Lyme Disease Authors Eng Eong Ooi BMBS Ph

Lyme Disease Author(s): Eng Eong Ooi BMBS Ph. D Academic Affiliation: Associate Professor Program in Emerging Infectious Diseases Duke-NUS Graduate Medical School Level: Basic Version No: 1. 2 Submitted: April 2012 Editors’ Review: March 2013

2 Disclaimer/Liability • The information provided in the VAP is made available in good faith and is derived from sources believed to be reliable and accurate at the time of release. • The materials presented on the VAP may include links to external Internet sites. These external information sources are outside the control of Duke-NUS. The user of the Internet links is responsible for making his or her own decision about the accuracy, reliability and correctness of the information found. • In no event shall Duke-NUS be liable for any indirect, special, incidental, or consequential damages arising out of any use of reliance of any information contained in the VAP. Nor does Duke-NUS assume any responsibility for failure or delay in updating or removing the information contained in the VAP. • Moreover, information provided on the VAP does not constitute medical advice or treatment nor should it be considered as a replacement of the patient/physician relationship or a physician’s professional judgment. Duke-NUS expressly disclaims all liability for treatment, diagnosis, decisions and actions taken or not taken in reliance upon information contained in the VAP. This work is licensed under a Creative Commons Attribution-Non. Commercial-No. Derivs 3. 0 Unported License To view a copy of this license, visit [http: //creativecommons. org/licenses/by-nc-nd/3. 0/]

3 Financial Disclosures (past 3 years) No Disclosures

4 Lyme disease - background • Physicians have recognized relapsing fevers since the time of Hippocrates – The recognition of Lyme disease as a clinical entity is a more recent event • Few other diseases are characterized by two or more episodes of fever separated by week-long period of well-being • Occurs in two forms – Louse-borne – Tick-borne

5 The agent The causative agent of Lyme disease is a spirochete • Borrelia burgdorferi in North America and also in Europe • B afzelii or B garinii are the causative agents in most cases in Europe, Russia and northern Asia • Can be visualized by dark-field or phase contrast microscopy • Light microscopy requires special stains

6 The agent • Spiral, filamentous bacterium • Infection of reservoir and vector hosts is extracellular • The endotoxins of Borrelia are lipoproteins that are potent B-cell mitogens – Not LPS

7 The vectors • Hard ticks – Ixodes genus • In North America – Ixodes scapularis and Ixodes pacificus • Ticks become infected when they feed as larvae or nymphs on infected mammals or birds • Humans are accidental hosts and commonly become infected through the bite of nymphs – Nymphs are small and hence go unnoticed – Ticks feed for several days before dropping off
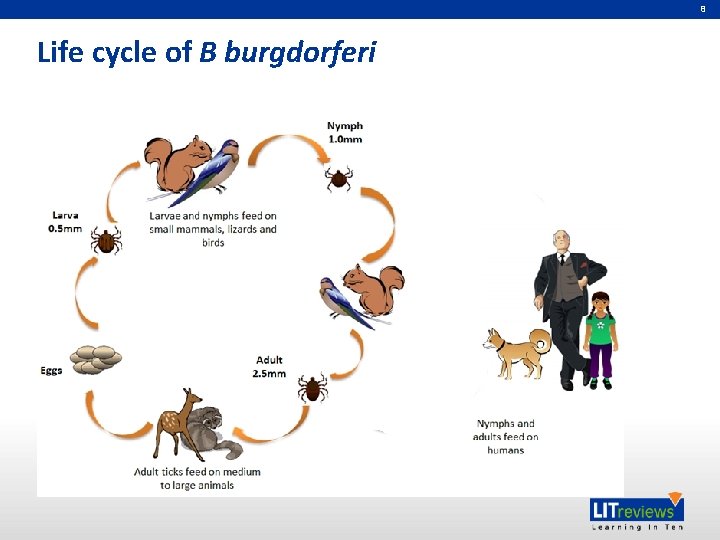
8 Life cycle of B burgdorferi

9 Epidemiology • Lyme disease occur in the following areas: – Northeastern states Virginia to Maine – North-central states Wisconsin and Minnesota – West Coast Northern California • Risk factors for Lyme disease – Outdoor activities that increase tick exposure Gardening, hunting, or hiking in an area where Lyme disease is known to occur Having a pet that may carry ticks home Walking in tall grasses

10 B burgdorferi infection 3 stages of Lyme disease • Stage 1 - early localized Lyme disease • Stage 2 - early disseminated Lyme disease • Stage 3 - late disseminated Lyme disease.
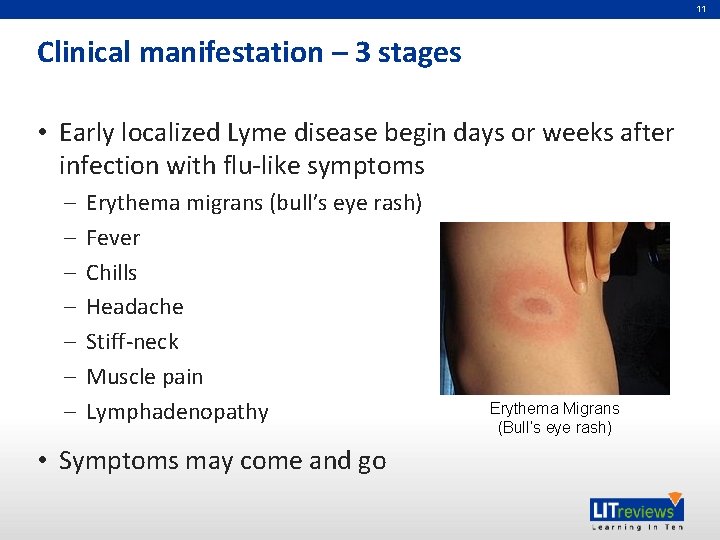
11 Clinical manifestation – 3 stages • Early localized Lyme disease begin days or weeks after infection with flu-like symptoms – – – – Erythema migrans (bull’s eye rash) Fever Chills Headache Stiff-neck Muscle pain Lymphadenopathy • Symptoms may come and go Erythema Migrans (Bull’s eye rash)

12 Symptoms • Early disseminated stage may occur weeks to months after the initial tick bite – – – Facial palsy Myalgia Pain or swelling in the knees and other large joints Cardiac arrhythmia Shooting pains that may interfere with sleep • Late disseminated stage can occur months or years after the initial infection – – – Muscle and joint inflammation (Lyme arthritis) Muscle weakness Numbness and tingling Speech problems Memory and sleep disorders

13 Diagnosis • Serological – Two-step Enzyme immunoassay/immunofluorescence assay If positive or equivocal, western blot is used to confirm infection • Most other tests are unvalidated

14 Treatment – early Lyme disease • Without neurologic manifestation or atrioventricular block) – Oral doxycycline (100 mg twice daily), amoxicillin (500 mg 3 X/day) or cefuroxime (500 mg twice daily) for 2 weeks – Macrolides not recommended • With neurologic manifestation – IV Ceftriaxone (2 g/day for 14 days) – Alternatively IV penicillin G (18 -24 million U per day) Doses shown here are for adults. See Wormser et al, Clin Infect Dis 2006; 43: 1089 -134 for more details

15 Treatment – late Lyme disease • Lyme arthritis – Oral doxycycline (100 mg twice daily), amoxicillin (500 mg 3 X/day) or cefuroxime (500 mg twice daily) for 4 weeks • Late neurologic Lyme disease – IV Ceftriaxone (2 g/day for 2 -4 weeks) Doses shown here are for adults. See Wormser et al, Clin Infect Dis 2006; 43: 1089 -134 for more details

16 Post-treatment 10 -20% of patients may have persistent or recurrent symptoms • Post-treatment Lyme disease syndrome • No well-accepted definition

Partners in Academic Medicine
- Slides: 17