Lymphoma Thyroid Unni krishnan R 2002 batch MBBS

Lymphoma Thyroid Unni krishnan. R 2002 batch MBBS

Introduction • Primary thyroid lymphoma can be defined as a lymphoma that arises from the thyroid gland. • Excludes lymphomas that invade thyroid gland because of either metastasis or direct extension from an adjacent lymph node

• Contributes for about 1% of thyroid malignancies. • Most of the primary leisions are non hodgkins Bcell type.

Pathophysiology • Frequently associated with Hashimoto thyroiditis, • Pathogenetic link exists between this autoimmune disorder and thyroid NHL (Holm, 1985). • Hypothyroidism has been observed in 3040% of patients with thyroid lymphoma.
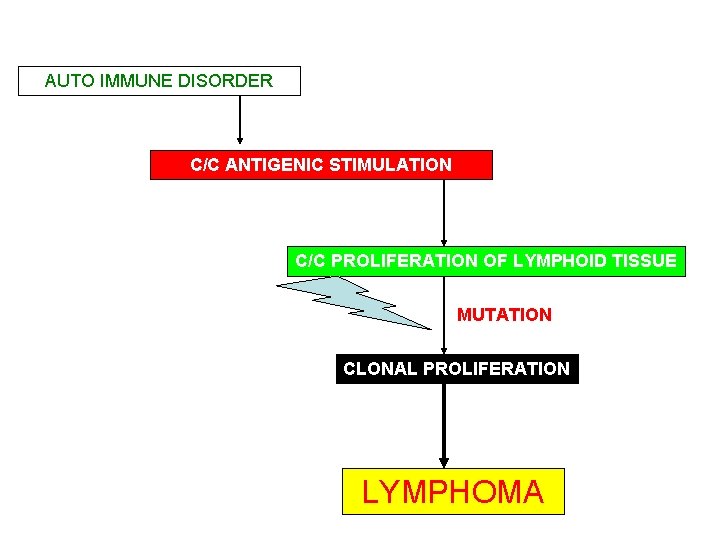
AUTO IMMUNE DISORDER C/C ANTIGENIC STIMULATION C/C PROLIFERATION OF LYMPHOID TISSUE MUTATION CLONAL PROLIFERATION LYMPHOMA
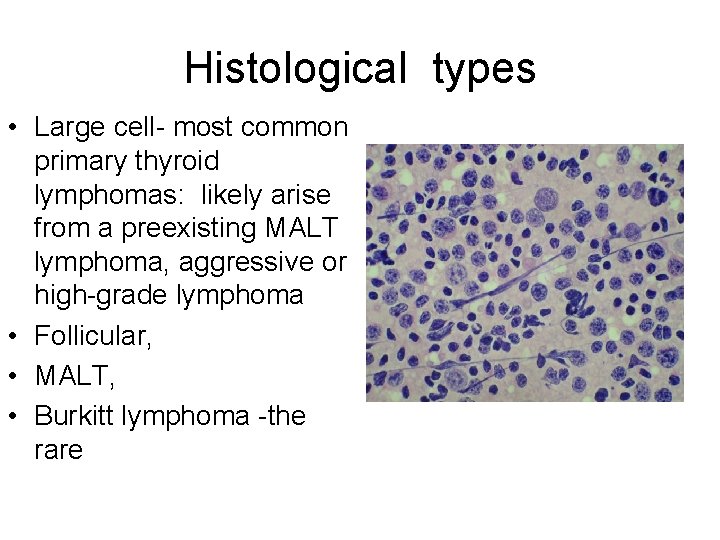
Histological types • Large cell- most common primary thyroid lymphomas: likely arise from a preexisting MALT lymphoma, aggressive or high-grade lymphoma • Follicular, • MALT, • Burkitt lymphoma -the rare

IMPORTANT Although thyroid NHL is not common, it is highly curable without extensive surgery; for this reason, it should be recognized early and treated correctly.
Clinical features • History – more in women – median age of 60 yrs – rapidly enlarging neck mass – frequently in association with neck adenopathy – Hoarseness, respiratory difficulty, cough, and dysphagia
Clinical features • Physical – neck mass – Cervical lymphadenopathy – Pressure signs
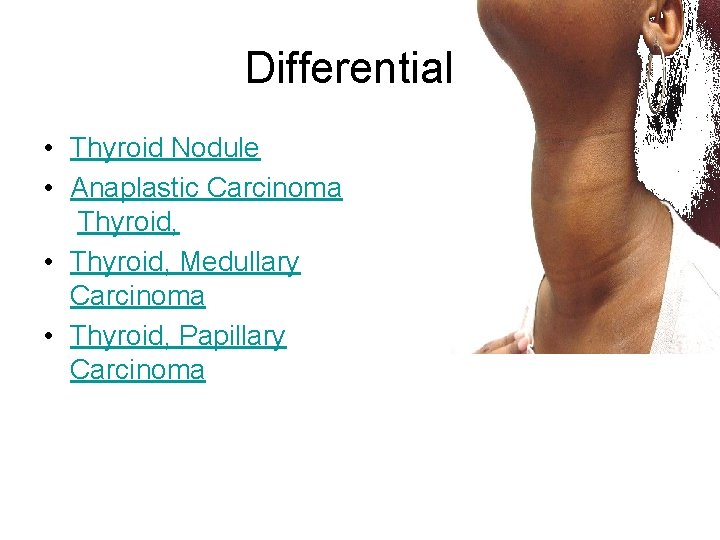
Differentials • Thyroid Nodule • Anaplastic Carcinoma Thyroid, • Thyroid, Medullary Carcinoma • Thyroid, Papillary Carcinoma

Lab work up • FNAC/ CORE BIOPSY: avoids extensive surgeries. • Larger specimen is desirable to ensure that the sample is representative and that divergent histology is not missed

Lab work up • Immunophenotyping – NHL should be easy to distinguish from thyroid carcinoma. – distinction between large-cell lymphoma and follicular center cell lymphoma is possible

Lab work up – CBC count: CBC count and bone marrow important for the staging. – Serum LDH and beta 2 -microglobulin values are indicative of the prognosis – Thyroid function tests: the high incidence of hypothyroidism. – Antithyroglobulin or antimicrosomal antibodies
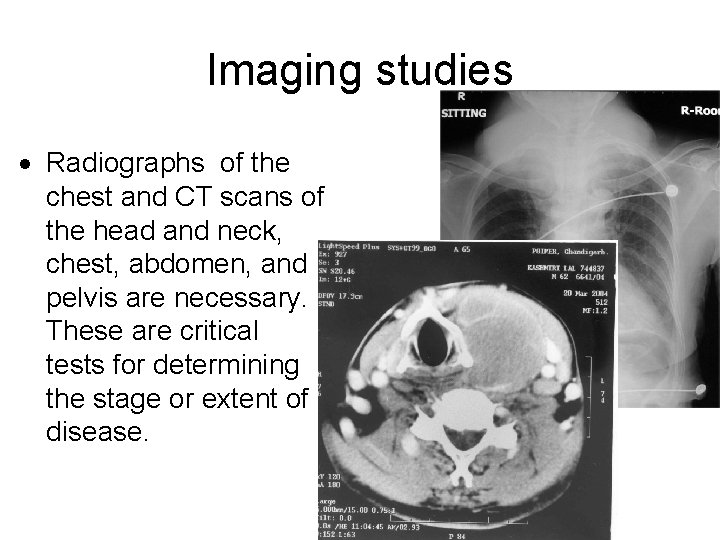
Imaging studies Radiographs of the chest and CT scans of the head and neck, chest, abdomen, and pelvis are necessary. These are critical tests for determining the stage or extent of disease.

Imaging studies • Gallium scanning or positron emission tomography (PET) in patients with bulky disease because these can help in determining if any residual abnormality observed on post treatment radiographs contains active lymphoma or scar tissue • In patients with MALT lymphoma of the thyroid, PET scans should be interpreted cautiously because this subtype can give rise to falsenegative results because of low metabolic rate

Imaging studies • The presence of an inflammatory condition, such as Hashimoto thyroiditis, can result in a false-positive PET scan. The amount of uptake, as measured by the standard uptake value (SUV), tends to be low in inflammatory conditions (SUV <6) and higher in large-cell lymphomas

Staging • Determines the prognosis and treatment. • Only the early Ann Arbor stages (i. e. , I-II) can be considered as primary thyroid in origin, causing a conceptual problem. This is because advanced presentations can represent metastatic lymphoma to the thyroid rather than primary lymphoma in the thyroid

The conceptual problem • Primary thyroid lymphomas have metastatic potential and can present with stage III-IV disease; however, because no histologic marker separate primary thyroid lymphomas metastatic thyroid lymphomas, most series include only stage I-II cases (by definition).

• International Prognostic Index (IPI) This prognostic system assigns 1 point to each of the following variables: – Age older than 60 years – Performance status higher than 1 – Elevated LDH – Number of extra nodal sites more than 1 – Ann Arbor stage III-IV

• The 5 -year survival rate for patients with an IPI of 0 was 86% versus 50% for patients with an IPI of greater than 0. (International Non Hodgkin's Lymphoma Prognostic Factors Project, 1993).
TREATMENT • Medical Care: Treatment is based on the lymphoma subtype and the extent of disease

• Chemo therapy – CHOP REGIME • • VINCRISTIENE DOXORUBICIN CYCLOPHOSPHOMIDE PREDNISOLONE
• Radiation therapy is most commonly given after 3 -6 courses of chemotherapy.

• MALT lymphomas – Local treatment with radiation therapy appears to be adequate (Laing, 1994). – Intermediate - or high-grade lymphoma arising from MALT lymphoma appear to have the worst prognoses, and these patients need aggressive treatment with combined-modality therapy.

• Relapsed thyroid lymphomas – High -dose chemotherapy with autologous stem-cell transplantation is considered the treatment of choice. – Before the use of high-dose chemotherapy, a conventional dose-salvage regimen (eg, one containing Ara-C and platinum or ifosfamide and VP 16) is administered, usually for 1 -2 courses. This step is typically followed by mobilization of peripheral blood stem cells with the same or another chemotherapeutic regimen. After adequate numbers of autologous hematopoietic stem cells are collected, patients receive high-dose chemotherapy, followed by autologous stem-cell transplantation for hematopoietic rescue.

MEDICATION • The standard CHOP regimen, followed by irradiation consolidation in patients with Ann Arbor stages I-II. Three to 6 courses of chemotherapy are administered • The combination of rituximab and CHOP improved rates of complete response, failure-free survival, and survival.

Cyclophosphamide (Cytoxan, Neosar) • Chemically related to nitrogen mustards. Alkylating agent; mechanism of action of active metabolites may involve crosslinking of DNA, which may interfere with growth of normal and neoplastic cells. • Adult Dose: 750 mg/m 2 IV on day 1 of each course • Pediatric Dose: Not established

• Contraindications: – Documented hypersensitivity; – Severely depressed bone marrow function

Interactions: • Allopurinol may increase risk of bleeding or infection and enhance myelosuppressive effects; • Potentiate doxorubicin-induced cardiotoxicity; • Reduce digoxin serum levels • Reduce antimicrobial effects of quinolones; chloramphenicol • increase half-life while decreasing metabolite concentrations; • increase effect of anticoagulants; • coadministration with high doses of phenobarbital may increase rate of metabolism and leukopenic activity; • thiazide diuretics may prolong cyclophosphamide-induced leukopenia and neuromuscular blockade by inhibiting cholinesterase activity

• Pregnancy: Unsafe in pregnancy • Precautions: Regularly examine hematologic profile (particularly neutrophils and platelets) to monitor for hematopoietic suppression; regularly examine urine for RBCs, which may precede hemorrhagic cystitis

Doxorubicin (Adriamycin, Rubex) • Intercalates DNA and inhibits opoisomerase II; produces free radicals that may cause destruction of DNA and inhibit growth of neoplastic cells. • Adult Dose: 50 mg/m 2 IV on day 1 of each course • Pediatric Dose: Not established

• Contraindications: Documented hypersensitivity; severe heart failure, cardiomyopathy, impaired cardiac function, preexisting myelosuppression

• Interactions May decrease phenytoin and digoxin plasma levels; phenobarbital may decrease plasma levels; cyclosporine may induce coma or seizures; mercaptopurine increases toxicity; cyclophosphamide increases cardiac toxicity • Pregnancy: Unsafe in pregnancy • Precautions: Can cause birth defects particularly when administered during first trimester of pregnancy

Vincristine (Oncovin, Vincasar VFS) • Mechanism of action is uncertain. May involve decrease in reticulo endothelial cell function or increase in platelet production. • Adult Dose: 1. 4 mg/m 2 IV on day 1 of each course • Pediatric. Dose: Not established • Contraindications: Hypersensitivity

• Interactions: Acute pulmonary reaction may occur when taken concurrently with mitomycin-C • Pregnancy - Unsafe in pregnancy • Precautions: Caution in severe cardiopulmonary or hepatic impairment and preexisting neuromuscular disease; can cause birth defects particularly when administered during first trimester of pregnancy

Prednisone (Deltasone, Meticorten, Orasone, Sterapred) • Immunosuppressant for treatment of autoimmune disorders. May decrease inflammation by reversing increased capillary permeability and suppressing PMN activity • Adult Dose: 100 mg PO on days 1 -5 of CHOP • Pediatric Dose: Not established

• Contraindications: – Documented hypersensitivity; – Viral infection, – Peptic ulcer disease, – Hepatic dysfunction, – connective tissue infections, – fungal or tubercular skin infections; – GI disease

• Interactions: Coadministration with estrogens may decrease clearance; concurrent use with digoxin may cause digitalis toxicity due to hypokalemia; phenobarbital, phenytoin, and rifampin may increase metabolism of glucocorticoids (consider increasing maintenance dose); monitor for hypokalemia with coadministered diuretics • Pregnancy. B - Usually safe but benefits must outweigh the risks.

Precautions: – Abrupt discontinuation of glucocorticoids may cause adrenal crisis; hyperglycemia, edema, osteonecrosis, myopathy, peptic ulcer disease, hypokalemia, osteoporosis, euphoria, psychosis, myasthenia gravis, growth suppression, and infections may occur with glucocorticoid use

Rituximab (Rituxan) • Genetically engineered chimeric murine/human monoclonal antibody against CD 20 antigen on surface of normal and malignant B-lymphocytes. Antibody is Ig. G 1 kappa immunoglobulin. • **Not to be administered as IV bolus

• Adult Dose: 375 mg/m 2 on day 1 of CHOP • Pediatric Dose: Not established • Contraindications: Documented hypersensitivity • Interactions: None reported

• Pregnancy - Safety for use during pregnancy has not been established. • Precautions: Caution in preexisting cardiac conditions; regularly obtain CBC during therapy and more frequently if cytopenia develops

Follow up • See patients approximately every 3 months during the first year and every 4 months during the second year.

Follow up – After the second year, the risk of relapse diminishes substantially for patients with tumors of the large-cell (ie, aggressive) types. – In contrast, the risk of recurrence for the indolent lymphoma types (ie, low-grade variants), does not decline as sharply after 2 years of observation

Follow up • After 3 years of follow-up, the probability of cure in a patient with diffuse large-cell lymphoma is more than 90%.

Complications: • Complications are usually related to adverse effects (eg, myelosuppression) of chemotherapy, which can be associated with infections or bleeding. • Radiation therapy can induce xerostomia, depending on the fields used.

Prognosis: • The prognosis for patients with thyroid large-cell lymphoma usually is favorable because this condition typically presents with localized disease, which is amenable to treatment with chemotherapy and radiation. • The cure rate is usually high.

What I just wanted to say…. • Medullary carcinoma arises from para follicular cells • Occurs in familial & Sporadic forms • Familial form is associated with MEN • Characteristic histologic finding is prresence of amyloid

• Metastasis to local lymph nodes lungs, liver and bone. • Treatment option is mainly surgical. Total thyriodectomy combined with or without modified radical neck dissection is performed

Lymphoma thyroid • • Lymphoma arising from the gland Auto immune etiology is associated CHOP regime is the mainstay of treatment. Surgical treatment is aimed at alleviating pressure symptoms

BIBLIOGRAPHY BAILEY & LOVE SABISTON’S TEXT BOOK OF SURGERY SCHWARTZ www. emedicine. com www. radiologyreferance. com www. mdconsult. com

Acknowledgement Dr. SUMIT S MALIK Dr. GIREESHAN Mr. KURIAN Mr. DIPIN Mr. JACOB Mr. AARIF

- Slides: 53