Low Dose Prophylaxis Lisa N Boggio MS MD

Low Dose Prophylaxis Lisa N Boggio, MS, MD RUSH University Medical Center Chicago, Illinois USA © Rush University Medical Center 2016

Treatment Regimens Before Blood Products n Avoidance of activity n R. I. C. E. – Rest, Ice Compression, Elevation n Quackery n Alternative medicine 90% of persons with hemophilia were dead by age 21 © Rush University Medical Center 2016

Treatment n 1940 s FFP n 1950 -60 s Cryoprecipitate n 1970 s purified FVIII +v. WF n 1980 s highly purified FVIII and IX n 1990 s recombinant FVIII and IX n 2000 s recombinant FVIII with little or no human proteins n 2010 s prolonged half life Hambleton J. Curr Opin Hematol. 2001; 8: 306 -311. © Rush University Medical Center 2016
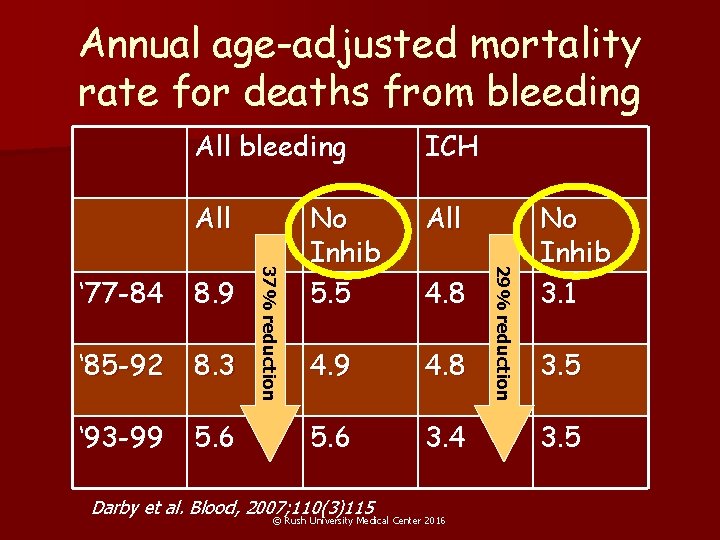
Annual age-adjusted mortality rate for deaths from bleeding All No Inhib 5. 5 All 4. 9 4. 8 5. 6 3. 4 ‘ 77 -84 8. 9 ‘ 85 -92 8. 3 ‘ 93 -99 5. 6 Darby et al. Blood, 2007; 110(3)115 4. 8 © Rush University Medical Center 2016 29% reduction ICH 37% reduction All bleeding No Inhib 3. 1 3. 5

Mortality severe Darby et al. Blood, 2007; 110(3)815 © Rush University Medical Center 2016

Joint Scope of n Occurs n Joint Disease: the Problem in 90% of severe hemophilia bleeds per year: 15 + 12 n Restriction in activity: at least 50% of patients Aledort L. J Int Med. 1994; 236: 391 © Rush University Medical Center 2016

Development of Joint Disease n Synovial membrane vessels bleed into articular space n Iron inflammatory reaction n Synovium hyperemic and hypertrophic n Eventual cartilage/bone destruction © Rush University Medical Center 2016

Elbow XRAY © Rush University Medical Center 2016
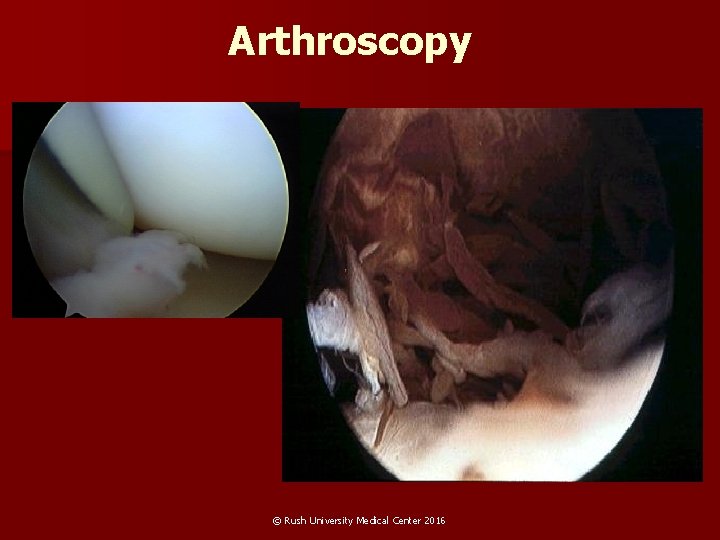
Arthroscopy © Rush University Medical Center 2016

On Demand Therapy n Does not prevent the development of hemarthrosis n In the US, Cost $130, 102/yr n Prophylaxis – Better outcomes – More normal life – More cost Globe DR. Haemophilia 2004. 10(Sup 1): 63 -70 © Rush University Medical Center 2016

Prophylaxis – Early Studies Dose and interval are important Factor Dose No prophylaxis Bleeds/Month 5. 5 4 U/kg/day 2. 5 8 U/kg/day* 1. 5 24 U/kg 3 x/wk 1. 0 32 U/kg once/wk 4. 5 * Cost equivalent: no prophylaxis Kasper. Arch Intern Med. 1970; 125: 1004. © Rush University Medical Center 2016

Secondary Prophylaxis for Joint Disease Conclusions: 1) Physical findings generally improve 2) X-ray: stable to progressive deterioration © Rush University Medical Center 2016

When to Start: Swedish Experience Patients: n = 121; age <10; at least one infusion/week n Decreased bleeds correlated with: – shorter infusion interval (p < 0. 005) – age < 3 years (p < 0. 0002) n Joint disease correlated with: – age when treatment started (p = 0. 0002) – dose and interval at start age not significant n Astermark. Brit J Haematol. 1999; 105: 1109 © Rush University Medical Center 2016

Swedish Experience All values are mean Nilsson. J Int Med. 1992; 232: 25 © Rush University Medical Center 2016
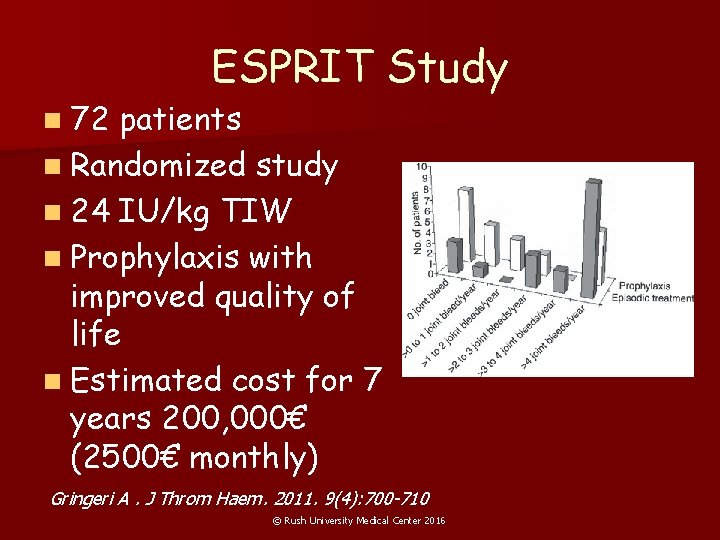
n 72 ESPRIT Study patients n Randomized study n 24 IU/kg TIW n Prophylaxis with improved quality of life n Estimated cost for 7 years 200, 000€ (2500€ monthly) Gringeri A. J Throm Haem. 2011. 9(4): 700 -710 © Rush University Medical Center 2016

Is Prophylaxis ‘Worth It’? n Inherited – not the person’s fault they have it n Children primarily effected – Individuals place greater weight on health gains by children than adults n Rare condition – small public impact n Prophylaxis is preventive treatment n Expensive due to need for safety Feldman BM. Haemophilia 2012. 18: 680 -684 © Rush University Medical Center 2016

Outcomes Modeling n Swedish model – trough >1% – 25 -40 IU/kg 3 x/wk or QOD n Netherlands bleeding – prevent spontaneous – 10 -15 IU/kg 3 x/wk or QOD n 24 year follow up – Swedish with a 66% increased annual cost – Outcomes similar QOL and Employment Fischer K. Blood 2013; 122: 1129 -36 © Rush University Medical Center 2016
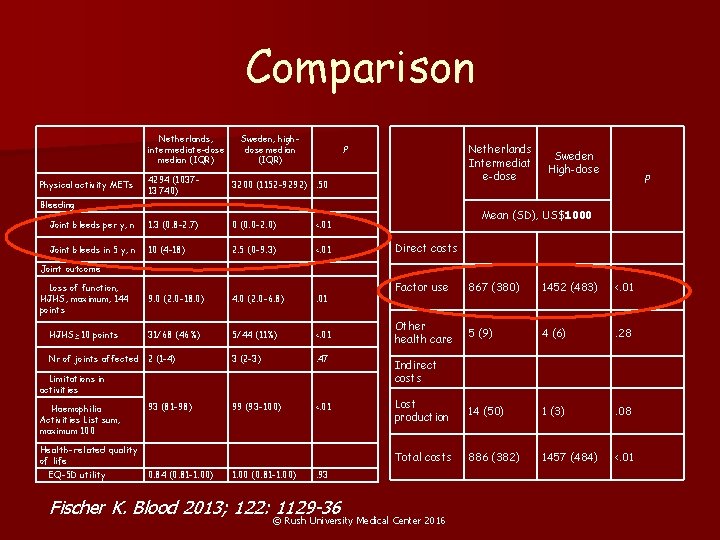
Comparison Netherlands, intermediate-dose median (IQR) Sweden, highdose median (IQR) Netherlands Intermediat e-dose P 4294 (103713 740) 3200 (1152 -9292). 50 Joint bleeds per y, n 1. 3 (0. 8 -2. 7) 0 (0. 0 -2. 0) <. 01 Joint bleeds in 5 y, n 10 (4 -18) 2. 5 (0 -9. 3) <. 01 Loss of function, HJHS, maximum, 144 points 9. 0 (2. 0 -18. 0) 4. 0 (2. 0 -6. 8) . 01 HJHS≥ 10 points 31/68 (46%) 5/44 (11%) <. 01 3 (2 -3) . 47 Indirect costs 99 (93 -100) <. 01 Physical activity METs Bleeding Sweden High-dose P Mean (SD), US$1000 Direct costs Joint outcome Nr of joints affected 2 (1 -4) Limitations in activities Haemophilia Activities List sum, maximum 100 93 (81 -98) Health-related quality of life EQ-5 D utility 0. 84 (0. 81 -1. 00) 1. 00 (0. 81 -1. 00) Factor use 867 (380) 1452 (483) <. 01 Other health care 5 (9) 4 (6) . 28 Lost production 14 (50) 1 (3) . 08 Total costs 886 (382) 1457 (484) <. 01 . 93 Fischer K. Blood 2013; 122: 1129 -36 © Rush University Medical Center 2016

Should prophy be for children and On-demand for adults? n Compared to on-demand, prophylaxis has better outcomes – Even at lowest dose (1000 IU/kg/yr or 10 IU/kg twice weekly) – Increased effectiveness up to 4500 IU/kg/yr (25 IU/kg 3 -3. 5 times/week) n Switch to on-demand as adults – Pristine joints at start of on-demand – 10 year increase in Petterson scores Fischer K. Haemophilia 2016; 1 -8 © Rush University Medical Center 2016

What to Do with Limited Resources? n Short term pilot study from China n Indian study – randomized open label study n Children aged 1 -10 – 10 IU/kg twice a week – 25 IU/kg on-demand – Xray & HJHS – 12 month follow up Verma SP. Haemophilia 2016; 22: 342 -348 © Rush University Medical Center 2016

Study Groups Variables Prophylaxis group (n = 11) Mean ± SD Episodic treatment group (n = 10) Mean ± SD P value Age at diagnosis (months) 11. 6 ± 4. 7 11. 2 ± 3. 19 ns Age at study entry (years) 4. 32 ± 2. 55 7. 9 ± 1. 97 <0. 05 Baseline weight (kg) 13. 45 ± 3. 42 18. 40 ± 4. 0 <0. 05 Weight at 6 months (kg) 16. 64 ± 4. 4 20. 8 ± 4. 1 <0. 05 Baseline bleeding frequency/month (range) 0. 8 (0– 2) 1. 0 (0– 2) ns Number of months in study Median (minmax) 11. 5 (10– 12) ns Clinical score – baseline 0 (0– 3) (HJHS 2. 1) 0. 5 (0– 2) ns Pettersson Score (Baseline) Median (range) 0. 5 (0– 2) ns 0 (0– 2) © Rush University Medical Center 2016
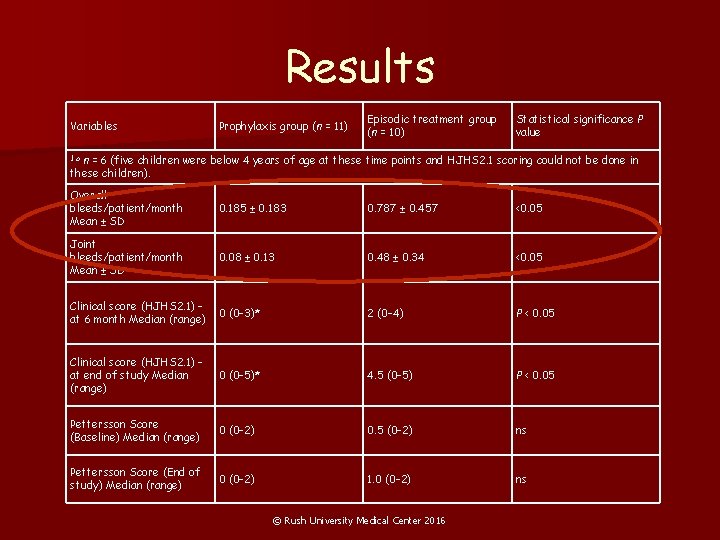
Results Variables Prophylaxis group (n = 11) Episodic treatment group (n = 10) Statistical significance P value n = 6 (five children were below 4 years of age at these time points and HJHS 2. 1 scoring could not be done in these children). 1. a Overall bleeds/patient/month Mean ± SD 0. 185 ± 0. 183 0. 787 ± 0. 457 <0. 05 Joint bleeds/patient/month Mean ± SD 0. 08 ± 0. 13 0. 48 ± 0. 34 <0. 05 Clinical score (HJHS 2. 1) – at 6 month Median (range) 0 (0– 3)* 2 (0– 4) P < 0. 05 Clinical score (HJHS 2. 1) – at end of study Median (range) 0 (0– 5)* 4. 5 (0– 5) P < 0. 05 Pettersson Score (Baseline) Median (range) 0 (0– 2) 0. 5 (0– 2) ns Pettersson Score (End of study) Median (range) 0 (0– 2) 1. 0 (0– 2) ns © Rush University Medical Center 2016
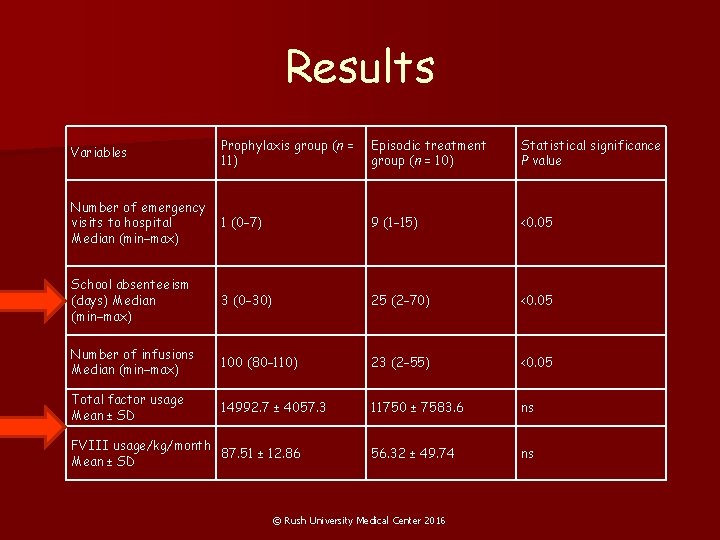
Results Variables Prophylaxis group (n = 11) Episodic treatment group (n = 10) Statistical significance P value Number of emergency visits to hospital Median (min−max) 1 (0– 7) 9 (1– 15) <0. 05 School absenteeism (days) Median (min−max) 3 (0– 30) 25 (2– 70) <0. 05 Number of infusions Median (min−max) 100 (80– 110) 23 (2– 55) <0. 05 Total factor usage Mean ± SD 14992. 7 ± 4057. 3 11750 ± 7583. 6 ns 56. 32 ± 49. 74 ns FVIII usage/kg/month 87. 51 ± 12. 86 Mean ± SD © Rush University Medical Center 2016

Costs/Benefits n Prophylaxis demand 1. 5 times higher than on- – Most of this is factor n Fewer days lost from school – 3 days prophylaxis v 25 days on -demand n No change in Petterson score © Rush University Medical Center 2016

Prophylaxis Advantages Disdvantages n Decreased bleeding n Cost n Reduced joint damage n Increase n Intravenous access activity n Increase school attendance © Rush University Medical Center 2016

The Cost of Prophylaxis 100, 000 Episodic Care Prophylaxis 60, 000 40, 000 Cost per Year ($) 80, 000 20, 000 0 Factor Medical Total Factor Care Smith P et al. J Pediatr. 1996; 129(3): 424 -431 © Rush University Medical Center 2016 Medical Care Total

What’s Reasonable? n Primary prophylaxis – start early – < 2 bleeds/joint – 1 bleed/several joints – Age < 3 years n Secondary prophylaxis – short term n Preventive prophylaxis – 4 bleeds/joint over 6 months – Treat for 3 -6 months – Prior to strenuous or high risk activities or surgeries © Rush University Medical Center 2016

Thank you! © Rush University Medical Center 2016
- Slides: 28