Low Back Pain Dabbas W M D Neurosurgeon
Low Back Pain Dabbas W, M. D. Neurosurgeon Dept. of Neurosciences, School of Medicine, Al Balqa University

Objectives Review the functional anatomy of lumbo-sacral spine List essential components of a LBP history, including RED FLAGS Describe common causes of LBP Review proper indications for imaging and referral Review Physical Examination of LS spine Correlate pathology with pertinent physical findings

Epidemiology Incidence of LBP: 60 -90 % lifetime incidence 5 % annual incidence 90 % of cases of LBP resolve without treatment within 6 -12 weeks 40 -50 % LBP cases resolve without treatment in 1 week 75 % of cases with nerve root involvement can resolve in 6 months LBP and lumbar surgery are: 2 nd and 3 rd highest reasons for physician visits 5 th leading cause for hospitalization 3 rd leading cause for surgery 3

Disability Age and LBP: Leading cause of disability of adults < 45 years old Third cause of disability in those > 45 years old Prevalence rate: Increased 140 % from 1991 to 2000 with only 125 % population growth Nearly 5 million people in the U. S. are on disability for LBP 4

Lifetime Return to Work Success of < 50 % if off work > 6 months 25 % success rate if off work > 1 year Nearly 0 % success if return to work has not occurred in 2 years 5

Differential Diagnoses Lumbar Strain Disc Bulge / Protrusion / Extrusion producing Radiculopathy Degenerative Disc Disease (DDD) Spinal Stenosis Spondyloarthropathy Spondylosis Spondylolisthesis Sacro-iliac Dysfunction 6
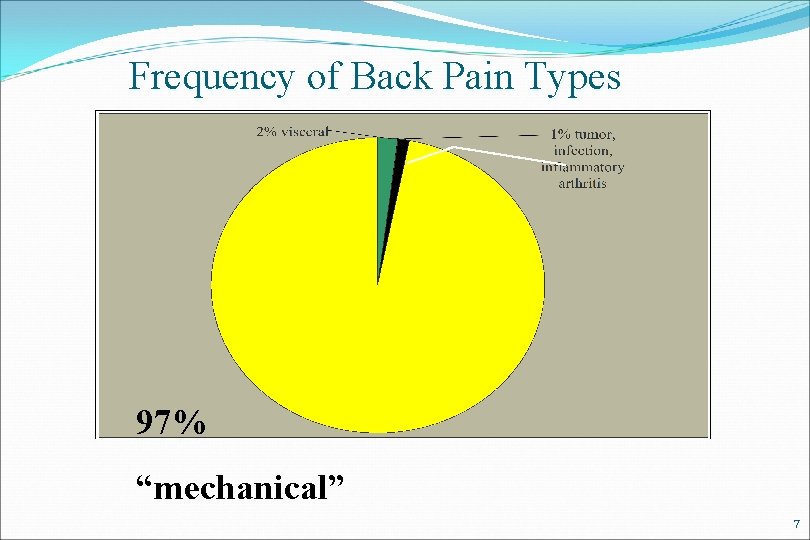
Frequency of Back Pain Types 97% “mechanical” 7

Better anatomy knowledge = Better diagnoses and treatments
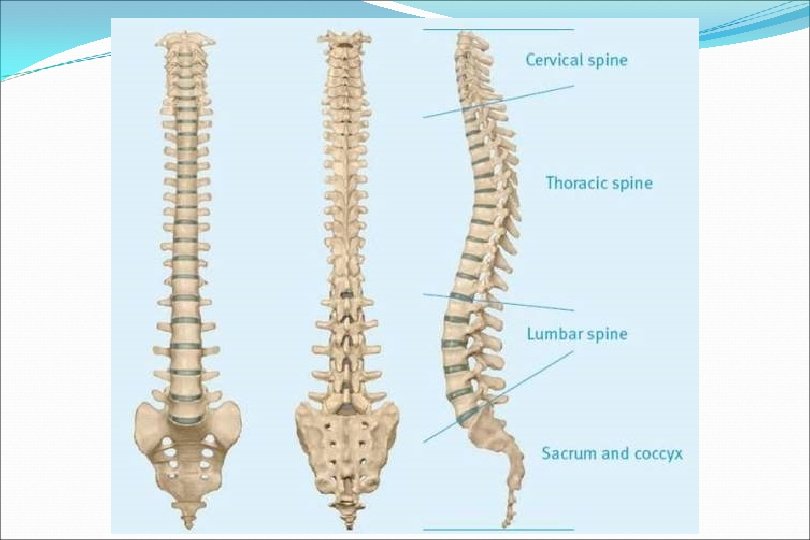
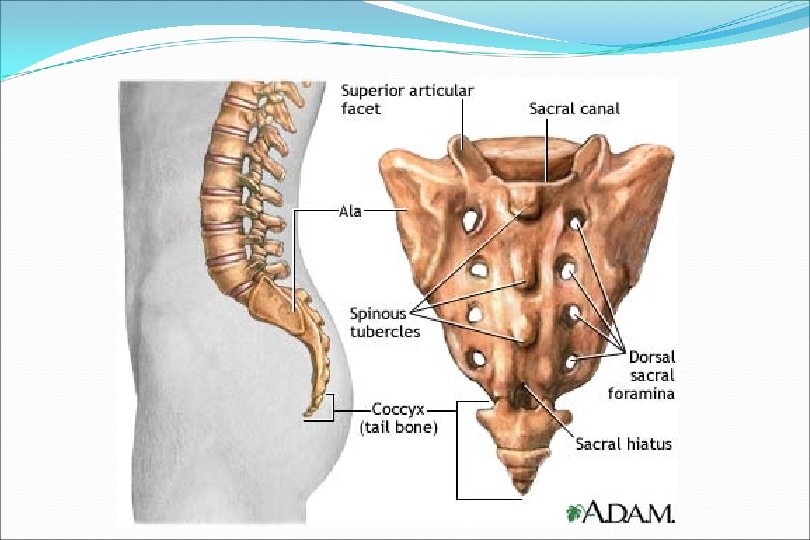
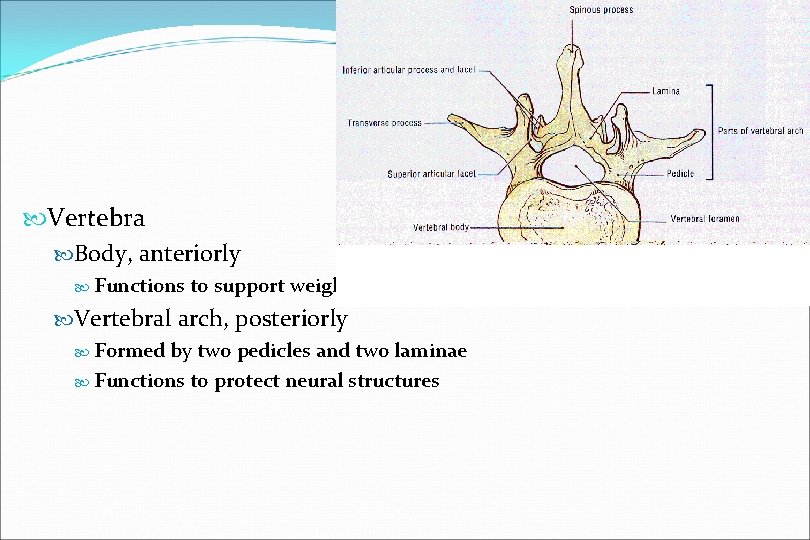
Vertebra Body, anteriorly Functions to support weight Vertebral arch, posteriorly Formed by two pedicles and two laminae Functions to protect neural structures
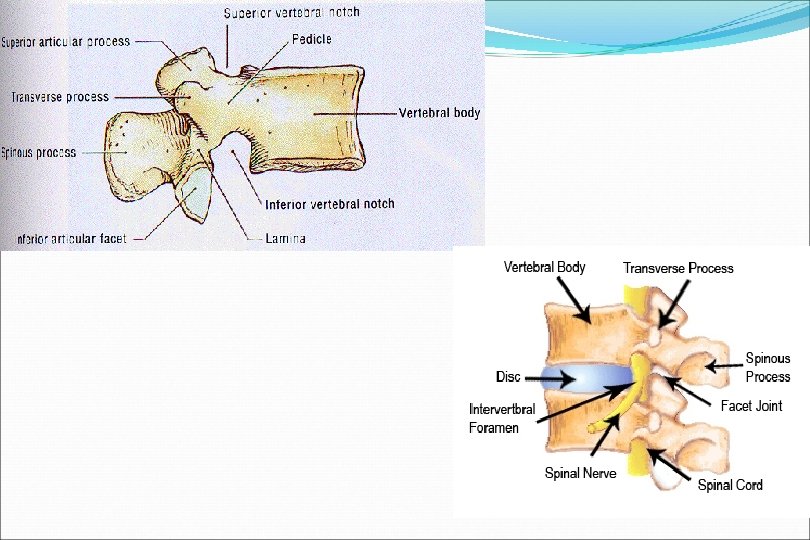

Biomechanics 80% Anterior 20% Posterior The 80 -20 rule of Spine loading www. brain 101. info 13

Ligaments Anterior longitudinal ligament Posterior longitudinal ligament Ligamentum flavum Interspinous ligament Supraspinous ligament
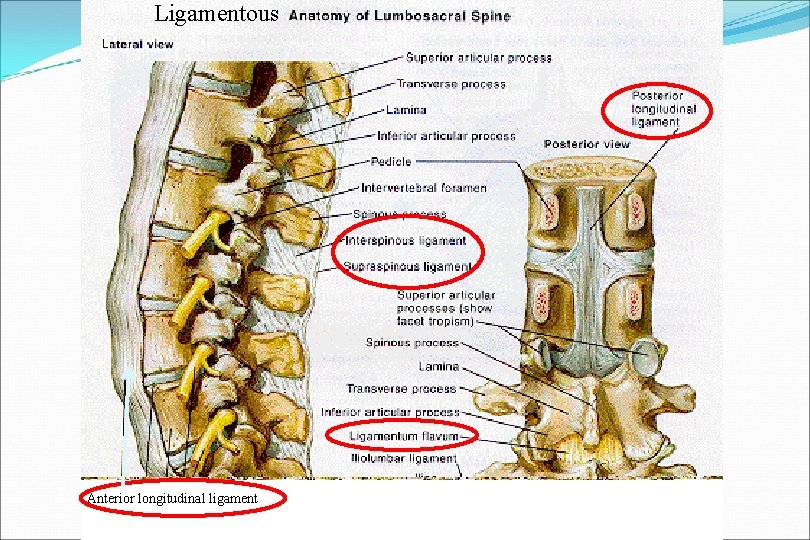
Ligamentous Anterior longitudinal ligament
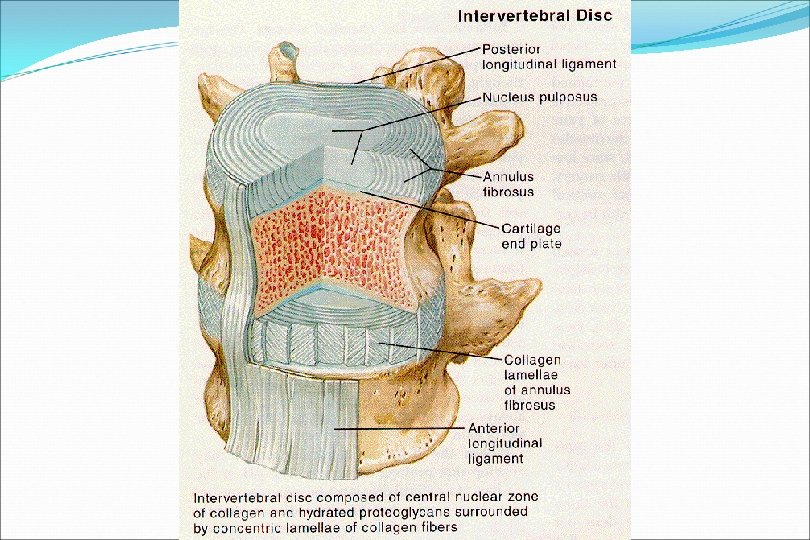
Sciatica is defined as… 1. Pain radiating up the 2. 3. 4. back Pain radiating to the thigh Pain radiating below the knee Pain in the butt

PATIENT HISTORY “OPQRSTU” Onset Palliative/Provocative factors Quality Radiation Severity/Setting in which it occurs Timing of pain during day Understanding - how it affects the patient

“Red Flags” in back pain Age < 15 or > 50 Fever, chills, UTI Significant trauma Unrelenting night pain; pain at rest Progressive sensory deficit Neurologic deficits Saddle-area anesthesia Urinary and/or fecal incontinence Major motor weakness Unexplained weight loss Hx or suspicion of Cancer Hx of Osteoporosis Hx of IV drug use, steroid use, immunosuppression Failure to improve after 6 weeks conservative tx

Onset Acute - Lift/twist, fall, MVA Subacute - inactivity, occupational (sitting, driving, flying) Pain effect on: work/occupation sport/activity (during or after)
Other History Prior h/o back pain Prior treatments and response Exercise habits Occupation/recreational activities Cough/valsalva exacerbation

Diagnoses & Red Flags Cancer Age > 50 History of Cancer Weight loss Unrelenting night pain Failure to improve Infection IVDU Steroid use Fever Unrelenting night pain Failure to improve Fracture Age >50 Trauma Steroid use Osteoporosis Cauda Equina Syndrome Saddle anesthesia Bowel/bladder dysfunction Loss of sphincter control Major motor weakness

Physical Examination Inspection Palpation Strength testing Neurologic examination Special tests

Approach to LBP History & physical exam Classify into 1 of 4: LBP from other serious causes Cancer, infection, cauda equina, fracture LBP from radiculopathy or spinal stenosis Non-specific LBP Non-back LBP Workup or treatment

Diagnostic Tools 1. Laboratory: Performed primarily to screen for other disease etiologies Infection Cancer Spondyloarthropathies • No evidence to support value in first month unless with red flags • Specifics: WBC ESR or CRP HLA-B 27 Tumor markers: Kidney Breast Lung Thyroid Prostate • 26

2. Radiographs: • Pre-existing Degenerative Joint Disease (Osteoarthritis) is most common diagnosis • Usually 3 views adequate with obliques only if equivocal findings • Indications: History of trauma with continued pain < 20 years or > 55 years with severe or persistent pain Noted spinal deformity on exam Signs / symptoms suggestive of spondylo-arthropathy Suspicion for infection or tumor 27
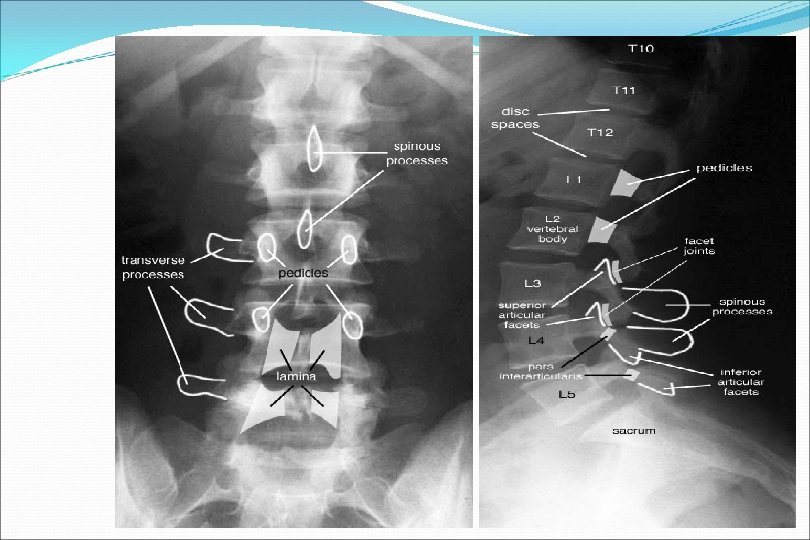
www. brain 101. info 28

3. Electromylogram (EMG): Measures muscle function Would not be appropriate in clinically obvious radiculopathy 4. Bone Scan: Very sensitive but nonspecific Useful for: Malignancy screening Detection for early infection Detection for early or occult fracture 29
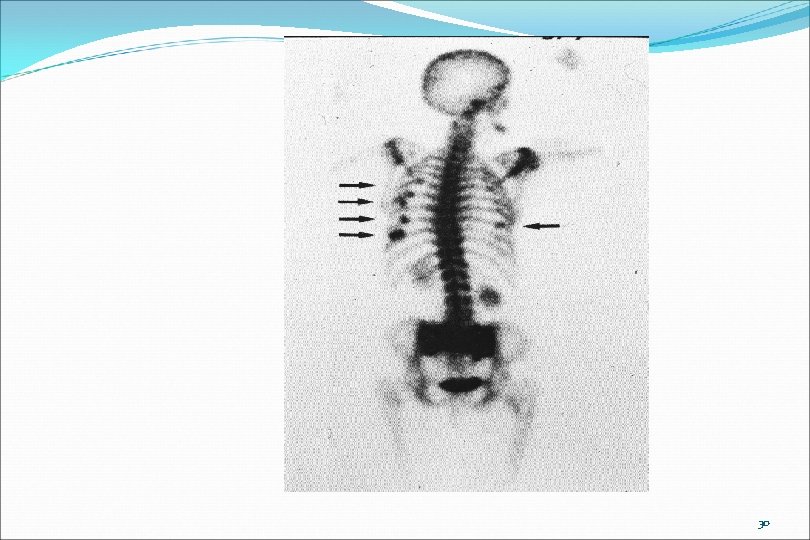
30

5. Myelogram: Procedure of injecting contrast material into the spinal canal with imaging via plain radiographs versus CT 31

6. CT with Myelogram: Can demonstrate much better anatomical detail than Myelogram alone Utilized for: Demonstrating anatomical detail in multi-level disease in preoperative state Determining nerve root compression etiology of disc versus osteophyte Surgical screening tool if equivocal MRI or CT 32

7. CT: Best for bony changes of spinal or foraminal stenosis Also best for bony detail to determine: Fracture Degenerative Joint Disease (DJD) Malignancy 33

9. MRI • Best diagnostic tool for: Soft tissue abnormalities: • Infection • Bone marrow changes • Spinal canal and neural foraminal contents Emergent screening: • Cauda equina syndrome • Spinal cord injury • Vascular occlusion • Radiculopathy Benign vs. malignant compression fractures Osteomyelitis evaluation Evaluation with prior spinal surgery 34

Break for Physical Examination Hands-on Session
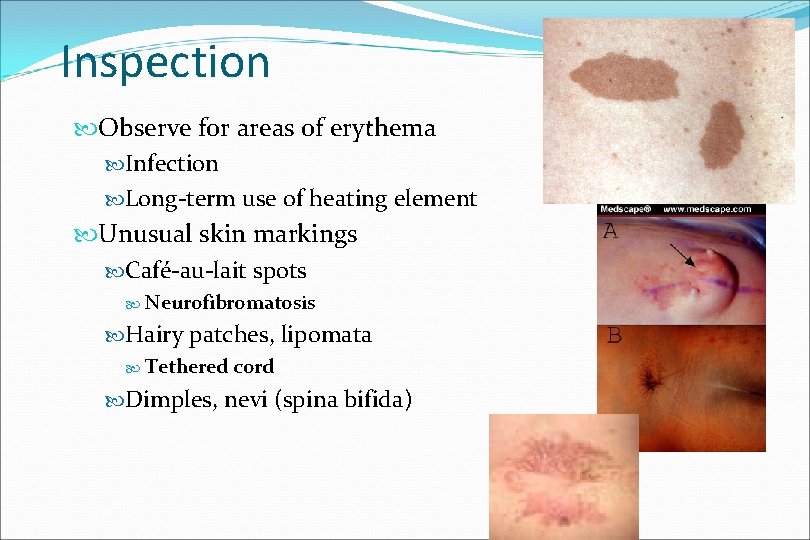
Inspection Observe for areas of erythema Infection Long-term use of heating element Unusual skin markings Café-au-lait spots Neurofibromatosis Hairy patches, lipomata Tethered cord Dimples, nevi (spina bifida)

Inspection (cont. ) Posture Shoulders and pelvis should be level Bony and soft-tissue structures should appear symmetrical Normal lumbar lordosis Exaggerated lumbar lordosis is common characteristic of weakened abdominal wall

Neurologic Examinaion Includes an exam of entire lower extremity, as lumbar spine pathology is frequently manifested in extremity as altered reflexes, sensation and muscle strength Describes the clinical relationship between various muscles, reflexes, and sensory areas in the lower extremity and their particular cord levels
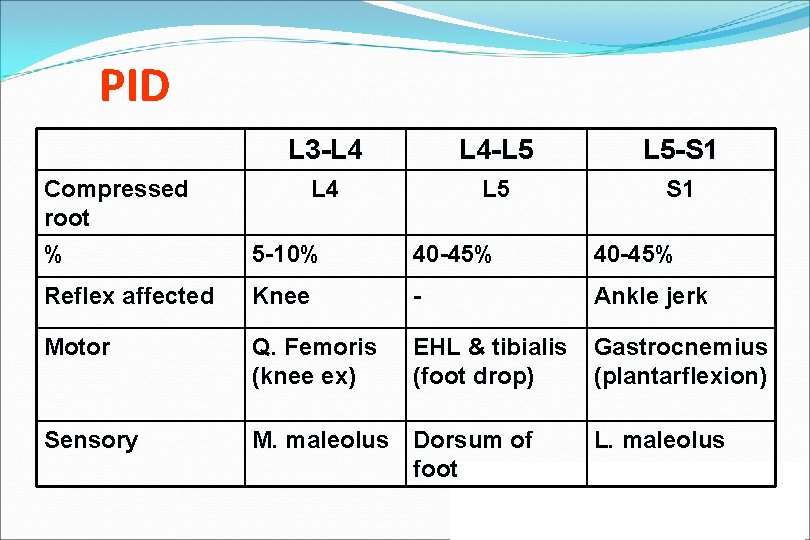
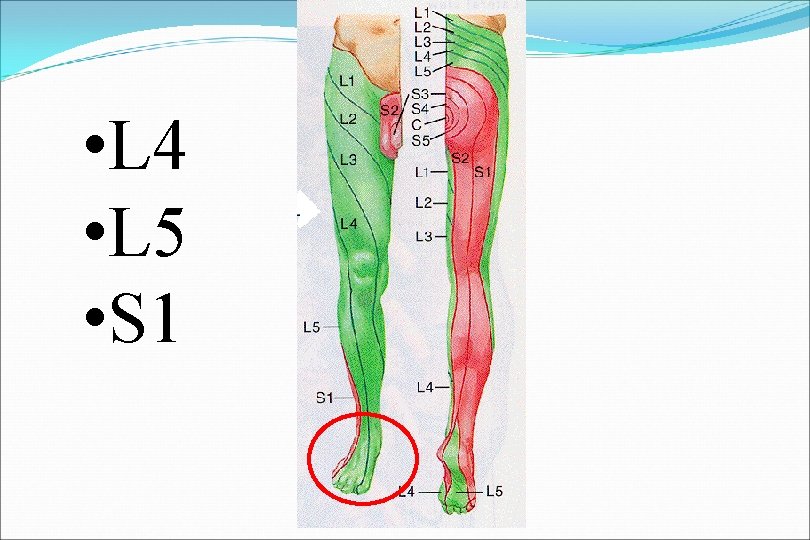
PID L 3 -L 4 L 4 -L 5 L 5 -S 1 L 4 L 5 S 1 Compressed root % 5 -10% 40 -45% Reflex affected Knee - Ankle jerk Motor Q. Femoris (knee ex) EHL & tibialis (foot drop) Gastrocnemius (plantarflexion) Sensory M. maleolus Dorsum of foot L. maleolus

Neurologic Examination (T 12, L 1, L 2, L 3 level) Motor Iliopsoas - main flexor of hip With pt in sitting position, raise thigh against resistance Reflexes - none Sensory Anterior thigh

Neurologic Examination (L 2, L 3, L 4 level) Motor Quadriceps - L 2, L 3, L 4, Femoral Nerve Hip adductor group - L 2, L 3, L 4, Obturator N. Reflexes Patellar - supplied by L 2, L 3, and L 4, although essentially an L 4 reflex and is tested as such
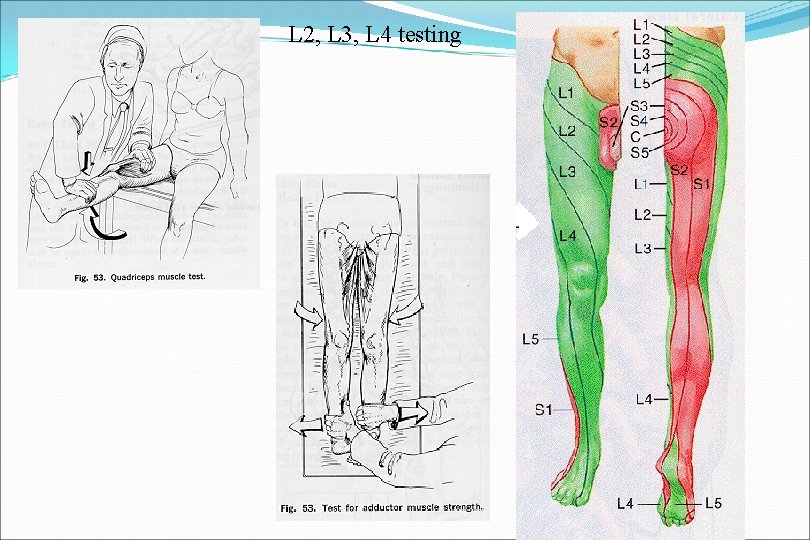
L 2, L 3, L 4 testing

Neurologic Examination (L 4 level) Motor Tibialis Anterior Resisted inversion of ankle Reflexes Patellar Reflex (L 4) Sensory Medial side of leg
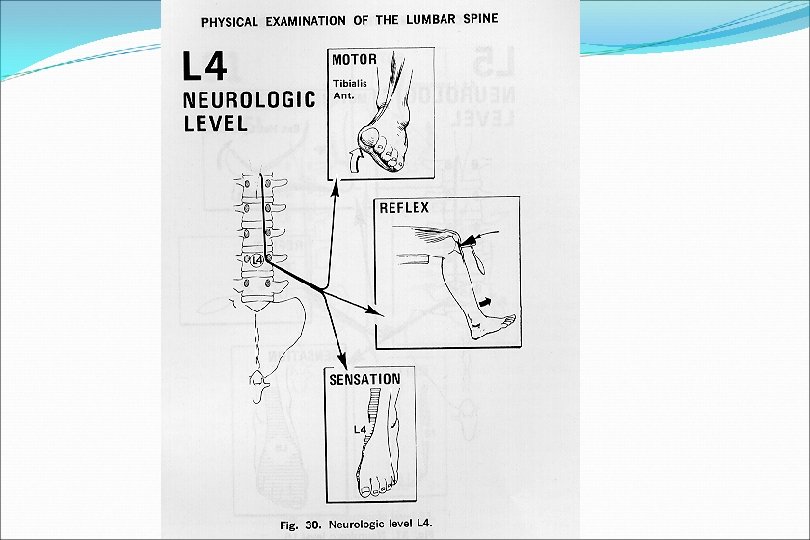

Neurologic Examination (L 5 level) Motor Extensor Hallicus Longus Resisted dorsiflexion of great toe dorsifexion Reflexes - none Sensory Dorsum of foot in midline
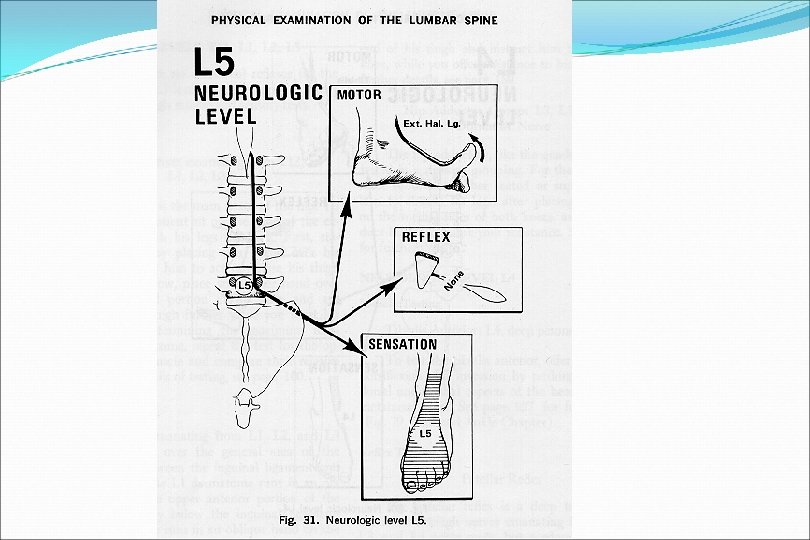

Neurologic Examination (S 1 level) Motor Peroneus Longus and Brevis Resisted eversion of foot Planter flexion Reflexes Achilles Sensory Lateral side of foot
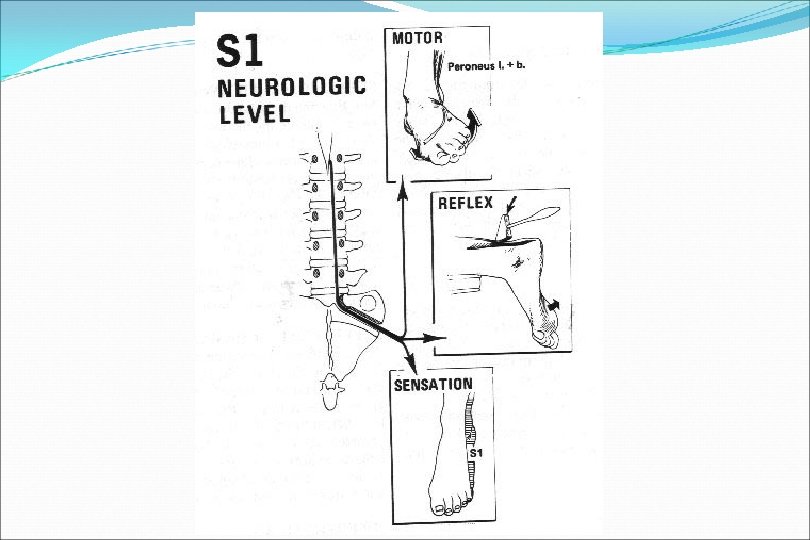

Special Tests to stretch spinal cord or sciatic nerve Tests to increase intrathecal pressure Tests to stress the sacroiliac joint

Tests to Stretch the Spinal Cord or Sciatic Nerve Straight Leg Raise Cross Leg SLR Kernig Test

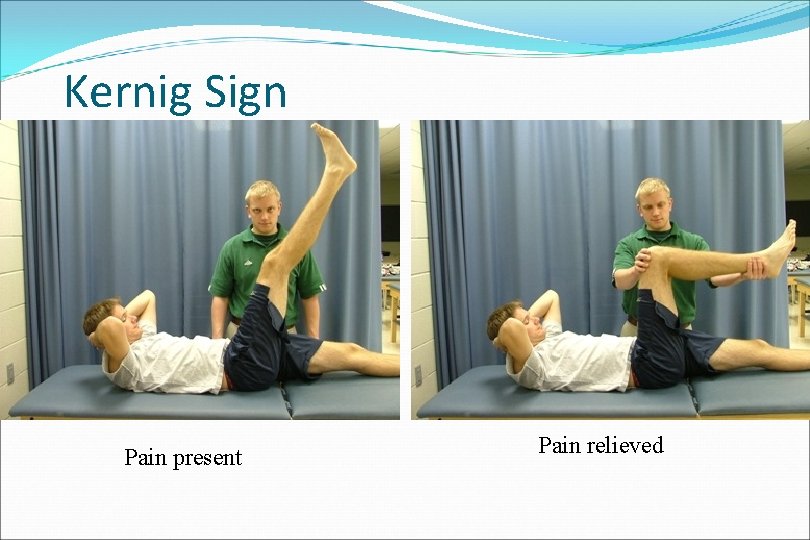
Kernig Sign Pain present Pain relieved

Test to increase intrathecal pressure Valsalva Maneuver Reproduction of pain suggestive of lesion pressing on thecal sac

Tests to stress the Sacroiliac Joint FABER Test

FABER test: Flexion ABduction External Rotation
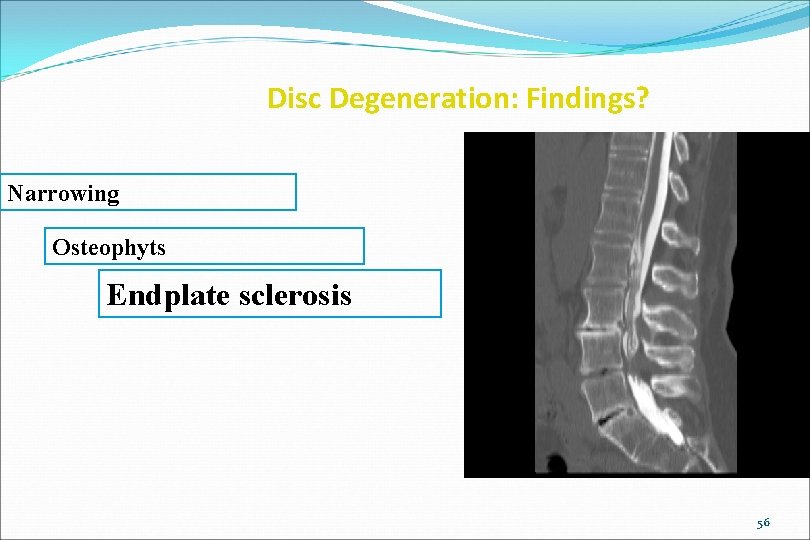
Disc Degeneration: Findings? Narrowing Osteophyts Endplate sclerosis 56
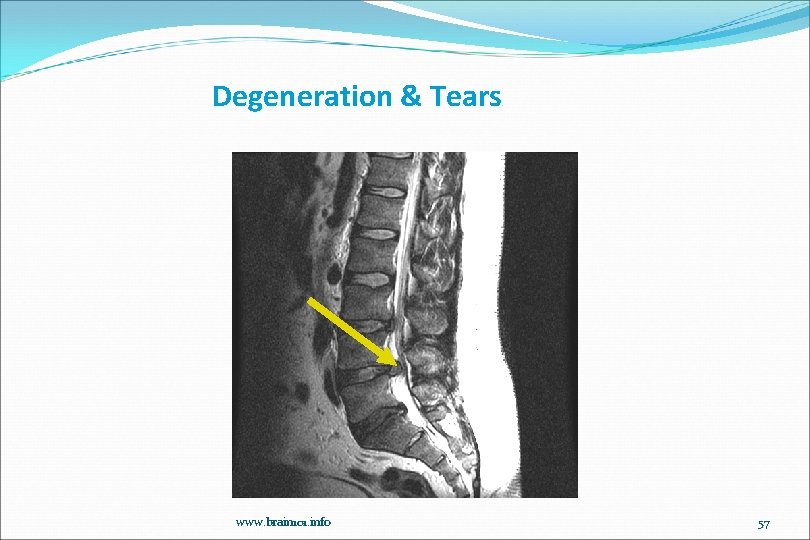
Degeneration & Tears www. brain 101. info 57
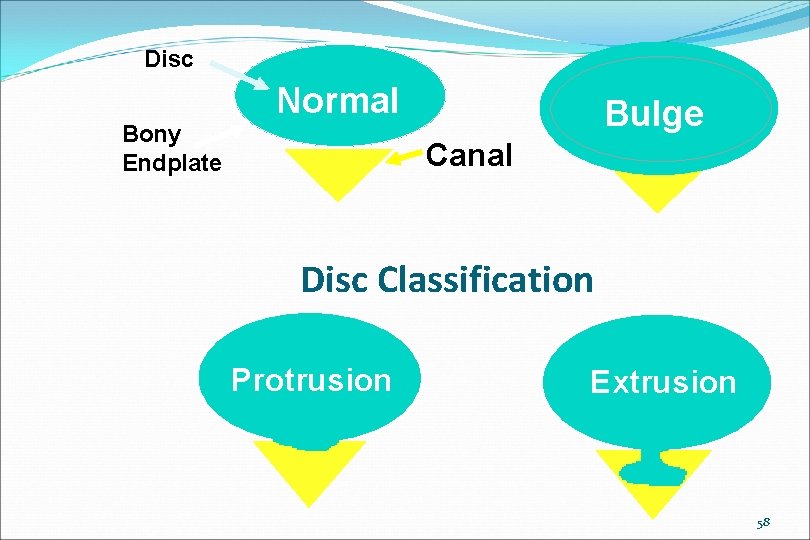
Disc Normal Bony Endplate Bulge Canal Disc Classification Protrusion Extrusion 58
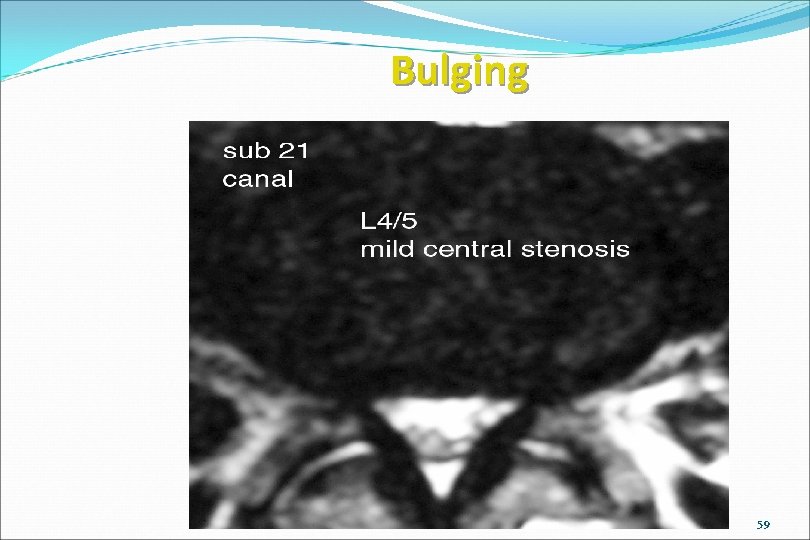
Bulging www. brain 101. info 59
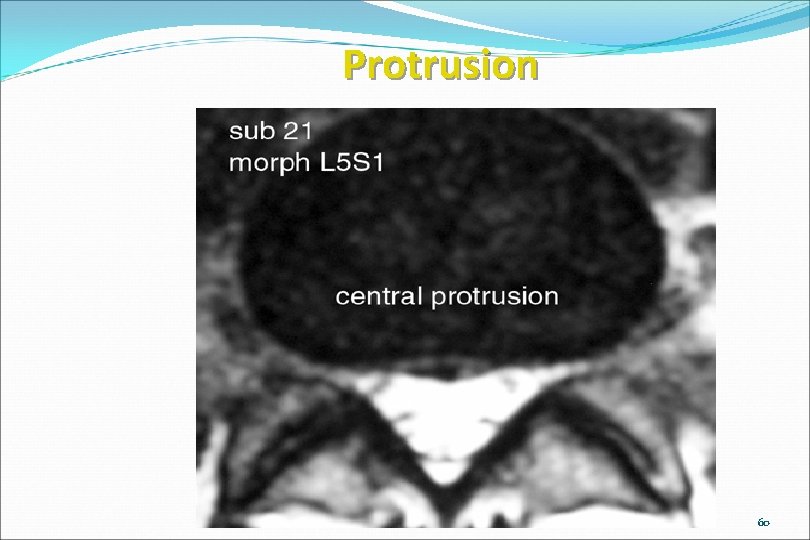
Protrusion www. brain 101. info 60
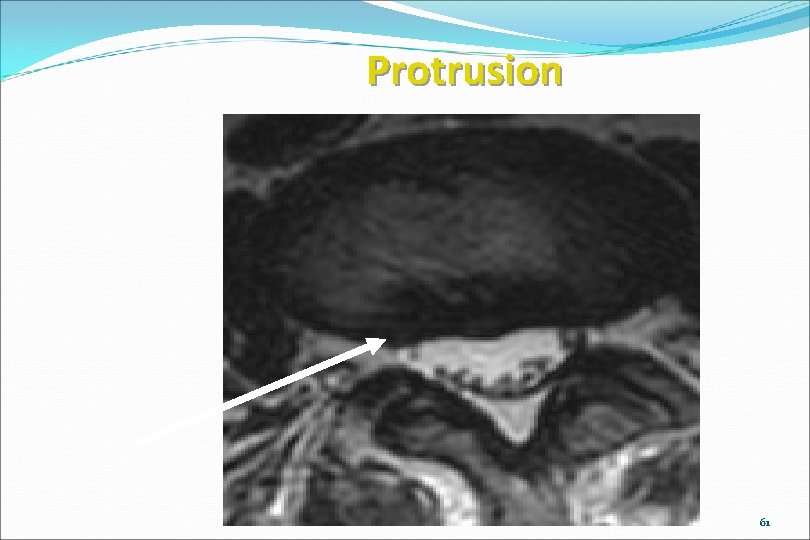
Protrusion www. brain 101. info 61
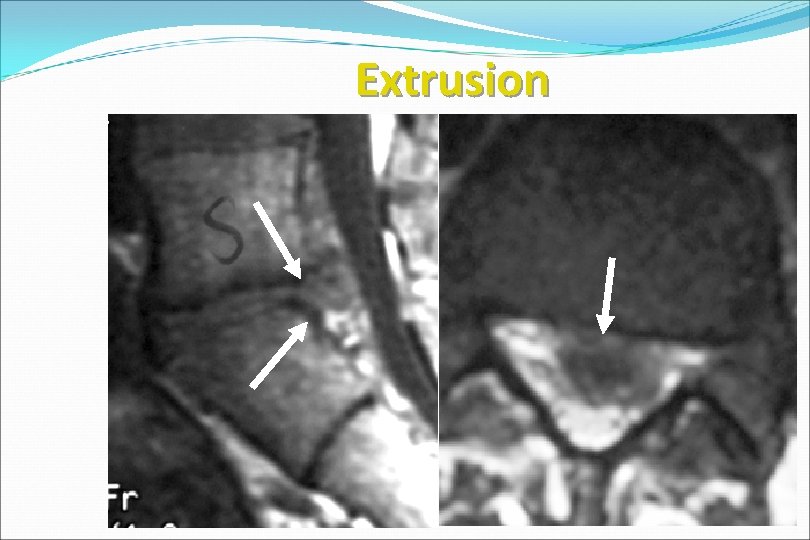
Extrusion www. brain 101. info 62
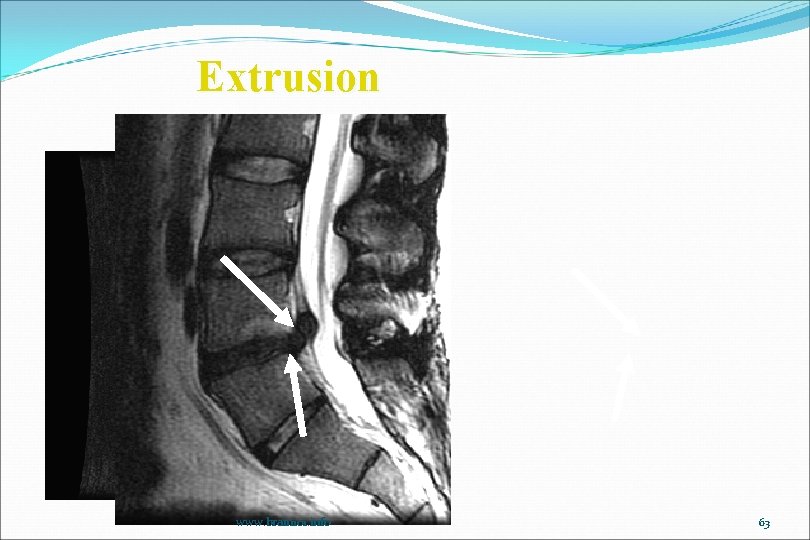
Extrusion www. brain 101. info 63
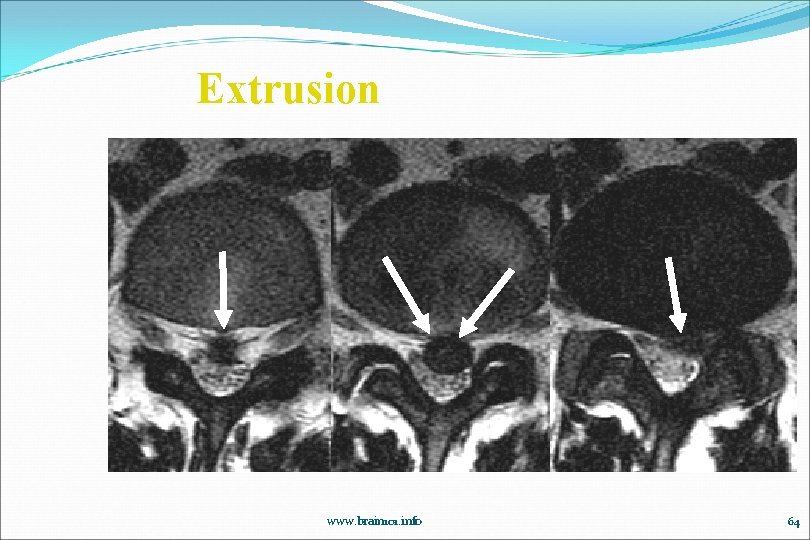
Extrusion www. brain 101. info 64

Treatment Pharmacological NSAIDS Muscle relaxents: Re-establish sleep patterns More useful in myofascial/muscular pain Membrane stabilizers TCA / Neurontin Re-establish sleep pain Reduce radicular dysesthesias Narcotics: rarely indicated Morphine, Oxy/hydrocodone, Oxymorphone, Hydromorphone, Fentanyl, Methadone Steroids: more useful for radiculitis Non-narcotic analgesics: Ultram (Tramadol) 65

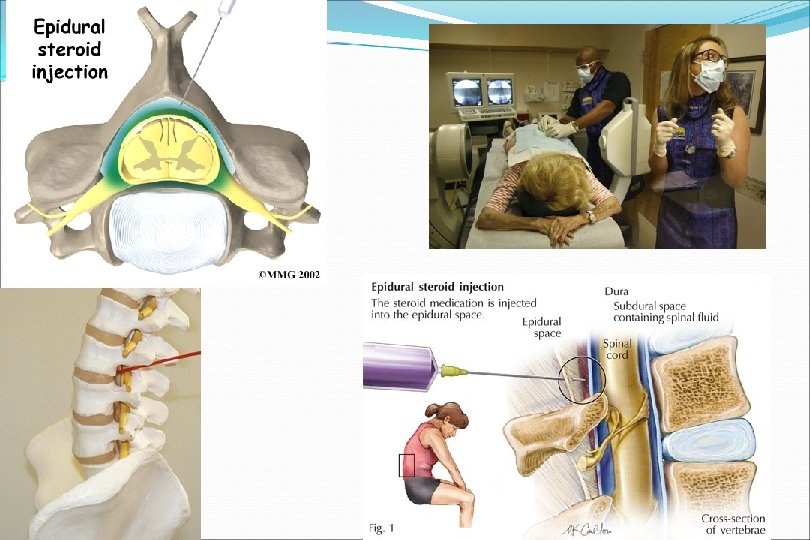
Physical Therapy Modalities • Electrical Stimulation/TENS • Postural Education / Body Mechanics • Massage / Mobilization / Myofascial Release • Stretching / Body Work • Exercise / Strengthening • Traction • Pre-conditioning / Work-conditioning Injections (Neural blockade) • Epidural blocks • Facet blocks • Trigger point • SI joint 66

Epidural Steroid Injections Indicated for radiculopathy not responding to conservative management Conflicting evidence Small improvement up to 3 months Less effective in spinal stenosis

Surgery Laminectomy Hemilaminectomy Discectomy Fusion Instrumented Non-instrumented fusion Minimally Invasive Spine Surgery (MISS) Kyphoplasty Percutaneous Disc Decompression (PDD) www. brain 101. info 69

Management of an acute low back muscle strain should consist of all the following EXCEPT: 1. X-rays to rule out a fracture 2. Educate the patient on generally good prognosis 3. Non-opiate analgesics 4. Remain active

Your patient with LBP has paresthesias in the lateral foot, decreased toe-raise strength, diminished sensation lateral foot, and diminished Achilles reflex. This is suggestive of dysfunction of which nerve root? 1. 2. 3. 4. L 4 L 5 S 1 S 2

Thank you
- Slides: 72