Lowering sugars in diabetes a cardiovascular waste of

Lowering sugars in diabetes – a cardiovascular waste of time? Hamish Courtney Regional Endocrine Centre Royal Victoria Hospital Belfast

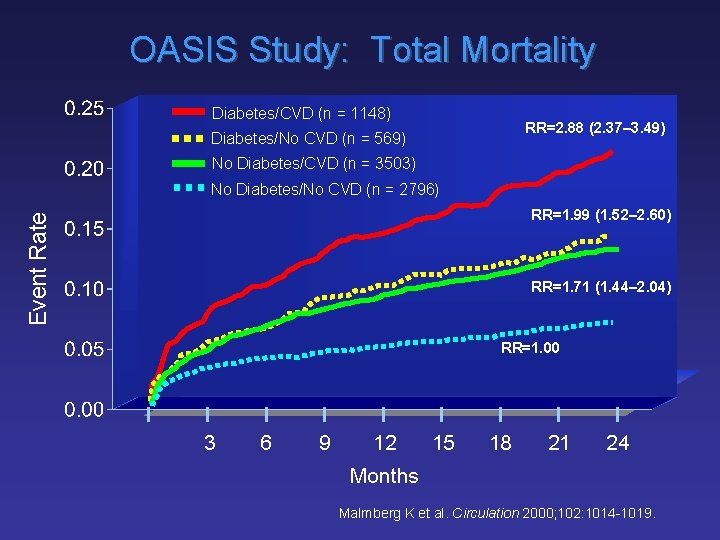
OASIS Study: Total Mortality Diabetes/CVD (n = 1148) RR=2. 88 (2. 37– 3. 49) Diabetes/No CVD (n = 569) No Diabetes/CVD (n = 3503) No Diabetes/No CVD (n = 2796) Event Rate RR=1. 99 (1. 52– 2. 60) RR=1. 71 (1. 44– 2. 04) RR=1. 00 3 6 9 12 15 18 21 24 Months Malmberg K et al. Circulation 2000; 102: 1014 -1019.
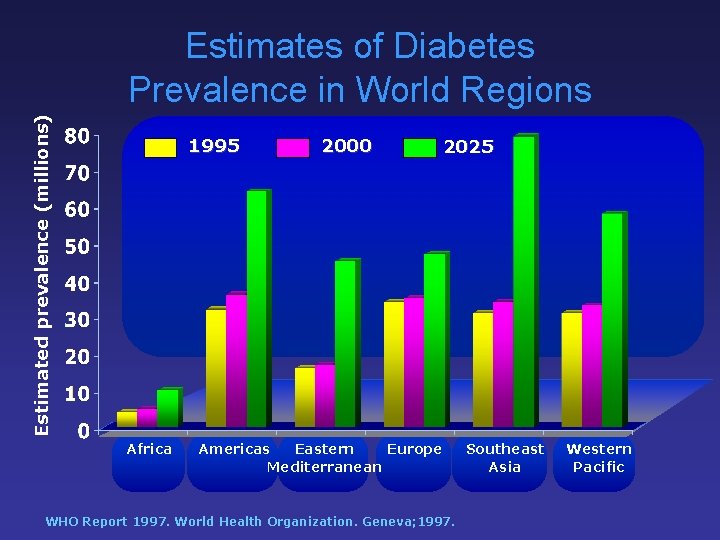
Estimated prevalence (millions) Estimates of Diabetes Prevalence in World Regions 1995 Africa 2000 2025 Americas Eastern Europe Mediterranean WHO Report 1997. World Health Organization. Geneva; 1997. Southeast Asia Western Pacific



How low can you go. . . safely?

UKPDS United Kingdom Prospective Diabetes Study
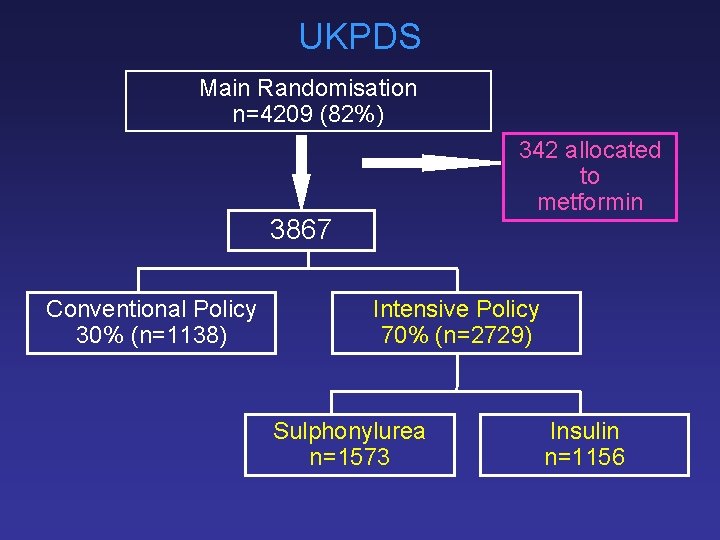
UKPDS Main Randomisation n=4209 (82%) 342 allocated to metformin 3867 Conventional Policy 30% (n=1138) Intensive Policy 70% (n=2729) Sulphonylurea n=1573 Insulin n=1156
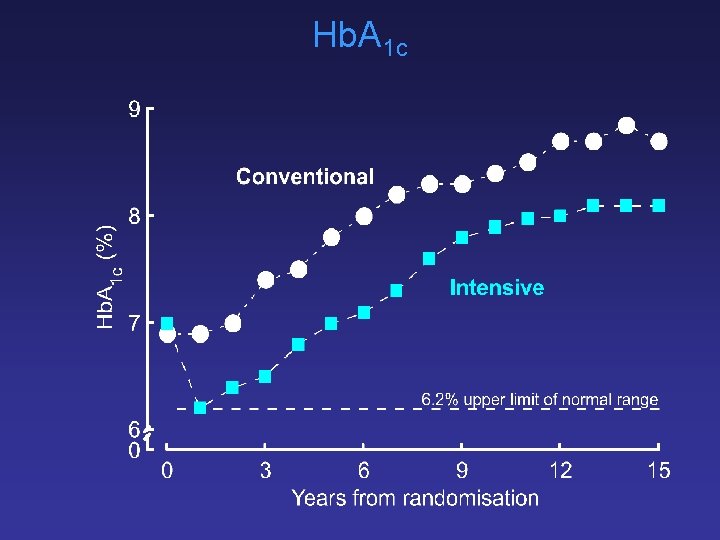
Hb. A 1 c
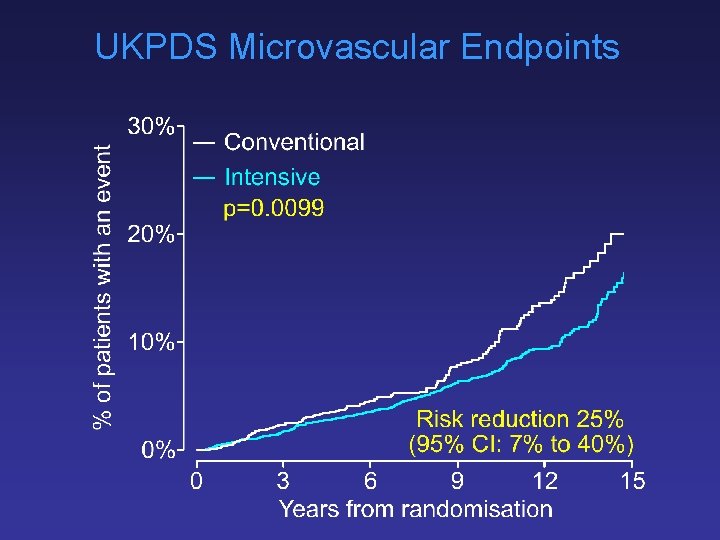
UKPDS Microvascular Endpoints

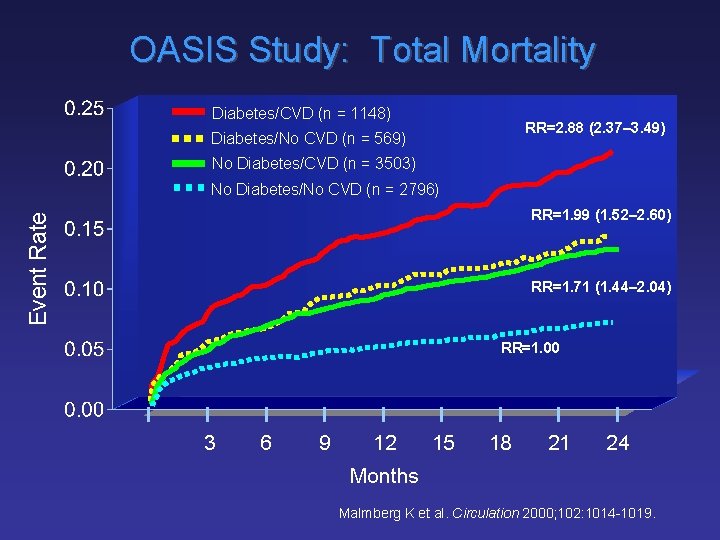
OASIS Study: Total Mortality Diabetes/CVD (n = 1148) RR=2. 88 (2. 37– 3. 49) Diabetes/No CVD (n = 569) No Diabetes/CVD (n = 3503) No Diabetes/No CVD (n = 2796) Event Rate RR=1. 99 (1. 52– 2. 60) RR=1. 71 (1. 44– 2. 04) RR=1. 00 3 6 9 12 15 18 21 24 Months Malmberg K et al. Circulation 2000; 102: 1014 -1019.
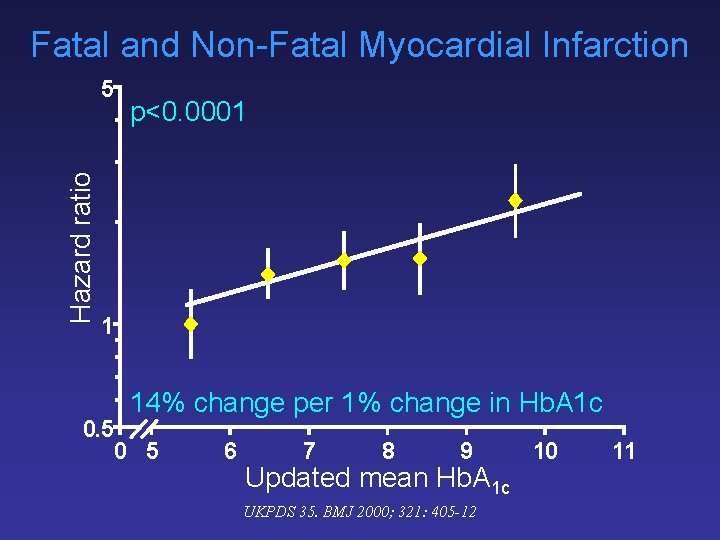
Fatal and Non-Fatal Myocardial Infarction Hazard ratio 5 p<0. 0001 1 14% change per 1% change in Hb. A 1 c 0. 5 0 5 6 7 8 9 Updated mean Hb. A 1 c UKPDS 35. BMJ 2000; 321: 405 -12 10 11
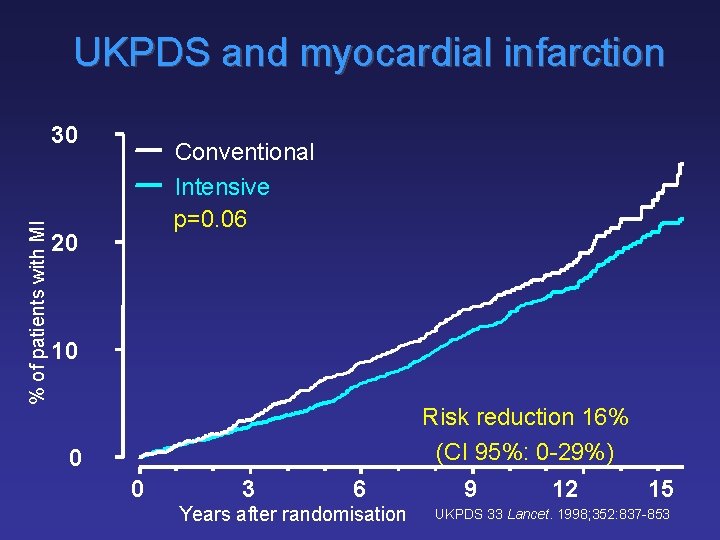
UKPDS and myocardial infarction % of patients with MI 30 Conventional Intensive p=0. 06 20 10 Risk reduction 16% (CI 95%: 0 -29%) 0 0 3 6 Years after randomisation 9 12 15 UKPDS 33 Lancet. 1998; 352: 837 -853
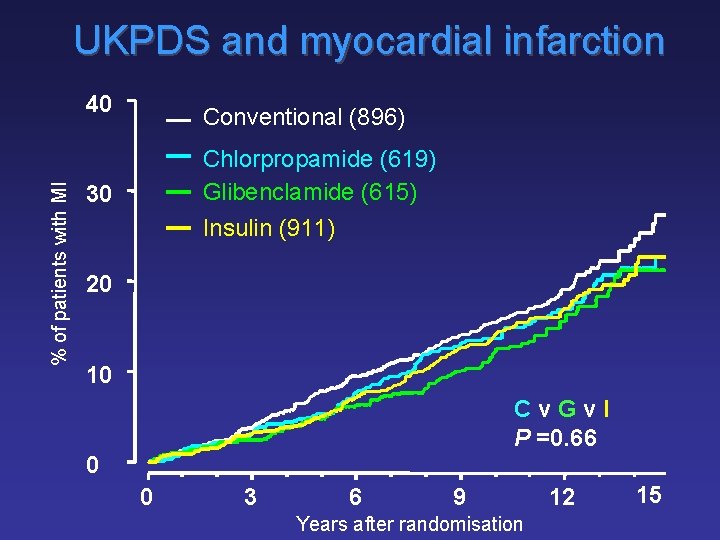
UKPDS and myocardial infarction % of patients with MI 40 Conventional (896) Chlorpropamide (619) Glibenclamide (615) Insulin (911) 30 20 10 Cv. Gv. I P =0. 66 0 0 3 6 9 Years after randomisation 12 15
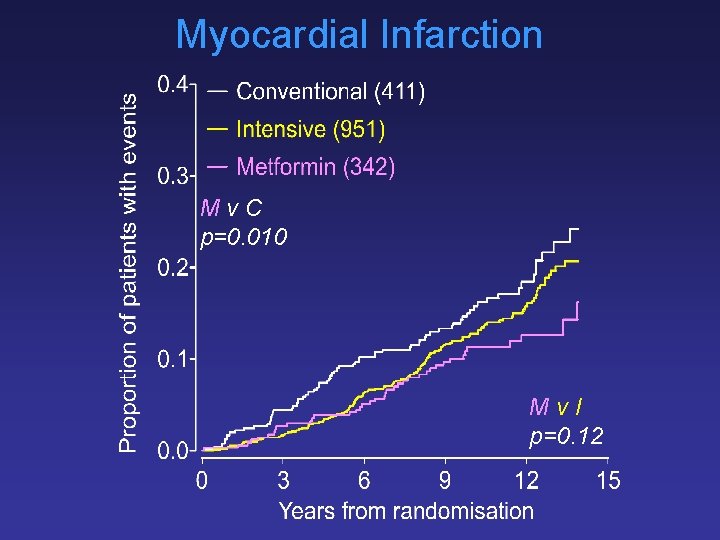
Myocardial Infarction Mv. C p=0. 010 Mv. I p=0. 12

University Group Diabetes Program (UGDP) North-American multicentre study Duration: 8 years (1961 -1969) 1027 patients randomised into 5 groups Placebo Tolbutamide Phenformin Insulin - diet - fixed dosage 1. 5 g/d - fixed dosage 100 mg/d - fixed dosage Insulin - adjusted dosage Klimt et al. Diabetes. 1970; 19(suppl 2): 747 -783
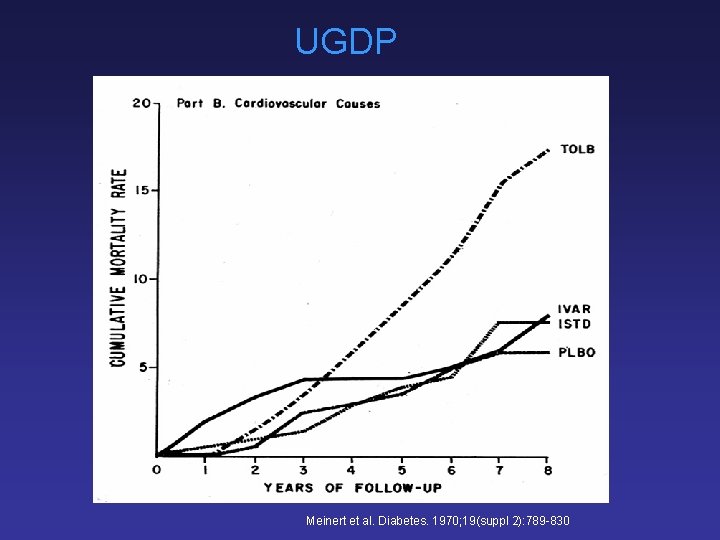
UGDP Meinert et al. Diabetes. 1970; 19(suppl 2): 789 -830

Intensive glycaemic control Does intensive glycaemic control reduce cardiovascular outcomes in T 2 DM? - ACCORD - ADVANCE - VADT - UKPDS follow up

ACCORD ADVANCE VADT Number 10251 11140 1791 Age (±SD) 62 ± 7 yrs 66 ± 6 yrs 60 ± 9 yrs Duration 10 yrs 8 yrs 11 yrs Hb. A 1 c 8. 1% 7. 5% 9. 4% Glycaemic intervention Agents <6 vs 77. 9% Any <6. 5% vs <6% vs local targets Gliclazide Any

ACCORD Glycaemic intervention Intensive (Hb. A 1 c <6%) vs Standard (Hb. A 1 c 7. 0 -7. 9%) Primary end point nonfatal MI, stroke or cardiovascular death
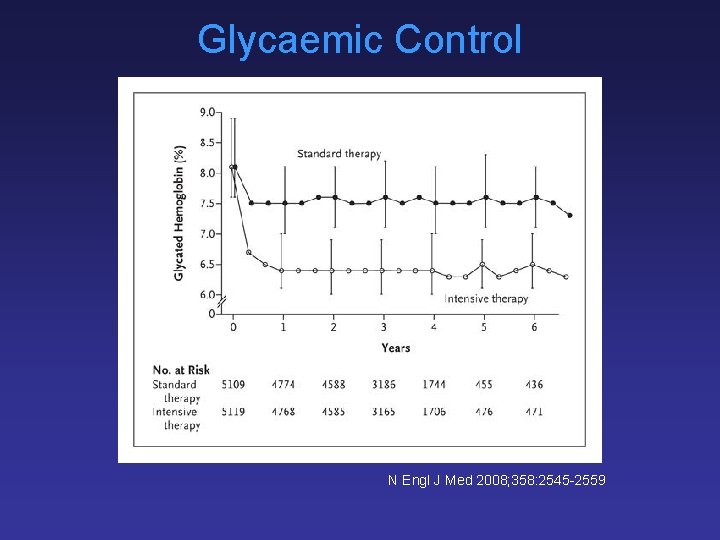
Glycaemic Control N Engl J Med 2008; 358: 2545 -2559
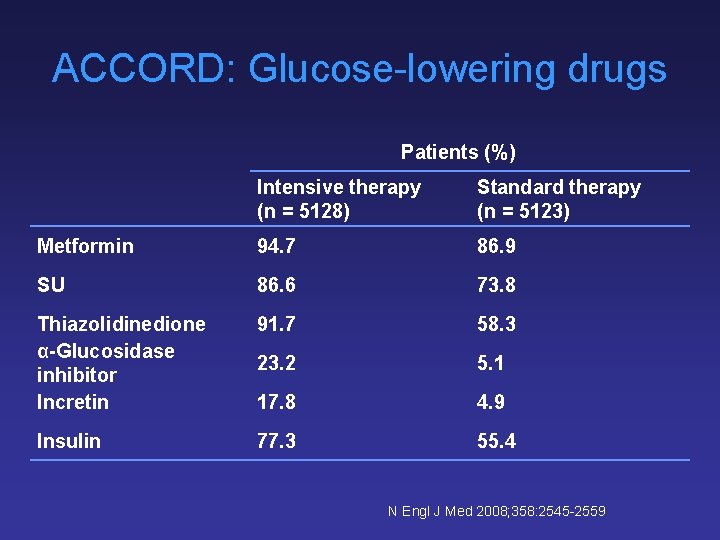
ACCORD: Glucose-lowering drugs Patients (%) Intensive therapy (n = 5128) Standard therapy (n = 5123) Metformin 94. 7 86. 9 SU 86. 6 73. 8 Thiazolidinedione α-Glucosidase inhibitor Incretin 91. 7 58. 3 23. 2 5. 1 17. 8 4. 9 Insulin 77. 3 55. 4 N Engl J Med 2008; 358: 2545 -2559

ACCORD Primary Outcome N Engl J Med 2008; 358: 2545 -2559

ADVANCE Glycaemic intervention Intensive using gliclazide (Hb. A 1 c <6. 5%) vs Standard (Hb. A 1 c to local guidelines) Primary end point composite macrovascular and microvascular events
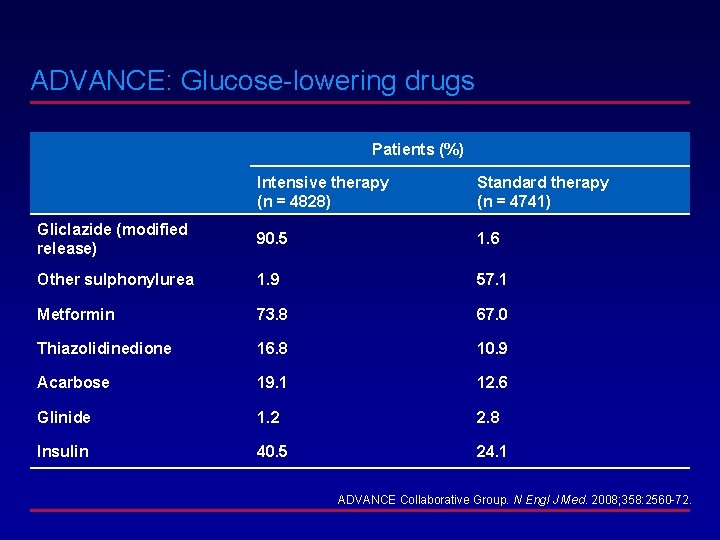
ADVANCE: Glucose-lowering drugs Patients (%) Intensive therapy (n = 4828) Standard therapy (n = 4741) Gliclazide (modified release) 90. 5 1. 6 Other sulphonylurea 1. 9 57. 1 Metformin 73. 8 67. 0 Thiazolidinedione 16. 8 10. 9 Acarbose 19. 1 12. 6 Glinide 1. 2 2. 8 Insulin 40. 5 24. 1 ADVANCE Collaborative Group. N Engl J Med. 2008; 358: 2560 -72.
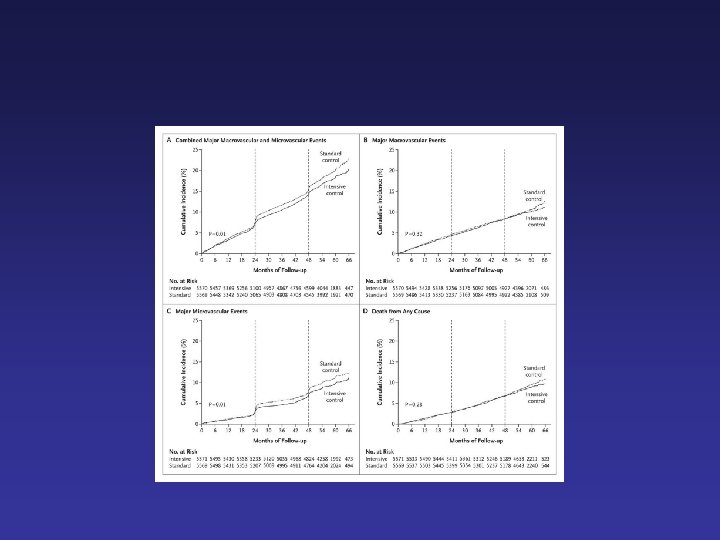
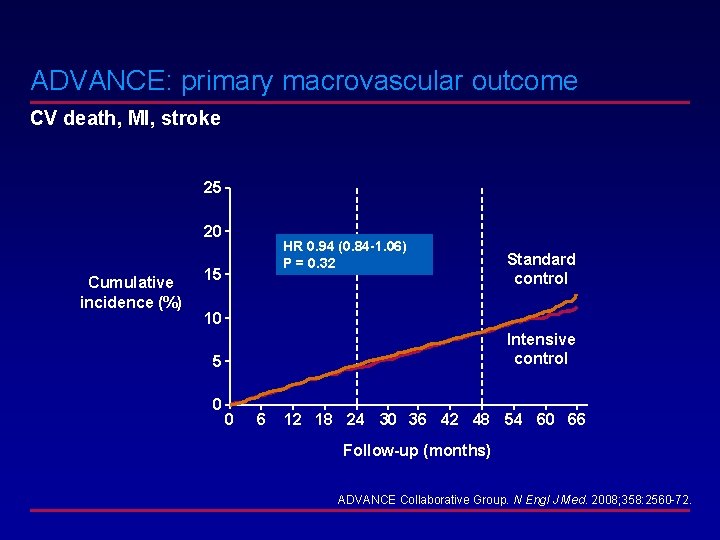
ADVANCE: primary macrovascular outcome CV death, MI, stroke 25 20 Cumulative incidence (%) HR 0. 94 (0. 84 -1. 06) P = 0. 32 15 Standard control 10 Intensive control 5 0 0 6 12 18 24 30 36 42 48 54 60 66 Follow-up (months) ADVANCE Collaborative Group. N Engl J Med. 2008; 358: 2560 -72.
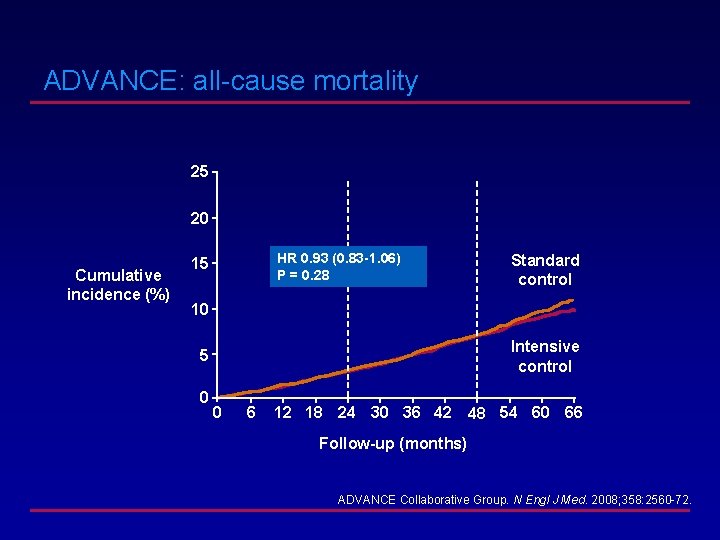
ADVANCE: all-cause mortality 25 20 Cumulative incidence (%) HR 0. 93 (0. 83 -1. 06) P = 0. 28 15 Standard control 10 Intensive control 5 0 0 6 12 18 24 30 36 42 48 54 60 66 Follow-up (months) ADVANCE Collaborative Group. N Engl J Med. 2008; 358: 2560 -72.
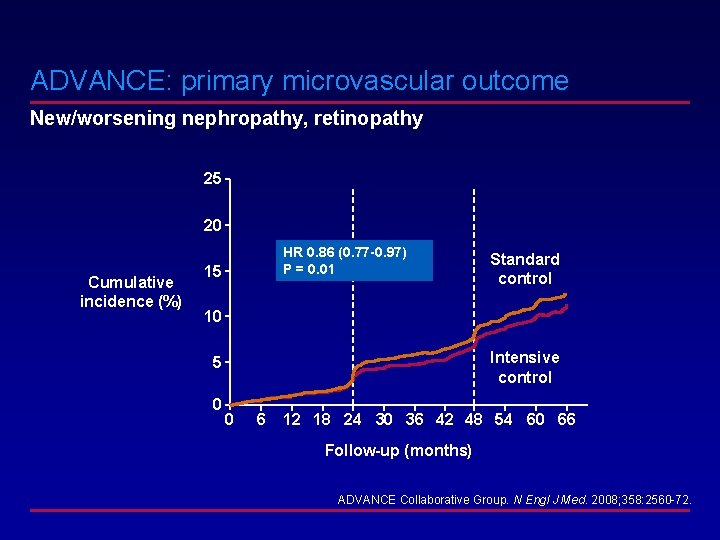
ADVANCE: primary microvascular outcome New/worsening nephropathy, retinopathy 25 20 Cumulative incidence (%) HR 0. 86 (0. 77 -0. 97) P = 0. 01 15 Standard control 10 Intensive control 5 0 0 6 12 18 24 30 36 42 48 54 60 66 Follow-up (months) ADVANCE Collaborative Group. N Engl J Med. 2008; 358: 2560 -72.

VADT Glycaemic intervention Intensive (Hb. A 1 c <6. 0%) vs Standard (Hb. A 1 c to local guidelines) Primary end point composite macrovascular event
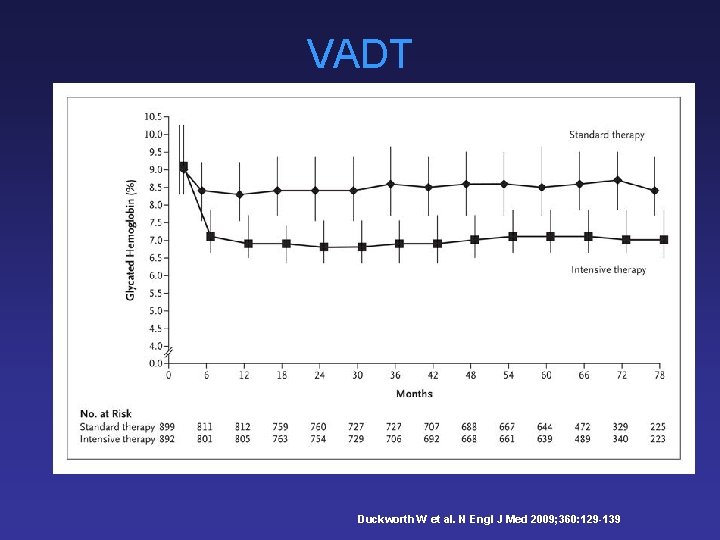
VADT Duckworth W et al. N Engl J Med 2009; 360: 129 -139
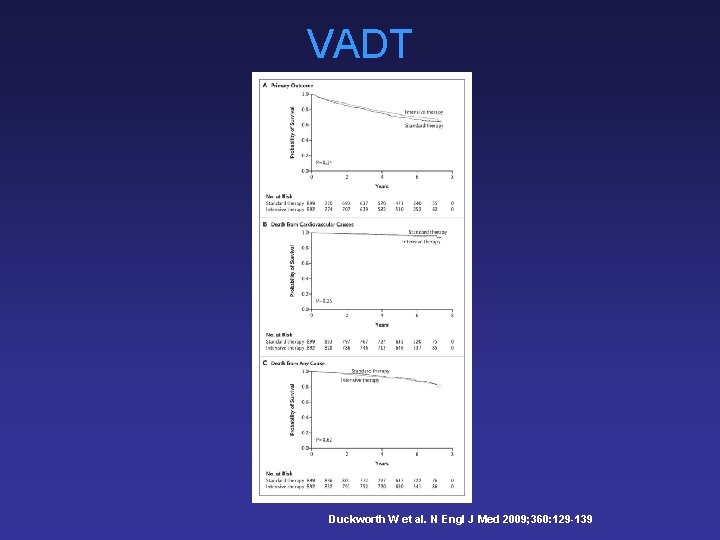
VADT Duckworth W et al. N Engl J Med 2009; 360: 129 -139


Reasons? Drugs used?
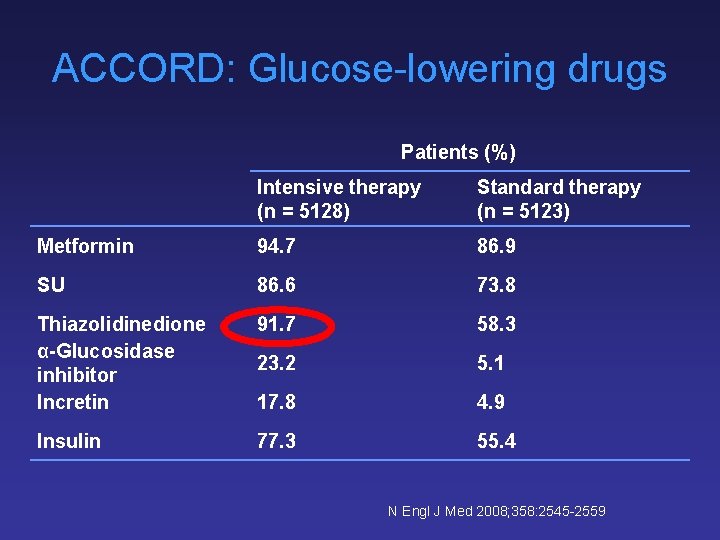
ACCORD: Glucose-lowering drugs Patients (%) Intensive therapy (n = 5128) Standard therapy (n = 5123) Metformin 94. 7 86. 9 SU 86. 6 73. 8 Thiazolidinedione α-Glucosidase inhibitor Incretin 91. 7 58. 3 23. 2 5. 1 17. 8 4. 9 Insulin 77. 3 55. 4 N Engl J Med 2008; 358: 2545 -2559

Reasons? Drugs used? Increase in hypoglycaemia? Increase in weight? Too rapid reduction in Hb. A 1 c?
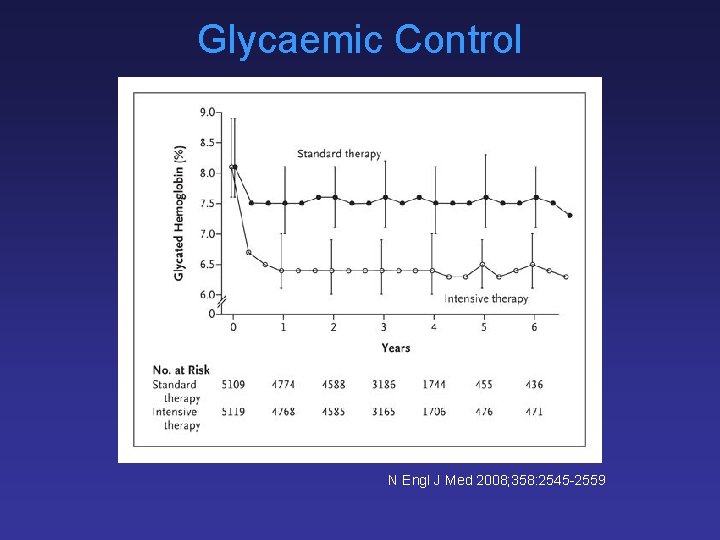
Glycaemic Control N Engl J Med 2008; 358: 2545 -2559

Reasons? Drugs used? Increase in hypoglycaemia? Increase in weight? Too rapid reduction in Hb. A 1 c? Chance?
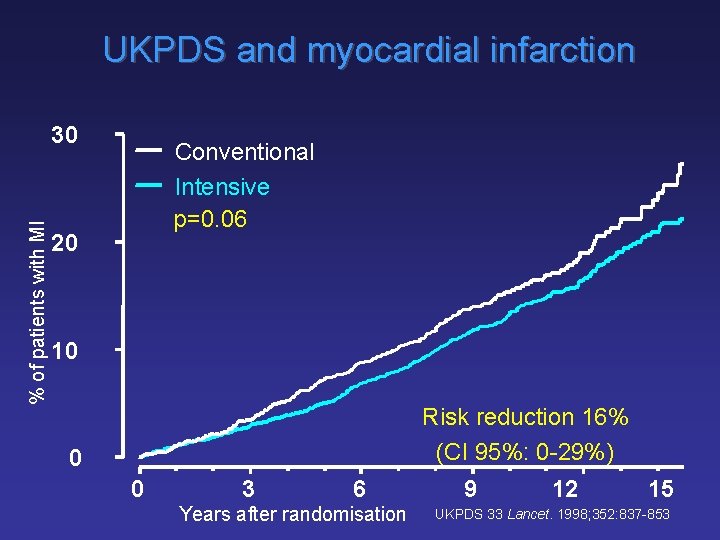
UKPDS and myocardial infarction % of patients with MI 30 Conventional Intensive p=0. 06 20 10 Risk reduction 16% (CI 95%: 0 -29%) 0 0 3 6 Years after randomisation 9 12 15 UKPDS 33 Lancet. 1998; 352: 837 -853
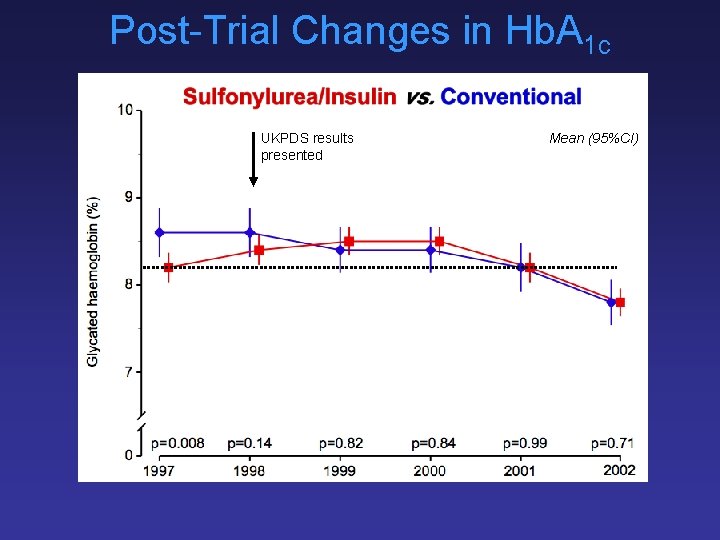
Post-Trial Changes in Hb. A 1 c UKPDS results presented Mean (95%CI)
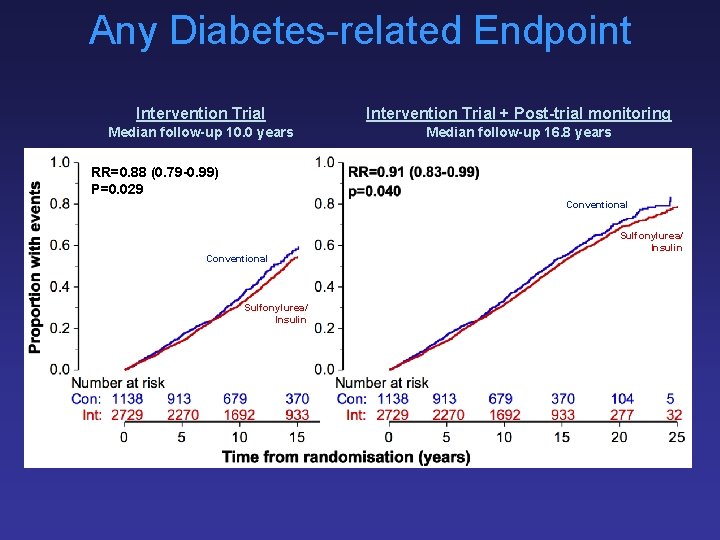
Any Diabetes-related Endpoint Intervention Trial + Post-trial monitoring Median follow-up 10. 0 years Median follow-up 16. 8 years RR=0. 88 (0. 79 -0. 99) P=0. 029 Conventional Sulfonylurea/ Insulin
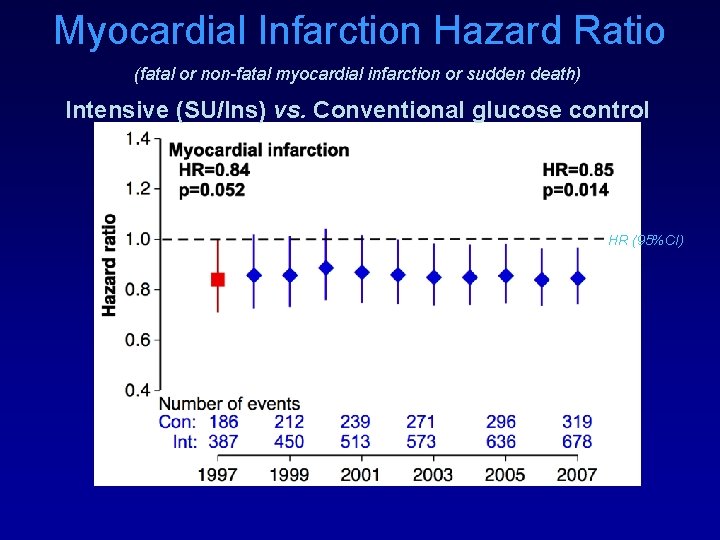
Myocardial Infarction Hazard Ratio (fatal or non-fatal myocardial infarction or sudden death) Intensive (SU/Ins) vs. Conventional glucose control HR (95%CI)
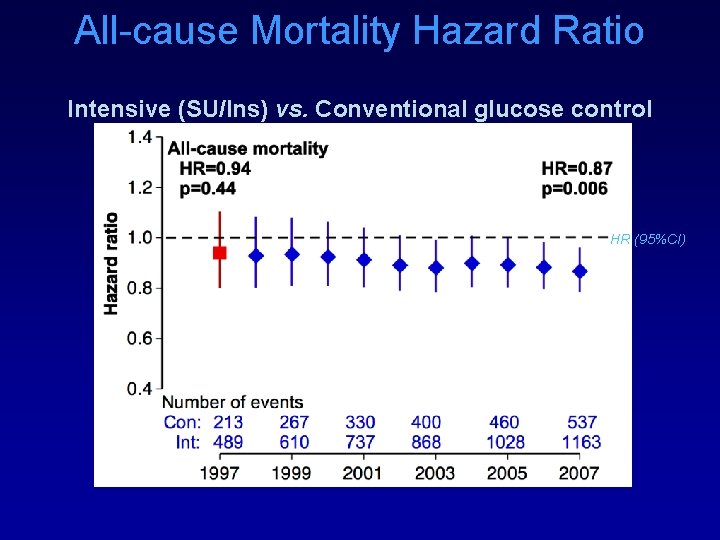
All-cause Mortality Hazard Ratio Intensive (SU/Ins) vs. Conventional glucose control HR (95%CI)
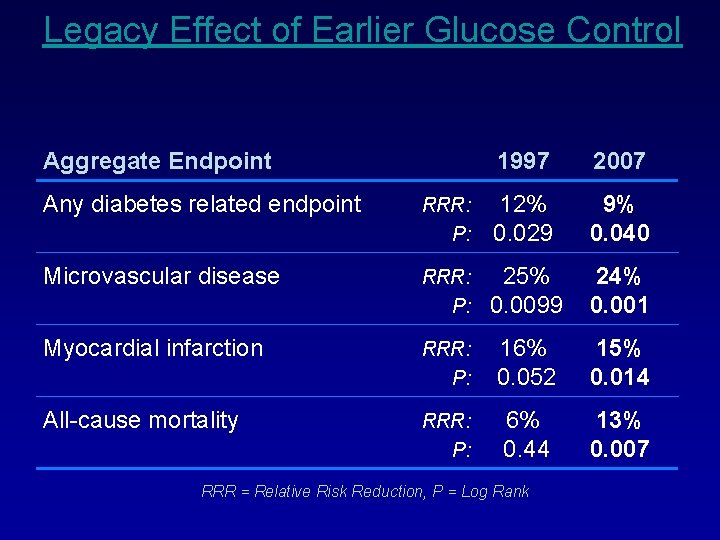
Legacy Effect of Earlier Glucose Control Aggregate Endpoint 1997 2007 Any diabetes related endpoint RRR: P: 12% 0. 029 9% 0. 040 Microvascular disease RRR: P: 25% 0. 0099 24% 0. 001 Myocardial infarction RRR: P: 16% 0. 052 15% 0. 014 All-cause mortality RRR: P: 6% 0. 44 13% 0. 007 RRR = Relative Risk Reduction, P = Log Rank

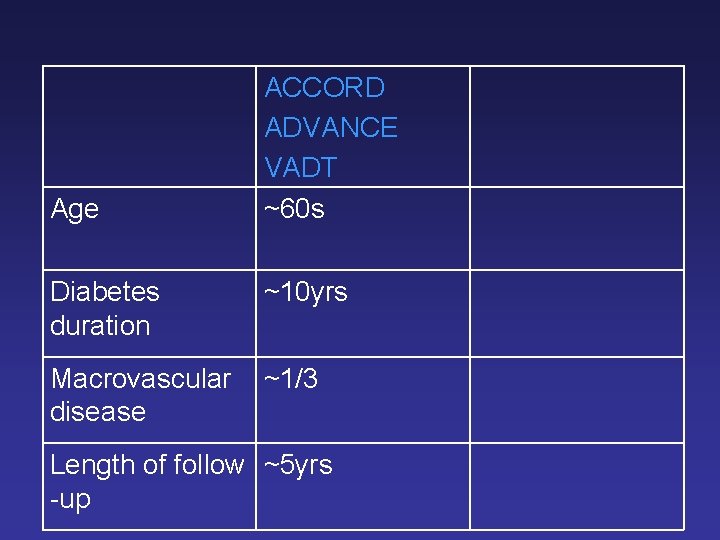
Age ACCORD ADVANCE VADT ~60 s Diabetes duration ~10 yrs Macrovascular disease ~1/3 Length of follow ~5 yrs -up
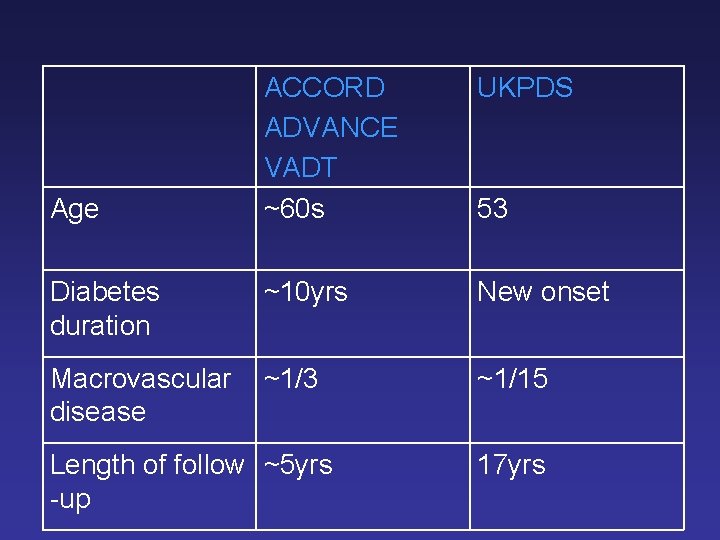
ACCORD ADVANCE VADT ~60 s UKPDS Diabetes duration ~10 yrs New onset Macrovascular disease ~1/3 ~1/15 Age Length of follow ~5 yrs -up 53 17 yrs
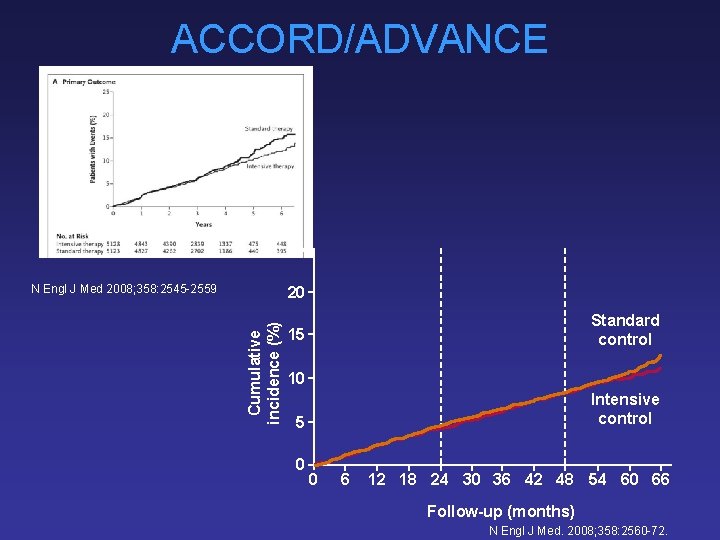
ACCORD/ADVANCE 25 N Engl J Med 2008; 358: 2545 -2559 Cumulative incidence (%) 20 Standard control 15 10 Intensive control 5 0 0 6 12 18 24 30 36 42 48 54 60 66 Follow-up (months) N Engl J Med. 2008; 358: 2560 -72.

Glucose lowering? 1. Glucose lowering reduces microvascular complications 2. Intensive glucose lowering with complex regimens in patients with “established” diabetes is unlikely to have a short term cardiovascular benefit and may indeed be harmful

Glucose lowering? 3. The presence of a legacy effect argues for early intensive glucose lowering 4. Target Hb. A 1 c to 6. 5% except where this requires complex treatment regimens or life expectancy is less than 5 years
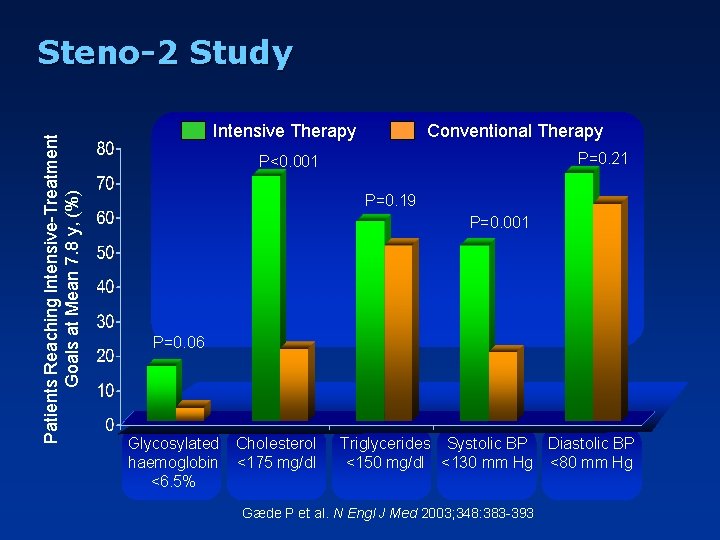
Patients Reaching Intensive-Treatment Goals at Mean 7. 8 y, (%) Steno-2 Study Intensive Therapy Conventional Therapy P=0. 21 P<0. 001 P=0. 19 P=0. 001 P=0. 06 Glycosylated haemoglobin <6. 5% Cholesterol <175 mg/dl Triglycerides Systolic BP Diastolic BP <150 mg/dl <130 mm Hg <80 mm Hg Gæde P et al. N Engl J Med 2003; 348: 383 -393 Slide Source Lipids Online Slide Library www. lipidsonline. org
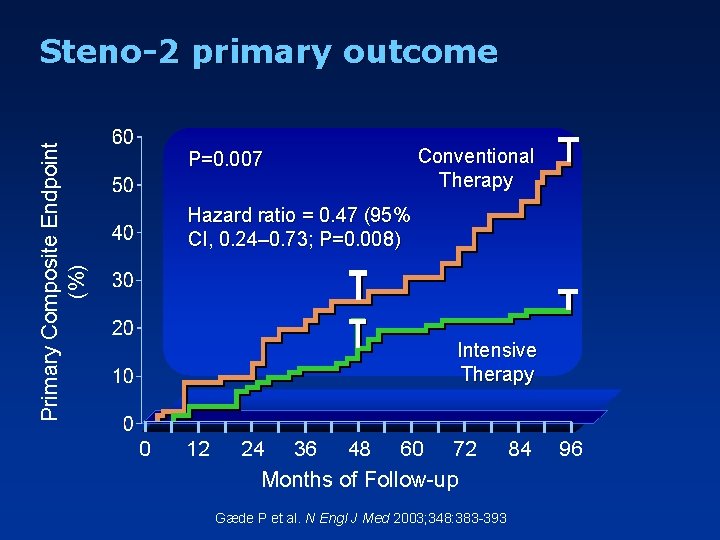
Primary Composite Endpoint (%) Steno-2 primary outcome P=0. 007 Conventional Therapy Hazard ratio = 0. 47 (95% CI, 0. 24– 0. 73; P=0. 008) Intensive Therapy 0 12 24 36 48 60 72 Months of Follow-up Gæde P et al. N Engl J Med 2003; 348: 383 -393 84 96 Slide Source Lipids Online Slide Library www. lipidsonline. org
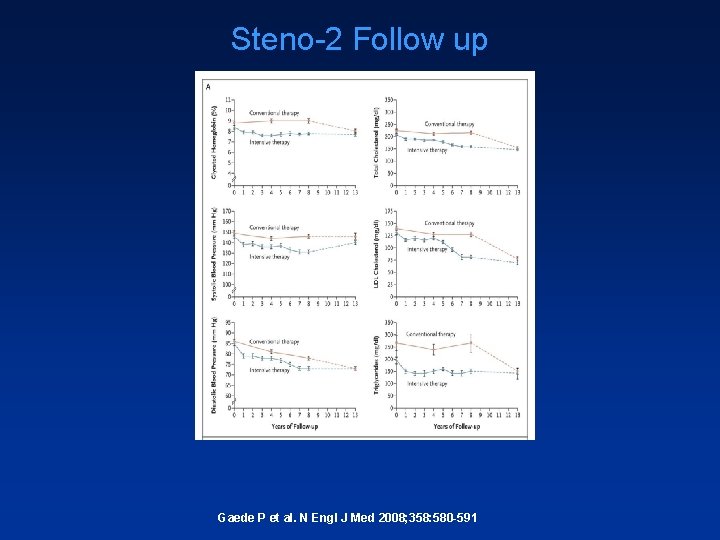
Steno-2 Follow up Gaede P et al. N Engl J Med 2008; 358: 580 -591 Slide Source Lipids Online Slide Library www. lipidsonline. org
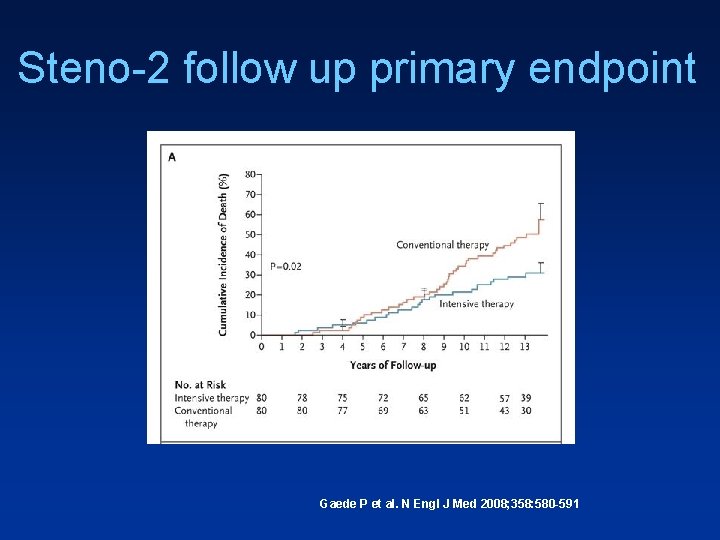
Steno-2 follow up primary endpoint Gaede P et al. N Engl J Med 2008; 358: 580 -591
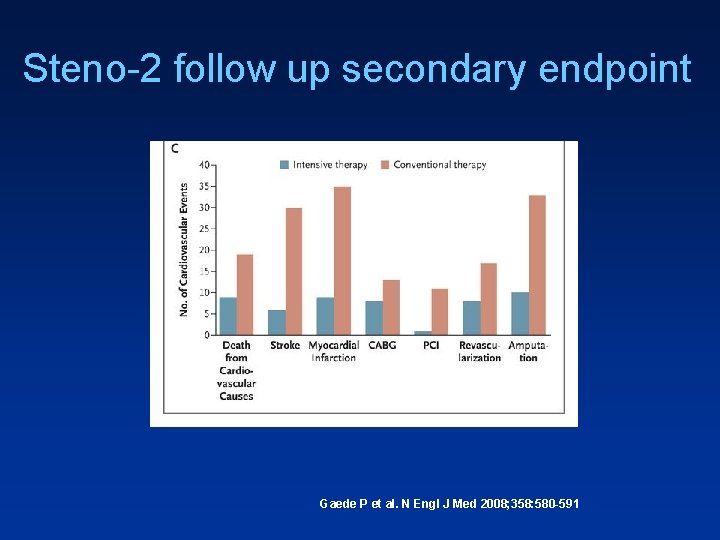
Steno-2 follow up secondary endpoint Gaede P et al. N Engl J Med 2008; 358: 580 -591

Glucose lowering – waste of time? § Glucose lowering, started early, may have long term cardiovascular benefits § Multifactorial risk reduction is imperative
- Slides: 58