Long Term Care Objectives 1 Define longterm care

Long -Term Care

Objectives 1) Define long-term care 2) Who uses LTC? 3) Future growth of LTC? 4) Who pays for LTC? 5) Examine the latest approaches taken by Germany, Japan, & U. S. 2

Long-Term Care • Informal care • Home health care • Assisted living/ residential arrangements • Nursing homes Different fields use different terms! LTC: assistance with ADL LTSS: assistance with IADLs 3

Who uses LTC? • 10. 9 Million community residents o ½ are elderly o 92 percent receiving informal care o 13 percent receiving paid care • 1. 8 Million nursing home residents o Almost all elderly • • • Single Female White Poor Childless 4

What does this tell you about the future demands for LTC? • What do Lakdawalla and Philipson think? 5
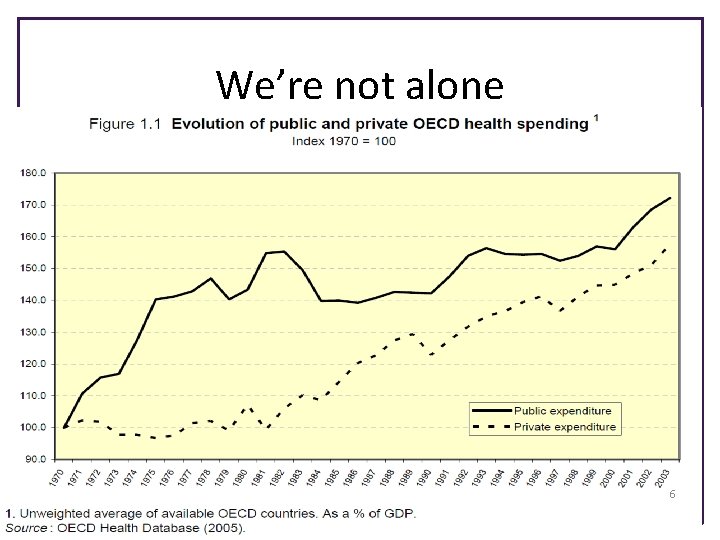
We’re not alone 6
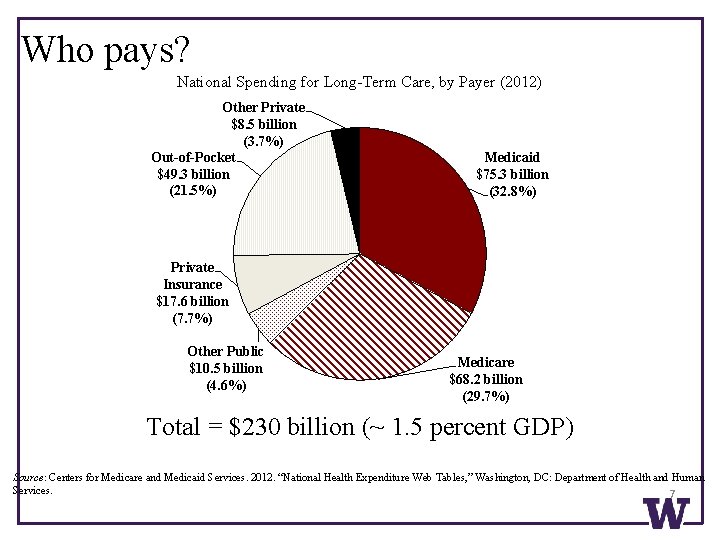
Who pays? National Spending for Long-Term Care, by Payer (2012) Other Private $8. 5 billion (3. 7%) Out-of-Pocket $49. 3 billion (21. 5%) Medicaid $75. 3 billion (32. 8%) Private Insurance $17. 6 billion (7. 7%) Other Public $10. 5 billion (4. 6%) Medicare $68. 2 billion (29. 7%) Total = $230 billion (~ 1. 5 percent GDP) Source: Centers for Medicare and Medicaid Services. 2012. “National Health Expenditure Web Tables, ” Washington, DC: Department of Health and Human Services. 7
Compare to acute care spending… • And over time… • http: //www. chcf. org/publications/2014/07/d ata-viz-hcc-national 8
Home health care insurance Medicare – 43% • Homebound, need part-time or intermittent skilled care • $2. 2 billion in 1989 - $33. 8 billion in 2012 Beneficiaries doubled, visits tripled Medicaid – 37% • Waiver program started in 1970’s • 28. 9 billion in 2012: more than nursing home care Private Insurance – 7% Source: Centers for Medicare and Medicaid Services. 2012. “National Health Expenditures by type of service and source of funds, CY 1960 -2012. ” Washington, DC: Department of Health and Human Services. 9
Nursing home insurance Medicare – 23% • Dismissed from hospital with 30 days • Chance of recovery • First 100 days Medicaid – 31% • Means tested • Unlimited benefit once qualify Private Insurance – 8% • ~15 percent of current 65+ have private insurance. Source: (1) Centers for Medicare and Medicaid Services. 2012. “National Health Expenditure Web Tables, ” Washington, DC: Department of Health 10 and Human Services. (2) University of Michigan. Health and Retirement Study (HRS) 2012. Ann Arbor, MI.

Who should pay? Different countries take different approaches • Social insurance • Users • Children • Charities/religious organizations What should be included? • “hotel costs” or just care? 11
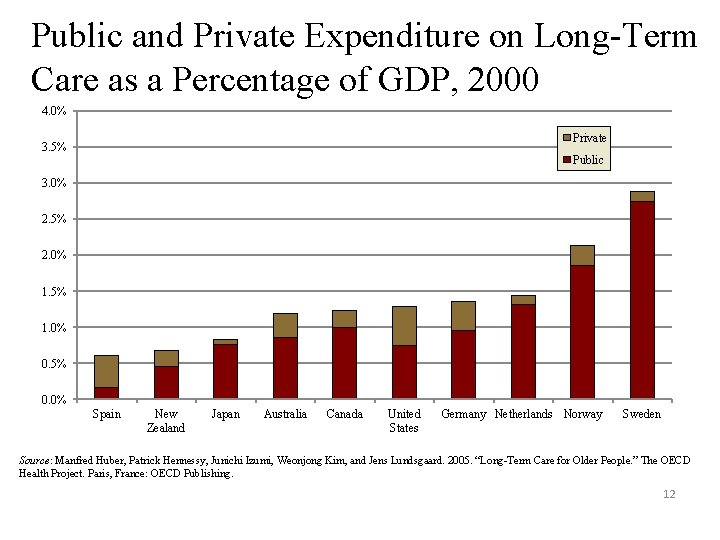
Public and Private Expenditure on Long-Term Care as a Percentage of GDP, 2000 4. 0% Private 3. 5% Public 3. 0% 2. 5% 2. 0% 1. 5% 1. 0% 0. 5% 0. 0% Spain New Zealand Japan Australia Canada United States Germany Netherlands Norway Sweden Source: Manfred Huber, Patrick Hennessy, Junichi Izumi, Weonjong Kim, and Jens Lundsgaard. 2005. “Long-Term Care for Older People. ” The OECD Health Project. Paris, France: OECD Publishing. 12
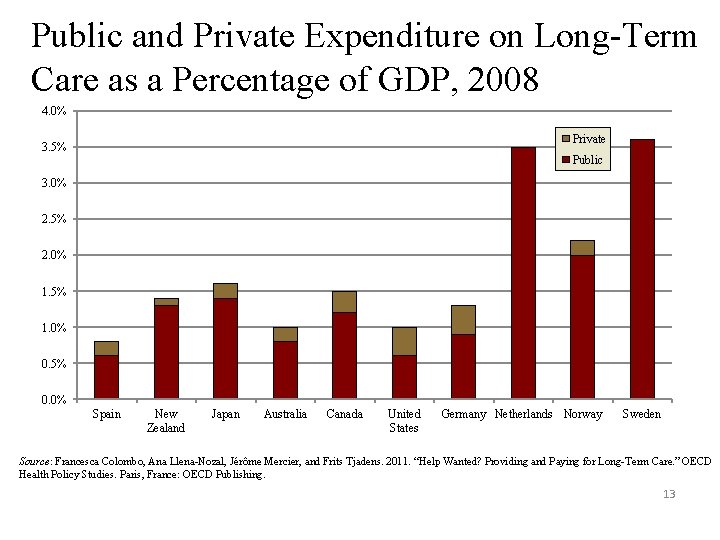
Public and Private Expenditure on Long-Term Care as a Percentage of GDP, 2008 4. 0% Private 3. 5% Public 3. 0% 2. 5% 2. 0% 1. 5% 1. 0% 0. 5% 0. 0% Spain New Zealand Japan Australia Canada United States Germany Netherlands Norway Sweden Source: Francesca Colombo, Ana Llena-Nozal, Jérôme Mercier, and Frits Tjadens. 2011. “Help Wanted? Providing and Paying for Long-Term Care. ” OECD Health Policy Studies. Paris, France: OECD Publishing. 13
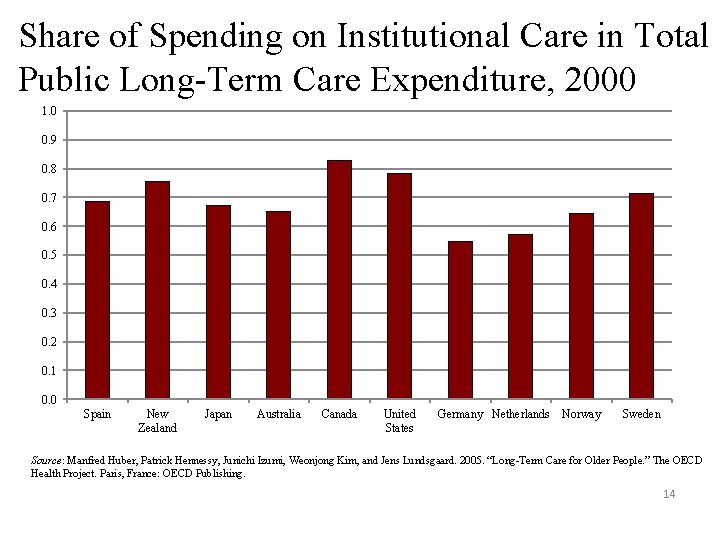
Share of Spending on Institutional Care in Total Public Long-Term Care Expenditure, 2000 1. 0 0. 9 0. 8 0. 7 0. 6 0. 5 0. 4 0. 3 0. 2 0. 1 0. 0 Spain New Zealand Japan Australia Canada United States Germany Netherlands Norway Sweden Source: Manfred Huber, Patrick Hennessy, Junichi Izumi, Weonjong Kim, and Jens Lundsgaard. 2005. “Long-Term Care for Older People. ” The OECD Health Project. Paris, France: OECD Publishing. 14
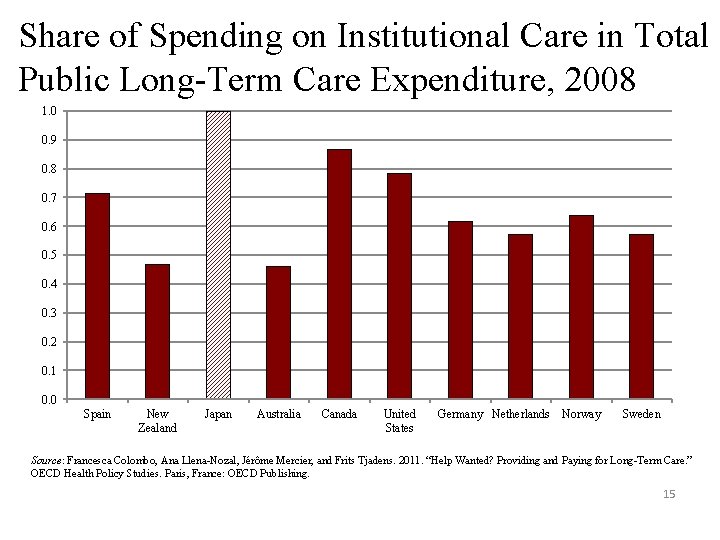
Share of Spending on Institutional Care in Total Public Long-Term Care Expenditure, 2008 1. 0 0. 9 0. 8 0. 7 0. 6 0. 5 0. 4 0. 3 0. 2 0. 1 0. 0 Spain New Zealand Japan Australia Canada United States Germany Netherlands Norway Sweden Source: Francesca Colombo, Ana Llena-Nozal, Jérôme Mercier, and Frits Tjadens. 2011. “Help Wanted? Providing and Paying for Long-Term Care. ” OECD Health Policy Studies. Paris, France: OECD Publishing. 15
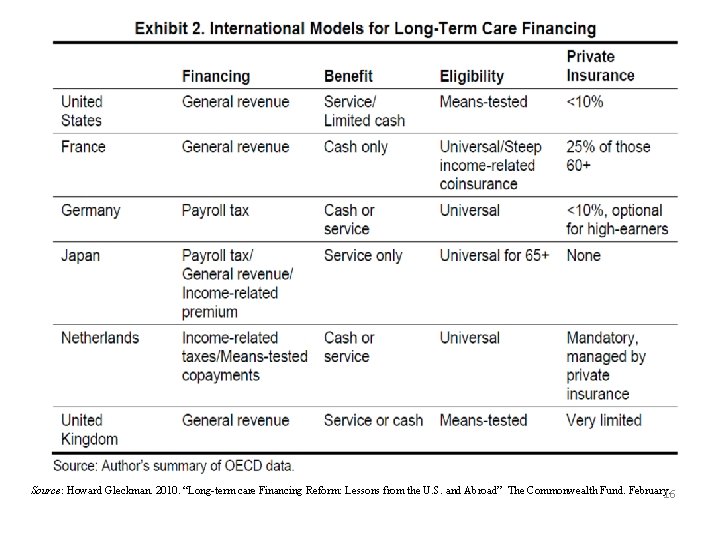
Source: Howard Gleckman. 2010. “Long-term care Financing Reform: Lessons from the U. S. and Abroad” The Commonwealth Fund. February. 16

LTC insurance: Germany • Compulsory Statutory Social Insurance (1995) o Self-employed and rich may opt out o 75 percent must, 90 percent covered in pubic system • All workers (and employers) pay premium (1. 95 percent) o Not-working and spouses covered o One less holiday • Childless adults pay higher premium (2001; effective 2005) Source: (1) Heinz Rothgang. 2010. “Social Insurance for Long-term Care: An Evaluation of the German Model. ” Social Policy & Administration 44(4): 436 -460. (2) Katrin Heinick and Stephan L. Thomsen. 2010. “The Social Long-Term Care Insurance in Germany: Origin, Situation, Threats and Perspectives. ” Discussion Paper No. 10 -012. Mannheim, Germany: Center for European Economic Research. 17
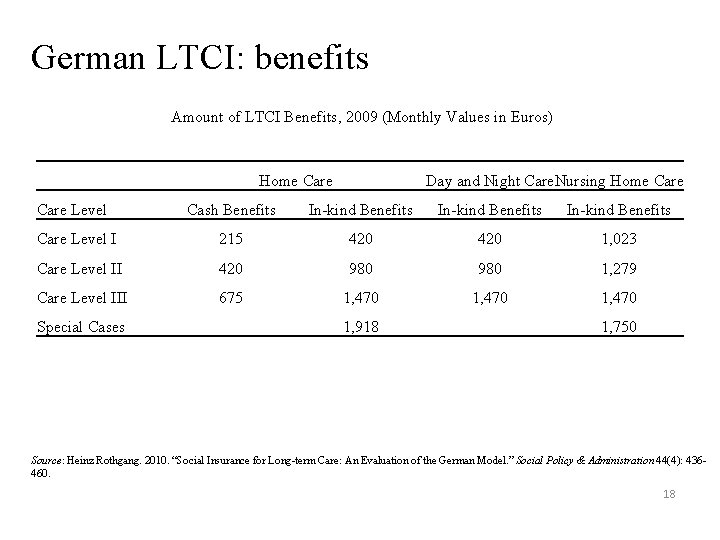
German LTCI: benefits Amount of LTCI Benefits, 2009 (Monthly Values in Euros) Home Care Day and Night Care. Nursing Home Care Level Cash Benefits In-kind Benefits Care Level I 215 420 1, 023 Care Level II 420 980 1, 279 Care Level III 675 1, 470 Special Cases 1, 918 1, 750 Source: Heinz Rothgang. 2010. “Social Insurance for Long-term Care: An Evaluation of the German Model. ” Social Policy & Administration 44(4): 436460. 18
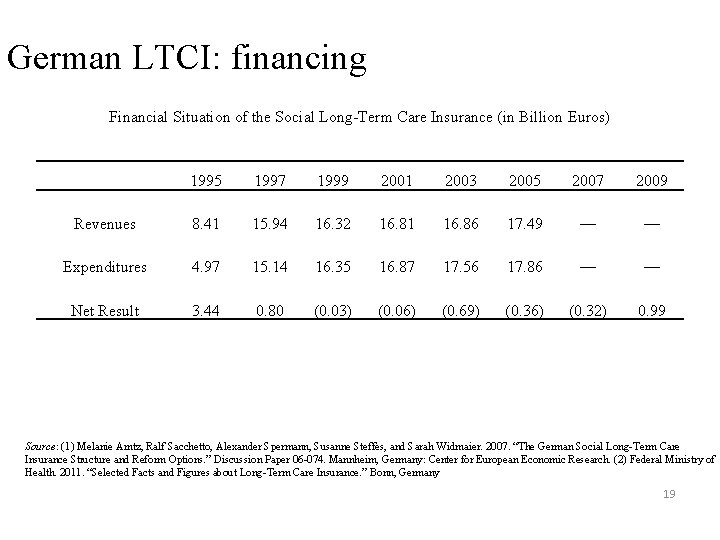
German LTCI: financing Financial Situation of the Social Long-Term Care Insurance (in Billion Euros) 1995 1997 1999 2001 2003 2005 2007 2009 Revenues 8. 41 15. 94 16. 32 16. 81 16. 86 17. 49 — — Expenditures 4. 97 15. 14 16. 35 16. 87 17. 56 17. 86 — — Net Result 3. 44 0. 80 (0. 03) (0. 06) (0. 69) (0. 36) (0. 32) 0. 99 Source: (1) Melanie Arntz, Ralf Sacchetto, Alexander Spermann, Susanne Steffes, and Sarah Widmaier. 2007. “The German Social Long-Term Care Insurance Structure and Reform Options. ” Discussion Paper 06 -074. Mannheim, Germany: Center for European Economic Research. (2) Federal Ministry of Health. 2011. “Selected Facts and Figures about Long-Term Care Insurance. ” Bonn, Germany 19

LTC in Japan • April 2000: Mandatory insurance for 40+ – – Services accessible 65+ (with exceptions for younger) 50% taxes, 50% income-related premiums 10% co-insurance rate Govt sets premiums and prices for services • Emphasis on HCBC – Reduce family burden – 203% increase in use – (83% increase in institutional use) • Financial sustainability remains an issue – 16% eligible instead of estimated 12% 20

LTC insurance: U. S. Private LTCI rates are currently low. Why? (Brown and Finkelstein) 21

CLASS Act • Community Living Assistance Services and Supports Act o Part of Patient Protection and Affordable Care Act – ACA • Employer-offered benefit • Voluntary program • Automatic enrollment if employer offers plan • Lifetime coverage after 5 -years of premium payments • Benefit: cash -based on severity of need ~$75/day Source: Alicia H. Munnell, and Josh Hurwitz. 2011. “What is “CLASS’? And Will it Work? ” Issue in Brief 11 -3. Chestnut Hill, MA: Center for Retirement Research at Boston College. 22

CLASS Act (cont’d) • Premiums: ~$123/month o Assumes 10 million take-up (3. 5% of adults) o Do not vary based on gender, marital status, children, health o Will not increase except…. • Premiums subsidized o Working college students o Below poverty line Source: Alicia H. Munnell, and Josh Hurwitz. 2011. “What is “CLASS’? And Will it Work? ” Issue in Brief 11 -3. Chestnut Hill, MA: Center for Retirement Research at Boston College. 23

CLASS Act – potential problems? 24 18

Cash and Counseling Demonstration and Evaluation Project (CCDE) • Within the HCBS program • Treatment group: received a flexible budget and decide what mix of goods and services best meet their personal care needs. • Control group: eligible for the standard agencyprovided home care • Well-designed and implemented randomization 25

CCDE has been studied… a lot • Cash & Counseling: – reduced unmet needs – participants experienced positive health outcomes – improved quality of life for participants and their caregivers – did not result in misuse of funds or abuse of patients – Increased Medicaid costs • enrollees received more of the care they qualified for • partially offset by savings in institutional and other long-term -care costs 26

Coe et al. (2015) paper: • Use the CCDE randomization as an instrument for the type of care received: – Agency care: Paid care in the home provided by a Medicaid-approved agency – Family Care: Care provided by family and friends • Paid OR unpaid, largely untrained – Treatment more likely to get Agency+Family compared to Agency-only care than Control group • What is the marginal benefit of Family Care? – For Medicaid spending? – What does it mean for quality of care? 27
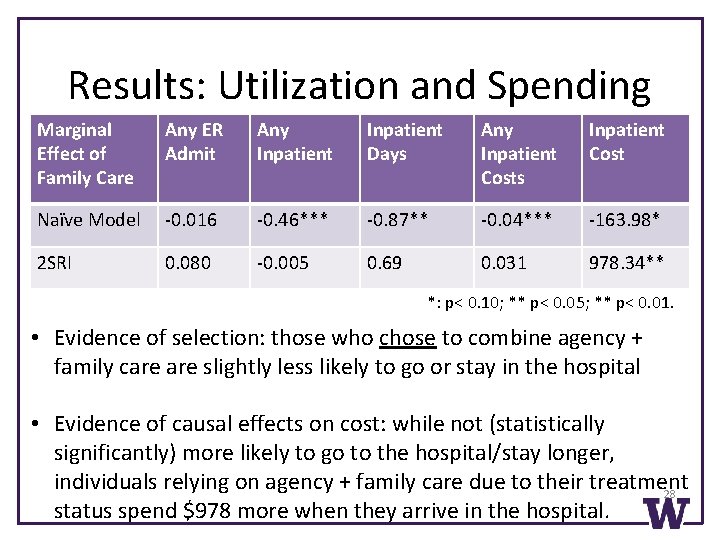
Results: Utilization and Spending Marginal Effect of Family Care Any ER Admit Any Inpatient Days Any Inpatient Costs Inpatient Cost Naïve Model -0. 016 -0. 46*** -0. 87** -0. 04*** -163. 98* 2 SRI 0. 080 -0. 005 0. 69 0. 031 978. 34** *: p< 0. 10; ** p< 0. 05; ** p< 0. 01. • Evidence of selection: those who chose to combine agency + family care slightly less likely to go or stay in the hospital • Evidence of causal effects on cost: while not (statistically significantly) more likely to go to the hospital/stay longer, individuals relying on agency + family care due to their treatment 28 status spend $978 more when they arrive in the hospital.
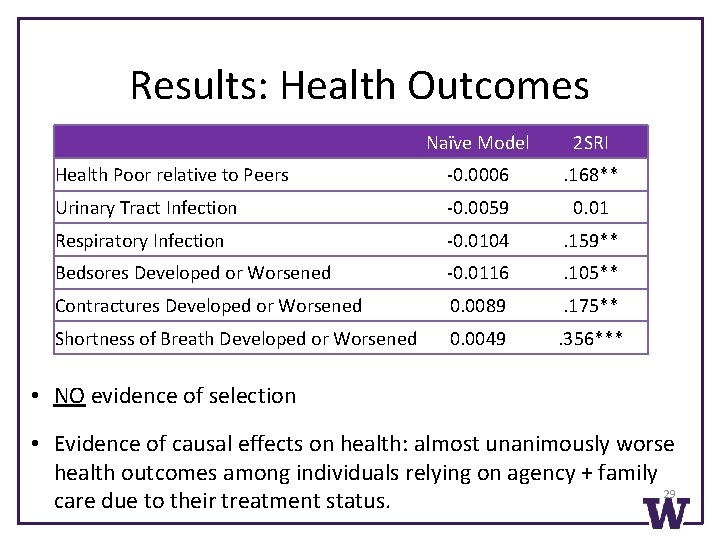
Results: Health Outcomes Naïve Model 2 SRI Health Poor relative to Peers -0. 0006 . 168** Urinary Tract Infection -0. 0059 0. 01 Respiratory Infection -0. 0104 . 159** Bedsores Developed or Worsened -0. 0116 . 105** Contractures Developed or Worsened 0. 0089 . 175** Shortness of Breath Developed or Worsened 0. 0049 . 356*** • NO evidence of selection • Evidence of causal effects on health: almost unanimously worse health outcomes among individuals relying on agency + family 29 care due to their treatment status.

Summary • LTC expensive • Historically separate from acute care – may change • Insurance is partial in U. S. o Form of insurance influences who gets what care • LOTS of international variation on how to o Finance o Insure o Delivery • Concerns about financing have to be balances with quality concerns 30
- Slides: 30