of treatment withdrawal should not be adjusted to promote donation • Complete withdrawal of all cardio-respiratory treatments – Inotropes – Ventilation – Endotracheal tube • Nursed in supine position • Pharmacological comfort cares as required 18 th TPM course, November 2012

Location of treatment withdrawal Theatre Critical Care Reduces warm ischaemia Fewer staffing issues May give family more privacy Stand downs easily managed Need back up plan for stand down Longer warm ischaemia Creates staffing problems Undignified rush to theatre May create conflicts for retrieval teams Not ideal environments for families 18 th TPM course, November 2012

Diagnosis of Death www. aomrc. org. uk/publications/ reports-guidance. html 18 th TPM course, November 2012 In the UK, death can be confirmed after 5 minutes of complete and continuous absence of cardiorespiratory function…………

Diagnosis of Death • Asystole is absence of mechanical cardiac function, not electrical silence on ECG • It is best diagnosed by – Invasive arterial pressure monitoring – Echocardiography • If invasive pressure monitoring or echocardiography are not available, identify on basis of isoelectric ECG 18 th TPM course, November 2012 Death can be diagnosed after five minutes of continuous asystole

Diagnosis of Death • Death is confirmed by demonstrating the absence of neurological function (respiration, consciousness and brainstem reflexes) after 5 minutes of continuous asystole • Any return of cardiac or respiratory function must prompt further 5 minutes of observation 18 th TPM course, November 2012 Death is regarded as the simultaneous and irreversible loss of consciousness and respiration

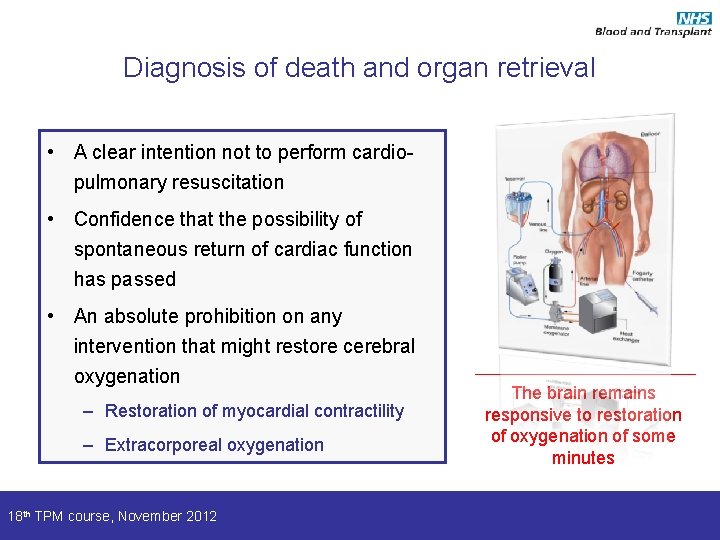
Diagnosis of death and organ retrieval • A clear intention not to perform cardiopulmonary resuscitation • Confidence that the possibility of spontaneous return of cardiac function has passed • An absolute prohibition on any intervention that might restore cerebral oxygenation – Restoration of myocardial contractility – Extracorporeal oxygenation 18 th TPM course, November 2012 The brain remains responsive to restoration of oxygenation of some minutes

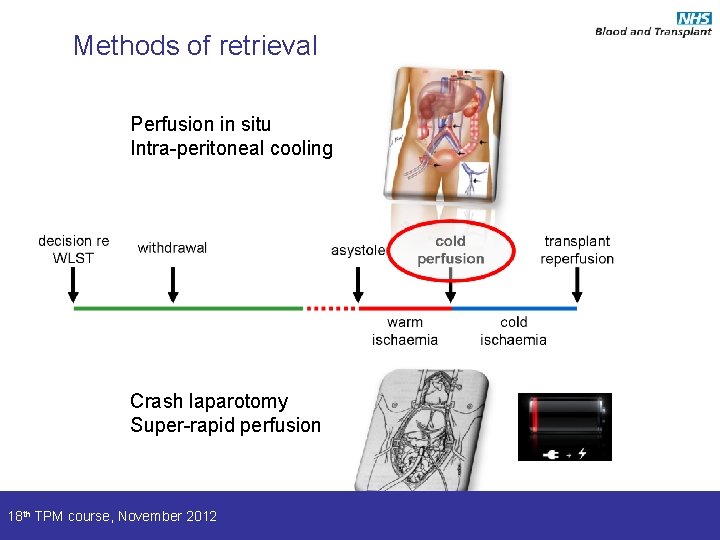
Methods of retrieval Perfusion in situ Intra-peritoneal cooling Crash laparotomy Super-rapid perfusion 18 th TPM course, November 2012

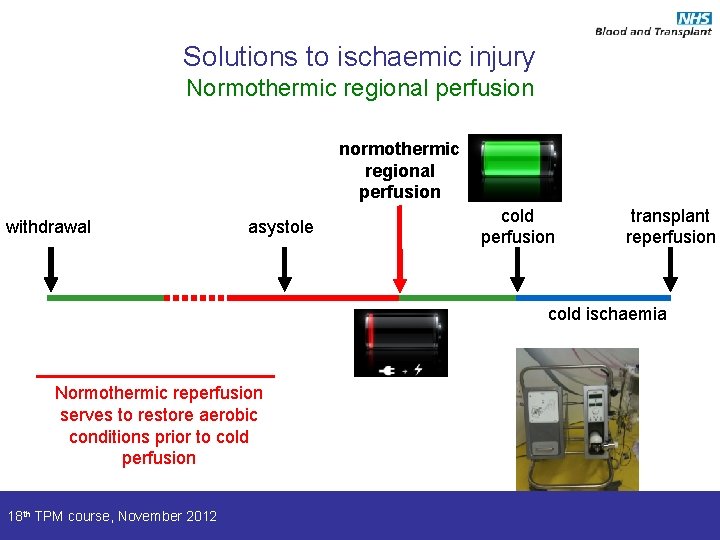
Solutions to ischaemic injury Normothermic regional perfusion normothermic regional perfusion withdrawal asystole cold perfusion transplant reperfusion cold ischaemia Normothermic reperfusion serves to restore aerobic conditions prior to cold perfusion 18 th TPM course, November 2012

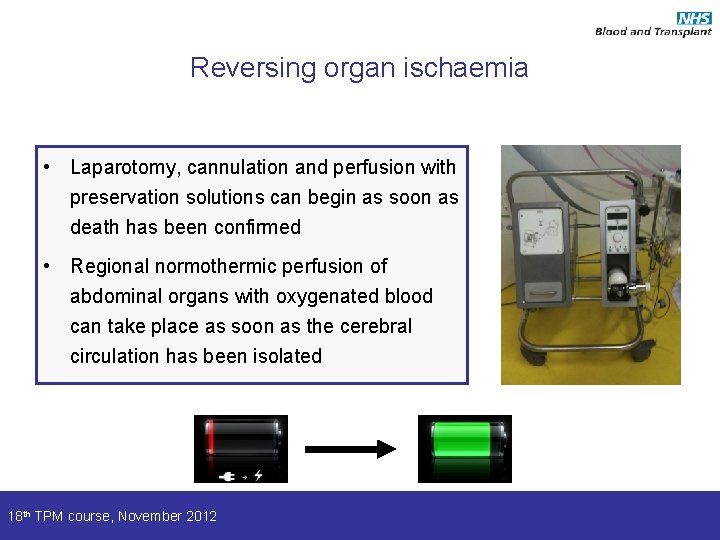
Reversing organ ischaemia • Laparotomy, cannulation and perfusion with preservation solutions can begin as soon as death has been confirmed • Regional normothermic perfusion of abdominal organs with oxygenated blood can take place as soon as the cerebral circulation has been isolated 18 th TPM course, November 2012

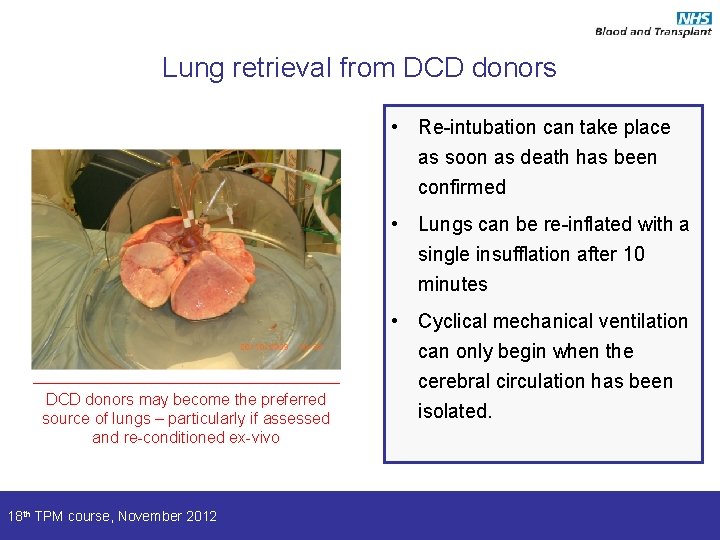
Lung retrieval from DCD donors • Re-intubation can take place as soon as death has been confirmed • Lungs can be re-inflated with a single insufflation after 10 minutes DCD donors may become the preferred source of lungs – particularly if assessed and re-conditioned ex-vivo 18 th TPM course, November 2012 • Cyclical mechanical ventilation can only begin when the cerebral circulation has been isolated.

Deceased donation in UK, 2000 -12 25% of DD transplants in the UK come from MC 3 DCD donors 18 th TPM course, November 2012

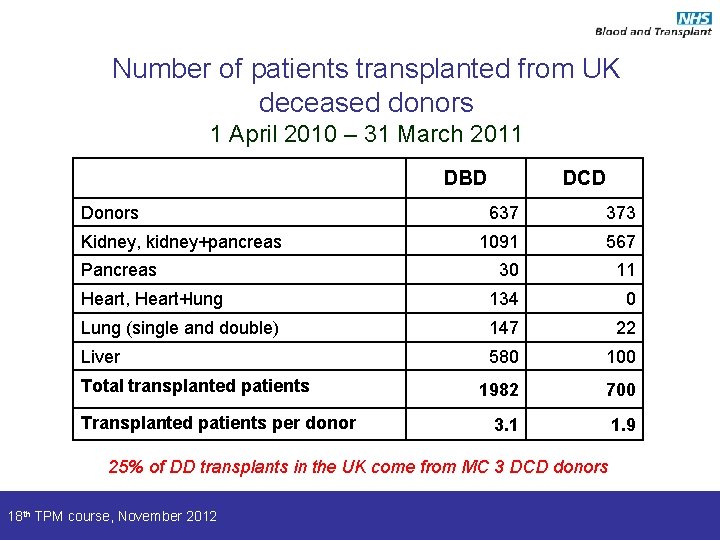
Number of patients transplanted from UK deceased donors 1 April 2010 – 31 March 2011 DBD Donors DCD 637 373 1091 567 30 11 Heart, Heart+lung 134 0 Lung (single and double) 147 22 Liver 580 100 1982 700 3. 1 1. 9 Kidney, kidney+pancreas Pancreas Total transplanted patients Transplanted patients per donor 25% of DD transplants in the UK come from MC 3 DCD donors 18 th TPM course, November 2012

Cause of death in MC III DCD donors UK Potential Donor Audit (October 2009 – March 2012) 7504 patients referred as potential DCD donors 877 actual DCD donors 18 th TPM course, November 2012

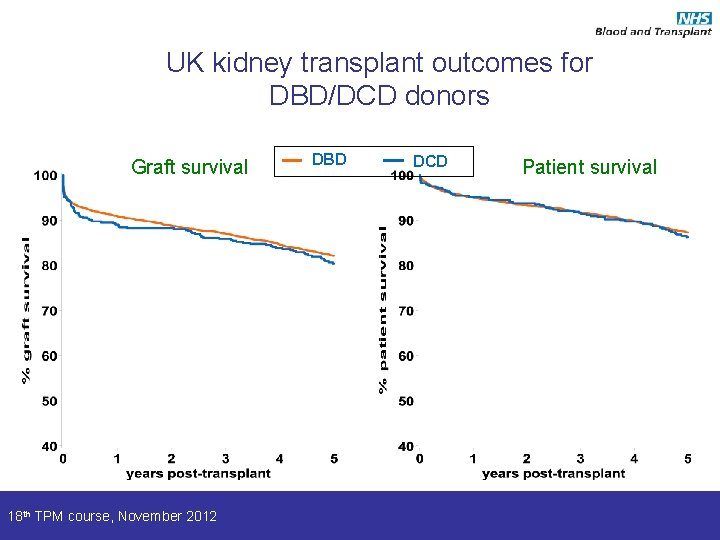
UK kidney transplant outcomes for DBD/DCD donors Graft survival 18 th TPM course, November 2012 DBD DCD Patient survival

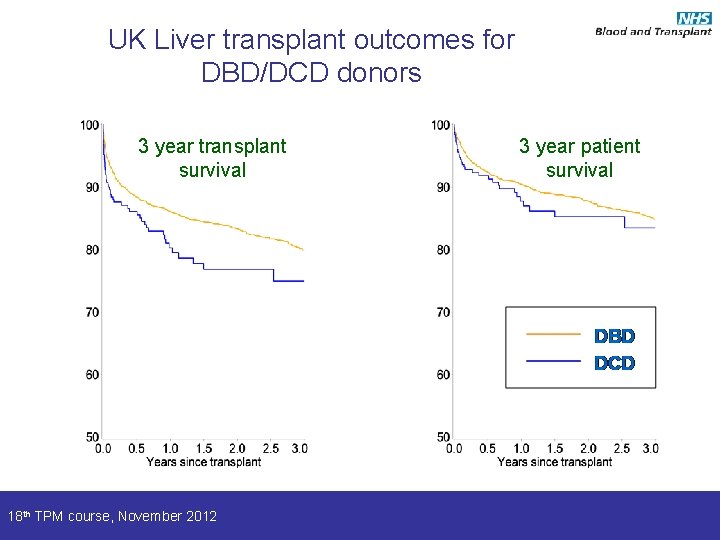
UK Liver transplant outcomes for DBD/DCD donors 3 year transplant survival 18 th TPM course, November 2012 3 year patient survival

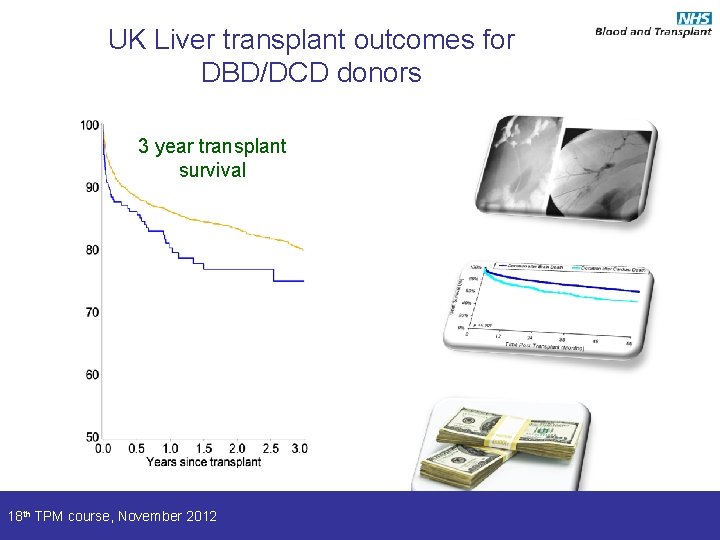
UK Liver transplant outcomes for DBD/DCD donors 3 year transplant survival 18 th TPM course, November 2012

Summary • MC 3 DCD requires – modification to end of life care – organ retrieval to begin within minutes of diagnosis of death – considerable commitment from retrieval teams • There anxieties over ischaemic injury – outcomes for kidney transplantation are acceptable – Interest in restoring circulation soon after death • MC 3 DCD accounts for almost all the increase in deceased donation in the UK over last 5 years 18 th TPM course, November 2012