Lower limb mobilization Initiation and Progression of Treatment
Lower limb mobilization

Initiation and Progression of Treatment a. Prepare the tissue around the joint prior to stretching with soft tissue mobilization, or muscle relaxation techniques. The initial treatment is the same whether treating for pain or increased joint play. The purpose is to determine joint reactivity before proceeding.

Grades of oscillation techniques (Maitland technique) Grade I: Small amplitude rhythmic oscillations at the beginning of the range Grade II: Large amplitude rhythmic oscillations within the range, not reaching the limit (till resistance occurred). Grade III: Large amplitude rhythmic oscillations up to the limit of the available motion (till muscle spasm) Grade IV: Very small amplitude rhythmic oscillations at the limit of the available motion (at the end of range). Grade V: (Joint manipulation) small amplitude, high velocity thrust technique is performed to snap adhesions at the limit of the available motion.


Grade I, 2 is used for relief of pain - Grade 3, 4 • is used to stretch the joint structures, and increase joint play. • Increase periarticular extensibility • Correct positional faults • Released impinged meniscoid tissue All grades of oscillation increase nutrition to articular structures Grade 5 is used to redduce spinal disc herniation and also are appropriate when grades 3, 4 have failed to accomblish the goal of treatment
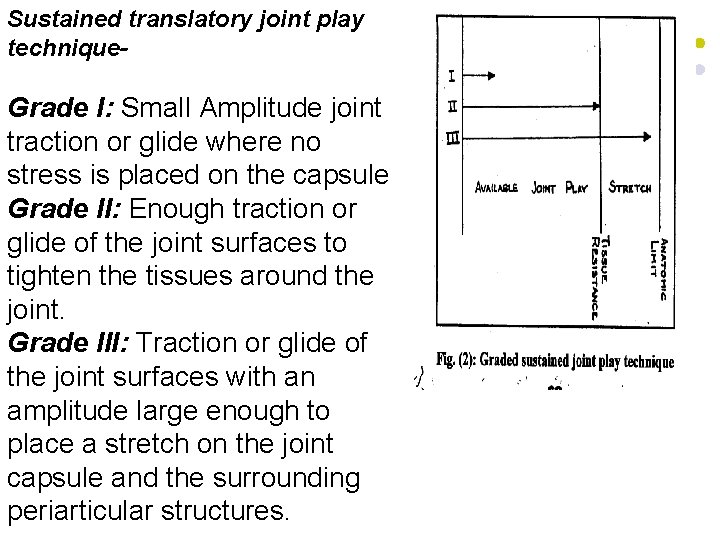
Sustained translatory joint play technique Grade I: Small Amplitude joint traction or glide where no stress is placed on the capsule Grade II: Enough traction or glide of the joint surfaces to tighten the tissues around the joint. Grade III: Traction or glide of the joint surfaces with an amplitude large enough to place a stretch on the joint capsule and the surrounding periarticular structures.

Grade I is used for relief of pain - - Grade II is used for the initial treatment to determine how sensitive the joint is. Grade III: is used to stretch the joint structures, and increase joint play to separate

Use a sustained Grade II distraction of the joint surfaces with the joint held in resting position or the position of greatest relaxation. Note the immedi ate joint response relative to irritability and range.

The next day, evaluate joint response. If there is increased pain and sensitivity, reduce the amplitude of treatment to Grade I oscillations. if the joint is the same or better. (1)Repeat the same maneuver if the goal of treatment is to maintain joint play. (2)Or progress the maneuver to sustained Grade III traction or glides if the goal of treatment is to increase joint play.

As the range plateaus, move the joint to the end of the available range of motion, then apply the sustained Grade III distraction or glide techniques. Advanced progressions include rotating the part at the end of the available range prior to applying Grade III distraction or glide techniques. b. When using sustained gliding techniques, a Grade I distraction should be used with it. A Grade II or III distraction should not be used with Grade III glide in order to avoid excessive trauma to the joint.

c. If gliding in the restricted direction is too painful, begin gliding mobilization in the painless direction. Progress to gliding in the restricted direction when mobility improves a little and it is not painful, d. When applying stretching techniques, move the bony partner through the available range of joint play first, that is, "take up the slack. when tissue resistance is felt, apply the stretch force against the restriction.

. 5 To maintain joint play by using gliding techniques when range of motion techniques are contraindication or not possible for a period of time. Use sustained Grade II or Grade II oscillation techniques. Speed, Rhythm, and Duration of Movements oscillations" a. Apply smooth, regular oscillations, at 2 or 3 per second , for 1 or 2 minutes b. Vary the speed of oscillations for different effects such as amplitude, high speed to inhibit pain, or slow speed to relax muscle guarding. .

2 - Sustained' a. For painful joints, apply intermittent distraction for 10 seconds with few seconds of rest in between for several cycles. Note response and either repeat or discontinue. b. For restricted joints apply a minimum of a 6 second stretch force, followed by partial release (to Grade I or II), then repeat at 3 to 4 second intervals.

Treatment Soreness Stretching maneuvers usually cause soreness. Perform the maneuvers on alternate days in order to allow soreness to decrease and tissue healing to occur between stretching sessions. If there is increased pain after 24 hours, the dosage (amplitude) or duration of treatment was too vigorous. Decrease the dosage or duration until the pain is under control.

K. Reassessment The patient's joint and range of motion should be reassessed after treatment and again before the next treatment. Alterations in treatment are dictated by the joint response. I. Total Program Mobilization techniques are one part of a total treatment for decreased func tion. Therapy should also include appropriate range of motion, strengthening, and functional techniques

The hip joint is a ball and socket joint. It deforms in weight bearing to increase congruency between the two joint surfaces. Its construction is similar to that of the shoulder, but the hip is far more stable.

This is due to: • negative intracapsular atmospheric pressure, • a stronger joint capsule, • a more spherical femoral head, • and a deeper socket made even deeper by the labrum , which provides greater joint surface contact area.

Most functional activities occur between 0 and 120 degrees of flexion and between 0 and 20 degrees of both external rotation and abduction. Because of the oblique angulation of the acetabulum and the femoral angle of inclination, flexion is restored by dorsally gliding the femur and extension by ventrally gliding the femur.

ABDUCTION AND ADDUCTION • Abduction is restored by caudally gliding the femur, • and adduction by laterally gliding the femur. ROTATION • • External rotation is restored by ventrally gliding the femur, • and internal rotation by dorsally and laterally gliding the femur. Internal rotation can be restored by performing the two glides separately or in combination with one another
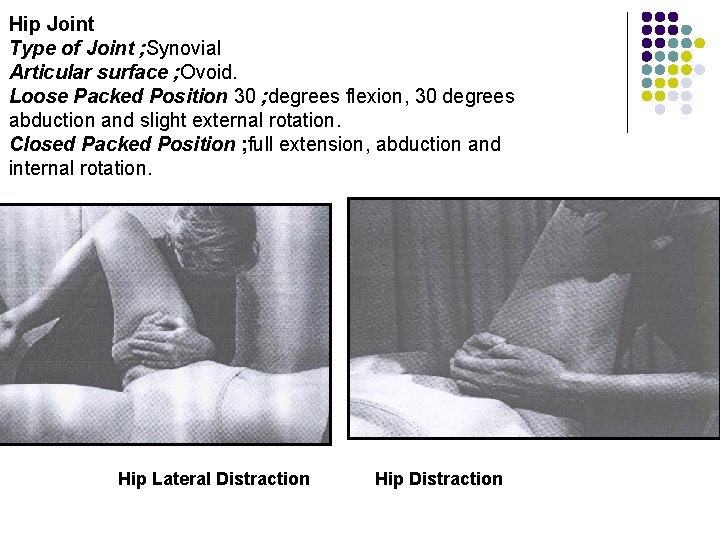
Hip Joint Type of Joint ; Synovial Articular surface ; Ovoid. Loose Packed Position 30 ; degrees flexion, 30 degrees abduction and slight external rotation. Closed Packed Position ; full extension, abduction and internal rotation. Hip Lateral Distraction Hip Distraction
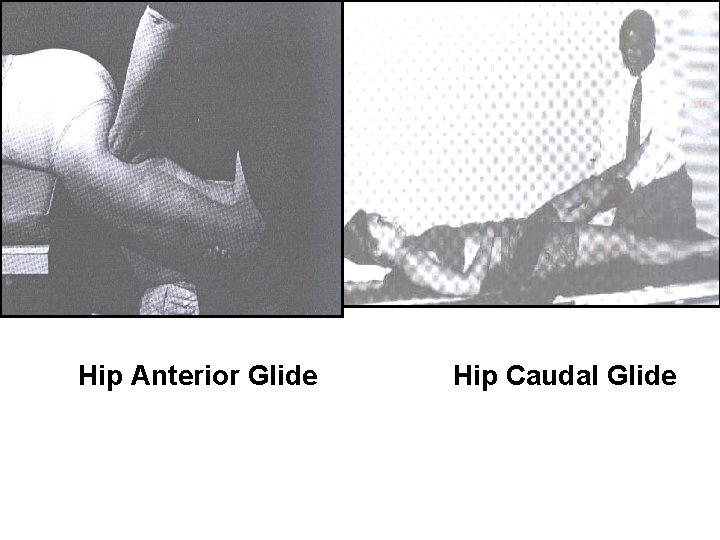
Hip Anterior Glide Hip Caudal Glide
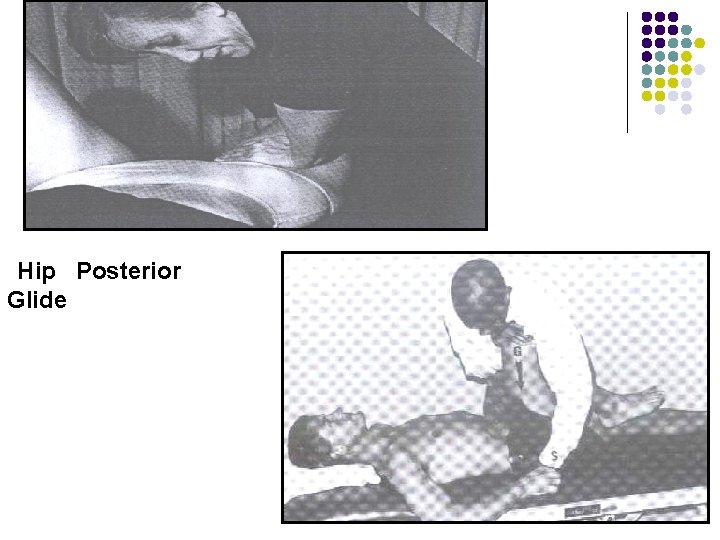
Hip Posterior Glide

The knee joint consists of two sets of articulating surfaces, the tibiofemoral joint and the patellofemoral joint. To perform most activities of daily living, these two joints surfaces must permit at least 110 degrees of motion in the sagittal plane, 15 degrees in the frontal plane, and 15 degrees of rotation

FLEXION AND EXTENSION Flexion at the knee is accompanied by internal rotation and adduction of the tibia, and extension is accompanied by external rotation and abduction'. External rotation occurs during the last 30 degrees of extension. This rotational motion is produced by tightening of ligamentous structures and by muscular forces, as well as by the configuration of the two articular surfaces.

Flexion is accompanied by dorsal gliding and rolling of the tibia on the femur, and extension by a similar ventral motion. The lateral femoral condyle moves more than two times farther than does the medial femoral condyle. The relative ratio of rolling to gliding at the lateral joint is approximately equal, whereas medially, gliding is the predominant motion. This partially explains why external rotation accompanies extension and internal rotation ac companies flexion.

To restore normal knee biomechanics , it therefore may be necessary to ensure that a greater amount of motion exists laterally and that the appropriate amount of gliding relative to rolling is restored at both the medial and lateral articulations. Oscillations are extremely important for restoring motion to the tibiofemoral joint. Most often the manipulations to increase knee motion involve dorsal and ventral gliding. Because the femur is a convex articulation on a concave tibia, the manipulation glide is in the direction of the restriction.

Excessive medial and lateral motion is prevented by the spine of the tibia and its articulation into the femoral condylar notch. The patellofemoral joint moves 5 to 7 cm cranially in the femoral groove as the knee extends. It is positioned laterally when the knee is in full flexion, glides medially as the knee begins to extend, and returns to a slightly more lateral position as the knee approaches full extension.

The five facets on the dorsal side of the patella compose the patellar articulation with the femoral groove. The patellar surface is convex on a concave femur. The direction in which the patella is glided corresponds to the motion being restored, despite the fact that the moving bone is convex. This is because the ventral surface of the patella tilts in the direction opposite the ' restriction when the patella is glided in the direction of the restriction.

A careful evaluation should precede lateral glide techniques, as this motion is sometimes hypermobile in dysfunctional knees, and if hypermobility is present, treatment with lateral gliding could cause the patella to sublux laterally. Conversely, dysfunction at the patellofemoral joint frequently results from decreased medial gliding.
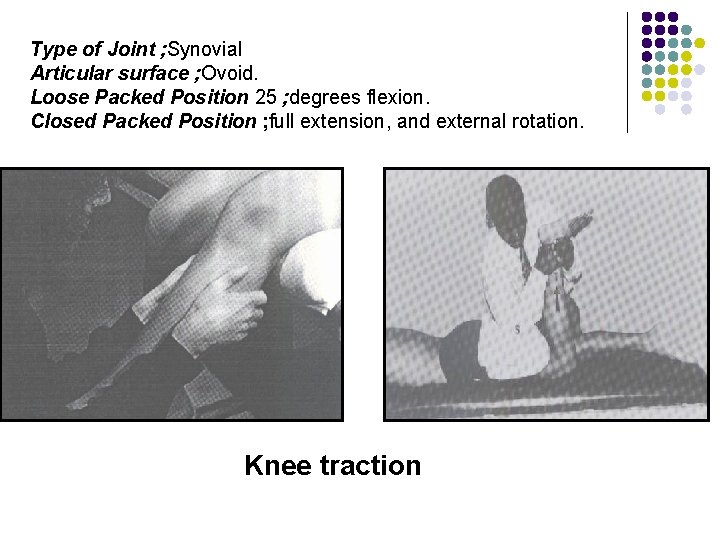
Type of Joint ; Synovial Articular surface ; Ovoid. Loose Packed Position 25 ; degrees flexion. Closed Packed Position ; full extension, and external rotation. Knee traction
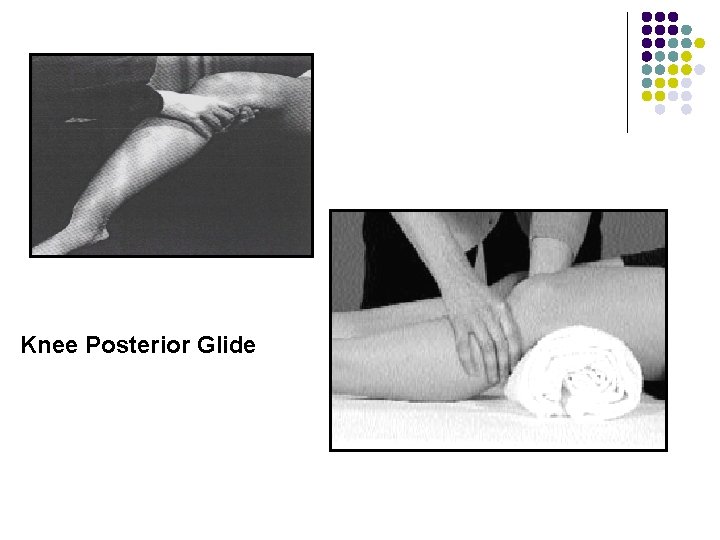
Knee Posterior Glide
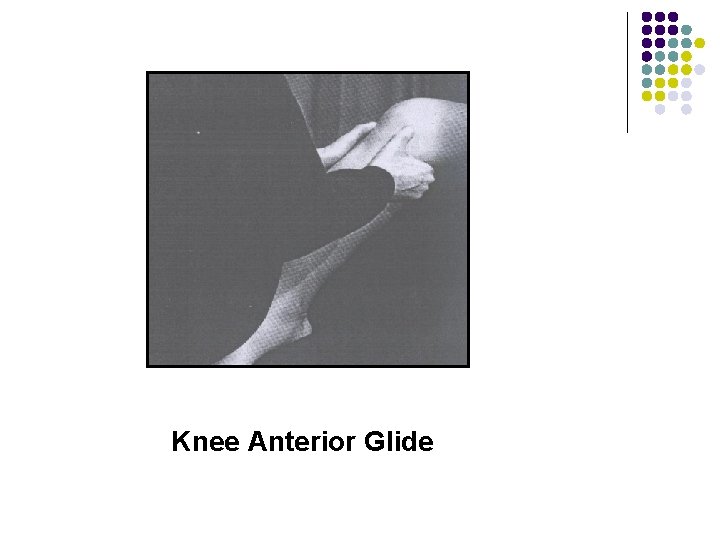
Knee Anterior Glide
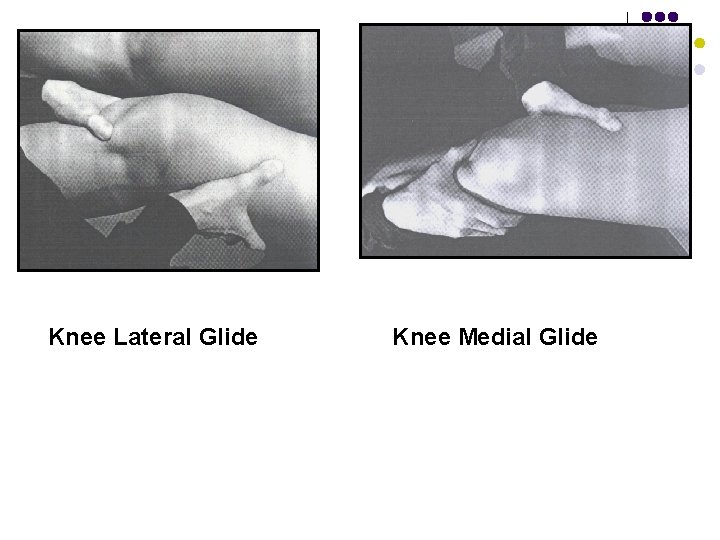
Knee Lateral Glide Knee Medial Glide
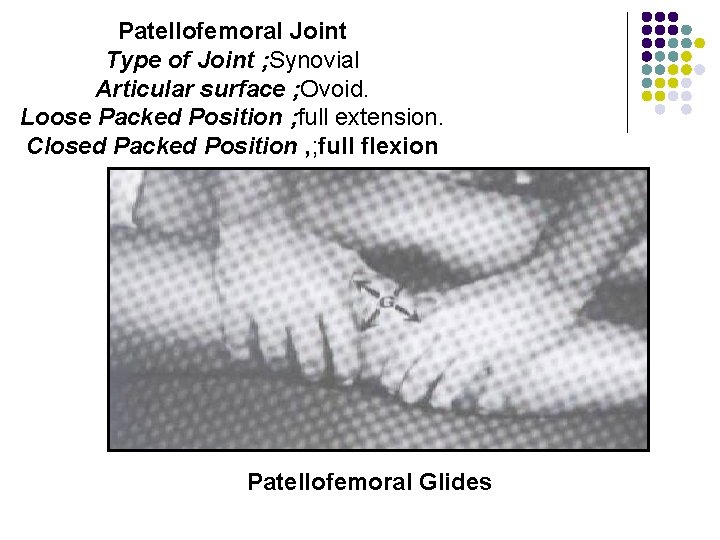
Patellofemoral Joint Type of Joint ; Synovial Articular surface ; Ovoid. Loose Packed Position ; full extension. Closed Packed Position , ; full flexion Patellofemoral Glides

The lower leg consists of the proximal and distal tibiofibular joints. Motion at the tibiofibular joints corresponds primarily with motion at the foot, although a small degree of fibular ventral. movement occurs with knee flexion. Because the tibia and fibula are connected by the inter osseus membrane, movement at the two joints is interrelated in a manner similar to that of the proximal and distal radioulnar joints of the forearm.

Positional faults are not uncommon at the proximal tibiofibular joint. A dorsal positional fault is especially common after an inversion injury of the ankle. DORSIFLEXION AND PLANTAR FLEXION With dorsiflexion the fibula glides cranially, and rotates laterally. With plantar flexion it glides caudally. Distracting the distal tibiofibular joint therefore may help restore ankle dorsiflexion. Motion is so slight at both of these joints, however, that it is doubtful that either ankle or knee motion will improve significantly after manipulation to these joints. In addition, these joints are often hypermobile. A careful evaluation therefore should precede any manipulation of the tibiofibular joints.

(Ankle) Joint Type of Joint ; Synovial. Articular surface ; Sellar. Loose Packed Position 10 ; degrees planterflexion, midway between inversion and eversion. Closed Packed Position , ; full dorsiflexion Ankle Distraction
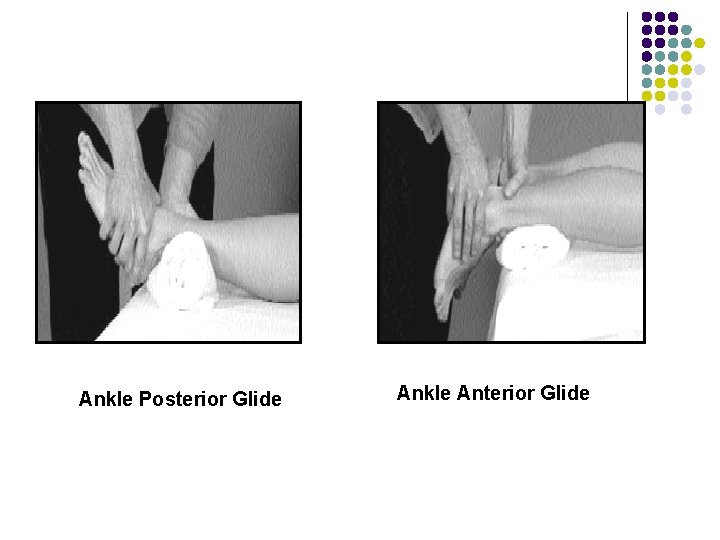
Ankle Posterior Glide Ankle Anterior Glide
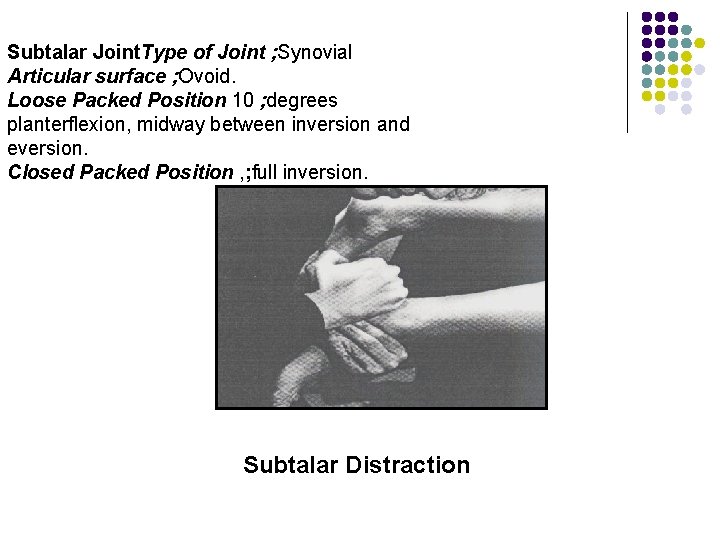
Subtalar Joint. Type of Joint ; Synovial Articular surface ; Ovoid. Loose Packed Position 10 ; degrees planterflexion, midway between inversion and eversion. Closed Packed Position , ; full inversion. Subtalar Distraction

Subtalar Medial and Lateral Glides
- Slides: 40