Loves Labours Lost CCM InterHospital Grand Round 13

Love’s Labour’s Lost CCM Inter-Hospital Grand Round 13 Nov 2012 SK Yung Chairman: Dr Osburga Chan Queen Elizabeth Hospital

Case 1 F/34 Para 0 Twin pregnancy USG at 22 weeks 6 days both twins size appropriate for gestation Placenta both not low Liqour normal for both fetuses No gross fetal abnormalities for both

Case 1 OGTT –ve, AN Blood unremarkable AN follow up 34 weeks 5 days BP 133/56, Urine alb trace AN follow up 36 weeks 5 days BP 131/72, urine alb >= 3+ MSU saved no significant growth Clinically admitted for elective Cesarean section for twins 16/11/2010 (37 weeks 5 days)

Case 1 BP/P 159/89, 80/min, Urine alb 2+ Rechecked BP 165/98, 78/min No symptoms of PET Blood test Hb 13. 6, WCC 6. 9, Plt 121 RFT 139/4. 2/4. 7/82 ALP 179 Alb 29, ALT 18 Urate 0. 42 (0. 16 -0. 39)
Case 1 Diagnosis: Pre-eclampsia complicating twin pregnancy Emergency Lower segment Cesarean Section under spinal anaesthesia Operation uneventful, blood loss 300 ml Both twins’ Apgar scores satisfactory BP at end of operation 130/74, 88/min Transferred to labour ward post op

Case 1 Upon arrival to Labour ward BP 186/93, 55/min Headache +ve, no blurred vision/ other symptoms of PET Started on Mg. SO 4 infusion 4 g as loading, 1 g/hr Given nifedipine 5 mg q 4 h po prn if SBP >= 160 for BP control

Case 1 Noticed sudden onset of slurring of speech the next morning Examination showed cerebellar signs with nystagmus, GCS 15/15, no other symptoms of PET e. g. epigastric pain Urgent CT Brain
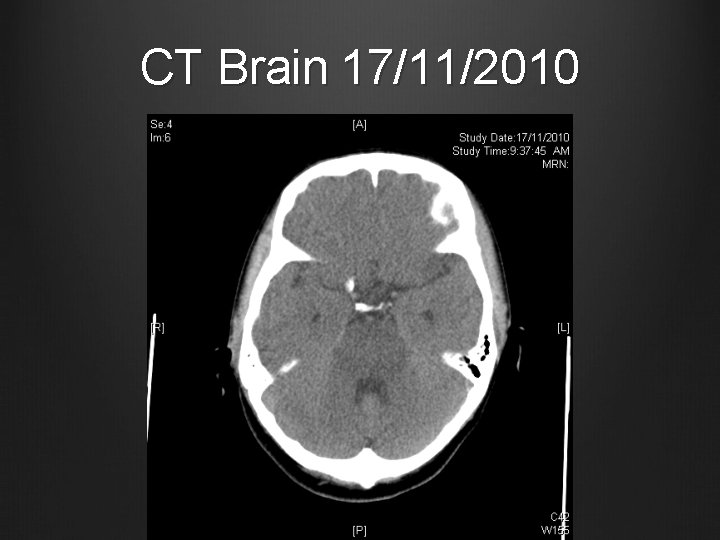
CT Brain 17/11/2010

CT Brain 17/11/2010

CT Brain 17/11/2010
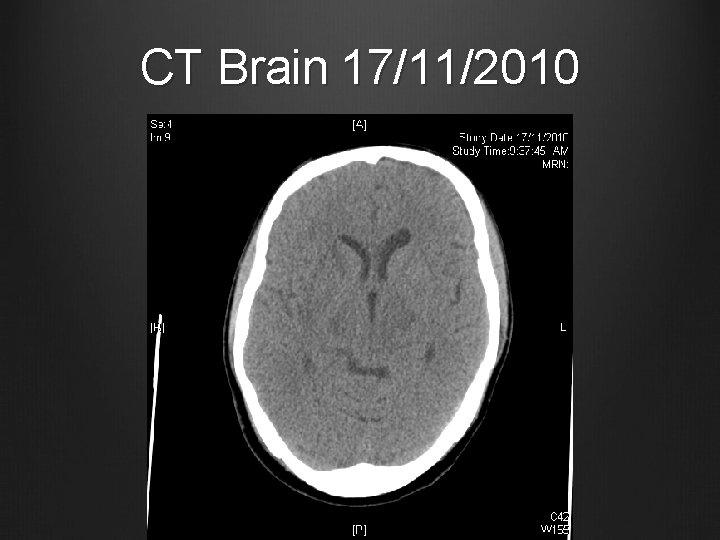
CT Brain 17/11/2010

Case 1 Urgent CT Brain Hypodense areas in pons, midbrain, bilateral basal ganglia and thalami Taken over to ICU for close monitoring

Case 1 Seen by Neurology colleagues: Bilateral past pointing Horizontal gaze limited in abduction and adduction, left worse than right side Slurred speech No other focal neurological deficits CT Brain: hypo-densities over bilateral pons, midbrain, thalami, basal ganglia Likely pre-eclampsia related cerebral dysfunction, causing cerebral flow limitation over posterior circulation For BP control

Case 1 BP controlled by labetalol infusion Reviewed by neurology 18/11/2010 Sustained bilateral horizontal nystagmus with impaired left lateral and vertical gaze, mild divergent squint, features suggestive of left pontine, midbrain and thalamic dysfunction, dysarthria with wet voice compatible with bulbar dysfunction Condition showed improvement after control of BP and Mg. SO 4 infusion Suggested for MRI
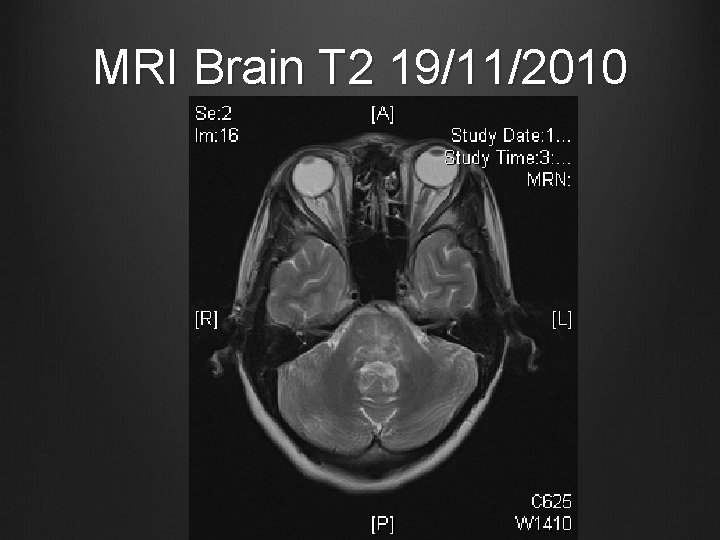
MRI Brain T 2 19/11/2010
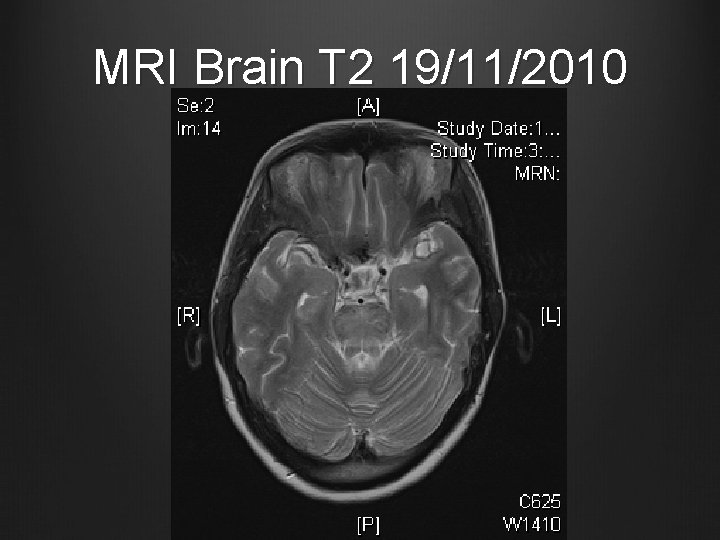
MRI Brain T 2 19/11/2010
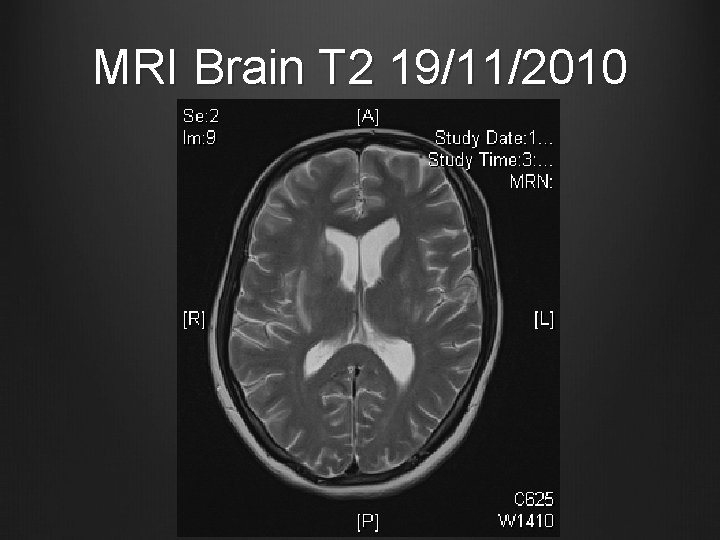
MRI Brain T 2 19/11/2010
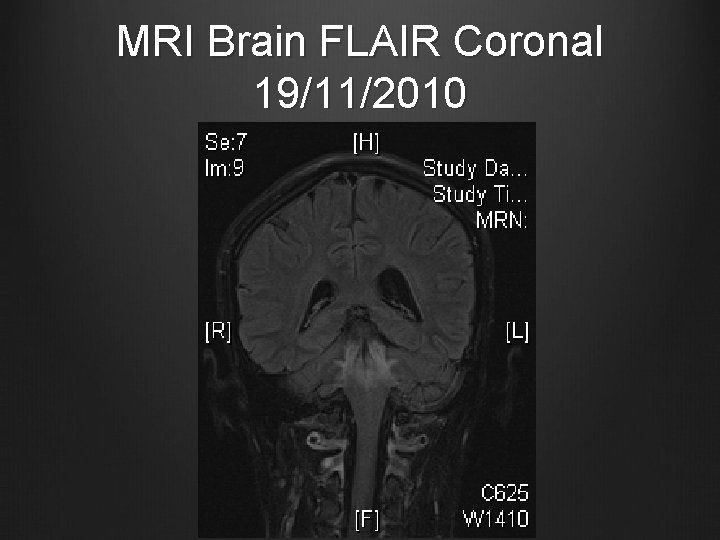
MRI Brain FLAIR Coronal 19/11/2010
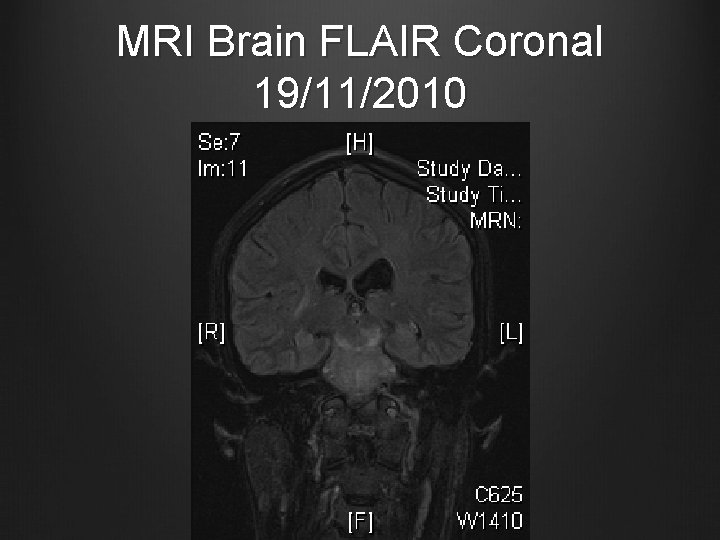
MRI Brain FLAIR Coronal 19/11/2010
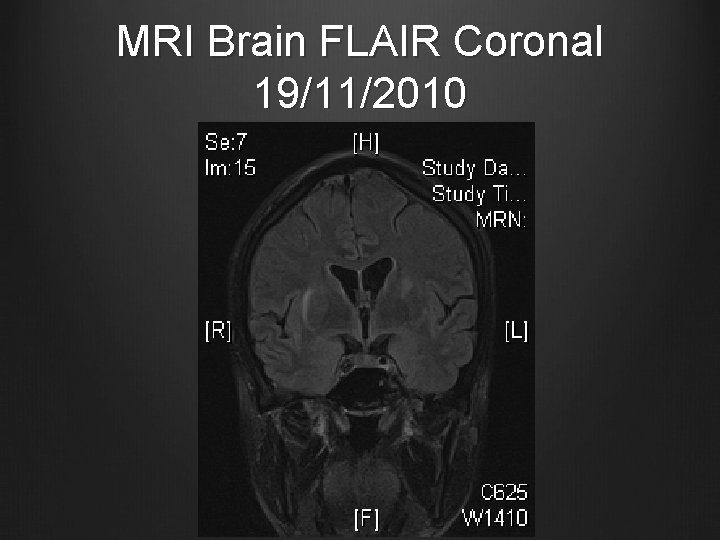
MRI Brain FLAIR Coronal 19/11/2010

Case 1 MRI Brain and brain stem with contrast + MR angiography 19/11/2010 T 2 hyperintense signal in central portion of the pons, medulla and midbrain, also patchy seen in bilateral basal ganglia & external capsular regions No abnormal contrast enhancement Small patchy areas of restricted diffusion in pons and medulla No obvious signal change suggestive of intracranial haemorrhage MRA showed patent and normal intracerebral arteries

Case 1 BP gradually stabilized with amlodipine, methyldopa, minoxidil, weaned off labetalol Clinically improving diplopia/ slurring of speech Discharged from ICU on 22/11/2010 CT Brain repeated 24/11/2010
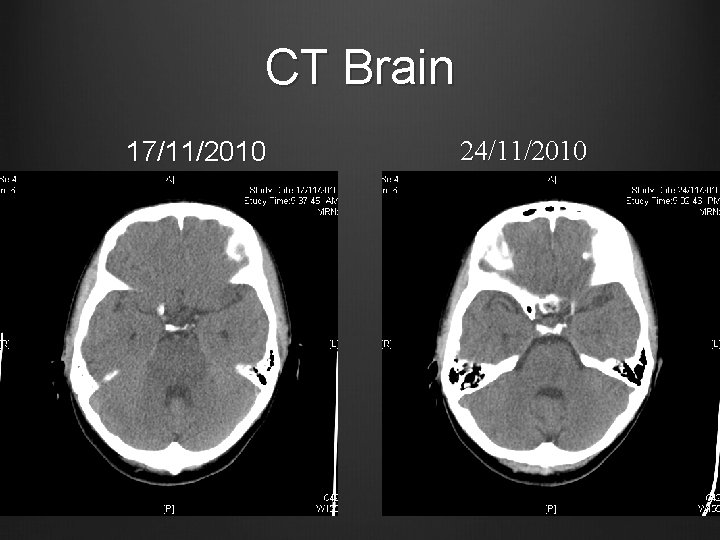
CT Brain 17/11/2010 24/11/2010
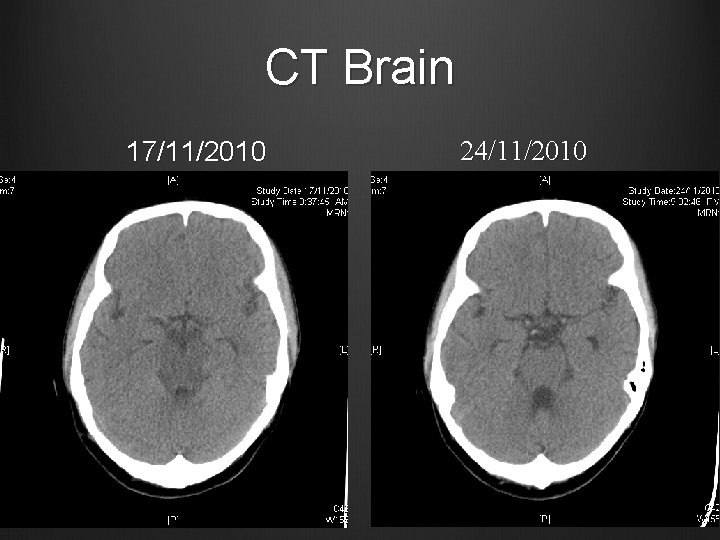
CT Brain 17/11/2010 24/11/2010
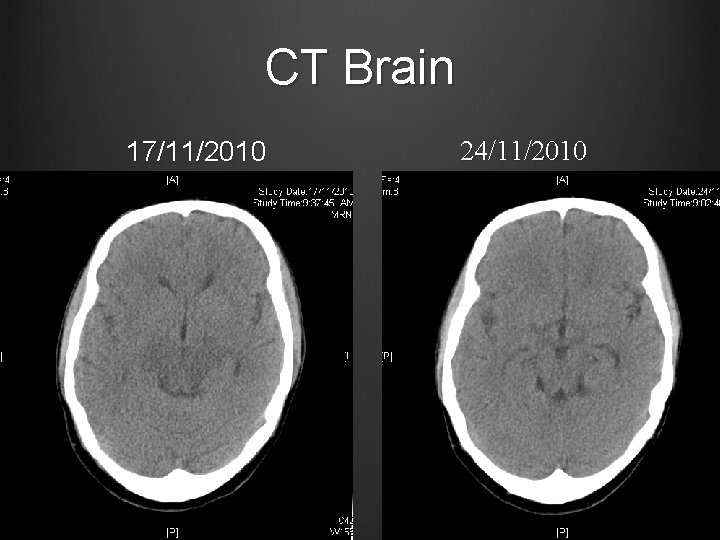
CT Brain 17/11/2010 24/11/2010
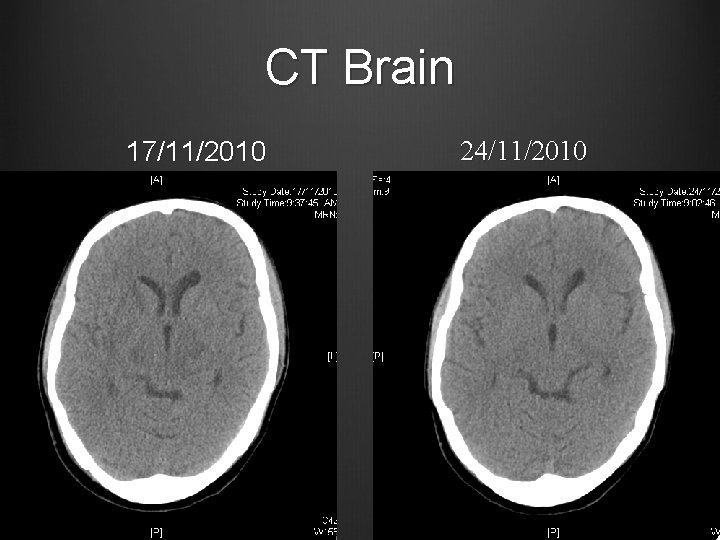
CT Brain 17/11/2010 24/11/2010

Case 1 Neurological symptoms completely resolved ~ 2 months post delivery No longer need antihypertensives

Case 2 F/35 Non smoker, non drinker 3 rd pregnancy (same partner)

Case 2 Past obstetric history 1 st delivery in 1999 Full term NSD Tonic clonic seizure during episiotomy wound suturing CT Brain unremarkable EEG no definite epileptiform activities, intermittent generalized slow waves both hemispheres compatible with interictal changes Not on anticonvulsants all along and defaulted follow up in neurology clinic 2 nd delivery 2007 Full term NSD, uneventful

Case 2 Current (3 rd pregnancy) AN uneventful Admitted to UCH 26/4/2012 (39+ 3 weeks) for uterine contraction and show BP 160/80, urine alb + No symptoms of PET

Case 2 Blood test CBC, R/LFT, urate, clotting profile within normal ranges Noticed abnormal CTG and decided for emergency Caesarean Section Developed generalized tonic clonic seizure during anaesthesic assessment

Case 2 Emergency LSCS under GA for fetal distress and eclampsia Intraoperatively given Mg. SO 4 infusion BP controlled by hydralazine infusion Not extubated and transferred to UCH ICU 2 more GTC, aborted by valium each time Started on phenytoin CT Brain done
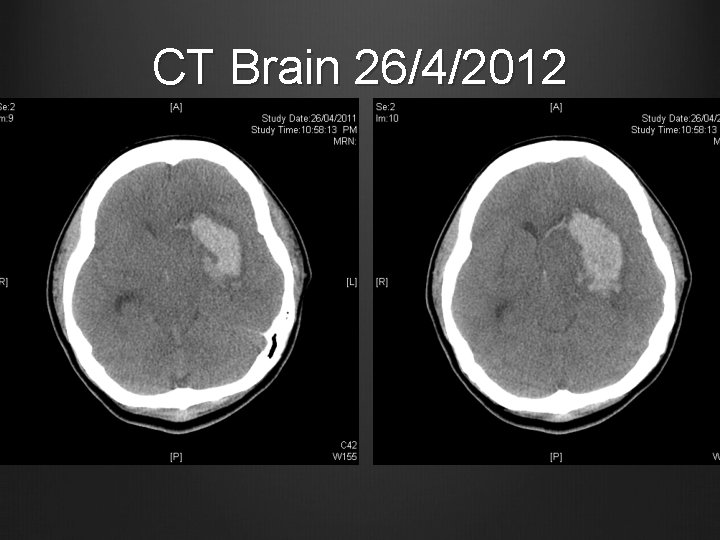
CT Brain 26/4/2012

Case 2 Pupils 2 mm, reactive and symmetrical BP stable, given mannitol Transferred to QEH for further management Noticed unequal pupils shortly after arrival to QEH Proceeded to emergency left craniectomy + EVD insertion

Case 2 ICP remained high side ~ 40 -50 mm. Hg with asymmetrical pupil sizes (2, 3 mm, reactive) Given 1 more dose of mannitol CT Brain repeated ~ 1 hour post op
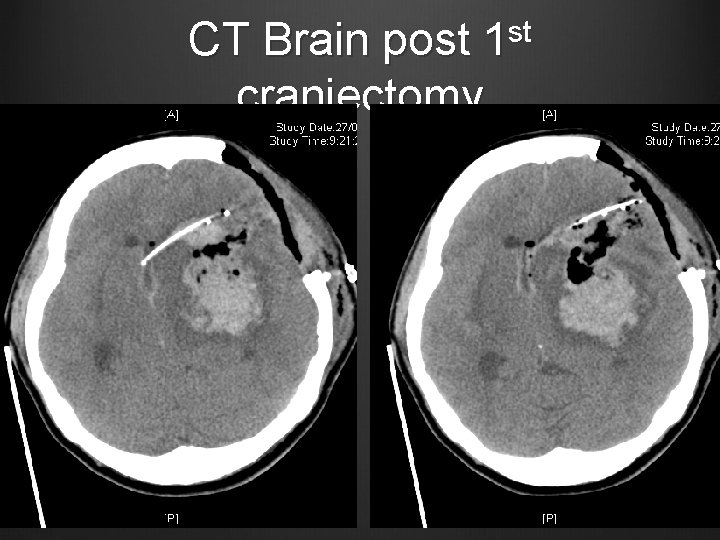
CT Brain post 1 st craniectomy

Case 2 Decided for 2 nd craniectomy + clot evacuation Pupils 3 mm bilaterally post op, reactive CT Brain repeated ~ 3 hours post 2 nd craniectomy
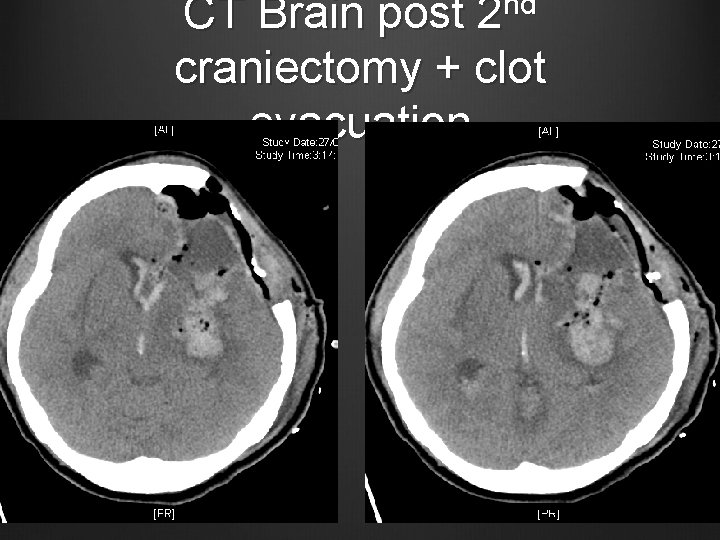
CT Brain post 2 nd craniectomy + clot evacuation

Case 2 BP under control with labetalol infusion, later weaned off to oral amlodipine and methyldopa Mg. SO 4 infusion off, remained seizure free, continued on phenytoin GC remained poor

Case 2 Septic workup negative. Empirically given ceftriaxone Autoimmune markers including ANA, Antids. DNA, Anti. ENA, RF, ANCA, Anticardiolipin Ab were negative ECHO Mild MR, AR, TR LVEF 60% No vegetations No pericardial effusions

Case 2 Noticed asymmetrical pupil sizes with Cushing’s reflex day 5 post op CT Brain repeated
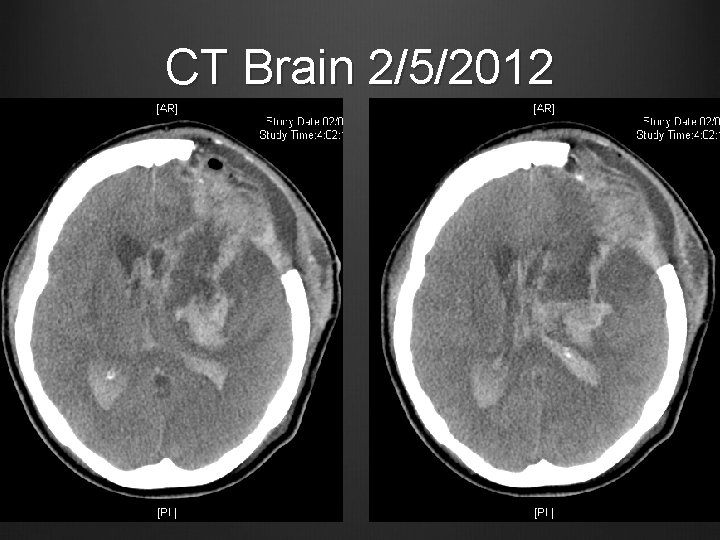
CT Brain 2/5/2012

Case 2 Urgent left craniectomy, clot evacuation, EVD, partial left temporal lobectomy Post op pupils equal CT Brain repeated
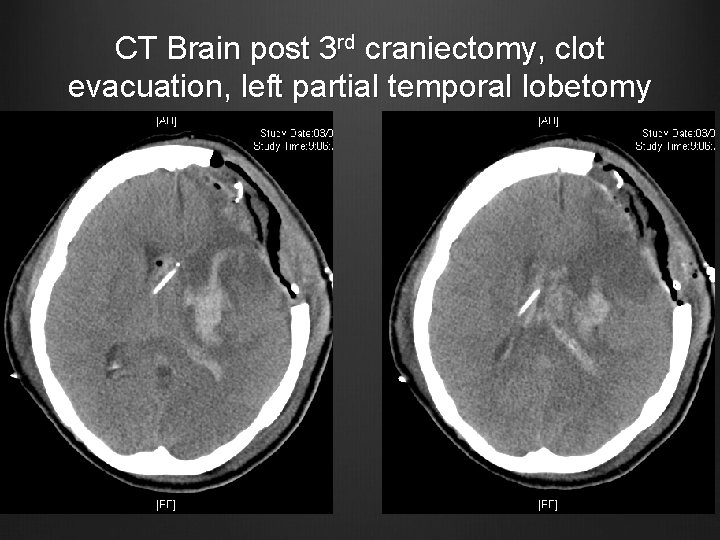
CT Brain post 3 rd craniectomy, clot evacuation, left partial temporal lobetomy

Case 2 Tracheostomized EVD off 11/5/2012 (9 days after last craniectomy) To neurosurgical ward on 12/5/2012 GCS E 4 VTM 4 CT angiogram of brain revealed no aneurysm / AVM

Case 2 Left cranioplasty done, however complicated with wound infection requiring debridement Persistent hydrocephalus on CT Brain with multiple LPs done and eventually VP shunt inserted To Kowloon Hospital with prolonged stay Wean off tracheostomy Dense right hemiplegia, wheelchair bound NG feeding, aphasic
- Slides: 46