LUTEAL PHASE SUPPORT IN ART AN EVIDENCE BASED

LUTEAL PHASE SUPPORT IN ART { AN EVIDENCE BASED APPROACH} DR DEEPTHI BAWA CONSULTANT IN REPRODUCTIVE MEDICINE ASTER CMI HOSPITAL BANGALORE INDIA
• Luteal phase is defined as the period between ovulation and either the establishment of a pregnancy or the onset of menstrual cycle two weeks later
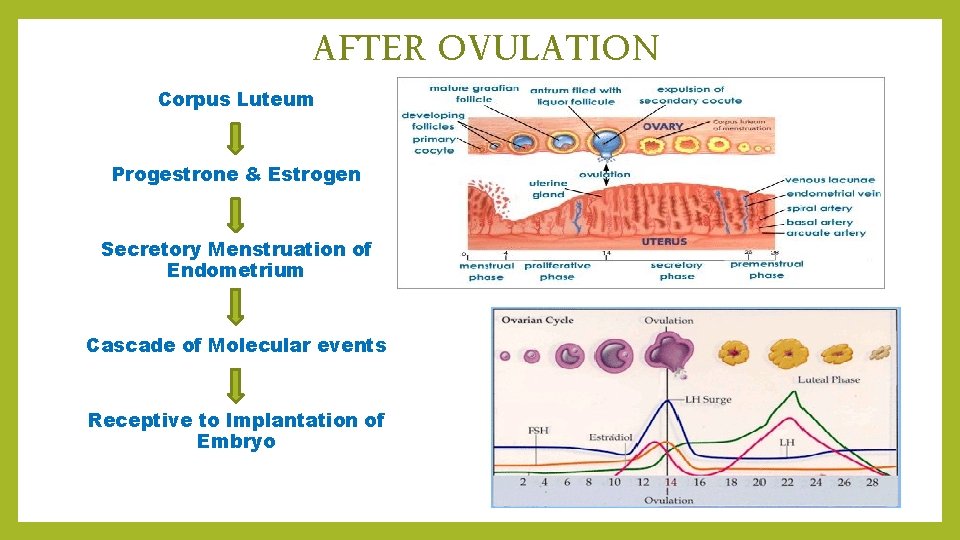
AFTER OVULATION Corpus Luteum Progestrone & Estrogen Secretory Menstruation of Endometrium Cascade of Molecular events Receptive to Implantation of Embryo
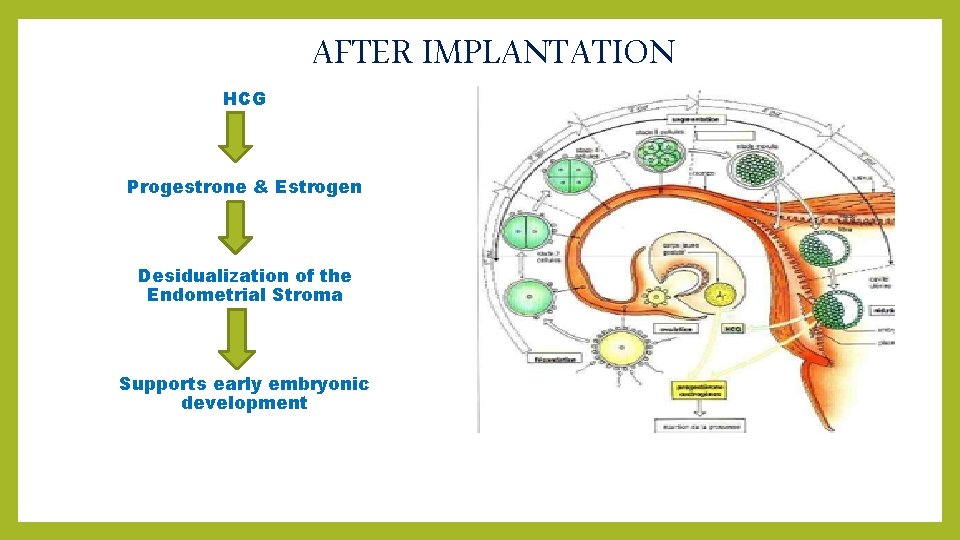
AFTER IMPLANTATION HCG Progestrone & Estrogen Desidualization of the Endometrial Stroma Supports early embryonic development
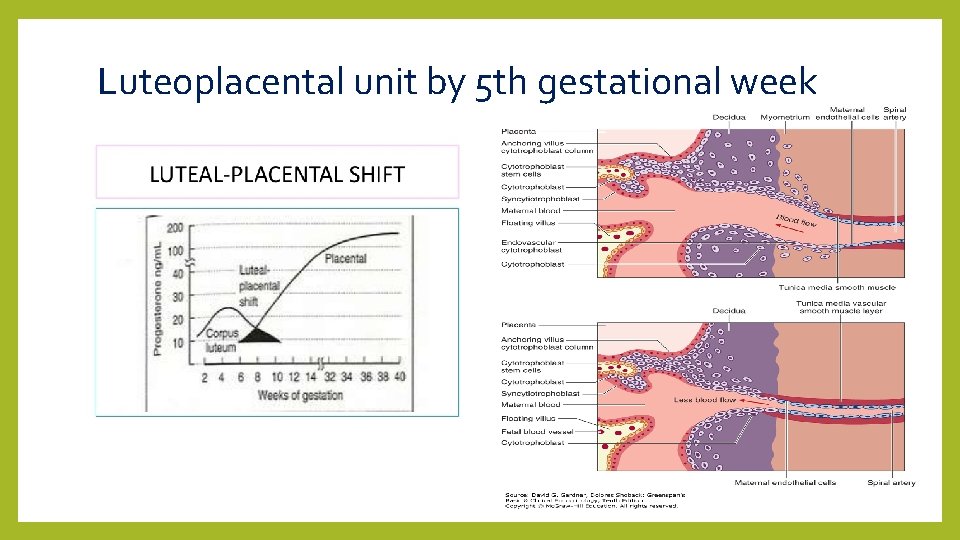
Luteoplacental unit by 5 th gestational week

Once upon a time…. . • In 1949 , the premature onset of menses was recognized as indicative of a luteal phase deficiency of progesterone production, which was shown to be correctable by exogenous progesterone administration • ( Jones , 1979 ) The prevalence of a luteal phase defect in natural cycles in normo-ovulatory patients with primary or secondary infertility was demonstrated to be about 8. 1% Rosenberg et al. , 1980

APRIL 2015 Summary , currently there is no reproducible pathophysiologically relevant & clinically practical standard to diagnose LPD & distinguish fertile from infertile women. v. In v. The roles of BBT , urinary LH detection kits , luteal progesterone levels , endometrial biopsy & other diagnostic studies have not been established & performance of these tests cannot be recommended.

Contents 1) Why 2) Indications 3) When to start ? 4) When to stop ? 5) What to use ? 6) Co treatment Conclusion

1. WHY ? ? ? Abnormal Luteal Function after COS for IVF v. Suppression v. Continued v. Removal v. Supra v. HCG of LH down-regulation by Gn. RHa of Granulosa cells at oocyte retrieval Physiological E 2/P 4 in early luteal phase injection before oocyte retrieval

2. INDICATIONS v Agonist and Antagonist protocol A. PR are significantly reduced in Gn. RHa ovarian stimulation without LPS ( Day & Gunby , 2004 ) B. Both Gn. RHa & Antagonist IVF cycles : abnormal LPD in all stimulated IVF cycles C. Luteolysis is also initiated prematurely in antagonist cotreated IVF cycles ( Albano et al. , 1998 ; Beckers et al. , 2002 )

v Frozen natural cycles ? Controversial Ø LPS increases LBR after frozen ET (Bjuresten et al. 2010 ) Ø LPS has no effect on ongoing PR in HCG – induced natural frozen – thawed ET cycles ( Kyrou et al. 2010 ) Ø Endometrial preparation for women undergoing ET with frozen embryos or embyros derived from donor oocytes (Glujovsky et al. , 2010)

v OPTIMAL TIMING OF INITIATION IN IVF CYCLE 24 to 48 hrs after oocyte retrieval for initiation of supplement with optimal cycle results. Ø

3. When to stop ? ? ? v Limited data v Can be safely withdrawn after first positive B-hcg result (Nyboe Anderson et al- prospective study –vag 600 mg ) v No advantage to continue support beyond first USG viability study(Aboulghar and collegues) v 3 randomized study comparing early and late cessation of prog combined studies of Nyboe, Anderson and Aboulghar concluded progesterone supplementation beyond first positive Beta h. CG may be unnecessary

4. What to use for LPS ? ? ? v HCG v PROGESTERONE

HOW TO CHOOSE ? ? ? v. Optimally v. Minimal v. Ease Efficacious side effects of administration v. Convenience (2011 Cochrane review compared vaginal progesterone , IM progesterone & HCG injection – reported similar IVF pregnancy rates , but odds for OHSS complication 20 hold higher with HCG than with progesterone. )

HCG : • Rescue corpus luteum (Hutchins Williams et al. 1990) • Improves the implantation by increasing relaxin, integrin & placental ptn (Mochtar, 1998) • Increase the risk of OHSS (van der Linden et al. , 2012) Aboubakr Elnashar)

PROGESTERONE SUPPORT IN IVF • Definite benefit (van der Linden et al. , 2012) Ø Improves endometrial receptivity (Kolibianakis & Devroy, 2002) Ø Promotes local VD and uterine musculature quiescence by inducing nitric oxide synthesis in decidua (Bulletti & de Ziegler, 2005) Ø Act as immunologic suppressant blocking Th 1 and inducing release of Th 2 cytokines � (Ng et al. 2002) Ø No value as regards miscarriage (van der Linden et al. , 2012) Aboubakr Elnashar

Oral progesterone • Only 10% of oral dose circulates as active P 4 {first pass effect} • No secretory transformation of the endometrium in patients with POF who had been treated with oral micronized progesterone (Devroey et al. 1989; Bourgain et al. 1990) Aboubakr Elnashar

IM progesterone • Serum P 4 levels well above the physiological range with adequate endometrial secretory changes • Dose: natural progesterone in oil, 25 and 100 mg/d: No significant difference in outcome (Costabile et al. , 2001, Pritts & Atwood, 2002) Aboubakr Elnashar SIDE EFFECTS �Welts , infection , abscess, allergic reaction & pulmonary complication , inconvenient to administer & painful. Subcutaneous Aqueous , lyophilized progesterone injection (25 mg daily )

Vaginal progesterone • “Targeted drug delivery” from vagina to uterus: better endometrial histology • High uterine progesterone concentrations {anatomically close blood vessels: uterine first pass effect} (Cicinelli et al. , 2000, de Ziegler et al. , 1995) Aboubakr Elnashar) DOSE ØMicronized ØVaginal Progestrone capsule 300 -600 mg daily cream/gel 90 mg once or twice daily ( Crinone 8% )

Which vaginal preparation? ? ? Gel or capsules ? • Both are equally effective • Capsule: solid evidence of effectiveness and convenience (Elenany et al, 2011) more cost effective than gel • Gel is at least 4 times more expensive than Capsules No difference exists regarding CPR between vaginal P gel and all other vaginal preparations for LPS (MA: Polyzoz et al, 2010) Aboubakr Elnashar • Progestrone vaginal ring ( MILPROSA ) - once a week insertion compared with crinone gel daily – no statistical difference , in PR , LBR , but 3 hold higher vaginal discharge with ring.

Rectal application • Resulted in serum concentration during the first 8 h twice as high as other forms • No prospective RCT to compare the rectal administration of progesterone with other administration routes for IVF • (Chakmakijan & Zachariah, 1987) Aboubakr Elnashar

Oral or I. M. progesterone ? Definitely - I. M. progesterone Grundy, 2004) Oral or vaginal progesterone ? Definitely - vaginal progesterone Grundy, 2004) (Daya & I. M. or vaginal progesterone ? Both are equally effective No difference in CPR (Daya & Grundy, 2004; MA: Zarutiski & Philips, 2009) Aboubakr Elnashar

OPTIMAL LUTEAL PHASE SUPPORT IN Gn. RH AGONIST – TRIGGERED CYCLE • • • Half life of HCG – 2. 3 days In addition to effecting the final oocyte maturation , it also contributes to OHSS Current evidence suggest Gn. RH agonist & HCG triggered cycles results in equalent oocyte maturity but , Gn. RH trigger are associated with much lower OHSS rates. In IVF cycles were pituitary secretion achieved with antagonist cycles there is a option to use Gn. RH Agonist trigger(Triptoriline 0. 2 mg or r. HCG 250 mcg ) instead of HCG. All cycles that do not involve fresh embryo transfer ( egg donor , Fertility preservation ) should be triggered with Gn. RH agonist only. Gn. Rh agonist triggered cycles are associated with higher degree of luteal phase impairment compared with HCG triggered cycles , but addition of small doses of HCG ( 1500 IU / IM on day of oocyte retrieval ) , not associated with OHSS.

PROGESTERONE IN FET CYCLES & DONOR OOCYTE RECIPIENT CYCLE v No endogenous progesterone production , therefore there is a need for luteal phase "creation" or replacement. v Only 2 small prospective studies compared IM progesterone 50 mg /. day & crinone gel 90 mg BD in FET cycle , were blastocyst was transferred , found no difference in clinical implantation or LBR.

Estrogen - co treatment with progesterone • No proven improved outcome • More studies are needed to evaluate the potential benefits of vaginal Estradiol (6 mg) supplementation. • Elgandy. etal , conducted a randomized study in patient undergoing ICSI cycle in long agonist protocol , concluded that addition of vaginal estradiol in luteal phase , improved the PR.

TO CONCLUDE ü PROGESTRONE SUPPLEMENTATION IN LUTEAL PHASE LEADS TO HIGHER PR ü VAGINAL PROGESTRONE ARE EQUALLY EFFECTIVE & TOLERATATED THAN IM ü ONCE DAILY CRINONE GEL OR TWICE OR THRICE ENDOMETRIN OR MICRONIZED PROGESTRONE TID ARE OPTIMAL DOSE OF VAGINAL PROGESTRONE ü VAGINAL SUPPLEMENTATION BEST STARTED WITHIN 24 -48 HRS OF OOCYTE RETRIVAL ü NO NEED FOE SERUM PROGESTRONE LEVEL MONITORING WITH VAGINAL SUPPLEMNTATION ü CONTINUED LPS SUPPORT IN EARLY PREGNANCY BEYOND 1 ST POSITIVE PREGANCY TEST IS OF LITTLE VALUE

Cont. . ü IVF CYCLES THAT DO NOT INVOLVE FRESH ET IS BEST CONDUCTED WITH GNRH ANTAGONIST PITUTARY SUPRESSION & Gn. RH AGONIST TRIGGER ü Gn. RH ANTAG CYCLE TRIGGERED WITH AGONIST , INVOLVING FRESH ET SHOULD HAVE MODIFIED LUTEAL PHASE SUPPORT INCLUDING SMALL DOSE OF HCG OR LH , IN ADDITION TO PROGESTRONE SUPPORT ü NEW DEVELOPMENT RELATED WITH SC & ORAL SYNTHETIC PREPARATION REQUIRE CAREFUL ATTENTION. üNo evidence to support co-tt to progesterone including aspirin, heparin, Viagra…. apart from midluteal phase Gn. RHa which is promising and needs further evaluation.


- Slides: 30