Lymphatic and Immune Systems Maintain fluid balance Protect
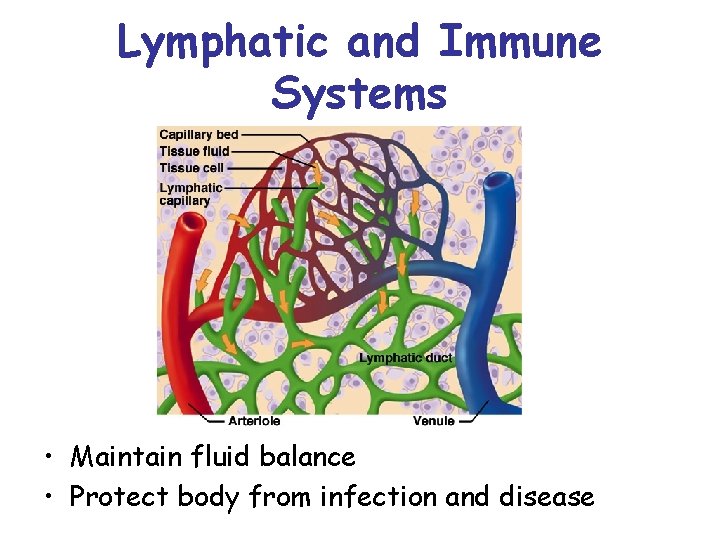
Lymphatic and Immune Systems • Maintain fluid balance • Protect body from infection and disease
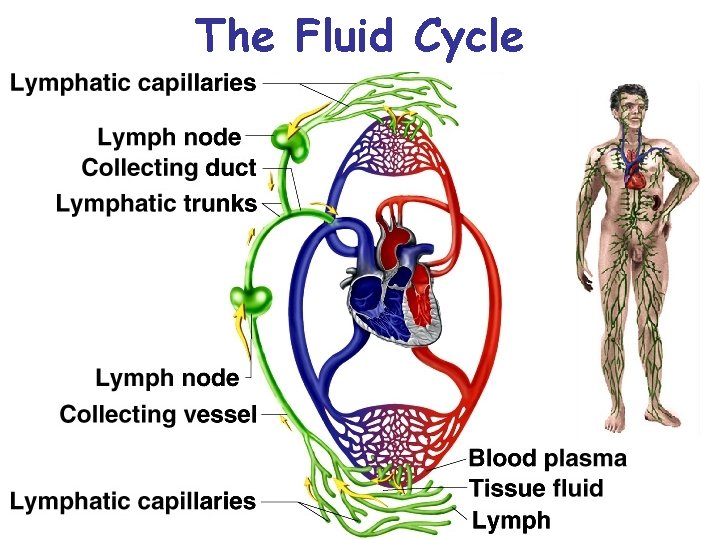
The Fluid Cycle

Lymphatic Cells • T lymphocytes – Mature in thymus • B lymphocytes – Activation causes proliferation and differentiation into plasma cells that produce antibodies • Antigen Presenting Cells – Macrophages (from monocytes) – Dendritic cells (in epidermis, mucous membranes and lymphatic organs) – Reticular cells (also contribute to stroma of lymph organs)

The Body’s Defenses The vertebrate body posses two mechanisms which protect it from potentially dangerous viruses, bacteria, other pathogens, and abnormal cells which could develop into cancer.

Two Mechanisms for Protection: 1. Nonspecific – does not distinguish between infective agents. 2. Specific – responds in a very specific manner to the particular type of infective agent (i. e. , production of antibodies)

The Skin and Mucous Membranes • Act as physical barriers preventing entry of pathogens, and as chemical barriers of antipathogen secretions. - Oil and sweat gland secretions – acidify the skin - Normal bacteria flora may release acids and other metabolic wastes - Saliva, tears, mucous secretions – antimicrobial proteins; also wash away invading microbes - Lysozyme – tears, saliva, perspiration – attacks cell walls of bacteria - Respiratory – nostril hairs, mucous, ciliated cells - Digestive – stomach acid

Phagocytic WBCs and Natural Killer Cells • Microbes that penetrate the skin or mucous membranes encounter amoeboid WBCs capable of phagocytosis or cell lysis: 1. Neutrophils – 60 -70% of total WBCs -Attracted by chemical signals -Enter infected tissues by amoeboid movement -Only live a few days
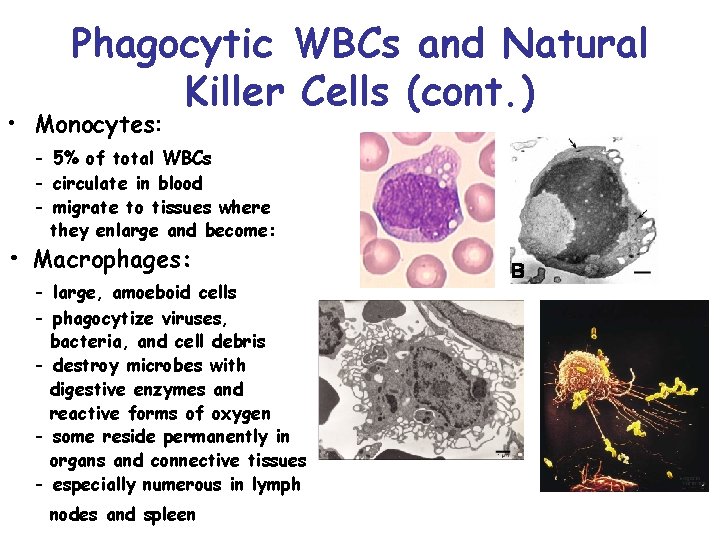
Phagocytic WBCs and Natural Killer Cells (cont. ) • Monocytes: - 5% of total WBCs - circulate in blood - migrate to tissues where they enlarge and become: • Macrophages: - large, amoeboid cells - phagocytize viruses, bacteria, and cell debris - destroy microbes with digestive enzymes and reactive forms of oxygen - some reside permanently in organs and connective tissues - especially numerous in lymph nodes and spleen
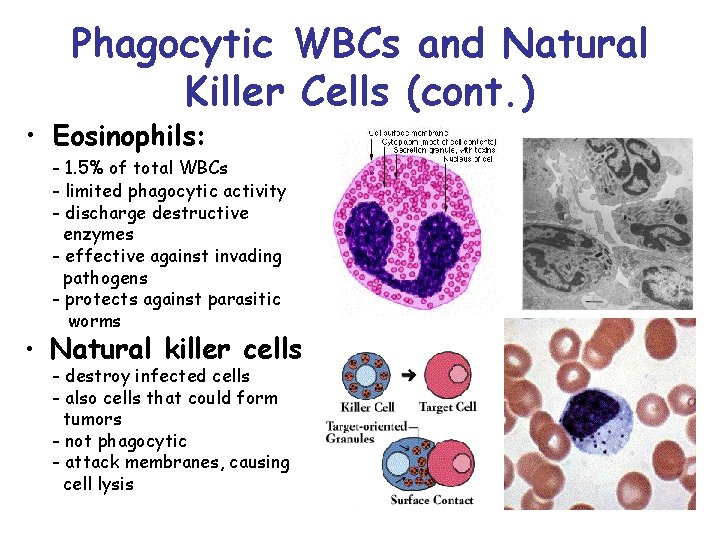
Phagocytic WBCs and Natural Killer Cells (cont. ) • Eosinophils: - 1. 5% of total WBCs - limited phagocytic activity - discharge destructive enzymes - effective against invading pathogens - protects against parasitic worms • Natural killer cells - destroy infected cells - also cells that could form tumors - not phagocytic - attack membranes, causing cell lysis
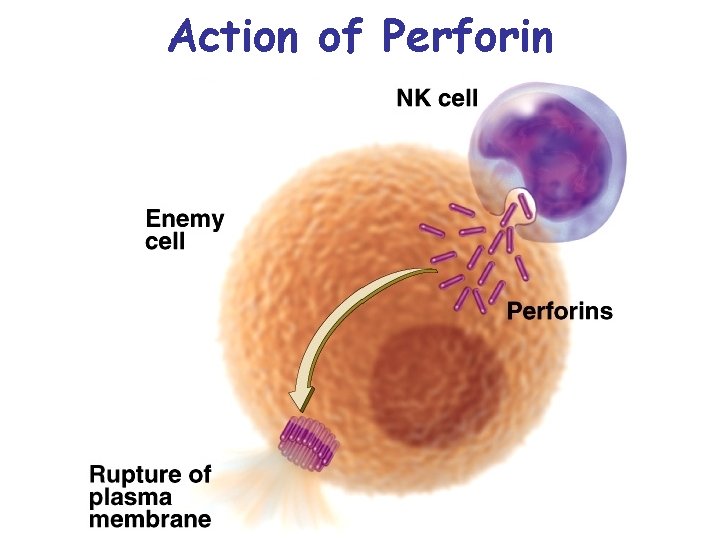
Action of Perforin
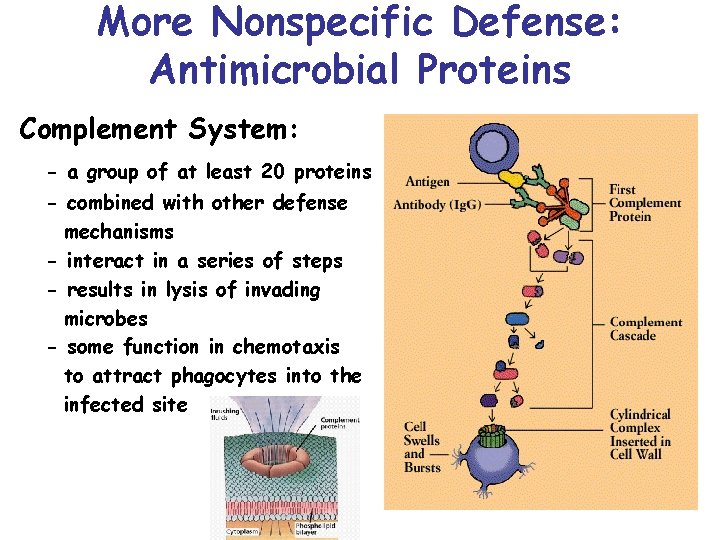
More Nonspecific Defense: Antimicrobial Proteins Complement System: - a group of at least 20 proteins - combined with other defense mechanisms - interact in a series of steps - results in lysis of invading microbes - some function in chemotaxis to attract phagocytes into the infected site

Other Antimicrobial Proteins: • Interferons: - produced and secreted by virus-infected cells - nonspecific defense before the production of antibodies stimulates production of proteins that inhibit viral replication gamma interferon activates phagocytes not virus specific most effective against short-term infections (colds, flu)
The Inflammatory Response • • Localized, nonspecific Occurs after tissue damage or entry of microorganisms Vasodilation – to increase BF to the area (redness) BVs become more permeable - allow fluids to leak into surrounding tissues (swelling ) - migration of phagocytic cells into the injured area • Initiated by chemical signals – histamine (mast cells), prostaglandins (WBCs)
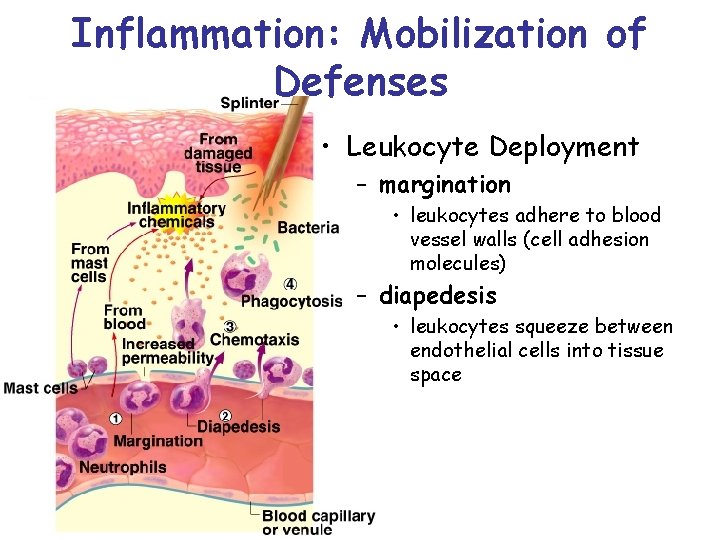
Inflammation: Mobilization of Defenses • Leukocyte Deployment – margination • leukocytes adhere to blood vessel walls (cell adhesion molecules) – diapedesis • leukocytes squeeze between endothelial cells into tissue space

Containment and Destruction of Pathogens • Fibrinogen now in tissue clots, trapping microbes • Heparin prevents clotting at site of injury – pathogens trapped in a fluid pocket surrounded by clot • Chemotaxis – leukocytes are attracted to inflammatory chemicals • Neutrophils are quickest to respond – phagocytosis – respiratory burst – rapid release of reactive oxygen sp. – secrete cytokines for recruitment of macrophages and T cells cytokines = small proteins or glycoproteins used in organisms as signaling compounds.
Tissue Cleanup • Monocytes are the primary agents of cleanup arrive in 8 to 12 hours, become macrophages • Edema - venous flow, lymphatic flow - removal of bacteria and debris • Formation of pus – mixture of tissue fluid, cellular debris, dying neutrophils and microbes
Tissue Repair • Platelets and endothelial cells in injured area secrete a cytokine, platelet derived growth factor (PDGF) - stimulates fibroblasts to multiply and synthesize collagen • Hyperemia (↑BF) provides materials needed and heat that increases metabolism • Fibrin clot may provide a scaffold for repair • Pain limits use of body part allowing for repair


Fever • Defense mechanism: good in most cases – promotes interferon activity – accelerates metabolic rate and tissue repair – inhibits pathogen reproduction • Interleukin 1 (a cytokine) is a pyrogen – secreted by macrophages – stimulates anterior hypothalamus to secrete PGE (a prostaglandin) – resets body thermostat higher Ø 105 F may cause delirium Ø 111 F- 115 F, coma-death • Stages of fever – onset, stadium, defervescence
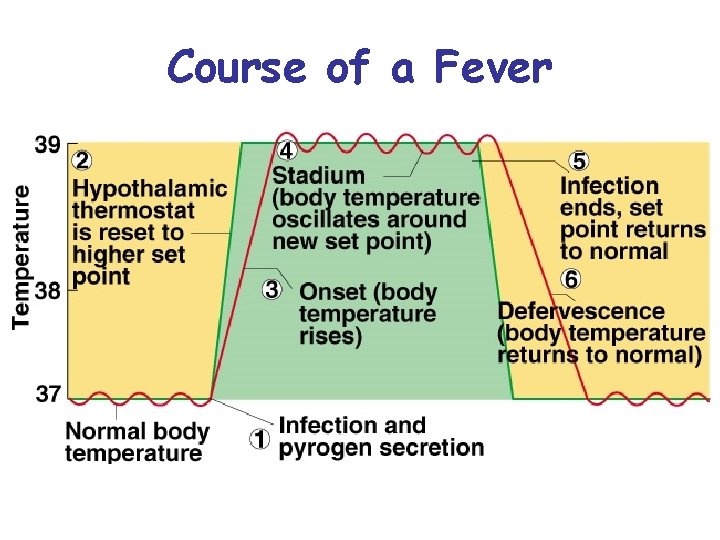
Course of a Fever

Characteristics of Specific Immunity • Specificity - antigen/antibody • Diversity - wide variety of lymphocytes - each population stimulated by a specific antigen - synthesize and secrete the appropriate antibody • Memory - ability to recognize previously encountered antigens - react faster to subsequent exposures - acquired immunity - resistance to some infections encountered early in life • Self/nonself recognition

Humoral vs. Cell-mediated Immunity • Humoral immunity - production of antibodies in response to toxins, bacteria, and viruses present in tissue fluids - synthesized by B lymphocytes - soluble proteins - circulate throughout the body in blood plasma and lymph • Cell-mediated immunity - response to intracellular bacteria, viruses, fungi, protozoans, worms, transplanted tissues, and cancer cells - depends on direct action of certain types of lymphocytes rather than antibodies

Passive and Active Immunity • Natural active immunity - produces memory cells – production of one’s own antibodies or T cells as a result of infection or natural exposure to antigen • Artificial active immunity - produces memory cells – production of one’s own antibodies or T cells as a result of vaccination • Natural passive immunity - through placenta, milk – temporary, fetus acquires antibodies from mother • Artificial passive immunity - emergency treatment for snakebite, rabies, tetanus – temporary - injection of immune serum (antibodies)

Antigens • Trigger an immune response • Complex molecules – proteins, polysaccharides, glycoproteins, glycolipids • Antigenic determinants – stimulate immune responses
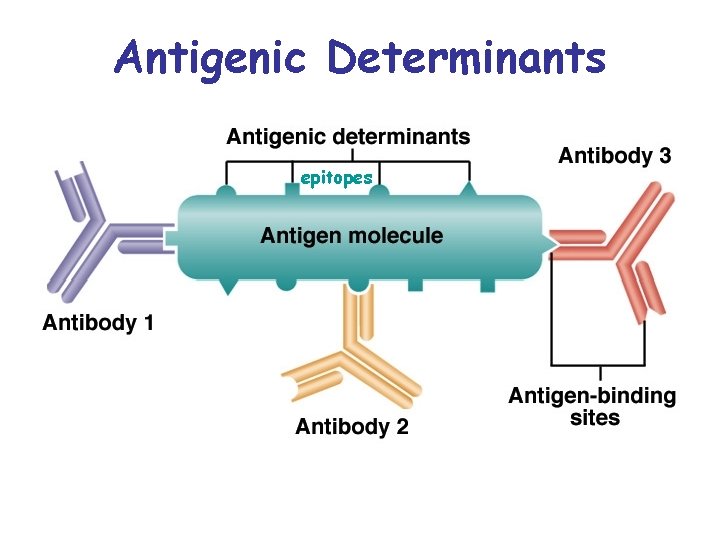
Antigenic Determinants epitopes

Cells of the Immune System Lymphocytes • Responsible for both cell-mediated and humoral immunity • Develop from multipotent cells in the bone marrow - B cells – humoral response – mature in bone marrow - T cells – cell-mediated response – mature in thymus • Concentrated in lymph nodes, spleen, and other lymphatic organs - most likely to contact antigens • Antigen receptors on surface - B cells – receptors are membrane bound antibodies - T cells – receptors are proteins embedded in the membrane

Cells of the Immune System T Lymphocytes (green): - - T cells are then immunocompetent - capable of recognizing antigens presented by APCs - Positive selection of T cells - form clones of identical T cells - each clone responds to a specific antigen
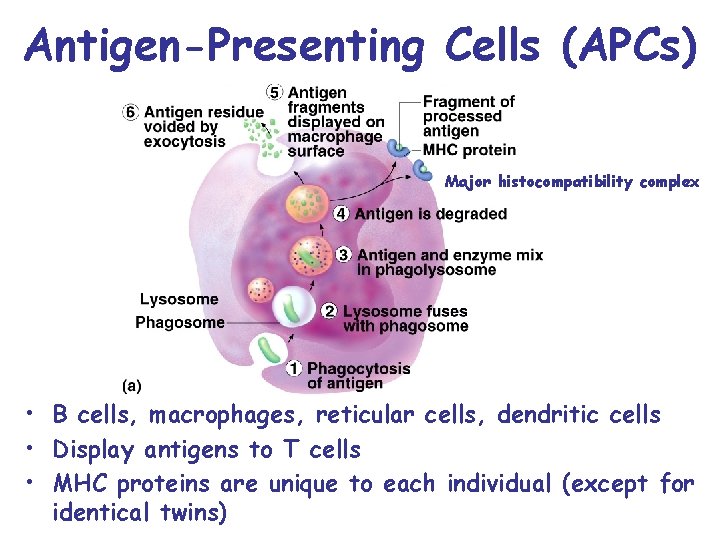
Antigen-Presenting Cells (APCs) Major histocompatibility complex • B cells, macrophages, reticular cells, dendritic cells • Display antigens to T cells • MHC proteins are unique to each individual (except for identical twins)

Antigen Presenting Cells • Internalize antigen by endocytosis • Digest antigen into fragments (antigen processing) • Wandering T cells regularly inspect APCs for displayed antigens • If MHC protein carries a non-self antigen, T cells initiate an attack

B Lymphocytes (B cells) • B cell selection 1. Should not bind to MHC on self cells (not cell mediated) 2. Should also not react to self antigens • Selected cells form B cell clones – synthesize antigen receptors, divide rapidly, produce immunocompetent clones

Interleukins • Hormone-like messengers between leukocytes • Lymphokines: produced by lymphocytes -Example: IL-2 – secreted by T cells after antigen binding - stimulates growth, differentiation, of antigen-selected cytotoxic T cells (memory) -Example: IL-3 – secreted by T cells -stimulates bone marrow stem cells

Cellular Immunity • • 1. 2. 3. 4. T lymphocytes attack and destroy foreign cells and diseased host cells Involves 4 classes of T cells: Cytotoxic (killer) T cells: carry out attack Helper T cells: help promote T cell and B cell action and nonspecific defense mechanisms Suppressor T cells: limit cell mediated attack Memory T cells: provide immunity from future exposure to antigen
TC cell Recognition • • – Antigen presentation MHC-I proteins • • found on nearly all nucleated body cells display peptides produced by host cells TC cell activation 1. Binding of cytotoxic T cells (CD 8 cells) to abnormal peptides on MHC-I and 2. Co-stimulation via a cytokine (interleukin) released by activated helper T cells (CD 4 cells) – Triggers clonal selection -clone of identical T cells against cells with same epitope

TH cell Recognition • Antigen presentation – MHC-II proteins • found only on antigen presenting cells (ex: macrophages) • stimulate helper T cells (CD 4 cells) • TH cell activation 1. Binding of helper T cells (CD 4 cells) to abnormal peptides on MHC-II and 2. Co-stimulation via a cytokine (interleukin) from the infected cell • attracts neutrophils and natural killer cells • attracts macrophages and stimulates their phagocytic activity • inhibit macrophages from leaving the area • stimulate T and B cell mitosis and maturation
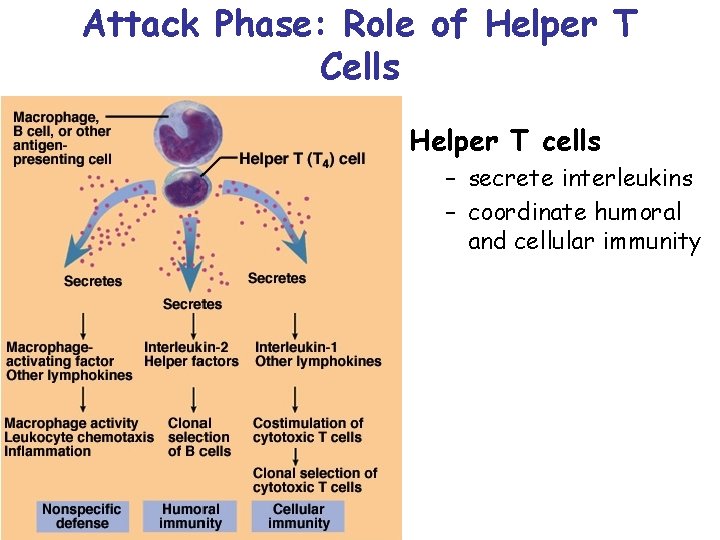
Attack Phase: Role of Helper T Cells Helper T cells – secrete interleukins – coordinate humoral and cellular immunity
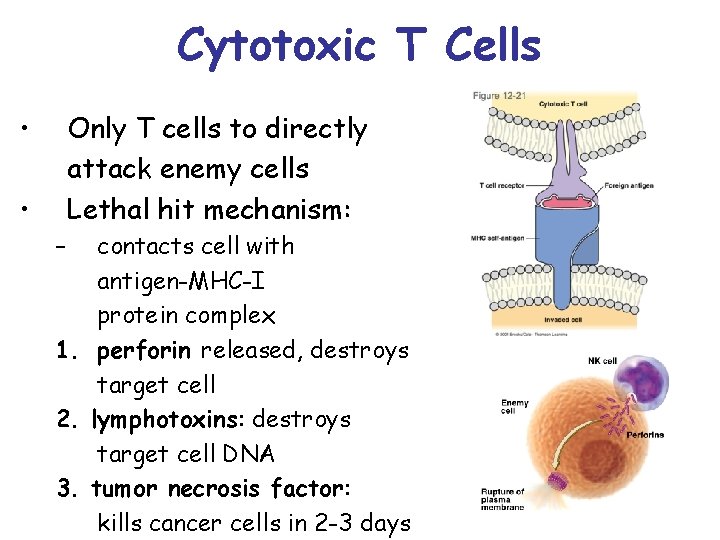
Cytotoxic T Cells • Only T cells to directly attack enemy cells Lethal hit mechanism: • – contacts cell with antigen-MHC-I protein complex 1. perforin released, destroys target cell 2. lymphotoxins: destroys target cell DNA 3. tumor necrosis factor: kills cancer cells in 2 -3 days
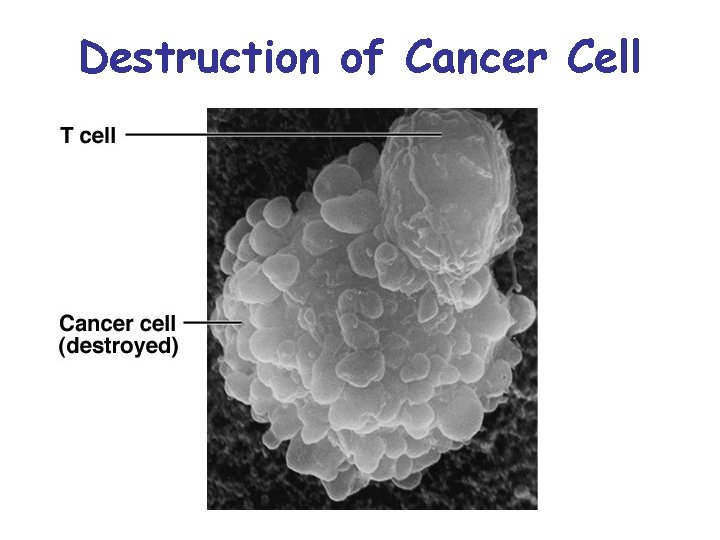
Destruction of Cancer Cell

Suppressor T Cells • As pathogen disappears, supressor T cells slow down immune reaction - Secrete interleukins that inhibit B and T cell activity • May help prevent autoimmune diseases

Memory • Memory T cells – following clonal selection some T cells become memory cells • T cell recall response – upon reexposure to same pathogen, memory cells launch a quick attack

Humoral Immunity • Recognition – B cell receptors bind antigen, take in and digest antigen then display epitopes on its MHC-II protein – After costimulation by TH cell, they divide repeatedly, differentiate into plasma cells, and produce antibodies specific to that antigen • Attack – antibodies bind to antigen, render it harmless, ‘tag it’ for destruction • Memory – some B cells differentiate into memory cells
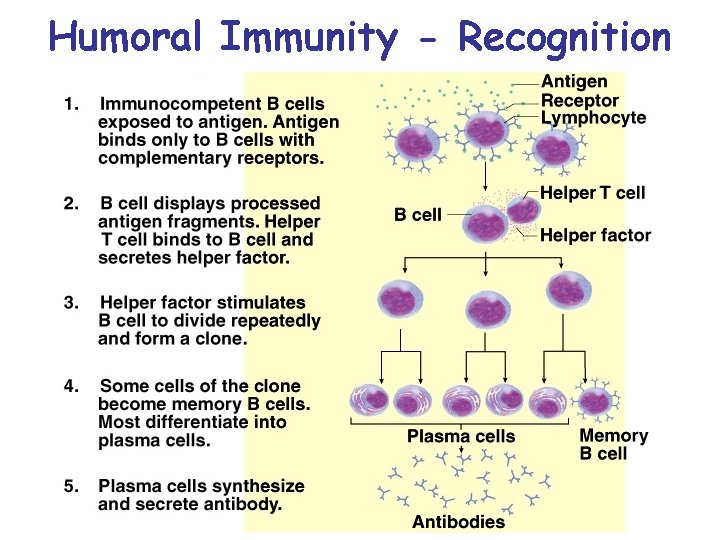
Humoral Immunity - Recognition
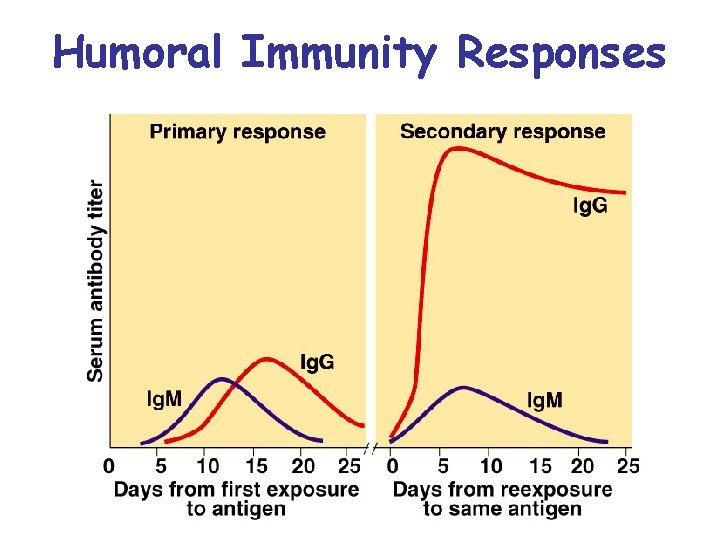
Humoral Immunity Responses

Hypersensitivity (Allergy) Excessive immune reaction against antigens that most people tolerate - allergens • Type I (immediate) hypersensitivity (most common) – anaphylaxis: occurs in sensitized people, allergen caps Ig. E on mast cells, basophils; release inflammatory chemicals, cause local edema, mucous hypersecretion, congestion; hives, watery eyes, runny nose are typical • Asthma (most common chronic illness in children) – inhaled allergens, histamines, bronchiole constriction • Anaphylactic shock: bronchiolar constriction, dyspnea, vasodilation, shock, death; treatment- epinephrine
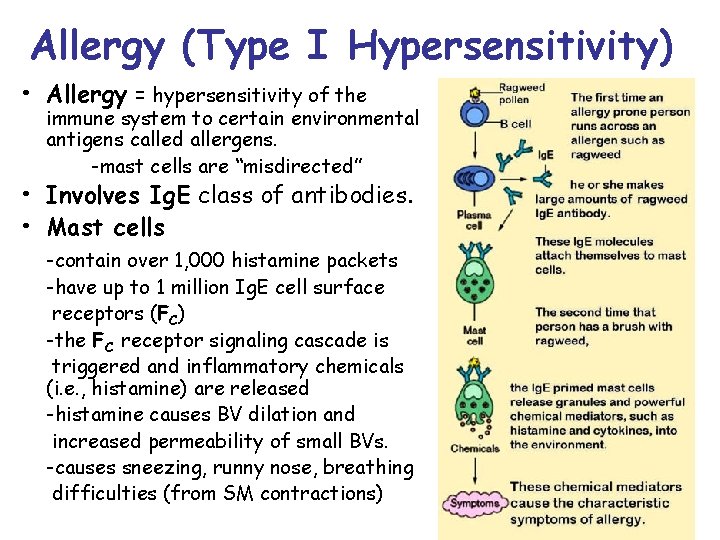
Allergy (Type I Hypersensitivity) • Allergy = hypersensitivity of the immune system to certain environmental antigens called allergens. -mast cells are “misdirected” • Involves Ig. E class of antibodies. • Mast cells -contain over 1, 000 histamine packets -have up to 1 million Ig. E cell surface receptors (FC) -the FC receptor signaling cascade is triggered and inflammatory chemicals (i. e. , histamine) are released -histamine causes BV dilation and increased permeability of small BVs. -causes sneezing, runny nose, breathing difficulties (from SM contractions)

Anaphylactic Shock • Most serious type of allergic reaction (lifethreatening) • Mast cell degranulation triggers an abrupt dilation of peripheral BVs – causes a precipitous drop in BP • Death may occur within a few minutes • Ex: hypersensitivity to bee or wasp stings, peanut allergies • Epi-pen = epinephrine to counteract the immune response.
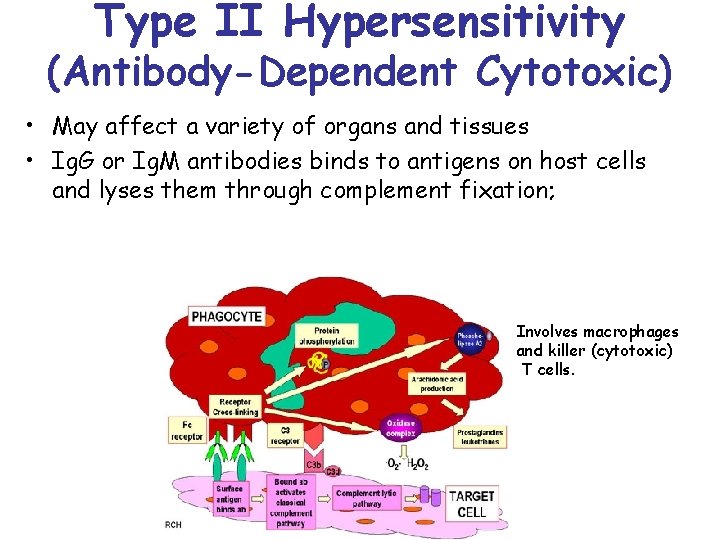
Type II Hypersensitivity (Antibody-Dependent Cytotoxic) • May affect a variety of organs and tissues • Ig. G or Ig. M antibodies binds to antigens on host cells and lyses them through complement fixation; Involves macrophages and killer (cytotoxic) T cells.
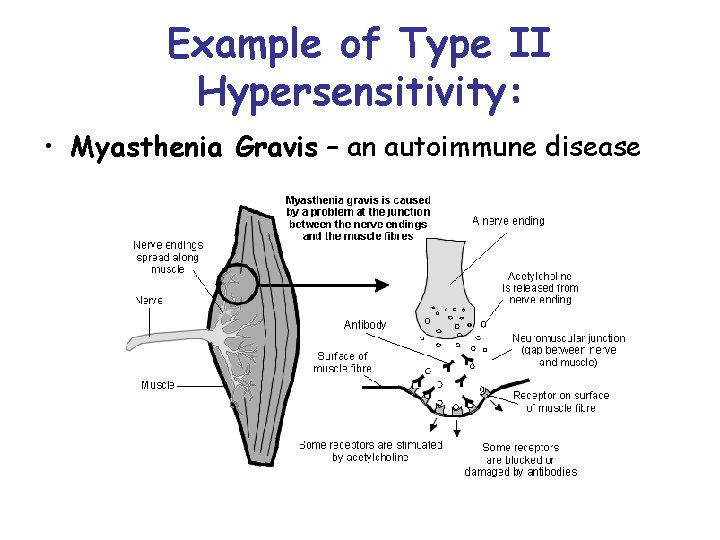
Example of Type II Hypersensitivity: • Myasthenia Gravis – an autoimmune disease
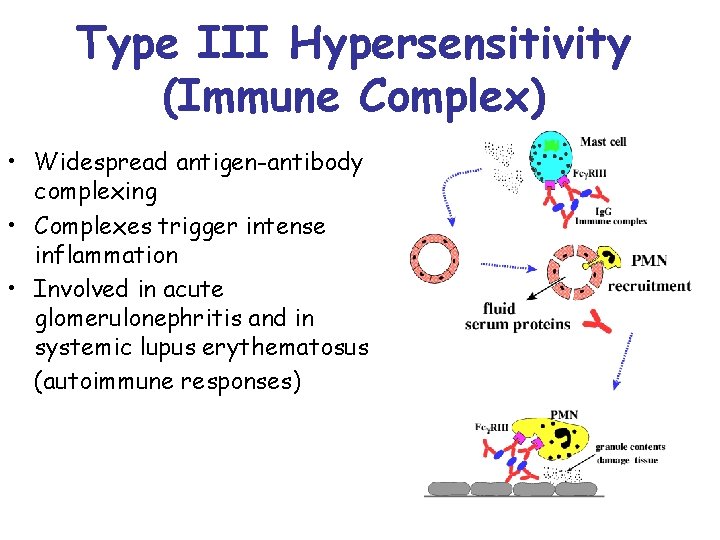
Type III Hypersensitivity (Immune Complex) • Widespread antigen-antibody complexing • Complexes trigger intense inflammation • Involved in acute glomerulonephritis and in systemic lupus erythematosus (autoimmune responses)
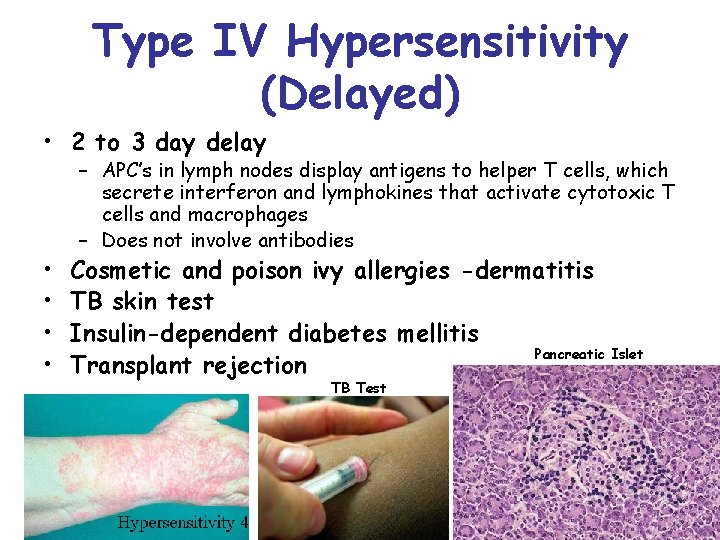
Type IV Hypersensitivity (Delayed) • 2 to 3 day delay • • – APC’s in lymph nodes display antigens to helper T cells, which secrete interferon and lymphokines that activate cytotoxic T cells and macrophages – Does not involve antibodies Cosmetic and poison ivy allergies -dermatitis TB skin test Insulin-dependent diabetes mellitis Pancreatic Islet Transplant rejection TB Test

Autoimmune Diseases • Failure of self tolerance – cross-reactivity – abnormal exposure of self-antigens – changes in structure of self-antigens • Production of autoantibodies

Autoimmune Diseases: • Systemic Lupus Erythematosus - immune reaction to nucleic acids released by the normal breakdown of skin and other tissues • Rheumatoid Arthritis - inflammation that damages the cartilage and bone of joints • Insulin-dependent diabetes mellitus - autoimmune reaction that causes the destruction of the insulin-producing cells of the pancreas • Rheumatic fever - antibodies produced in response to strep infections react with heart muscle tissue • Grave’s Disease - antibodies attach to TSH receptors on thyroid gland - stimulates oversecretion of thyroid hormones

Immunodeficiency Diseases • Severe Combined Immunodeficiency Disease – hereditary lack of T and B cells – vulnerability to opportunistic infection

Immunodeficiency Diseases • Severe combined immunodeficiency (SCID) - both humoral and cell-mediated immunity fail - genetic disease - long-term survival usually requires a bone marrow transplant • AIDS – HIV structure (next slide) – invades helper T cells, macrophages and dendritic cells by “tricking” them to internalize viruses by receptor mediated endocytosis – reverse transcriptase (retrovirus), uses viral RNA as a template to synthesize DNA, new DNA inserted into host cell DNA, may be dormant for months to years – most lethal pathogen ever encountered – 100% mortality
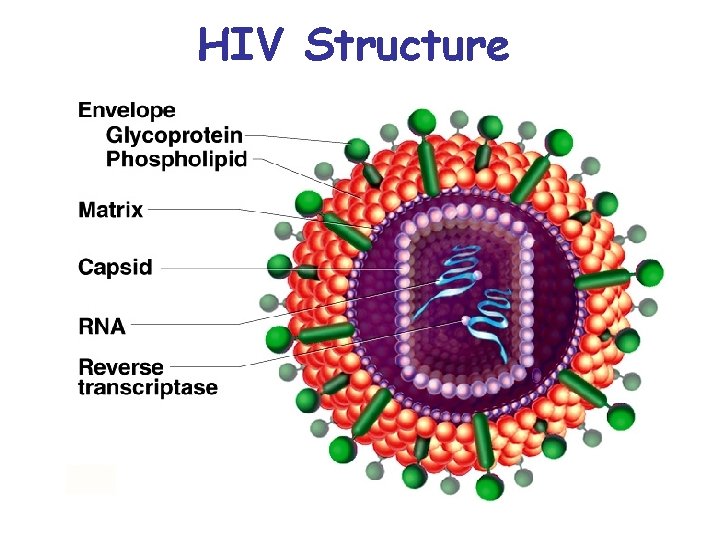
HIV Structure

AIDS Signs and symptoms: – early symptoms: flu-like chills and fever – progresses to night sweats, fatigue, headache, extreme weight loss, lymphadenitis – normal TH count is 600 to 1, 200 cells/ L of blood but in AIDS it is < 200 cells/ L • person susceptible to opportunistic infections (Toxoplasma, Pneumocystitis, herpes simplex virus, CMV or TB) – thrush: white patches on mucous membranes may appear – Kaposi sarcoma: cancer originates in endothelial cells of blood vessels causes purple lesions in skin
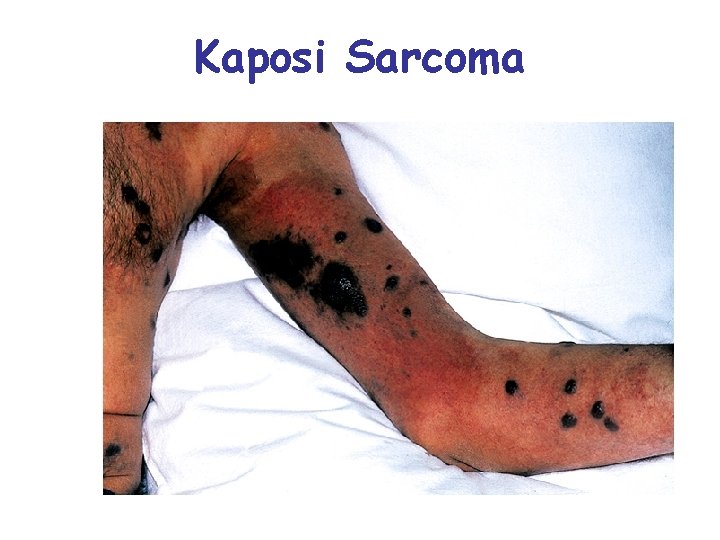
Kaposi Sarcoma

HIV Transmission • Through blood, semen, vaginal secretions, breast milk, or across the placenta • Most common means of transmission – sexual intercourse (vaginal, anal, oral) – contaminated blood products – contaminated needles • Not transmitted by casual contact • Undamaged latex condom is an effective barrier to HIV especially with the spermicide nonoxynol-9

Treatment Strategies • Prevent binding to CD 4 proteins of TH cells, disruption of reverse transcriptase action or inhibiting assembly of new viruses or their release from host cells • AZT azidothymidine inhibits reverse transcriptase – recommended for CD 4 counts below 500 cells/ L – side effects include bone marrow toxicity and anemia • Protease inhibitors: inhibit enzymes HIV needs to replicate • HIV is evolving resistance to the “triple cocktail”


- Slides: 60