Longterm effectiveness and costeffectiveness of cognitive behavioural therapy

Long-term effectiveness and cost-effectiveness of cognitive behavioural therapy for treatment resistant depression in primary care A follow-up of the Co. Bal. T trial Chris Williams on behalf of the Co. Balt Trial Team led by Nicola Wiles, Bristol

Background • Cognitive behavioural therapy (CBT) is an effective treatment for depression • New episodes • Severe and chronic depression • Non-responders to antidepressant medication (Co. Bal. T: 12 month follow-up) • CBT teaches patients skills to help them better manage their mood • Potential for benefit beyond end of therapy • Little evidence of long-term effectiveness • Most trial outcomes 6 -12 months and many small (n<75) • CBT for relapse prevention – benefits only lost after 4 years • Cost-effectiveness data also lacking

Research Objectives Amongst primary care patients with treatment resistant depression: • is CBT (+ usual care that includes pharmacotherapy) effective in reducing depressive symptoms and improving quality of life over the long-term (approximately 4 yrs), compared with usual care alone? • is this strategy cost-effective?

Co. Bal. T trial and inclusion in long-term follow-up • UK multi-centre trial: 73 general practices (Bristol, Exeter and Glasgow) • Eligible patients • 18 -75 years • Adhered to adequate dose of antidepressant medication for at least 6 weeks • Significant depressive symptoms (Beck Depression Inventory score ≥ 14 and met ICD-10 criteria for depression) • Randomised (n = 469) • 12 -18 sessions of individual face-to-face CBT in addition to usual care (incl. antidepressants) • Continue with usual care from their family doctor • Eligible for long-term follow-up (n = 430) • Given consent to be randomised into Co. Bal. T • Had not withdrawn from the study by 12 months • Given written informed consent indicating that they were willing to be re-contacted

Study Outline: Follow-up of participants • Contacted all practices ◦ died ◦ not appropriate to contact (excluded) ◦ moved – new address given or traced • Questionnaire mailing ◦ Additional information for economic evaluation gathered by telephone ◦ Double check of data from primary care medical records for random sample (n=50)

Outcomes • Main (primary) outcome : Beck Depression Inventory (BDI-II) score Secondary outcomes: • Response ◦ At least 50% reduction in symptoms compared to baseline • Remission of symptoms ◦ BDI-II score of < 10 • Percentage reduction in BDI-II score • PHQ-9 • Anxiety GAD-7 • Quality of Life (SF-12)
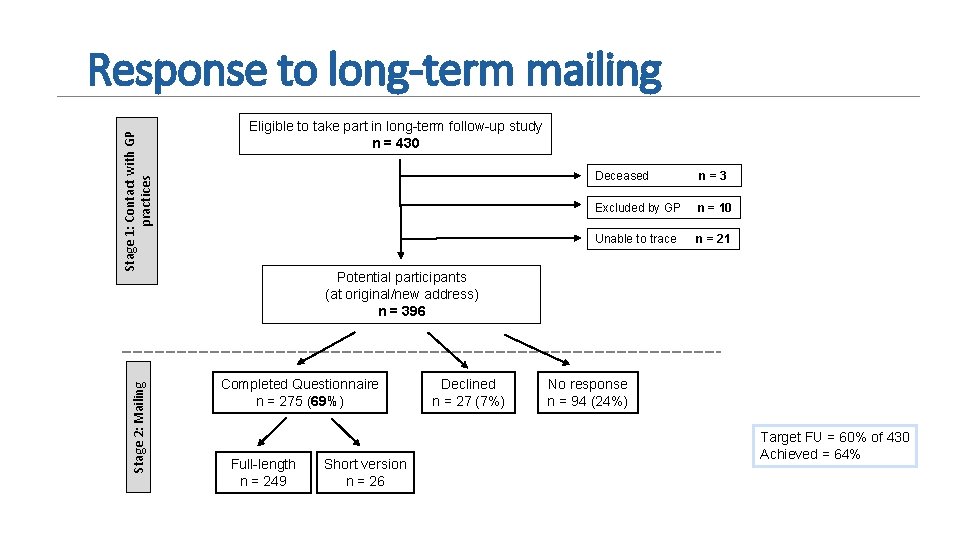
Stage 2: Mailing Stage 1: Contact with GP practices Response to long-term mailing Eligible to take part in long-term follow-up study n = 430 Deceased n=3 Excluded by GP n = 10 Unable to trace n = 21 Potential participants (at original/new address) n = 396 Completed Questionnaire n = 275 (69%) Full-length n = 249 Short version n = 26 Declined n = 27 (7%) No response n = 94 (24%) Target FU = 60% of 430 Achieved = 64%
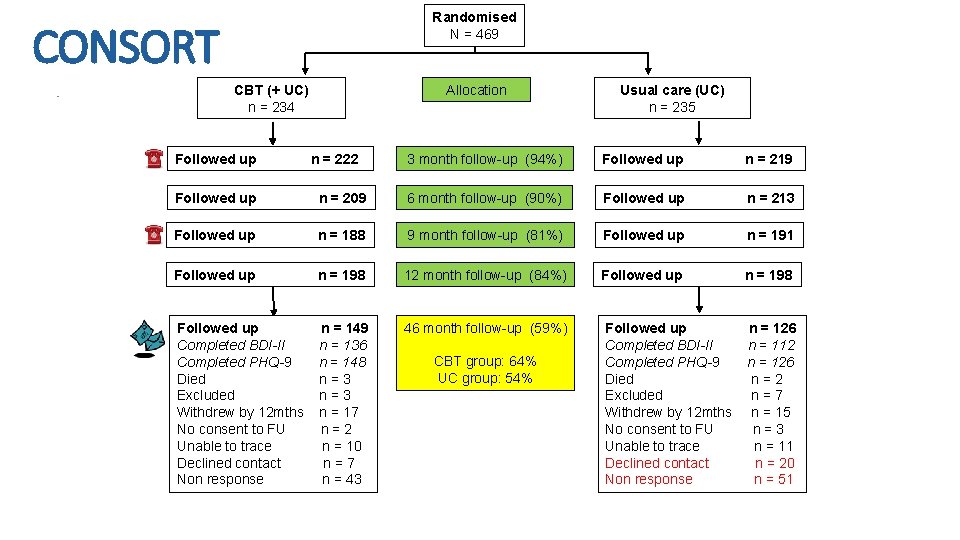
Randomised N = 469 CONSORT CBT (+ UC) n = 234 Followed up Allocation n = 222 Usual care (UC) n = 235 3 month follow-up (94%) Followed up n = 219 Followed up n = 209 6 month follow-up (90%) Followed up n = 213 Followed up n = 188 9 month follow-up (81%) Followed up n = 191 Followed up n = 198 12 month follow-up (84%) Followed up n = 198 Followed up Completed BDI-II Completed PHQ-9 Died Excluded Withdrew by 12 mths No consent to FU Unable to trace Declined contact Non response n = 149 n = 136 n = 148 n=3 n = 17 n=2 n = 10 n=7 n = 43 46 month follow-up (59%) CBT group: 64% UC group: 54% Followed up Completed BDI-II Completed PHQ-9 Died Excluded Withdrew by 12 mths No consent to FU Unable to trace Declined contact Non response n = 126 n = 112 n = 126 n=2 n=7 n = 15 n=3 n = 11 n = 20 n = 51

Length of follow-up and time since end of therapy • Follow-up: median: 45. 5 months since randomisation [IQR: 42. 5, 51. 1] • Range: 38. 4, 61. 6 months • For those who had at least 12 sessions of CBT (n = 105) • average 39. 7 months (SD 5. 2) since end of therapy

Baseline characteristics of Co. Bal. T participants • BDI-II score (mean): 30. 9 (severe range) • Duration of current episode of depression (>2 years): 59% • ICD-10 severe depressive episode: 24% • Physical and psychological co-morbidity common • Secondary diagnosis of an anxiety disorder: 75% • At follow-up • • musculoskeletal problems: n =115 high blood pressure: n = 53 Asthma/chest problems: n = 48 Diabetes: n = 34
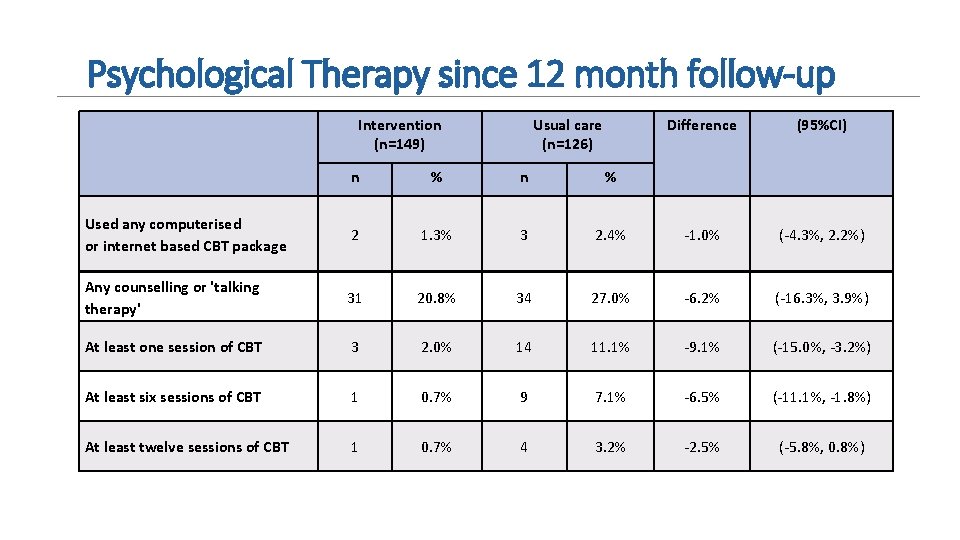
Psychological Therapy since 12 month follow-up Intervention (n=149) Usual care (n=126) Difference (95%CI) n % Used any computerised or internet based CBT package 2 1. 3% 3 2. 4% -1. 0% (-4. 3%, 2. 2%) Any counselling or 'talking therapy' 31 20. 8% 34 27. 0% -6. 2% (-16. 3%, 3. 9%) At least one session of CBT 3 2. 0% 14 11. 1% -9. 1% (-15. 0%, -3. 2%) At least six sessions of CBT 1 0. 7% 9 7. 1% -6. 5% (-11. 1%, -1. 8%) At least twelve sessions of CBT 1 0. 7% 4 3. 2% -2. 5% (-5. 8%, 0. 8%)
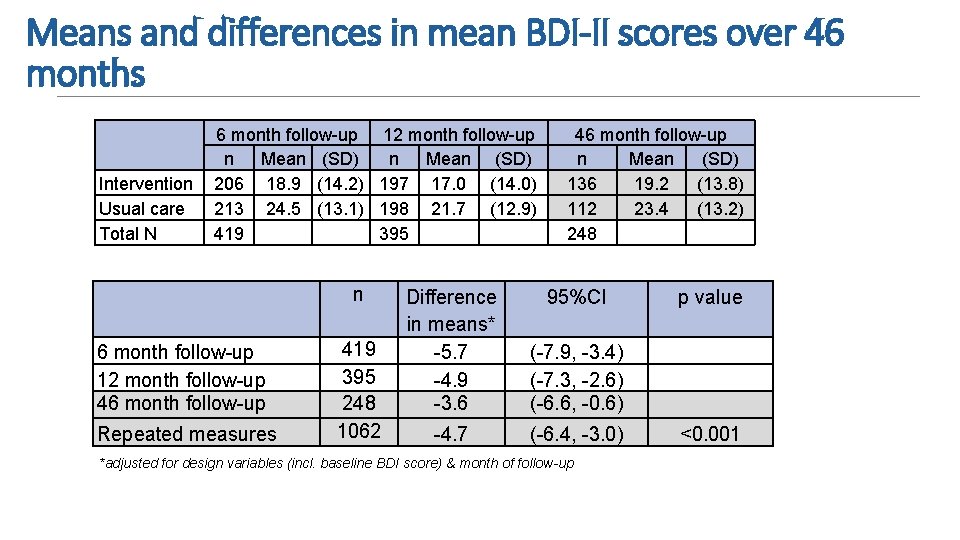
Means and differences in mean BDI-II scores over 46 months Intervention Usual care Total N 6 month follow-up 12 month follow-up n Mean (SD) 206 18. 9 (14. 2) 197 17. 0 (14. 0) 213 24. 5 (13. 1) 198 21. 7 (12. 9) 419 395 n 6 month follow-up 12 month follow-up 46 month follow-up Repeated measures 419 395 248 1062 46 month follow-up n Mean (SD) 136 19. 2 (13. 8) 112 23. 4 (13. 2) 248 Difference in means* -5. 7 -4. 9 -3. 6 95%CI (-7. 9, -3. 4) (-7. 3, -2. 6) (-6. 6, -0. 6) -4. 7 (-6. 4, -3. 0) *adjusted for design variables (incl. baseline BDI score) & month of follow-up p value <0. 001
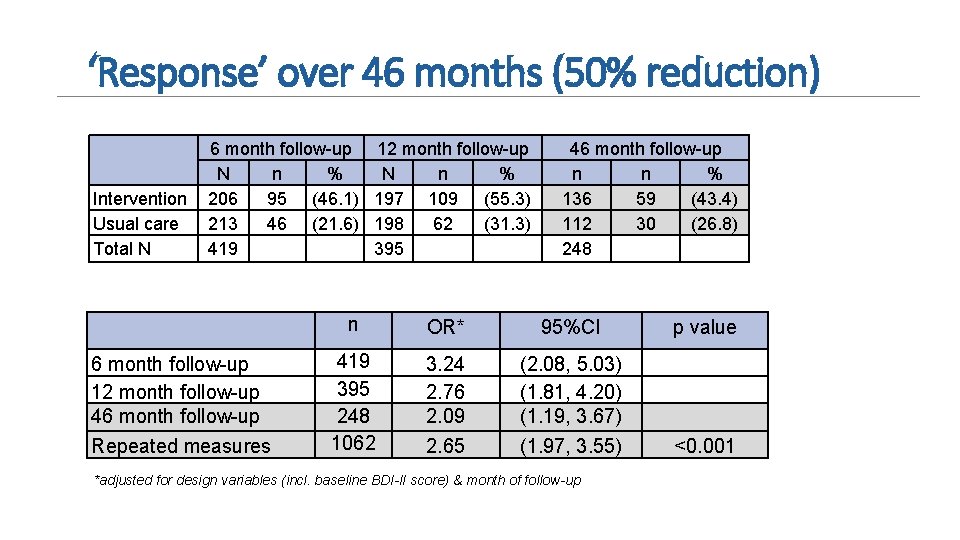
‘Response’ over 46 months (50% reduction) Intervention Usual care Total N 6 month follow-up 12 month follow-up N n % 206 95 (46. 1) 197 109 (55. 3) 213 46 (21. 6) 198 62 (31. 3) 419 395 6 month follow-up 12 month follow-up 46 month follow-up Repeated measures 46 month follow-up n n % 136 59 (43. 4) 112 30 (26. 8) 248 n OR* 95%CI 419 395 248 1062 3. 24 2. 76 2. 09 (2. 08, 5. 03) (1. 81, 4. 20) (1. 19, 3. 67) 2. 65 (1. 97, 3. 55) *adjusted for design variables (incl. baseline BDI-II score) & month of follow-up p value <0. 001
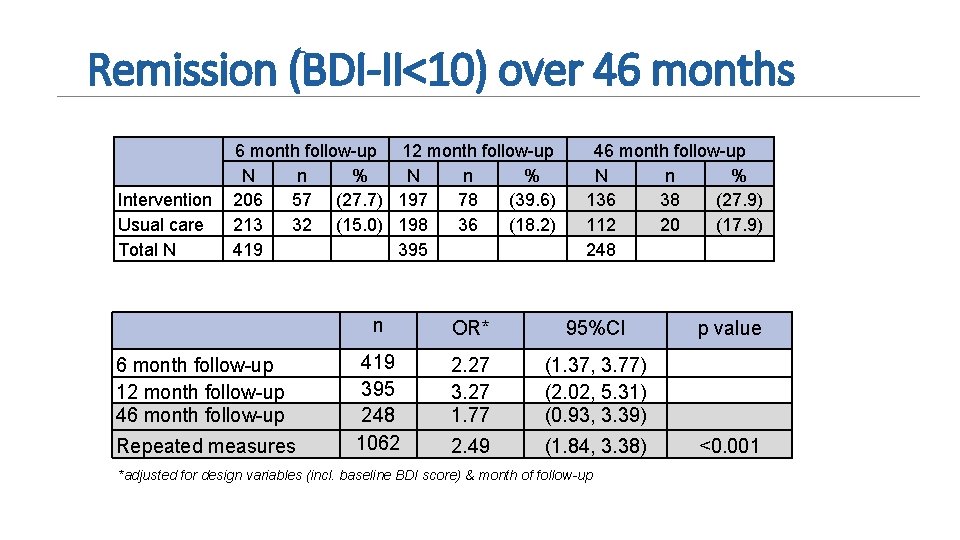
Remission (BDI-II<10) over 46 months Intervention Usual care Total N 6 month follow-up 12 month follow-up N n % 206 57 (27. 7) 197 78 (39. 6) 213 32 (15. 0) 198 36 (18. 2) 419 395 6 month follow-up 12 month follow-up 46 month follow-up Repeated measures 46 month follow-up N n % 136 38 (27. 9) 112 20 (17. 9) 248 n OR* 95%CI 419 395 248 1062 2. 27 3. 27 1. 77 (1. 37, 3. 77) (2. 02, 5. 31) (0. 93, 3. 39) 2. 49 (1. 84, 3. 38) *adjusted for design variables (incl. baseline BDI score) & month of follow-up p value <0. 001

Costs to the Health Service (NHS) and PSS • Perspective – Health Service (NHS) and personal social services (PSS) • Use of health care services • all primary and community care • GP, nurse, other HCP, community etc. • antidepressant medication • hospital (mental health-related) • A&E, outpatient visits, inpatient stays • Personal social services • social worker, day centres, home help • Data from postal questionnaire and medical records (random sample)
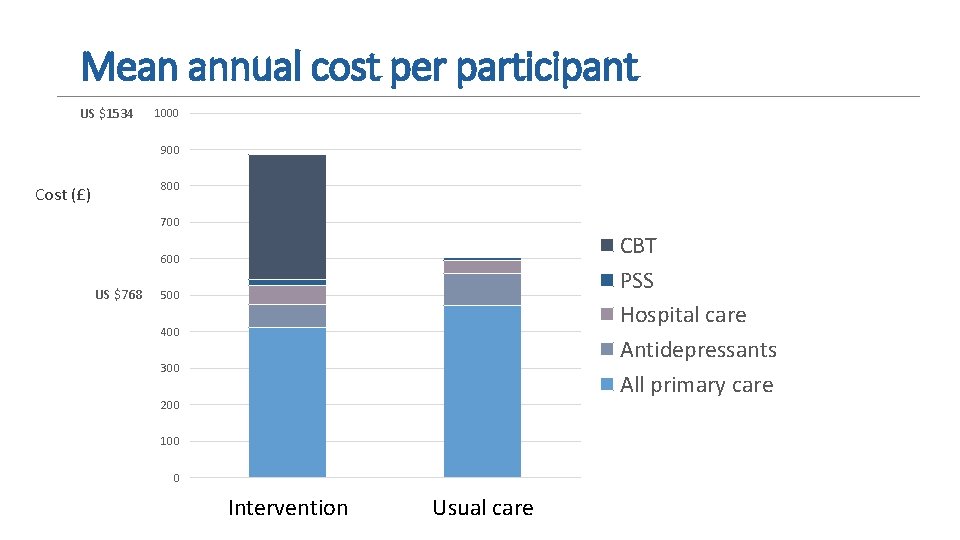
Mean annual cost per participant US $1534 1000 900 800 Cost (£) 700 CBT PSS Hospital care Antidepressants All primary care 600 US $768 500 400 300 200 100 0 Intervention Usual care
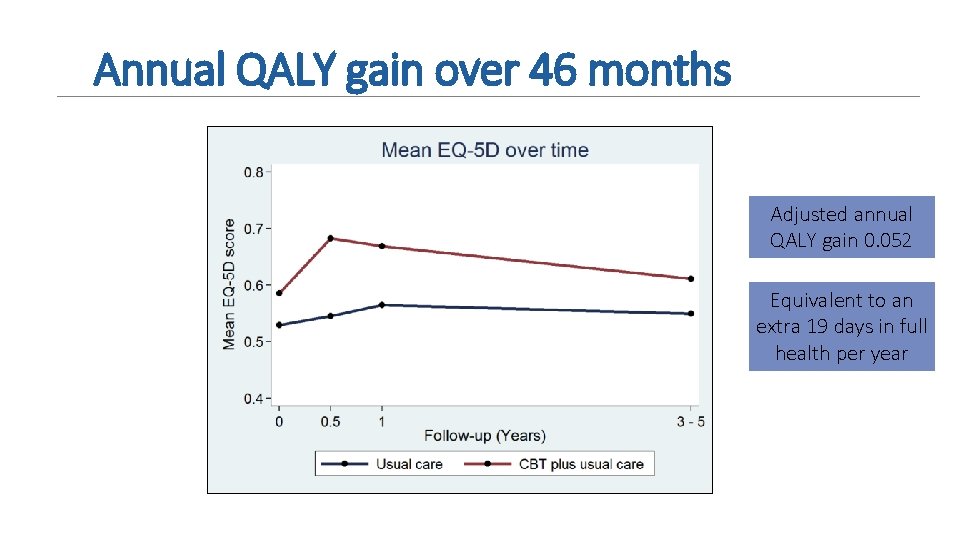
Annual QALY gain over 46 months Adjusted annual QALY gain 0. 052 Equivalent to an extra 19 days in full health per year
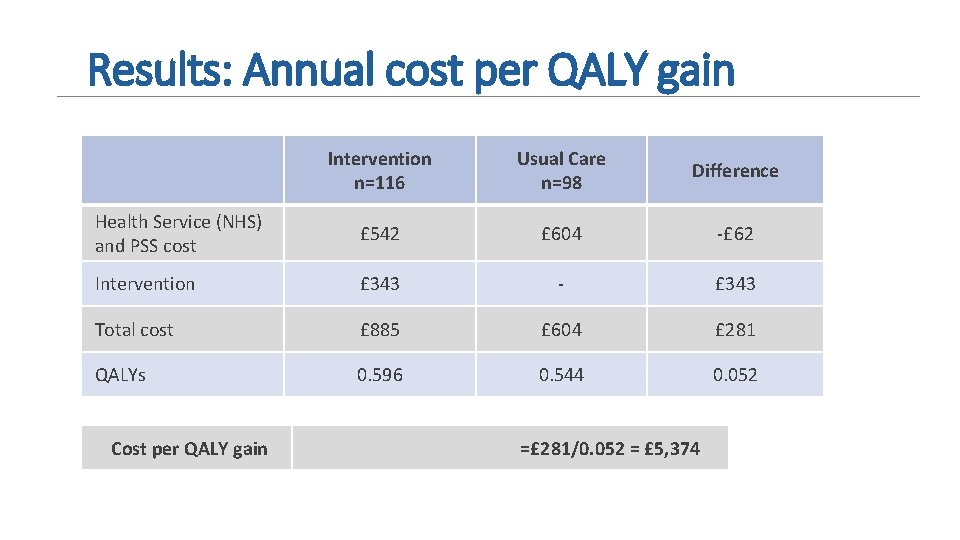
Results: Annual cost per QALY gain Intervention n=116 Usual Care n=98 Difference Health Service (NHS) and PSS cost £ 542 £ 604 -£ 62 Intervention £ 343 - £ 343 Total cost £ 885 £ 604 £ 281 QALYs 0. 596 0. 544 0. 052 Cost per QALY gain =£ 281/0. 052 = £ 5, 374

Summary • CBT as an adjunct to usual care is an effective treatment for primary care patients with TRD over the long-term • reduced depressive symptoms • improved quality of life • average of 40 months after the end of therapy and • Good value for money from the perspective of a healthcare provider

Implications for clinical practice • This is an effective intervention for a population of people not responding to antidepressants alone • Clinicians need to discuss referral for CBT with all those for whom antidepressants are not effective • Initiatives to improve access to psychological treatments have (mainly) increased provision of ‘low intensity’ treatments • Many patients receive less than the 12 -18 sessions of ‘high-intensity’ CBT as delivered in Co. Bal. T • Translating findings into patient benefit will require • more investment • future innovation • how to best use technology to increase efficiency in delivery and maintain these benefits

Conflict of interest declaration CW is President of BABCP- the lead body for CBT in the UK, and a CBT researcher and trainer. He is also author of a range of CBT-based resources that address anxiety, depression and other disorders. These are available commercially as books, c. CBT products, and classes. He receives royalty, and is shareholder and director of a company that commercialises these resources.
- Slides: 21