Low Back Pain in Primary Care Implications for

Low Back Pain in Primary Care Implications for Primary Care Management Richard Kelly Clinical Lead Physiotherapist – City. Care MSK Service November 2017

Aims • Review the biomedical model and low back pain (LBP) • Discuss the iatrogenic nature of chronic LBP • Review of risk stratification with relation to the NICE LBP Guidelines (2016) • Provide useful resources for patients presenting to primary care Slide 2

Low Back Pain: In numbers • 80% of adults will experience an episode of LBP (Rubin, 2007) • 20% of those with LBP will consult their GP (Rubin, 2007) • 5 -10% of people will develop chronic (persistent) LBP (Maniadakis & Gray, 2000) • Leading cause of work absence and economic loss in the UK (Bamford et al, 2017) Slide 3
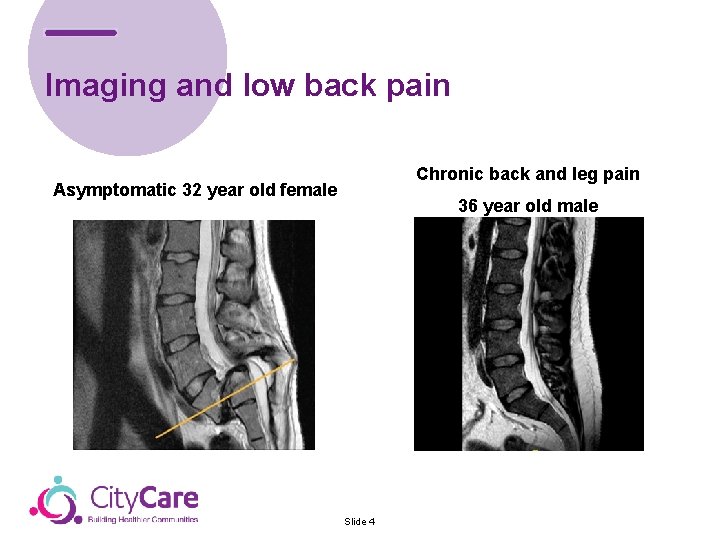
Imaging and low back pain Chronic back and leg pain Asymptomatic 32 year old female 36 year old male Slide 4

MRI findings in the asymptomatic population (Brinjikji et al, 2014) Slide 5

Imaging and low back pain Slide 6

Imaging and low back pain Slide 7

Opioid therapy and back pain • Opioid prescriptions have increased worldwide (Boudreau et al, 2009) • Opioid therapy for persistent back pain has grown disproportionately (Dhalla et al, 2011) • Back pain patients more likely to receive higher doses (Morasco et al, 2010) • Patients receiving opioid therapy have poorer outcome at 6 months and more likely to report/demonstrate: o Worse pain o Worse function o Poorer self efficacy o Greater catastrophising o Fear of movement o Depression Slide 8

Injections and back pain • 271% increase in epidural injections over a 7 year interval (Friedly et al, 2007) • Epidurals do not reduce the rate of subsequent surgery (Airaksinen et al, 2006) • 231% increase in facet joint injections (Friedly et al, 2007) • No more effective than saline (Chou et al, 2008) Slide 9

Is chronic low back pain an iatrogenic disorder? Slide 10

Confession Disc bulge! Slide 11

Confession Slide 12

Mind your language What patients hear What we say • Chronic • Two steps to a wheelchair • Instability • Liable to pop out • Wear & Tear • It’s rotting away • Neurological • Could be a tumour • Don’t bend or lift • Spine is vulnerable/weak Darlow et al (2013) Slide 13

The impact of terminology “Basically all I’v e kind of been told to do by physio s is to work on my co re. . . I’m appare ntly ridiculously we ak. . I had an abort ion because I d idn’t think I could h ave a baby. I didn’t think I c ould handle carrying it” things o d ld u o w d that. . . I ie r r o w s a w “I at would h t ] k r o w t. . [The k [a c a b y m age further dam lly said that I sica r lifting. o g doctor] ba in d n e b o any shouldn’t d of the job” lot Which is a “It’s the doc that said that, you know if I don’t slow down or quit playing sport or whatever I could, you know, do more damage…. . If I don’t have sport…. . I feel bored…. . I don’t have life” Darlow et al (2013) and Lin et al (2013) Slide 14

The Nocebo effect Negative biomedical information induces fear & anxiety (the Nocebo effect) by perpetuating a single faulty structure phenomenon Louw & Puentedura (2013). https: //thesportsphysio. wordpress. com/2014/08/09/a-tigers-sacrum/ Slide 15
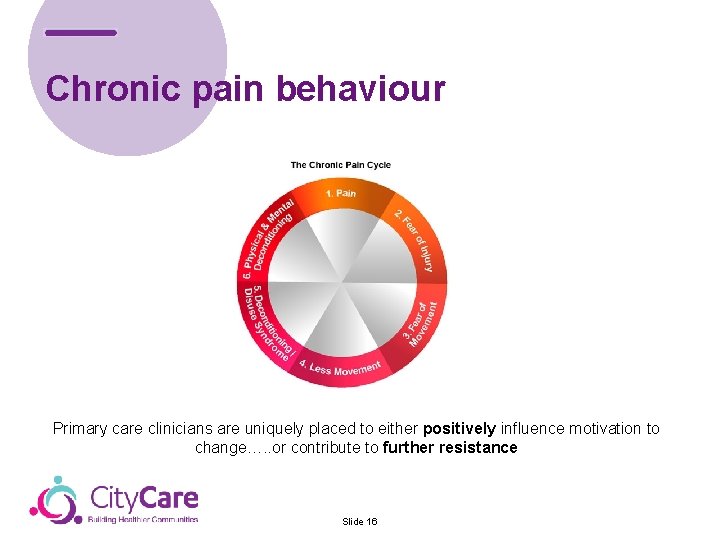
Chronic pain behaviour Primary care clinicians are uniquely placed to either positively influence motivation to change…. . or contribute to further resistance Slide 16

Break Any questions? Slide 17

NICE LBP Guidelines: 2016 • Emphasis on selfmanagement • Early identification of risk factors (STar. T Back) rather than after failed treatment • Targeted care based on risk (not symptom duration) • Caution with referrals for investigation & intervention • Opportunities or Obstacles to implementation? Slide 18
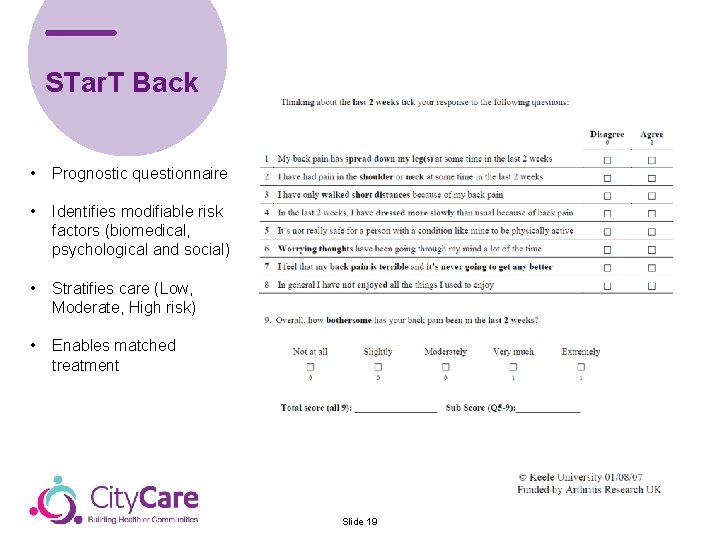
STar. T Back • Prognostic questionnaire • Identifies modifiable risk factors (biomedical, psychological and social) • Stratifies care (Low, Moderate, High risk) • Enables matched treatment Slide 19

Risk stratification: Benefits • Small but significant benefit on disability at 6 months (RMDQ) • 50% less work absenteeism (4 vs 8 days) • 30% less sickness certificates • No increase in healthcare costs (Foster et al, 2014) Local context • Locally, 20% of LBP in physio were high risk (approx 1, 100 per annum) - ? more appropriate for back pain programme (pain service) Slide 20
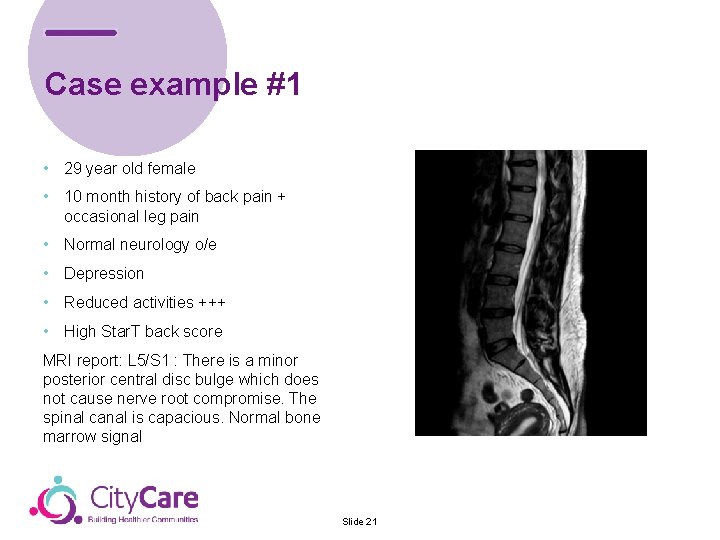
Case example #1 • 29 year old female • 10 month history of back pain + occasional leg pain • Normal neurology o/e • Depression • Reduced activities +++ • High Star. T back score MRI report: L 5/S 1 : There is a minor posterior central disc bulge which does not cause nerve root compromise. The spinal canal is capacious. Normal bone marrow signal Slide 21
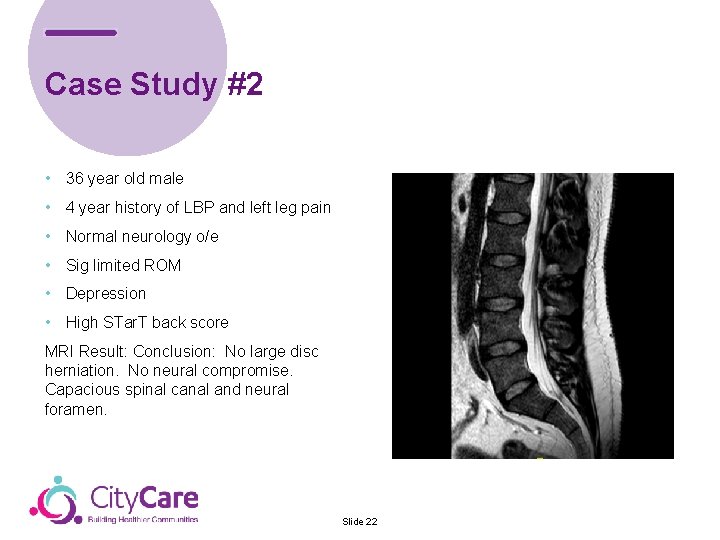
Case Study #2 • 36 year old male • 4 year history of LBP and left leg pain • Normal neurology o/e • Sig limited ROM • Depression • High STar. T back score MRI Result: Conclusion: No large disc herniation. No neural compromise. Capacious spinal canal and neural foramen. Slide 22

Explaining persistent pain Slide 23

So what can we do? • Keep it CRISP • Clearance…. . of any sinister features and remain vigilant. • Reassurance…. . explain pain as predominantly defence over defect • Independence…. encourage self management. Define roles between patient and HCP • Simplify…. . become comfortable at being vague. Language is important • Promote…. activity and remaining at work where able and maintaining fitness (Chew & Nawoor, 2015) Slide 24

Useful resources • www. citycarephysio. org. uk Slide 25

Useful resources • Chartered Society of Physiotherapy – Myth busters • Understanding pain in 5 minutes – video • Understanding persistent pain booklet (http: //knowpain. co. uk/wpcontent/uploads/2014/05/Tazzy. Persistent. Pain. Booklet. pdf) • Pain toolkit - https: //www. paintoolkit. org/ Slide 26

Take home messages • Low back pain is a growing problem • Biomedical model appears ineffective • CLBP may in part be iatrogenic • Primary care is pivotal in long term prognosis • Language can have both a –ve and +ve impact on pain behaviour • Embedding risk stratification is beneficial • Reassurance and ensuring patients remain active are key! Slide 27

References Airaksinen O, Brox JI, Cedraschi C, et al. European guidelines for the management of chronic nonspecific low back pain. European Spine Journal. 2006; 15(Suppl 2): S 192 -S 300 Bamford A, Nation A, Durrell S, Andronis L, Rule E, Mc. Leod H. (2017) Implementing the Kelle Stratified care model for patients with low back pain: an observational impact study. BMC Musculoskeletal Disorders 18: 66 Boudreau D, Von Korff M, Rutter CM, Saunders K, Ray GT, Sullivan MD, et al. Trends in long-term opioid therapy for chronic noncancer pain. Pharmacoepidemiol Drug Safety 2009; 18: 1166 -75. Darlow, B, Dowell, A, Baxter, G, Mathieson, F, Perry, M, Dean, S. (2013). The enduring impact of what clinicians say to people with low back pain. The Annals of Family Medicine. 11 (6) 527 -34. Dhalla IA, Persaud N, Juurlink DN. Facing up to the prescription opioid crisis. BMJ 2011; 343: d 5142. Foster NE, Mullis R, Hi JC, Lewis M, et al. (2014). Effect of Stratified Care for Low Back Pain in Family Practice (IMPa. CT Back): A Prospective Population-Based Sequential Comparison. The Annals of Family Medicine. 12: 102 -111 Lin, Ivan & O'Sullivan, Peter & A Coffin, Juli & B Mak, Donna & Toussaint, Sandy & Straker, Leon. (2013). Disabling chronic low back pain as an iatrogenic disorder: A qualitative study in Aboriginal Australians. BMJ open. 3. 10. 1136/bmjopen-2013 -002654. Maniadakis N, Gray A. The ecomonic burden of low back pain in the United Kingdom. Pain. 2000; 84(1): 95 -103 Morasco BJ, Duckart JP, Carr TP, Deyo RA, Dobscha SK. Clinical characteristics of veterans prescribed high doses of opioid medications for chronic non-cancer pain. Pain 2010; 151: 625 -32. Rubin DI. Epidemiology and risk factors for spine pain. Neurol Clin. 2007; 25(2): 353– 371. Slide 28

Nottingham City. Care Partnership CIC 1 Standard Court Park Row Nottingham NG 1 6 GN e: citycare@nottinghamcitycare. nhs. uk t : 0115 883 9600 www. nottinghamcitycare. nhs. uk
- Slides: 29