LRTIPart 5 Tuberculosis Chitra Pai MD Liisa Russell

LRTI-Part 5 Tuberculosis Chitra Pai, MD Liisa Russell, MD Athena Lin, Ph. D

Tuberculosis-Introduction A chronic progressive disease associated with very high morbidity and mortality. A potentially serious disease that mainly affects the lungs but can disseminate to different parts of the body. One of the world’s top infectious killers Caused by the acid fast bacteria-Mycobacterium tuberculosis. TB is the leading cause of death among people with AIDS Multi-drug resistant strains of TB-greatest challenge for effective treatment.

Epidemiology More than 1. 7 billion people (about 25 percent of the world population) are estimated to be infected with M. tuberculosis. Worldwide, in 2017, 10 million individuals became ill with TB and 1. 6 million died. Highest rates are seen in sub-Saharan Africa, India, and the islands of Southeast Asia and Micronesia. No country has ever eliminated TB. An estimated 490, 000 people were infected with MDR-TB 95% of TB deaths occurred in low- and middle-income countries.

TB statistics in the US • In 2017, a total of 9, 105 TB cases were reported in the United States. • This represents a 1. 6% decrease from 2016. Key finding (CDC) The rate of decline in the United States remains too slow to achieve TB elimination in this century. Eleven states, the District of Columbia (DC), and New York City reported incidence rates above the national average of 2. 8 cases per 100, 000. • More than 2, 000 people are diagnosed with TB disease in CA each year (20 -30 in Solano County) • 2. 4 million in CA are living with TB infection

Epidemiology-High risk groups HIV (+) / Immunocompromised patients Close contacts of a person with infectious TB disease Persons who have immigrated from areas of the world with high rates of TB Children less than 5 years of age who have a positive TB test Homeless persons Injection drug users Persons who work or reside with people who are at high risk for TB in facilities or institutions such as hospitals, homeless shelters, nursing homes and residential homes for those with HIV

Presentations of TB Latent TB Infection (LTBI) • Asymptomatic • Non infectious • Usually have a positive Tuberculin test • Chest X ray findings- normal • Sputum smears-negative • May develop TB disease if they do not receive treatment for latent TB infection TB disease Symptomatic May be infectious and contagious Tuberculin test mostly positive Chest X-ray findings-may be abnormal Sputum smear for AFB may be positive Curable with multiple antibiotics

TB-disease presentation Symptoms will depend on the body-site of involvement. Pulmonary TB -most common. Classical symptoms: Fever with sweating at night Chronic cough, productive cough and hemoptysis Chest pain Others- Weight loss, weakness, loss of appetite Extra-pulmonary TB TB disease in any part of the body other than the lungs (for example, the kidney, spine, bones, brain, or lymph nodes).

Clinical features PRIMARY TB REACTIVATION/ SECONDARY TB May be asymptomatic/ symptomatic Fever , malaise, cough Chest Radiographs: infiltrates in the mid-zones of the lung and enlarged draining lymph nodes in the area around the hilum. Features of disseminated TB (if it occurs) Cough ( productive) Fever, malaise, fatigue Night sweats and weight loss Chest Radiograph: infiltrates in the apices of the lung coalesce to form cavities with progressive destruction of lung tissue. Extra-pulmonary TB: Kidneys, bones, Brain and meninges, bowel

Etiology and Transmission of TB Reservoirs Human host-for Mycobacterium tuberculosis Active and open cases of TB transmit infection Infected cows/ livestock- for Mycobacterium bovis Acid fast bacilli • Mycobacterium tuberculosis • Mycobacterium bovis Modes of infection Inhalation of droplet nuclei/ aerosols Ingestion of raw milk from infected animals

M. tuberculosis- characteristics Acid-fast bacteria ( due to mycolic acid) Rod-shaped Obligate aerobe Prefers growth in highly oxygenated tissues (e. g. upper lobes of lung) Slow growth- grown on Lowenstein Jensen medium-Rough, Tough and Buff colonies Growth seen after 3 -6 weeks of incubation Facultative intracellular pathogen Survival inside of macrophages Able to establish life-long infection Z. N stain of sputum showing inflammatory exudate with acid fast bacilli Auramine Rhodamine stain of sputum showing fluorescent apple green, acid fast bacilli

M. tuberculosis – Virulence Factors Cell wall components- very complex cell wall Sulfolipids Inhibition of phagosome-lysosome fusion and intracellular growth Cord factor (trehalose dimycolate) Inhibits leukocyte migration Disrupts mitochondrial respiration and oxidative phosphorylation Serpentine cord colonies Tuberculin proteins and mycolic acid Delayed hypersensitivity and cell-mediated immunity granulomas and caseation No toxins – damage due to host immune response 11

PATHOGENESIS SOURCE: For pulmonary TB: Open (active) case of TB SOURCE: For bovine TB: Ingestion of contaminated milk (unpasteurized) Primary tuberculosis is the response to the initial infection in a previously un-sensitized individual Latent Tuberculosis Seen as an intermediate and quiescent stage Secondary TB/ Reactivation tuberculosis is the response to reinfection or reactivation of dormant lesion in a previously sensitized individual
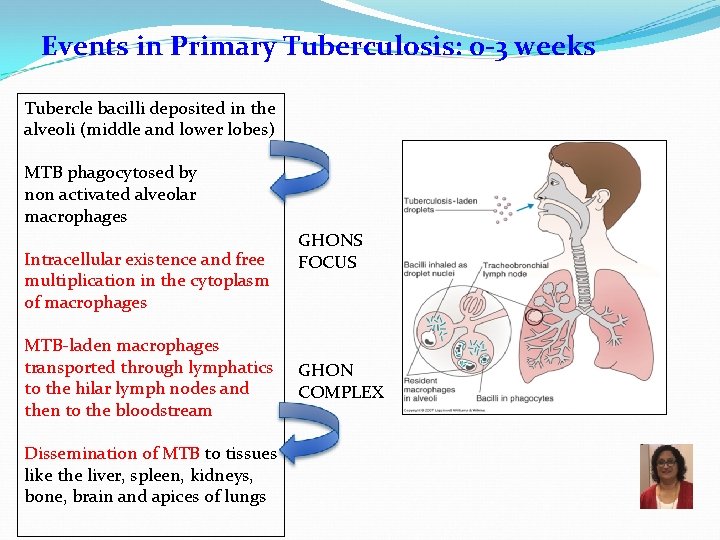
Events in Primary Tuberculosis: 0 -3 weeks Tubercle bacilli deposited in the alveoli (middle and lower lobes) MTB phagocytosed by non activated alveolar macrophages Intracellular existence and free multiplication in the cytoplasm of macrophages MTB-laden macrophages transported through lymphatics to the hilar lymph nodes and then to the bloodstream Dissemination of MTB to tissues like the liver, spleen, kidneys, bone, brain and apices of lungs GHONS FOCUS GHON COMPLEX
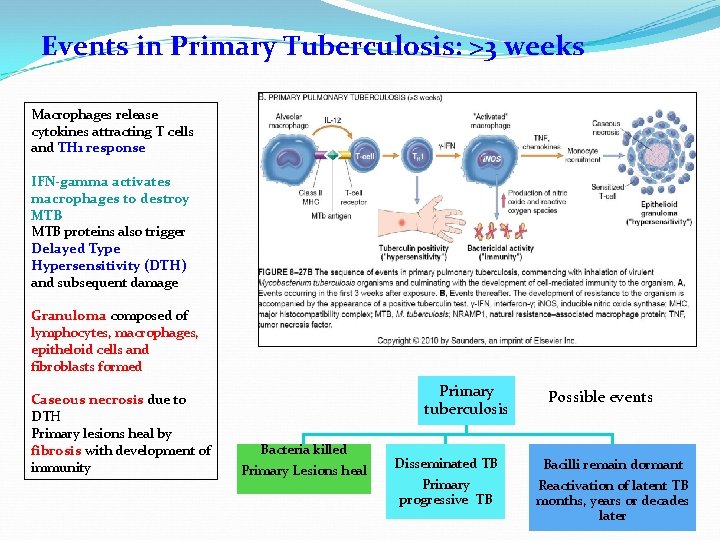
Events in Primary Tuberculosis: >3 weeks Macrophages release cytokines attracting T cells and TH 1 response IFN-gamma activates macrophages to destroy MTB proteins also trigger Delayed Type Hypersensitivity (DTH) and subsequent damage Granuloma composed of lymphocytes, macrophages, epitheloid cells and fibroblasts formed Caseous necrosis due to DTH Primary lesions heal by fibrosis with development of immunity Primary tuberculosis Bacteria killed Primary Lesions heal Disseminated TB Primary progressive TB Possible events Bacilli remain dormant Reactivation of latent TB months, years or decades later
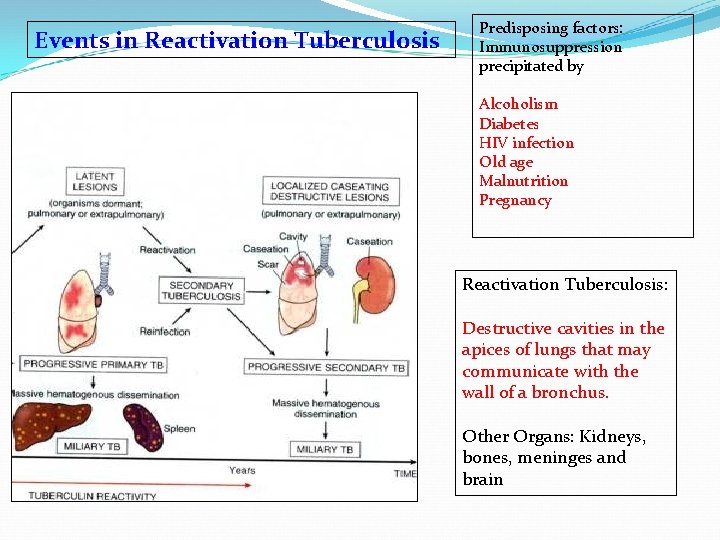
Events in Reactivation Tuberculosis Predisposing factors: Immunosuppression precipitated by Alcoholism Diabetes HIV infection Old age Malnutrition Pregnancy Reactivation Tuberculosis: Destructive cavities in the apices of lungs that may communicate with the wall of a bronchus. Other Organs: Kidneys, bones, meninges and brain

Disease Course Depends on Outcome of Battle between M. tuberculosis and Cellular Immune Defenses Primary TB In most cases the host prevails granulomas and foci fibrose, scar 90% and calcify (Ghon complex) the infection remains clinically silent. 10% Progressive primary (active) TB Local disease or lesion break down spread of infection via lymph and blood to distant tissues Miliary TB. Infectious. Skin test (+); X-ray (+); Sputum (+) Latent (dormant) TB No disease; not infectious. Skin test (+); X-ray (+/-); Sputum (-) 10% Secondary (reactivation) TB Impairment in immune status free organisms; possible dissemination. Infectious. Skin test (+); X-ray (+); Sputum (+) 16
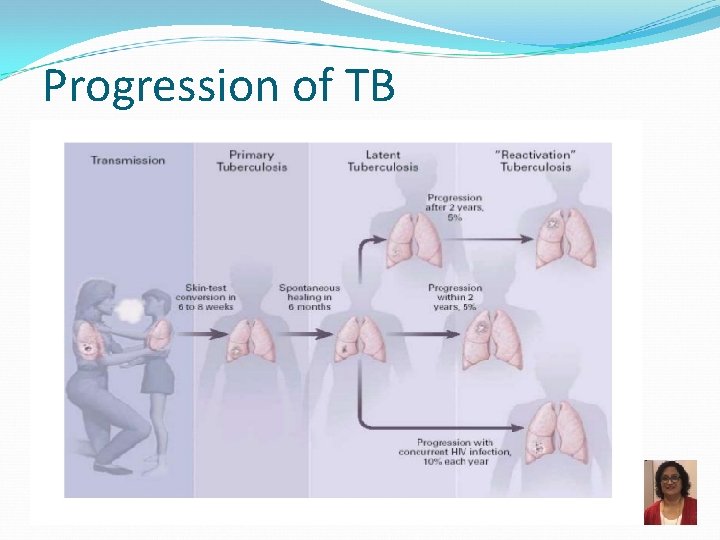
Progression of TB
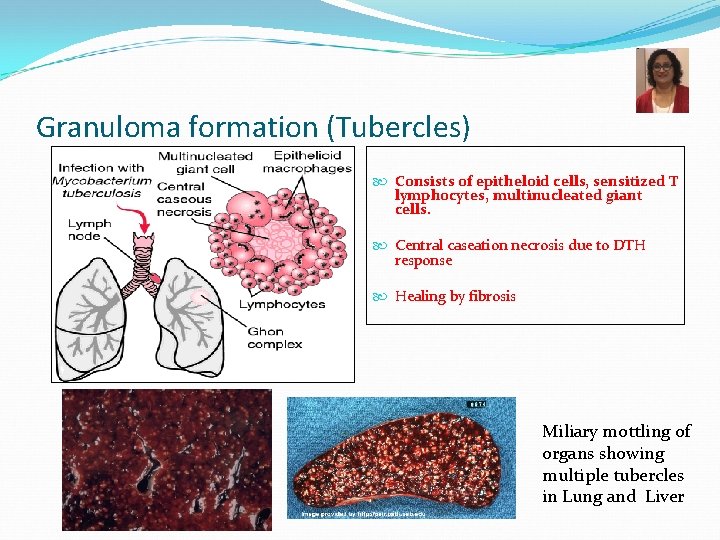
Granuloma formation (Tubercles) Consists of epitheloid cells, sensitized T lymphocytes, multinucleated giant cells. Central caseation necrosis due to DTH response Healing by fibrosis Miliary mottling of organs showing multiple tubercles in Lung and Liver

Radiology and Pathology of TB

TB Radiology • • • Primary pattern • Unilateral consolidation • Middle/lower lobes, predilection for right lung • Segmental, lobar, multifocal • Unilateral lymphadenopathy, typically in children • Right hilar and paratracheal • Ipsilateral to lung consolidation • Pleural effusion • Unilateral, ipsilateral to pulmonary disease • Usually self-limited, resolves in several weeks • Atelectasis & hyperinflation in children Progressive primary pattern • Cavitary consolidation • Bronchogenic dissemination (acinar nodules) Post-primary pattern • Upper lobe apical/posterior segments and lower lobe superior segments, multiple segments involved • Poorly defined airspace disease • Heterogeneous consolidation ± cavitation • Pleural effusion: small, loculated, ± calcification
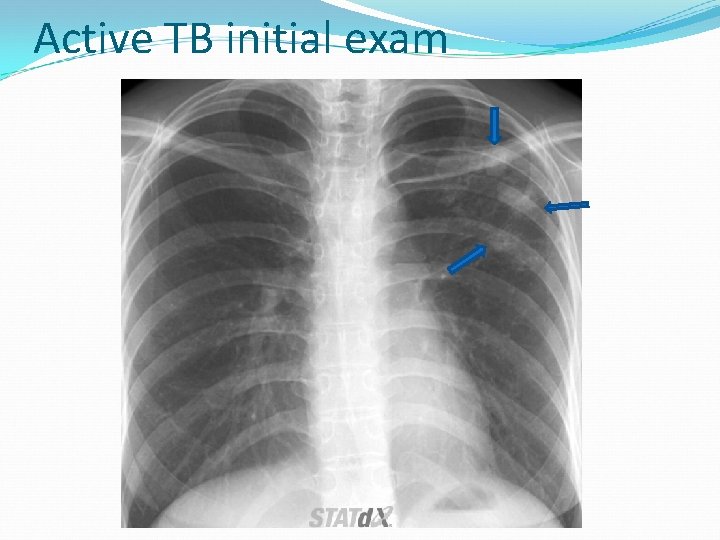
Active TB initial exam
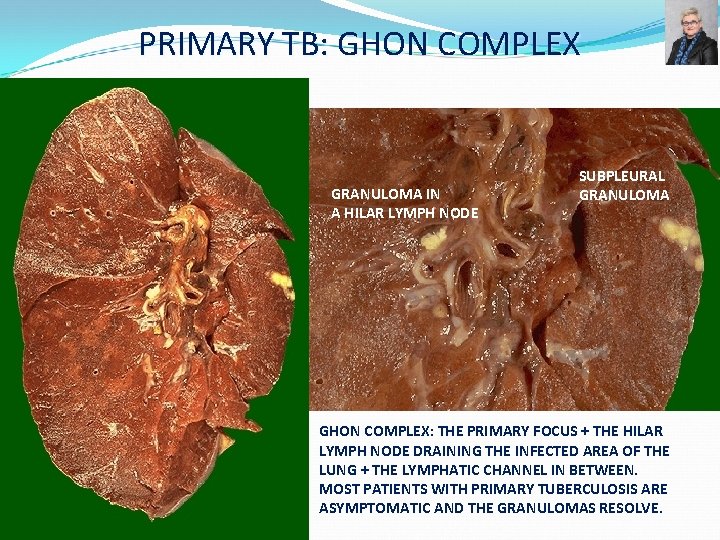
PRIMARY TB: GHON COMPLEX GRANULOMA IN A HILAR LYMPH NODE SUBPLEURAL GRANULOMA GHON COMPLEX: THE PRIMARY FOCUS + THE HILAR LYMPH NODE DRAINING THE INFECTED AREA OF THE LUNG + THE LYMPHATIC CHANNEL IN BETWEEN. MOST PATIENTS WITH PRIMARY TUBERCULOSIS ARE ASYMPTOMATIC AND THE GRANULOMAS RESOLVE.
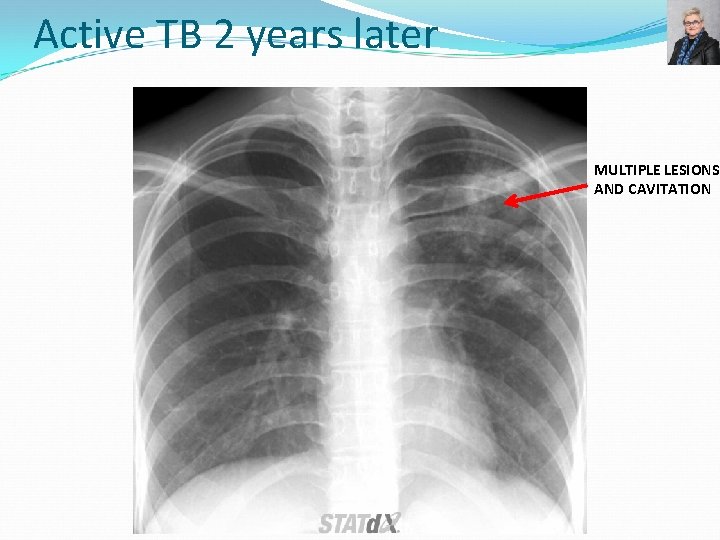
Active TB 2 years later MULTIPLE LESIONS AND CAVITATION
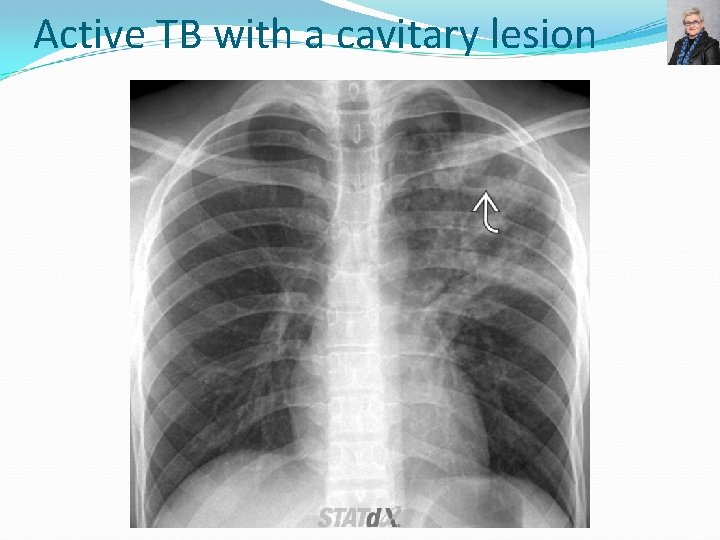
Active TB with a cavitary lesion
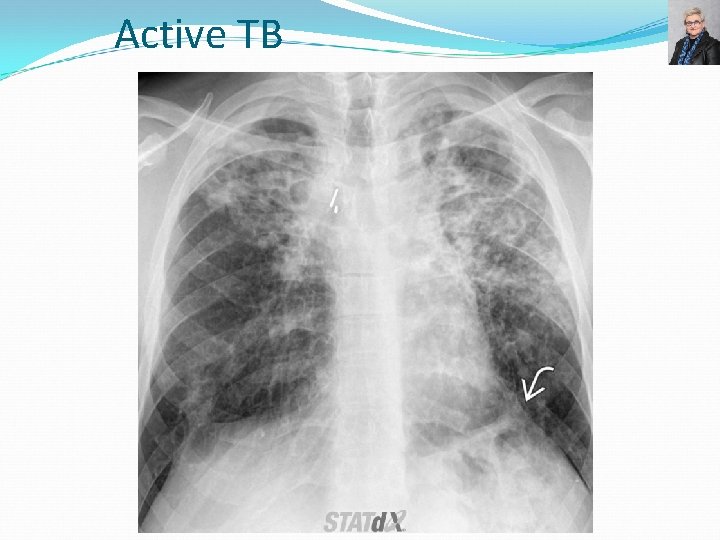
Active TB
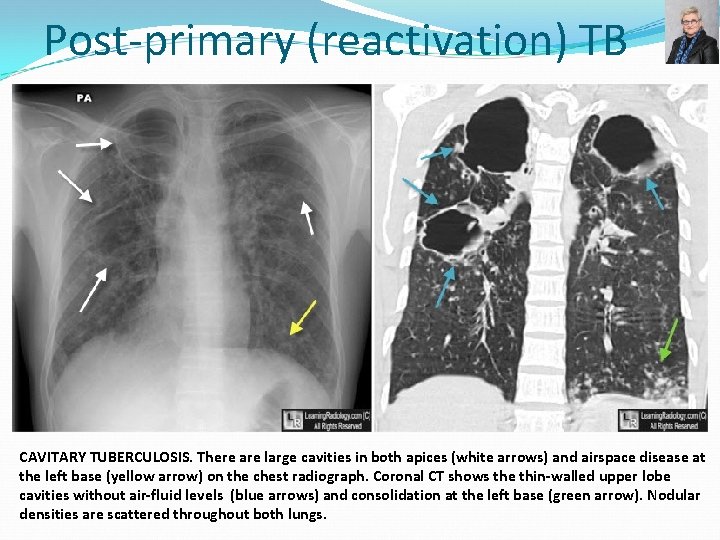
Post-primary (reactivation) TB CAVITARY TUBERCULOSIS. There are large cavities in both apices (white arrows) and airspace disease at the left base (yellow arrow) on the chest radiograph. Coronal CT shows the thin-walled upper lobe cavities without air-fluid levels (blue arrows) and consolidation at the left base (green arrow). Nodular densities are scattered throughout both lungs.
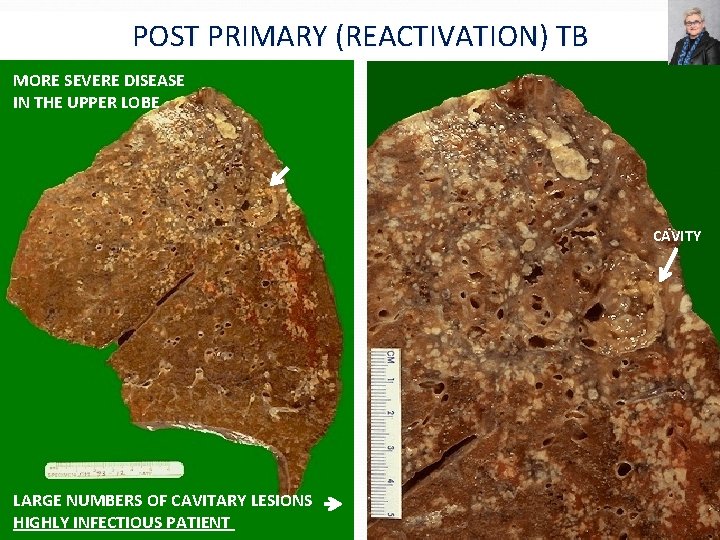
POST PRIMARY (REACTIVATION) TB MORE SEVERE DISEASE IN THE UPPER LOBE CAVITY LARGE NUMBERS OF CAVITARY LESIONS HIGHLY INFECTIOUS PATIENT
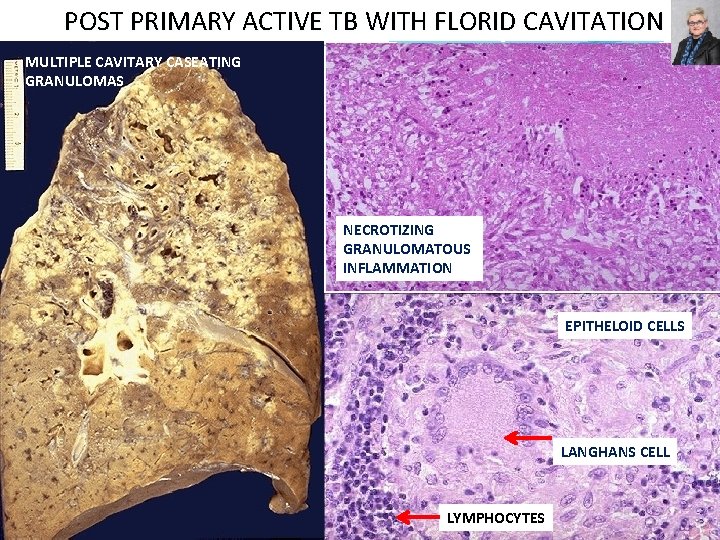
POST PRIMARY ACTIVE TB WITH FLORID CAVITATION MULTIPLE CAVITARY CASEATING GRANULOMAS NECROTIZING GRANULOMATOUS INFLAMMATION EPITHELOID CELLS LANGHANS CELL LYMPHOCYTES
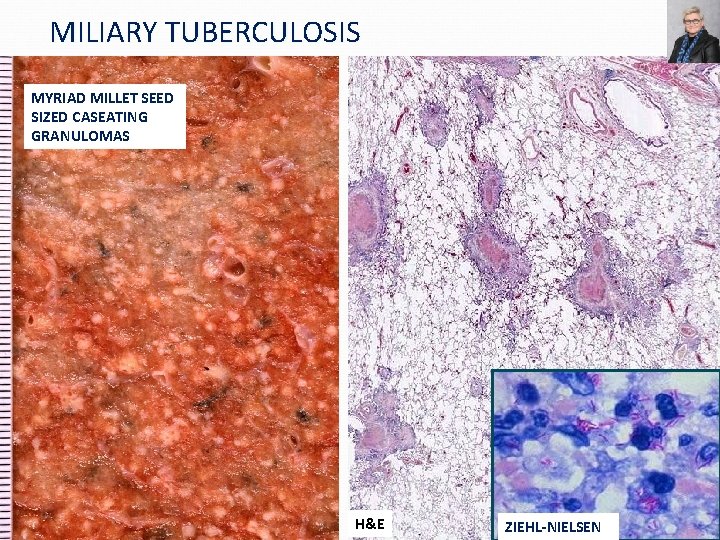
MILIARY TUBERCULOSIS MYRIAD MILLET SEED SIZED CASEATING GRANULOMAS H&E ZIEHL-NIELSEN
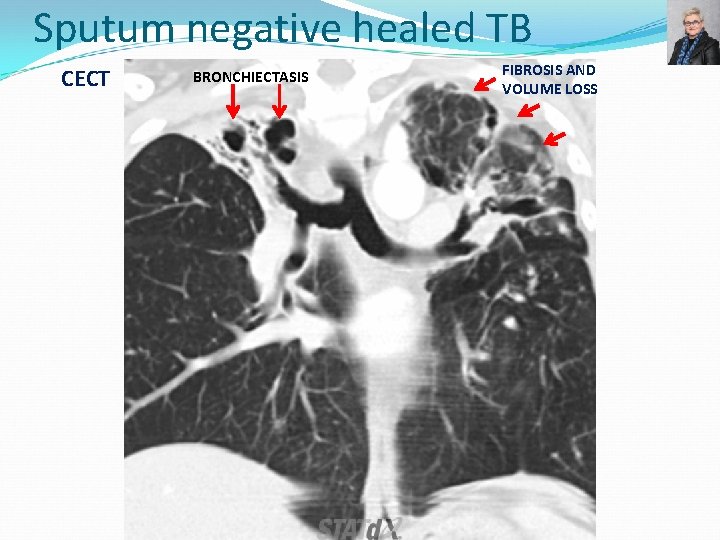
Sputum negative healed TB CECT BRONCHIECTASIS FIBROSIS AND VOLUME LOSS
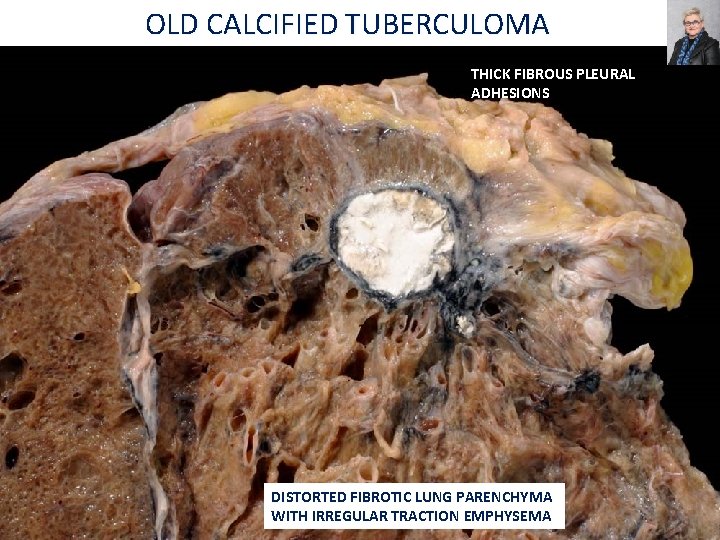
OLD CALCIFIED TUBERCULOMA THICK FIBROUS PLEURAL ADHESIONS DISTORTED FIBROTIC LUNG PARENCHYMA WITH IRREGULAR TRACTION EMPHYSEMA
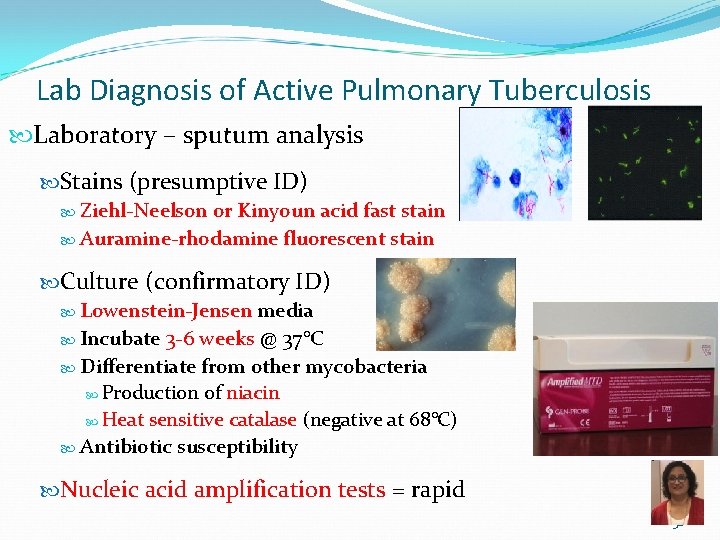
Lab Diagnosis of Active Pulmonary Tuberculosis Laboratory – sputum analysis Stains (presumptive ID) Ziehl-Neelson or Kinyoun acid fast stain Auramine-rhodamine fluorescent stain Culture (confirmatory ID) Lowenstein-Jensen media Incubate 3 -6 weeks @ 37°C Differentiate from other mycobacteria Production of niacin Heat sensitive catalase (negative at 68°C) Antibiotic susceptibility Nucleic acid amplification tests = rapid 32

Other tests Quantiferon TB Gold test: For measurement of IFN-gamma Other serological tests are not recommended Molecular Techniques-PCR- for rapid diagnosis Gene Amplification techniques Line Immunoassays for detection of Mtb DNA/ drug resistance

Tuberculin Skin Test (TST) How to read: Measure induration (not erythema) at 48 -72 hrs Record millimeters Positive test: ≥ 5 mm for immunosuppressed including HIV, recent contacts ≥ 10 mm for all others with TB risk 34

BCG Vaccine Live vaccine from attenuated strains of Mycobacterium bovis Currently used in over 100 countries Given to children to protect against disseminated TB (~80% effective) TST reactivity often affected by. BCG Use IGRA

Multidrug-Resistant Tuberculosis Noncompliance is major factor in development of resistance Multidrug-resistant TB (MDR-TB) = strains of tuberculosis that are resistant to the two first-line TB drugs - isoniazid and rifampicin Reference: WHO Global TB Report Extensive Drug Resistant TB (XDR-TB ) = MDR-TB with resistant to secondline medications: fluoroquinolones and at least one of three injectable drugs (i. e. , amikacin, kanamycin, or capreomycin). 36

Mycobacteria Other Than Tuberculosis MOTTS or atypical mycobacteria Usually acquired from environment Low level of pathogenicity M. avium Complex (MAC) M. avium and M. intracellulare Transmission via inhalation or ingestion Cause tuberculosis-like disease in immunocompromised Opportunistic infection Disseminated disease in AIDS patients M. kansasii TB-like disease M. bovis Causes tuberculosis in cattle but can infect humans Transmission via infected milk or aerosol droplets M. scrofulaceum Causes lymphadenitis Contaminated water M. marinum Causes soft tissue infection “Fish tank granuloma” Transmission thru abrasion 37

Other Acid Fast Organisms

Nocardiosis Nocardia asteroides 39
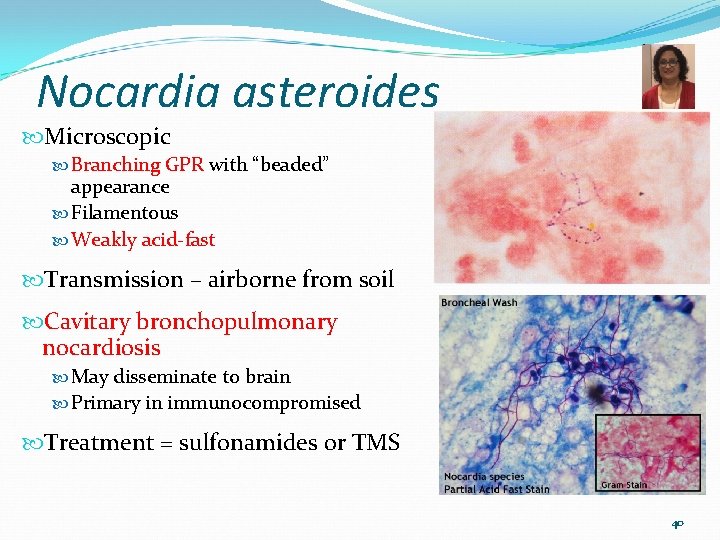
Nocardia asteroides Microscopic Branching GPR with “beaded” appearance Filamentous Weakly acid-fast Transmission – airborne from soil Cavitary bronchopulmonary nocardiosis May disseminate to brain Primary in immunocompromised Treatment = sulfonamides or TMS 40

Questions?

References www. cdc. gov/tb. html www. who. int/tb/publications/global_report/gtbr 14 Pozniak A. Clinical manifestations and evaluation of pulmonary tuberculosis. Up. To. Date online. Sterling T. Treatment of pulmonary tuberculosis in HIV-negative patients. Up. To. Date online. Murray’s Medical Microbiology 8 th edition Ch. 24 – Nocardia asteroides Ch. 25 - Mycobacterium tuberculosis and MOTTS Other References Up. To. Date: https: //www. uptodate. com WHO: http: //www. who. int/tb/
Antimycobacterial Drugs CDC-TB Infograph

Agents Used in the Treatment of Tuberculosis 2 nd -line agents 1 st -line agents Isoniazid Rifampin Pyrazinamide Ethambutol Streptomycin Amikacin Ciprofloxacin Levofloxacin Rifabutin Rifapentine Ethionamide Cycloserine Capreomycin Aminosalicylic acid Agents Used in the Treatment of Leprosy Rifampin Clofazimine Dapsone

TB Drugs Major Side Effects Isoniazid liver toxicity, peripheral neuropathy, seizure Rifampin renal toxicity, red secretion, p 450 inducer Pyrazinamide liver toxicity, hyperuricemia Ethambutol retrobulbar neuritis (Color blindness & loss of visual acuity) Streptomycin renal toxicity & ototoxicity

Antimycobacterial Agents Drugs Mechanism of Action Isoniazid Inhibits mycolic acid synthesis Rifampin Inhibits bacterial RNA polymerase Ethambutol Inhibits arabinoglycan synthesis Pyrazinamide Inhibits fatty acid synthesis? Streptomycin Inhibits bacterial protein synthesis Dapsone Inhibits bacterial folate synthesis Clofazamine Inhibits bacterial DNA synthesis

Alternative 2 nd-line Drugs for TB Amikacin Rifabutin Rifapentine Ciprofloxacin Protein synthesis inhibitor RNA polymerase inhibitor DNA synthesis inhibitor Levofloxacin Ethionamide P- Aminosalicylic acid Mycolic acid syn. inhibitor Folate synthesis inhibitor Capreomycin Protein synthesis inhibitor Cycloserine Cell wall synthesis inhibitor

Study Aid Upon completion of this lecture, medical students should be able to • Summarize the unique structure of mycobacteria for therapeutic intervention • Summarize the standard treatment regimen for infections caused by mycobacteria • Comprehend the MOA of drugs used for infections caused by mycobacteria and mechanisms of drug resistance • List the major side effects/toxicities of drugs used for infections caused by mycobacteria • Evaluate the potential drug interactions with isoniazid and rifampin • Understand the unique use of rifabutine (but not refapentine) in HIV/TB p’ts • Comprehend the MOA of drugs used as alternative TB drugs • Know the use of clarithromycin or azithromycin for infection caused by mycobacterium-avium complex


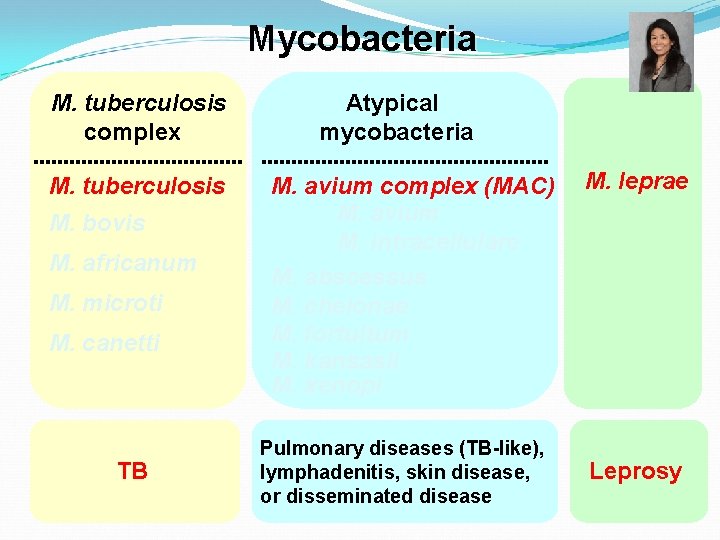
Mycobacteria M. tuberculosis complex M. tuberculosis M. bovis M. africanum M. microti M. canetti TB Atypical mycobacteria M. avium complex (MAC) M. avium M. intracellulare M. abscessus M. chelonae M. fortuitum M. kansasii M. xenopi Pulmonary diseases (TB-like), lymphadenitis, skin disease, or disseminated disease M. leprae Leprosy
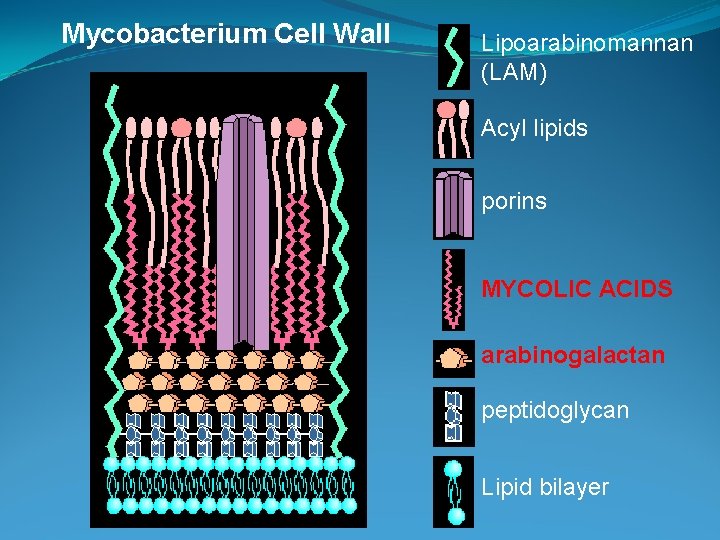
Mycobacterium Cell Wall Lipoarabinomannan (LAM) Acyl lipids porins MYCOLIC ACIDS arabinogalactan peptidoglycan Lipid bilayer
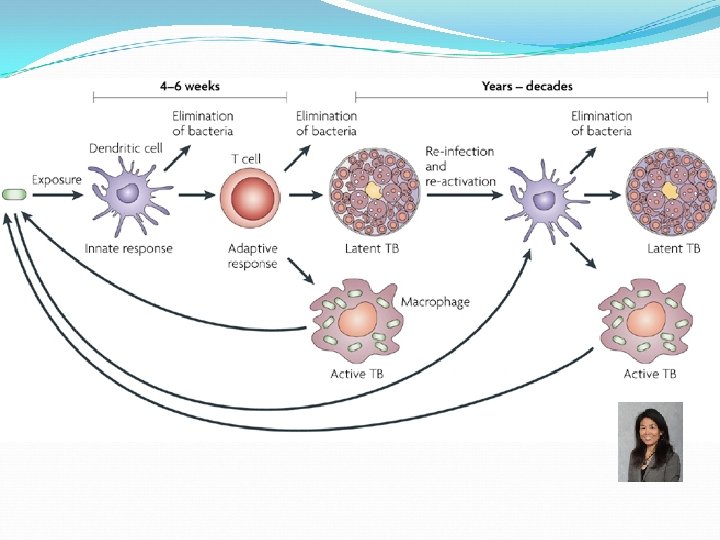
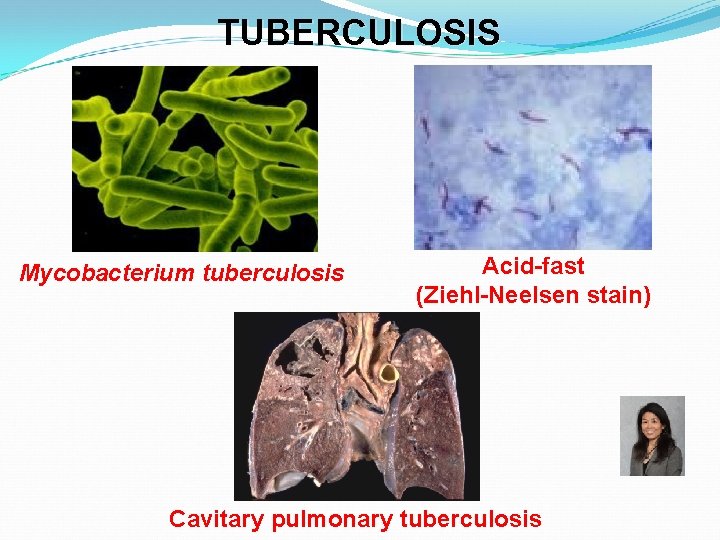
TUBERCULOSIS Mycobacterium tuberculosis Acid-fast (Ziehl-Neelsen stain) Cavitary pulmonary tuberculosis

A 55 -year-old female suffers from fever, bloody cough, fatigue and night sweats. She thinks the symptoms started about a month ago and notices that she has lost a lot of weight recently. Chest xray reveals a cavitary nodule in the right upper lobe with involvement of nearby lymph nodes. The lab test comes back positive for acid fast bacilli, the pathologist indicates the presence of Mycobacterium tuberculosis…………

Phthisis (consumption) Robert Koch 1839 Tuberculosis 1859 TB sanatorium 1882 M. tuberculosis 1943 Streptomycin Current Isoniazid, rifampin, pyrazinamide, ethambutol or streptomycin

Agents Used in the Treatment of Tuberculosis 1 st -line agents Isoniazid (INH) Rifampin (RIF) Pyrazinamide (PZA) Ethambutol Streptomycin 2 nd -line agents Amikacin Ethionamide Cycloserine Ciprofloxacin Capreomycin Levofloxacin Rifabutin P-Aminosalicylic acid Rifapentine

Tuberculosis Latent TB Infection (LTBI) • Patients are infected with M. tuberculosis, but do not have active tuberculosis disease • Not infectious Active TB • Feelings of sickness or weakness, weight loss, fever, and night sweats. The symptoms of TB disease of the lungs may also include coughing, chest pain, and coughing up blood • Symptoms of TB disease in other parts of the body depend on the area affected

MDR-TB (Multidrug Resistant TB) • Strains of tuberculosis that are resistant to at least the two main first-line TB drugs - isoniazid & rifampicin XDR-TB (Extensive Drug Resistant TB) (also referred to as Extreme Drug Resistance) • MDR-TB that is also resistant to the best second-line medications: fluoroquinolones and at least one of three injectable drugs (i. e. , amikacin, kanamycin, or capreomycin)
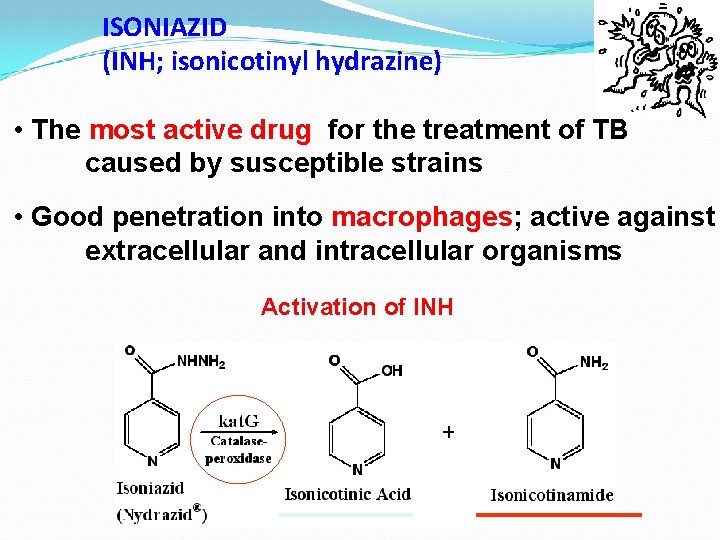
ISONIAZID (INH; isonicotinyl hydrazine) • The most active drug for the treatment of TB caused by susceptible strains • Good penetration into macrophages; active against extracellular and intracellular organisms Activation of INH
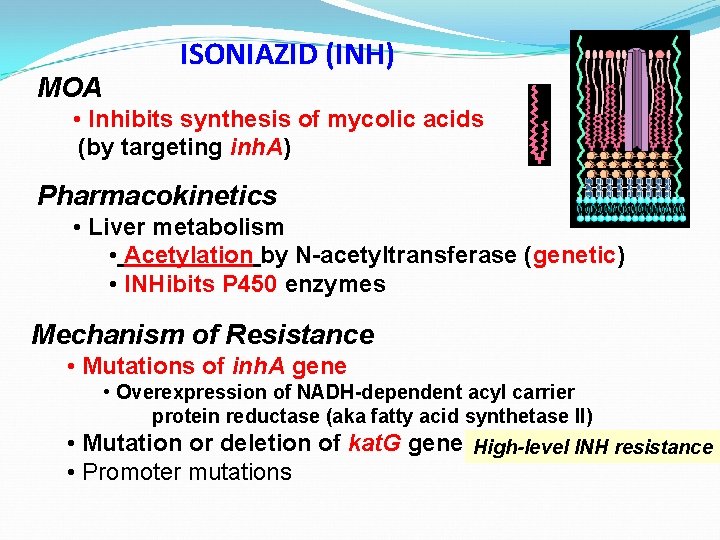
MOA ISONIAZID (INH) • Inhibits synthesis of mycolic acids (by targeting inh. A) Pharmacokinetics • Liver metabolism • Acetylation by N-acetyltransferase (genetic) • INHibits P 450 enzymes Mechanism of Resistance • Mutations of inh. A gene • Overexpression of NADH-dependent acyl carrier protein reductase (aka fatty acid synthetase II) • Mutation or deletion of kat. G gene High-level INH resistance • Promoter mutations

ISONIAZID (INH) Adverse Reactions (dosage & duration-related) • Increased serum aminotransferase (> 3 x) • Hepatotoxicity (can be fatal) • Peripheral neuropathy (due to pyridoxine deficiency) • Seizure (↓GABA), psychosis, optic neuritis Drug Interactions • INHibits many P 450 -mediated drug metabolism (increase serum drug conc. and toxicity of phenytoin, carbamazepine, warfarin, etc) Contraindications • Isoniazid allergy • Previous isoniazid-induced hepatotoxicity • Acute Liver Disease
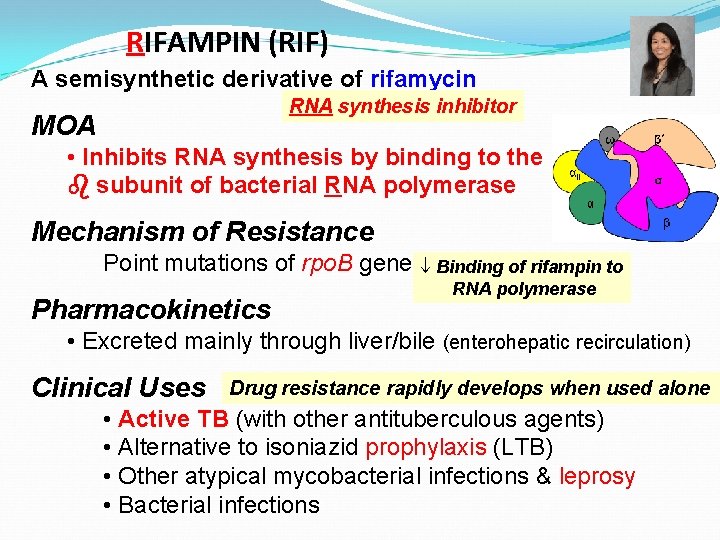
RIFAMPIN (RIF) A semisynthetic derivative of rifamycin RNA synthesis inhibitor MOA • Inhibits RNA synthesis by binding to the b subunit of bacterial RNA polymerase Mechanism of Resistance Point mutations of rpo. B gene Pharmacokinetics ¯ Binding of rifampin to RNA polymerase • Excreted mainly through liver/bile (enterohepatic recirculation) Clinical Uses Drug resistance rapidly develops when used alone • Active TB (with other antituberculous agents) • Alternative to isoniazid prophylaxis (LTB) • Other atypical mycobacterial infections & leprosy • Bacterial infections

RIFAMPIN (RIF) Adverse Reactions • Reddish color in urine. sweat, tears & contact lenses • Rashes • Renal failure (nephritis) • Thrombocytopenia • Cholestatic jaundice, hepatitis • Light-chain proteinuria • Flu-like symptoms • Acute tubular necrosis Drug Interactions • A strong INDUCER of most P 450 enzymes • elimination of anticoagulants, cyclosporine, some anticonvulsants, protease inhibitors, NRTI, NNRTI, and oral contraceptives

Drug Interaction with Rifampin Increased elimination of Anticoagulants: warfarin Anti-arrhythmic: digoxin, quinidine Anticonvulsants: phenytoin Antifungal: ketoconazole, fluconazole, itraconazole Anti-HIV NRTI: zidovudine Anti-HIV NNRTI: nevirapine, delavirdine Anti-HIV PI: ritonavir, saquinavir Bronchodilator: aminophylline, theophylline Immunosuppressants: cyclosporine Oral contraceptives http: //i-base. info/ttfa/learning-resources/tb-and-arv-drug-interactions-summary/

ETHAMBUTOL MOA • Inhibits mycobacterial arabinosyl transferase (interferes with the polymerization of arabinoglycan) • Bacteriostatic against susceptible M. tuberculosis Mechanism of Resistance • Overexpression of the arabinosyl transferase Pharmacokinetics • Accumulate in renal failure (dosage adjustment is needed) Adverse Reactions • Dose-related retrobulbar neuritis (loss of visual acuity and red-green color blindness)

PYRAZINAMIDE (PZA) • Structurally related to nicotinamide • Active against mycobacteria in the acidic phagosome Pyrazinamide (prodrug) Mycobacterial Pyrazinamidase Pyrazinoic acid (active) MOA unknown (inhibits fatty acid synthetase I ? ) Shortens the treatment regimen Mechanism of Resistance • Mutations in pnc. A gene (encodes pyrazinamidase) Adverse Reactions Hepatotoxicity, nausea, vomiting, fever, hyperuricemia, polyarthralgia

Fixed Dose Combinations (FDC) Rifater • A fixed combination of isoniazid rifampin pyrazinamide 4 -FDC • A fixed combination of isoniazid rifampin pyrazinamide Ethambutol • Reduces pill burden • Prevents the development of drug resistance

STREPTOMYCIN MOA Aminoglycoside • Irreversible inhibition of 30 S ribosome Mechanism of Resistance • Altered ribosomal binding site Pharmacokinetics • Poor cell penetration (mainly against extracellular bacilli) Clinical Uses • Used as an injectable drug (streptomycin sulfate) for life-threatening forms of tuberculosis Adverse Reaction (concentration- and time-dependent) • Ototoxicity and nephrotoxicity
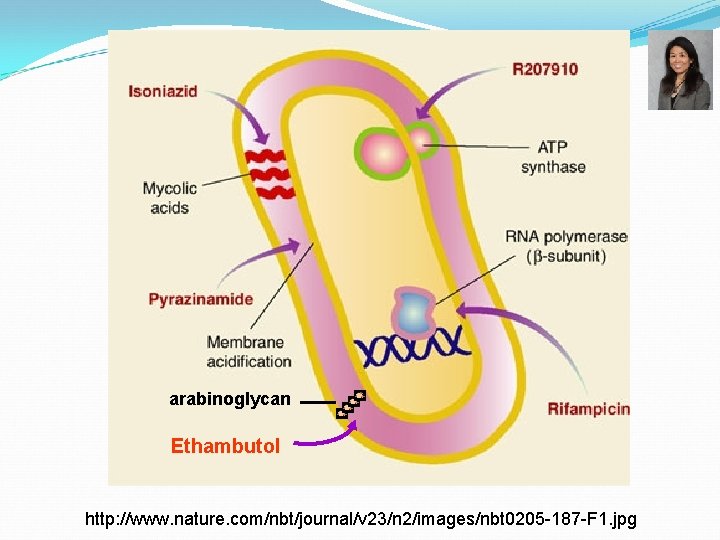
arabinoglycan Ethambutol http: //www. nature. com/nbt/journal/v 23/n 2/images/nbt 0205 -187 -F 1. jpg

Alternative 2 nd-line Drugs for TB Amikacin Rifabutin Rifapentine Ciprofloxacin Aminoglycoside Rifamycin derivative Fluoroquinolone Levofloxacin Ethionamide P- Aminosalicylic acid Similar to INH Similar to PABA Capreomycin Protein synthesis inhibitor Cycloserine Cell wall synthesis inhibitor

Amikacin (aminoglycoside) • Used for treatment of streptomycin-resistant TB Ciprofloxacin & levofloxacin (fluoroquinolones) • DNA gyrase inhibitors • Active against M. tuberculosis and atypical mycobacteria Rifabutin & Rifapentine (similar to rifampin) • Inhibit bacterial RNA polymerase • Rifabutin: Less potent inducer of P 450 enzymes • Indicated in place of rifampin for treatment of TB in HIV-infected patients who are receiving concurrent antiretroviral therapy • Rifapentine: Potent inducer of p 450 enzymes • Avoided in HIV patients (high relapse rate with rifampin-resistant strains)

Ethionamide • Blocks the synthesis of mycolic acid • Adverse reactions: hepatotoxicity, GI irritation, neurologic symptoms (take pyridoxine supplement) Aminosalicylic acid (PAS) • Folate synthesis antagonist • Adverse reactions: GI upset, hepatitis, hemolysis Capreomycin • Protein synthesis inhibitor • An injectable agent for treatment of drug-resistant TB • Adverse reactions: nephrotoxicity and ototoxicity Cycloserine • Inhibits cell wall synthesis • Adverse reactions: peripheral neuropathy, CNS dysfunction • Taken with pyridoxine Serum conc. should be monitored

Treatment for Acute TB Directly Observed Therapy (DOT) Combination of Isoniazid, Rifampin, pyrazinamide, ethambutol • Initial phase: INH, RIF, PZA, ethambutol (2 months) • Continuation phase: INH, RIF (4 -7 months) 2 HREZ / 4 HR Treatment for Latent TB PZA/RIF combo should Not be used in LTB!! Source: CDC Drugs Months of Duration INH 9* INH 6 RIF 4 *Preferred

Drugs Against Atypical Mycobacteria Species Clinical Features M avium complex (MAC) Pulmonary disease in patients with chronic lung disease; disseminated infection in AIDS Treatment Options Clarithromycin or azithromycin + ethambutol with or w/o rifabutin Clarithromycin & azithromycin • Macrolides (similar to erythromycin) • Bind to inhibit 50 S ribosomes • More acid-stable than erythromycin • Clarithromycin inhibits p 450 enzymes
Leprosy (“The living Death”) Chaulmoogra nut oil Alice Ball
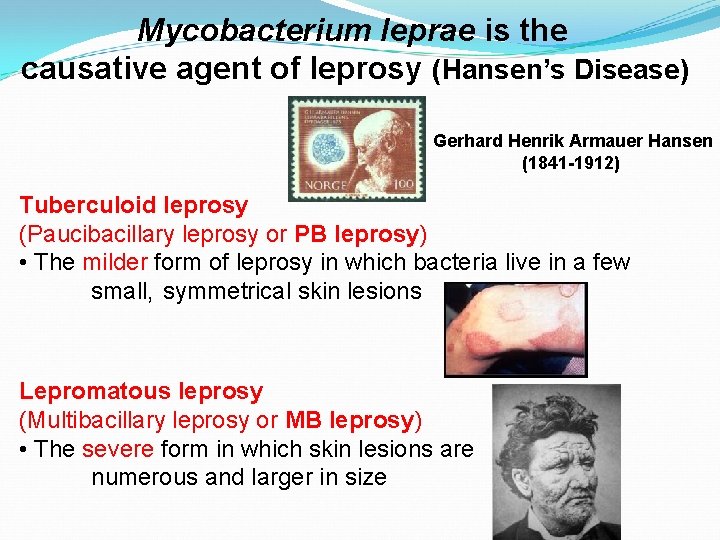
Mycobacterium leprae is the causative agent of leprosy (Hansen’s Disease) Gerhard Henrik Armauer Hansen (1841 -1912) Tuberculoid leprosy (Paucibacillary leprosy or PB leprosy) • The milder form of leprosy in which bacteria live in a few small, symmetrical skin lesions Lepromatous leprosy (Multibacillary leprosy or MB leprosy) • The severe form in which skin lesions are numerous and larger in size
WHO Multidrug Therapy (MDT) for Leprosy PB leprosy • A combination of rifampin dapsone MB leprosy • A combination of rifampin dapsone clofazimine

Drugs Used in Leprosy Dapsone & other sulfones • Inhibit folate synthesis • Combination of dapsone, rifampin and clofazimine is recommended to prevent resistant strains • Adverse reaction: hemolysis (esp. in patients with G 6 PD deficiency), erythema nodosum leprosum (ENL; can be suppressed by thalidomide or corticosteroids) Rifampin (rifampicin) • Inhibits RNA polymerase • Induces p 450 enzymes (potential drug interactions) ENL
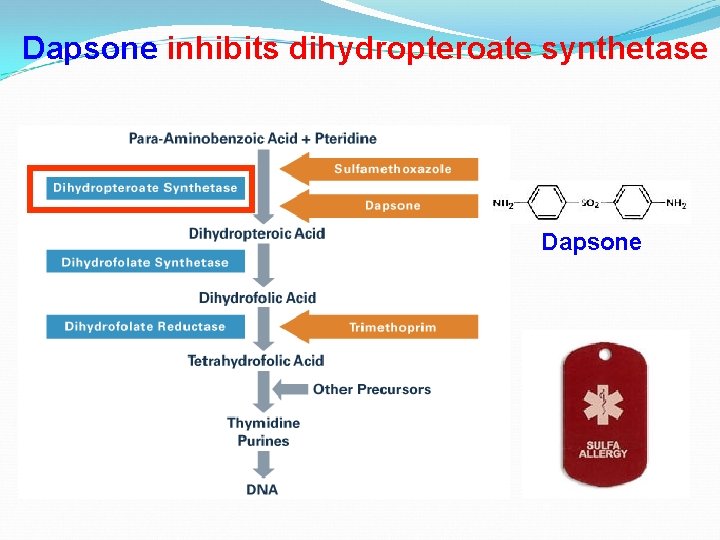
Dapsone inhibits dihydropteroate synthetase Dapsone

Drugs Used in Leprosy Clofazimine • A phenazine dye that can be used as an alternative to dapsone Immunosuppressive function • Lipophilic (accumulate in fatty & reticuloendothelial tissues) • Used for sulfone-resistant leprosy or when patients are intolerant to sulfones; useful in the treatment of erythema nodosum leprosum • Adverse reaction: GI intolerance, dry skin & discoloration

Drugs Used to treat Mycobacterial Infections Mycobacteria 1 st-line Therapy M. tuberculosis Isoniazid + rifampin* + pyrazinamide + ethambutol or streptomycin M. avium complex (MAC) Clarithromycin or azithromycin + ethambutol with or w/o rifabutin M. kansasii Isoniazid + rifampin* + ethambutol M. leprae Dapsone + rifampin ± clofazimine *In HIV-infected patients, the substitution of rifabutin for rifampin minimizes drug interactions with PI and NNRTI

REFERENCE Katzung, Chapter 47 https: //www. cdc. gov/tb/topic/basics/ http: //www. who. int/tb/en/ http: //www. who. int/lep/mdt/en/ http: //www. hrsa. gov/hansens/ Important drug interactions:
- Slides: 83